Dysphagia pathophysiology: Difference between revisions
Feham Tariq (talk | contribs) |
Feham Tariq (talk | contribs) |
||
| Line 283: | Line 283: | ||
===Zenkers diverticulum=== | ===Zenkers diverticulum=== | ||
[[Image:Micro Zenker.jpg|200px|<br> Source:Librepathology<ref name="urlFile:Pharyngoesophageal diverticulum - alt -- very low mag.jpg - Libre Pathology">{{cite web |url=https://librepathology.org/wiki/File:Pharyngoesophageal_diverticulum_-_alt_--_very_low_mag.jpg |title=File:Pharyngoesophageal diverticulum - alt -- very low mag.jpg - Libre Pathology |format= |work= |accessdate=}}</ref> | [[Image:Micro Zenker.jpg|200px|thumb|<br> Source:Librepathology<ref name="urlFile:Pharyngoesophageal diverticulum - alt -- very low mag.jpg - Libre Pathology">{{cite web |url=https://librepathology.org/wiki/File:Pharyngoesophageal_diverticulum_-_alt_--_very_low_mag.jpg |title=File:Pharyngoesophageal diverticulum - alt -- very low mag.jpg - Libre Pathology |format= |work= |accessdate=}}</ref> | ||
<nowiki></gallery></nowiki>]] | <nowiki></gallery></nowiki>]] | ||
Revision as of 16:07, 2 February 2018
|
Dysphagia Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Dysphagia pathophysiology On the Web |
|
American Roentgen Ray Society Images of Dysphagia pathophysiology |
|
Risk calculators and risk factors for Dysphagia pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]Associate Editor(s)-in-Chief: Feham Tariq, MD [2]
Overview
Dysphagia can result from propulsive failure, motility disorders, structural disorders, intrinsic or extrinsic compression of the oropharynx or esophagus. Propulsive failure can result from dysfunction of the central nervous system control mechanisms, intrinsic musculature, or peripheral nerves. Structural abnormalities may result from surgery, neoplasm, caustic injury, or congenital anomalies.
Pathophysiology
Physiology of normal swallowing
Anatomically, swallowing can be divided into three phases:[1][2][3][4]
- Oral preparatory phase
- Oral voluntary phase
- Pharyngeal phase
- Esophageal phase
(a)Oral preparatory phase:
- This phase involves mastication and formation of a bolus in the oral cavity.
(b)Oral voluntary phase:
- It is characterized by propelling the bolus into the pharyngeal phase.
- It is controlled by the corticobulbar tracts and cranial nerves V(trigemenal),VII(facial)and XII(hypoglossal).
(c)Pharyngeal phase:
- This phase is a reflex
- It is controlled by the cranial nerves V(trigemenal),X(vagus)XI(accessory) and, XII(hypoglossal).
(d)Esophageal phase:
- The esophagus is a part of the gastrointestinal tract which is responsible of moving the food from the mouth to the rectum.[5]
- The esophagus has anti-reflux barrier which prevents the return of the acidic contentof the stomach back to the esophagus. The anti-reflux barrier consists of the lower esophageal sphincter (LES) and the related part of the diaphragm.
- The lower esophageal sphincter is contracting smooth muscle at the end of the esophagus responsible for the food passage to the stomach. LES has high pressure tone which helps keeping it a strong barrier between the esophagus and the stomach.
