Blastic NK cell lymphoma
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Synonyms and keywords: Agranular CD4+CD56+ hematodermic neoplasm; CD4+CD56+ hematodermic neoplasm; HDT; Blastic plasmacytoid dendritic cell neoplasm; BPDCN; Blastic natural killer cell lymphoma
Overview
Blastic natural killer cell lymphoma was first discovered by Adachi, an American hematologist, in 1994 following an unusual presentation of cutaneous lymphoma that express CD4 and CD56 antigens but no other T cell and B cell antigens. The deletion in 5q has been associated with the development of blastic natural killer cell lymphoma. Blastic natural killer cell lymphoma must be differentiated from other malignancies such as acute myeloid leukemia, human T-cell lymphotropic virus 1 associated adult T-cell leukemia/lymphoma, cutaneous NK/T-cell lymphoma, primary and secondary cutaneous pleomorphic T-cell lymphomas, undifferentiated carcinoma, and malignant melanoma. Blastic NK cell lymphoma is more commonly observed among middle-aged or elderly patients. The mean age at diagnosis is 66 years.[1]Males are more commonly affected with blastic natural killer cell lymphoma than females. Prognosis is generally poor, and the median survival rate is 15 months. Symptoms of blastic natural killer cell lymphoma may include nodules, plaques and patches of variable sizes on skin. Immunohistochemical staining is positive for r CD4 and CD56, with variable positivity for CD43, TdT, and CD68. The mainstay of therapy for blastic natural killer cell lymphoma is chemotherapy with CHOP or COP-like regimens.
Historical Perspective
- Blastic natural killer cell lymphoma was first discovered by Adachi, an American hematologist, in 1994 following an unusual presentation of cutaneous lymphoma that express CD4 and CD56 antigens but no other T cell and B cell antigens.[2]
- Chaperot et al demonstrated that predendritic cells (plasmacytoid monocytes) and CD4/CD56 leukemic cells are similar in the production of alpha-interferon in response to influenza virus stimulation, which on maturation with interleukin 3 (IL-3) become powerful inducers for CD4 proliferation and Th-2 polarization. .[3]
- Petrella and Karube demonstrated that CD123, which is a marker of predendritic cells, are expressed on the tumor cells in blastic natural killer cell lymphoma and proposed an oncogenic transformation of NCAM-expressing plasmacytoid monocyte-like cells as cell of origin in CD4/CD56 blastic natural killer cell lymphoma.[4][5]
Pathophysiology
- Blastic natural killer cell lymphoma is a type of lymphoma. It does not appear to be associated with Epstein Barr virus (EBV) .[6]
- Blastic natural killer cell lymphoma is derived from plasmacytoid type 2 dendritic cell precursors. These dendritic cell precursors are possibly related to a common myeloid/NK-cell precursor cell.[7]
- Blastic natural killer cell lymphoma is currently classified by World Health Organization (WHO) Classification of Tumors of Hematopoietic and Lymphoid Tissues as an aggressive neoplasm derived from the precursors of plasmacytoid dendritic cells and categorically placed under the heading “Acute myeloid leukemia (AML) and related precursor neoplasms.”
- The deletion in 5q has been associated with the development of blastic natural killer cell lymphoma.
- Other genetic abnormalities associated with blastic natural killer cell lymphoma are deletion of 12p, abnormalities of chromosome 13, deletion of 6q, and loss of chromosomes 15 and 9.
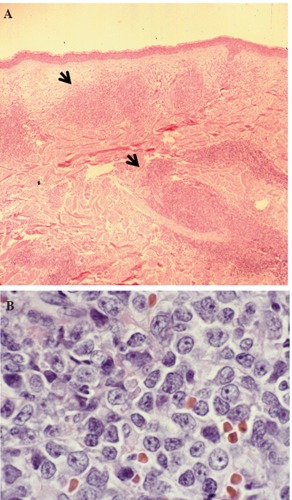
- On hematoxylin and eosin (H&E) staining, fine chromatin and scanty cytoplasm resembling lymphoblasts, or in some cases, myeloblasts, and may on occasion exhibit sub-membranous cytoplasmic vacuolations surrounding the nucleus are characteristic findings of blastic natural killer cell lymphoma.
- Tumor cells are invariably CD4+ and CD56+, and usually HLA-DR and CD45RA are positive as well.
