Deep vein thrombosis
|
Deep Vein Thrombosis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Special Scenario |
|
Trials |
|
Case Studies |
|
Deep vein thrombosis On the Web |
For patient information page, click here
For main page on Venous Thrombosis, click here
| Deep vein thrombosis | |
| ICD-10 | I80.2 |
|---|---|
| ICD-9 | 453.40 |
| DiseasesDB | 3498 |
| MeSH | D020246 |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor-In-Chief: Cafer Zorkun, M.D., Ph.D. [2] Ujjwal Rastogi, MBBS [3]
Overview
Pathophysiology
Epidemiology and Demographics
Risk factors
Diagnosis
Treatment
Medical Therapy | Surgery | Primary Prevention | Secondary Prevention
Signs and symptoms
There may be no symptoms referrable to the location of the DVT, but the classical symptoms of DVT include pain, swelling and redness of the leg and dilation of the surface veins. In up to 25% of all hospitalized patients, there may be some form of DVT, which often remains clinically inapparent (unless pulmonary embolism develops).
There are several techniques during physical examination to increase the detection of DVT, such as measuring the circumference of the affected and the contralateral limb at a fixed point (to objectivate edema), and palpating the venous tract, which is often tender. Physical examination is unreliable for excluding the diagnosis of deep vein thrombosis.
In phlegmasia alba dolens, the leg is pale and cool with a diminished arterial pulse due to spasm. It usually results from acute occlusion of the iliac and femoral veins due to DVT.
In phlegmasia cerulea dolens, there is an acute and nearly total venous occlusion of the entire extremity outflow, including the iliac and femoral veins. The leg is usually painful, cyanosed and oedematous. Venous gangrene may supervene.
It is vital that the possibility of pulmonary embolism be included in the history, as this may warrant further investigation (see pulmonary embolism).
A careful history has to be taken considering risk factors (see below), including the use of estrogen-containing methods of hormonal contraception, recent long-haul flying, and a history of miscarriage (which is a feature of several disorders that can also cause thrombosis). A family history can reveal a hereditary factor in the development of DVT.
-
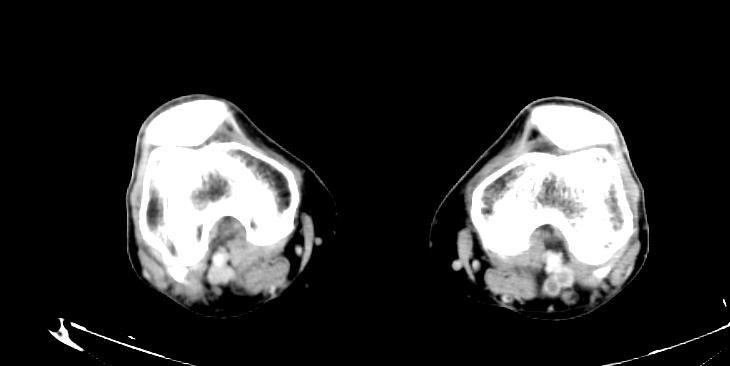
Deep venous thrombosis
-
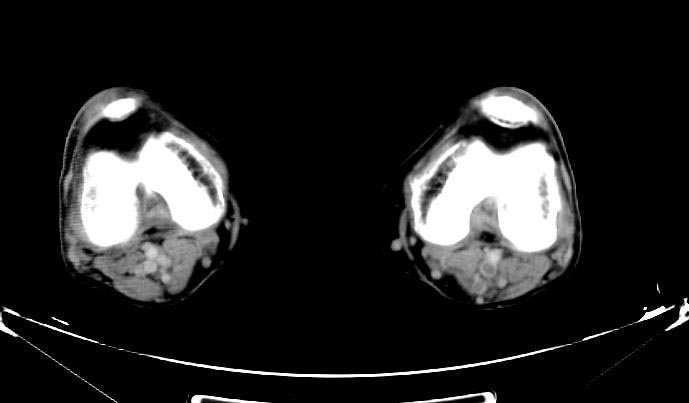
Deep venous thrombosis
-
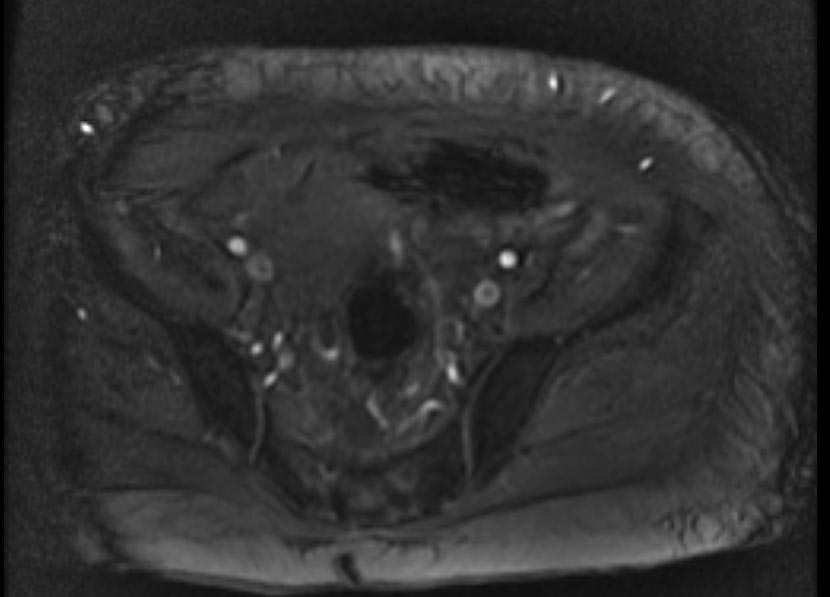
