Primary Intestinal Lymphangiectasia: Difference between revisions
Sara Mohsin (talk | contribs) |
Sara Mohsin (talk | contribs) |
||
| Line 222: | Line 222: | ||
==Epidemiology and Demographics== | ==Epidemiology and Demographics== | ||
*The prevalence of PIL is unknown as it can be [[asymptomatic]]. | *The prevalence of PIL is unknown as it can be [[asymptomatic]]. | ||
*It primarily affects children (generally diagnosed before the age of 3) and young adults but may be diagnosed later in adults.<ref name="pmid50050">{{cite journal| author=Tift WL, Lloyd JK| title=Intestinal lymphangiectasia. Long-term results with MCT diet. | journal=Arch Dis Child | year= 1975 | volume= 50 | issue= 4 | pages= 269-76 | pmid=50050 | doi=10.1136/adc.50.4.269 | pmc=1544468 | url=https://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=50050 }} </ref> | *It primarily affects children (generally diagnosed before the age of 3) and young adults but may be diagnosed later in adults.<ref name="pmid50050">{{cite journal| author=Tift WL, Lloyd JK| title=Intestinal lymphangiectasia. Long-term results with MCT diet. | journal=Arch Dis Child | year= 1975 | volume= 50 | issue= 4 | pages= 269-76 | pmid=50050 | doi=10.1136/adc.50.4.269 | pmc=1544468 | url=https://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=50050 }} </ref> | ||
| Line 228: | Line 227: | ||
===Age=== | ===Age=== | ||
*PIL is more commonly observed among children (less than 3 years old) and young adults. | *PIL is more commonly observed among children (less than 3 years old) and young adults. | ||
===Race=== | ===Race=== | ||
*There is no racial predilection for PIL. | *There is no racial predilection for PIL. | ||
Revision as of 01:00, 23 January 2021
|
Primary Intestinal Lymphangiectasia Microchapters |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [2] Associate Editor(s)-in-Chief: Mohamed Riad, M.D.[3]
Synonyms and keywords: PIL
Overview
Primary intestinal lymphangiectasia (Waldmann's disease) was first discovered by Waldmann T.A. in 1961 when he reported 18 cases of patients having edema with low serum albumin and gammaglobulin and proteins levels idiopathic hypercatabolic hypoproteinemia". PIL develops as a result of enlargement or dilatation of intestinal lymphatic vessels (lacteals) with leakage of their contents into the bowel lumen leading to hypoalbuminemia, hypogammaglobulinemia, and lymphopenia. The cause of PIL has not been identified. The prevalence of PIL is unknown. It can be asymptomatic. It primarily affects children (generally diagnosed before the age of 3) and young adults but may be diagnosed later in adults. Symptoms include pitting edema, diarrhea, fatigue, abdominal discomfort, and malabsorption syndrome. PIL is diagnosed by biopsy revealing dilated intestinal lymphatics. Video-capsule endoscopy may be helpful when endoscopic findings are not conclusive. Common complications of PIL include infections, malignant transformation (lymphoma), and skin warts. There is no definitive treatment for PIL; the mainstay of therapy is a low-fat high protein diet with medium-chain triglyceride oral supplementation and supplemental calcium and vitamins. PIL is associated with significant morbidity and requires adherence to dietary modification and oral supplements; otherwise. it would be associated with poor outcomes and low quality of life. It can be fatal in some cases if anasarca or malignancy develops.
Historical Perspective
- In 1961, primary intestinal lymphangiectasia (Waldmann's disease) was first discovered by Waldmann T.A., who reported 18 cases of patients having edema with low serum albumin and gammaglobulin and proteins levels ''idiopathic hypercatabolic hypoproteinemia". Assessment using radio-labeled 131I-albumin resulted in low levels in those patients. In addition, small intestinal biopsies were examined under a microscope revealing different degrees of lymphatic vessel dilatation.[1][2]
- In 1964, Samman and White first described the yellow nail syndrome, a very rare condition that may be associated with PIL. This syndrome is associated with the following symptoms:[3]
- Dystrophic yellow nails
- Nail ridging
- Loss of lunula on the hands
- Lymphedema
- Pleural effusions
Pathophysiology
Pathology
- PIL develops as a result of enlargement or dilatation of intestinal lymphatic vessels (lacteals) with leakage of their contents into the bowel lumen leading to hypoalbuminemia, hypogammaglobulinemia, and lymphopenia.
- Hypoproteinemia leads to edema.
