Vibrio cholerae: Difference between revisions
Shanshan Cen (talk | contribs) |
Ahmed Younes (talk | contribs) |
||
| (8 intermediate revisions by 2 users not shown) | |||
| Line 17: | Line 17: | ||
| binomial_authority = Pacini 1854 | | binomial_authority = Pacini 1854 | ||
}} | }} | ||
__NOTOC__ | |||
{{About0|Cholera}} | |||
{{CMG}} | |||
==Overview== | |||
'''''Vibrio cholerae''''' is a [[gram negative]] [[bacterium]] with a curved-rod shape that causes [[cholera]] in [[human]]s.<ref name=Sherris>{{cite book | author = Ryan KJ; Ray CG (editors) | title = Sherris Medical Microbiology | edition = 4th ed. | publisher = McGraw Hill | year = 2004 | id = ISBN 0838585299 }}</ref> ''V. cholerae'' and other species of the [[genus]] ''[[Vibrio]]'' belong to the gamma subdivision of the [[Proteobacteria]]. There are two major strains of ''V. cholerae'', classic and [[El Tor]], and numerous other serogroups. | '''''Vibrio cholerae''''' is a [[gram negative]] [[bacterium]] with a curved-rod shape that causes [[cholera]] in [[human]]s.<ref name=Sherris>{{cite book | author = Ryan KJ; Ray CG (editors) | title = Sherris Medical Microbiology | edition = 4th ed. | publisher = McGraw Hill | year = 2004 | id = ISBN 0838585299 }}</ref> ''V. cholerae'' and other species of the [[genus]] ''[[Vibrio]]'' belong to the gamma subdivision of the [[Proteobacteria]]. There are two major strains of ''V. cholerae'', classic and [[El Tor]], and numerous other serogroups. | ||
| Line 33: | Line 37: | ||
Finally, ''Vibrio cholerae'' produces what is called a ZOT toxin, termed as "Zona Occludans Toxin". This toxin specifically attacks the zona occludans or "tight" junctions joining epithelial cells. | Finally, ''Vibrio cholerae'' produces what is called a ZOT toxin, termed as "Zona Occludans Toxin". This toxin specifically attacks the zona occludans or "tight" junctions joining epithelial cells. | ||
==Differential diagnosis== | |||
Vibrio cholerae infection must be differentiated from other causes of viral, bacterial, and parasitic gastroentritis. | |||
{| style="border: 0px; font-size: 90%; margin: 3px;" align=center | |||
::* | ! colspan="3" rowspan="2" align="center" style="background:#4479BA; color: #FFFFFF;"|Organism | ||
: | ! rowspan="2" align="center" style="background:#4479BA; color: #FFFFFF;"|Age predilection | ||
! rowspan="2" align="center" style="background:#4479BA; color: #FFFFFF;"|Travel History | |||
! rowspan="2" align="center" style="background:#4479BA; color: #FFFFFF;"|Incubation Size (cell) | |||
! rowspan="2" align="center" style="background:#4479BA; color: #FFFFFF;"|Incubation Time | |||
! colspan="3" align="center" style="background:#4479BA; color: #FFFFFF;"|History and Symptoms | |||
! colspan="4" align="center" style="background:#4479BA; color: #FFFFFF;"|Diarrhea type8 | |||
! rowspan="2" align="center" style="background:#4479BA; color: #FFFFFF;"|Food source | |||
! rowspan="2" align="center" style="background:#4479BA; color: #FFFFFF;"|Specific consideration | |||
|- | |||
!style="background:#4479BA; color: #FFFFFF|Fever | |||
!style="background:#4479BA; color: #FFFFFF|N/V | |||
!style="background:#4479BA; color: #FFFFFF|Cramping Abd Pain | |||
!style="background:#4479BA; color: #FFFFFF|Small Bowel | |||
!style="background:#4479BA; color: #FFFFFF|Large Bowel | |||
!style="background:#4479BA; color: #FFFFFF|Inflammatory | |||
!style="background:#4479BA; color: #FFFFFF|Non-inflammatory | |||
|- | |||
| rowspan="4" align="center" style="background:#4479BA; color: #FFFFFF;"|'''Viral''' | |||
| colspan="2" style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Rotavirus]] | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<2 y | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<10<sup>2</sup> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<48 h | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<nowiki>-</nowiki> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Mostly in day cares, most common in winter. | |||
|- | |||
| colspan="2" style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Norovirus]] | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any age | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10 -10<sup>3</sup> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |24-48 h | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Most common cause of gastroenteritis, abdominal tenderness, | |||
|- | |||
| colspan="2" style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Adenoviridae|Adenovirus]] | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<2 y | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10<sup>5</sup> -10<sup>6</sup> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |8-10 d | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |No seasonality | |||