- CD2 and CD34 are usually negative; and expression of TdT, CD7 and cytoplasmic CD3 is variable.[8]
-
Hematoxylin & Eosin stain of skin lesion biopsy. Low power view of leukemic infiltrate corresponding to the raised plaque (A, black arrows) and high power view of the malignant cells in the skin infiltrate
-
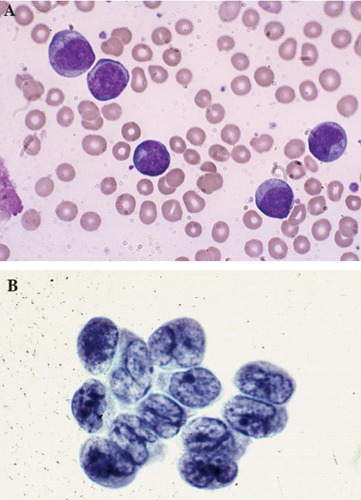
Large malignant-appearing cells, with agranular cytoplasm, cleaved nuclei and prominent neocleoli on peripheral blood smear using Wright stain (A) and similar blast cells present in cerebrospinal fluid
Differentiating Blastic NK cell Lymphoma from other Diseases
ABBREVIATIONS
N/A: Not available, NL: Normal, FISH: Fluorescence in situ hybridization, PCR: Polymerase chain reaction, LDH: Lactate dehydrogenase, PUD: Peptic ulcer disease, EPO: Erythropoietin, LFTs: Liver function tests, RFTs: Renal function tests, LAP: Leukocyte alkaline phosphatase, LAD: Leukocyte alkaline dehydrgenase, WBCs: White blood cells.
| Myeloproliferative neoplasms (MPN) | Clinical manifestations | Diagnosis | Other features | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Symptoms | Physical examination | CBC & Peripheral smear | Bone marrow biopsy | Other investigations | |||||||||||
| WBCs | Hb | Plat- elets | |||||||||||||
| Leuko-cytes | Blasts | Left shift |
Baso- phils |
Eosino- phils |
Mono- cytes |
Others | |||||||||
| Chronic myeloid leukemia (CML), BCR-ABL1+[9][10] |
|
|
↑ | <2% | + | ↑ | ↑ | ↑ | N/A | ↓ | NL |
|
|
| |
| Chronic neutrophilic leukemia (CNL)[11][12][13] |
|
↑ | Minimal | + | NL | NL | NL | ↓ | ↓ |
|
|
| |||
| Polycythemia vera (PV)[14][15][16][17] |
|
|
NL or ↑ | None | - | ↑ or ↓ | NL or ↑ | NL | ↑↑ | NL |
|
| |||
| Primary myelofibrosis (PMF)[18][19][20][21] |
|
↓ | Erythroblasts | - | Absent | NL | NL | ↓ | ↓ |
|
| ||||
| Essential thrombocythemia (ET)[22][23][24] |
|
NL or ↑ |
None |
- |
↓ or absent |
NL |
NL |
|
↑↑ |
|
|||||
| Chronic eosinophilic leukemia, not otherwise specified (NOS)[25][26][27][28] |
|
↑ | Present | + | ↑ | ↑↑ | ↑ | ↓ | ↓ |
|
|
||||
| MPN, unclassifiable |
|
|
↑ | Variable | ± | ↑ or ↓ | ↑ or ↓ | ↑ or ↓ |
|
↓ | ↑ |
|
|
| |
| Mastocytosis[29][30][31][32] |
|
↑ | None | - | NL | ↑ | NL | ↓ | ↓ or ↑ |
|
| ||||
| Myeloid/lymphoid neoplasms with eosinophilia and rearrangement of PDGFRA, PDGFRB, or FGFR1, or with PCM1-JAK2[33][34][35][36] |
|
↑ | NL | - | NL | ↑ | ↑ |
|
NL | ↓ |
|
|
| ||
| B-lymphoblastic leukemia/lymphoma[37][38] | NL or ↑ | >25% | N/A | ↑ or ↓ | ↑ or ↓ | ↑ or ↓ | ↓ | ↓ |
|
| |||||
| Myelodysplastic syndromes (MDS)[39][40] |
↓ | Variable | - | ↓ | ↓ | ↓ |
|
↓ | ↓ |
|
| ||||
| Acute myeloid leukemia (AML) and related neoplasms[41][42] |
|
|
NL or ↑ | ↑ | N/A | ↑ or ↓ | ↑ or ↓ | ↑ or ↓ |
|
↓ | ↓ |
with dysplasia |
| ||
