COVID-19-associated dermatologic manifestations: Difference between revisions
Aditya Ganti (talk | contribs) |
Jose Loyola (talk | contribs) |
||
| (25 intermediate revisions by 5 users not shown) | |||
| Line 1: | Line 1: | ||
__NOTOC__ | __NOTOC__ | ||
{{COVID-19}} | {{COVID-19}} | ||
{{CMG}} {{AE}} {{Nuha}} [[Ogechukwu Hannah Nnabude, MD]]; {{ADG}} | {{Main|COVID-19}} | ||
'''For COVID-19 frequently asked inpatient questions, click [[COVID-19 frequently asked inpatient questions|here]]'''<br> | |||
'''For COVID-19 frequently asked outpatient questions, click [[COVID-19 frequently asked outpatient questions|here]]'''<br> | |||
{{CMG}} {{AE}} {{Nuha}} [[Ogechukwu Hannah Nnabude, MD]]; {{ADG}} <br> | |||
{{SK}} [[COVID-19-associated exanthematous rash]]; [[COVID-19-associated livedo reticularis]]; [[COVID-19-associated livedoid lesions]]; [[COVID-19-associated multisystem inflammatory syndrome in children]]; [[COVID-19-associated retiform purpura]]; [[COVID-19-associated urticaria]]; [[COVID-19-associated vasculitis]]; [[COVID-19-associated vesicular eruptions]] | |||
==Overview== | ==Overview== | ||
| Line 15: | Line 21: | ||
*The etiological agent, a novel coronavirus, SARS-CoV-2, is a [[virus]] identified as the cause of an outbreak of [[respiratory illness]] first detected in Wuhan, China.<ref>{{Cite web|url=https://www.cdc.gov/coronavirus/2019-ncov/about/index.html|title=|last=|first=|date=|website=|archive-url=|archive-date=|dead-url=|access-date=}}</ref><ref name="LuCui2020">{{cite journal|last1=Lu|first1=Jian|last2=Cui|first2=Jie|last3=Qian|first3=Zhaohui|last4=Wang|first4=Yirong|last5=Zhang|first5=Hong|last6=Duan|first6=Yuange|last7=Wu|first7=Xinkai|last8=Yao|first8=Xinmin|last9=Song|first9=Yuhe|last10=Li|first10=Xiang|last11=Wu|first11=Changcheng|last12=Tang|first12=Xiaolu|title=On the origin and continuing evolution of SARS-CoV-2|journal=National Science Review|year=2020|issn=2095-5138|doi=10.1093/nsr/nwaa036}}</ref><ref name="HuangWang2020">{{cite journal|last1=Huang|first1=Chaolin|last2=Wang|first2=Yeming|last3=Li|first3=Xingwang|last4=Ren|first4=Lili|last5=Zhao|first5=Jianping|last6=Hu|first6=Yi|last7=Zhang|first7=Li|last8=Fan|first8=Guohui|last9=Xu|first9=Jiuyang|last10=Gu|first10=Xiaoying|last11=Cheng|first11=Zhenshun|last12=Yu|first12=Ting|last13=Xia|first13=Jiaan|last14=Wei|first14=Yuan|last15=Wu|first15=Wenjuan|last16=Xie|first16=Xuelei|last17=Yin|first17=Wen|last18=Li|first18=Hui|last19=Liu|first19=Min|last20=Xiao|first20=Yan|last21=Gao|first21=Hong|last22=Guo|first22=Li|last23=Xie|first23=Jungang|last24=Wang|first24=Guangfa|last25=Jiang|first25=Rongmeng|last26=Gao|first26=Zhancheng|last27=Jin|first27=Qi|last28=Wang|first28=Jianwei|last29=Cao|first29=Bin|title=Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China|journal=The Lancet|volume=395|issue=10223|year=2020|pages=497–506|issn=01406736|doi=10.1016/S0140-6736(20)30183-5}}</ref><ref>{{Cite web|url=https://www.cdc.gov/coronavirus/2019-ncov/about/transmission.html|title=|last=|first=|date=|website=|archive-url=|archive-date=|dead-url=|access-date=}}</ref> | *The etiological agent, a novel coronavirus, SARS-CoV-2, is a [[virus]] identified as the cause of an outbreak of [[respiratory illness]] first detected in Wuhan, China.<ref>{{Cite web|url=https://www.cdc.gov/coronavirus/2019-ncov/about/index.html|title=|last=|first=|date=|website=|archive-url=|archive-date=|dead-url=|access-date=}}</ref><ref name="LuCui2020">{{cite journal|last1=Lu|first1=Jian|last2=Cui|first2=Jie|last3=Qian|first3=Zhaohui|last4=Wang|first4=Yirong|last5=Zhang|first5=Hong|last6=Duan|first6=Yuange|last7=Wu|first7=Xinkai|last8=Yao|first8=Xinmin|last9=Song|first9=Yuhe|last10=Li|first10=Xiang|last11=Wu|first11=Changcheng|last12=Tang|first12=Xiaolu|title=On the origin and continuing evolution of SARS-CoV-2|journal=National Science Review|year=2020|issn=2095-5138|doi=10.1093/nsr/nwaa036}}</ref><ref name="HuangWang2020">{{cite journal|last1=Huang|first1=Chaolin|last2=Wang|first2=Yeming|last3=Li|first3=Xingwang|last4=Ren|first4=Lili|last5=Zhao|first5=Jianping|last6=Hu|first6=Yi|last7=Zhang|first7=Li|last8=Fan|first8=Guohui|last9=Xu|first9=Jiuyang|last10=Gu|first10=Xiaoying|last11=Cheng|first11=Zhenshun|last12=Yu|first12=Ting|last13=Xia|first13=Jiaan|last14=Wei|first14=Yuan|last15=Wu|first15=Wenjuan|last16=Xie|first16=Xuelei|last17=Yin|first17=Wen|last18=Li|first18=Hui|last19=Liu|first19=Min|last20=Xiao|first20=Yan|last21=Gao|first21=Hong|last22=Guo|first22=Li|last23=Xie|first23=Jungang|last24=Wang|first24=Guangfa|last25=Jiang|first25=Rongmeng|last26=Gao|first26=Zhancheng|last27=Jin|first27=Qi|last28=Wang|first28=Jianwei|last29=Cao|first29=Bin|title=Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China|journal=The Lancet|volume=395|issue=10223|year=2020|pages=497–506|issn=01406736|doi=10.1016/S0140-6736(20)30183-5}}</ref><ref>{{Cite web|url=https://www.cdc.gov/coronavirus/2019-ncov/about/transmission.html|title=|last=|first=|date=|website=|archive-url=|archive-date=|dead-url=|access-date=}}</ref> | ||
*The outbreak was declared a Public Health Emergency of International Concern on 30 January 2020. | *The outbreak was declared a Public Health Emergency of International Concern on 30 January 2020. | ||
*On March 12, | *On March 12. 2020, the World Health Organization declared the COVID-19 outbreak a [[pandemic]]. | ||
== Classification == | |||
There is no established system for the classification of covid-19 induced cutaneous lesions. | |||
== Pathophysiology == | == Pathophysiology == | ||
| Line 31: | Line 40: | ||
*[[IL-1]], [[Interferon|IFN-γ]], and [[TNF-α|TNF]]-α are produced to recruit [[eosinophils]], [[CD8+ T cells|CD8]]+ , [[B cells]] and [[Natural Killer T cell|natural killer]] cells resulting in [[Arteritis|lymphocytic thrombophilic arteritis]]. | *[[IL-1]], [[Interferon|IFN-γ]], and [[TNF-α|TNF]]-α are produced to recruit [[eosinophils]], [[CD8+ T cells|CD8]]+ , [[B cells]] and [[Natural Killer T cell|natural killer]] cells resulting in [[Arteritis|lymphocytic thrombophilic arteritis]]. | ||
*[[Keratinocyte]]<nowiki/>s are destroyed by the [[Cytotoxic T lymphocytes|cytotoxic lymphocytes]] which is secondary to [[Langerhans cell|langherhans]] cell activation resulting in [[vasodilation]] and spongiosis. | *[[Keratinocyte]]<nowiki/>s are destroyed by the [[Cytotoxic T lymphocytes|cytotoxic lymphocytes]] which is secondary to [[Langerhans cell|langherhans]] cell activation resulting in [[vasodilation]] and spongiosis. | ||
*Microvascular injury occurs mediated by activation of complement pathways and an associated | *Microvascular injury occurs mediated by activation of [[Complement|complement pathways]] and an associated procoagulant state. | ||
*The purpuric skin lesions showed a pauci-inflammatory thrombogenic vasculopathy, with deposition of C5b-9 and C4d | *The purpuric skin lesions showed a pauci-inflammatory thrombogenic [[vasculopathy]], with deposition of C5b-9 and C4d | ||
*In addition, there was co-localization of COVID-19 spike glycoproteins with C4d and C5b-9 in the interalveolar septa and the cutaneous microvasculature. | *In addition, there was co-localization of COVID-19 spike [[glycoproteins]] with [[Complement|C4d]] and [[C5|C5b-9]] in the interalveolar septa and the cutaneous microvasculature. | ||
=== Microscopic pathology === | === Microscopic pathology === | ||
| Line 48: | Line 57: | ||
**Dense perivascular lymphocytic infiltration | **Dense perivascular lymphocytic infiltration | ||
**Eosinophilic rich around the swollen blood vessels | **Eosinophilic rich around the swollen blood vessels | ||
**Extravasated erythrocytes. | **Extravasated [[erythrocytes]]. | ||
** Lymphocytic vasculitis. | **[[Vasculitis|Lymphocytic vasculitis]]. | ||
== Causes == | |||
Coronavirus disease 2019 (COVID-19) is caused by [[SARS-CoV-2|severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)]]. | |||
== Differentiating COVID-19 Dermatologic manifestations with other Diseases == | == Differentiating COVID-19 Dermatologic manifestations with other Diseases == | ||
*COVID-19 skin manifestations can often look similar to other diseases that can present with a rash such as [[toxic shock syndrome]], [[meningococcemia]], [[Rickettsial|rickettsial diseases]], [[measles]], and [[scarlet fever]]. | *COVID-19 skin manifestations can often look similar to other diseases that can present with a rash such as [[toxic shock syndrome]], [[meningococcemia]], [[Rickettsial|rickettsial diseases]], [[measles]], and [[scarlet fever]]. | ||
