Hydatidiform mole
For patient information, click here
| Hydatidiform mole | |
 | |
|---|---|
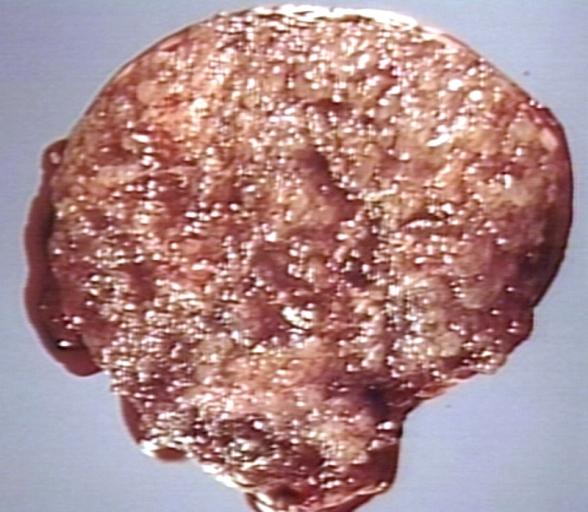
| MOLE, HYDATIDIFORM, HYSTERECTOMY SPECIMEN. VARIABLY SIZED VESICLES, NO NORMAL PLACENTA, NO FETUS. Image courtesy of Professor Peter Anderson DVM PhD and published with permission. © PEIR, University of Alabama at Birmingham, Department of Pathology |
Template:Search infobox Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]Associate Editor(s)-in-Chief: Monalisa Dmello, M.B,B.S., M.D. [2]
Synonyms and keywords: Molar pregancy, Complete mole, Incomplete mole, Complete hydatidiform mole, Incomplete hydatidiform mole, Hmole, Complete hmole, Incomplete hmole.
Overview
Hydatidiform mole (or mola hydatidiforma) is a common complication of pregnancy, it consists of a nonviable embryo which implants and proliferates within the uterus.[1] The term is derived from hydatidiform ("like a bunch of grapes") and mole (from Latin mola = millstone).
Most moles present with painless vaginal bleeding during the second trimester of pregnancy. They are diagnosed by ultrasound imaging. Extremely high levels of human chorionic gonadotropin (HCG) are suggestive, but not diagnostic, of molar pregnancy.[2] Hydatidiform moles are surgically removed by curettage, in order to avoid the risks of choriocarcinoma.[3]
Incidence and Mortality
Hydatidiform mole is a common complication of pregnancy, occurring once in every 1000 pregnancies in the US, with much higher rates in Asia (e.g. up to one in 100 pregnancies in Indonesia).[4]
Region No of cases Ratio per 100 000 Ref Pregnancies Deliveries Live births Europe Denmark 1520 110 ·· ·· 6 England and Wales 5124 ·· ·· 154 7 Italy 347 66 ·· ·· 8 Sweden ·· 91 146 ·· 9 North America Canada 171 83 ·· ·· 10 United States ·· ·· 389 ·· 11 128 ·· ·· 460 12 185 108 ·· ·· 13 180 121 ·· ·· 14 939 121 ·· 145 15 Oceania Australia 455 ·· ·· 74 16 New Zealand 350 67 ·· ·· 17 Latin America Brazil 65 465 ·· ·· 18 Mexico 83 ·· ·· 240 19 Paraguay 227 23 ·· ·· 20 ·· 25 ·· ·· 21 Middle East Iran 113 320 ·· 370 22 Saudi Arabia ·· ·· 223 ·· 23 71 ·· ·· 148 24 Turkey 2227 580 260 ·· 25 Asia China 8832 81 ·· ·· 26 Indonesia 406 1299 1754 ·· 27 Japan 91 ·· ·· 165 28 Korea 3831 ·· 230 ·· 29 Pakistan 413 389 212 ·· 30 Singapore 198 ·· 115 ·· 31 Africa Nigeria ·· ·· 543 ·· 32
Classification
Gestational trophoblastic disease (GTD) may be classified as follows:[5]
- Hydatidiform mole (HM)
- Complete HM
- Partial HM
Pathophysiology
A hydatidiform mole is characterized by a conceptus of hyperplastic trophoblastic tissue attached to the placenta. The conceptus does not contain the inner cell mass. The hydatidiform mole can be of two types:
- Complete moles usually occur when an empty ovum is fertilized by a sperm that then duplicates its own DNA. A 46, XY genotype may occur when 2 sperm (one 23, X and the other 23, Y) fertilize an empty egg.[6] Their DNA is purely paternal in origin, and is diploid. Ninety percent are 46,XX, and 10% are 46,XY. In a complete mole, the fetus fails to develop.
- Partial moles can develop either if a normal haploid ovum is fertilized by two sperm or if an ovum is fertilized by one sperm which further duplicates its chromosomes. Thus their DNA is both maternal and paternal in origin. They can be triploid (e.g. 69 XXX, 69 XXY) or even tetraploid.
