Childbirth
| https://https://www.youtube.com/watch?v=s1EXJYKtxHs%7C350}} |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Childbirth (also called labour, birth, partus or parturition) is the culmination of a human pregnancy or gestation period with the delivery of one or more newborn infants from a woman's uterus. The process of human childbirth is categorized in 3 stages of labour. In the first stage, the uterus begins rhythmic contractions which steadily increase in strength and frequency, gradually widening and thinning the cervix. During the second stage, the infant passes from the uterus, through the cervix and birth canal. In the third stage, the placenta pulls from the uterine wall and is expelled through the birth canal.[1]
The Natural Birth

First Stage: Contractions
Normal childbirth begins with the onset of contractions of the uterus. The frequency and duration of these contractions varies with the individual. The onset of labour may be sudden or gradual, and is defined as regular uterine activity in the presence of cervical dilatation.
During a contraction, long muscles of the uterus contract, starting at the top of the uterus and working their way down to the bottom. At the end of the contraction, the muscles relax to a state shorter than at the beginning of the contraction. This draws the cervix up over the baby's head. Each contraction dilates the cervix until it becomes completely dilated, often referred to as 10+ centimeters (cm) or 4+ inches (in) in diameter by midwives or doctors.
A gradual onset with slow cervical change towards 3 cm (just over 1 inch) dilation is referred to as the "latent phase". A woman is said to be in "active labour" when contractions have become regular in frequency (3 to 4 in 10 minutes) and about 60 seconds in duration. The cervix must shorten (efface) before it can dilate; for women giving birth for the first time, this can take a substantial period of time and can be a tiring and difficult time. However, once the cervix is effaced dilatation can occur and the downward journey of the baby can commence. The now powerful contractions are accompanied by cervical effacement and dilation greater than 3 cm (1¼ in) . The labour may begin with a rupture of the amniotic sac, the paired amnion and chorion ("breaking of the water"). The contractions will strengthen and accelerate in frequency. In the "transition phase" from 8 cm–10 cm (3 or 4 in) of dilation, the contractions often come every two minutes and typically last 70–90 seconds. Transition is often regarded as the most challenging and intense for the woman. It is also the shortest phase.
During this stage, the woman giving birth typically goes through several emotional phases. At first, she may be excited and nervous. Then, as the contractions become stronger, demanding more energy from the woman, she may become more serious and focused. However, as the cervix finishes its dilation, some women experience confusion or bouts of self-doubt or giving up. It is important during this time for the birth partners to stay positive and supportive of the woman; to actively encourage if this is what she wishes and to provide nutrition and hydration in order to keep her energy reserves up.
The duration of labour varies widely, but averages some 13 hours for women giving birth to their first child ("primiparae") and 8 hours for women who have already given birth ("multiparae").
If there is a significant medical risk to continuing the pregnancy, induction may be necessary. As this carries some risk, it is only done if the fetus or the woman are in danger from prolonged pregnancy. Forty-two weeks' gestation without spontaneous labour is often said to be an indication for induction although evidence does not show improved outcomes when labour is induced for post-term pregnancies. Inducing labour increases the risk of cesarean section uterine rupture in women that have had a previous cesarean section.
Second Stage: Delivery
In the second stage of labour, the baby is pushed through the womb through the vagina by both the uterine contractions and by the additional maternal efforts of "bearing down," which many women describe as similar in sensation to straining to expel a large bowel movement. The imminence of this stage can be evaluated by the Malinas score. In a vertex (normal head first delivery) when the top of the head is visible at the vagina or in other words the birth canal, this is called crowning (the perineum or the region between the vagina and anus could tear or needs to be cut in a procedure called episiotomy); at this point the woman may feel a burning or stinging sensation, but this soon passes (some people refer the crowning stage as 'The ring of fire').
This stage begins when the cervix is fully dilated. This can be determined by the woman's onset of her desire to 'push' or it can be determined by performing a vaginal exam.
Mechanism of Labor-(Head First) Flexion, Internal Rotation, Extension, External Rotation, Expulsion. Flexion- When the descending head meets resistance if flexes so that the chin is brought closer to the chest. Internal Rotation- It begins at the ischial spine and is not completed until it reaches lower pelvis. Extension- When fetal head reaches perineum it is deflected anteriorly by perineum. External Rotation-After head is born it rotates 45 degrees to realign with its shoulders and back. Expulsion- After birth of shoulders, the shoulders are lifted up and trunk of body is born by flexing in laterally.
