Megakaryocyte


|
WikiDoc Resources for Megakaryocyte |
|
Articles |
|---|
|
Most recent articles on Megakaryocyte Most cited articles on Megakaryocyte |
|
Media |
|
Powerpoint slides on Megakaryocyte |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Megakaryocyte at Clinical Trials.gov Trial results on Megakaryocyte Clinical Trials on Megakaryocyte at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Megakaryocyte NICE Guidance on Megakaryocyte
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Megakaryocyte Discussion groups on Megakaryocyte Patient Handouts on Megakaryocyte Directions to Hospitals Treating Megakaryocyte Risk calculators and risk factors for Megakaryocyte
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Megakaryocyte |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
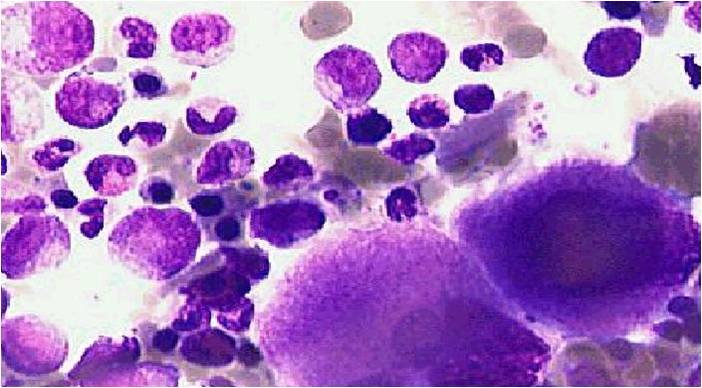
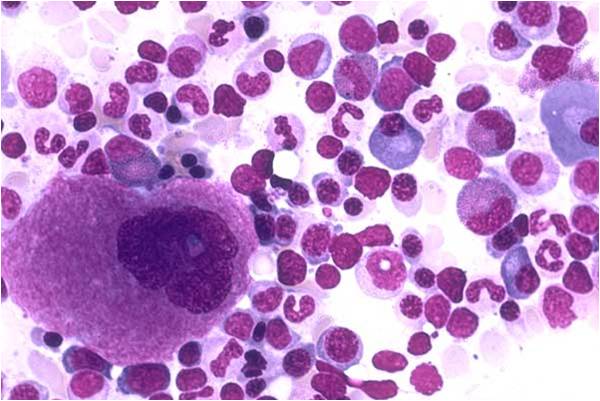
The megakaryocyte is a bone marrow cell responsible for the production of blood platelets necessary for normal blood clotting. Megakaryocytes normally account for 1 out of 10,000 bone marrow cells but can increase in number nearly 10-fold in certain diseases.[1] In general, megakaryocytes are 10 to 15 times larger than a typical red blood cell, averaging 50-100 μm in diameter. During its maturation, the megakaryocyte grows in size and replicates its DNA without cytokinesis. As a result, the nucleus of the megakaryocyte can become very large and lobulated, which, under a light microscope, can give the false impression that there are several nuclei. In some cases, the nucleus may contain up to 64N DNA, or 32 copies of the normal complement of DNA in a human cell.
Megakaryocyte development
Megakaryocytes are derived from hematopoietic stem cell precursor cells in the bone marrow. These pluripotent stem cells live in the marrow sinusoids and are capable of producing all types of blood cells depending on the signals they receive. The primary signal for megakaryocyte production is thrombopoietin or TPO. TPO is necessary for inducing differentiation of progenitor cells in the bone marrow towards a final megakaryocyte phenotype. Other molecular signals for megakaryocyte differentiation include GM-CSF, IL-3, IL-6, IL-11, and erythropoietin.[2] The megakaryocyte develops through the following lineage:
CFU-Me (pluripotential hemopoietic stem cell or hemocytoblast) -> megakaryoblast -> promegakaryocyte -> megakaryocyte.
The cell eventually reaches megakaryoblast stage and loses its ability to divide. However, it is still able to replicate its DNA and continue development.[2] The cytoplasm continues to expand and the DNA complement can increase up to 64N.

Platelet release
Once the cell has completed differentiation and become a mature megakaryocyte, it begins the process of producing platelets. Thrombopoietin plays a role in inducing the megakaryocyte to form small proto-platelet processes. Platelets are held within these internal membranes within the cytoplasm of megakaryocytes. There are two proposed mechanisms for platelet release. In one scenario, these proto-platelet processes break up explosively to become platelets.[3] Alternatively, the cell may form platelet ribbons into blood vessels. The ribbons are formed via psuedopodia and they are able to continuously emit platelets into circulation. In either scenario, each of these proto-platelet processes can give rise to 2000-5000 new platelets upon breakup. Overall, 2/3 of these newly-producd platelets will remain in circulation while 1/3 will be sequestered by the spleen.