| Blastic plasmacytoid dendritic cell neoplasm[43][44][45][46] |
|
|
NL | ↑ | NL | NL | NL | ↓ | ↓ |
|
| ||||
| Myelodysplastic /myeloproliferative neoplasms (MDS/MPN) |
Chronic myelomonocytic leukemia (CMML)[47] |
|
↑ | < 20% | NL | ↑ | ↑↑ |
|
↓ | ↓ |
|
| |||
| Atypical chronic myeloid leukemia (aCML), BCR-ABL1-[50][51] |
|
|
↑ | <20% | + | <2% of WBCs | N/A | N/A |
|
↓ | ↓ |
|
|||
| Juvenile myelomonocytic leukemia (JMML)[52][53] |
|
↑ | ↑ | N/A | N/A | N/A | ↑ | ↓ | ↓ |
|
| ||||
| MDS/MPN with ring sideroblasts and thrombocytosis (MDS/MPN-RS-T)[54][55][56] |
|
|
NL or ↑ | NL | - | NL | N/A | N/A | ↓ | ↑ |
|
| |||
| T-lymphoblastic leukemia/ lymphoma |
T-lymphoblastic leukemia/ lymphoma[57][58][59] |
|
↑ | >25% blasts (Leukemia) | ± | ↑ or ↓ | ↑ or ↓ | ↑ or ↓ |
|
↓ | ↓ |
|
|||
| Provisional entity: Natural killer (NK) cell lymphoblastic leukemia/lymph[60] |
|
↑ | ↑ | ± | ↑ or ↓ | ↑ or ↓ | ↑ or ↓ |
|
↓ | ↓ |
|
||||
| Provisional entity: Early T-cell precursor lymphoblastic leukemia[61][62] |
|
↑ | ↑ | ± | ↑ or ↓ | ↑ or ↓ | ↑ or ↓ |
|
↓ | ↓ |
|
||||
Epidemiology and Demographics
- The prevalence of blastic natural killer cell lymphoma is unknown as it is an extremely rare disorder.[63]
Age
- Blastic natural killer cell lymphoma is more commonly observed amongmiddle-aged or elderly patients. The mean age at diagnosis is 66 years.[1]
Gender
- Males are more commonly affected with blastic natural killer cell lymphoma than females.
Natural History, Complications and Prognosis
- The majority of patients with blastic natural killer cell lymphoma have an aggressive clinical course.
- Prognosis is generally poor, and the median survival rate is 15 months.[8]
Diagnosis
Symptoms
- Symptoms of blastic natural killer cell lymphoma may include:
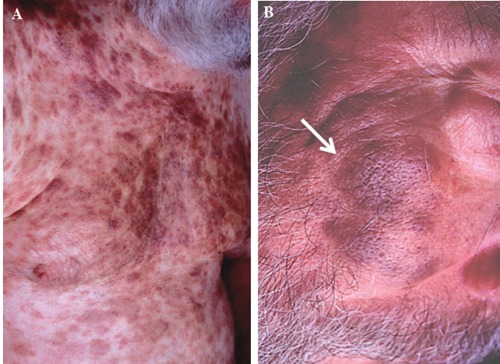
- Nodules, plaques and patches of variable sizes on skin
Physical Examination
- Physical examination may be remarkable for:
- Nodules, plaques and patches of variable sizes on skin
Laboratory Findings
- There are no specific laboratory findings associated with blastic natural killer cell lymphoma.
Imaging Findings
- There are no imaging study findings associated with blastic natural killer cell lymphoma
Other Diagnostic Studies
- Blastic natural killer cell lymphoma may also be diagnosed using immunochemistry.
- Immunohistochemical staining is positive for r CD4 and CD56, with variable positivity for CD43, TdT, and CD68.
Treatment
Medical Therapy
- The mainstay of therapy for blastic NK cell lymphoma is chemotherapy with CHOP or COP-like regimens.
- Immunomodulation or immunotherapy with IL-3 or with antiCD123 antibody is also being considered for chemotherapy-resistant patients.
Prevention
- There are no primary preventive measures available for blastic natural killer cell lymphoma.