|- | |||
| colspan="2" style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Astrovirus]] | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<5 y | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |72-96 h | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Seafood | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Mostly during winter | |||
|- | |||
| rowspan="11" align="center" style="background:#4479BA; color: #FFFFFF;"|'''Bacterial''' | |||
| rowspan="5" style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Escherichia coli]]'' | |||
| style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[ETEC]] | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any age | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10<sup>8</sup> -10<sup>10</sup> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |24 h | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |- | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |- | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Causes travelers diarrhea, contains heat-labile toxins (LT) and heat-stable toxins (ST) | |||
|- | |||
|style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[EPEC]] | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<1 y | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<nowiki>-</nowiki> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10<sup>†</sup> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |6-12 h | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |- | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Raw beef and chicken | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|- | |||
|style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[EIEC]] | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<nowiki>-</nowiki> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10<sup>†</sup> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |24 h | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Hamburger meat and unpasteurized milk | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Similar to [[shigellosis]], can cause bloody diarrhea | |||
|- | |||
|style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[EHEC]] | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<nowiki>-</nowiki> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10 | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |3-4 d | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<nowiki>-</nowiki> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Undercooked or raw hamburger (ground beef) | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Known as ''[[Escherichia coli O157:H7|E. coli]]'' [[Escherichia coli O157:H7|O157:H7]], can cause [[Hemolytic-uremic syndrome|HUS]]/[[TTP]]. | |||
|- | |||
|style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[EAEC]] | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10<sup>10</sup> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |8-18 h | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |- | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |- | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<nowiki>-</nowiki> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |May cause prolonged or persistent diarrhea in children | |||
|- | |||
| colspan="2" style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Salmonella|Salmonella sp.]]'' | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |1 | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |6 to 72 h | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Meats, poultry, eggs, milk and dairy products, fish, shrimp, spices, yeast, coconut, sauces, freshly prepared salad. | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Can cause [[salmonellosis]] or [[typhoid fever]]. | |||
|- | |||
| colspan="2" style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Shigella|Shigella sp.]]'' | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
| style="padding: 5px 5px; background: #F5F5F5;" align="center" |- | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10 - 200 | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |8-48 h | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Raw foods, for example, lettuce, salads (potato, tuna, shrimp, macaroni, and chicken) | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Some strains produce enterotoxin and Shiga toxin similar to those produced by E. coli O157:H7 | |||
|- | |||