Pathology
Shown below is a table depicting the gross and microscopic pathology of hydatidiform mole.[7]
| Type of hydatidiform mole | Gross pathology | Microscopic pathology | Immunohistochemistry |
| Complete hydatidiform mole |
|
Chorionic villi:
Cisterns:
Blood vessels
|
p57(KIP2) -ve |
| Incomplete hydatidiform mole |
|
Chorionic villi:
Cisterns:
Blood vessels
|
p57(KIP2) +ve |
{{#ev:youtube|QO3QF6n4xuo}}
Symptoms
Early symptoms of gestational trophoblastic disease
- Vaginal bleeding[8]
- Nausea and vomiting
- Passing of tissue resembling a “bunch of grapes” from the vagina
- Absent fetal movement during pregnancy
- Abdominal distention
Rare symptoms of gestational trophoblastic disease
- Headache
- Edema of the hands and feet
- Abdominal or pelvic pain
- Vaginal discharge
- Overactive thyroid gland (hyperthyroidism) that causes:
- Tachycardia
- Sweating
- Shaking
- Heat intolerance
- Fever
Diagnosis
Laboratory Findings
Quantitative serum HCG
- Human chorionic gonadotropin (HCG or b-HCG) is the most common tumor marker test used to diagnose GTD[5]
- HCG is a very sensitive test for diagnosing most gestational trophoblastic tumors. HCG is usually measured in the blood, but it can also be measured in the urine
- HCG levels are much higher in women with complete hydatidiform mole compared to HCG levels in women with a normal pregnancy
- With partial moles, the HCG level is higher than normal, but it is not as high as with other types of GTD
- An HCG test can help find GTD after pregnancy or miscarriage as this hormone should not be present in the blood or urine soon afterward
Complete blood count
- Complete blood count can check for anemia from long-term (chronic) vaginal bleeding.
Thyroid-stimulating hormone
Sometimes symptoms of hyperthyroidism are seen, due to the extremely high levels of hCG, which can mimic the normal thyroid-stimulating hormone (TSH).[9]
Diagnostic Findings
Ultrasonography
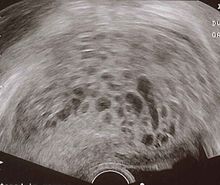
Complete hydatidiform mole
- Enlarged uterus[11]
- Classic sonographic appearance is that of a solid collection of echoes with numerous small (3-10 mm 6) anechoic spaces (snowstorm or granular appearance)
- The term snowstorm sign usually dates back to earlier ultrasound equipment with inferior resolution
- The molar tissue demonstrates the bunch of grapes sign which represents hydropic swelling of trophoblastic villi
- Variable appearance