The baby is most commonly born head-first. In some cases the baby is "breech" meaning either the feet or buttocks are descending first. Babies in the breech position can be helped to be born vaginally by a midwife, although caesarean births are becoming more common for breech presentation.
There are several types of breech presentations, but the most common is where the baby's buttocks are born first and the legs are folded onto the baby's body with the knees bent and feet near the buttocks (full or breech). Others include frank breech, much like full breech but the baby's legs are extended toward its ears, and footling or incomplete breech, in which one or both legs are extended and the foot or feet are the presenting part. Another rare presentation is a transverse lie. This is where the baby is sideways in the womb and a hand or elbow has entered the birth canal first. While babies who present transverse will often move to a different position, this is not always the case and a cesarean birth then becomes necessary.
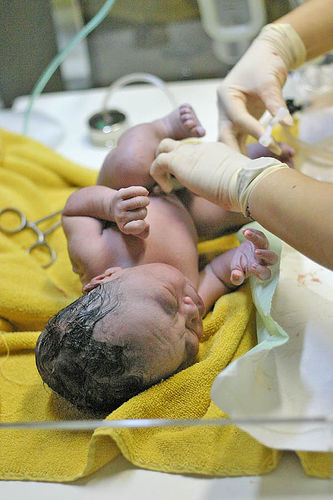
The length of the second stage varies and may be affected by whether a woman has given birth before, the position she is in and mobility. The length of the second stage should be guided by the condition of the fetus and health of the woman. Problems may be encountered at this stage due to reasons such as maternal exhaustion, the front of the baby's head facing forwards instead of backwards (posterior baby), or extremely rarely, because the baby's head does not fit properly into the woman's pelvis (Cephalo-Pelvic Disproportion (CPD)). True CPD is typically seen in women with rickets and bone deforming illnesses or injuries, as well as arbitrary time limits placed on second stage by caregivers or medical facilities.
Immediately after birth, the child undergoes extensive physiological modifications as it acclimates to independent breathing. Several cardiovascular structures start regressing soon after birth, such as the ductus arteriosus and the foramen ovale. In some cultures, the father cuts the umbilical cord and the infant is given a lukewarm bath to remove blood and some of the vernix on its skin before being handed back to its parents.
The medical condition of the child is assessed with the Apgar score, based on five parameters: heart rate, respiration, muscle tone, skin color, and response to stimuli. Apgar scores are typically assessed at both 1 and 5 minutes after birth.
Third Stage: Placenta

In this stage, the uterus expels the placenta (afterbirth). Breastfeeding the baby will help to cause this. The woman normally loses less than 500 mL (2 cups, or 1 pint) of blood. The placenta should never be pulled from the woman by an untrained person; this could cause it to tear and not be expelled whole. It is essential that the placenta be examined to ensure that it was expelled whole. Remaining parts can cause postpartum bleeding or infection.
The alternative to natural delivery of the placenta is what is called Active Management: this involves administration of a prophylactic oxytocic before delivery of the placenta, and usually early cord clamping and cutting, and controlled cord traction of the umbilical cord.
A Cochrane database study[2] suggests strongly that blood loss and the risk of postpartum bleeding will be reduced in women offered active management of the third stage of labour. However, there was an increased risk of unpleasant side effects to the baby or mother (such as nausea or vomiting) and hypertension. The authors suggest that this is due to the use of ergometrine as a component of the oxytocic. No advantages or disadvantages were apparent for the baby.
Details of CCT are available. This procedure must not be attempted except by appropriately trained providers.
After the Birth
Medical professionals typically recommend breastfeeding of the first milk, colostrum, to reduce postpartum bleeding/hemorrhage in the mother, and to pass immunities and other benefits to the baby.
Parents usually bestow the infant its given name soon after birth.
Often people visit and bring a gift for the baby.
Many cultures feature initiation rites for newborns, such as naming ceremonies, baptism, and others.
Mothers are often allowed a period where they are relieved of their normal duties to recover from childbirth. The length of this period varies. In China it is 30 days and is referred to as "doing the month" or "sitting month" (see Postpartum period). In other countries taking time off from work to care for a newborn is called "maternity leave" and varies from a few days to several months.