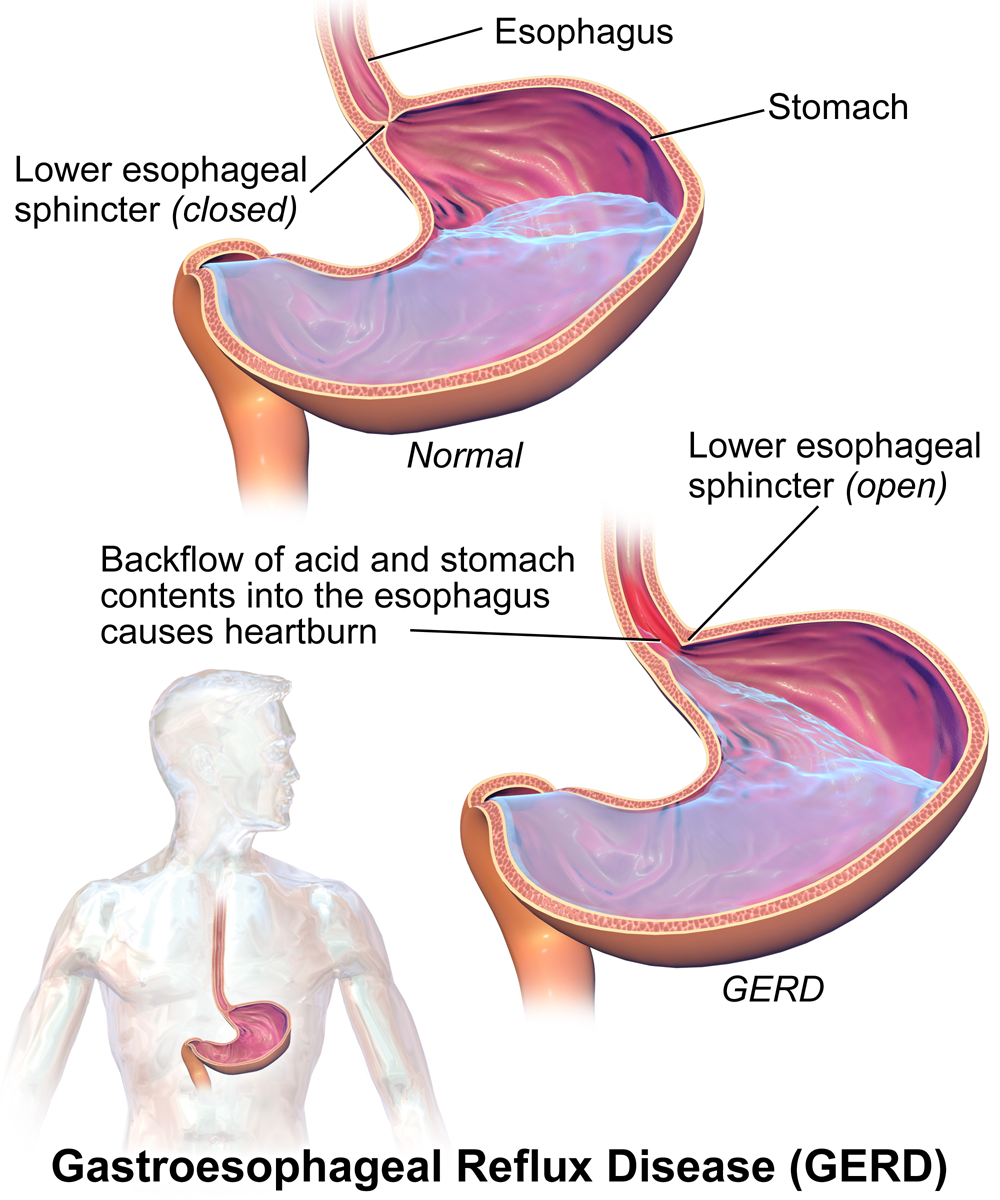
Pathogenesis of Dysphagia
The pathogenesis of dysphagia can be explained on the basis of etiology. It can be
- Physiological
- Pathological
{{#ev:youtube|X4ryV6wGK1Y}}
Effect of aging on swallowing mechanism
Physiological dysphagia
Normal aging results in following changes in the swallowing mechanism:[6][7][8][9][10]
- Reduced lingual movement
- Delayed onset of the pharyngeal swallow
- Delayed upper esophageal sphincter manometric relaxation during swallowing
- Diminished pharyngolaryngeal sensory discrimination
- Cerebral atrophy
- Deterioration in nerve function
- Region-dependent decline in muscle mass
Pathological dysphagia
Following mechanisms can lead to pathological dysphagia.