References
- ↑ 1.0 1.1 Hou, Steve; Jaworski, Joseph; Swami, Vanlila; Heintzelman, Rebecca; Cusack, Carrie; Chung, Christina; Peck, Jeremy; Fanelli, Matthew; Styler, Michael; Rizk, Sanaa (2015). "Blastic plasmacytoid dendritic cell neoplasm with absolute monocytosis at presentation". Pathology and Laboratory Medicine International: 7. doi:10.2147/PLMI.S71492. ISSN 1179-2698.
- ↑ Adachi M, Maeda K, Takekawa M, Hinoda Y, Imai K, Sugiyama S; et al. (1994). "High expression of CD56 (N-CAM) in a patient with cutaneous CD4-positive lymphoma". Am J Hematol. 47 (4): 278–82. PMID 7526680.
- ↑ Chaperot L, Bendriss N, Manches O, Gressin R, Maynadie M, Trimoreau F; et al. (2001). "Identification of a leukemic counterpart of the plasmacytoid dendritic cells". Blood. 97 (10): 3210–7. PMID 11342451.
- ↑ Petrella T, Meijer CJ, Dalac S, Willemze R, Maynadié M, Machet L; et al. (2004). "TCL1 and CLA expression in agranular CD4/CD56 hematodermic neoplasms (blastic NK-cell lymphomas) and leukemia cutis". Am J Clin Pathol. 122 (2): 307–13. doi:10.1309/0QPP-AVTU-PCV9-UCLV. PMID 15323148.
- ↑ Karube K, Ohshima K, Tsuchiya T, Yamaguchi T, Suefuji H, Suzumiya J; et al. (2003). "Non-B, non-T neoplasms with lymphoblast morphology: further clarification and classification". Am J Surg Pathol. 27 (10): 1366–74. PMID 14508398.
- ↑ Chan JK, Sin VC, Wong KF; et al. (1997). "Nonnasal lymphoma expressing the natural killer cell marker CD56: a clinicopathologic study of 49 cases of an uncommon aggressive neoplasm". Blood. 89 (12): 4501–13. PMID 9192774. Unknown parameter
|month=ignored (help) - ↑ Willemze R, Jaffe ES, Burg G, Cerroni L, Berti E, Swerdlow SH; et al. (2005). "WHO-EORTC classification for cutaneous lymphomas". Blood. 105 (10): 3768–85. doi:10.1182/blood-2004-09-3502. PMID 15692063.
- ↑ 8.0 8.1 Petrella T, Bagot M, Willemze R, Beylot-Barry M, Vergier B, Delaunay M; et al. (2005). "Blastic NK-cell lymphomas (agranular CD4+CD56+ hematodermic neoplasms): a review". Am J Clin Pathol. 123 (5): 662–75. PMID 15981806.
- ↑ Savage DG, Szydlo RM, Goldman JM (January 1997). "Clinical features at diagnosis in 430 patients with chronic myeloid leukaemia seen at a referral centre over a 16-year period". Br. J. Haematol. 96 (1): 111–6. PMID 9012696.
- ↑ Thompson PA, Kantarjian HM, Cortes JE (October 2015). "Diagnosis and Treatment of Chronic Myeloid Leukemia in 2015". Mayo Clin. Proc. 90 (10): 1440–54. doi:10.1016/j.mayocp.2015.08.010. PMC 5656269. PMID 26434969.
- ↑ Szuber N, Tefferi A (February 2018). "Chronic neutrophilic leukemia: new science and new diagnostic criteria". Blood Cancer J. 8 (2): 19. doi:10.1038/s41408-018-0049-8. PMC 5811432. PMID 29440636.
- ↑ Maxson JE, Tyner JW (February 2017). "Genomics of chronic neutrophilic leukemia". Blood. 129 (6): 715–722. doi:10.1182/blood-2016-10-695981. PMC 5301820. PMID 28028025.
- ↑ Menezes J, Cigudosa JC (2015). "Chronic neutrophilic leukemia: a clinical perspective". Onco Targets Ther. 8: 2383–90. doi:10.2147/OTT.S49688. PMC 4562747. PMID 26366092.
- ↑ Vannucchi AM, Guglielmelli P, Tefferi A (March 2018). "Polycythemia vera and essential thrombocythemia: algorithmic approach". Curr. Opin. Hematol. 25 (2): 112–119. doi:10.1097/MOH.0000000000000402. PMID 29194068.
