Colitis
|
WikiDoc Resources for Colitis |
|
Articles |
|---|
|
Most recent articles on Colitis |
|
Media |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Colitis at Clinical Trials.gov Clinical Trials on Colitis at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Colitis
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Directions to Hospitals Treating Colitis Risk calculators and risk factors for Colitis
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Colitis |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
For more information on allergic colitis, please click here
For more information on infectious colitis, please click here
For more information on ischemic colitis, please click here
For more information on chemical colitis, please click here
For more information on drug-induced colitis, please click here
For more information on radiation colitis, please click here
For patient information on this topic, click here
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: M.Umer Tariq [2]; Maham Khan [3]; Ogheneochuko Ajari, MB.BS, MS [4]; Rim Halaby, M.D. [5]; Qasim Salau, M.B.B.S., FMCPaed [6]
Synonyms and keywords: Proctocolitis, Proctitis, Enterocolitis.
Overview
Colitis is the inflammation of the colon, that can be either acute or chronic. Causes of colitis include infectious causes such as Chlamydia trachomatis, Neisseria gonorrhoeae, Shigella dysenteriae, HSV, allergy (food potein-induced proctocolitis) and radiation. Colitis may co-exist with enteritis (inflammation of the small bowel), proctitis (inflammation of the rectum) or both. The mainstay of therapy for infectious proctocolitis is antimicrobial therapy. The preferred regimen is a combination of Ceftriaxone and Doxycycline.
Classification
There is no established classification system for colitis. However, it may be classified based on etiology, age and duration of symptom.
Classification by etiology
| Classes of Colitis | Disorders |
| Autoimmune | |
| Allergic | |
| Infectious colitis |
|
| Idiopathic | |
| Iatrogenic | |
| Vascular | |
| Drug induced | |
| Unclassifiable |
|
Classification by Anatomy
Colitis may co-exist with inflammation involving other parts of the gastrointestinal tract. It can be classified based on anatomy into;
- Proctitis: When it involves the rectum
- Colitis: When it involves the inflammation is limited to the colon
- Proctocolitis: When it involves the rectum and colon (usually the distal part of the colon 12cm to 15cm above the anus (sigmoid colon)[1][2]
- Enterocolitis: When it involves the small intestine in addition to the colon
Schematic of Anatomical Classification of Colitis
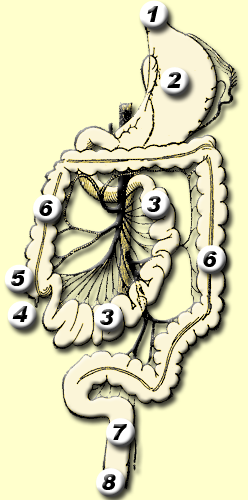
*Regions 4 to 6: Enterocolitis
*Region 6: Colitis
*Regions 6 to 8: Proctocolitis
*Regions 7 to 8:Proctitis
Classification by Age
Classification by duration of symptoms
Notes:
- Fulminant colitis is any colitis with a rapid downhill clinical course; in addition to the diarrhea, fever, and anemia seen in colitis, the patient has severe abdominal pain and presents a clinical picture similar to that of septicemia, where shock is present.
- Irritable bowel syndrome, a separate disease, has been called spastic colitis or spastic colon. This name causes confusion, since colitis is not a feature of irritable bowel syndrome.
- Immune mediated colitis is the experimental name in animal studies of ulcerative colitis. It is a synonym of ulcerative colitis, but it should not be used as a synonym when referring to ulcerative colitis.
Pathophysiology
The pathophysiology of colitis depends on the cause. Some pathogenetic mechanisms are not clearly understood.
Genetics
There is no specific genetic cause for proctocolitis. However, genetic predisposition may play a role in some causes.[8][9]
Gross pathology
-
Allergic proctocolitis[10]
-
Radiation Proctitis[11]
-
Pseudomembranous colitis. (WC) [12]
-
Pseudomembranous colitis. [13]
-
Ulcerative colitis.[14]
Microscopic pathology
-
Ulcerative colitis. H&E staining showing crypt abscess, a characteristic finding in ulcerative colitis [15]
-
Ulcerative colitis. H&E stain showing marked lymphocytic infiltration (blue/purple) of the intestinal mucosa and distortion of the architecture of the crypts. [16]
-
Ischemic colitis. H&E staining showing changes seen in ischemic colitis [17]
-
Pseudomembranous colitis. H& E staining showing pseudomembranes in Clostridium colitis [18]
Causes
Common Causes
Common causes of Proctocolitis include infectious agents such as Chlamydia trachomatis (which causes LGV (Lymphogranuloma Venereum), Neisseria gonorrhoeae, HSV, Shigella dysenteriae and Campylobacter species. It can also be allergic (for example food protein-induced proctocolitis), idiopathic (for example microscopic colitis), vascular (for example ischemic colitis), or autoimmune (for example inflammatory bowel disease).
