Lymphadenopathy physical examination
|
Lymphadenopathy Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Lymphadenopathy physical examination On the Web |
|
American Roentgen Ray Society Images of Lymphadenopathy physical examination |
|
Risk calculators and risk factors for Lymphadenopathy physical examination |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Raviteja Guddeti, M.B.B.S. [2]Amandeep Singh M.D.[3] Ogechukwu Hannah Nnabude, MD
Overview
Common physical examination findings of lymphadenopathy include fever and tachycardia in infectious causes. There is an enlargement of different groups of lymph node chains depending upon the site of involvement and the underlying causes.
Physical Examination
Vitals
- Temperature
Skin
- A rash may be present
- A fistula draining pus can be seen in bubos
- Color change (indicative of inflammation)
- Ulcers are formed when the abscess ruptures in chronic infections
Head
- The major lymph node groups are located along with the anterior and posterior aspects of the neck and on the underside of the jaw. If the nodes are quite big, they can be seen bulging under the skin, particularly if the enlargement is asymmetric (i.e. it will be more obvious if one side is larger than the other). To palpate, the pads of all four fingertips are used as they are the most sensitive parts of the hands. The major groups of lymph nodes, as well as the structures that they drain, are listed below.
- Nodes are generally examined in the following order:[1][2]
- Anterior Cervical (both superficial and deep): Nodes that lie both on top of and beneath the sternocleidomastoid muscles (SCM) on either side of the neck, from the angle of the jaw to the top of the clavicle. This muscle allows the head to turn to the right and left. The right SCM turns the head to the left and vice versa. They can be easily identified by asking the patient to turn their head into your hand while you provide resistance. Drainage: The internal structures of the throat as well as part of the posterior pharynx, tonsils, and thyroid gland.
- Posterior Cervical: Extend in a line posterior to the SCMs but in front of the trapezius, from the level of the mastoid bone to the clavicle. Drainage: The skin on the back of the head. Also frequently enlarged during upper respiratory infections (e.g. mononucleosis).
- Tonsillar: Located just below the angle of the mandible. Drainage: The tonsilar and posterior pharyngeal regions.
- Sub-Mandibular: Along the underside of the jaw on either side. Drainage: The structures on the floor of the mouth.
- Sub-Mental: Just below the chin. Drainage: The teeth and intra-oral cavity.
- Supra-clavicular: In the hollow above the clavicle, just lateral to where it joins the sternum. Drainage: Part of the thoracic cavity, abdomen.
- A number of other lymph node groups exist. However, palpation of these areas is limited to those situations when a problem is identified in that specific region (e.g. the pre-auricular nodes, located in front of the ears, may become inflamed during infections of the external canal of the ear).
- Characteristics to be noted while palpating lymph nodes:
- Size
- Pain/ tenderness
- Consistency
- Matting
- Location
- Infected lymph nodes tend to be firm, tender, enlarged, and warm. Inflammation can spread to the overlying skin, causing it to appear reddened.
- Malignancies may also involve the lymph nodes, either primarily (e.g. lymphoma) or as a site of metastasis. In either case, these nodes are generally firm, non-tender, matted (i.e. stuck to each other), fixed (i.e. not freely mobile but rather stuck down to underlying tissue), and increase in size over time.
