Epstein Barr virus
| Epstein-Barr Virus | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Virus classification | ||||||||||
|
|
Mononucleosis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Epstein Barr virus On the Web |
|
American Roentgen Ray Society Images of Epstein Barr virus |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor-In-Chief: Cafer Zorkun, M.D., Ph.D. [2]
Related Key Words and Synonyms: EBV
Overview
The Epstein-Barr Virus (EBV), also called Human herpesvirus 4 (HHV-4), is a virus of the herpes family (which includes Herpes simplex virus and Cytomegalovirus), and is one of the most common viruses in humans. Most people become infected with EBV, which is often asymptomatic but commonly causes infectious mononucleosis.
EBV is named after Michael Epstein and Yvonne Barr, who together with Bert Achong, discovered the virus in 1964.[1]
Biology
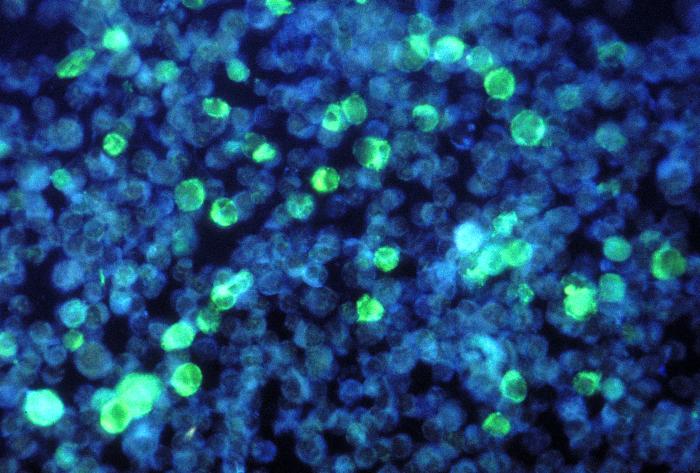
- On infecting the B-lymphocyte, the linear virus genome circularizes and the virus subsequently persists within the cell as an episome.
- The virus can execute many distinct programs of gene expression which can be broadly categorized as being lytic cycle or latent cycle.
- The lytic cycle or productive infection results in staged expression of a host of viral proteins with the ultimate objective of producing infectious virions. Formally, this phase of infection does not inevitably lead to lysis of the host cell as EBV virions are produced by budding from the infected cell.
- The latent cycle (lysogenic) programs are those that do not result in production of virions. A very limited, distinct set of viral proteins are produced during latent cycle infection. These include Epstein-Barr nuclear antigen (EBNA)-1, EBNA-2, EBNA-3A, EBNA-3B, EBNA-3C, EBNA-leader protein (EBNA-LP) and latent membrane proteins (LMP)-1, LMP-2A and LMP-2B and the Epstein-Barr encoded RNAs (EBERs). In addition, EBV codes for at least twenty microRNAs which are expressed in latently infected cells.[2]
- From studies of EBV gene expression in cultured Burkitt's lymphoma cell lines, at least three programs exist:
- EBNA1 only (group I)
- EBNA1 + EBNA2 (group II)
- Latent cycle proteins (group III).
- It is also postulated that a program in which all viral protein expression is shut off exists.
- When EBV infects B-lymphocytes in vitro, lymphoblastoid cell lines eventually emerge that are capable of indefinite growth. The growth transformation of these cell lines is the consequence of viral protein expression.
- EBNA-2, EBNA-3C and LMP-1 are essential for 'transformation' while EBNA-LP and the EBERs are not. The EBNA-1 protein is essential for maintenance of the virus genome.[3]
- It is postulated that following natural infection with EBV, the virus executes some or all of its repertoire of gene expression programs to establish a persistent infection. Given the initial absence of host immunity, the lytic cycle produces large amounts of virus to infect other (presumably) B-lymphocytes within the host.
- The latent programs reprogram and subvert infected B-lymphocytes to proliferate and bring infected cells to the sites at which the virus presumably persists. Eventually, when host immunity develops, the virus persists by turning off most (or possibly all) of its genes, only occasionally reactivating to produce fresh virions. A balance is eventually struck between occasional viral reactivation and host immune surveillance removing cells that activate viral gene expression.
- The site of persistence of EBV may be bone marrow. EBV-positive patients who have had their own bone marrow replaced with bone marrow from an EBV-negative donor are found to be EBV-negative after transplantation.[4]
EBV latent antigens
All EBV nuclear proteins are produced by alternative splicing of a transcript starting at either the Cp or Wp promoters at the left end of the genome (in the conventional nomenclature). The genes are ordered EBNA-LP/EBNA-2/EBNA-3A/EBNA-3B/EBNA-3C/EBNA-1 within the genome.
