SLE resident survival guide: Difference between revisions
Iqra Qamar (talk | contribs) |
Aditya Ganti (talk | contribs) No edit summary |
||
| (20 intermediate revisions by one other user not shown) | |||
| Line 21: | Line 21: | ||
__NOTOC__ | __NOTOC__ | ||
{{CMG}}; | {{CMG}} ; {{AE}} {{IQ}} ; {{ADG}} | ||
== Overview == | == Overview == | ||
| Line 47: | Line 47: | ||
=== Diagnostic criteria: === | === Diagnostic criteria: === | ||
<small> | |||
In 2012, Systemic Lupus International Collaboration Criteria (SLICC) developed a new criteria for SLE diagnosis. SLICC criteria for the classification of [[systemic lupus erythematosus]] was developed based on the old ACR criteria for the classification of [[systemic lupus erythematosus]] to address a more sensitive diagnostic criteria and also to cover weaknesses of the previous ACR criteria.<ref name="pmid7138600">{{cite journal |vauthors=Tan EM, Cohen AS, Fries JF, Masi AT, McShane DJ, Rothfield NF, Schaller JG, Talal N, Winchester RJ |title=The 1982 revised criteria for the classification of systemic lupus erythematosus |journal=Arthritis Rheum. |volume=25 |issue=11 |pages=1271–7 |year=1982 |pmid=7138600 |doi= |url=}}</ref><ref name="pmid9324032">{{cite journal |vauthors=Hochberg MC |title=Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus |journal=Arthritis Rheum. |volume=40 |issue=9 |pages=1725 |year=1997 |pmid=9324032 |doi=10.1002/1529-0131(199709)40:9<1725::AID-ART29>3.0.CO;2-Y |url=}}</ref> | |||
Based on SLICC criteria, diagnosis of SLE is defined as:<ref name="pmid22553077">{{cite journal |vauthors=Petri M, Orbai AM, Alarcón GS, Gordon C, Merrill JT, Fortin PR, Bruce IN, Isenberg D, Wallace DJ, Nived O, Sturfelt G, Ramsey-Goldman R, Bae SC, Hanly JG, Sánchez-Guerrero J, Clarke A, Aranow C, Manzi S, Urowitz M, Gladman D, Kalunian K, Costner M, Werth VP, Zoma A, Bernatsky S, Ruiz-Irastorza G, Khamashta MA, Jacobsen S, Buyon JP, Maddison P, Dooley MA, van Vollenhoven RF, Ginzler E, Stoll T, Peschken C, Jorizzo JL, Callen JP, Lim SS, Fessler BJ, Inanc M, Kamen DL, Rahman A, Steinsson K, Franks AG, Sigler L, Hameed S, Fang H, Pham N, Brey R, Weisman MH, McGwin G, Magder LS |title=Derivation and validation of the Systemic Lupus International Collaborating Clinics classification criteria for systemic lupus erythematosus |journal=Arthritis Rheum. |volume=64 |issue=8 |pages=2677–86 |year=2012 |pmid=22553077 |pmc=3409311 |doi=10.1002/art.34473 |url=}}</ref> | |||
* Meeting at least 4 of 17 criteria, including at least 1 of the 11 clinical criteria and one of the six [[Immunological|immunologic]] criteria | |||
'''OR''' | |||
* Biopsy-proven [[nephritis]] compatible with [[SLE]] in the presence of [[Antinuclear antibodies|antinuclear antibodies (ANA)]] or [[Double stranded DNA antibody|anti-double-stranded DNA]] (dsDNA) [[antibodies]] | |||
</small> | |||
'''A criterion is considered positive if one or more of the observations listed in the definition for the criterion are present in the patient. A criterion should only be counted once, regardless of the number of observations in the definition that the patient presents with.''' | |||
<small> | |||
{| class="wikitable" | |||
! align="center" style="background: #4479BA; color: #FFFFFF; " |Category | |||
! align="center" style="background: #4479BA; color: #FFFFFF; " |Criterion | |||
! align="center" style="background: #4479BA; color: #FFFFFF; " |Definition | |||
|- | |||
| rowspan="8" |<small>Clinical</small> | |||
! style="background: #DCDCDC; " | Acute cutaneous lupus | |||
| | |||
* Lupus [[malar rash]] | |||
** Fixed [[erythema]], flat or raised, over the [[malar]] eminences, tending to spare the [[nasolabial folds]] | |||
* [[Bullous]] lupus | |||
* [[Toxic epidermal necrolysis]] variant of SLE | |||
* [[Maculopapular rash|Maculopapular]] lupus [[rash]] | |||
* [[Photosensitive]] lupus [[rash]] (in the absence of [[dermatomyositis]]); | |||
** Skin [[rash]] as a result of unusual reaction to sunlight, by patient history or physician observation | |||
* Subacute cutaneous lupus | |||
** Nonindurated psoriaform and/or annular polycyclic [[lesions]] that resolve without [[scarring]], although occasionally with [[Postinflammatory hypopigmentation|postinflammatory dyspigmentation]] or [[Telangiectasia|telangiectasias]] | |||
|- | |||
! style="background: #DCDCDC; " |Chronic cutaneous lupus | |||
| | |||
* Classic [[Discoid lupus|discoid rash]] | |||
** Localized (above the neck) | |||
** Generalized (above and below the neck) | |||
** [[Hypertrophic]] (verrucous) lupus | |||
** Lupus [[panniculitis]] (profundus) | |||
** [[Mucosal]] lupus | |||
** [[Lupus erythematosus]] tumidus | |||
** Chilblains lupus OR | |||
** Discoid lupus[[Lichen planus|/lichen planus]] overlap | |||
|- | |||
! style="background: #DCDCDC; " |Nonscarring [[alopecia]] | |||
| | |||
* Diffuse thinning or hair fragility with visible broken hairs (in the absence of other causes, such as [[alopecia areata]], drugs, [[iron deficiency]], and [[androgenic alopecia]]) | |||
|- | |||
! style="background: #DCDCDC; " |[[Oral ulcer|Oral]] or nasal ulcers | |||
| | |||
* [[Palate]], [[buccal]], [[tongue]], or nasal [[ulcers]] (in the absence of other causes, such as [[vasculitis]], [[Behçet's disease]], [[infection]], [[inflammatory bowel disease]], [[reactive arthritis]], and acidic foods) | |||
|- | |||
! style="background: #DCDCDC; " |[[Arthralgia|Joint disease]] | |||
| | |||
* [[Synovitis]] involving two or more [[joints]], characterized by [[swelling]] or effusion | |||
* [[Tenderness]] in two or more [[joints]] and at least 30 minutes of morning stiffness | |||
|- | |||
! style="background: #DCDCDC; " |[[Serositis]] | |||
| | |||
* Typical [[pleurisy]] for more than one day, [[Pleural effusion|pleural effusions]], or [[pleural]] rub | |||
* Typical pericardial pain (pain with recumbency improved by sitting forward) for more than one day, [[pericardial effusion]], pericardial rub, or [[pericarditis]] by [[electrocardiography]] in the absence of other causes, such as [[infection]], [[uremia]], and [[Dressler's syndrome]] | |||
|- | |||
! style="background: #DCDCDC; " |[[Renal]] | |||
| | |||
* Urine protein-to-[[creatinine]] ratio (or 24-hour urine protein) representing 500 mg protein/24 hours | |||
* [[Red blood cell]] casts | |||
|- | |||
! style="background: #DCDCDC; " |[[Neurological|Neurologic]] | |||
| | |||
* [[Seizure|Seizures]] | |||
* [[Psychosis]] | |||
* [[Mononeuritis multiplex]] (in the absence of other known causes, such as primary [[vasculitis]]) | |||
* [[Myelitis]] | |||
* [[Peripheral neuropathy|Peripheral]] or [[Neuropathy|cranial neuropathy]] (in the absence of other known causes, such as primary [[vasculitis]], [[infection]], and [[diabetes mellitus]]) | |||
* [[Confusion|Acute confusional state]] (in the absence of other causes, including toxic/metabolic, [[uremia]], drugs) | |||
|- | |||
| rowspan="3" |<small>[[Hematologic]]</small> | |||
! style="background: #DCDCDC; " |[[Hemolytic anemia]] | |||
| | |||
* [[Hemoglobin]] less than 12 g/dL in females and 13 g/dL in males | |||
|- | |||
! style="background: #DCDCDC; " |[[Leukopenia]] or [[lymphopenia]] | |||
| | |||
* [[Leukopenia]] (<4000/mm3 at least once) (in the absence of other known causes, such as [[Felty's syndrome]], [[drugs]], and [[portal hypertension]]) | |||
* [[Lymphopenia]] (<1000/mm3 at least once) (in the absence of other known causes, such as [[glucocorticoids]], [[drugs]], and [[infection]]) | |||
|- | |||
! style="background: #DCDCDC; " |[[Thrombocytopenia]] | |||
| | |||
* [[Thrombocytopenia]] (<100,000/mm3) at least once in the absence of other known causes, such as [[drugs]], [[portal hypertension]], and [[thrombotic thrombocytopenic purpura]] | |||
|- | |||
| rowspan="6" |<small>[[Immunological|Immunologic]]</small> | |||
! style="background: #DCDCDC; " |[[ANA]] | |||
| | |||
* [[ANA]] level above laboratory reference range | |||
|- | |||
! style="background: #DCDCDC; " |[[Anti-dsDNA antibody|Anti-dsDNA]] | |||
| | |||
* [[Anti-dsDNA antibody]] level above laboratory reference range (or >twofold the reference range if tested by [[Enzyme linked immunosorbent assay (ELISA)|ELISA]]) | |||