| colspan="2" style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Campylobacter|Campylobacter sp.]]'' | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<5 y, 15-29 y | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10<sup>4</sup> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |2-5 d | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Undercooked poultry products, unpasteurized milk and cheeses made from unpasteurized milk, vegetables, seafood and contaminated water. | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |May cause [[bacteremia]], [[Guillain-Barré syndrome]] (GBS), [[Hemolytic-uremic syndrome|hemolytic uremic syndrome]] (HUS) and recurrent [[colitis]] | |||
|- | |||
| colspan="2" style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Yersinia enterocolitica]]'' | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<10 y | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10<sup>4</sup> -10<sup>6</sup> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |1-11 d | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Meats (pork, beef, lamb, etc.), oysters, fish, crabs, and raw milk. | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |May cause [[reactive arthritis]]; [[glomerulonephritis]]; [[endocarditis]]; [[erythema nodosum]]. | |||
can mimic [[appendicitis]] and mesenteric [[lymphadenitis]]. | |||
|- | |||
| colspan="2" style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Clostridium perfringens]]'' | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |> 10<sup>6</sup> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |16 h | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Meats (especially beef and poultry), meat-containing products (e.g., gravies and stews), and Mexican foods. | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Can survive high heat, | |||
|- | |||
| colspan="2" style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Vibrio cholerae]]'' | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<nowiki>-</nowiki> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10<sup>6</sup>-10<sup>10</sup> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |24-48 h | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<nowiki>-</nowiki> | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Seafoods, including molluscan shellfish (oysters, mussels, and clams), crab, lobster, shrimp, squid, and finfish. | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |[[Hypotension]], [[tachycardia]], decreased [[Turgor|skin turgor]]. Rice-water stools | |||
|- | |||
| rowspan="7" align="center" style="background:#4479BA; color: #FFFFFF;"|'''Parasites''' | |||
| rowspan="4" style="padding: 5px 5px; background: #DCDCDC;" align="center" |Protozoa | |||
|style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Giardia lamblia]]'' | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |2-5 y | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |1 cyst | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |1-2 we | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Contaminated water | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |May cause [[malabsorption syndrome]] and severe [[weight loss]] | |||
|- | |||
|style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Entamoeba histolytica]]'' | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |4-11 y | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |<10 cysts | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |2-4 we | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Contaminated water and raw foods | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |May cause intestinal amebiasis and amebic liver abscess | |||
|- | |||
|style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Cryptosporidium parvum]]'' | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10-100 oocysts | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |7-10 d | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Juices and milk | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |May cause copious diarrhea and [[dehydration]] in patients with [[AIDS]] especially with 180 > [[CD4|CD<sub>4</sub>]] | |||
|- | |||
|style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Cyclospora cayetanensis]]'' | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |10-100 oocysts | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |7-10 d | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Fresh produce, such as raspberries, basil, and several varieties of lettuce. | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |More common in rainy areas | |||
|- | |||
| rowspan="3" style="padding: 5px 5px; background: #DCDCDC;" align="center" |Helminths | |||
|style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Trichinella]]'' [[Trichinella|spp]] | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Two viable larvae (male and female) | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |1-4 we | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