<small> | |||
{| class="wikitable" | |||
|+ | |||
! rowspan="2" style="width: 200px; background: #4479BA; text-align: center;"| {{fontcolor|#FFF|Disease}} | |||
! rowspan="2" style="width: 200px; background: #4479BA; text-align: center;"| {{fontcolor|#FFF|Epidemiology}} | |||
! rowspan="2" style="width: 200px; background: #4479BA; text-align: center;"| {{fontcolor|#FFF|Predisposing factors}} | |||
! colspan="5" style="width: 200px; background: #4479BA; text-align: center;" | {{fontcolor|#FFF|Clinical features}}<ref name="pmid3069202">{{cite journal |vauthors=Todd JK |title=Toxic shock syndrome |journal=Clin. Microbiol. Rev. |volume=1 |issue=4 |pages=432–46 |year=1988 |pmid=3069202 |pmc=358064 |doi= |url=}}</ref><ref name="pmid264839892">{{cite journal |vauthors=Kang JH |title=Febrile Illness with Skin Rashes |journal=Infect Chemother |volume=47 |issue=3 |pages=155–66 |year=2015 |pmid=26483989 |pmc=4607768 |doi=10.3947/ic.2015.47.3.155 |url=}}</ref><ref name="pmid12720556">{{cite journal |vauthors=Sivagnanam S, Deleu D |title=Red man syndrome |journal=Crit Care |volume=7 |issue=2 |pages=119–20 |year=2003 |pmid=12720556 |pmc=270616 |doi= |url=}}</ref> | |||
! rowspan="2" style="width: 200px; background: #4479BA; text-align: center;"| {{fontcolor|#FFF|'''Lab abnormalities'''}} | |||
|- | |||
| colspan="4" style="width: 200px; background: #4479BA; text-align: center;"| {{fontcolor|#FFF|'''Signs'''}} | |||
| style="width: 200px; background: #4479BA; text-align: center;"| {{fontcolor|#FFF|'''Symptoms'''}} | |||
|- | |||
| rowspan="2" text-align: center;"|[[Toxic shock syndrome]] | |||
| rowspan="2" |Occurs in both adults and children (9:1 female predominance) | |||
| rowspan="2" text-align: center;"| | |||
* Occurs in association with [[vaginitis]] during [[menstruation]] following tampon use (S. aureus); | |||
* As a complication of soft tissue infections ([[Streptococcus pyogenes|S. pyogenes]] or GAS) | |||
* In females undergoing medical [[abortion]] | |||
([[Clostridium sordellii|C. sordellii]])<ref name="pmid2801850">{{cite journal |vauthors=McGregor JA, Soper DE, Lovell G, Todd JK |title=Maternal deaths associated with Clostridium sordellii infection |journal=Am. J. Obstet. Gynecol. |volume=161 |issue=4 |pages=987–95 |year=1989 |pmid=2801850 |doi= |url=}}</ref><ref name="pmid16049422">{{cite journal |vauthors= |title=Clostridium sordellii toxic shock syndrome after medical abortion with mifepristone and intravaginal misoprostol--United States and Canada, 2001-2005 |journal=MMWR Morb. Mortal. Wkly. Rep. |volume=54 |issue=29 |pages=724 |year=2005 |pmid=16049422 |doi= |url=}}</ref><ref name="pmid16319384">{{cite journal |vauthors=Fischer M, Bhatnagar J, Guarner J, Reagan S, Hacker JK, Van Meter SH, Poukens V, Whiteman DB, Iton A, Cheung M, Dassey DE, Shieh WJ, Zaki SR |title=Fatal toxic shock syndrome associated with Clostridium sordellii after medical abortion |journal=N. Engl. J. Med. |volume=353 |issue=22 |pages=2352–60 |year=2005 |pmid=16319384 |doi=10.1056/NEJMoa051620 |url=}}</ref><ref name="pmid12439811">{{cite journal |vauthors=Sinave C, Le Templier G, Blouin D, Léveillé F, Deland E |title=Toxic shock syndrome due to Clostridium sordellii: a dramatic postpartum and postabortion disease |journal=Clin. Infect. Dis. |volume=35 |issue=11 |pages=1441–3 |year=2002 |pmid=12439811 |doi=10.1086/344464 |url=}}</ref><ref name="pmid19628200">{{cite journal |vauthors=Ho CS, Bhatnagar J, Cohen AL, Hacker JK, Zane SB, Reagan S, Fischer M, Shieh WJ, Guarner J, Ahmad S, Zaki SR, McDonald LC |title=Undiagnosed cases of fatal Clostridium-associated toxic shock in Californian women of childbearing age |journal=Am. J. Obstet. Gynecol. |volume=201 |issue=5 |pages=459.e1–7 |year=2009 |pmid=19628200 |doi=10.1016/j.ajog.2009.05.023 |url=}}</ref> | |||
| text-align: center;"| '''[[Fever]]''' | |||
| text-align: center;"| '''[[Hypotension]]''' | |||
| text-align: center;"| '''Diffuse [[Rash]]''' | |||
| text-align: center;" | '''Other signs''' | |||
| rowspan="2" text-align: center;"| | |||
* Diarrhea | |||
* Vomiting | |||
* Rash: '''Diffuse scarlantiform rash (red sunburn-like rash. It is flat and turns white if pressed)''' | |||
* '''Thick skin desquamation appears on the hands and feet at around 1-2 weeks of disease progression, and might be followed by hair desquamation or shedding of fingernails and toenails after 2-3 months'''<ref name="pmid26483989">{{cite journal |vauthors=Kang JH |title=Febrile Illness with Skin Rashes |journal=Infect Chemother |volume=47 |issue=3 |pages=155–66 |year=2015 |pmid=26483989 |pmc=4607768 |doi=10.3947/ic.2015.47.3.155 |url=}}</ref> | |||
| rowspan="2" | | |||
* [[Hyponatremia]]<ref name="pmid3256819">{{cite journal |vauthors=Brook MG, Bannister BA |title=Scarlet fever can mimic toxic shock syndrome |journal=Postgrad Med J |volume=64 |issue=758 |pages=965–7 |year=1988 |pmid=3256819 |pmc=2429080 |doi= |url=}}</ref> | |||
* [[Uremia]] | |||
* Hepatic dysfunction (total [[bilirubin]], serum asparate aminotransferase or serum alanine aminotransferase levels >2 times upper normal limit)<ref name="pmid25276279">{{cite journal |vauthors=Minemura M, Tajiri K, Shimizu Y |title=Liver involvement in systemic infection |journal=World J Hepatol |volume=6 |issue=9 |pages=632–42 |year=2014 |pmid=25276279 |pmc=4179142 |doi=10.4254/wjh.v6.i9.632 |url=}}</ref> | |||
* [[Leukocytosis]] with a [[Polymorphonuclear cells|polymorphonuclear shift]] to the left | |||
* [[Platelet|Platelets]] < 100,000 per mm<sup>3</sup>([[thrombocytopenia]]) | |||
* [[Pyuria]] of [[renal]] origin.<ref name="pmid7282746">{{cite journal |vauthors=Chesney RW, Chesney PJ, Davis JP, Segar WE |title=Renal manifestations of the staphylococcal toxic-shock syndrome |journal=Am. J. Med. |volume=71 |issue=4 |pages=583–8 |year=1981 |pmid=7282746 |doi= |url=}}</ref> | |||
|- | |||
| + | |||
| + | |||
| + | |||
| | |||
* Nonpitting systemic [[edema]] | |||
* [[Tachycardia]] | |||
* [[Mucous membrane]] [[Hyperaemia|hyperemia]] (vaginal, oral, [[Conjunctiva|conjunctival]]) | |||
|- | |||
|[[Meningococcemia]] | |||
|Occurs in young adults living in close proximity (college dorms, military recruits)<ref name="pmid20144015">{{cite journal |vauthors=Harrison LH |title=Epidemiological profile of meningococcal disease in the United States |journal=Clin. Infect. Dis. |volume=50 Suppl 2 |issue= |pages=S37–44 |year=2010 |pmid=20144015 |pmc=2820831 |doi=10.1086/648963 |url=}}</ref> | |||
| | |||
* Close contact with a carrier | |||
* Intimate kissing and cigarette smoking are associated with increased risk of meningococcal carriage<ref name="pmid16707051">{{cite journal |vauthors=MacLennan J, Kafatos G, Neal K, Andrews N, Cameron JC, Roberts R, Evans MR, Cann K, Baxter DN, Maiden MC, Stuart JM |title=Social behavior and meningococcal carriage in British teenagers |journal=Emerging Infect. Dis. |volume=12 |issue=6 |pages=950–7 |year=2006 |pmid=16707051 |pmc=3373034 |doi= |url=}}</ref> | |||
| + | |||
| + | |||
| + | |||
| | |||
* Positive [[Kernig's sign]] | |||
* Positive [[Brudzinski's sign]]<ref name="pmid14779273">{{cite journal |vauthors=WARTENBERG R |title=The signs of Brudzinski and of Kernig |journal=J. Pediatr. |volume=37 |issue=4 |pages=679–84 |year=1950 |pmid=14779273 |doi= |url=}}</ref> | |||
* [[Photophobia]]<ref name="pmid25470712">{{cite journal |vauthors=Bush LM |title=Case 28-2014: A man with a rash, headache, fever, nausea, and photophobia |journal=N. Engl. J. Med. |volume=371 |issue=23 |pages=2238–9 |year=2014 |pmid=25470712 |doi=10.1056/NEJMc1412237#SA2 |url=}}</ref> | |||
| | |||
* [[Vomiting]] | |||
* [[Nausea]] | |||
* [[Headache]] | |||
* Cool extremities | |||
* [[Seizure|Seizures]] | |||
* Rash: [[petechiae]] and [[purpura]] ('''star-shaped rash, which can develop into purple bruising. [[Meningococcal]] rash can usually be confirmed by a glass test in which the rash does not fade away under pressure'''.<ref name="urlMeningitis Symptoms - Meningitis Research Foundation">{{cite web |url=http://www.meningitis.org/symptoms |title=Meningitis Symptoms - Meningitis Research Foundation |format= |work= |accessdate=}}</ref> | |||