Luminal Stenosis
Esophageal lumen can be narrowed by the following factors:[11][12][13][14]
- Stricture
- Inflammation
- Web
- Malignancy
Non-obstructing gastro-esophageal disease
Many patients that describe dysphagia will have normal investigations including UGE and high-resolution manometry (HRM), suggesting that a dysfunction of the somatosensory as opposed to neuromuscular apparatus might be present[15]
Primary motility disorder
Rheumatological conditions
Medication induced
Neurological disorders
The following table summarizes the mechanism, genetic association, gross pathology features and microscopic findings of each cause.
| Cause of dysphagia | Type of food | Type of progression | Pathophysiological changes | Genetic association | Gross pathology features | Microscopic findings | |
|---|---|---|---|---|---|---|---|
| Oropharyngeal dysphagia | Soilds | Liquids | Intermittent/Progressive | ||||
| •Zenker's diverticulum
•Webs |
Yes | No | Progressive | •Zenker's diverticulum(ZD):
|
Diverticulum or a sac is seen in the esophagus |
| |
| •Webs | |||||||
| •Neoplasm | Yes | Yes | Progressive | •Neoplasm | |||
| Myogenic causes
•Myasthenia gravis •Connective tissue disorder •Myotonic dystrophy Neurogenic causes •ALS •Parkinsonism •Stroke |
Yes | Yes | Progressive | ||||
| Esophageal dysphagia | |||||||
| •Pill esophagitis
•Caustic injury •Chemotherapy |
Yes | No | |||||
| •Strictures
•Esophageal Cancer |
Yes | No | Progressive | Esophageal stricture is the result of:[16][17]
|
The following genes can be involved:
|
On gross pathology, circumferential thickening of the lower esophageal wall are characteristic finding of esophageal stricture due to gastroesophageal reflux disease.[18]
|
On microscopic histopathological analysis, characteristic findings of esophageal stricture due to gastroesophageal reflux disease are:[22]
|
| •Esophageal Cancer: |
Mutations in the following genes can cause esophageal cancer: |
Squamous cell carcinoma or adenocarcinoma of the esophagus may appear as:[24]
|
Nuclear atypia of malignancy:
| ||||
| •Rings
•Webs |
Yes | No | Intermittent | Rings:
Webs: Multiple theories have been found:
|
|||
| •Achalasia
•Diffuse esophageal spasm(DES) |
Yes | Yes | Intermittent | •Achalasia:
|
|
| |
•Diffuse esophageal spasm(DES):
|
There is a genetic association between DES and achalasia[29] | Gross thickening of muscularis propria layer and lower esophageal sphincter (LES) due to hyperplasia are characteristic findings of DES | There is degeneration of vagal fibres, inflammatory infiltration of myenteric plexus, and hyperplasia of smooth muscles are characteristic findings of DES | ||||
| •Scleroderma | Yes | Yes | Progressive | ||||
Gallery
Zenkers diverticulum
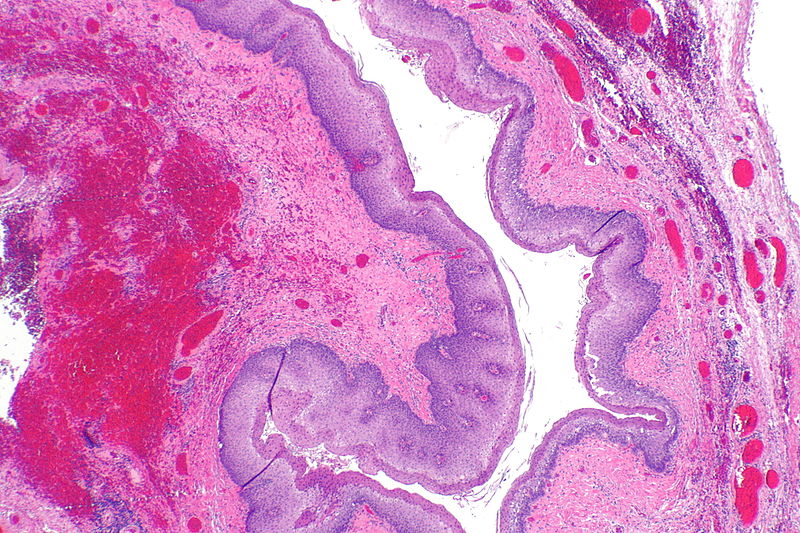
Source:Librepathology[30] </gallery>
Esophageal cancer

Esophagitis

Esophageal stricture


References
- ↑ Cook, Ian J.; Kahrilas, Peter J. (1999). "AGA technical review on management of oropharyngeal dysphagia". Gastroenterology. 116 (2): 455–478. doi:10.1016/S0016-5085(99)70144-7. ISSN 0016-5085.