| style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Undercooked meats | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |More common in hunters or people who eat traditionally uncooked meats | |||
|- | |||
|style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Taenia (tapeworm)|Taenia]]'' [[Taenia (tapeworm)|spp]] | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |1 larva or egg | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |2-4 m | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Undercooked beef and pork | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |[[Neurocysticercosis]]: Cysts located in the brain may be asymptomatic or [[seizures]], increased [[intracranial pressure]], [[headache]]. | |||
|- | |||
|style="padding: 5px 5px; background: #DCDCDC;" align="center" |''[[Diphyllobothrium|Diphyllobothrium latum]]'' | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Any ages | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |1 larva | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |15 d | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |- | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | - | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |- | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" | + | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |Raw or undercooked fish. | |||
|style="padding: 5px 5px; background: #F5F5F5;" align="center" |May cause vitamin B<sub>12</sub> deficiency | |||
|} | |||
<br><br> | |||
<small><small> | |||
8'''Small bowel diarrhea''': watery, voluminous with less than 5 WBC/high power field | |||
'''Large bowel diarrhea''': Mucousy and/or bloody with less volume and more than 10 WBC/high power field<br> | |||
† It could be as high as 1000 based on patient's immunity system. | |||
</small></small> | |||
'''The table below summarizes the findings that differentiate inflammatory causes of chronic diarrhea'''<ref name="pmid8209928">{{cite journal| author=Konvolinka CW| title=Acute diverticulitis under age forty. | journal=Am J Surg | year= 1994 | volume= 167 | issue= 6 | pages= 562-5 | pmid=8209928 | doi= | pmc= | url=https://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=8209928 }} </ref><ref name="pmid16151544">{{cite journal| author=Silverberg MS, Satsangi J, Ahmad T, Arnott ID, Bernstein CN, Brant SR et al.| title=Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: report of a Working Party of the 2005 Montreal World Congress of Gastroenterology. | journal=Can J Gastroenterol | year= 2005 | volume= 19 Suppl A | issue= | pages= 5A-36A | pmid=16151544 | doi= | pmc= | url=https://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=16151544 }} </ref><ref name="pmid16698746">{{cite journal| author=Satsangi J, Silverberg MS, Vermeire S, Colombel JF| title=The Montreal classification of inflammatory bowel disease: controversies, consensus, and implications. | journal=Gut | year= 2006 | volume= 55 | issue= 6 | pages= 749-53 | pmid=16698746 | doi=10.1136/gut.2005.082909 | pmc=1856208 | url=https://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=16698746 }} </ref><ref name="pmid12700377">{{cite journal| author=Haque R, Huston CD, Hughes M, Houpt E, Petri WA| title=Amebiasis. | journal=N Engl J Med | year= 2003 | volume= 348 | issue= 16 | pages= 1565-73 | pmid=12700377 | doi=10.1056/NEJMra022710 | pmc= | url=https://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=12700377 }} </ref><ref name="pmid12700377">{{cite journal| author=Haque R, Huston CD, Hughes M, Houpt E, Petri WA| title=Amebiasis. | journal=N Engl J Med | year= 2003 | volume= 348 | issue= 16 | pages= 1565-73 | pmid=12700377 | doi=10.1056/NEJMra022710 | pmc= | url=https://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=12700377 }} </ref> | |||
{| class="wikitable" | |||
!Cause | |||
!History | |||
!Laboratory findings | |||
!Diagnosis | |||
!Treatment | |||
|- | |||
|[[Diverticulitis]] | |||
| | |||
* [[Bloody diarrhea]] | |||
* Left lower quadrant [[abdominal pain]] | |||
* [[Abdominal tenderness]] on [[physical examination]] | |||
* Low grade [[fever]] | |||
| | |||
* [[Leukocytosis]] | |||
* Elevated serum [[amylase]] and [[lipase]] | |||
* [[Sterile]] [[pyuria]] on [[urinalysis]] | |||
|Abdominal [[CT scan]] with oral and intravenous [[Contrast medium|(IV) contrast]] | |||
|bowel rest, [[Intravenous fluids|IV fluid]] resuscitation, and [[Broad-spectrum antibiotic|broad-spectrum antimicrobial therapy]] which covers [[Anaerobic organism|anaerobic]] [[bacteria]] and [[gram-negative]] [[Bacteria|rods]] | |||
|- | |||
|[[Ulcerative colitis]] | |||
| | |||
* [[Diarrhea]] mixed with blood and [[mucus]], of gradual onset. | |||
* Signs of [[weight loss]] | |||
* [[Rectal pain|Rectal urgency]] | |||
* [[Tenesmus]] | |||