Variations
When the amniotic sac has not ruptured during labour or pushing, the infant can be born with the membranes intact. This is referred to as "being born in the caul." The caul is harmless and its membranes are easily broken and wiped away. In medieval times, and in some cultures still today, a caul was seen as a sign of good fortune for the baby, even giving the child psychic gifts such as clairvoyance, and in some cultures was seen as protection against drowning. The caul was often impressed onto paper and stored away as an heirloom for the child. With the advent of modern interventive obstetrics, premature artificial rupture of the membranes has become common, so babies are rarely born in the caul.
Pain
The amounts of pain experienced by women during childbirth varies. For some women, the pain is intense and agonizing; for other women there is little to no pain. Many factors affect pain perception; fear, number of previous births, fetal presentation, cultural ideas of childbirth, birthing position, support given during labor, beta-endorphin levels, and a woman's natural pain threshold. Uterine contractions are always intense during childbirth. Some women report these sensations as painful, though the degree of pain varies from individual to individual.
Non-medical Pain Control
Some women believe that reliance on analgesic medication is unnatural, or believe that it may harm the child. They still can alleviate labour pain using psychological preparation, education, massage, hypnosis, or water therapy in a tub or shower. Some women like to have someone to support them during labour and birth, such as the woman's mother, a sister, the father of the baby, a close friend, a partner or a trained professional doula. Some women deliver in a squatting or crawling position in order to more effectively push during the second stage and so that gravity can aid the descent of the baby through the birth canal.
The human body also has its own method of pain control for labour and childbirth in the form of beta-endorphins. As a naturally occurring opiate, beta-endorphin has properties similar to pethidine, morphine, and heroin, and has been shown to work on the same receptors of the brain.[3] Like oxytocin, beta-endorphin is secreted from the pituitary gland, and high levels are present during sex, pregnancy, birth, and breastfeeding. This hormone can induce feelings of pleasure and euphoria during childbirth.[4]
Water birth is an option chosen by some women for pain relief during labour and childbirth, and some studies have shown waterbirth in an uncomplicated pregnancy to reduce the need for analgesia, without evidence of increased risk to mother or newborn.[5] The American Academy of Pediatrics still considers underwater birthing "an experimental procedure that should not be performed except within the context of an appropriately designed [randomized controlled trial] after informed parental consent."[6] Many hospitals and birthing centres now offer women the option of waterbirth, either via custom-made 'birthing pools' or large bath tubs, and have policies to safeguard their use.
Meditation and mind medicine techniques for the use of pain control during labor and delivery. These techniques are used in conjunction with progressive muscle relaxation and many other forms of relaxation for the mind and body to aid in pain control for women during childbirth. These techniques are a form of natural pain control. One such technique is the use of hypnosis in childbirth. This technique is a form of meditation that empowers and liberates the woman by uplifting her body and its natural process to welcoming her new child into the world.
Medical Pain Control
In some countries of Europe, doctors commonly prescribe inhaled nitrous oxide gas for pain control; in the UK, midwives may use this gas without a doctor's prescription. Pethidine (with or without promethazine) may be used early in labour, as well as other opioids, but if given too close to birth there is a risk of respiratory depression in the infant.
Popular medical pain control in hospitals include the regional anesthetics epidural blocks, and spinal anaesthesia. Doctors and many parents favor the epidural block because medication does not enter the woman's circulatory system, thus it does not cross the placenta and enter the bloodstream of the fetus. Some studies find that although epidural use can lengthen the labour and increase the need for operative intervention, it has no adverse effect on perinatal outcome, and is a safe and effective method of pain control.[7]
Different measures for pain control have varying degrees of success and side effects to the woman and her baby. The risks of medical pain control should be balanced against the fact that childbirth can be extremely painful, and anesthetics are an effective and generally safe way to control pain.
Complications and Risks of Birth
Problems that occur during childbirth are called complications. They can affect the woman, the baby, or both. Sometimes they cause injury or even death. Doctors and midwives are trained to deal with these problems if they should occur.