- ↑ Pillai AA, Babiker HM. PMID 30252337. Missing or empty
|title=(help) - ↑ Tefferi A, Barbui T (January 2019). "Polycythemia vera and essential thrombocythemia: 2019 update on diagnosis, risk-stratification and management". Am. J. Hematol. 94 (1): 133–143. doi:10.1002/ajh.25303. PMID 30281843.
- ↑ Rumi E, Cazzola M (February 2017). "Diagnosis, risk stratification, and response evaluation in classical myeloproliferative neoplasms". Blood. 129 (6): 680–692. doi:10.1182/blood-2016-10-695957. PMC 5335805. PMID 28028026.
- ↑ Cervantes F, Correa JG, Hernandez-Boluda JC (May 2016). "Alleviating anemia and thrombocytopenia in myelofibrosis patients". Expert Rev Hematol. 9 (5): 489–96. doi:10.1586/17474086.2016.1154452. PMID 26891375.
- ↑ Hoffman, Ronald (2018). Hematology : basic principles and practice. Philadelphia, PA: Elsevier. ISBN 9780323357623.
- ↑ Michiels JJ, Bernema Z, Van Bockstaele D, De Raeve H, Schroyens W (March 2007). "Current diagnostic criteria for the chronic myeloproliferative disorders (MPD) essential thrombocythemia (ET), polycythemia vera (PV) and chronic idiopathic myelofibrosis (CIMF)". Pathol. Biol. 55 (2): 92–104. doi:10.1016/j.patbio.2006.06.002. PMID 16919893.
- ↑ Hoffman, Ronald (2018). Hematology : basic principles and practice. Philadelphia, PA: Elsevier. ISBN 9780323357623.
- ↑ Schmoldt A, Benthe HF, Haberland G (1975). "Digitoxin metabolism by rat liver microsomes". Biochem Pharmacol. 24 (17): 1639–41. PMID http://dx.doi.org/10.1182/blood-2007-04-083501 Check
|pmid=value (help). - ↑ Daniel A. Arber, Attilio Orazi, Robert Hasserjian, Jurgen Thiele, Michael J. Borowitz, Michelle M. Le Beau, Clara D. Bloomfield, Mario Cazzola & James W. Vardiman (2016). "The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia". Blood. 127 (20): 2391–2405. doi:10.1182/blood-2016-03-643544. PMID 27069254. Unknown parameter
|month=ignored (help) - ↑ A. Tefferi, R. Fonseca, D. L. Pereira & H. C. Hoagland (2001). "A long-term retrospective study of young women with essential thrombocythemia". Mayo Clinic proceedings. 76 (1): 22–28. doi:10.4065/76.1.22. PMID 11155408. Unknown parameter
|month=ignored (help) - ↑ Vidyadharan S, Joseph B, Nair SP (2016). "Chronic Eosinophilic Leukemia Presenting Predominantly with Cutaneous Manifestations". Indian J Dermatol. 61 (4): 437–9. doi:10.4103/0019-5154.185716. PMC 4966405. PMID 27512192.
- ↑ Hofmans M, Delie A, Vandepoele K, Van Roy N, Van der Meulen J, Philippé J, Moors I (2018). "A case of chronic eosinophilic leukemia with secondary transformation to acute myeloid leukemia". Leuk Res Rep. 9: 45–47. doi:10.1016/j.lrr.2018.04.001. PMC 5993353. PMID 29892549.
- ↑ Yamada Y, Rothenberg ME, Cancelas JA (2006). "Current concepts on the pathogenesis of the hypereosinophilic syndrome/chronic eosinophilic leukemia". Transl Oncogenomics. 1: 53–63. PMC 3642145. PMID 23662039.
- ↑ Kim TH, Gu HJ, Lee WI, Lee J, Yoon HJ, Park TS (September 2016). "Chronic eosinophilic leukemia with FIP1L1-PDGFRA rearrangement". Blood Res. 51 (3): 204–206. doi:10.5045/br.2016.51.3.204. PMID 27722133.
- ↑ Carter MC, Metcalfe DD, Komarow HD (February 2014). "Mastocytosis". Immunol Allergy Clin North Am. 34 (1): 181–96. doi:10.1016/j.iac.2013.09.001. PMC 3863935. PMID 24262698.