* [[Blood]] is often noticed on underwear | |||
* Different degrees of [[abdominal pain]] | |||
| | |||
* [[Anemia]] | |||
* [[Thrombocytosis]] | |||
* A high [[platelet]] count | |||
* Elevated [[ESR]] (>30mm/hr) | |||
* Low [[albumin]] | |||
|[[Endoscopy]] | |||
|Induction of [[Remission (medicine)|remission]] with [[mesalamine]] and [[corticosteroids]] followed by the administration of [[sulfasalazine]] and [[Mercaptopurine|6-Mercaptopurine]] depending on the severity of the [[disease]]. | |||
|- | |||
|[[Entamoeba histolytica]] | |||
| | |||
* [[Abdominal cramps]] | |||
* [[Diarrhea]] | |||
** Passage of 3 - 8 semiformed [[stools]] per day | |||
** Passage of soft [[stools]] with [[mucus]] and occasional [[blood]] | |||
* [[Fatigue]] | |||
* [[Intestinal]] gas (excessive [[flatus]]) | |||
* [[Rectal pain]] while having a [[bowel movement]] ([[tenesmus]]) | |||
* Unintentional [[weight loss]] | |||
|cysts shed with the stool | |||
|detects ameba [[DNA]] in feces | |||
|[[Amebic dysentery]] | |||
* [[Metronidazole]] 500-750mg three times a day for 5-10 days | |||
* [[Tinidazole]] 2g once a day for 3 days is an alternative to [[metronidazole]] | |||
Luminal amebicides for ''[[E. histolytica]]'' in the [[colon]]: | |||
* [[Paromomycin]] 500mg three times a day for 10 days | |||
* [[Diloxanide furoate]] 500mg three times a day for 10 days | |||
* [[Iodoquinol]] 650mg three times a day for 20 days | |||
For [[Amoebiasis|amebic liver abscess]]: | |||
* [[Metronidazole]] 400mg three times a day for 10 days | |||
* [[Tinidazole]] 2g once a day for 6 days is an alternative to [[metronidazole]] | |||
* [[Diloxanide furoate]] 500mg three times a day for 10 days must always be given afterwards. | |||
|} | |||
==References== | ==References== | ||
| Line 73: | Line 491: | ||
[[nl:Vibrio cholerae]] | [[nl:Vibrio cholerae]] | ||
[[ja:コレラ菌]] | [[ja:コレラ菌]] | ||
[[sk:Vibrio cholerae | [[sk:Vibrio cholerae] | ||
[[zh:霍亂弧菌]] | [[zh:霍亂弧菌]] | ||
{{WikiDoc Help Menu}} | {{WikiDoc Help Menu}} | ||
{{WikiDoc Sources}} | {{WikiDoc Sources}} | ||
Latest revision as of 01:21, 11 September 2017
| Vibrio cholerae | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
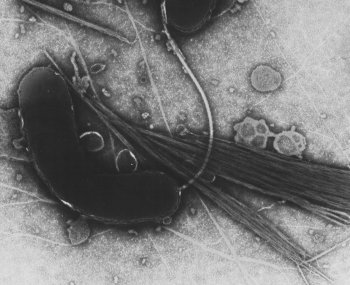 TEM image
| ||||||||||||||
| Scientific classification | ||||||||||||||
| ||||||||||||||
| Binomial name | ||||||||||||||
| Vibrio cholerae Pacini 1854 |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Vibrio cholerae is a gram negative bacterium with a curved-rod shape that causes cholera in humans.[1] V. cholerae and other species of the genus Vibrio belong to the gamma subdivision of the Proteobacteria. There are two major strains of V. cholerae, classic and El Tor, and numerous other serogroups.
V. cholerae was first isolated as the cause of cholera by Italian anatomist Filippo Pacini in 1854, but his discovery was not widely known until Robert Koch, working independently thirty years later, publicized the knowledge and the means of fighting the disease.
Habitat
V. cholerae occurs naturally in the plankton of fresh, brackish, and salt water, attached primarily to copepods in the zooplankton. Coastal cholera outbreaks typically follow zooplankton blooms. This makes cholera a typical zoonosis.
Pathogenesis
V. cholerae colonizes the gastrointestinal tract, where it adheres to villous absorptive cells via pili, and secretes a binary toxin, called cholera toxin (CT). The two CT subunits are named A and B, and are synthesised in a 1:5 ratio. B subunits bind and internalize A subunits, which are processed to A1. The A1 form catalyses ADP ribosylation from NAD to the regulatory component of adenylate cyclase, thereby activating it. Increased adenylate cyclase activity increases cyclic AMP (cAMP) synthesis causing massive fluid and electrolyte efflux, resulting in diarrhea.
CT is encoded by the ctxAB genes on a specific filamentous bacteriophage. Transduction of this phage is dependent upon bacterial expression of the Toxin Coregulated Pilus (TCP), which is encoded by the V. cholerae pathogenicity island (VPI). VPI is generally only present in virulent strains and is laterally transferred. VPI was originally thought to encode a filamentous phage responsible for transfer. This theory was discredited by a study of 46 diverse V. cholerae isolates which found no evidence of VPI phage production. The generalized transduction phage CP-T1 has been shown to transduce the entire VPI which is then integrated at the same chromosomal location. Also, VPI has been shown to excise and circularize to produce pVPI via a specialised mechanism involving VPI-encoded recombinases. It is not known whether pVPI is involved in CP-T1 transduction or if it is perhaps a component of an alternative VPI mobilization mechanism.