The initiation codon of the EBNA-LP coding region is created by an alternate splice of the nuclear protein transcript. In the absence of this initiation codon, EBNA-2/EBNA-3A/EBNA-3B/EBNA-3C/EBNA-1 will be expressed depending on which of these genes is alternatively spliced into the transcript.
EBNA-1
EBNA-1 protein binds to a replication origin (oriP) within the viral genome and mediates replication and partitioning of the episome during division of the host cell. It is the only viral protein expressed during group I latency. EBNA-1 possesses a glycine-alanine repeat that impairs antigen processing and MHC class I-restricted antigen presentation thereby inhibiting the CD8-restricted cytotoxic T-cell response against virus infected cells.[5]
EBNA-1 was initially identified as the target antigen of sera from rheumatoid arthritis patients (rheumatoid arthritis-associated nuclear antigen; RANA).
EBNA-2
EBNA-2 is the main viral transactivator, switching transcription from the Wp promoters used during initially after infection to the Cp promoter. Together with EBNA-3C, it also activates the LMP-1 promoter. It is known to bind the host RBP-Jκ protein that is a key player in the Notch pathway. EBNA-2 is essential for EBV-mediated growth transformation.
EBNA-3A/EBNA-3B/EBNA-3C
These genes also bind the host RBP-Jκ protein.
EBNA-3C
EBNA-3C is also a ubiquitin-ligase and has been shown to target cell cycle regulators like pRb[6][7]
LMP-1
LMP-1 is a six-span transmembrane protein that is also essential for EBV-mediated growth transformation. LMP-1 mediates signaling through the Tumor necrosis factor-alpha/CD40 pathway.
LMP-2A/LMP-2B
LMP-2A/LMP-2B are transmembrane proteins that act to block tyrosine kinase signaling. It is believed that they act to inhibit activation of the viral lytic cycle. It's unknown whether LMP-2B is required for EBV-mediated growth transformation, while different groups have reported that LMP-2A alternatively is, or is not needed for transformation.
EBER-1/EBER-2
EBER-1/EBER-2 are small nuclear RNAs of an unknown role. They are not required for EBV-mediated growth transformation.
miRNAs
EBV microRNAs are encoded by two transcripts, one set in the BART gene and one set near the BHRF1 cluster. The three BHRF1 miRNAS are expressed during type III latency while the large cluster of BART miRNAs (up to 20 miRNAs) are expressed during type II latency. The functions of these miRNAs are currently unknown.
EBV surface receptors
- The Epstein-Barr Virus surface glycoprotein H (gH) is essential for penetration of B cells but also plays a role in attachment of virus to epithelial cells. [8]
- In laboratory and animal trials in 2000, it was shown that both antagonism of RA-mediated growth inhibition and promotion of LCL proliferation were efficiently reversed by the glucocorticoid receptor (GR) antagonist RU486.[3]
Diseases associated with EBV
- Infectious states:
- Cancers:
- Non-Hodgkin's lymphomas, including primary cerebral lymphoma
- Hodgkin's disease
- Hairy leukoplakia
- Nasopharyngeal carcinoma
- Smooth muscle tumors [9]
- Immunocompromised/suppressed states:
- Common variable immunodeficiency (CVID)
- Following organ transplantation with associated immunosuppression (post-transplant lymphoproliferative disorder)
- Multiple Sclerosis (higher risk in patients infected as teenagers than as children)
- AIDS
- It has been postulated to be a trigger for a subset of chronic fatigue syndrome patients [10] and other autoimmune diseases.[11]
Diagnosis
In most cases of infectious mononucleosis, the clinical diagnosis can be made from the characteristic triad of fever, pharyngitis, and lymphadenopathy lasting for 1 to 4 weeks. Serologic test results include a normal to moderately elevated white blood cell count, an increased total number of lymphocytes, greater than 10% atypical lymphocytes, and a positive reaction to a "mono spot" test. In patients with symptoms compatible with infectious mononucleosis, a positive Paul-Bunnell heterophile antibody test result is diagnostic, and no further testing is necessary. Moderate-to-high levels of heterophile antibodies are seen during the first month of illness and decrease rapidly after week 4. False-positive results may be found in a small number of patients, and false-negative results may be obtained in 10% to 15% of patients, primarily in children younger than 10 years of age. True outbreaks of infectious mononucleosis are extremely rare. A substantial number of pseudo-outbreaks have been linked to laboratory error, as reported in CDC's Morbidity and Mortality Weekly Report, vol. 40, no. 32, on August 16, 1991.