- ↑ Macri A, Cook C. PMID 29494109. Missing or empty
|title=(help) - ↑ Lladó AC, Mihon CE, Silva M, Galzerano A (2014). "Systemic mastocytosis - a diagnostic challenge". Rev Bras Hematol Hemoter. 36 (3): 226–9. doi:10.1016/j.bjhh.2014.03.003. PMC 4109736. PMID 25031064.
- ↑ Valent P, Akin C, Metcalfe DD (March 2017). "Mastocytosis: 2016 updated WHO classification and novel emerging treatment concepts". Blood. 129 (11): 1420–1427. doi:10.1182/blood-2016-09-731893. PMC 5356454. PMID 28031180.
- ↑ Kumar, Kirthi R.; Chen, Weina; Koduru, Prasad R.; Luu, Hung S. (2015). "Myeloid and Lymphoid Neoplasm With Abnormalities of FGFR1 Presenting With Trilineage Blasts and RUNX1 Rearrangement". American Journal of Clinical Pathology. 143 (5): 738–748. doi:10.1309/AJCPUD6W1JLQQMNA. ISSN 1943-7722.
- ↑ Paolo Strati, Guilin Tang, Dzifa Y. Duose, Saradhi Mallampati, Rajyalakshmi Luthra, Keyur P. Patel, Mohammad Hussaini, Abu-Sayeef Mirza, Rami S. Komrokji, Stephen Oh, John Mascarenhas, Vesna Najfeld, Vivek Subbiah, Hagop Kantarjian, Guillermo Garcia-Manero, Srdan Verstovsek & Naval Daver (2018). "Myeloid/lymphoid neoplasms with FGFR1 rearrangement". Leukemia & lymphoma. 59 (7): 1672–1676. doi:10.1080/10428194.2017.1397663. PMID 29119847. Unknown parameter
|month=ignored (help) - ↑ Ximena Montenegro-Garreaud, Roberto N. Miranda, Alexandra Reynolds, Guilin Tang, Sa A. Wang, Mariko Yabe, Wei Wang, Lianghua Fang, Carlos E. Bueso-Ramos, Pei Lin, L. Jeffrey Medeiros & Xinyan Lu (2017). "Myeloproliferative neoplasms with t(8;22)(p11.2;q11.2)/BCR-FGFR1: a meta-analysis of 20 cases shows cytogenetic progression with B-lymphoid blast phase". Human pathology. 65: 147–156. doi:10.1016/j.humpath.2017.05.008. PMID 28551329. Unknown parameter
|month=ignored (help) - ↑ Paola Villafuerte-Gutierrez, Montserrat Lopez Rubio, Pilar Herrera & Eva Arranz (2018). "A Case of Myeloproliferative Neoplasm with BCR-FGFR1 Rearrangement: Favorable Outcome after Haploidentical Allogeneic Transplantation". Case reports in hematology. 2018: 5724960. doi:10.1155/2018/5724960. PMID 30647980.
- ↑ Kamiya-Matsuoka C, Garciarena P, Amin HM, Tremont-Lukats IW, de Groot JF (December 2013). "B lymphoblastic leukemia/lymphoma presenting as seventh cranial nerve palsy". Neurol Clin Pract. 3 (6): 532–534. doi:10.1212/CPJ.0b013e3182a78ef0. PMC 6082360. PMID 30107017.
- ↑ Zhang X, Rastogi P, Shah B, Zhang L (September 2017). "B lymphoblastic leukemia/lymphoma: new insights into genetics, molecular aberrations, subclassification and targeted therapy". Oncotarget. 8 (39): 66728–66741. doi:10.18632/oncotarget.19271. PMC 5630450. PMID 29029550.
- ↑ Germing U, Kobbe G, Haas R, Gattermann N (November 2013). "Myelodysplastic syndromes: diagnosis, prognosis, and treatment". Dtsch Arztebl Int. 110 (46): 783–90. doi:10.3238/arztebl.2013.0783. PMC 3855821. PMID 24300826.
- ↑ Gangat N, Patnaik MM, Tefferi A (January 2016). "Myelodysplastic syndromes: Contemporary review and how we treat". Am. J. Hematol. 91 (1): 76–89. doi:10.1002/ajh.24253. PMID 26769228.