| | |||
* Positive blood cultures ([[Neisseria meningitidis]]) | |||
* CSF findings typical of bacterial meningitis:[[Bacterial meningitis differential diagnosis|[24]]] | |||
** Cells '''>300/uL''' | |||
** Predominantly granulocytes | |||
** Total protein 100-500mg/dl | |||
** Glucose ratio (CSF/plasma) <0.3 | |||
** Lactate >2.1 mmol/L | |||
** CSF gram stain and culture may be positive | |||
|- | |||
|[[Stevens-Johnson syndrome|Stevens Johnson syndrome]] ([[Stevens-Johnson syndrome|SJS]]) | |||
|[[HLA-B]]*1502 [[gene]] leads to increased susceptibility<ref name="pmid15057820">{{cite journal |vauthors=Chung WH, Hung SI, Hong HS, Hsih MS, Yang LC, Ho HC, Wu JY, Chen YT |title=Medical genetics: a marker for Stevens-Johnson syndrome |journal=Nature |volume=428 |issue=6982 |pages=486 |year=2004 |pmid=15057820 |doi=10.1038/428486a |url=}}</ref> | |||
|Triggered by certain medications, most commonly: | |||
* [[Anticonvulsant|Anticonvulsants]] | |||
* [[Non-steroidal anti-inflammatory drug|Non-steroidal anti-inflammatory drugs]] | |||
* [[Antibiotic|Antibiotics]]<ref name="pmid27650525">{{cite journal |vauthors=Techasatian L, Panombualert S, Uppala R, Jetsrisuparb C |title=Drug-induced Stevens-Johnson syndrome and toxic epidermal necrolysis in children: 20 years study in a tertiary care hospital |journal=World J Pediatr |volume= |issue= |pages= |year=2016 |pmid=27650525 |doi=10.1007/s12519-016-0057-3 |url=}}</ref> | |||
* [[Mycoplasma pneumoniae]] | |||
* [[Herpes simplex virus]]<ref name="pmid211627212">{{cite journal |vauthors=Harr T, French LE |title=Toxic epidermal necrolysis and Stevens-Johnson syndrome |journal=Orphanet J Rare Dis |volume=5 |issue= |pages=39 |year=2010 |pmid=21162721 |pmc=3018455 |doi=10.1186/1750-1172-5-39 |url=}}</ref> | |||
| + | |||
| + | |||
| + | |||
| | |||
* Positive Nikolsky sign (exerting mechanical pressure on several [[erythematous]] zones resluts in peeling of skin) | |||
* Skin [[Macule|macules]] which rapidly [[Coalescence (chemistry)|coalescence]].<ref name="pmid211627213">{{cite journal |vauthors=Harr T, French LE |title=Toxic epidermal necrolysis and Stevens-Johnson syndrome |journal=Orphanet J Rare Dis |volume=5 |issue= |pages=39 |year=2010 |pmid=21162721 |pmc=3018455 |doi=10.1186/1750-1172-5-39 |url=}}</ref> | |||
| | |||
* [[Ocular]] involvement: eyelid [[edema]], [[erythema]], crusts, and ocular [[discharge]], to [[Conjunctival|conjunctival membrane]] or pseduomembrane formation or [[Cornea|corneal]] erosion<ref name="pmid17251797">{{cite journal |vauthors=Chang YS, Huang FC, Tseng SH, Hsu CK, Ho CL, Sheu HM |title=Erythema multiforme, Stevens-Johnson syndrome, and toxic epidermal necrolysis: acute ocular manifestations, causes, and management |journal=Cornea |volume=26 |issue=2 |pages=123–9 |year=2007 |pmid=17251797 |doi=10.1097/ICO.0b013e31802eb264 |url=}}</ref> | |||
* Rash: '''[[Purpura|Purpuric]] [[Macule|macules]] and targetoid lesions; full-thickness [[epidermal]] [[necrosis]],''' '''presenting as [[Blister|blisters]] and areas of denuded skin; and [[mucous membrane]] involvement'''<ref name="pmid21162721">{{cite journal |vauthors=Harr T, French LE |title=Toxic epidermal necrolysis and Stevens-Johnson syndrome |journal=Orphanet J Rare Dis |volume=5 |issue= |pages=39 |year=2010 |pmid=21162721 |pmc=3018455 |doi=10.1186/1750-1172-5-39 |url=}}</ref> | |||
| | |||
* Serum levels of the following are typically elevated in patients with [[Stevens-Johnson syndrome]]: | |||
** [[Tumor necrosis factor-alpha|Tumor necrosis factor (TNF)-alpha]] | |||
** Soluble [[interleukin 2]]-receptor | |||
** [[Interleukin 6]] | |||
** [[C-reactive protein]] | |||
* Histological work up of skin sections reveal widespread [[Necrosis|necrotic]] [[Epidermis (skin)|epidermis]] involving all layers | |||
|- | |||
|[[DRESS syndrome|Drug Reaction with Eosinophilia and Systemic Symptoms]] ([[DRESS syndrome|DRESS]]) Syndrome | |||
| | |||
| | |||
* [[Human herpes virus 6|HHV-6]]<ref name="pmid23882307">{{cite journal |vauthors=Choudhary S, McLeod M, Torchia D, Romanelli P |title=Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) Syndrome |journal=J Clin Aesthet Dermatol |volume=6 |issue=6 |pages=31–7 |year=2013 |pmid=23882307 |pmc=3718748 |doi= |url=}}</ref> | |||
* [[Carbamazepine]] | |||
* [[Minocycline]] | |||
* [[Allopurinol]] | |||
* [[Abacavir]] | |||
* [[Nevirapine]] | |||
* [[Clindamycin]] | |||
| + | |||
| + | |||
| + | |||
| | |||
* Multi-organ dysfunction:<ref name="pmid19153346">{{cite journal |vauthors=Eshki M, Allanore L, Musette P, Milpied B, Grange A, Guillaume JC, Chosidow O, Guillot I, Paradis V, Joly P, Crickx B, Ranger-Rogez S, Descamps V |title=Twelve-year analysis of severe cases of drug reaction with eosinophilia and systemic symptoms: a cause of unpredictable multiorgan failure |journal=Arch Dermatol |volume=145 |issue=1 |pages=67–72 |year=2009 |pmid=19153346 |doi=10.1001/archderm.145.1.67 |url=}}</ref> | |||
** Pneumonitis | |||
** Hepatitis | |||
** Renal failure | |||
** Encephalitis | |||
** Cardiac failure | |||
* [[Hemophagocytosis]] | |||
| | |||
* [[Lymphadenopathy]] | |||
* Rash: '''[[Urticaria|Urticarial]], [[maculopapular]] eruption and, in some instances, [[Vesicle|vesicles]], bullae, [[pustules]], [[purpura]], target lesions, [[facial edema]], [[cheilitis]], and [[erythroderma]]'''<ref name="pmid16882184">{{cite journal |vauthors=Peyrière H, Dereure O, Breton H, Demoly P, Cociglio M, Blayac JP, Hillaire-Buys D |title=Variability in the clinical pattern of cutaneous side-effects of drugs with systemic symptoms: does a DRESS syndrome really exist? |journal=Br. J. Dermatol. |volume=155 |issue=2 |pages=422–8 |year=2006 |pmid=16882184 |doi=10.1111/j.1365-2133.2006.07284.x |url=}}</ref> | |||
| | |||
* [[Eosinophilia]] | |||
* [[Leukocytosis]] | |||
* [[Uremia]] | |||
* Increased [[ALT]] and [[Aspartate transaminase|AST]]<ref name="pmid191533462">{{cite journal |vauthors=Eshki M, Allanore L, Musette P, Milpied B, Grange A, Guillaume JC, Chosidow O, Guillot I, Paradis V, Joly P, Crickx B, Ranger-Rogez S, Descamps V |title=Twelve-year analysis of severe cases of drug reaction with eosinophilia and systemic symptoms: a cause of unpredictable multiorgan failure |journal=Arch Dermatol |volume=145 |issue=1 |pages=67–72 |year=2009 |pmid=19153346 |doi=10.1001/archderm.145.1.67 |url=}}</ref> | |||
|- | |||
|[[Red man syndrome]] | |||
|Patients in whom the offending drug infusion is given over less than 1 hour and who are not pre-treated with [[diphenhydramine]]<ref name="pmid1955716">{{cite journal |vauthors=Wallace MR, Mascola JR, Oldfield EC |title=Red man syndrome: incidence, etiology, and prophylaxis |journal=J. Infect. Dis. |volume=164 |issue=6 |pages=1180–5 |year=1991 |pmid=1955716 |doi= |url=}}</ref> | |||
|Hypersensitivity to:<ref name="pmid127205562">{{cite journal |vauthors=Sivagnanam S, Deleu D |title=Red man syndrome |journal=Crit Care |volume=7 |issue=2 |pages=119–20 |year=2003 |pmid=12720556 |pmc=270616 |doi= |url=}}</ref> | |||
* [[Vancomycin]] | |||
* [[Ciprofloxacin]] | |||
* [[Amphotericin B]] | |||
* [[Rifampin|Rifampicin]] | |||
* [[Teicoplanin]] | |||
* [[Cefepime]] | |||
| + | |||
| + | |||
| + | |||
| | |||
* Local infusion site [[erythema]] | |||
* [[Angioedema]] (rare) | |||
| | |||
* [[Headache]] | |||
* Chills | |||
* [[Dizziness]] | |||
* [[Chest pain]] | |||
* [[Dyspnea]] | |||
* [[Pruritis]] | |||
* Rash: '''An [[erythematous]] rash that involves the face, neck, and upper [[torso]]''' | |||
|No elevation in tryptase levels indicating that it is an anaphylactoid reaction<ref name="pmid9743397">{{cite journal |vauthors=Renz CL, Laroche D, Thurn JD, Finn HA, Lynch JP, Thisted R, Moss J |title=Tryptase levels are not increased during vancomycin-induced anaphylactoid reactions |journal=Anesthesiology |volume=89 |issue=3 |pages=620–5 |year=1998 |pmid=9743397 |doi= |url=}}</ref> | |||
|- | |||
|[[Kawasaki disease|Kawasaki]] | |||
[[Kawasaki disease|disease]] | |||
|Occurs in children, usually age 1-4 years | |||
| | |||
* Interaction of [[genetic]] and environmental factors | |||
* Infection in combination with [[genetic predisposition]] to an [[autoimmune]] mechanism | |||
([[Vasculitis|autoimmune vasculitis]]) | |||
| + | |||
| + | |||
| + | |||
| | |||