|- | |||
! style="background: #DCDCDC; " |Anit-SM | |||
| | |||
* Presence of [[antibody]] to [[Smith antigen|Sm nuclear antigen]] | |||
|- | |||
! style="background: #DCDCDC; " |[[Antiphospholipid antibody|Antiphospholipid]] | |||
| | |||
* [[Antiphospholipid antibodies|Antiphospholipid antibody]] positivity as determined by any of the following: | |||
** Positive test result for [[lupus anticoagulant]] | |||
** False-positive test result for [[rapid plasma reagin]] | |||
** Medium- or high-titer [[anticardiolipin antibody]] level ([[IgA]], [[IgG]], or [[IgM]]) | |||
** Positive test result for anti-beta 2-glycoprotein I ([[IgA]], [[IgG]], or [[IgM]]) | |||
|- | |||
! style="background: #DCDCDC; " |Low [[complement]] | |||
| | |||
* Low [[C3 glomerular disease|C3]] | |||
* Low [[C4 disease|C4]] | |||
* Low CH50 | |||
|- | |||
! style="background: #DCDCDC; " |[[Coombs' Test|Direct Coombs' test]] | |||
| | |||
* [[Coombs' Test|Direct Coombs' test]] in the absence of [[hemolytic anemia]] | |||
|} | |||
</small> | |||
=== Complete diagnostic approach: === | === Complete diagnostic approach: === | ||
<div style="font-size: 90%;"> | |||
{{Familytree/start}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| A01 | | |A01=<div style="padding: 10px;"> | |||
==SLE Presentation== | |||
*[[Fatigue]]<ref name="pmid11085805">{{cite journal |vauthors=Tench CM, McCurdie I, White PD, D'Cruz DP |title=The prevalence and associations of fatigue in systemic lupus erythematosus |journal=Rheumatology (Oxford) |volume=39 |issue=11 |pages=1249–54 |year=2000 |pmid=11085805 |doi= |url=}}</ref><ref name="pmid7779127">{{cite journal |vauthors=McKinley PS, Ouellette SC, Winkel GH |title=The contributions of disease activity, sleep patterns, and depression to fatigue in systemic lupus erythematosus. A proposed model |journal=Arthritis Rheum. |volume=38 |issue=6 |pages=826–34 |year=1995 |pmid=7779127 |doi= |url=}}</ref><ref name="pmid9598886">{{cite journal |vauthors=Wang B, Gladman DD, Urowitz MB |title=Fatigue in lupus is not correlated with disease activity |journal=J. Rheumatol. |volume=25 |issue=5 |pages=892–5 |year=1998 |pmid=9598886 |doi= |url=}}</ref> | |||
*[[Fever]] | |||
*[[Myalgia]] | |||
*Joint [[tenderness]] | |||
*[[Muscle weakness]] | |||
*[[Weight]] changes | |||
==Less common Presentation== | |||
*Dysphagia | |||
*Peptic ulcer disease | |||
*Intestinal pseudo-obstruction | |||
*Protein-losing enteropathy | |||
*Acute pancreatitis | |||
*Pneumonitis | |||
*Pleuritis | |||
*Pulmonary hemorrhage | |||
*Interstitial lung disease | |||
*Pulmonary emboli | |||
*Pulmonary hypertension | |||
*Pericarditis | |||
*Myocarditis | |||
*Seizures | |||
*Stroke | |||
*Psychosis | |||
*Nephrotic syndrome | |||
</div>}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| |!| | | |}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| A01 | | |A01=<div style="padding: 10px;"> | |||
==Focused History== | |||
* Onset, duration and progression of symptoms | |||
* History of [[Weight change|weight changes]] (gain or loss) | |||
* [[Anorexia]] | |||
* [[Arthritis]], [[Arthralgia|arthralgias]], or [[muscle pain]] | |||
* Morning [[stiffness]] | |||
* [[Skin rashes]] and their association to flare ups, especially after exposure to sunlight | |||
* [[Medications]] and their association to flare ups | |||
* [[Infections]] especially [[mononucleosis]] | |||
* Sores in the mouth, nose, or other [[Mucous membrane|mucous membranes]] | |||
* Symptoms of other organ failure | |||
** [[Renal failure]]: Recent peripheral [[edema]] and [[weight gain]] | |||
** [[Cardiac]] involvement: [[Tachycardia]], [[dyspnea]], [[Chest pain|chest pains]] | |||
* History of having a pet | |||
* [[Hair loss]] | |||
* Job history | |||
* [[Comorbid|Co-morbid]] conditions include: | |||
** Other [[Rheumatologic disease|rheumatologic]] and [[autoimmune diseases]] | |||
** [[Hypertension]] | |||
** [[Diabetes]], [[immunodeficiency]] | |||
* [[Seizure|Seizures]], or other [[nervous system]] symptoms | |||
* [[Family history]] of [[Rheumatologic disease|rheumatologic diseases]] | |||
</div>}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| |!| | | |}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| A01 | | |A01=<div style="padding: 10px;"> | |||
==Physical Examination== | |||
===Appearance of the Patient=== | |||
*Patient appears well in the earlier stages of the disease | |||
*Patient appears ill in the late stages of the disease due to multi-organ involvement | |||
===Vital Signs=== | |||
*[[Fever]] higher than 38 after the exclusion of [[infection]] | |||
*[[Tachycardia]]/[[bradycardia]] depends on the accompanying complication | |||
*[[Tachypnea]]/[[bradypnea]] depends on the accompanying complication | |||
=== Skin<ref name="pmid25077888">{{cite journal |vauthors=Parodi A, Cozzani E |title=Cutaneous manifestations of lupus erythematosus |journal=G Ital Dermatol Venereol |volume=149 |issue=5 |pages=549–54 |year=2014 |pmid=25077888 |doi= |url=}}</ref><ref name="pmid26985173">{{cite journal |vauthors=Szczęch J, Rutka M, Samotij D, Zalewska A, Reich A |title=Clinical characteristics of cutaneous lupus erythematosus |journal=Postepy Dermatol Alergol |volume=33 |issue=1 |pages=13–7 |year=2016 |pmid=26985173 |pmc=4793050 |doi=10.5114/pdia.2014.44031 |url=}}</ref><ref name="pmid19824738">{{cite journal |vauthors=Walling HW, Sontheimer RD |title=Cutaneous lupus erythematosus: issues in diagnosis and treatment |journal=Am J Clin Dermatol |volume=10 |issue=6 |pages=365–81 |year=2009 |pmid=19824738 |doi=10.2165/11310780-000000000-00000 |url=}}</ref> === | |||
*[[Cyanosis]] | |||
**Secondary to [[respiratory]] complications | |||
*[[Jaundice]] | |||
**Secondary to [[hepatitis]] | |||
*[[Pallor]] | |||
**Secondary to [[anemia]] | |||
*Generalised [[erythema]] | |||
*[[Bruises]] | |||
**Secondary to [[thrombocytopenia]] | |||
*[[Urticaria]] | |||
*[[Bullous|Bullous lesions]] | |||
*[[Sclerodactyly]] | |||
*Skin [[Ulcerations|ulceration]] | |||
*[[Malar rash]]: the classic lupus ‘butterfly’ rash | |||
** [[Erythema|Erythematous]], elevated [[Lesions|lesion]], [[Pruritis|pruritic]] or painful, in a [[malar]] distribution, commonly precipitated by exposure to sunlight | |||
* Annular or psoriasiform skin [[lesions]] | |||
** Small, [[erythematous]], slightly scaly [[papules]] that evolve into either a psoriasiform (papulosquamous) or annular form and tend to involve shoulders, forearms, neck, and upper torso | |||
* [[Scarring]] [[chronic]] [[alopecia]] | |||
** Mostly present on face, neck, and scalp | |||
* [[Telangiectasias]] | |||
* Dyspigmentation ([[hyperpigmentation]] or [[hypopigmentation]]) of skin in [[scar]] places | |||
* Follicular plugging | |||
** Discrete, [[erythematous]], slightly infiltrated [[plaques]] covered by a well-formed adherent scale that extends into dilated [[hair follicles]] | |||
* [[Nodules]] | |||
** Can be firm (Lupus profundus) and painful | |||
* Photodistributed [[lesions]] with chronic pink indurated plaques or broad [[lesions]] that are slow to heal (more seen in lupus tumidus) | |||
* Thin hair that easily fractures (lupus hair) | |||
* Irregularly shaped raised white plaques, areas of erythema, silvery white scarred [[lesions]], and [[ulcers]] with surrounding [[erythema]] on the soft or hard palate or buccal [[mucosa]] | |||
* Periungual [[erythema]] | |||
** Dilated tortuous loops of [[capillaries]] and a prominent subcapillary venous plexus along | |||
** Involves the base of the nail and edges of the upper [[eyelid]] | |||
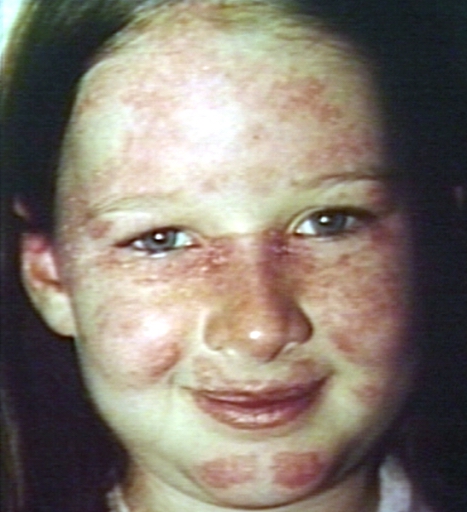
[[File:Systemic lupus erythematosus 055.jpg|300px]] | |||
'''For more pictures of the rash presentation in lupus, click [[Systemic lupus eryhthematosus physical examination:Gallery|here]].''' | |||
===HEENT=== | |||
*[[Ophthalmology]]<ref name="pmid26367085">{{cite journal |vauthors=Preble JM, Silpa-archa S, Foster CS |title=Ocular involvement in systemic lupus erythematosus |journal=Curr Opin Ophthalmol |volume=26 |issue=6 |pages=540–5 |year=2015 |pmid=26367085 |doi=10.1097/ICU.0000000000000209 |url=}}</ref><ref name="pmid25904124">{{cite journal |vauthors=Silpa-archa S, Lee JJ, Foster CS |title=Ocular manifestations in systemic lupus erythematosus |journal=Br J Ophthalmol |volume=100 |issue=1 |pages=135–41 |year=2016 |pmid=25904124 |doi=10.1136/bjophthalmol-2015-306629 |url=}}</ref> | |||