- It is a form of protein-losing enteropathy.
Genetics
- Abnormal expression of the following genes is associated with the pathogenesis of PIL:[4]
Associated conditions
- Following five syndromes have been reported to be associated with PIL:
Gross pathology
- On gross pathology, the jejunal villi appear creamy yellowish or whitish due to the dilated lymphatics in the intestinal mucosa.
Microscopic Pathology
- The most important histopathological characteristics of PIL include:
- Dilated intestinal lymphatic vessels
- Lacteal juice in the biopsies from duodenum, jejunum, and ileum
Causes
- The exact underlying cause of PIL has not yet been identified.
- Abnormal expression of the following several genes involved in the development of the lymphatic system is associated with PIL:[4]
Differentiating PIL from other Diseases
- PIL must be differentiated from the secondary causes that lead to intestinal lymphangiectasia such as:
- Intestinal tuberculosis
- Inflammatory bowel disease
- Intestinal lymphoma
- Constrictive pericarditis
- Sarcoidosis
- Systemic sclerosis
- Whipple disease
- Radiation and/or chemotherapy with retroperitoneal fibrosis
- HIV-related enteropathy
- PIL must be differentiated from other diseases causing enteric loss of plasma proteins but do not involve intestinal lymphangiectasia such as:
- Menetrier's disease
- Inflammatory states of systemic lupus erythematosus
| Disease | Clinical manifestations | Diagnostic studies |
|---|---|---|
| Intestinal Tuberculosis[6] |
|
|
| Inflammatory bowel disease[7] |
|
|
| Intestinal lymphoma[8] |
|
|
| Constrictive pericarditis[9] |
|
|
| Sarcoidosis[10] |
|
|
| Systemic sclerosis[11] |
|
|
| Whipple disease[12] |
|
|
| Radiation and/or chemotherapy with retroperitoneal fibrosis[13] |
|
|
| HIV-related enteropathy[14] |
|
|
| Menetrier's disease |
|
|
| Inflammatory states of systemic lupus erythematosus |
|
Epidemiology and Demographics
- The prevalence of PIL is unknown as it can be asymptomatic.
- It primarily affects children (generally diagnosed before the age of 3) and young adults but may be diagnosed later in adults.[15]
- There are rare familial forms that have been reported.
Age
- PIL is more commonly observed among children (less than 3 years old) and young adults.
Race
- There is no racial predilection for PIL.
Risk Factors
- In 1964, Samman and White first described the yellow nail syndrome, a very rare condition that may be associated with PIL. This syndrome is associated with the following symptoms:[3]
- Dystrophic yellow nails
- Nail ridging
- Loss of lunula on the hands
- Lymphedema
- Pleural effusions
- Other five syndromes considered as risk factors and associated with intestinal lymphangiectasia include:[5]
- von Recklinghausen disease or Neurofibromatosis 1 (NF1)
- Turner syndrome (X0)
- Noonan syndrome
- Klippel-Trenaunay syndrome
- Hennekam syndrome
Natural History, Complications and Prognosis
- The majority of patients with PIL remain asymptomatic for years.
- Early clinical features include edema of the lower limbs, diarrhea, and steatorrhea.
- If left untreated, patients with PIL may progress to develop edema of the external genitalia, edema of serous membranes, and life-threatening anasarca.
- Common complications of PIL include:
- A very rare complication is the gelatinous transformation of bone marrow in which hematopoietic cells and adipocytes are replaced by amorphous extracellular material composed of acid mucopolysaccharides.[23]
- PIL is associated with significant morbidity and requires adherence to dietary modification and oral supplements; otherwise. it would be associated with poor outcomes and low quality of life. It can be fatal in some cases if anasarca or malignancy develops.
Diagnosis
Diagnostic Criteria
Biopsy
- PIL is diagnosed by biopsy revealing dilated intestinal lymphatics.
Video-capsule endoscopy
- Video-capsule endoscopy may be helpful when endoscopic findings are not conclusive.