Causes by Organ System
Causes in Alphabetical Order
Life Threatening Causes
Example include toxic megacolon, ischemic colitis, infectious colitis such as escherichia coli O157:H7 and shigella.
Diagnosis
Symptoms
Physical Examination
Diagnostic Tests
Colitis is associated with the following findings:
- Swelling of the colon tissue
- Bleeding
- Erythema (redness) of the surface of the colon
- Ulcerations of the colon
Common tests which reveal these signs include:
- X-rays of the colon
- Testing the stool for blood and pus
- Sigmoidoscopy
- Colonoscopy
Additional tests include stool cultures and blood tests, including blood chemistry tests. A high erythrocyte sedimentation rate (ESR) is one typical finding in acute exacerbations of colitis.
Treatment
Medical Therapy
Treatment of colitis may include the administration of antibiotics and general anti-inflammatory medications such as Mesalamine or its derivatives, steroids, or one of a number of other drugs that ameliorate inflammation.
Changes in diet can be effective at treating the symptoms of colitis and easing the side effects. These can include reducing the intake of carbohydrates, lactose products, soft drinks, and caffeine. This approach has been championed by Elaine Gottschall.
Hygienic and naturopathic doctors have taken the diet approach further, attributing bowel inflammation to toxemia stemming from high-protein, fatty diets and other dietary irritants. Changing to a low-fat, minimally-processed, whole-foods diet per the Natural Hygiene self-healing system has been effective in eliminating symptoms and rebuilding health. Dr. Zarin Azar, MD,, is one advocate of this healing system.
Infliximab (or REMICADE) - a drug originally produced to treat Rheumatoid Arthritis - has recently been approved for the treatment of Colitis where traditional treatments have failed. REMICADE is a biologic therapy that recognizes, attaches to, and blocks the action of a protein in your body called tumor necrosis factor alpha (TNF-alpha). TNF-alpha is made by certain blood cells in your body. It is administered through a series of infusions.
Surgery
Approximately half of patients with fulminant colitis require surgery. Surgery usually entails removing the colon and bowel and creating a "pouch" with portions of the small intestine.
Differentiating Colitis from Other Diseases
Causes of proctocolitis are diverse and may overlap with other disease. The differential diagnosis of proctocolitis can be classified into two according to age group.
Differential diagnosis in Infants
- Swallowed maternal blood syndrome
- Anorectal fissure
- Necrotizing enterocolitis especially in preterm babies
- Vitamin K dependent hemorrhage
- Other Coagulopathies: (hereditary such as coagulation factor deficiency or acquired such as disseminated intravascular coagulopathy)
- Food protein-induced enterocolitis
- Intussusception
- Gastrointestinal Infections
- Meckel diverticulum
- Intestinal duplication cysts
- Vascular malformations
- Inflammatory bowel disease(early onset)
- Hirschsprung disease complicated by enterocolitis
- Volvolus
- Gastro-duodenal ulcers
- Gastrointestinal duplication cyst
- Liver disease with clotting factor deficiency
- Lymphonodular hyperplasia
Differential diagnosis in Infants
- Colorectal malignancy
- Crohn's disease
- Behcet's disease
- Arteriovenous malformation
- Diverticuclosis
- Infection
- Coagulopathy
- Systemic lupus erythematosus(SLE)
Treatment
Medical Therapy
- All patients with proctocolitis should be treated.
- Treatment of proctocolitis is similar to that of proctitis.
- Generally, the following regimen is recommended:
- Preferred regimen: Ceftriaxone 250 mg IM AND Doxycycline 100 mg PO bid for 7 days
To view additional treatment and special considerations for the management of proctitis/proctocolitis, click here.
Surgery
Prevention
See also
References
- ↑ 2015 Sexually Transmitted Diseases Treatment Guidelines. Centers for Disease Control and Prevention (2015).http://www.cdc.gov/std/tg2015/proctitis.htm Accessed on August 29, 2016
- ↑ Hamlyn E, Taylor C (2006). "Sexually transmitted proctitis". Postgrad Med J. 82 (973): 733–6. doi:10.1136/pmj.2006.048488. PMC 2660501. PMID 17099092.
- ↑ WikiMedia Commons https://commons.wikimedia.org/wiki/File:Gastro-intestinal_tract.png. Accessed on September 09, 2016
- ↑ Nowak-Węgrzyn A (2015). "Food protein-induced enterocolitis syndrome and allergic proctocolitis". Allergy Asthma Proc. 36 (3): 172–84. doi:10.2500/aap.2015.36.3811. PMC 4405595. PMID 25976434.