**[[Nystagmus]] | |||
**Visual [[Retinal|retinal changes]] from systemic lupus erythematosus cytoid bodies, [[Retina|retinal]] [[haemorrhages]], serous exudate or [[haemorrhage]] in the [[choroid]], [[optic neuritis]] (not due to [[hypertension]], drugs or [[infection]]) | |||
**[[Cataract]] | |||
**[[Optic nerve atrophy]] | |||
**[[Icterus|Icteric sclera]] | |||
**[[Cotton wool spots]] in the [[retina]] in [[Ophthalmoscopy|ophthalmoscopic exam]] | |||
*Nasal [[ulcers]]<ref name="pmid1526055">{{cite journal |vauthors=Robson AK, Burge SM, Millard PR |title=Nasal mucosal involvement in lupus erythematosus |journal=Clin Otolaryngol Allied Sci |volume=17 |issue=4 |pages=341–3 |year=1992 |pmid=1526055 |doi= |url=}}</ref> | |||
**Mostly painless | |||
**Mostly in lower [[nasal septum]] and [[bilateral]] and parallel | |||
**Nasal perforation secondary to [[vasculitis]] may happen rarely | |||
*Oral [[ulcers]]<ref name="pmid23780804">{{cite journal |vauthors=Anyanwu CO, Ang CC, Werth VP |title=Oral mucosal involvement in bullous lupus |journal=Arthritis Rheum. |volume=65 |issue=10 |pages=2622 |year=2013 |pmid=23780804 |pmc=4333153 |doi=10.1002/art.38051 |url=}}</ref><ref name="pmid23248469">{{cite journal |vauthors=Ranginwala AM, Chalishazar MM, Panja P, Buddhdev KP, Kale HM |title=Oral discoid lupus erythematosus: A study of twenty-one cases |journal=J Oral Maxillofac Pathol |volume=16 |issue=3 |pages=368–73 |year=2012 |pmid=23248469 |pmc=3519212 |doi=10.4103/0973-029X.102487 |url=}}</ref> | |||
**Mostly painless | |||
**White plaques with areas of [[erythema]], or punched-out erosions or ulcers with surrounding [[erythema]] on the soft or hard palate or [[buccal mucosa]] | |||
===Neck<ref name="pmid19107085">{{cite journal |vauthors=Melikoglu MA, Melikoglu M |title=The clinical importance of lymphadenopathy in systemic lupus erythematosus |journal=Acta Reumatol Port |volume=33 |issue=4 |pages=402–6 |year=2008 |pmid=19107085 |doi= |url=}}</ref><ref name="pmid24722263">{{cite journal |vauthors=Sacre K, Escoubet B, Pasquet B, Chauveheid MP, Zennaro MC, Tubach F, Papo T |title=Increased arterial stiffness in systemic lupus erythematosus (SLE) patients at low risk for cardiovascular disease: a cross-sectional controlled study |journal=PLoS ONE |volume=9 |issue=4 |pages=e94511 |year=2014 |pmid=24722263 |pmc=3983200 |doi=10.1371/journal.pone.0094511 |url=}}</ref>=== | |||
*[[Jugular venous distension]] | |||
**Secondary to [[hypertension]] and cardiac complications | |||
*[[Lymphadenopathy]] | |||
** [[Lymph node|Lymph nodes]] are soft, non-tender, discrete | |||
** Usually detected in the [[cervical]], [[axillary]], and [[inguinal]] | |||
===Lungs<ref name="pmid21194884">{{cite journal |vauthors=Torre O, Harari S |title=Pleural and pulmonary involvement in systemic lupus erythematosus |journal=Presse Med |volume=40 |issue=1 Pt 2 |pages=e19–29 |year=2011 |pmid=21194884 |doi=10.1016/j.lpm.2010.11.004 |url=}}</ref><ref name="pmid26550810">{{cite journal |vauthors=Salvati F |title=[The involvement of pulmonary interstitial tissue in multisystemic lupus erythematosus: interdisciplinarity and role of the pneumologists] |language=Italian |journal=Clin Ter |volume=166 |issue=5 |pages=205–7 |year=2015 |pmid=26550810 |doi= |url=}}</ref><ref name="pmid25639532">{{cite journal |vauthors=Alamoudi OS, Attar SM |title=Pulmonary manifestations in systemic lupus erythematosus: association with disease activity |journal=Respirology |volume=20 |issue=3 |pages=474–80 |year=2015 |pmid=25639532 |pmc=4418345 |doi=10.1111/resp.12473 |url=}}</ref>=== | |||
*Fine and coarse [[crackles]] upon auscultation of the [[lung]] | |||
**May be due to [[pneumonitis]] | |||
*In case of [[pleural effusion]]: | |||
**Asymmetric [[tactile fremitus]] | |||
**Asymmetric [[chest expansion]] | |||
===Heart<ref name="pmid24790989">{{cite journal |vauthors=Mak A, Kow NY |title=Imbalance between endothelial damage and repair: a gateway to cardiovascular disease in systemic lupus erythematosus |journal=Biomed Res Int |volume=2014 |issue= |pages=178721 |year=2014 |pmid=24790989 |pmc=3984775 |doi=10.1155/2014/178721 |url=}}</ref><ref name="pmid24722263">{{cite journal |vauthors=Sacre K, Escoubet B, Pasquet B, Chauveheid MP, Zennaro MC, Tubach F, Papo T |title=Increased arterial stiffness in systemic lupus erythematosus (SLE) patients at low risk for cardiovascular disease: a cross-sectional controlled study |journal=PLoS ONE |volume=9 |issue=4 |pages=e94511 |year=2014 |pmid=24722263 |pmc=3983200 |doi=10.1371/journal.pone.0094511 |url=}}</ref><ref name="pmid23052654">{{cite journal |vauthors=Canpolat N, Kasapcopur O, Caliskan S, Gokalp S, Bor M, Tasdemir M, Sever L, Arisoy N |title=Ambulatory blood pressure and subclinical cardiovascular disease in patients with juvenile-onset systemic lupus erythematosus |journal=Pediatr. Nephrol. |volume=28 |issue=2 |pages=305–13 |year=2013 |pmid=23052654 |doi=10.1007/s00467-012-2317-3 |url=}}</ref>=== | |||
*Chest [[tenderness]] or discomfort upon palpation | |||
**May be due to [[costochondritis]] | |||
*[[Diastolic murmurs|Diastolic murmur]], or [[Systolic murmurs|systolic murmur]] >3/6 due to [[valvular disease]] | |||
*Loud second heart sound (due to [[pulmonary hypertension]]) | |||
*Loud S1-S2 due to [[cardiomegaly]] | |||
*Decrease heart sounds if associated with [[pericardial effusion]] | |||
===Abdomen<ref name="pmid20572299">{{cite journal |vauthors=Tian XP, Zhang X |title=Gastrointestinal involvement in systemic lupus erythematosus: insight into pathogenesis, diagnosis and treatment |journal=World J. Gastroenterol. |volume=16 |issue=24 |pages=2971–7 |year=2010 |pmid=20572299 |pmc=2890936 |doi= |url=}}</ref><ref name="pmid27329649">{{cite journal |vauthors=Alves SC, Fasano S, Isenberg DA |title=Autoimmune gastrointestinal complications in patients with systemic lupus erythematosus: case series and literature review |journal=Lupus |volume=25 |issue=14 |pages=1509–1519 |year=2016 |pmid=27329649 |doi=10.1177/0961203316655210 |url=}}</ref><ref name="pmid27055518">{{cite journal |vauthors=Fawzy M, Edrees A, Okasha H, El Ashmaui A, Ragab G |title=Gastrointestinal manifestations in systemic lupus erythematosus |journal=Lupus |volume=25 |issue=13 |pages=1456–1462 |year=2016 |pmid=27055518 |doi=10.1177/0961203316642308 |url=}}</ref><ref name="pmid28523968">{{cite journal |vauthors=Li Z, Xu D, Wang Z, Wang Y, Zhang S, Li M, Zeng X |title=Gastrointestinal system involvement in systemic lupus erythematosus |journal=Lupus |volume= |issue= |pages=961203317707825 |year=2017 |pmid=28523968 |doi=10.1177/0961203317707825 |url=}}</ref>=== | |||
*[[Abdominal distention]] | |||
*[[Ascites]] | |||
**Due to [[nephrotic syndrome]] | |||
*[[Abdominal pain]] | |||
**Due to [[Vasculitis|mesentric vasculitis]] | |||
*[[Hepatomegaly]] | |||
*[[Splenomegaly]] | |||
*Costo-vertebral angle tenderness | |||
===Extremities<ref name="pmid15580980">{{cite journal |vauthors=Zoma A |title=Musculoskeletal involvement in systemic lupus erythematosus |journal=Lupus |volume=13 |issue=11 |pages=851–3 |year=2004 |pmid=15580980 |doi=10.1191/0961203303lu2021oa |url=}}</ref><ref name="pmid22956550">{{cite journal |vauthors=Gabba A, Piga M, Vacca A, Porru G, Garau P, Cauli A, Mathieu A |title=Joint and tendon involvement in systemic lupus erythematosus: an ultrasound study of hands and wrists in 108 patients |journal=Rheumatology (Oxford) |volume=51 |issue=12 |pages=2278–85 |year=2012 |pmid=22956550 |doi=10.1093/rheumatology/kes226 |url=}}</ref><ref name="pmid19591780">{{cite journal |vauthors=Grossman JM |title=Lupus arthritis |journal=Best Pract Res Clin Rheumatol |volume=23 |issue=4 |pages=495–506 |year=2009 |pmid=19591780 |doi=10.1016/j.berh.2009.04.003 |url=}}</ref><ref name="pmid24862229">{{cite journal |vauthors=Zhu KK, Xu WD, Pan HF, Zhang M, Ni J, Ge FY, Ye DQ |title=The risk factors of avascular necrosis in patients with systemic lupus erythematosus: a meta-analysis |journal=Inflammation |volume=37 |issue=5 |pages=1852–64 |year=2014 |pmid=24862229 |doi=10.1007/s10753-014-9917-y |url=}}</ref><ref name="pmid23731640">{{cite journal |vauthors=Voulgari PV, Kosta P, Argyropoulou MI, Drosos AA |title=Avascular necrosis in a patient with systemic lupus erythematosus |journal=Joint Bone Spine |volume=80 |issue=6 |pages=665 |year=2013 |pmid=23731640 |doi=10.1016/j.jbspin.2013.03.018 |url=}}</ref>=== | |||