History and Symptoms
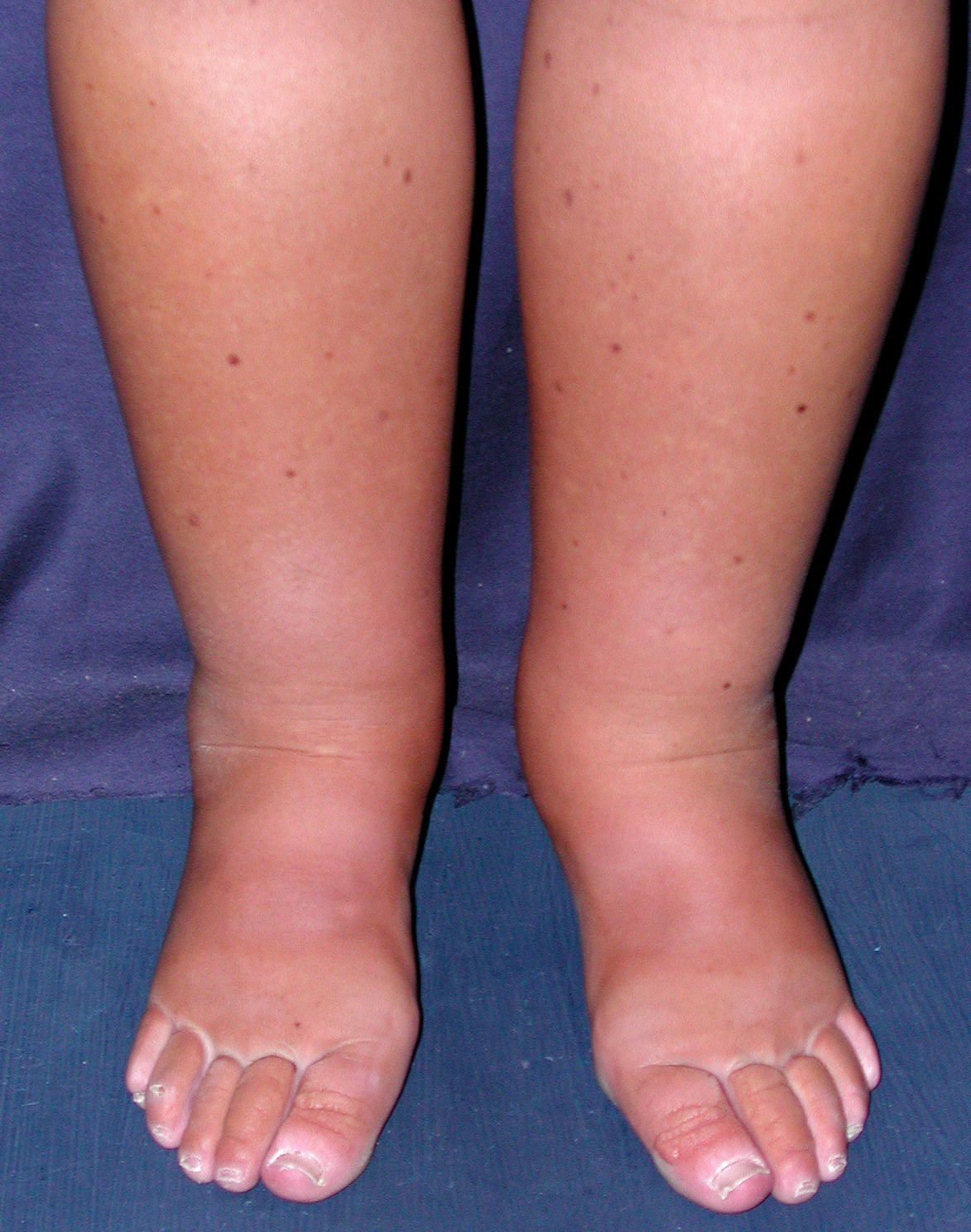
- The hallmark of PIL is pitting edema which usually affects lower limbs in moderate cases and face and external genitalia in severe cases. In some cases, it can extend to serous membranes causing pericardial effusion, pleural effusion, and chylous ascites. Rarely, it can cause anasarca.
- Other symptoms include:
- Diarrhea
- Steatorrhea
- Malabsorption syndrome[24]
- Fatigue
- Abdominal pain
- Abdominal mass[25]
- Immunodeficiency
- Vitamin D deficiency Leading to osteomalacia and convulsions
- Iron deficiency anemia
- Mechanical ileus[26]
- Chylous reflux into skin[27]
- Necrolytic migratory erythema[28]
- Recurrent GI bleeding.[29]
- Recurrent hemolytic uremic syndrome.[30]
- Children have growth retardation, abdominal pain, nausea, and vomiting.
- Lymphedema may be associated with PIL:[31]
- It is less pitting and usually localized to the lower limbs; however, it may involve the upper limbs, breast, and external genitalia.