When "mono spot" or heterophile test results are negative, additional laboratory testing may be needed to differentiate EBV infections from a mononucleosis-like illness induced by cytomegalovirus, adenovirus, or Toxoplasma gondii. Direct detection of EBV in blood or lymphoid tissues is a research tool and is not available for routine diagnosis. Instead, serologic testing is the method of choice for diagnosing primary infection.
References
- ↑ Epstein MA, Achong BG, Barr YM (1964). "Virus particles in cultured lymphblasts from Burkitt's Lymphoma". Lancet. 1: 702–3. PMID 14107961.
- ↑ The nomenclature used here is that of the Kieff lab. Other laboratories use different nomenclatures.
- ↑ Yates JL, Warren N, Sugden B (1985). "Stable replication of plasmids derived from Epstein-Barr virus in various mammalian cells". Nature. 313 (6005): 812–5. PMID 2983224.
- ↑ Gratama JW, Oosterveer MA, Zwaan FE, Lepoutre J, Klein G, Ernberg I (1988). "Eradication of Epstein-Barr virus by allogeneic bone marrow transplantation: implications for sites of viral latency". Proc. Natl. Acad. Sci. U.S.A. 85 (22): 8693–6. PMID 2847171.
- ↑ Levitskaya J, Coram M, Levitsky V; et al. (1995). "Inhibition of antigen processing by the internal repeat region of the Epstein-Barr virus nuclear antigen-1". Nature. 375 (6533): 685–8. doi:10.1038/375685a0. PMID 7540727.
- ↑ Knight JS, Sharma N, Robertson ES (2005). "SCFSkp2 complex targeted by Epstein-Barr virus essential nuclear antigen". Mol. Cell. Biol. 25 (5): 1749–63. doi:10.1128/MCB.25.5.1749-1763.2005. PMID 15713632.
- ↑ Knight JS, Sharma N, Robertson ES (2005). "Epstein-Barr virus latent antigen 3C can mediate the degradation of the retinoblastoma protein through an SCF cellular ubiquitin ligase". Proc. Natl. Acad. Sci. U.S.A. 102 (51): 18562–6. doi:10.1073/pnas.0503886102. PMID 16352731.
- ↑ Sara J. Molesworth, Cathleen M. Lake, Corina M. Borza, Susan M. Turk, and Lindsey M. Hutt-Fletcher. "Epstein-Barr Virus gH Is Essential for Penetration of B Cells but Also Plays a Role in Attachment of Virus to Epithelial Cells". Journal of Virology. July 2000, p. 6324-6332, Vol. 74, No. 14. External link in
|title=(help) - ↑ Deyrup AT, Lee VK, Hill CE, Cheuk W, Toh HC, Kesavan S, Chan EW, Weiss SW. "Epstein-Barr virus-associated smooth muscle tumors are distinctive mesenchymal tumors reflecting multiple infection events: a clinicopathologic and molecular analysis of 29 tumors from 19 patients". Am J Surg Pathol. 2006 Jan;30(1):75-82. PMID 16330945.
- ↑ Lerner AM, Beqaj SH, Deeter RG, Fitzgerald JT (2004). "IgM serum antibodies to Epstein-Barr virus are uniquely present in a subset of patients with the chronic fatigue syndrome". In Vivo. 18 (2): 101–6. PMID 15113035.
- ↑ Lünemann JD, Münz C (2007). "Epstein-Barr virus and multiple sclerosis". Current neurology and neuroscience reports. 7 (3): 253–8. PMID 17488592.
Resources
- Article in The Scientist 13(6):1, Mar. 15, 1999 (registration required)
- CDC website on EBV
- Epstein Barr Virus Editor: Erle S. Robertson Department of Microbiology and the Abramson Comprehensive Cancer Center, University of Pennsylvania Medical School, Philadelphia, Pennsylvania 19104, USA
- International Association for Research on EBV Body that organizes the two-yearly EBV research meeting.
- Wikipedia
Template:Baltimore classification Template:Viral diseases
bg:Вирус на Епщайн-Бар
de:Epstein-Barr-Virus
it:Virus di Epstein-Barr
he:וירוס אפשטיין בר
nl:Epstein-Barr virus
id:Virus Epstein-Barr
fi:Epstein-Barrin virus
sv:Epstein-Barr-virus