- ↑ Islam A, Catovsky D, Goldman JM, Galton DA (September 1985). "Bone marrow biopsy changes in acute myeloid leukaemia. I: Observations before chemotherapy". Histopathology. 9 (9): 939–57. PMID 3864727.
- ↑ Orazi A (2007). "Histopathology in the diagnosis and classification of acute myeloid leukemia, myelodysplastic syndromes, and myelodysplastic/myeloproliferative diseases". Pathobiology. 74 (2): 97–114. doi:10.1159/000101709. PMID 17587881.
- ↑ F. Julia, T. Petrella, M. Beylot-Barry, M. Bagot, D. Lipsker, L. Machet, P. Joly, O. Dereure, M. Wetterwald, M. d'Incan, F. Grange, J. Cornillon, G. Tertian, E. Maubec, P. Saiag, S. Barete, I. Templier, F. Aubin & S. Dalle (2013). "Blastic plasmacytoid dendritic cell neoplasm: clinical features in 90 patients". The British journal of dermatology. 169 (3): 579–586. doi:10.1111/bjd.12412. PMID 23646868. Unknown parameter
|month=ignored (help) - ↑ Livio Pagano, Caterina Giovanna Valentini, Alessandro Pulsoni, Simona Fisogni, Paola Carluccio, Francesco Mannelli, Monia Lunghi, Gianmatteo Pica, Francesco Onida, Chiara Cattaneo, Pier Paolo Piccaluga, Eros Di Bona, Elisabetta Todisco, Pellegrino Musto, Antonio Spadea, Alfonso D'Arco, Stefano Pileri, Giuseppe Leone, Sergio Amadori & Fabio Facchetti (2013). "Blastic plasmacytoid dendritic cell neoplasm with leukemic presentation: an Italian multicenter study". Haematologica. 98 (2): 239–246. doi:10.3324/haematol.2012.072645. PMID 23065521. Unknown parameter
|month=ignored (help) - ↑ Joseph D. Khoury (2018). "Blastic Plasmacytoid Dendritic Cell Neoplasm". Current hematologic malignancy reports. 13 (6): 477–483. doi:10.1007/s11899-018-0489-z. PMID 30350260. Unknown parameter
|month=ignored (help) - ↑ Shinichiro Sukegawa, Mamiko Sakata-Yanagimoto, Ryota Matsuoka, Haruka Momose, Yusuke Kiyoki, Masayuki Noguchi, Naoya Nakamura, Rei Watanabe, Manabu Fujimoto, Yasuhisa Yokoyama, Hidekazu Nishikii, Takayasu Kato, Manabu Kusakabe, Naoki Kurita, Naoshi Obara, Yuichi Hasegawa & Shigeru Chiba (2018). "[Blastic plasmacytoid dendritic cell neoplasm accompanied by chronic myelomonocytic leukemia successfully treated with azacitidine]". [[[Rinsho ketsueki] The Japanese journal of clinical hematology]]. 59 (12): 2567–2573. doi:10.11406/rinketsu.59.2567. PMID 30626790.
- ↑ Patnaik MM, Tefferi A (June 2016). "Chronic myelomonocytic leukemia: 2016 update on diagnosis, risk stratification, and management". Am. J. Hematol. 91 (6): 631–42. doi:10.1002/ajh.24396. PMID 27185207.
- ↑ Parikh SA, Tefferi A (June 2012). "Chronic myelomonocytic leukemia: 2012 update on diagnosis, risk stratification, and management". Am. J. Hematol. 87 (6): 610–9. doi:10.1002/ajh.23203. PMID 22615103.
- ↑ Benton CB, Nazha A, Pemmaraju N, Garcia-Manero G (August 2015). "Chronic myelomonocytic leukemia: Forefront of the field in 2015". Crit. Rev. Oncol. Hematol. 95 (2): 222–42. doi:10.1016/j.critrevonc.2015.03.002. PMC 4859155. PMID 25869097.
- ↑ Dao KH, Tyner JW (2015). "What's different about atypical CML and chronic neutrophilic leukemia?". Hematology Am Soc Hematol Educ Program. 2015: 264–71. doi:10.1182/asheducation-2015.1.264. PMC 5266507. PMID 26637732.