* Non-[[suppurative]], painless bilateral conjunctival [[inflammation]] ([[conjunctivitis]]) | |||
* Strawberry tongue (marked redness with prominent [[Papillae of the tongue|gustative papillae]]), | |||
* Deep transverse grooves across the nails may develop (Beau’s lines), | |||
* [[lymphadenopathy]] present(acute, non-[[purulent]], cervical), | |||
* [[Coronary arteries|Coronary artery]] [[Aneurysm|aneurysms]]. | |||
| | |||
* High and persistent fever that is not very responsive to normal treatment with [[acetaminophen]] or [[Non-steroidal anti-inflammatory drug|NSAIDs]], | |||
* Rash: '''diffuse [[Maculopapular|macular-papular]] [[erythematous]] rash''' | |||
| | |||
* Liver function tests may show evidence of hepatic [[inflammation]] and low serum [[albumin]] levels | |||
* Low hemoglobulin and age-adjusted hemoglobulin concentrations | |||
* '''[[thrombocytosis]]''' | |||
* [[anemia]]. | |||
* [[Echocardiography|Echocardiographic]] abnormalities, such as [[valvulitis]] ([[Mitral valve|mitral]] or [[Tricuspid valve|tricuspid]] [[Regurgitation (circulation)|regurgitation]]) and [[Coronary arteries|coronary artery]] lesions, are significantly more common in [[Kawasaki disease]]<ref name="pmid26222065">{{cite journal |vauthors=Lin YJ, Cheng MC, Lo MH, Chien SJ |title=Early Differentiation of Kawasaki Disease Shock Syndrome and Toxic Shock Syndrome in a Pediatric Intensive Care Unit |journal=Pediatr. Infect. Dis. J. |volume=34 |issue=11 |pages=1163–7 |year=2015 |pmid=26222065 |doi=10.1097/INF.0000000000000852 |url=}}</ref> | |||
* [[Pyuria]] of uretheral origin. | |||
|- | |||
|[[Scarlet fever]] | |||
|Distributed equally among both genders. Most commonly affects children between five and fifteen years of age. | |||
|Occurs after streptococcal [[pharyngitis]]/[[tonsillitis]] | |||
| + | |||
|<nowiki>+/-</nowiki> | |||
| + | |||
| | |||
* Pastia's sign (puncta and skin crease accentuation of the [[erythema]]) | |||
* Strawberry tongue | |||
* Cervical [[lymphadenopathy]] may be present. | |||
* [[Scarlet fever]] appears similar to [[Kawasaki disease|Kawasaki's disease]] in some aspects, but lacks the eye signs or the swollen, red fingers and toes | |||
|Rash''':''' | |||
* '''Characteristic sandpaper-like rash which appears days after the illness begins (although the rash can appear before illness or up to 7 days later), rash may first appear on the neck, underarm, and groin''' | |||
| | |||
* [[Leukocytosis]] with [[left shift]] and possibly [[eosinophilia]] a few weeks after convalescence. | |||
* Anti-deoxyribonuclease B antibody positive | |||
* [[Antistreptolysin O titer|Antistreptolysin-O]] titers (antibodies to streptococcal [[extracellular]] products) | |||
* Antihyaluronidase, and antifibrinolysin may be positive. | |||
|}For differentiating diseases presenting with [[rash]] and [[fever]] click [[Measles differential diagnosis|here]].</small> | |||
== Epidemiology and Demographics == | == Epidemiology and Demographics == | ||
| Line 71: | Line 289: | ||
**Individuals in long term care facilities | **Individuals in long term care facilities | ||
==History and Symptoms == | == Screening == | ||
There is insufficient evidence to recommend routine for cutaneous manifestations related to covid-19. | |||
== Natural History, Complications and Prognosis == | |||
* The skin lesions are initially reddish and papular resembling chilblains. | |||
* Subsequently, in the span of approximately 1 week they become more purpuric and flattened. | |||
* Finally, they seem to resolve by themselves without requiring any treatment. | |||
* Aggravation of previous skin diseases, such as [[rosacea]], [[eczema]], [[atopic dermatitis]] and [[neurodermatitis]], was also observed in some Covid‐19 patients. | |||
== Diagnosis == | |||
=== Diagnostic studies === | |||
* Diagnosis of COVID-19 infection was successfully confirmed by [[RT-PCR]]. | |||
* Histopathological studies and [[PCR]] investigation on skin [[Biopsy|biopsies]] are necessary to confirm infection of skin with SARS-CoV-2 infection. | |||
=== History === | |||
*History of [[Patient|patients]] [[Infection|infected]] with Coronavirus disease 2019 (COVID-19) can include international travel to where COVID-19 is highly [[Prevalence|prevalent]]. | |||
*History should also be focused on the possible exposure to a confirmed COVID-19 [[patient]]. | |||
===Symptoms === | |||
* The timing of skin lesions depends on various factors and not really known but 3 days before diagnosis to 13 days after diagnosis. | * The timing of skin lesions depends on various factors and not really known but 3 days before diagnosis to 13 days after diagnosis. | ||
*The most common cutaneous manifestation of COVID-19 is a maculopapular exanthem (morbilliform). | *The most common cutaneous manifestation of COVID-19 is a maculopapular exanthem (morbilliform). | ||
*Majority of lesions were localized on the trunk, however, some patients experienced cutaneous manifestations in the hands and feet. | * The Majority of lesions were localized on the trunk, however, some patients experienced cutaneous manifestations in the hands and feet. | ||
*Skin lesion development occurred before the onset of respiratory symptoms or COVID-19 diagnosis in some of the patients , and lesions spontaneously healed in all patients within 10 days | *Skin lesion development occurred before the onset of respiratory symptoms or COVID-19 diagnosis in some of the patients, and lesions spontaneously healed in all patients within 10 days | ||
* The other cutaneous manifestations | * The other cutaneous manifestations include: | ||
**Morbilliform rash | **Morbilliform rash | ||
**[[Urticaria]] | **[[Urticaria]] | ||
| Line 82: | Line 323: | ||
**Petechial skin rash | **Petechial skin rash | ||
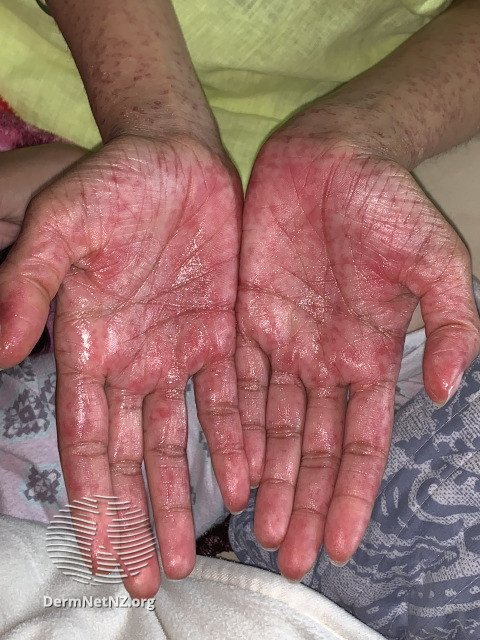
== Physical Examination == | [[File:Covid-5.jpeg|center|thumb|267x267px|Suspected COVID-19 rash Courtesy: Images in accordance with the licensing requirements of Creative Commons Attribution-NonCommercial-NoDerivs 3.0 (New Zealand).]] | ||
<br /> | |||
=== Physical Examination === | |||
*Acral eruption of erythemato‐violaceous [[papules]] and [[macules]], with possible bullous evolution, or [[Clubbing|digital swelling]]. | |||
*Acute acro-ischemia in the child | |||
**Presentations of acro-ischemia including [[finger]]/toe [[cyanosis]], [[Bulla ethmoidalis|skin bulla]], and [[Gangrene|dry gangrene]]. | |||
**Expression of secondary micro thrombosis due to [[Endothelium|endothelial damage]] and vascular disorders. | |||
*[[Erythema multiforme]]-like lesions that might be another pattern of [[exanthem]] associated with COVID-19 infection. | |||
*Further studies are needed to evaluate whether these lesions are associated with the virus, the drug intake or any other conditions. | |||
*COVID-19 Toes. | |||
**Similar to the type of cold related changes we have seen in the feet of people for many years, but often occurring in places where the conditions are not cold and damp. | |||
**These seem to happen more commonly in younger patients. | |||
*Chilblain‐like lesions | |||
**The pseudo‐chilblain pattern frequently appears late in the evolution of the COVID‐19 disease. | |||
**The lesion was red–purple papules on the dorsal aspect of the fingers on both hands and diffused erythema in the subungual area of thumb. | |||
=== Laboratory Findings === | |||
*[[D-dimer]], [[fibrinogen]], and [[Fibrinogen|fibrinogen degradation product]] (FDP) were significantly elevated in most patients. | |||
*D-dimer, fibrinogen, and fibrinogen degradation product (FDP) were significantly elevated in most patients. | *[[Prothrombin time]] was prolonged in 4 patients. D-dimer and FDP levels progressively elevated consistent with COVID-2019 exacerbation. | ||
*Prothrombin time was prolonged in 4 patients. D-dimer and FDP levels progressively elevated consistent with COVID-2019 exacerbation. | *[[Disseminated intravascular coagulation]]. | ||
* | *HSV is suspected of provoking stimulation of immunopathological mechanisms in [[erythema multiforme]]. | ||
**The herpes virus could play a role in [[Cross-reactivity|autoimmune cross-reactivity]], triggering the [[keratinocyte]] that activates [[IL-1]], [[Interferon|IFN-γ]], and [[TNF-α]], recruiting [[cytotoxic]] and [[NK cells]] that target the keratinocytes itself. | |||
*HSV is suspected of provoking stimulation of immunopathological mechanisms in erythema multiforme. | |||