Gallery
(Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA)
-
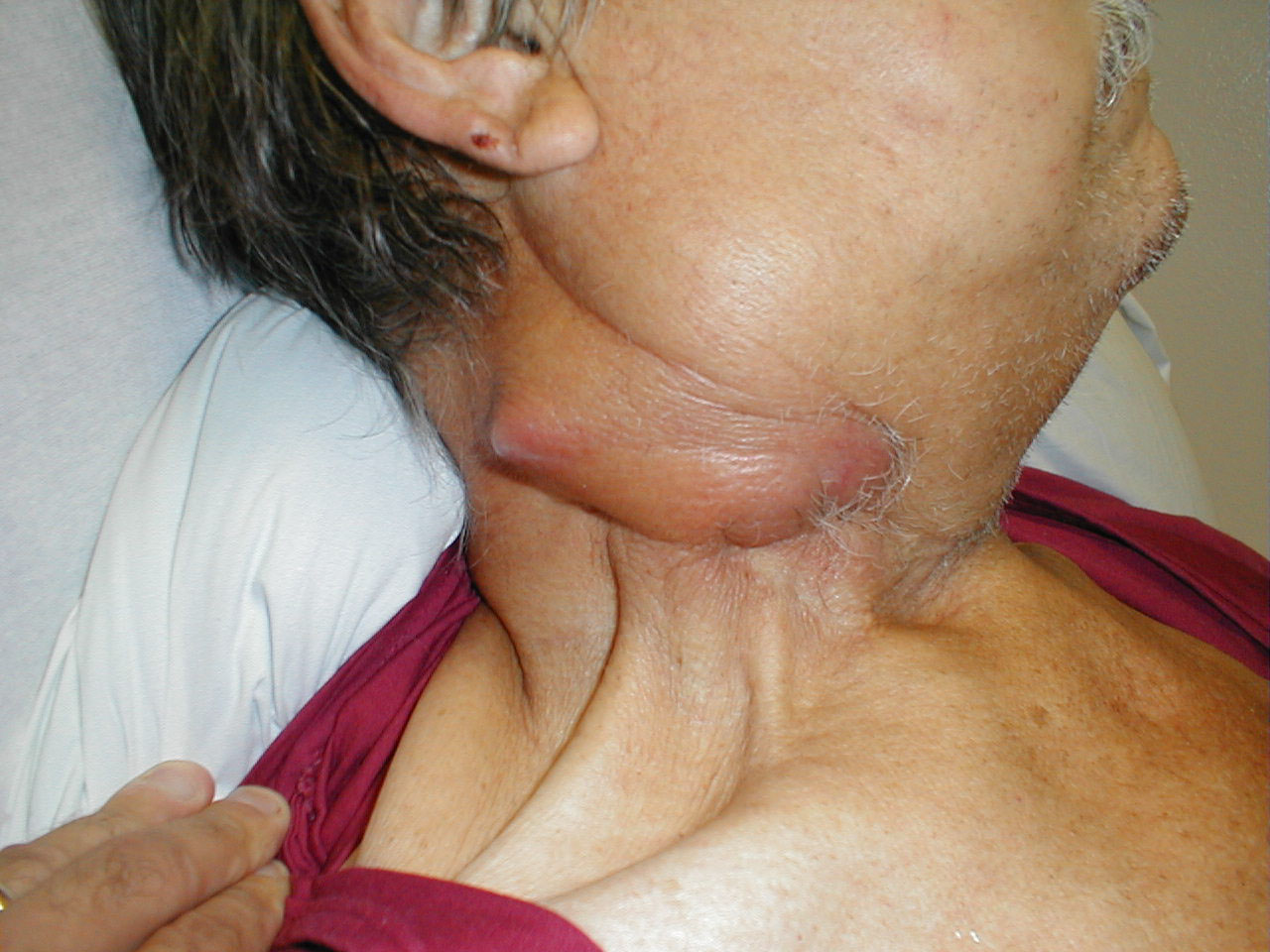
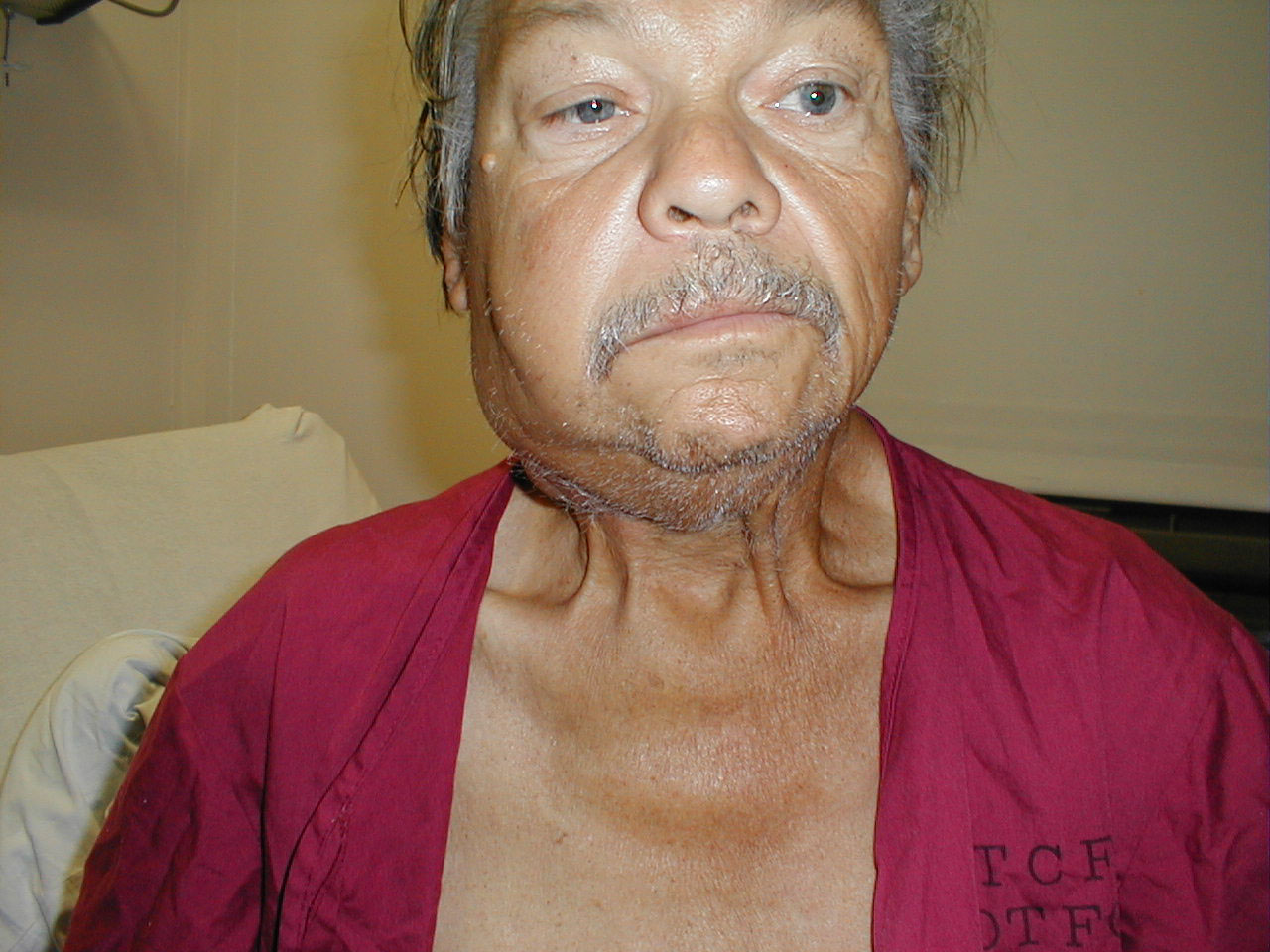
Cervical adenopathy: massive right side cervical adenopathy and facial asymmetry due to metastatic, intraoral squamous cell cancer. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