- ↑ Muramatsu H, Makishima H, Maciejewski JP (February 2012). "Chronic myelomonocytic leukemia and atypical chronic myeloid leukemia: novel pathogenetic lesions". Semin. Oncol. 39 (1): 67–73. doi:10.1053/j.seminoncol.2011.11.004. PMC 3523950. PMID 22289493.
- ↑ Aricò M, Biondi A, Pui CH (July 1997). "Juvenile myelomonocytic leukemia". Blood. 90 (2): 479–88. PMID 9226148.
- ↑ Hasle H (March 1994). "Myelodysplastic syndromes in childhood--classification, epidemiology, and treatment". Leuk. Lymphoma. 13 (1–2): 11–26. doi:10.3109/10428199409051647. PMID 8025513.
- ↑ Patnaik MM, Tefferi A (March 2017). "Refractory anemia with ring sideroblasts (RARS) and RARS with thrombocytosis (RARS-T): 2017 update on diagnosis, risk-stratification, and management". Am. J. Hematol. 92 (3): 297–310. doi:10.1002/ajh.24637. PMID 28188970.
- ↑ Alshaban A, Padilla O, Philipovskiy A, Corral J, McAlice M, Gaur S (2018). "Lenalidomide induced durable remission in a patient with MDS/MPN-with ring sideroblasts and thrombocytosis with associated 5q- syndrome". Leuk Res Rep. 10: 37–40. doi:10.1016/j.lrr.2018.08.001. PMID 30186759.
- ↑ Bouchla A, Papageorgiou SG, Tsakiraki Z, Glezou E, Pavlidis G, Stavroulaki G, Bazani E, Foukas P, Pappa V (2018). "Plasmablastic Lymphoma in an Immunocompetent Patient with MDS/MPN with Ring Sideroblasts and Thrombocytosis-A Case Report". Case Rep Hematol. 2018: 2525070. doi:10.1155/2018/2525070. PMC 6247723. PMID 30524760.
- ↑ You MJ, Medeiros LJ, Hsi ED (September 2015). "T-lymphoblastic leukemia/lymphoma". Am. J. Clin. Pathol. 144 (3): 411–22. doi:10.1309/AJCPMF03LVSBLHPJ. PMID 26276771.
- ↑ Patel KJ, Latif SU, de Calaca WM (March 2009). "An unusual presentation of precursor T cell lymphoblastic leukemia/lymphoma with cholestatic jaundice: case report". J Hematol Oncol. 2: 12. doi:10.1186/1756-8722-2-12. PMC 2663564. PMID 19284608.
- ↑ Elreda L, Sandhu M, Sun X, Bekele W, Cohen AJ, Shah M (2014). "T-cell lymphoblastic leukemia/lymphoma: relapse 16 years after first remission". Case Rep Hematol. 2014: 359158. doi:10.1155/2014/359158. PMC 4005062. PMID 24822133.
- ↑ Sedick Q, Alotaibi S, Alshieban S, Naheet KB, Elyamany G (2017). "Natural Killer Cell Lymphoblastic Leukaemia/Lymphoma: Case Report and Review of the Recent Literature". Case Rep Oncol. 10 (2): 588–595. doi:10.1159/000477843. PMID 28868017.
- ↑ Jain N, Lamb AV, O'Brien S, Ravandi F, Konopleva M, Jabbour E, Zuo Z, Jorgensen J, Lin P, Pierce S, Thomas D, Rytting M, Borthakur G, Kadia T, Cortes J, Kantarjian HM, Khoury JD (April 2016). "Early T-cell precursor acute lymphoblastic leukemia/lymphoma (ETP-ALL/LBL) in adolescents and adults: a high-risk subtype". Blood. 127 (15): 1863–9. doi:10.1182/blood-2015-08-661702. PMC 4915808. PMID 26747249.
- ↑ Haydu JE, Ferrando AA (July 2013). "Early T-cell precursor acute lymphoblastic leukaemia". Curr. Opin. Hematol. 20 (4): 369–73. doi:10.1097/MOH.0b013e3283623c61. PMC 3886681. PMID 23695450.
- ↑ 63.0 63.1 Saeed H, Awasthi M, Al-Qaisi A, Massarweh S (2014). "Blastic plasmacytoid dendritic cell neoplasm with extensive cutaneous and central nervous system involvement". Rare Tumors. 6 (4): 5474. doi:10.4081/rt.2014.5474. PMC 4274438. PMID 25568744.