**The herpes virus could play a role in autoimmune cross-reactivity, triggering the keratinocyte that activates IL-1, IFN-γ, and TNF-α, recruiting cytotoxic and NK cells that target the keratinocytes itself. | |||
== | === Electrocardiogram === | ||
There are no ECG findings associated with covid-19 rash. | |||
== | === X-ray === | ||
There are no x-ray findings associated with covid-19 rash. | |||
=== Echocardiography or Ultrasound === | |||
There are no echocardiography/ultrasound findings associated with covid-19 rash. | |||
=== CT scan === | |||
There are no CT scan findings associated with covid-19 rash. | |||
=== MRI === | |||
There are no MRI findings associated with covid-19 rash.. | |||
=== Other Imaging Findings === | |||
There are no other imaging findings associated with covid-19 rash.. | |||
== Treatment == | == Treatment == | ||
| Line 121: | Line 372: | ||
* Currently, infection prevention and control are considered urgent and critical due to the lack of specific treatment and heightened risk of spreading during the incubation period. | * Currently, infection prevention and control are considered urgent and critical due to the lack of specific treatment and heightened risk of spreading during the incubation period. | ||
===Primary Prevention=== | |||
* | |||
* Effective measures for the [[primary prevention]] of COVID-19 include:<ref name="urlHow to Protect Yourself & Others | CDC">{{cite web |url=https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/prevention.html |title=How to Protect Yourself & Others | CDC |format= |work= |accessdate=}}</ref> | |||
**Frequent handwashing with soap and water for at least 20 seconds or using a [[Alcohol rub|alcohol based hand sanitizer]] with at least 60% alcohol | |||
**Staying at least 6 feet (about 2 arms’ length) from other people who do not live with you | |||
**Covering your mouth and nose with a cloth face cover when around others and covering sneezes and coughs | |||
**Cleaning and [[disinfect]]ing | |||
*There have been rigorous efforts in order to develop a [[vaccine]] for [[COVID-10|novel coronavirus]] and several vaccines are in the later phases of trials.<ref name="urlNIH clinical trial of investigational vaccine for COVID-19 begins | National Institutes of Health (NIH)">{{cite web |url=https://www.nih.gov/news-events/news-releases/nih-clinical-trial-investigational-vaccine-covid-19-begins |title=NIH clinical trial of investigational vaccine for COVID-19 begins | National Institutes of Health (NIH) |format= |work= |accessdate=}}</ref> | |||
===Secondary prevention=== | |||
*Effective measures for the [[secondary prevention]] of COVID-19 include: | |||
**Use of [[personal protective equipment]] (PPE) by the personnel handling the fecal matter. | |||
**Screening of fecal [[Microbiome|microbiota]] [[transplant]] donors for [[COVID-19]] is also recommended.<ref name="pmid32240618">{{cite journal |vauthors=Green CA, Quraishi MN, Shabir S, Sharma N, Hansen R, Gaya DR, Hart AL, Loman NJ, Iqbal TH |title=Screening faecal microbiota transplant donors for SARS-CoV-2 by molecular testing of stool is the safest way forward |journal=Lancet Gastroenterol Hepatol |volume=5 |issue=6 |pages=531 |date=June 2020 |pmid=32240618 |pmc=7225406 |doi=10.1016/S2468-1253(20)30089-3 |url=}}</ref> | |||
**[[Contact tracing]] helps reduce the spread of the disease.<ref name="urlContact Tracing for COVID-19 | CDC">{{cite web |url=https://www.cdc.gov/coronavirus/2019-ncov/php/contact-tracing/contact-tracing-plan/contact-tracing.html |title=Contact Tracing for COVID-19 | CDC |format= |work= |accessdate=}}</ref> | |||
<br /> | <br /> | ||
* | * | ||
Latest revision as of 15:21, 2 November 2021
|
COVID-19 Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
COVID-19-associated dermatologic manifestations On the Web |
|
American Roentgen Ray Society Images of COVID-19-associated dermatologic manifestations |
|
Risk calculators and risk factors for COVID-19-associated dermatologic manifestations |
For COVID-19 frequently asked inpatient questions, click here
For COVID-19 frequently asked outpatient questions, click here
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Nuha Al-Howthi, MD[2] Ogechukwu Hannah Nnabude, MD; Aditya Ganti M.B.B.S. [3]
Synonyms and keywords: COVID-19-associated exanthematous rash; COVID-19-associated livedo reticularis; COVID-19-associated livedoid lesions; COVID-19-associated multisystem inflammatory syndrome in children; COVID-19-associated retiform purpura; COVID-19-associated urticaria; COVID-19-associated vasculitis; COVID-19-associated vesicular eruptions
Overview
COVID-19 infections is caused by the novel coronavirus or also known as SARS-2 virus. The disease is believed to incline towards respiratory organs due to the high expression of ACE receptors. However, skin rashes have been uncommonly described in patients with COVID-19 infection. Dermatologic manifestations of COVID-19 though rare include an erythematous exanthem, livedo reticularis, vasculitis, urticaria, vesicles. Common clinical features of covid-19 infection includes fever, dry cough, shortness of breath, myalgia and fatigue.
Historical Perspective
- In 1937, coronavirus was first isolated from chickens.
- In 1965, Tyrrell and Bynoe used cultures of human ciliated embryonal trachea to propagate the first human coronavirus (HCoV) in vitro.
- The etiological agent, a novel coronavirus, SARS-CoV-2, is a virus identified as the cause of an outbreak of respiratory illness first detected in Wuhan, China.[1][2][3][4]
- The outbreak was declared a Public Health Emergency of International Concern on 30 January 2020.
- On March 12. 2020, the World Health Organization declared the COVID-19 outbreak a pandemic.
Classification
There is no established system for the classification of covid-19 induced cutaneous lesions.
Pathophysiology
- The exact mechanisms of COVID-19 induced cutaneous manifestations are not yet well known.
- Transmission of COVID-19 takes place during the prodromal period when those infected are mildly ill and are carrying on with their usual activities.[5][6]
- The virus infects epithelial cells of the lung alveoli by receptor‐mediated endocytosis via the angiotensin‐converting enzyme II (ACE-II) as an entry receptor.[7][8][9]
- ACE-II receptors's presence in the extrapulmonary tissues (heart, kidney, endothelium, and intestine) could explain the multi-organ dysfunction.[10][11][12][13][14][15][16][17]
- Following transmission, the novel coronavirus spreads hematogenously to invade the cutaneous tissue.
- This spread is believed to activate the immune system with mobilization of lymphocytes and langerhans cells resulting in immune complex depositions.
Immune Response
- Immune complexes deposition stimulate T-helper cells to initiate cytokines cascade.
- IL-1, IFN-γ, and TNF-α are produced to recruit eosinophils, CD8+ , B cells and natural killer cells resulting in lymphocytic thrombophilic arteritis.
- Keratinocytes are destroyed by the cytotoxic lymphocytes which is secondary to langherhans cell activation resulting in vasodilation and spongiosis.
- Microvascular injury occurs mediated by activation of complement pathways and an associated procoagulant state.
- The purpuric skin lesions showed a pauci-inflammatory thrombogenic vasculopathy, with deposition of C5b-9 and C4d
- In addition, there was co-localization of COVID-19 spike glycoproteins with C4d and C5b-9 in the interalveolar septa and the cutaneous microvasculature.
Microscopic pathology
- Histopathological studies and PCR investigation on skin biopsies are necessary to clarify the close relationship between skin and SARS-CoV-2 infection. On microscopy features
- Classic dyskeratotic cells
- Ballooning multinucleated cells
- Sparse necrotic keratinocytes
- Lymphocytic satellitosis.
- Punch biopsy of the upper dermis demonstrated
- Diffuse telangiectatic small blood vessels
- Nests of Langerhans cells within the epidermis
- Perivascular spongiotic dermatitis with exocytosis al
- Dense perivascular lymphocytic infiltration
- Eosinophilic rich around the swollen blood vessels
- Extravasated erythrocytes.
- Lymphocytic vasculitis.