*[[Clubbing]] | |||
*[[Cyanosis]] | |||
*[[Muscle weakness|Muscle atrophy or weakness]] | |||
*[[Livedo reticularis]] | |||
**Reddish-cyanotic, reticular pattern on the skin of the arms, legs, and torso, particularly with cold exposure | |||
*[[Arthritis]] | |||
**Symmetrical | |||
**Polyarticular | |||
**Mostly involve knees, carpal joints, and joints of the fingers, especially the proximal [[interphalangeal]] (PIP) joint | |||
**Decrease range of motion in affected joints | |||
*Joints [[erythema]] | |||
**Due to [[synovitis]] | |||
*Joint effusion | |||
*Muscle [[atrophy]] | |||
*[[Fasciculations]] in the upper/lower extremity | |||
*[[Claudication]] | |||
*Loss of digit or limb | |||
===Neuromuscular<ref name="pmid19366083">{{cite journal |vauthors=Cojocaru IM, Cojocaru M, Tănăsescu R, Burcin C, Atanasiu AN, Silosi I |title=Detection of autoantibodies to ribosome P in lupus patients with neurological involvement |journal=Rom J Intern Med |volume=46 |issue=3 |pages=239–42 |year=2008 |pmid=19366083 |doi= |url=}}</ref><ref name="pmid22594009">{{cite journal |vauthors=Madrane S, Ribi C |title=[Central neuropsychiatric involvement in systemic lupus erythematosus] |language=French |journal=Rev Med Suisse |volume=8 |issue=337 |pages=848–53 |year=2012 |pmid=22594009 |doi= |url=}}</ref><ref name="pmid7555923">{{cite journal |vauthors=Sivri A, Hasçelik Z, Celiker R, Başgöze O |title=Early detection of neurological involvement in systemic lupus erythematosus patients |journal=Electromyogr Clin Neurophysiol |volume=35 |issue=4 |pages=195–9 |year=1995 |pmid=7555923 |doi= |url=}}</ref><ref name="pmid19217587">{{cite journal |vauthors=Juncal Gallego L, Almuíña Simón C, Muíños Esparza LF, Díaz Soto R, Ramil Fraga C, Quiroga Ordóñez E |title=[Systemic lupus erythematosus with fulminant neurological involvement] |language=Spanish; Castilian |journal=An Pediatr (Barc) |volume=70 |issue=2 |pages=202–4 |year=2009 |pmid=19217587 |doi=10.1016/j.anpedi.2008.09.009 |url=}}</ref>=== | |||
*Patient is usually oriented to persons, place, and time based on the disease course | |||
*[[Cognitive impairment]] | |||
*[[Hallucination|Hallucinations]] | |||
**[[Visual hallucinations|Visual]] | |||
**[[Auditory hallucinations|Auditory]] | |||
*Memory deficit | |||
**Loose associations | |||
**Impoverished thought content | |||
**Illogical thinking | |||
**Bizarre disorganised or catatonic behaviour | |||
</div>}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| |!| | | |}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| A01 | | |A01=<div style="padding: 10px;"> | |||
==Laboratory Workup== | |||
* [[Complete blood count|CBC with DC]] | |||
* [[Basic metabolic panel|SMA-7]] | |||
* [[Creatine kinase]] | |||
* [[Urinalysis]] with [[Urinalysis#Microscopic examination|microscopic examination]] | |||
* [[Erythrocyte sedimentation rate]] | |||
* [[C-reactive protein]] | |||
* [[Coombs test]] | |||
* [[Antinuclear antibodies]] | |||
* [[Rheumatoid factor]] | |||
* [[Cryoglobulins]] | |||
* Antiphospholipid antibodies | |||
* Complement levels | |||
* Urine protein-to-creatinine ratio | |||
* Anti-dsDNA antibody | |||
* Anti-SM antibodies | |||
* Anti-Ro/SSA antibodies | |||
* Anti-La/SSB antibodies | |||
* Anti-U1 RNP antibodies | |||
* Antiribosomal P protein antibodies | |||
</div>}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| |!| | | |}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| A01 | | |A01=<div style="padding: 10px;"> | |||
==Imaging Study== | |||
===Plain radiographs of swollen joints=== | |||
*Erosions | |||
===Ultrasonography of painful joints=== | |||
*Detect synovitis and tenosynovitis in the hands and wrists in patients with SLE | |||
===Renal ultrasonography=== | |||
*To assess kidney size | |||
*To rule out urinary tract obstruction | |||
===Chest radiography=== | |||
*For suspected pleural effusion, interstitial lung disease, cardiomegaly | |||
===Echocardiography=== | |||
*For suspected pericardial involvement, to assess for a source of emboli, or noninvasive estimation of pulmonary artery pressure; and for evaluation of suspected valvular lesions, such as verrucae | |||
===Computed tomography (CT)=== | |||
*For abdominal pain, suspected pancreatitis, interstitial lung disease | |||
===Magnetic resonance imaging (MRI)=== | |||
*For focal neurologic deficits or cognitive dysfunction | |||
</div>}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| |!| | | |}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| A01 | | |A01=<div style="padding: 10px;"> | |||
==Other Investigation== | |||
===Bronchoscopy=== | |||
Fiberoptic [[bronchoscopy]] with [[Bronchoalveolar lavage|bronchoalveolar lavage (BAL)]] and transbronchial lung biopsies:<ref name="pmid16409858">{{cite journal |vauthors=Shen M, Wang Y, Xu WB, Zeng XJ, Zhang FC |title=[Pleuropulmonary manifestations of systemic lupus erythematosus] |language=Chinese |journal=Zhonghua Yi Xue Za Zhi |volume=85 |issue=48 |pages=3392–5 |year=2005 |pmid=16409858 |doi= |url=}}</ref><ref name="pmid9187214">{{cite journal |vauthors=Susanto I, Peters JI |title=Acute lupus pneumonitis with normal chest radiograph |journal=Chest |volume=111 |issue=6 |pages=1781–3 |year=1997 |pmid=9187214 |doi= |url=}}</ref> | |||
* To substantiate the diagnosis of alveolar [[hemorrhage]] | |||
=== Barium swallow or esophagography === | |||
*[[Esophageal]] stricture<ref name="pmid12873055">{{cite journal |vauthors=Jiménez-Alonso J, Estev D, Vera C, Sabio JM |title=Dysphagia in patients with systemic lupus erythematosus |journal=Lupus |volume=12 |issue=6 |pages=493 |year=2003 |pmid=12873055 |doi= |url=}}</ref> | |||
**Peptic strictures that appear as smooth, tapered narrowing in the distal [[esophagus]] | |||
*[[Esophageal dilatation]]<ref name="pmid12873055" /> | |||
=== Biopsy === | |||
* [[Renal]] biopsies:<ref name="pmid22977215">{{cite journal |vauthors=Giannico G, Fogo AB |title=Lupus nephritis: is the kidney biopsy currently necessary in the management of lupus nephritis? |journal=Clin J Am Soc Nephrol |volume=8 |issue=1 |pages=138–45 |year=2013 |pmid=22977215 |doi=10.2215/CJN.03400412 |url=}}</ref><ref name="pmid24969191">{{cite journal |vauthors=Singh A, Ghosh R, Kaur P, Golay V, Pandey R, Roychowdhury A |title=Protocol renal biopsy in patients with lupus nephritis: a single center experience |journal=Saudi J Kidney Dis Transpl |volume=25 |issue=4 |pages=801–7 |year=2014 |pmid=24969191 |doi= |url=}}</ref> | |||
** Determining the degree of renal involvement | |||
** Delineating treatment decisions and prognosis in certain clinical scenarios | |||
** Assess activity and damage (i.e., chronicity) | |||
** Helping with classification | |||
* [[Endomyocardial]] biopsy:<ref name="pmid2684953">{{cite journal |vauthors=Salomone E, Tamburino C, Bruno G, Di Paola R, Silvestri F |title=The role of endomyocardial biopsy in the diagnosis of cardiac involvement in systemic lupus erythematosus |journal=Heart Vessels |volume=5 a|issue=1 |pages=52–3 |year=1989 |pmid=2684953 |doi= |url=}}</ref> | |||
** May be helpful in guiding treatment towards the use of [[corticosteroids]] | |||
=== Paracentesis === | |||
* [[Paracentesis]] in the presence of the following conditions either for symptomatic relief (therapeutic) or fluid evaluation (diagnostic): | |||