Deep venous thrombosis
Physical examination
- Homan's test: Dorsiflexion of foot elicits pain in posterior calf
- Pratt's sign: Squeezing of posterior calf elicits pain
However, these medical signs do not perform well and are not included in clinical prediction rules that combine best findings in order to diagnose DVT.[1]
Probability scoring
In 2006, Scarvelis and Wells overviewed a set of clinical prediction rules for DVT,[2] on the heels of a widely adopted set of clinical criteria for pulmonary embolism.[3][4]
Wells score or criteria
(Possible score -2 to 9)
- 1) Active cancer (treatment within last 6 months or palliative) -- 1 point
- 2) Calf swelling >3 cm compared to other calf (measured 10 cm below tibial tuberosity) -- 1 point
- 3) Collateral superficial veins (non-varicose) -- 1 point
- 4) Pitting edema (confined to symptomatic leg) -- 1 point
- 5) Swelling of entire leg - 1 point
- 6) Localized pain along distribution of deep venous system -- 1 point
- 7) Paralysis, paresis, or recent cast immobilization of lower extremities -- 1 point
- 8) Recently bedridden > 3 days, or major surgery requiring regional or general anesthetic in past 12 weeks -- 1 point
- 9) Previously documented DVT -- 1 point
- 10) Alternative diagnosis at least as likely -- Subtract 2 points
Interpretation
- Score of 2 or higher - deep vein thrombosis is likely. Consider imaging the leg veins.
- Score of less than 2 - deep vein thrombosis is unlikely. Consider blood test such as d-dimer test to further rule out deep vein thrombosis.
Blood tests
D-dimer
In a low-probability situation, current practice is to commence investigations by testing for D-dimer levels. This cross-linked fibrin degradation product is an indication that thrombosis is occurring, and that the blood clot is being dissolved by plasmin. A low D-dimer level should prompt other possible diagnoses (such as a ruptured Baker's cyst, if the patient is at sufficiently low clinical probability of DVT.[5][6]
Other blood tests
Other blood tests usually performed at this point are:
- complete blood count
- Primary coagulation studies: PT, APTT, Fibrinogen
- liver enzymes
- renal function and electrolytes
Imaging the leg veins
Impedance plethysmography, Doppler ultrasonography, compression ultrasound scanning of the leg veins, combined with duplex measurements (to determine blood flow), can reveal a blood clot and its extent (i.e. whether it is below or above the knee).