-
Cervical adenopathy: massive right side cervical adenopathy and facial asymmetry due to metastatic, intraoral squamous cell cancer. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
-
Cervical adenopathy: large right anterior cervical lymph node. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
-
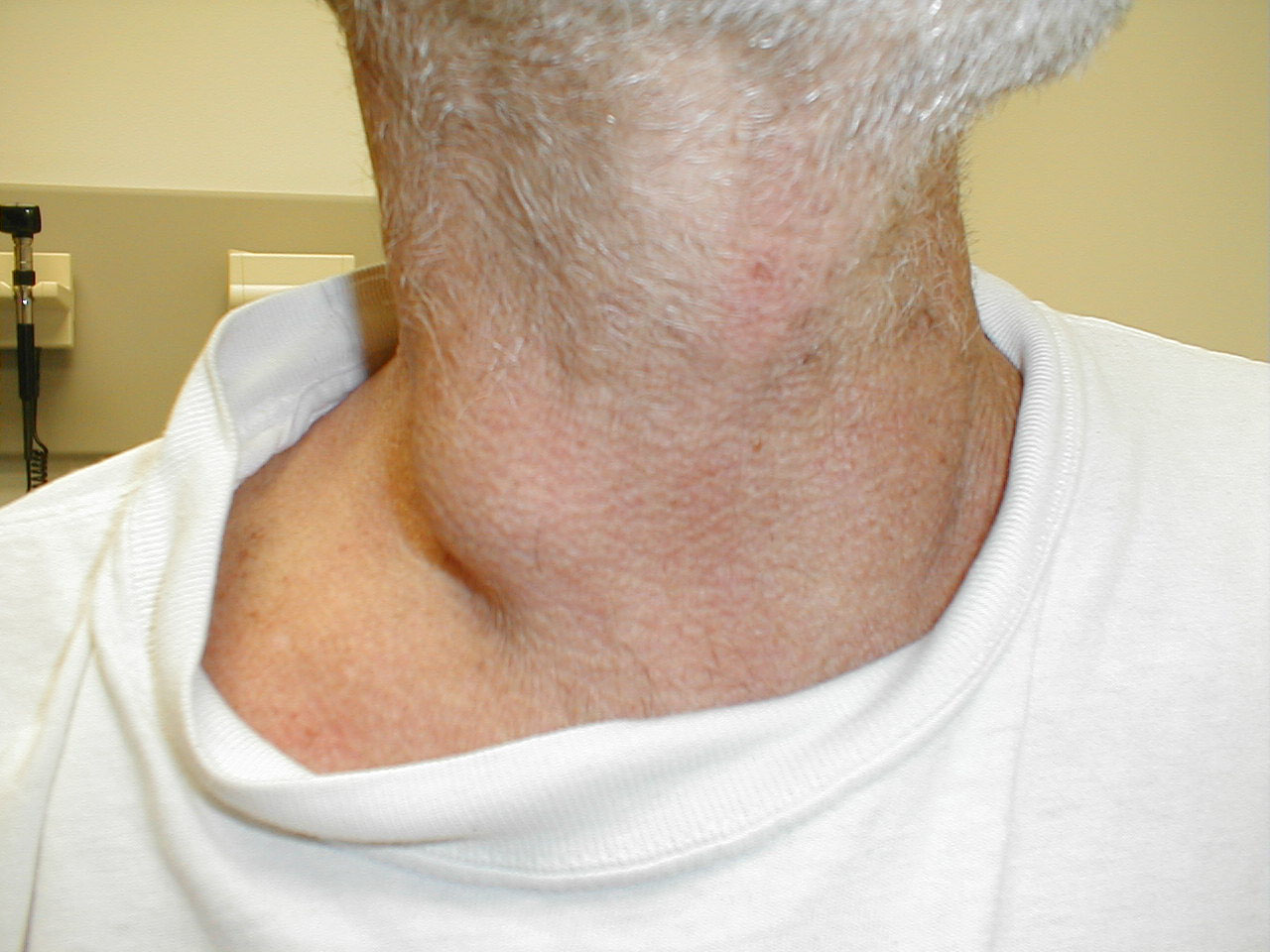
Cervical lymphadenopathy. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
-
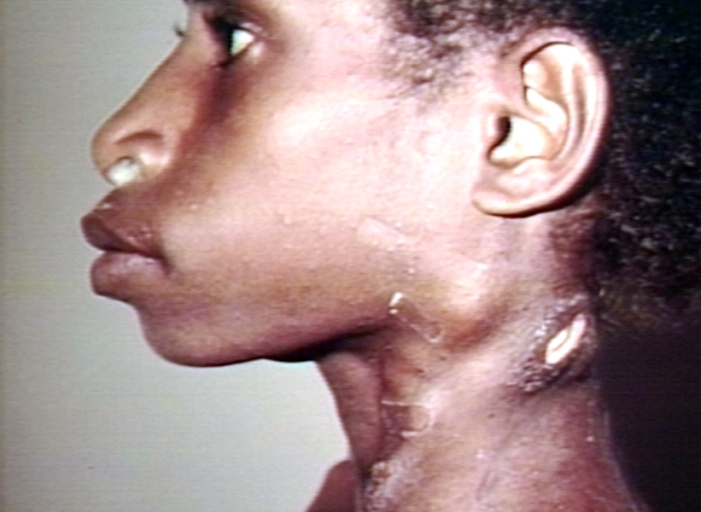
Cervical Adenopathy: multiple right-sided cervical lymph nodes. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.