Causes
Coronavirus disease 2019 (COVID-19) is caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
Differentiating COVID-19 Dermatologic manifestations with other Diseases
- COVID-19 skin manifestations can often look similar to other diseases that can present with a rash such as toxic shock syndrome, meningococcemia, rickettsial diseases, measles, and scarlet fever.
| Disease | Epidemiology | Predisposing factors | Clinical features[18][19][20] | Lab abnormalities | ||||
|---|---|---|---|---|---|---|---|---|
| Signs | Symptoms | |||||||
| Toxic shock syndrome | Occurs in both adults and children (9:1 female predominance) |
|
Fever | Hypotension | Diffuse Rash | Other signs |
|
|
| + | + | + |
| |||||
| Meningococcemia | Occurs in young adults living in close proximity (college dorms, military recruits)[30] |
|
+ | + | + |
|
| |
| Stevens Johnson syndrome (SJS) | HLA-B*1502 gene leads to increased susceptibility[35] | Triggered by certain medications, most commonly: | + | + | + |
|
| |
| Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) Syndrome | + | + | + |
|
|
| ||
| Red man syndrome | Patients in whom the offending drug infusion is given over less than 1 hour and who are not pre-treated with diphenhydramine[45] | Hypersensitivity to:[46] | + | + | + |
|
|
No elevation in tryptase levels indicating that it is an anaphylactoid reaction[47] |
| Kawasaki | Occurs in children, usually age 1-4 years |
|
+ | + | + |
|
|
|
| Scarlet fever | Distributed equally among both genders. Most commonly affects children between five and fifteen years of age. | Occurs after streptococcal pharyngitis/tonsillitis | + | +/- | + |
|
Rash:
|
|
For differentiating diseases presenting with rash and fever click here.
Epidemiology and Demographics
- The incidence of dermatologic manifestations with COVID-19 infections increases with age; the median age at diagnosis is 53 years.
- Males are more commonly affected than females.
- Most of the patients were children (median 13 years) and young adults (median 31, average 36, range 18–91 years old).
Risk Factors
There are no established risk factors to determine what conditions or diseases predispose Covid-19 infection to manifest as cutaneous complications. However, similar to all viral illnesses, exposure is considered the most significant risk factor for infection with Coronavirus disease 2019 (COVID-19).
- CDC has proposed the following list of conditions that may increase the risk of a severe disease regardless of the individual's age:[49][50][51][52][53][54][55][56]
- Elderly (those aged 60+)
- Cardiovascular disease patients
- Diabetics
- Chronic respiratory disease patients
- Hypertensive patients
- Cancer patients
- Individuals in long term care facilities
Screening
There is insufficient evidence to recommend routine for cutaneous manifestations related to covid-19.
Natural History, Complications and Prognosis
- The skin lesions are initially reddish and papular resembling chilblains.
- Subsequently, in the span of approximately 1 week they become more purpuric and flattened.
- Finally, they seem to resolve by themselves without requiring any treatment.
- Aggravation of previous skin diseases, such as rosacea, eczema, atopic dermatitis and neurodermatitis, was also observed in some Covid‐19 patients.
Diagnosis
Diagnostic studies
- Diagnosis of COVID-19 infection was successfully confirmed by RT-PCR.
- Histopathological studies and PCR investigation on skin biopsies are necessary to confirm infection of skin with SARS-CoV-2 infection.
History
- History of patients infected with Coronavirus disease 2019 (COVID-19) can include international travel to where COVID-19 is highly prevalent.
- History should also be focused on the possible exposure to a confirmed COVID-19 patient.
Symptoms
- The timing of skin lesions depends on various factors and not really known but 3 days before diagnosis to 13 days after diagnosis.
- The most common cutaneous manifestation of COVID-19 is a maculopapular exanthem (morbilliform).
- The Majority of lesions were localized on the trunk, however, some patients experienced cutaneous manifestations in the hands and feet.
- Skin lesion development occurred before the onset of respiratory symptoms or COVID-19 diagnosis in some of the patients, and lesions spontaneously healed in all patients within 10 days
- The other cutaneous manifestations include:
- Morbilliform rash
- Urticaria
- Livedo reticularis
- Petechial skin rash
Physical Examination
- Acral eruption of erythemato‐violaceous papules and macules, with possible bullous evolution, or digital swelling.
- Acute acro-ischemia in the child
- Presentations of acro-ischemia including finger/toe cyanosis, skin bulla, and dry gangrene.
- Expression of secondary micro thrombosis due to endothelial damage and vascular disorders.
- Erythema multiforme-like lesions that might be another pattern of exanthem associated with COVID-19 infection.
- Further studies are needed to evaluate whether these lesions are associated with the virus, the drug intake or any other conditions.
- COVID-19 Toes.
- Similar to the type of cold related changes we have seen in the feet of people for many years, but often occurring in places where the conditions are not cold and damp.
- These seem to happen more commonly in younger patients.
- Chilblain‐like lesions
- The pseudo‐chilblain pattern frequently appears late in the evolution of the COVID‐19 disease.
- The lesion was red–purple papules on the dorsal aspect of the fingers on both hands and diffused erythema in the subungual area of thumb.
Laboratory Findings
- D-dimer, fibrinogen, and fibrinogen degradation product (FDP) were significantly elevated in most patients.
- Prothrombin time was prolonged in 4 patients. D-dimer and FDP levels progressively elevated consistent with COVID-2019 exacerbation.
- Disseminated intravascular coagulation.
- HSV is suspected of provoking stimulation of immunopathological mechanisms in erythema multiforme.
- The herpes virus could play a role in autoimmune cross-reactivity, triggering the keratinocyte that activates IL-1, IFN-γ, and TNF-α, recruiting cytotoxic and NK cells that target the keratinocytes itself.
Electrocardiogram
There are no ECG findings associated with covid-19 rash.
X-ray
There are no x-ray findings associated with covid-19 rash.
Echocardiography or Ultrasound
There are no echocardiography/ultrasound findings associated with covid-19 rash.
CT scan
There are no CT scan findings associated with covid-19 rash.
MRI
There are no MRI findings associated with covid-19 rash..
Other Imaging Findings
There are no other imaging findings associated with covid-19 rash..
Treatment
- Supportive care for patients is typically the standard protocol because no specific effective antiviral therapies have been identified.
- Currently, infection prevention and control are considered urgent and critical due to the lack of specific treatment and heightened risk of spreading during the incubation period.
Primary Prevention
- Effective measures for the primary prevention of COVID-19 include:[57]
- Frequent handwashing with soap and water for at least 20 seconds or using a alcohol based hand sanitizer with at least 60% alcohol
- Staying at least 6 feet (about 2 arms’ length) from other people who do not live with you
- Covering your mouth and nose with a cloth face cover when around others and covering sneezes and coughs
- Cleaning and disinfecting
- There have been rigorous efforts in order to develop a vaccine for novel coronavirus and several vaccines are in the later phases of trials.[58]
Secondary prevention
- Effective measures for the secondary prevention of COVID-19 include:
- Use of personal protective equipment (PPE) by the personnel handling the fecal matter.
- Screening of fecal microbiota transplant donors for COVID-19 is also recommended.[59]
- Contact tracing helps reduce the spread of the disease.[60]
References
- ↑ https://www.cdc.gov/coronavirus/2019-ncov/about/index.html. Missing or empty
|title=(help) - ↑ Lu, Jian; Cui, Jie; Qian, Zhaohui; Wang, Yirong; Zhang, Hong; Duan, Yuange; Wu, Xinkai; Yao, Xinmin; Song, Yuhe; Li, Xiang; Wu, Changcheng; Tang, Xiaolu (2020). "On the origin and continuing evolution of SARS-CoV-2". National Science Review. doi:10.1093/nsr/nwaa036. ISSN 2095-5138.
- ↑ Huang, Chaolin; Wang, Yeming; Li, Xingwang; Ren, Lili; Zhao, Jianping; Hu, Yi; Zhang, Li; Fan, Guohui; Xu, Jiuyang; Gu, Xiaoying; Cheng, Zhenshun; Yu, Ting; Xia, Jiaan; Wei, Yuan; Wu, Wenjuan; Xie, Xuelei; Yin, Wen; Li, Hui; Liu, Min; Xiao, Yan; Gao, Hong; Guo, Li; Xie, Jungang; Wang, Guangfa; Jiang, Rongmeng; Gao, Zhancheng; Jin, Qi; Wang, Jianwei; Cao, Bin (2020). "Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China". The Lancet. 395 (10223): 497–506. doi:10.1016/S0140-6736(20)30183-5. ISSN 0140-6736.
- ↑ https://www.cdc.gov/coronavirus/2019-ncov/about/transmission.html. Missing or empty
|title=(help) - ↑ Heymann, David L; Shindo, Nahoko (2020). "COVID-19: what is next for public health?". The Lancet. 395 (10224): 542–545. doi:10.1016/S0140-6736(20)30374-3. ISSN 0140-6736.
- ↑ Rothe, Camilla; Schunk, Mirjam; Sothmann, Peter; Bretzel, Gisela; Froeschl, Guenter; Wallrauch, Claudia; Zimmer, Thorbjörn; Thiel, Verena; Janke, Christian; Guggemos, Wolfgang; Seilmaier, Michael; Drosten, Christian; Vollmar, Patrick; Zwirglmaier, Katrin; Zange, Sabine; Wölfel, Roman; Hoelscher, Michael (2020). "Transmission of 2019-nCoV Infection from an Asymptomatic Contact in Germany". New England Journal of Medicine. 382 (10): 970–971. doi:10.1056/NEJMc2001468. ISSN 0028-4793.