** [[Ascites]]<ref name="pmid22324961">{{cite journal |vauthors=Prasad S, Abujam B, Lawrence A, Aggarwal A |title=Massive ascites as a presenting feature of lupus |journal=Int J Rheum Dis |volume=15 |issue=1 |pages=e15–6 |year=2012 |pmid=22324961 |doi=10.1111/j.1756-185X.2011.01659.x |url=}}</ref> | |||
** Massive [[pleural effusion]]<ref name="pmid25417677">{{cite journal |vauthors=Palavutitotai N, Buppajarntham T, Katchamart W |title=Etiologies and outcomes of pleural effusions in patients with systemic lupus erythematosus |journal=J Clin Rheumatol |volume=20 |issue=8 |pages=418–21 |year=2014 |pmid=25417677 |doi=10.1097/RHU.0000000000000179 |url=}}</ref> | |||
** Massive [[pericardial effusion]] and [[tamponade]]<ref name="pmid24579442">{{cite journal |vauthors=Kruzliak P, Novak M, Piler P, Kovacova G |title=Pericardial involvement in systemic lupus erythematosus: current diagnosis and therapy |journal=Acta Cardiol |volume=68 |issue=6 |pages=629–33 |year=2013 |pmid=24579442 |doi=10.2143/AC.68.6.8000011 |url=}}</ref> | |||
=== Arthrocentesis === | |||
* In the presence of joint effusion to differentiate between different causes of [[arthritis]]<ref name="pmid642792">{{cite journal |vauthors=Goldenberg DL, Cohen AS |title=Synovial membrane histopathology in the differential diagnosis of rheumatoid arthritis, gout, pseudogout, systemic lupus erythematosus, infectious arthritis and degenerative joint disease |journal=Medicine (Baltimore) |volume=57 |issue=3 |pages=239–52 |year=1978 |pmid=642792 |doi= |url=}}</ref> | |||
</div>}} | |||
{{Familytree/end}} | |||
</div> | |||
== Treatment == | == Treatment == | ||
<div style="font-size: 90%;"> | |||
{{Familytree/start}} | |||
{{Familytree|boxstyle=width: 700px; text-align: left; font-size: 100%; padding: 0px;| A01 | | |A01=<div style="padding: 10px;"> | |||
==Treatment goals== | |||
Treatment goals in systemic lupus erythematosus (SLE) include: | |||
* Ensure long-term survival | |||
* Achieve the lowest possible disease activity | |||
* Prevent organ damage | |||
* Minimize [[drug toxicity]] | |||
* Improve quality of life | |||
===== General treatment ===== | |||
* [[Hydroxychloroquine]]: 200 to 400 mg daily as a single daily dose or in 2 divided doses. | |||
** Generally, all patients with any type of SLE manifestation should be treated with [[hydroxychloroquine]] regardless of the severity of the disease. | |||
The treatment choice for systemic lupus erythematosus (SLE) is varied based on the severity of the disease and symptoms: | |||
* Mild cases are defined as disease pattern with one or two organ involvement. | |||
* Moderate cases are defined as more than 2 organ involvement during disease flares with low grade of involvement and complications or one or two organ involvement with more extensive involvements. | |||
* Severe cases are defined as presentation of the disease with life threatening complications and multiple (more than 2) organ involvements. | |||
== Severe disease == | |||
* Preferred regimen (1): [[Hydroxychloroquine]] PO 200 to 400 mg daily as a single daily dose or in 2 divided doses '''AND''' [[methylprednisolone]] as [[intravenous]] "pulse"; 0.5 to 1 g/day for three days in acutely ill patients, or 1 to 2 mg/kg/day in more stable patients | |||
* Alternative regimen(1): [[Hydroxychloroquine]] PO 200 to 400 mg daily as a single daily dose or in 2 divided doses '''AND''' [[prednisone]] oral; 40-60 mg/day | |||
* Alternative regimen (2): [[Mycophenolate]] | |||
** For induction: 1 g twice daily for 6 months in combination with a [[glucocorticoid]] | |||
** For maintenance: 0.5-3 g daily or 1 g twice daily | |||
*** Initial period of intensive [[immunosuppressive therapy]] (induction therapy) to control the disease and halt tissue injury | |||
* Alternative regimen (3): [[Cyclophosphamide]] IV 500 mg once every 2 weeks for 6 doses or 500 to 1,000 mg/m2 once every month for 6 doses or 500 to 1,000 mg/m2 every month for 6 months, then every 3 months for a total of at least 2.5 years | |||
* Alternative regimen (4): [[Rituximab]] IV: 375 mg/m2 once weekly for 4 doses or 1,000 mg (flat dose) on days 0 and 15 or 500 to 1,000 mg on days 1 and 15 | |||
== Less Severe (mild and moderate) disease == | |||
* Preferred regimen (1): [[Hydroxychloroquine]] PO 200 to 400 mg daily as a single daily dose or in 2 divided doses | |||
* Preferred regimen (2): [[Prednisone]] PO low doses of 10 mg/d or less for a short term therapy | |||
** For milder SLE | |||
** For treatment of [[cutaneous]] and musculoskeletal symptoms not responding to other therapies | |||
** It should be tapered once [[hydroxychloroquine]] has taken effect | |||
* Alternative regimen (1): [[Azathioprine]] PO initial 2 mg/kg/day; may reduce to 1.5 mg/kg/day after 1 month | |||
** Can be used to control symptoms | |||
* Alternative regimen (2): [[Methotrexate]] PO initial therapy with 7.5 mg once weekly; may increase by 2.5 mg increments weekly | |||
** Can be used to control symptoms | |||
== Other organ specific treatments == | |||
===== Fever management<ref name="pmid27529058">{{cite journal |vauthors=Jordan N, D'Cruz D |title=Current and emerging treatment options in the management of lupus |journal=Immunotargets Ther |volume=5 |issue= |pages=9–20 |year=2016 |pmid=27529058 |pmc=4970629 |doi=10.2147/ITT.S40675 |url=}}</ref><ref name="pmid24830791">{{cite journal |vauthors=Cobo-Ibáñez T, Loza-Santamaría E, Pego-Reigosa JM, Marqués AO, Rúa-Figueroa I, Fernández-Nebro A, Cáliz Cáliz R, López Longo FJ, Muñoz-Fernández S |title=Efficacy and safety of rituximab in the treatment of non-renal systemic lupus erythematosus: a systematic review |journal=Semin. Arthritis Rheum. |volume=44 |issue=2 |pages=175–85 |year=2014 |pmid=24830791 |doi=10.1016/j.semarthrit.2014.04.002 |url=}}</ref> ===== | |||
* Preferred regimen: [[Celecoxib]] PO 100 to 200 mg twice daily | |||
** For [[fever]] management even in SLE patients with [[Sulfa allergy|“sulfa” allergy]] | |||
* Alternative regimen: [[Acetaminophen]] 1000 mg every 6 hours; maximum daily dose: 3000 mg daily | |||
==== Raynaud's phenomenon treatment<ref name="pmid3691593">{{cite journal |vauthors=Challenor VF, Waller DG, Francis DA, Francis JL, Mani R, Roath S |title=Nisoldipine in primary Raynaud's phenomenon |journal=Eur. J. Clin. Pharmacol. |volume=33 |issue=1 |pages=27–30 |year=1987 |pmid=3691593 |doi= |url=}}</ref> ==== | |||
* Preferred regimen (1): [[Calcium channel blocker]] ([[nifedipine]]) 10 to 30 mg 3 times daily | |||
* Preferred regimen (2): Antiplatelet therapy with low-dose [[aspirin]] (75 or 81 mg/day) in all patients with secondary [[Raynaud phenomenon]] | |||
* Alternative regimen (1): [[Phosphodiesterase inhibitors|Phosphodiesterase (PDE) inhibitor]] ([[sildenafil]]) 20 mg once or twice daily | |||
** Inadequate response to a [[CCB]] | |||
* Alternative regimen (2): Addition of [[Nitroglycerin (Topical ointment)|topical nitroglycerin (NTG)]] | |||
** Inadequate response to a [[CCB]] | |||
** A [[Sildenafil|PDE inhibitor]] is not available, effective, or well-tolerated | |||
* Alternative regimen (3): Intravenous (IV) infusions of a [[Prostaglandin|prostaglandin (PG)]] especially [[Prostacyclin|prostacyclin (PGI2) analogue]] for extremely severe patients with [[Raynaud's phenomenon|raynaud's phenomenon]]<ref name="pmid6890719">{{cite journal |vauthors=Pardy BJ, Hoare MC, Eastcott HH, Miles CC, Needham TN, Harbourne T, Ellis BW |title=Prostaglandin E1 in severe Raynaud's phenomenon |journal=Surgery |volume=92 |issue=6 |pages=953–65 |year=1982 |pmid=6890719 |doi= |url=}}</ref> | |||
===== Chronic pain management<ref name="pmid24938194">{{cite journal |vauthors=Di Franco M, Guzzo MP, Spinelli FR, Atzeni F, Sarzi-Puttini P, Conti F, Iannuccelli C |title=Pain and systemic lupus erythematosus |journal=Reumatismo |volume=66 |issue=1 |pages=33–8 |year=2014 |pmid=24938194 |doi= |url=}}</ref> ===== | |||
* Moderate pain should be treated with mild prescription [[opiates]] such as: | |||
** Preferred regimen: [[Dextropropoxyphene]] 600 mg maximum daily dosage divided into 2 or 3 doses | |||
** Alternative regimen: [[Co-codamol|Co-codamol (Acetaminophene+opioid)]]: [[Acetaminophen]] (300 to 1,000 mg/dose)/[[codeine]] (15 to 60 mg/dose) every 4 hours as needed; adjust dose according to severity of pain and response of patient (maximum: [[acetaminophen]] 4,000 mg/[[codeine]] 360 mg per 24 hours) | |||
* Moderate to severe [[chronic pain]] should be treated with stronger [[Opioid|opioids]] such as: | |||