Effects of cytokines
Cytokines are signals used in the immune system for intercellular communication. There are many cytokines which affect megakaryocytes. Certain cytokines such as IL-3, IL-6, IL-11, LIF, erythropoietin, and thrombopoietin all stimulate the maturation of megakaryocytic progenitor cells.[4] Other signals such as PF4, CXCL5, CXCL7, and CCL5 inhibit platelet formation.[5]
Thrombopoietin
Thrombopoietin (TPO) is a 353-amino acid protein located on chromosome 3p27. TPO is primarily synthesized in the liver[6] but can be made by kidneys, testes, brain, and even bone marrow stromal cells. It has high homology with erythropoietin. It is necessary but not required for the formation of platelets. Mice lacking TPO or the TPO receptor (Mpl) have a 90% reduction in circulating platelet number, although the platelets are normal in morphology and function.[7]
Disorders involving megakaryocytes
Megakaryocytes are directly responsible for producing platelets which are needed for the formation of a thrombus, or blood clot. There are several diseases which are directly attributable to abnormal megakaryocyte function or abnormal platelet function.[8]
Essential Thrombocythemia
Essential thrombocythemia (ET) is a disorder characterized by extremely high numbers of circulating platelets. The disease occurs in 1-2 per 100,000 people. The current WHO requirements for diagnosis include > 600,000 platelets/μL of blood (normal 150,000-400,000) and a bone marrow biopsy. Some of the consequences of having such high numbers of platelets include thrombosis or clots throughout the body. Thrombi form more frequently in arteries than veins. Ironically, having platelet counts above 1,000,000 platelets/μL can lead to hemorrhagic events.[9]
Recent evidence suggests that the majority of ET cases are due to a mutation in the JAK2 protein, a member of the JAK-STAT pathway.[10] Evidence suggests this mutation renders the megakaryocyte hypersensitive to thrombopoietin and causes clonal proliferation of megakaryocytes. There is a significant risk of transformation to leukemia with this disorder. The primary treatment consists of anegrelide or hydroxyurea to lower platelet levels.
Congenital amegakaryocytic thrombocytopenia
Congenital amegakaryocytic thrombocytopenia (CAMT) is a rare inherited disorder. The primary manifestations are thrombocytopenia and megakaryocytopenia, or low numbers of platelets and megakaryocytes. There is an absence of megakaryocytes in the bone marrow with no associated physical abnormalities.[11] The cause for this disorder appears to be a mutation in the gene for the TPO receptor, c-mpl, despite high levels of serum TPO.[12][13] In addition, there may be abnormalities with the central nervous system including the cerebrum and cerebellum which could cause symptoms.[12] The primary treatment for CAMT is bone marrow transplantation.
Additional Images
(Images courtesy of Melih Aktan MD.)
External links
- Immature megakaryocyte Presented by the University of Virginia
- Megakaryocytes: Mature Many microscopic images of mature megakaryocytes including in disease settings.
- Cell size comparison
- Infant Bone Marrow Transplant Journal
References
- ↑ Branehog I, Ridell B, Swolin B, Weinfeld A (1975). "Megakaryocyte quantifications in relation to thrombokinetics in primary thrombocythaemia and allied diseases". Scand. J. Haematol. 15: 321–332.
- ↑ 2.0 2.1 Deutsch VR, Torner A (2006 September). "Megakaryocyte development and platelet production". Brit. J. Haem. 134 (5): 453–466. doi:10.1111/j.1365-2141.2006.06215.x. Check date values in:
|date=(help) - ↑ Choi ES, Nichol JL, Hokom MM; et al. (1995). "Platelets generated in vitro from proplatelet-displaying human megakaryocytes are functional". Blood. 85 (2): 402–13.
- ↑ Gordon MS, Hoffman R (1992). "Growth factors affecting human thrombocytopoiesis: potential agents for the treatment of thrombocytopenia". Blood. 80: 302–307.
- ↑ Pang L, Weiss MJ, Poncz M (2005). "Megakaryocyte biology and related disorders". J. Clin. Invest. 115: 3332–3338. doi:10.1172/JCI26720.
- ↑ Jelkmann W (2001). "The role of the liver in the production of thrombopoietin compared with erythropoietin". Eur. J. Gastroenterol. Hepatol. 13: 791–801.
- ↑ Murone M, Carpenter DA, de Sauvage FJ (1998). "Hematopoietic deficiencies in c-mpl and TPO knockout mice". Stem Cells. 16: 1–6.
- ↑ Nurden AT (2005). "Qualitative disorders of platelets and megakaryocytes". J. Thromb. and Haem. 3 (8): 1773–1782. doi:10.1111/j.1538-7836.2005.01428.x.
- ↑ Michiels JJ, Berneman ZN, Schroyens W, Van Vliet HH (2004). "Pathophysiology and treatment of platelet-mediated microvascular disturbances, major thrombosis and bleeding complications in essential thrombocythaemia and polycythaemia vera". Platelets. 15: 67–84.
- ↑ Kralovics R, Passamonti F, Buser AS, Teo SS; et al. (2005 Apr 28). "A gain-of-function mutation of JAK2 in myeloproliferative disorders". N Engl J Med. 352 (17): 1779–90. Check date values in:
|date=(help) - ↑ Freedman MH, Estrov Z (1990). "Congenital amegakaryocytic thrombocytopenia: an intrinsic hematopoietic stem cell defect". Am. J. Pediatr. Hematol. Oncol. 12: 225–230.
- ↑ 12.0 12.1 Ihara K, Ishii E, Eguchi M, Takada H, Suminoe A, Good RA, Hara T (1999). "Identification of mutations in the c-mpl gene in congenital amegakaryocytic thrombocytopenia". Proc. Natl. Acad. Sci. 96: 3133–6.
- ↑ Ballmaier M, Germeshausen M, Schulze H, Cherkaoui K, Lang S, Gaudig A, Krukemeier S, Eilers M, Strauss G, Welte K (2001). "C-mpl mutations are the cause of congenital amegakaryocytic thrombocytopenia". Blood. 97: 139–46.