- ↑ Zhou, Peng; Yang, Xing-Lou; Wang, Xian-Guang; Hu, Ben; Zhang, Lei; Zhang, Wei; Si, Hao-Rui; Zhu, Yan; Li, Bei; Huang, Chao-Lin; Chen, Hui-Dong; Chen, Jing; Luo, Yun; Guo, Hua; Jiang, Ren-Di; Liu, Mei-Qin; Chen, Ying; Shen, Xu-Rui; Wang, Xi; Zheng, Xiao-Shuang; Zhao, Kai; Chen, Quan-Jiao; Deng, Fei; Liu, Lin-Lin; Yan, Bing; Zhan, Fa-Xian; Wang, Yan-Yi; Xiao, Geng-Fu; Shi, Zheng-Li (2020). "A pneumonia outbreak associated with a new coronavirus of probable bat origin". Nature. doi:10.1038/s41586-020-2012-7. ISSN 0028-0836.
- ↑ Lu R, Zhao X, Li J, Niu P, Yang B, Wu H, Wang W, Song H, Huang B, Zhu N, Bi Y, Ma X, Zhan F, Wang L, Hu T, Zhou H, Hu Z, Zhou W, Zhao L, Chen J, Meng Y, Wang J, Lin Y, Yuan J, Xie Z, Ma J, Liu WJ, Wang D, Xu W, Holmes EC, Gao GF, Wu G, Chen W, Shi W, Tan W (February 2020). "Genomic characterisation and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding". Lancet. 395 (10224): 565–574. doi:10.1016/S0140-6736(20)30251-8. PMID 32007145 Check
|pmid=value (help). - ↑ Zhou P, Yang XL, Wang XG, Hu B, Zhang L, Zhang W, Si HR, Zhu Y, Li B, Huang CL, Chen HD, Chen J, Luo Y, Guo H, Jiang RD, Liu MQ, Chen Y, Shen XR, Wang X, Zheng XS, Zhao K, Chen QJ, Deng F, Liu LL, Yan B, Zhan FX, Wang YY, Xiao GF, Shi ZL (February 2020). "A pneumonia outbreak associated with a new coronavirus of probable bat origin". Nature. doi:10.1038/s41586-020-2012-7. PMID 32015507 Check
|pmid=value (help). - ↑ Crackower, Michael A.; Sarao, Renu; Oudit, Gavin Y.; Yagil, Chana; Kozieradzki, Ivona; Scanga, Sam E.; Oliveira-dos-Santos, Antonio J.; da Costa, Joan; Zhang, Liyong; Pei, York; Scholey, James; Ferrario, Carlos M.; Manoukian, Armen S.; Chappell, Mark C.; Backx, Peter H.; Yagil, Yoram; Penninger, Josef M. (2002). "Angiotensin-converting enzyme 2 is an essential regulator of heart function". Nature. 417 (6891): 822–828. doi:10.1038/nature00786. ISSN 0028-0836.
- ↑ Danilczyk, Ursula; Sarao, Renu; Remy, Christine; Benabbas, Chahira; Stange, Gerti; Richter, Andreas; Arya, Sudha; Pospisilik, J. Andrew; Singer, Dustin; Camargo, Simone M. R.; Makrides, Victoria; Ramadan, Tamara; Verrey, Francois; Wagner, Carsten A.; Penninger, Josef M. (2006). "Essential role for collectrin in renal amino acid transport". Nature. 444 (7122): 1088–1091. doi:10.1038/nature05475. ISSN 0028-0836.
- ↑ Gu, Jiang; Gong, Encong; Zhang, Bo; Zheng, Jie; Gao, Zifen; Zhong, Yanfeng; Zou, Wanzhong; Zhan, Jun; Wang, Shenglan; Xie, Zhigang; Zhuang, Hui; Wu, Bingquan; Zhong, Haohao; Shao, Hongquan; Fang, Weigang; Gao, Dongshia; Pei, Fei; Li, Xingwang; He, Zhongpin; Xu, Danzhen; Shi, Xeying; Anderson, Virginia M.; Leong, Anthony S.-Y. (2005). "Multiple organ infection and the pathogenesis of SARS". The Journal of Experimental Medicine. 202 (3): 415–424. doi:10.1084/jem.20050828. ISSN 1540-9538.
- ↑ Ding, Yanqing; He, Li; Zhang, Qingling; Huang, Zhongxi; Che, Xiaoyan; Hou, Jinlin; Wang, Huijun; Shen, Hong; Qiu, Liwen; Li, Zhuguo; Geng, Jian; Cai, Junjie; Han, Huixia; Li, Xin; Kang, Wei; Weng, Desheng; Liang, Ping; Jiang, Shibo (2004). "Organ distribution of severe acute respiratory syndrome(SARS) associated coronavirus(SARS-CoV) in SARS patients: implications for pathogenesis and virus transmission pathways". The Journal of Pathology. 203 (2): 622–630. doi:10.1002/path.1560. ISSN 0022-3417.
- ↑ Hamming, I; Timens, W; Bulthuis, MLC; Lely, AT; Navis, GJ; van Goor, H (2004). "Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis". The Journal of Pathology. 203 (2): 631–637. doi:10.1002/path.1570. ISSN 0022-3417.
- ↑ Wang, Dawei; Hu, Bo; Hu, Chang; Zhu, Fangfang; Liu, Xing; Zhang, Jing; Wang, Binbin; Xiang, Hui; Cheng, Zhenshun; Xiong, Yong; Zhao, Yan; Li, Yirong; Wang, Xinghuan; Peng, Zhiyong (2020). "Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus–Infected Pneumonia in Wuhan, China". JAMA. doi:10.1001/jama.2020.1585. ISSN 0098-7484.
- ↑ Huang, Chaolin; Wang, Yeming; Li, Xingwang; Ren, Lili; Zhao, Jianping; Hu, Yi; Zhang, Li; Fan, Guohui; Xu, Jiuyang; Gu, Xiaoying; Cheng, Zhenshun; Yu, Ting; Xia, Jiaan; Wei, Yuan; Wu, Wenjuan; Xie, Xuelei; Yin, Wen; Li, Hui; Liu, Min; Xiao, Yan; Gao, Hong; Guo, Li; Xie, Jungang; Wang, Guangfa; Jiang, Rongmeng; Gao, Zhancheng; Jin, Qi; Wang, Jianwei; Cao, Bin (2020). "Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China". The Lancet. 395 (10223): 497–506. doi:10.1016/S0140-6736(20)30183-5. ISSN 0140-6736.
- ↑ Guan, Wei-jie; Ni, Zheng-yi; Hu, Yu; Liang, Wen-hua; Ou, Chun-quan; He, Jian-xing; Liu, Lei; Shan, Hong; Lei, Chun-liang; Hui, David SC; Du, Bin; Li, Lan-juan; Zeng, Guang; Yuen, Kowk-Yung; Chen, Ru-chong; Tang, Chun-li; Wang, Tao; Chen, Ping-yan; Xiang, Jie; Li, Shi-yue; Wang, Jin-lin; Liang, Zi-jing; Peng, Yi-xiang; Wei, Li; Liu, Yong; Hu, Ya-hua; Peng, Peng; Wang, Jian-ming; Liu, Ji-yang; Chen, Zhong; Li, Gang; Zheng, Zhi-jian; Qiu, Shao-qin; Luo, Jie; Ye, Chang-jiang; Zhu, Shao-yong; Zhong, Nan-shan (2020). doi:10.1101/2020.02.06.20020974. Missing or empty
|title=(help) - ↑ Todd JK (1988). "Toxic shock syndrome". Clin. Microbiol. Rev. 1 (4): 432–46. PMC 358064. PMID 3069202.
- ↑ Kang JH (2015). "Febrile Illness with Skin Rashes". Infect Chemother. 47 (3): 155–66. doi:10.3947/ic.2015.47.3.155. PMC 4607768. PMID 26483989.
- ↑ Sivagnanam S, Deleu D (2003). "Red man syndrome". Crit Care. 7 (2): 119–20. PMC 270616. PMID 12720556.
- ↑ McGregor JA, Soper DE, Lovell G, Todd JK (1989). "Maternal deaths associated with Clostridium sordellii infection". Am. J. Obstet. Gynecol. 161 (4): 987–95. PMID 2801850.
- ↑ "Clostridium sordellii toxic shock syndrome after medical abortion with mifepristone and intravaginal misoprostol--United States and Canada, 2001-2005". MMWR Morb. Mortal. Wkly. Rep. 54 (29): 724. 2005. PMID 16049422.
- ↑ Fischer M, Bhatnagar J, Guarner J, Reagan S, Hacker JK, Van Meter SH, Poukens V, Whiteman DB, Iton A, Cheung M, Dassey DE, Shieh WJ, Zaki SR (2005). "Fatal toxic shock syndrome associated with Clostridium sordellii after medical abortion". N. Engl. J. Med. 353 (22): 2352–60. doi:10.1056/NEJMoa051620. PMID 16319384.
- ↑ Sinave C, Le Templier G, Blouin D, Léveillé F, Deland E (2002). "Toxic shock syndrome due to Clostridium sordellii: a dramatic postpartum and postabortion disease". Clin. Infect. Dis. 35 (11): 1441–3. doi:10.1086/344464. PMID 12439811.
- ↑ Ho CS, Bhatnagar J, Cohen AL, Hacker JK, Zane SB, Reagan S, Fischer M, Shieh WJ, Guarner J, Ahmad S, Zaki SR, McDonald LC (2009). "Undiagnosed cases of fatal Clostridium-associated toxic shock in Californian women of childbearing age". Am. J. Obstet. Gynecol. 201 (5): 459.e1–7. doi:10.1016/j.ajog.2009.05.023. PMID 19628200.
- ↑ Kang JH (2015). "Febrile Illness with Skin Rashes". Infect Chemother. 47 (3): 155–66. doi:10.3947/ic.2015.47.3.155. PMC 4607768. PMID 26483989.
- ↑ Brook MG, Bannister BA (1988). "Scarlet fever can mimic toxic shock syndrome". Postgrad Med J. 64 (758): 965–7. PMC 2429080. PMID 3256819.