** Preferred regimen (1): [[Hydrocodone]]: Single doses >40 mg or >60 mg with a total daily dose ≥80 mg | |||
** Preferred regimen (2): [[Oxycodone]]: 5 to 15 mg every 4 to 6 hours as needed | |||
** Alternative regimen (1): [[MS Contin|MS Contin:]] Opioid naive patients can have 5 to 10 mg every 4 hours; usual dosage range between 5 to 15 mg every 4 hours | |||
*** Higher initial doses in patients with prior [[opioid]] exposure | |||
** Alternative regimen (2): [[Methadone]]: Maximum initial dose 30 mg | |||
** Alternative regimen (3): [[Fentanyl]] Duragesic Transdermal patch: A convenient treatment option for [[Systemic lupus erythematosus|lupus]] chronic pain. It has a long lasting effect as well | |||
===== Cutaneous lupus erythematosus<ref name="pmid14162995">{{cite journal |vauthors=DOEGLAS HM |title=CHRONIC DISCOID LUPUS ERYTHEMATOSUS TREATED WITH TRIAMCINOLONE AND PLASTIC OCCLUSION |journal=Dermatologica |volume=128 |issue= |pages=384–6 |year=1964 |pmid=14162995 |doi= |url=}}</ref><ref name="pmid16966017">{{cite journal |vauthors=Rothfield N, Sontheimer RD, Bernstein M |title=Lupus erythematosus: systemic and cutaneous manifestations |journal=Clin. Dermatol. |volume=24 |issue=5 |pages=348–62 |year=2006 |pmid=16966017 |doi=10.1016/j.clindermatol.2006.07.014 |url=}}</ref><ref name="pmid18797893">{{cite journal |vauthors=Sárdy M, Ruzicka T, Kuhn A |title=Topical calcineurin inhibitors in cutaneous lupus erythematosus |journal=Arch. Dermatol. Res. |volume=301 |issue=1 |pages=93–8 |year=2009 |pmid=18797893 |doi=10.1007/s00403-008-0894-6 |url=}}</ref><ref name="pmid13971327">{{cite journal |vauthors=BJORNBERG A, HELLGREN L |title=Treatment of chronic discoid lupus erythematosus with fluocinolone acetonide ointment |journal=Br. J. Dermatol. |volume=75 |issue= |pages=156–60 |year=1963 |pmid=13971327 |doi= |url=}}</ref><ref name="pmid359493">{{cite journal |vauthors=Ritschel WA, Hammer GV, Thompson GA |title=Pharmacokinetics of antimalarials and proposals for dosage regimens |journal=Int J Clin Pharmacol Biopharm |volume=16 |issue=9 |pages=395–401 |year=1978 |pmid=359493 |doi= |url=}}</ref> ===== | |||
* Preferred regimen (1): Super high potency or high potency [[Steroid|topical steroid]] twice daily for patients with DLE or SCLE | |||
** [[Hydrocortisone]] 1% or 2.5% for facial involvement | |||
** [[Triamcinolone acetonide]] 0.1% cream or [[fluocinonide]] 0.05% cream: [[trunk]], extremity, or scalp disease | |||
** [[Clobetasol propionate]] for acute flares of DLE | |||
*** Discontinue treatment in the absence of disease activity | |||
* Alternative regimen (1): [[Calcineurin inhibitor|Topical calcineurin inhibitor]] such as [[tacrolimus]] 0.1% ointment or [[pimecrolimus]] 1% cream | |||
* Preferred regimen (2): Intralesional [[corticosteroid]] injections for DLE or SCLE if an acute flare of DLE or SCLE doesn't respond to [[Topical steroid|topical steroid therapy]] for two to four week | |||
* Alternative regimen (2): Systemic medications; [[hydroxychloroquine]] 200 to 400 mg/day for at least six weeks | |||
** After improvement it should be decreased to 200 mg/day for maintenance therapy | |||
** Administered in the case of failure of local therapy or extensive disease manifestation | |||
* Alternative regimen (3): [[Quinacrine]] 100 mg/day | |||
** In case of [[Antimalarial drug|antimalarial drugs]] failure | |||
===== Lupus nephritis treatment<ref name="pmid25014039">{{cite journal |vauthors=Schwartz N, Goilav B, Putterman C |title=The pathogenesis, diagnosis and treatment of lupus nephritis |journal=Curr Opin Rheumatol |volume=26 |issue=5 |pages=502–9 |year=2014 |pmid=25014039 |pmc=4221732 |doi=10.1097/BOR.0000000000000089 |url=}}</ref><ref name="pmid23328501">{{cite journal |vauthors=Hogan J, Appel GB |title=Update on the treatment of lupus nephritis |journal=Curr. Opin. Nephrol. Hypertens. |volume=22 |issue=2 |pages=224–30 |year=2013 |pmid=23328501 |doi=10.1097/MNH.0b013e32835d921c |url=}}</ref><ref name="pmid25778500">{{cite journal |vauthors=Tunnicliffe DJ, Singh-Grewal D, Kim S, Craig JC, Tong A |title=Diagnosis, Monitoring, and Treatment of Systemic Lupus Erythematosus: A Systematic Review of Clinical Practice Guidelines |journal=Arthritis Care Res (Hoboken) |volume=67 |issue=10 |pages=1440–52 |year=2015 |pmid=25778500 |doi=10.1002/acr.22591 |url=}}</ref> ===== | |||
* Aggressive [[antihypertensive therapy]] with [[blood pressure]] goal of 130/85 | |||
* In patients with [[proteinuria]], antiproteinuric therapy with blockade of the [[renin-angiotensin system]] include [[ACEIs]] and [[ARBs]]: | |||
** [[ACE inhibitor|ACE inhibitors]]; [[captopril]] PO 25 mg 3 times daily | |||
*** Antiproteinuric effect | |||
** [[ARBs]]; [[losartan]] PO initial: 50 mg once daily; can be increased to 100 mg once daily based on [[blood pressure]] response | |||
*** Slowing progression of [[GFR]] decline; | |||
* [[Lipid]] lowering with [[statin therapy]] with the goal of [[LDL]]< 130 | |||
* Diffuse or focal proliferative LN: | |||
** Preferred regimen: [[Immunosuppressive therapy]] with [[glucocorticoids]] plus either [[Intravenous therapy|intravenous]] or oral [[Mycophenolate sodium|mycophenolate mofetil]]: 0.5 g of [[Mycophenolate sodium|mycophenolate mofetil]] twice daily for the first week, then 1 g twice daily for the second week, and thereafter increase the dose to 1.5 g twice daily | |||
** Alternative regimen: [[Immunosuppressive therapy]] with [[glucocorticoids]] plus IV [[cyclophosphamide]] 500 mg every two weeks for a total of six doses | |||
* Severe active disease: | |||
** Preferred regimen: [[Glucocorticoid|Glucocorticoid therapy]] is initiated with [[Intravenous therapy|intravenous]] pulse [[methylprednisolone]] (250 mg to 1000 mg given over 30 minutes daily for three days) to induce a rapid [[immunosuppressive]] effect, followed by conventional doses | |||
** Alternative regimen: Conventional doses of oral [[glucocorticoids]] (eg, 0.5 to 1 mg/kg per day of prednisone) without a pulse. | |||
*** Oral [[prednisolone]] at a dose of 60 mg/day, tapered every two weeks by 10 mg/day until 40 mg/day is reached, then tapered by 5 mg/day until 10 mg/day is reached | |||
===== Considerations<ref name="pmid25778500" /> ===== | |||
* Appropriate adjunct therapy: | |||
** [[Vitamin D]] and [[calcium supplement|calcium supplements]]<nowiki/> for preventing [[osteoporosis]] in patients using [[corticosteroids]] | |||
** [[Antihypertensive drugs]] and [[statins]] were also recommended in patients using [[corticosteroids]] | |||
* Adverse effects: Cutaneous [[atrophy]] is a potential side effect of the long-term use of [[Topical steroid|topical steroids]] | |||
</div>}} | |||
{{Familytree/end}} | |||
</div> | |||
== Do's == | == Do's == | ||
Latest revision as of 17:57, 2 April 2018
| SLE Resident Survival Guide |
|---|
| Overview |
| Causes |
| FIRE |
| Diagnosis |
| Treatment |
| Do's |
| Don'ts |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] ; Associate Editor(s)-in-Chief: Iqra Qamar M.D.[2] ; Aditya Ganti M.B.B.S. [3]
Overview
Causes
- Genetic predisposition:[1]
- HLA class polymorphism
- Complement genes
- Female sexual gene due to high levels of estrogen and prolactin
- Auto-immune disease[2]
- Exposure to ultraviolet (UV) light[3]
- Can exacerbate or induce systemic manifestations of SLE
- Drug-induced lupus
FIRE
Diagnosis
Diagnostic criteria:
In 2012, Systemic Lupus International Collaboration Criteria (SLICC) developed a new criteria for SLE diagnosis. SLICC criteria for the classification of systemic lupus erythematosus was developed based on the old ACR criteria for the classification of systemic lupus erythematosus to address a more sensitive diagnostic criteria and also to cover weaknesses of the previous ACR criteria.[4][5]
Based on SLICC criteria, diagnosis of SLE is defined as:[6]
- Meeting at least 4 of 17 criteria, including at least 1 of the 11 clinical criteria and one of the six immunologic criteria
OR
- Biopsy-proven nephritis compatible with SLE in the presence of antinuclear antibodies (ANA) or anti-double-stranded DNA (dsDNA) antibodies
A criterion is considered positive if one or more of the observations listed in the definition for the criterion are present in the patient. A criterion should only be counted once, regardless of the number of observations in the definition that the patient presents with.