Infant deaths (neonatal deaths from birth to 28 days, or perinatal deaths if including fetal deaths at 28 weeks gestation and later) are around 1% in modernized countries. The risk of maternal death during childbirth in developed nations is comparatively low; only about 1 in 1800 women die in childbirth (only 1 in 3700 in North America). In the Third World, it is a much riskier proposition: neonatal deaths rates in Sub-Saharan Africa and South Asia are more than 3.7%,[8] and on average 1 in 48 women die during childbirth.[9] The "natural" mortality rate of childbirth—where nothing is done to avert maternal death—has been estimated as being between 1,000 and 1,500 deaths per 100,000 births.[10] (See main article: neonatal death, maternal death)
The most important factors affecting mortality in childbirth are adequate nutrition and access to quality medical care ("access" is affected both by the cost of available care, and distance from health services). "Medical care" in this context does not refer specifically to treatment in hospitals, but simply routine prenatal care and the presence, at the birth, of an attendant with midwifery skills. A 1983-1989 study by the Texas Department of Health revealed that the infant death rate was 0.57% for doctor-attended births, and 0.19% for births attended by non-nurse midwives. (The comparison may be misleading because higher-risk births are less likely to be attended solely by a midwife.) Conversely, some studies demonstrate a higher perinatal mortality rate with assisted home births.[11] Around 80% of pregnancies are low-risk. Factors that may make a birth high risk include prematurity, high blood pressure, gestational diabetes and a previous cesarean section.
One of the most dangerous risks to the fetus is that of premature birth, and its associated low neonatal weight. The more premature (or underweight) a baby is, the greater the risks for neonatal death and for pulmonary, respiratory, neurological or other sequelae. About 12% of all infants born in the United States are born prematurely. In the past 25 years, medical technology has greatly improved the chances of survival of premature infants in industrialized nations. In the 1950s and 1960s, approximately half of all low birth weight babies in the US died. Today, more than 90% survive. The first hours of life for "premies" are critical, especially the very first hour of life. Rapid access to a Neonatal Intensive Care Unit is of paramount importance.
Some of the possible complications are:
- Heavy bleeding during or after childbirth, which is the most common cause of mortality in new mothers, in both developed and undeveloped nations.[8] Heavy blood loss leads to hypovolemic shock, insufficient perfusion of vital organs and death if not rapidly treated by stemming the blood loss (medically with ergometrine and pitocin or surgically) and blood transfusion. Hypopituitarism after obstetric hypovolemic shock is termed Sheehan's syndrome.
- Non-progression of labour (longterm contractions without adequate cervical dilation) is generally treated with intravenous synthetic oxytocin preparations. If this is ineffective, Caesarean section may be necessary. Changes in maternal position is effective in many cases.
- Fetal distress is the development of signs of distress by the child. These may include rising or decreasing heartbeat (monitored on cardiotocography/CTG), shedding of meconium in the amniotic fluid, and other signs.
- Non-progression of expulsion (the head or presenting parts are not delivered despite adequate contractions): this can require interventions such as vacuum extraction, forceps extraction or Caesarean section.
- In the past, a large proportion of women died from infection puerperal fever, but since the introduction of basic hygiene during parturition by Ignaz Semmelweis, this number has fallen precipitously.
- Lacerations can be painful. An episiotomy was once thought necessary to avoid tears involving the anal sphincter, but its routine use—once normal—has now been shown to increase the risk of deep lacerations especially involving and extending through the anal sphincter.
- Pelvic girdle pain. Hormones and enzymes work together to produce ligamentous relaxation and widening of the symphysis pubis during the last trimester of pregnancy. The physiologic changes of pregnancy are superimposed by the trauma of birth. During delivery, the ligaments stretch and small amounts of tearing in the fibro cartilage occurs, this tearing can be in any direction, progressively loosening the symphysis, producing cartilage nodules, cysts and reactive bone formation. For some women an event during the delivery can cause some degree of injury to the symphysis pubis or sacroiliac joint. This could be the result of:
- A large baby.
- A mid to high forceps delivery.
- Previous pelvic trauma.
- Hypermobility.
- Pelvic girdle pain during the pregnancy.
Pain is usually felt low down over the symphysis pubis; which may be extremely tender to the touch. Swelling and/or inflammation will be present. She will experience difficulty lifting leg, pain pulling legs apart, standing on one leg, transferring weight through pelvis and legs, and restriction of hip movement. Pain may also be felt in the groin, hips, sacroiliac joints and lower abdomen and can radiate down the inner thighs. The woman and may be aware of an audible 'tearing' sound coming form the pelvis during the delivery as the fibrocartilage tears apart. For women who have pain and instability they can experience mild to major disabilities.