- ↑ Minemura M, Tajiri K, Shimizu Y (2014). "Liver involvement in systemic infection". World J Hepatol. 6 (9): 632–42. doi:10.4254/wjh.v6.i9.632. PMC 4179142. PMID 25276279.
- ↑ Chesney RW, Chesney PJ, Davis JP, Segar WE (1981). "Renal manifestations of the staphylococcal toxic-shock syndrome". Am. J. Med. 71 (4): 583–8. PMID 7282746.
- ↑ Harrison LH (2010). "Epidemiological profile of meningococcal disease in the United States". Clin. Infect. Dis. 50 Suppl 2: S37–44. doi:10.1086/648963. PMC 2820831. PMID 20144015.
- ↑ MacLennan J, Kafatos G, Neal K, Andrews N, Cameron JC, Roberts R, Evans MR, Cann K, Baxter DN, Maiden MC, Stuart JM (2006). "Social behavior and meningococcal carriage in British teenagers". Emerging Infect. Dis. 12 (6): 950–7. PMC 3373034. PMID 16707051.
- ↑ WARTENBERG R (1950). "The signs of Brudzinski and of Kernig". J. Pediatr. 37 (4): 679–84. PMID 14779273.
- ↑ Bush LM (2014). "Case 28-2014: A man with a rash, headache, fever, nausea, and photophobia". N. Engl. J. Med. 371 (23): 2238–9. doi:10.1056/NEJMc1412237#SA2. PMID 25470712.
- ↑ "Meningitis Symptoms - Meningitis Research Foundation".
- ↑ Chung WH, Hung SI, Hong HS, Hsih MS, Yang LC, Ho HC, Wu JY, Chen YT (2004). "Medical genetics: a marker for Stevens-Johnson syndrome". Nature. 428 (6982): 486. doi:10.1038/428486a. PMID 15057820.
- ↑ Techasatian L, Panombualert S, Uppala R, Jetsrisuparb C (2016). "Drug-induced Stevens-Johnson syndrome and toxic epidermal necrolysis in children: 20 years study in a tertiary care hospital". World J Pediatr. doi:10.1007/s12519-016-0057-3. PMID 27650525.
- ↑ Harr T, French LE (2010). "Toxic epidermal necrolysis and Stevens-Johnson syndrome". Orphanet J Rare Dis. 5: 39. doi:10.1186/1750-1172-5-39. PMC 3018455. PMID 21162721.
- ↑ Harr T, French LE (2010). "Toxic epidermal necrolysis and Stevens-Johnson syndrome". Orphanet J Rare Dis. 5: 39. doi:10.1186/1750-1172-5-39. PMC 3018455. PMID 21162721.
- ↑ Chang YS, Huang FC, Tseng SH, Hsu CK, Ho CL, Sheu HM (2007). "Erythema multiforme, Stevens-Johnson syndrome, and toxic epidermal necrolysis: acute ocular manifestations, causes, and management". Cornea. 26 (2): 123–9. doi:10.1097/ICO.0b013e31802eb264. PMID 17251797.
- ↑ Harr T, French LE (2010). "Toxic epidermal necrolysis and Stevens-Johnson syndrome". Orphanet J Rare Dis. 5: 39. doi:10.1186/1750-1172-5-39. PMC 3018455. PMID 21162721.
- ↑ Choudhary S, McLeod M, Torchia D, Romanelli P (2013). "Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) Syndrome". J Clin Aesthet Dermatol. 6 (6): 31–7. PMC 3718748. PMID 23882307.
- ↑ Eshki M, Allanore L, Musette P, Milpied B, Grange A, Guillaume JC, Chosidow O, Guillot I, Paradis V, Joly P, Crickx B, Ranger-Rogez S, Descamps V (2009). "Twelve-year analysis of severe cases of drug reaction with eosinophilia and systemic symptoms: a cause of unpredictable multiorgan failure". Arch Dermatol. 145 (1): 67–72. doi:10.1001/archderm.145.1.67. PMID 19153346.
- ↑ Peyrière H, Dereure O, Breton H, Demoly P, Cociglio M, Blayac JP, Hillaire-Buys D (2006). "Variability in the clinical pattern of cutaneous side-effects of drugs with systemic symptoms: does a DRESS syndrome really exist?". Br. J. Dermatol. 155 (2): 422–8. doi:10.1111/j.1365-2133.2006.07284.x. PMID 16882184.
- ↑ Eshki M, Allanore L, Musette P, Milpied B, Grange A, Guillaume JC, Chosidow O, Guillot I, Paradis V, Joly P, Crickx B, Ranger-Rogez S, Descamps V (2009). "Twelve-year analysis of severe cases of drug reaction with eosinophilia and systemic symptoms: a cause of unpredictable multiorgan failure". Arch Dermatol. 145 (1): 67–72. doi:10.1001/archderm.145.1.67. PMID 19153346.
- ↑ Wallace MR, Mascola JR, Oldfield EC (1991). "Red man syndrome: incidence, etiology, and prophylaxis". J. Infect. Dis. 164 (6): 1180–5. PMID 1955716.
- ↑ Sivagnanam S, Deleu D (2003). "Red man syndrome". Crit Care. 7 (2): 119–20. PMC 270616. PMID 12720556.
- ↑ Renz CL, Laroche D, Thurn JD, Finn HA, Lynch JP, Thisted R, Moss J (1998). "Tryptase levels are not increased during vancomycin-induced anaphylactoid reactions". Anesthesiology. 89 (3): 620–5. PMID 9743397.
- ↑ Lin YJ, Cheng MC, Lo MH, Chien SJ (2015). "Early Differentiation of Kawasaki Disease Shock Syndrome and Toxic Shock Syndrome in a Pediatric Intensive Care Unit". Pediatr. Infect. Dis. J. 34 (11): 1163–7. doi:10.1097/INF.0000000000000852. PMID 26222065.
- ↑ http://weekly.chinacdc.cn/en/article/id/e53946e2-c6c4-41e9-9a9b-fea8db1a8f51. Missing or empty
|title=(help) - ↑ Li, Qun; Guan, Xuhua; Wu, Peng; Wang, Xiaoye; Zhou, Lei; Tong, Yeqing; Ren, Ruiqi; Leung, Kathy S.M.; Lau, Eric H.Y.; Wong, Jessica Y.; Xing, Xuesen; Xiang, Nijuan; Wu, Yang; Li, Chao; Chen, Qi; Li, Dan; Liu, Tian; Zhao, Jing; Liu, Man; Tu, Wenxiao; Chen, Chuding; Jin, Lianmei; Yang, Rui; Wang, Qi; Zhou, Suhua; Wang, Rui; Liu, Hui; Luo, Yinbo; Liu, Yuan; Shao, Ge; Li, Huan; Tao, Zhongfa; Yang, Yang; Deng, Zhiqiang; Liu, Boxi; Ma, Zhitao; Zhang, Yanping; Shi, Guoqing; Lam, Tommy T.Y.; Wu, Joseph T.; Gao, George F.; Cowling, Benjamin J.; Yang, Bo; Leung, Gabriel M.; Feng, Zijian (2020). "Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus–Infected Pneumonia". New England Journal of Medicine. doi:10.1056/NEJMoa2001316. ISSN 0028-4793.
- ↑ Heymann, David L; Shindo, Nahoko (2020). "COVID-19: what is next for public health?". The Lancet. 395 (10224): 542–545. doi:10.1016/S0140-6736(20)30374-3. ISSN 0140-6736.
- ↑ https://www.cdc.gov/coronavirus/2019-ncov/specific-groups/high-risk-complications.html. Missing or empty
|title=(help) - ↑ Hu, Zhiliang; Song, Ci; Xu, Chuanjun; Jin, Guangfu; Chen, Yaling; Xu, Xin; Ma, Hongxia; Chen, Wei; Lin, Yuan; Zheng, Yishan; Wang, Jianming; Hu, Zhibin; Yi, Yongxiang; Shen, Hongbing (2020). "Clinical characteristics of 24 asymptomatic infections with COVID-19 screened among close contacts in Nanjing, China". Science China Life Sciences. doi:10.1007/s11427-020-1661-4. ISSN 1674-7305.
- ↑ Porcheddu, Rossella; Serra, Caterina; Kelvin, David; Kelvin, Nikki; Rubino, Salvatore (2020). "Similarity in Case Fatality Rates (CFR) of COVID-19/SARS-COV-2 in Italy and China". The Journal of Infection in Developing Countries. 14 (02): 125–128. doi:10.3855/jidc.12600. ISSN 1972-2680.
- ↑ Wilder-Smith, Annelies; Chiew, Calvin J; Lee, Vernon J (2020). "Can we contain the COVID-19 outbreak with the same measures as for SARS?". The Lancet Infectious Diseases. doi:10.1016/S1473-3099(20)30129-8. ISSN 1473-3099.
- ↑ (PDF) https://www.cdc.gov/coronavirus/2019-ncov/downloads/community-mitigation-strategy.pdf. Missing or empty
|title=(help) - ↑ "How to Protect Yourself & Others | CDC".
- ↑ "NIH clinical trial of investigational vaccine for COVID-19 begins | National Institutes of Health (NIH)".
- ↑ Green CA, Quraishi MN, Shabir S, Sharma N, Hansen R, Gaya DR, Hart AL, Loman NJ, Iqbal TH (June 2020). "Screening faecal microbiota transplant donors for SARS-CoV-2 by molecular testing of stool is the safest way forward". Lancet Gastroenterol Hepatol. 5 (6): 531. doi:10.1016/S2468-1253(20)30089-3. PMC 7225406 Check
|pmc=value (help). PMID 32240618 Check|pmid=value (help). - ↑ "Contact Tracing for COVID-19 | CDC".