Additionally, it produces two different proteases called chitinase and mucinase. Chitinase is responsible for the ability of Vibrio cholerae to enter copapods. Mucinase is a non-specific protease that assists entry into the human gastro-intestinal tract.
Finally, Vibrio cholerae produces what is called a ZOT toxin, termed as "Zona Occludans Toxin". This toxin specifically attacks the zona occludans or "tight" junctions joining epithelial cells.
Differential diagnosis
Vibrio cholerae infection must be differentiated from other causes of viral, bacterial, and parasitic gastroentritis.
| Organism | Age predilection | Travel History | Incubation Size (cell) | Incubation Time | History and Symptoms | Diarrhea type8 | Food source | Specific consideration | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Fever | N/V | Cramping Abd Pain | Small Bowel | Large Bowel | Inflammatory | Non-inflammatory | |||||||||
| Viral | Rotavirus | <2 y | - | <102 | <48 h | + | + | - | + | + | - | Mostly in day cares, most common in winter. | |||
| Norovirus | Any age | - | 10 -103 | 24-48 h | + | + | + | + | + | - | Most common cause of gastroenteritis, abdominal tenderness, | ||||
| Adenovirus | <2 y | - | 105 -106 | 8-10 d | + | + | + | + | + | - | No seasonality | ||||
| Astrovirus | <5 y | - | 72-96 h | + | + | + | + | + | Seafood | Mostly during winter | |||||
| Bacterial | Escherichia coli | ETEC | Any age | + | 108 -1010 | 24 h | - | + | + | + | + | - | Causes travelers diarrhea, contains heat-labile toxins (LT) and heat-stable toxins (ST) | ||
| EPEC | <1 y | - | 10† | 6-12 h | - | + | + | + | + | Raw beef and chicken | - | ||||
| EIEC | Any ages | - | 10† | 24 h | + | + | + | + | + | Hamburger meat and unpasteurized milk | Similar to shigellosis, can cause bloody diarrhea | ||||
| EHEC | Any ages | - | 10 | 3-4 d | - | + | + | + | + | Undercooked or raw hamburger (ground beef) | Known as E. coli O157:H7, can cause HUS/TTP. | ||||
| EAEC | Any ages | + | 1010 | 8-18 h | - | - | + | + | + | - | May cause prolonged or persistent diarrhea in children | ||||
| Salmonella sp. | Any ages | + | 1 | 6 to 72 h | + | + | + | + | + | Meats, poultry, eggs, milk and dairy products, fish, shrimp, spices, yeast, coconut, sauces, freshly prepared salad. | Can cause salmonellosis or typhoid fever. | ||||
| Shigella sp. | Any ages | - | 10 - 200 | 8-48 h | + | + | + | + | + | Raw foods, for example, lettuce, salads (potato, tuna, shrimp, macaroni, and chicken) | Some strains produce enterotoxin and Shiga toxin similar to those produced by E. coli O157:H7 | ||||
| Campylobacter sp. | <5 y, 15-29 y | - | 104 | 2-5 d | + | + | + | + | + | Undercooked poultry products, unpasteurized milk and cheeses made from unpasteurized milk, vegetables, seafood and contaminated water. | May cause bacteremia, Guillain-Barré syndrome (GBS), hemolytic uremic syndrome (HUS) and recurrent colitis | ||||
| Yersinia enterocolitica | <10 y | - | 104 -106 | 1-11 d | + | + | + | + | + | Meats (pork, beef, lamb, etc.), oysters, fish, crabs, and raw milk. | May cause reactive arthritis; glomerulonephritis; endocarditis; erythema nodosum.