- ↑ Pumberger W, Pomberger G, Geissler W (2001). "Proctocolitis in breast fed infants: a contribution to differential diagnosis of haematochezia in early childhood". Postgrad Med J. 77 (906): 252–4. PMC 1741985. PMID 11264489.
- ↑ Alfadda AA, Storr MA, Shaffer EA (2011). "Eosinophilic colitis: epidemiology, clinical features, and current management". Therap Adv Gastroenterol. 4 (5): 301–9. doi:10.1177/1756283X10392443. PMC 3165205. PMID 21922029.
- ↑ 7.0 7.1 Hauer-Jensen M, Denham JW, Andreyev HJ (2014). "Radiation enteropathy--pathogenesis, treatment and prevention". Nat Rev Gastroenterol Hepatol. 11 (8): 470–9. doi:10.1038/nrgastro.2014.46. PMC 4346191. PMID 24686268.
- ↑ Sekerkova A, Fuchs M, Cecrdlova E, Svachova V, Kralova Lesna I, Striz I; et al. (2015). "High Prevalence of Neutrophil Cytoplasmic Autoantibodies in Infants with Food Protein-Induced Proctitis/Proctocolitis: Autoimmunity Involvement?". J Immunol Res. 2015: 902863. doi:10.1155/2015/902863. PMC 4592904. PMID 26484355.
- ↑ Loddo I, Romano C (2015). "Inflammatory Bowel Disease: Genetics, Epigenetics, and Pathogenesis". Front Immunol. 6: 551. doi:10.3389/fimmu.2015.00551. PMC 4629465. PMID 26579126.
- ↑ The Korean Academy of Medical Sciences. Allergic proctocolitis. http://dx.doi.org/10.3346/jkms.2007.22.2.213 Accessed on 31 August, 2016
- ↑ Wikipedia. Proctitis. https://en.wikipedia.org/wiki/Proctitis#/media/File:Radiation_proctitis3.jpg Accessed on August 31, 2016
- ↑ Libre Pathology. Pseudomembranous colitis. https://librepathology.org/wiki/Pseudomembranous_colitis Accessed on August 31, 2016
- ↑ Libre Pathology. Pseudomembranous colitis. https://librepathology.org Accessed on September 1, 2016
- ↑ Ulcerative colitis. Wikidoc. http://www.wikidoc.org/index.php/File:UC_granularity.png#filehistory Accessed on August 31, 2016
- ↑ Libre Pathology. https://librepathology.org/wiki/File:Ulcerative_colitis_(2)_active.jpg Accessed on September 1, 2016
- ↑ Libre Pathology. https://librepathology.org/wiki/File:Ulcerative_colitis_(2)_endoscopic_biopsy.jpg Accessed on September 1, 2016
- ↑ Wikipedia. Ischemic colitis. https://en.wikipedia.org/wiki/Ischemic_colitis#/media/File:Ischemic_colitis_-_high_mag.jpg Accessed on August 31, 2016
- ↑ Libre Pathology. Pseudomembranous colitis. https://librepathology.org/wiki/File:Colonic_pseudomembranes_low_mag.jpg Accessed on September 1, 2016
- ↑ Mohan P, Ramakrishnan MK, Revathy S, Jayanthi V (2011). "Granulomatous colitis in oculocutaneous albinism". Dig Liver Dis. 43 (1): e1. doi:10.1016/j.dld.2009.09.006. PMID 19833565.
- ↑ Gié O, Clerc D, Giulieri S, Demartines N (2014). "[Clostridial colitis: diagnosis and strategies for management]". Rev Med Suisse. 10 (434): 1309–13. PMID 25073304.
![Radiation Proctitis[11]](/images/0/01/Radiation_proctitis3.jpg)
![Pseudomembranous colitis. (WC) [12]](/images/a/a1/Pseudomembranous_colitis.JPG)
![Pseudomembranous colitis. [13]](/images/c/c1/800px-Pseudomembranous_Colitis%2C_Colectomy_%28Gross%29_%287410584264%29.jpg)
![Ulcerative colitis.[14]](/images/c/cf/UC_granularity.png)
![Ulcerative colitis. H&E staining showing crypt abscess, a characteristic finding in ulcerative colitis [15]](/images/2/2e/Ulcerative_colitis_%282%29_active.jpg)
![Ulcerative colitis. H&E stain showing marked lymphocytic infiltration (blue/purple) of the intestinal mucosa and distortion of the architecture of the crypts. [16]](/images/0/02/Ulcerative_colitis_%282%29_endoscopic_biopsy.jpg)
![Ischemic colitis. H&E staining showing changes seen in ischemic colitis [17]](/images/f/f2/Ischemic_colitis.JPG)
![Pseudomembranous colitis. H& E staining showing pseudomembranes in Clostridium colitis [18]](/images/0/09/1440px-Colonic_pseudomembranes_low_mag.jpg)