- Stemmer sign differentiates lymphedema from the pitting edema; in lymphedema, it is impossible to lift and wrinkle the dorsal skin on the second toe due to fibrosis and skin thickening.
 |
Laboratory Findings
- Low albumin level
- Low immunoglobulin IgM, IgA, and IgG levels
- CBC shows lymphopenia
- Elevated 24-hour α1-antitrypsin clearance in stool, which is an indication of the degree of protein loss and disease severity Contrast lymphangiography
Ultrasound
- Ultrasound may be helpful in the diagnosis of PIL.
- Findings on ultrasound suggestive of PIL include:[32]
- Dilation of the intestinal loops
- Diffuse regular thickening of the intestinal wall
- Mesenteric edema
- Ascites (sometimes)
CT scan
- Abdominal CT scan with oral and intravenous contrast medium enhancement may be helpful in the diagnosis of PIL.
- Findings on CT scan suggestive of PIL include:[33]
- Diffuse thickening of the small intestinal wall and edema
- "Halo sign" (in some cases)
- CT scan can also detect the localized lesions.
Albumin scintigraphy
- 99mTechnetium-labeled human serum albumin (99mTc-HSA) scintigraphy may reveal enhancement in the bowel, which indicates protein and lymph leakage into this part.
Lymphangiography
- Lymphangiography may be helpful in the diagnosis of PIL.
- Findings on lymphangiography suggestive of PIL include the abnormal dilation of the intestinal lymphatics.
Treatment
Medical Therapy
- There is no definitive treatment for PIL.
- The mainstay of therapy is a low-fat high protein diet with medium-chain triglyceride oral supplementation and supplemental calcium and vitamins.
- Other reported therapeutic options include:
- Tranexamic acid (used to increase immunoglobulins and lymphocyte count)[34]
- Steroids[35]
- Octreotide[36]
- Albumin infusion
- It is a symptomatic treatment to improve hypoalbuminemia and edema but its effect is transient due to continuous lymph leakage into the bowel lumen.
Surgery
Prevention
- There are no primary preventive measures available for PIL.
References
- ↑ Vignes S, Bellanger J (2008). "Primary intestinal lymphangiectasia (Waldmann's disease)". Orphanet J Rare Dis. 3: 5. doi:10.1186/1750-1172-3-5. PMC 2288596. PMID 18294365.
- ↑ WALDMANN TA, STEINFELD JL, DUTCHER TF, DAVIDSON JD, GORDON RS (1961). "The role of the gastrointestinal system in "idiopathic hypoproteinemia"". Gastroenterology. 41: 197–207. PMID 13782654.
- ↑ 3.0 3.1 Samman, Peter D.; White, William F. (1964). "THE "YELLOW NAIL" SYNDROME". British Journal of Dermatology. 76 (4): 153–157. doi:10.1111/j.1365-2133.1964.tb14499.x. ISSN 0007-0963.
- ↑ 4.0 4.1 Hokari R, Kitagawa N, Watanabe C, Komoto S, Kurihara C, Okada Y; et al. (2008). "Changes in regulatory molecules for lymphangiogenesis in intestinal lymphangiectasia with enteric protein loss". J Gastroenterol Hepatol. 23 (7 Pt 2): e88–95. doi:10.1111/j.1440-1746.2007.05225.x. PMID 18005011.
- ↑ 5.0 5.1 Hennekam RC, Geerdink RA, Hamel BC, Hennekam FA, Kraus P, Rammeloo JA; et al. (1989). "Autosomal recessive intestinal lymphangiectasia and lymphedema, with facial anomalies and mental retardation". Am J Med Genet. 34 (4): 593–600. doi:10.1002/ajmg.1320340429. PMID 2624276.
- ↑ Ploddi A, Atisook K, Hargrove NS (1988). "Intestinal lymphangiectasia in intraabdominal tuberculosis". J Med Assoc Thai. 71 (9): 518–23. PMID 3249186.
- ↑ STEINFELD JL, DAVIDSON JD, GORDON RS, GREENE FE (1960). "The mechanism of hypoproteinemia in patients with regional enteritis and ulcerative colitis". Am J Med. 29: 405–15. doi:10.1016/0002-9343(60)90036-x. PMID 13834226.
- ↑ SUM PT, HOFFMAN MM, WEBSTER DR (1964). "PROTEIN-LOSING GASTROENTEROPATHY IN PATIENTS WITH GASTROINTESTINAL CANCER". Can J Surg. 7: 1–5. PMID 14103417.