- ↑ Aslam M, Vaezi MF (2013). "Dysphagia in the elderly". Gastroenterol Hepatol (N Y). 9 (12): 784–95. PMC 3999993. PMID 24772045.
- ↑ Cassiani RA, Santos CM, Parreira LC, Dantas RO (2011). "The relationship between the oral and pharyngeal phases of swallowing". Clinics (Sao Paulo). 66 (8): 1385–8. PMC 3161216. PMID 21915488.
- ↑ Dantas RO, Kern MK, Massey BT, Dodds WJ, Kahrilas PJ, Brasseur JG; et al. (1990). "Effect of swallowed bolus variables on oral and pharyngeal phases of swallowing". Am J Physiol. 258 (5 Pt 1): G675–81. doi:10.1152/ajpgi.1990.258.5.G675. PMID 2333995.
- ↑ Stein HJ, DeMeester TR (1992). "Outpatient physiologic testing and surgical management of foregut motility disorders". Curr Probl Surg. 29 (7): 413–555. PMID 1606845.
- ↑ Masoro EJ (1987). "Biology of aging. Current state of knowledge". Arch Intern Med. 147 (1): 166–9. PMID 3541821.
- ↑ Carucci LR, Turner MA (2015). "Dysphagia revisited: common and unusual causes". Radiographics. 35 (1): 105–22. doi:10.1148/rg.351130150. PMID 25590391.
- ↑ Cook IJ, Weltman MD, Wallace K, Shaw DW, McKay E, Smart RC; et al. (1994). "Influence of aging on oral-pharyngeal bolus transit and clearance during swallowing: scintigraphic study". Am J Physiol. 266 (6 Pt 1): G972–7. doi:10.1152/ajpgi.1994.266.6.G972. PMID 8023945.
- ↑ Shaw DW, Cook IJ, Gabb M, Holloway RH, Simula ME, Panagopoulos V; et al. (1995). "Influence of normal aging on oral-pharyngeal and upper esophageal sphincter function during swallowing". Am J Physiol. 268 (3 Pt 1): G389–96. doi:10.1152/ajpgi.1995.268.3.G389. PMID 7900799.
- ↑ Easterling, Caryn S.; Robbins, Elizabeth (2008). "Dementia and Dysphagia". Geriatric Nursing. 29 (4): 275–285. doi:10.1016/j.gerinurse.2007.10.015. ISSN 0197-4572.
- ↑ Starmer HM, Riley LH, Hillel AT, Akst LM, Best SR, Gourin CG (2014). "Dysphagia, short-term outcomes, and cost of care after anterior cervical disc surgery". Dysphagia. 29 (1): 68–77. doi:10.1007/s00455-013-9482-9. PMID 23943072.
- ↑ Inayat F, Hussain Q, Shafique K (2017). "Dysphagia Caused by Extrinsic Esophageal Compression From Mediastinal Lymphadenopathy in Patients With Sarcoidosis". Clin Gastroenterol Hepatol. 15 (7): e119–e120. doi:10.1016/j.cgh.2016.11.010. PMID 27840183.
- ↑ Oda K, Iwakiri R, Hara M, Watanabe K, Danjo A, Shimoda R; et al. (2005). "Dysphagia associated with gastroesophageal reflux disease is improved by proton pump inhibitor". Dig Dis Sci. 50 (10): 1921–6. doi:10.1007/s10620-005-2962-5. PMID 16187198.