Instrumental delivery (Forceps and Ventouse)
- The woman will have her legs apart supported in stirrups.
- If an anaesthetic is not already in place it will be given.
- For a forceps delivery an episiotomy will be done (a cut in the perineum or the region between the vagina and anus), for ventouse extraction an episiotomy is not always done.
- After the head is delivered the rest of the delivery is done in the manual method.
- After episiotomy or tears the woman is stitched up.
- In some cases a 'Trial of Forceps' will be tried out, this will be done in the operating theatre, meaning they will try a forceps delivery and will switch to a caesarean section if it fails.
Twins and Multiple Births
Twins can be delivered vaginally. In some cases twin delivery is done in a larger delivery room or in theatre, just in case complications occur e.g.
- Both twins born vaginally - one comes normally but the other is breech and/or helped by a forceps/ventouse delivery
- One twin born vaginally and the other by caesarean section.
- If the twins are joined at any part of the body - called conjoined twins, delivery is mostly by caesarean section.
Triplets or more are always delivered by caesarean section.
Professions Associated with Childbirth
Midwives are experts in normal birth. Midwives believe that childbirth is a normal process that is best accomplished with as little interference as possible. Midwives are trained to assist at births, either through direct-entry or nurse-midwifery programs. Lay midwives typically train in apprenticeship programs with experienced midwives.
Obstetricians are experts in dealing with abnormal births and pathological labour conditions, though they sometimes attend normal births as a precautionary measure. Obstetricians in most countries are trained as surgeons, so they can undertake surgical procedures relating to childbirth. Such procedures include caesarean sections, episiotomies, or emergency hysterectomies. Obstetricians' tendency to intervene surgically to overcome complications has led to criticism that they perform surgery too readily. In the United States, obstetric malpractice settlements are typically very large, so obstetricians argue that they are forced to intervene aggressively to limit their liability.
Maternal-fetal medicine specialists are experts in managing and treating high-risk pregnancy and delivery.
Obstetric nurses assist midwives, doctors, women, and babies prior to, during, and after the birth process. Some midwives are also obstetric nurses. Obstetric nurses hold various certifications and typically undergo additional obstetric training in addition to standard nursing training
Doulas are trained assistants who support mothers during pregnancy, labour, birth, and postpartum. They are not medical attendants; rather, they provide emotional support and non-medical pain relief for women during labour.
Social Aspects
In most cultures, childbirth is considered to be the beginning of a person's life, and their age is defined relative to it.
Some families view the placenta as a special part of birth, since it has been the child's life support for so many months. Some parents like to see and touch this organ. In some cultures, parents plant a tree along with the placenta on the child's first birthday. The placenta may be eaten by the newborn's family, ceremonially or otherwise.
Psychological Aspects
Childbirth can be a stressful event. As with any stressful event, strong emotions can be brought to the surface.
Some women report symptoms compatible with post-traumatic stress disorder (PTSD) after birth. Between 70 and 80% of mothers in the United States report some feelings of sadness or "baby blues" after childbirth. Postpartum depression may develop in some women; about 10% of mothers in the United States are diagnosed with this condition. Abnormal and persistent fear of childbirth is known as tokophobia.
Preventative group therapy has proven effective as a prophylactic treatment for postpartum depression.[12]
There are some who argue that childbirth is stressful for the infant. Stresses associated with breech birth, such as asphyxiation, may affect the infant's brain.
Partner and Other Support
There is increasing evidence to show that the participation of the woman's partner in the birth leads to better birth and also post-birth outcomes, providing the partner does not exhibit excessive anxiety.[13] Research also shows that when a labouring woman was supported by a female helper such as a family member or doula during labour, she had less need for chemical pain relief, the likelihood of caesarean section was reduced, use of forceps and other instrumental deliveries were reduced and there was a reduction in the length of labour and the baby had a higher Apgar score (Dellman 2004, Vernon 2006).
It is the traditional history of home labour that makes The Netherlands an attractive site for studies related to birth. One third of all baby deliveries there are still happening at home in contrast with other western industrialized countries. Apparently, Dutch fathers have been in the scene of labor for a long time as can be observed in paintings from the 17th and 18th centuries.