- ↑ Wilkinson P, Pinto B, Senior JR (1965). "Reversible protein-losing enteropathy with intestinal lymphangiectasia secondary to chronic constrictive pericarditis". N Engl J Med. 273 (22): 1178–81. doi:10.1056/NEJM196511252732202. PMID 5847556.
- ↑ Popović OS, Brkić S, Bojić P, Kenić V, Jojić N, Djurić V; et al. (1980). "Sarcoidosis and protein losing enteropathy". Gastroenterology. 78 (1): 119–25. PMID 7350018.
- ↑ van Tilburg AJ, van Blankenstein M, Verschoor L (1988). "Intestinal lymphangiectasia in systemic sclerosis". Am J Gastroenterol. 83 (12): 1418–9. PMID 3195550.
- ↑ Laster L, Waldmann TA, Fenster LF, Singleton JW (1966). "Albumin metabolism in patients with Whipple's disease". J Clin Invest. 45 (5): 637–44. doi:10.1172/JCI105379. PMC 292741. PMID 4160668.
- ↑ Rao SS, Dundas S, Holdsworth CD (1987). "Intestinal lymphangiectasia secondary to radiotherapy and chemotherapy". Dig Dis Sci. 32 (8): 939–42. doi:10.1007/BF01296718. PMID 3608736.
- ↑ Stockmann M, Fromm M, Schmitz H, Schmidt W, Riecken EO, Schulzke JD (1998). "Duodenal biopsies of HIV-infected patients with diarrhoea exhibit epithelial barrier defects but no active secretion". AIDS. 12 (1): 43–51. doi:10.1097/00002030-199801000-00006. PMID 9456254.
- ↑ Tift WL, Lloyd JK (1975). "Intestinal lymphangiectasia. Long-term results with MCT diet". Arch Dis Child. 50 (4): 269–76. doi:10.1136/adc.50.4.269. PMC 1544468. PMID 50050.
- ↑ Hallevy C, Sperber AD, Almog Y (2003). "Group G streptococcal empyema complicating primary intestinal lymphangiectasia". J Clin Gastroenterol. 37 (3): 270. doi:10.1097/00004836-200309000-00015. PMID 12960729.
- ↑ Jabeen SA, Murthy A, Kandadai RM, Meena AK, Borgohain R, Uppin MS (2012). "Cryptoccocal menigitis as a primary manifestation in a patient with intestinal lymphangictasia". Ann Indian Acad Neurol. 15 (3): 218–20. doi:10.4103/0972-2327.99725. PMC 3424804. PMID 22919199.
- ↑ 18.0 18.1 Ward M, Le Roux A, Small WP, Sircus W (1977). "Malignant lymphoma and extensive viral wart formation in a patient with intestinal lymphangiectasia and lymphocyte depletion". Postgrad Med J. 53 (626): 753–7. doi:10.1136/pgmj.53.626.753. PMC 2496800. PMID 604991.
- ↑ 19.0 19.1 Gumà J, Rubió J, Masip C, Alvaro T, Borràs JL (1998). "Aggressive bowel lymphoma in a patient with intestinal lymphangiectasia and widespread viral warts". Ann Oncol. 9 (12): 1355–6. doi:10.1023/a:1008496900822. PMID 9932170.
- ↑ Bouhnik Y, Etienney I, Nemeth J, Thevenot T, Lavergne-Slove A, Matuchansky C (2000). "Very late onset small intestinal B cell lymphoma associated with primary intestinal lymphangiectasia and diffuse cutaneous warts". Gut. 47 (2): 296–300. doi:10.1136/gut.47.2.296. PMC 1728014. PMID 10896925.
- ↑ Broder S, Callihan TR, Jaffe ES, DeVita VT, Strober W, Bartter FC; et al. (1981). "Resolution of longstanding protein-losing enteropathy in a patient with intestinal lymphangiectasia after treatment for malignant lymphoma". Gastroenterology. 80 (1): 166–8. PMID 7450403.
- ↑ Weiden PL, Blaese RM, Strober W, Block JB, Waldmann TA (1972). "Impaired lymphocyte transformation in intestinal lymphangiectasia: evidence for at least two functionally distinct lymphocyte populations in man". J Clin Invest. 51 (6): 1319–25. doi:10.1172/JCI106928. PMC 292269. PMID 4554185.