- ↑ Roman S, Kahrilas PJ (2014). "The diagnosis and management of hiatus hernia". BMJ. 349: g6154. doi:10.1136/bmj.g6154. PMID 25341679.
- ↑ Philpott H, Nandurkar S, Royce SG, Thien F, Gibson PR (2014). "Risk factors for eosinophilic esophagitis". Clin Exp Allergy. 44 (8): 1012–9. doi:10.1111/cea.12363. PMID 24990069.
- ↑ Holzheimer, R (2001). Surgical treatment : evidence-based and problem-oriented. München New York: Zuckschwerdt. ISBN 3-88603-714-2.
- ↑ Belevich VL, Ovchinnikov DV (2013). "[Treatment of benign esophageal stricture]". Vestn. Khir. Im. I. I. Grek. (in Russian). 172 (5): 111–4. PMID 24640761.
- ↑ Yamasaki, Yasushi; Ozawa, Soji; Oguma, Junya; Kazuno, Akihito; Ninomiya, Yamato (2016). "Long peptic strictures of the esophagus due to reflux esophagitis: a case report". Surgical Case Reports. 2 (1). doi:10.1186/s40792-016-0190-1. ISSN 2198-7793.
- ↑ Maejima, Ryuhei; Uno, Kaname; Iijima, Katsunori; Fujishima, Fumiyoshi; Noguchi, Tetsuya; Ara, Nobuyuki; Asano, Naoki; Koike, Tomoyuki; Imatani, Akira; Shimosegawa, Tooru (2016). "A Japanese case of lymphocytic esophagitis". Digestive Endoscopy. 28 (4): 476–480. doi:10.1111/den.12578. ISSN 0915-5635.
- ↑ Contini, Sandro (2013). "Caustic injury of the upper gastrointestinal tract: A comprehensive review". World Journal of Gastroenterology. 19 (25): 3918. doi:10.3748/wjg.v19.i25.3918. ISSN 1007-9327.
- ↑ Wilcox CM (2013). "Overview of infectious esophagitis". Gastroenterol Hepatol (N Y). 9 (8): 517–9. PMC 3980995. PMID 24719600.
- ↑ "Esophageal stricture - Libre Pathology".
- ↑
- ↑ Sugarbaker, David (2015). Adult chest surgery. New York: McGraw-Hill Education. ISBN 0071781897.
- ↑ "Squamous cell carcinoma of the esophagus".
- ↑ Paladini F, Cocco E, Cascino I, Belfiore F, Badiali D, Piretta L; et al. (2009). "Age-dependent association of idiopathic achalasia with vasoactive intestinal peptide receptor 1 gene". Neurogastroenterol Motil. 21 (6): 597–602. doi:10.1111/j.1365-2982.2009.01284.x. PMID 19309439.
- ↑ Alahdab YO, Eren F, Giral A, Gunduz F, Kedrah AE, Atug O; et al. (2012). "Preliminary evidence of an association between the functional c-kit rs6554199 polymorphism and achalasia in a Turkish population". Neurogastroenterol Motil. 24 (1): 27–30. doi:10.1111/j.1365-2982.2011.01793.x. PMID 21951831.
- ↑ de León AR, de la Serna JP, Santiago JL, Sevilla C, Fernández-Arquero M, de la Concha EG; et al. (2010). "Association between idiopathic achalasia and IL23R gene". Neurogastroenterol Motil. 22 (7): 734–8, e218. doi:10.1111/j.1365-2982.2010.01497.x. PMID 20367798.
- ↑ Frieling T, Berges W, Borchard F, Lübke HJ, Enck P, Wienbeck M (1988). "Family occurrence of achalasia and diffuse spasm of the oesophagus". Gut. 29 (11): 1595–602. PMC 1433819. PMID 3061886.
- ↑ "File:Pharyngoesophageal diverticulum - alt -- very low mag.jpg - Libre Pathology".
- ↑ From en.wikipedia.org, Public Domain, <"https://commons.wikimedia.org/w/index.php?curid=1931423">