| Category | Criterion | Definition |
|---|---|---|
| Clinical | Acute cutaneous lupus |
|
| Chronic cutaneous lupus |
| |
| Nonscarring alopecia |
| |
| Oral or nasal ulcers |
| |
| Joint disease |
| |
| Serositis |
| |
| Renal |
| |
| Neurologic |
| |
| Hematologic | Hemolytic anemia |
|
| Leukopenia or lymphopenia |
| |
| Thrombocytopenia |
| |
| Immunologic | ANA |
|
| Anti-dsDNA |
| |
| Anit-SM |
| |
| Antiphospholipid |
| |
| Low complement | ||
| Direct Coombs' test |
|
Complete diagnostic approach:
SLE Presentation
Less common Presentation
| |||||||||||
Focused History
| |||||||||||
Physical ExaminationAppearance of the Patient
Vital Signs
Skin[10][11][12]
HEENT
Neck[18][19]
Lungs[20][21][22]
Heart[23][19][24]
Abdomen[25][26][27][28]
Extremities[29][30][31][32][33]
Neuromuscular[34][35][36][37]
| |||||||||||
Laboratory Workup
| |||||||||||
Imaging StudyPlain radiographs of swollen joints
Ultrasonography of painful joints
Renal ultrasonography
Chest radiography
Echocardiography
Computed tomography (CT)
Magnetic resonance imaging (MRI)
| |||||||||||
Other InvestigationBronchoscopyFiberoptic bronchoscopy with bronchoalveolar lavage (BAL) and transbronchial lung biopsies:[38][39]
Barium swallow or esophagography
Biopsy
Paracentesis
Arthrocentesis | |||||||||||
Treatment
Treatment goalsTreatment goals in systemic lupus erythematosus (SLE) include:
General treatment
The treatment choice for systemic lupus erythematosus (SLE) is varied based on the severity of the disease and symptoms:
Severe disease
Less Severe (mild and moderate) disease
Other organ specific treatmentsFever management[48][49]
Raynaud's phenomenon treatment[50]
Chronic pain management[52]
Cutaneous lupus erythematosus[53][54][55][56][57]
Lupus nephritis treatment[58][59][60]
Considerations[60]
| |||||||||
Do's
Don'ts
References
- ↑ Schur PH (1995). "Genetics of systemic lupus erythematosus". Lupus. 4 (6): 425–37. doi:10.1177/096120339500400603. PMID 8749564.
- ↑ Cutolo M, Sulli A, Seriolo B, Accardo S, Masi AT (1995). "Estrogens, the immune response and autoimmunity". Clin. Exp. Rheumatol. 13 (2): 217–26. PMID 7656468.
- ↑ Cooper GS, Dooley MA, Treadwell EL, St Clair EW, Gilkeson GS (2002). "Risk factors for development of systemic lupus erythematosus: allergies, infections, and family history". J Clin Epidemiol. 55 (10): 982–9. PMID 12464374.
- ↑ Tan EM, Cohen AS, Fries JF, Masi AT, McShane DJ, Rothfield NF, Schaller JG, Talal N, Winchester RJ (1982). "The 1982 revised criteria for the classification of systemic lupus erythematosus". Arthritis Rheum. 25 (11): 1271–7. PMID 7138600.
- ↑ Hochberg MC (1997). "Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus". Arthritis Rheum. 40 (9): 1725. doi:10.1002/1529-0131(199709)40:9<1725::AID-ART29>3.0.CO;2-Y. PMID 9324032.
- ↑ Petri M, Orbai AM, Alarcón GS, Gordon C, Merrill JT, Fortin PR, Bruce IN, Isenberg D, Wallace DJ, Nived O, Sturfelt G, Ramsey-Goldman R, Bae SC, Hanly JG, Sánchez-Guerrero J, Clarke A, Aranow C, Manzi S, Urowitz M, Gladman D, Kalunian K, Costner M, Werth VP, Zoma A, Bernatsky S, Ruiz-Irastorza G, Khamashta MA, Jacobsen S, Buyon JP, Maddison P, Dooley MA, van Vollenhoven RF, Ginzler E, Stoll T, Peschken C, Jorizzo JL, Callen JP, Lim SS, Fessler BJ, Inanc M, Kamen DL, Rahman A, Steinsson K, Franks AG, Sigler L, Hameed S, Fang H, Pham N, Brey R, Weisman MH, McGwin G, Magder LS (2012). "Derivation and validation of the Systemic Lupus International Collaborating Clinics classification criteria for systemic lupus erythematosus". Arthritis Rheum. 64 (8): 2677–86. doi:10.1002/art.34473. PMC 3409311. PMID 22553077.
- ↑ Tench CM, McCurdie I, White PD, D'Cruz DP (2000). "The prevalence and associations of fatigue in systemic lupus erythematosus". Rheumatology (Oxford). 39 (11): 1249–54. PMID 11085805.
- ↑ McKinley PS, Ouellette SC, Winkel GH (1995). "The contributions of disease activity, sleep patterns, and depression to fatigue in systemic lupus erythematosus. A proposed model". Arthritis Rheum. 38 (6): 826–34. PMID 7779127.
- ↑ Wang B, Gladman DD, Urowitz MB (1998). "Fatigue in lupus is not correlated with disease activity". J. Rheumatol. 25 (5): 892–5. PMID 9598886.
- ↑ Parodi A, Cozzani E (2014). "Cutaneous manifestations of lupus erythematosus". G Ital Dermatol Venereol. 149 (5): 549–54. PMID 25077888.
- ↑ Szczęch J, Rutka M, Samotij D, Zalewska A, Reich A (2016). "Clinical characteristics of cutaneous lupus erythematosus". Postepy Dermatol Alergol. 33 (1): 13–7. doi:10.5114/pdia.2014.44031. PMC 4793050. PMID 26985173.
- ↑ Walling HW, Sontheimer RD (2009). "Cutaneous lupus erythematosus: issues in diagnosis and treatment". Am J Clin Dermatol. 10 (6): 365–81. doi:10.2165/11310780-000000000-00000. PMID 19824738.
- ↑ Preble JM, Silpa-archa S, Foster CS (2015). "Ocular involvement in systemic lupus erythematosus". Curr Opin Ophthalmol. 26 (6): 540–5. doi:10.1097/ICU.0000000000000209. PMID 26367085.
- ↑ Silpa-archa S, Lee JJ, Foster CS (2016). "Ocular manifestations in systemic lupus erythematosus". Br J Ophthalmol. 100 (1): 135–41. doi:10.1136/bjophthalmol-2015-306629. PMID 25904124.
- ↑ Robson AK, Burge SM, Millard PR (1992). "Nasal mucosal involvement in lupus erythematosus". Clin Otolaryngol Allied Sci. 17 (4): 341–3. PMID 1526055.
- ↑ Anyanwu CO, Ang CC, Werth VP (2013). "Oral mucosal involvement in bullous lupus". Arthritis Rheum. 65 (10): 2622. doi:10.1002/art.38051. PMC 4333153. PMID 23780804.
- ↑ Ranginwala AM, Chalishazar MM, Panja P, Buddhdev KP, Kale HM (2012). "Oral discoid lupus erythematosus: A study of twenty-one cases". J Oral Maxillofac Pathol. 16 (3): 368–73. doi:10.4103/0973-029X.102487. PMC 3519212. PMID 23248469.
- ↑ Melikoglu MA, Melikoglu M (2008). "The clinical importance of lymphadenopathy in systemic lupus erythematosus". Acta Reumatol Port. 33 (4): 402–6. PMID 19107085.
- ↑ 19.0 19.1 Sacre K, Escoubet B, Pasquet B, Chauveheid MP, Zennaro MC, Tubach F, Papo T (2014). "Increased arterial stiffness in systemic lupus erythematosus (SLE) patients at low risk for cardiovascular disease: a cross-sectional controlled study". PLoS ONE. 9 (4): e94511. doi:10.1371/journal.pone.0094511. PMC 3983200. PMID 24722263.
- ↑ Torre O, Harari S (2011). "Pleural and pulmonary involvement in systemic lupus erythematosus". Presse Med. 40 (1 Pt 2): e19–29. doi:10.1016/j.lpm.2010.11.004. PMID 21194884.