can mimic appendicitis and mesenteric lymphadenitis. | ||||
| Clostridium perfringens | Any ages | > 106 | 16 h | - | - | + | + | + | Meats (especially beef and poultry), meat-containing products (e.g., gravies and stews), and Mexican foods. | Can survive high heat, | |||||
| Vibrio cholerae | Any ages | - | 106-1010 | 24-48 h | - | + | + | + | + | Seafoods, including molluscan shellfish (oysters, mussels, and clams), crab, lobster, shrimp, squid, and finfish. | Hypotension, tachycardia, decreased skin turgor. Rice-water stools | ||||
| Parasites | Protozoa | Giardia lamblia | 2-5 y | + | 1 cyst | 1-2 we | - | - | + | + | + | Contaminated water | May cause malabsorption syndrome and severe weight loss | ||
| Entamoeba histolytica | 4-11 y | + | <10 cysts | 2-4 we | - | + | + | + | + | Contaminated water and raw foods | May cause intestinal amebiasis and amebic liver abscess | ||||
| Cryptosporidium parvum | Any ages | - | 10-100 oocysts | 7-10 d | + | + | + | + | + | Juices and milk | May cause copious diarrhea and dehydration in patients with AIDS especially with 180 > CD4 | ||||
| Cyclospora cayetanensis | Any ages | + | 10-100 oocysts | 7-10 d | - | + | + | + | + | Fresh produce, such as raspberries, basil, and several varieties of lettuce. | More common in rainy areas | ||||
| Helminths | Trichinella spp | Any ages | - | Two viable larvae (male and female) | 1-4 we | - | + | + | + | + | Undercooked meats | More common in hunters or people who eat traditionally uncooked meats | |||
| Taenia spp | Any ages | - | 1 larva or egg | 2-4 m | - | + | + | + | + | Undercooked beef and pork | Neurocysticercosis: Cysts located in the brain may be asymptomatic or seizures, increased intracranial pressure, headache. | ||||
| Diphyllobothrium latum | Any ages | - | 1 larva | 15 d | - | - | - | + | + | Raw or undercooked fish. | May cause vitamin B12 deficiency | ||||
8Small bowel diarrhea: watery, voluminous with less than 5 WBC/high power field
Large bowel diarrhea: Mucousy and/or bloody with less volume and more than 10 WBC/high power field
† It could be as high as 1000 based on patient's immunity system.
The table below summarizes the findings that differentiate inflammatory causes of chronic diarrhea[2][3][4][5][5]
| Cause | History | Laboratory findings | Diagnosis | Treatment |
|---|---|---|---|---|
| Diverticulitis |
|
|
Abdominal CT scan with oral and intravenous (IV) contrast | bowel rest, IV fluid resuscitation, and broad-spectrum antimicrobial therapy which covers anaerobic bacteria and gram-negative rods |
| Ulcerative colitis |
|
|
Endoscopy | Induction of remission with mesalamine and corticosteroids followed by the administration of sulfasalazine and 6-Mercaptopurine depending on the severity of the disease. |
| Entamoeba histolytica |
|
cysts shed with the stool | detects ameba DNA in feces | Amebic dysentery
Luminal amebicides for E. histolytica in the colon:
For amebic liver abscess:
|
References
- ↑ Ryan KJ; Ray CG (editors) (2004). Sherris Medical Microbiology (4th ed. ed.). McGraw Hill. ISBN 0838585299.
- ↑ Konvolinka CW (1994). "Acute diverticulitis under age forty". Am J Surg. 167 (6): 562–5. PMID 8209928.
- ↑ Silverberg MS, Satsangi J, Ahmad T, Arnott ID, Bernstein CN, Brant SR; et al. (2005). "Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: report of a Working Party of the 2005 Montreal World Congress of Gastroenterology". Can J Gastroenterol. 19 Suppl A: 5A–36A. PMID 16151544.
- ↑ Satsangi J, Silverberg MS, Vermeire S, Colombel JF (2006). "The Montreal classification of inflammatory bowel disease: controversies, consensus, and implications". Gut. 55 (6): 749–53. doi:10.1136/gut.2005.082909. PMC 1856208. PMID 16698746.
- ↑ 5.0 5.1 Haque R, Huston CD, Hughes M, Houpt E, Petri WA (2003). "Amebiasis". N Engl J Med. 348 (16): 1565–73. doi:10.1056/NEJMra022710. PMID 12700377.
External links
bn:ভিব্রিও কলেরী
de:Vibrio cholerae
it:Vibrio cholerae
he:Vibrio cholerae
nl:Vibrio cholerae
[[sk:Vibrio cholerae]