Examples
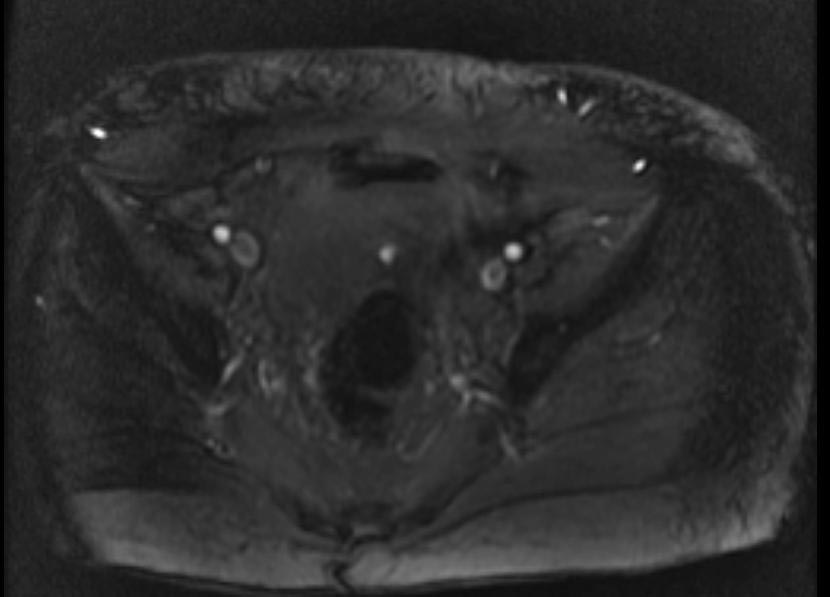
- Example #1: CT images: DVT at left leg
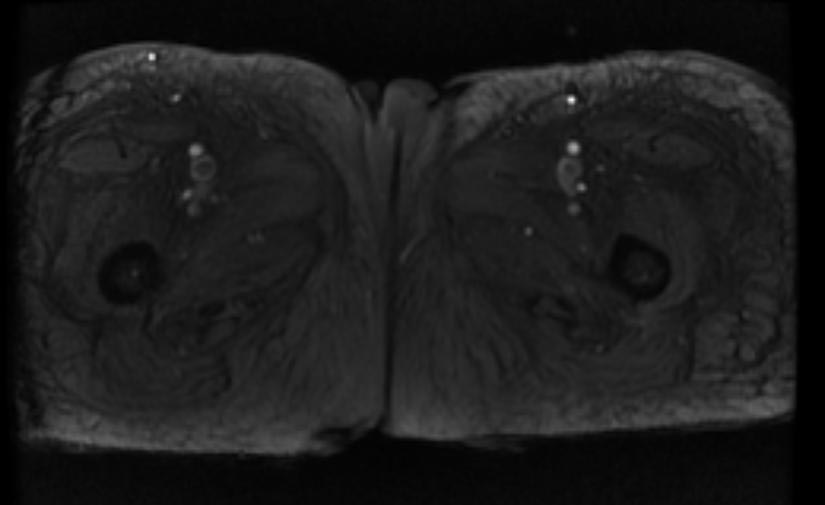
- Example #2: 2D TOF GRE MRV images: Bilateral deep vein thromboses
Prognosis
Post-phlebitic syndrome occurs in 10% of patients with deep vein thrombosis (DVT). It presents with leg oedema, pain, nocturnal cramping, venous claudication, skin pigmentation, dermatitis and ulceration (usually on the medial aspect of the lower leg).
Ongoing Health Care Needs
Medicines that thin your blood and prevent blood clots are used to treat DVT. These medicines can thin your blood too much and cause bleeding (sometimes inside the body). This side effect can be life threatening.
Bleeding may occur in the digestive system or the brain. Signs and symptoms of bleeding in the digestive system include:
- Bright red vomit or vomit that looks like coffee grounds
- Bright red blood in your stools or black, tarry stools
- Pain in your abdomen
Signs and symptoms of bleeding in the brain include:
- Severe pain in your head
- Sudden changes in your vision
- Sudden loss of movement in your arms or legs
- Memory loss or confusion
If you have any of these signs or symptoms, get treatment right away.
References
- ↑ Wells PS, Owen C, Doucette S, Fergusson D, Tran H (2006). "Does this patient have deep vein thrombosis?". JAMA. 295 (2): 199–207. doi:10.1001/jama.295.2.199. PMID 16403932.
- ↑ Scarvelis D, Wells P (2006). "Diagnosis and treatment of deep-vein thrombosis". CMAJ. 175 (9): 1087–92. PMID 17060659. Free Full Text.
- ↑ Neff MJ. ACEP releases clinical policy on evaluation and management of pulmonary embolism. American Family Physician. 2003; 68(4):759-?. Available at: http://www.aafp.org/afp/20030815/practice.html. Accessed on: December 8, 2006.
- ↑ Wells P, Anderson D, Rodger M, Ginsberg J, Kearon C, Gent M, Turpie A, Bormanis J, Weitz J, Chamberlain M, Bowie D, Barnes D, Hirsh J (2000). "Derivation of a simple clinical model to categorize patients probability of pulmonary embolism: increasing the models utility with the SimpliRED D-dimer". Thromb Haemost. 83 (3): 416–20. PMID 10744147.
- ↑ Wells PS, Anderson DR, Rodger M; et al. (2003). "Evaluation of D-dimer in the diagnosis of suspected deep-vein thrombosis". N. Engl. J. Med. 349 (13): 1227–35. doi:10.1056/NEJMoa023153. PMID 14507948.
- ↑ Bates SM, Kearon C, Crowther M; et al. (2003). "A diagnostic strategy involving a quantitative latex D-dimer assay reliably excludes deep venous thrombosis". Ann. Intern. Med. 138 (10): 787–94. PMID 12755550.
See also
ar:تجلط الوريد العميق it:Trombosi venosa profonda nl:Diep-veneuze trombose