- Normal interface between abnormal trophoblastic tissue and myometrium
- No identifiable fetal tissue or gestational sac is seen
- Color doppler interrogation may show high velocity, low impedance flow
Partial mole
- Placenta is enlarged and contains areas of multiple, diffuse anechoic lesions
- A fetus with severe structural abnormalities or growth restriction, oligohydramnios, or a deformed gestational sac may be noted
- Color doppler interrogation may show high velocity, low impedance flow
Other features may include
- Ovarian theca lutein cysts: may be seen bilaterally in 25-60% of cases
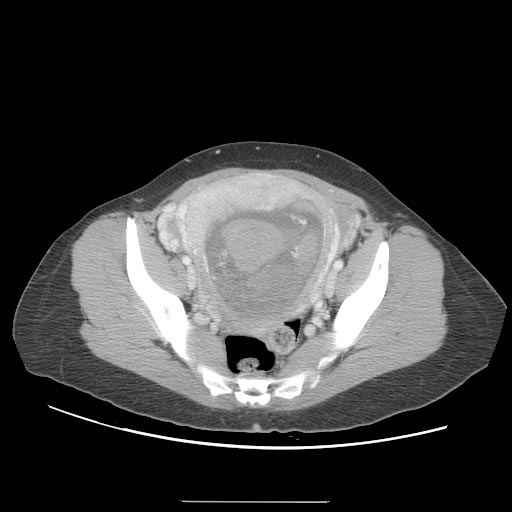
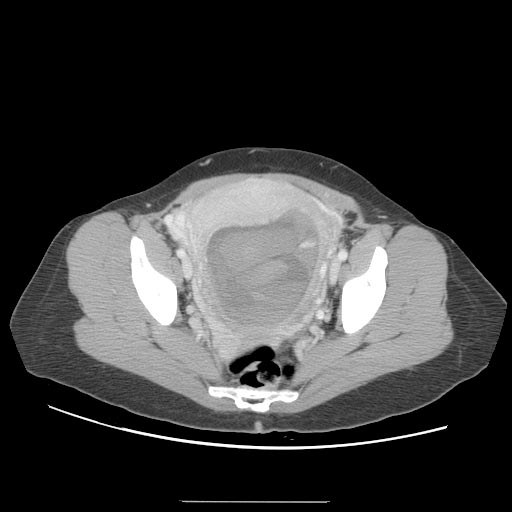
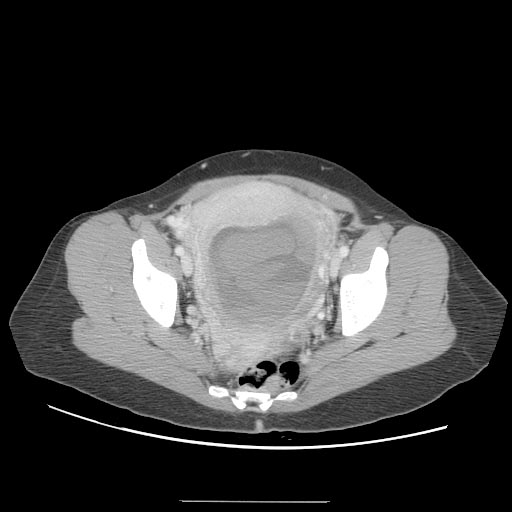
CT
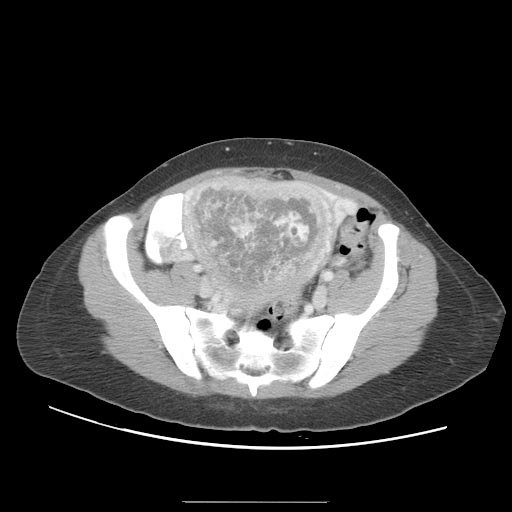
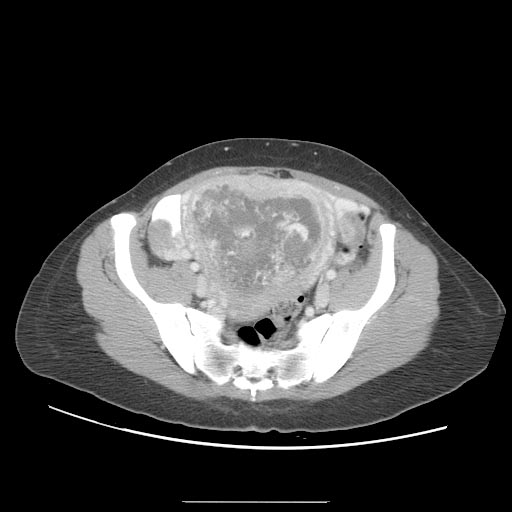
A CT scan usually demonstrates a normal-sized uterus with areas of low attenuation, an enlarged inhomogeneous uterus with a central area of low attenuation, or hypoattenuating foci surrounded by highly enhanced areas in the myometrium.[12]
Treatment
Dilation and curettage (D&C) [13]
- D&C is a treatment option for women diagnosed with complete or partial hydatidiform moles by human chorionic gonadotropin (HCG or b-HCG) testing or ultrasound.
- D&C will not be done if a gestational choriocarcinoma is suspected because this type of tumor bleeds very easily.
- Management is more complicated when the mole occurs together with one or more normal fetuses.
- D&C is a treatment option for women diagnosed with complete or partial hydatidiform moles by human chorionic gonadotropin (HCG or b-HCG) testing or ultrasound. D&C will not be done if a gestational choriocarcinoma is suspected because this type of tumor bleeds very easily.
Chemotherapy
- Indications:[8]
- Chemotherapy is necessary when patients present with the following:
- A rising beta-hCG titer for 2 weeks (3 titers)
- A tissue diagnosis of choriocarcinoma
- A plateau of the beta-hCG for 3 weeks
- Persistence of detectable beta-hCG 6 months after mole evacuation
- Metastatic disease
- An elevation in beta-hCG after a normal value
- Postevacuation hemorrhage not caused by retained tissues
- Chemotherapy is ultimately required for persistence or neoplastic transformation in about 15% to 20% of patients after evacuation of a complete HM but for fewer than 5% of patients with partial HM. Chemotherapy is determined by the patient's modified World Health Organization score.