During this study, it was found that fathers can have different roles during birth and that little is said about the conflicts between partners or partners and professionals. Among other findings were also: the interpretation of the presence of fathers during birth as a modern version of the anthropological couvade ritual to ease the woman's pain; the majority of fathers did not perceive any limitation to participate in their childbirth and upper generations did not play an important rule in the transmission of knowledge about birth to those fathers but the wives, feminine acquaintances and midwives.
The research was based, mainly, on in-depth interviews, where fathers described what was happening from their partner’s first signals of birth labour until the placenta delivery.
Postnatal Care
Well Known Authors on Childbirth
- Janet Balaskas
- Jeannine Parvati Baker
- Robert A. Bradley
- Ina May Gaskin
- Sheila Kitzinger
- Frederick Leboyer
- Francesca Naish & Janette Roberts
- Michel Odent
- William Sears
- Laura Shanley
- Miriam Stoppard
- David Vernon
- Erna Wright
- Robbie Davis-Floyd
- Penny Simkin
Related Chapters
- Pre- and perinatal psychology
- Postnatal
- Lamaze
- Natalism
- Homebirth
- Unassisted childbirth
- Waterbirth
- hypnosis in childbirth
- Pre-labor
External Links
- Discovery Health's Ultimate Guide to Pregnancy Tools, video, information for a healthy pregnancy.
References
- ↑ The Columbia Encyclopedia, Sixth Edition. Copyright 2006 Columbia University Press
- ↑ Prendiville WJ, Elbourne D, McDonald S. (2000). "Active versus expectant management in the third stage of labour". Cochrane Database of Systematic Reviews, Issue 3. Art. No.: CD000007. DOI: 10.1002/14651858.CD000007.
- ↑ H H Loh, L F Tseng, E Wei, and C H Li Beta-endorphin is a potent analgesic agent. Proc Natl Acad Sci U S A. 1976 August; 73(8): 2895–2898.
- ↑ M. Brinsmead et al., "Peripartum Concentrations of Beta Endorphin and Cortisol and Maternal Mood States," Australian and New Zealand Journal of Obstetrics and Gynaecology 25 (1985): 194-197
- ↑ Eberhard J, Stein S, Geissbuehler V (2005). "Experience of pain and analgesia with water and land births". Journal of psychosomatic obstetrics and gynaecology. 26 (2): 127–33. PMID 16050538.
- ↑ Pediatrics 2005;115;1413-1414
- ↑ Thorp JA, Breedlove G (1996). "Epidural analgesia in labor: an evaluation of risks and benefits". Birth (Berkeley, Calif.). 23 (2): 63–83. PMID 8826170.
- ↑ 8.0 8.1 World Health Organization 2005 World Health Report, Chapter 4: Risking Death To Give Life, The Greatest Risks to Life are in its Beginning
- ↑ Safer Motherhood Fact Sheet: Maternal Mortality
- ↑ Van Lerberghe W, De Brouwere V. Of blind alleys and things that have worked: history’s lessons on reducing maternal mortality. In: De Brouwere V, Van Lerberghe W, eds. Safe motherhood strategies: a review of the evidence. Antwerp, ITG Press, 2001 (Studies in Health Services Organisation and Policy, 17:7–33).
- ↑ "Perinatal death associated with planned home birth in Australia: population based study". BMJ. 317(7155):384-8. Unknown parameter
|accessyear=ignored (|access-date=suggested) (help); Unknown parameter|accessmonthday=ignored (help) - ↑ Zlotnick C, Johnson SL, Miller IW, Pearlstein T, Howard M. Postpartum depression in women receiving public assistance: pilot study of an interpersonal-therapy-oriented group intervention, Am J Psychiatry. 2001 Apr;158(4):638-40. [PMID 11282702]
- ↑ Men at Birth - Should your bloke be there?
bs:Porođaj br:Gwilioud cs:Porod de:Geburt el:Γέννηση eo:Nasko eu:Erditze io:Parturo it:Parto he:לידה lv:Dzemdības lt:Gimdymas nl:Bevalling oc:Jasilha qu:Paqariy sk:Pôrod sl:Porod sr:Порођај fi:Synnytys sv:Förlossning yi:געבורט