- ↑ Marie I, Levesque H, Heron F, Courtois H, Callat MP (1999). "Gelatinous transformation of the bone marrow: an uncommon manifestation of intestinal lymphangiectasia (Waldmann's disease)". Am J Med. 107 (1): 99–100. doi:10.1016/s0002-9343(99)00035-2. PMID 10403358.
- ↑ Lobo B, Casellas F, de Torres I, Chicharro L, Malagelada JR (2004). "Usefulness of jejunal biopsy in the study of intestinal malabsorption in the elderly". Rev Esp Enferm Dig. 96 (4): 259–64. doi:10.4321/s1130-01082004000400005. PMID 15117239.
- ↑ Rao R, Shashidhar H (2007). "Intestinal lymphangiectasia presenting as abdominal mass". Gastrointest Endosc. 65 (3): 522–3, discussion 523. doi:10.1016/j.gie.2006.10.026. PMID 17321261.
- ↑ Lenzhofer R, Lindner M, Moser A, Berger J, Schuschnigg C, Thurner J (1993). "Acute jejunal ileus in intestinal lymphangiectasia". Clin Investig. 71 (7): 568–71. doi:10.1007/BF00208483. PMID 8374252.
- ↑ O'Driscoll JB, Chalmers RJ, Warnes TW (1991). "Chylous reflux into abdominal skin simulating lymphangioma circumscriptum in a patient with primary intestinal lymphangiectasia". Clin Exp Dermatol. 16 (2): 124–6. doi:10.1111/j.1365-2230.1991.tb00322.x. PMID 2032374.
- ↑ Baricault S, Soubrane JC, Courville P, Young P, Joly P (2006). "[Necrolytic migratory erythema in Waldmann's disease]". Ann Dermatol Venereol. 133 (8-9 Pt 1): 693–6. doi:10.1016/s0151-9638(06)70994-2. PMID 17053741.
- ↑ Herfarth H, Hofstädter F, Feuerbach S, Jürgen Schlitt H, Schölmerich J, Rogler G (2007). "A case of recurrent gastrointestinal bleeding and protein-losing gastroenteropathy". Nat Clin Pract Gastroenterol Hepatol. 4 (5): 288–93. doi:10.1038/ncpgasthep0812. PMID 17476211.
- ↑ Kalman S, Bakkaloğlu S, Dalgiç B, Ozkaya O, Söylemezoğlu O, Buyan N (2007). "Recurrent hemolytic uremic syndrome associated with intestinal lymphangiectasia". J Nephrol. 20 (2): 246–9. PMID 17514630.
- ↑ Goktan C, Pekindil G, Orguc S, Coskun T, Serter S (2005). "Bilateral breast edema in intestinal lymphangiectasia". Breast J. 11 (5): 360. doi:10.1111/j.1075-122X.2005.21578.x. PMID 16174162.
- ↑ Dorne HL, Jequier S (1986). "Sonography of intestinal lymphangiectasia". J Ultrasound Med. 5 (1): 13–6. doi:10.7863/jum.1986.5.1.13. PMID 3511270.
- ↑ Fakhri A, Fishman EK, Jones B, Kuhajda F, Siegelman SS (1985). "Primary intestinal lymphangiectasia: clinical and CT findings". J Comput Assist Tomogr. 9 (4): 767–70. PMID 4019833.
- ↑ MacLean JE, Cohen E, Weinstein M (2002). "Primary intestinal and thoracic lymphangiectasia: a response to antiplasmin therapy". Pediatrics. 109 (6): 1177–80. doi:10.1542/peds.109.6.1177. PMID 12042562.
- ↑ Edworthy SM, Fritzler MJ, Kelly JK, McHattie JD, Shaffer EA (1990). "Protein-losing enteropathy in systemic lupus erythematosus associated with intestinal lymphangiectasia". Am J Gastroenterol. 85 (10): 1398–402. PMID 2220736.
- ↑ Klingenberg RD, Homann N, Ludwig D (2003). "Type I intestinal lymphangiectasia treated successfully with slow-release octreotide". Dig Dis Sci. 48 (8): 1506–9. doi:10.1023/a:1024707605493. PMID 12924644.
- ↑ Chen CP, Chao Y, Li CP, Lo WC, Wu CW, Tsay SH; et al. (2003). "Surgical resection of duodenal lymphangiectasia: a case report". World J Gastroenterol. 9 (12): 2880–2. doi:10.3748/wjg.v9.i12.2880. PMC 4612079. PMID 14669360.