- Studies have shown that a single course of prophylactic dactinomycin or methotrexate can decrease the risk of a postmolar gestational trophoblastic disease (GTD). However, there is concern that chemoprophylaxis increases tumor resistance to standard therapy in the women who subsequently develop GTD. Therefore, this practice is generally limited to countries in which a large number of women do not return for follow-up.
Prognosis
- More than 80% of hydatidiform moles are benign. The outcome after treatment is usually excellent. Close follow-up is essential. Highly effective means of contraception are recommended to avoid pregnancy for at least 6 to 12 months.
- In 10 to 15% of cases, hydatidiform moles may develop into invasive moles. These may intrude so far into the uterine wall that hemorrhage or other complications develop. It is for this reason that a post-operative full abdominal and chest x-ray will often be requested.
- In 2 to 3% of cases, hydatidiform moles may develop into choriocarcinoma, which is a malignant, rapidly-growing, and metastatic (spreading) form of cancer. Despite these factors which normally indicate a poor prognosis, the rate of cure after treatment with chemotherapy is high.
- Over 90% of women with malignant, non-spreading cancer are able to survive and retain their ability to have children. In those with metastatic (spreading) cancer, remission remains at 75 to 85%, although the ability to have children is usually lost.
In women with complete HM, risk of persistence or neoplastic transformation is approximately doubled in the setting of certain characteristics, which include the following:[8]
- Age older than 35 years or age younger than 20 years
- Pre-evacuation serum beta-hCG greater than 100,000 IU/L
- Large-for-date uterus
- Large uterine molar mass
- Large (>6 cm) ovarian cysts
- Pre-eclampsia
- Hyperthyroidism
- Hyperemesis of pregnancy
- Trophoblastic embolization
- Disseminated intravascular coagulation
The modified World Health Organization [WHO] prognostic scoring system is as follows:[14]
| Modified WHO Prognostic Scoring System as Adapted by FIGO | ||||
| Scores | 0 | 1 | 2 | 4 |
| Age | <40 | ≥40 | – | – |
| Antecedent pregnancy | mole | abortion | term | – |
| Interval months from index pregnancy | <4 | 4–6 | 7–12 | >12 |
| Pretreatment serum hCG (iu/1) | <103 | 103–104 | 104–105 | >105 |
| Largest tumor size (including uterus) | <3 | 3–4 cm | ≥5 cm | – |
| Site of metastases | lung | spleen, kidney | gastrointestinal | liver, brain |
| Number of metastases | – | 1–4 | 5–8 | >8 |
| Previous failed chemotherapy | – | – | single drug | ≥2 drugs |
References
- ↑ Robbins and Cotran's Pathological Basis of Disease, 7th ed., p. 1110
- ↑ McPhee S. and Ganong W.F. Pathophysiology of Disease, 5th ed., p. 639.
- ↑ Robbins and Cotran's Pathological Basis of Disease, 7th ed., p. 1112
- ↑ Title of page. Website title (date). URL Accessed on Month Day, 2015
- ↑ 5.0 5.1 Cellular Classification of Gestational Trophoblastic Disease. National Cancer Institute. http://www.cancer.gov/types/gestational-trophoblastic/hp/gtd-treatment-pdq/#section/_5 Accessed on October 8, 2015
- ↑ Woo J, Hsu C, Fung L, Ma H (1983). "Partial hydatidiform mole: ultrasonographic features". Aust N Z J Obstet Gynaecol. 23 (2): 103–7. PMID 6578773.
- ↑ Gestational trophoblastic disease. http://librepathology.org/wiki/index.php/Gestational_trophoblastic_disease#Hydatidiform_moles. URL Accessed on Nov 2, 2015
- ↑ 8.0 8.1 8.2 Signs and symptoms of gestational trophoblastic disease. Canadian Cancer Society. http://www.cancer.ca/en/cancer-information/cancer-type/gestational-trophoblastic-disease/signs-and-symptoms/?region=ns Accessed on October 10, 2015
- ↑ McPhee S. and Ganong W.F. Pathophysiology of Disease, 5th ed., p. 639.
- ↑ https://en.wikipedia.org/wiki/Molar_pregnancy
- ↑ Hydatidiform mole. http://radiopaedia.org/articles/hydatidiform-mole. URL Accessed on October 28, 2015
- ↑ Hydatidiform mole. http://radiopaedia.org/articles/hydatidiform-mole. URL Accessed on October 28, 2015
- ↑ Cotran RS, Kumar V, Fausto N, Nelso F, Robbins SL, Abbas AK (2005). Robbins and Cotran pathologic basis of disease (7th ed. ed.). St. Louis, Mo: Elsevier Saunders. p. 1112. ISBN 0-7216-0187-1.
- ↑ Stage Information for Gestational Trophoblastic Disease. National Cancer Institute. http://www.cancer.gov/types/gestational-trophoblastic/hp/gtd-treatment-pdq#section/_11 URL Accessed on October 27, 2015
See also