- ↑ Salvati F (2015). "[The involvement of pulmonary interstitial tissue in multisystemic lupus erythematosus: interdisciplinarity and role of the pneumologists]". Clin Ter (in Italian). 166 (5): 205–7. PMID 26550810.
- ↑ Alamoudi OS, Attar SM (2015). "Pulmonary manifestations in systemic lupus erythematosus: association with disease activity". Respirology. 20 (3): 474–80. doi:10.1111/resp.12473. PMC 4418345. PMID 25639532.
- ↑ Mak A, Kow NY (2014). "Imbalance between endothelial damage and repair: a gateway to cardiovascular disease in systemic lupus erythematosus". Biomed Res Int. 2014: 178721. doi:10.1155/2014/178721. PMC 3984775. PMID 24790989.
- ↑ Canpolat N, Kasapcopur O, Caliskan S, Gokalp S, Bor M, Tasdemir M, Sever L, Arisoy N (2013). "Ambulatory blood pressure and subclinical cardiovascular disease in patients with juvenile-onset systemic lupus erythematosus". Pediatr. Nephrol. 28 (2): 305–13. doi:10.1007/s00467-012-2317-3. PMID 23052654.
- ↑ Tian XP, Zhang X (2010). "Gastrointestinal involvement in systemic lupus erythematosus: insight into pathogenesis, diagnosis and treatment". World J. Gastroenterol. 16 (24): 2971–7. PMC 2890936. PMID 20572299.
- ↑ Alves SC, Fasano S, Isenberg DA (2016). "Autoimmune gastrointestinal complications in patients with systemic lupus erythematosus: case series and literature review". Lupus. 25 (14): 1509–1519. doi:10.1177/0961203316655210. PMID 27329649.
- ↑ Fawzy M, Edrees A, Okasha H, El Ashmaui A, Ragab G (2016). "Gastrointestinal manifestations in systemic lupus erythematosus". Lupus. 25 (13): 1456–1462. doi:10.1177/0961203316642308. PMID 27055518.
- ↑ Li Z, Xu D, Wang Z, Wang Y, Zhang S, Li M, Zeng X (2017). "Gastrointestinal system involvement in systemic lupus erythematosus". Lupus: 961203317707825. doi:10.1177/0961203317707825. PMID 28523968.
- ↑ Zoma A (2004). "Musculoskeletal involvement in systemic lupus erythematosus". Lupus. 13 (11): 851–3. doi:10.1191/0961203303lu2021oa. PMID 15580980.
- ↑ Gabba A, Piga M, Vacca A, Porru G, Garau P, Cauli A, Mathieu A (2012). "Joint and tendon involvement in systemic lupus erythematosus: an ultrasound study of hands and wrists in 108 patients". Rheumatology (Oxford). 51 (12): 2278–85. doi:10.1093/rheumatology/kes226. PMID 22956550.
- ↑ Grossman JM (2009). "Lupus arthritis". Best Pract Res Clin Rheumatol. 23 (4): 495–506. doi:10.1016/j.berh.2009.04.003. PMID 19591780.
- ↑ Zhu KK, Xu WD, Pan HF, Zhang M, Ni J, Ge FY, Ye DQ (2014). "The risk factors of avascular necrosis in patients with systemic lupus erythematosus: a meta-analysis". Inflammation. 37 (5): 1852–64. doi:10.1007/s10753-014-9917-y. PMID 24862229.
- ↑ Voulgari PV, Kosta P, Argyropoulou MI, Drosos AA (2013). "Avascular necrosis in a patient with systemic lupus erythematosus". Joint Bone Spine. 80 (6): 665. doi:10.1016/j.jbspin.2013.03.018. PMID 23731640.
- ↑ Cojocaru IM, Cojocaru M, Tănăsescu R, Burcin C, Atanasiu AN, Silosi I (2008). "Detection of autoantibodies to ribosome P in lupus patients with neurological involvement". Rom J Intern Med. 46 (3): 239–42. PMID 19366083.
- ↑ Madrane S, Ribi C (2012). "[Central neuropsychiatric involvement in systemic lupus erythematosus]". Rev Med Suisse (in French). 8 (337): 848–53. PMID 22594009.
- ↑ Sivri A, Hasçelik Z, Celiker R, Başgöze O (1995). "Early detection of neurological involvement in systemic lupus erythematosus patients". Electromyogr Clin Neurophysiol. 35 (4): 195–9. PMID 7555923.
- ↑ Juncal Gallego L, Almuíña Simón C, Muíños Esparza LF, Díaz Soto R, Ramil Fraga C, Quiroga Ordóñez E (2009). "[Systemic lupus erythematosus with fulminant neurological involvement]". An Pediatr (Barc) (in Spanish; Castilian). 70 (2): 202–4. doi:10.1016/j.anpedi.2008.09.009. PMID 19217587.
- ↑ Shen M, Wang Y, Xu WB, Zeng XJ, Zhang FC (2005). "[Pleuropulmonary manifestations of systemic lupus erythematosus]". Zhonghua Yi Xue Za Zhi (in Chinese). 85 (48): 3392–5. PMID 16409858.
- ↑ Susanto I, Peters JI (1997). "Acute lupus pneumonitis with normal chest radiograph". Chest. 111 (6): 1781–3. PMID 9187214.
- ↑ 40.0 40.1 Jiménez-Alonso J, Estev D, Vera C, Sabio JM (2003). "Dysphagia in patients with systemic lupus erythematosus". Lupus. 12 (6): 493. PMID 12873055.
- ↑ Giannico G, Fogo AB (2013). "Lupus nephritis: is the kidney biopsy currently necessary in the management of lupus nephritis?". Clin J Am Soc Nephrol. 8 (1): 138–45. doi:10.2215/CJN.03400412. PMID 22977215.
- ↑ Singh A, Ghosh R, Kaur P, Golay V, Pandey R, Roychowdhury A (2014). "Protocol renal biopsy in patients with lupus nephritis: a single center experience". Saudi J Kidney Dis Transpl. 25 (4): 801–7. PMID 24969191.
- ↑ Salomone E, Tamburino C, Bruno G, Di Paola R, Silvestri F (1989). "The role of endomyocardial biopsy in the diagnosis of cardiac involvement in systemic lupus erythematosus". Heart Vessels. 5 a (1): 52–3. PMID 2684953.
- ↑ Prasad S, Abujam B, Lawrence A, Aggarwal A (2012). "Massive ascites as a presenting feature of lupus". Int J Rheum Dis. 15 (1): e15–6. doi:10.1111/j.1756-185X.2011.01659.x. PMID 22324961.
- ↑ Palavutitotai N, Buppajarntham T, Katchamart W (2014). "Etiologies and outcomes of pleural effusions in patients with systemic lupus erythematosus". J Clin Rheumatol. 20 (8): 418–21. doi:10.1097/RHU.0000000000000179. PMID 25417677.
- ↑ Kruzliak P, Novak M, Piler P, Kovacova G (2013). "Pericardial involvement in systemic lupus erythematosus: current diagnosis and therapy". Acta Cardiol. 68 (6): 629–33. doi:10.2143/AC.68.6.8000011. PMID 24579442.
- ↑ Goldenberg DL, Cohen AS (1978). "Synovial membrane histopathology in the differential diagnosis of rheumatoid arthritis, gout, pseudogout, systemic lupus erythematosus, infectious arthritis and degenerative joint disease". Medicine (Baltimore). 57 (3): 239–52. PMID 642792.
- ↑ Jordan N, D'Cruz D (2016). "Current and emerging treatment options in the management of lupus". Immunotargets Ther. 5: 9–20. doi:10.2147/ITT.S40675. PMC 4970629. PMID 27529058.
- ↑ Cobo-Ibáñez T, Loza-Santamaría E, Pego-Reigosa JM, Marqués AO, Rúa-Figueroa I, Fernández-Nebro A, Cáliz Cáliz R, López Longo FJ, Muñoz-Fernández S (2014). "Efficacy and safety of rituximab in the treatment of non-renal systemic lupus erythematosus: a systematic review". Semin. Arthritis Rheum. 44 (2): 175–85. doi:10.1016/j.semarthrit.2014.04.002. PMID 24830791.
- ↑ Challenor VF, Waller DG, Francis DA, Francis JL, Mani R, Roath S (1987). "Nisoldipine in primary Raynaud's phenomenon". Eur. J. Clin. Pharmacol. 33 (1): 27–30. PMID 3691593.
- ↑ Pardy BJ, Hoare MC, Eastcott HH, Miles CC, Needham TN, Harbourne T, Ellis BW (1982). "Prostaglandin E1 in severe Raynaud's phenomenon". Surgery. 92 (6): 953–65. PMID 6890719.
- ↑ Di Franco M, Guzzo MP, Spinelli FR, Atzeni F, Sarzi-Puttini P, Conti F, Iannuccelli C (2014). "Pain and systemic lupus erythematosus". Reumatismo. 66 (1): 33–8. PMID 24938194.
- ↑ DOEGLAS HM (1964). "CHRONIC DISCOID LUPUS ERYTHEMATOSUS TREATED WITH TRIAMCINOLONE AND PLASTIC OCCLUSION". Dermatologica. 128: 384–6. PMID 14162995.
- ↑ Rothfield N, Sontheimer RD, Bernstein M (2006). "Lupus erythematosus: systemic and cutaneous manifestations". Clin. Dermatol. 24 (5): 348–62. doi:10.1016/j.clindermatol.2006.07.014. PMID 16966017.
- ↑ Sárdy M, Ruzicka T, Kuhn A (2009). "Topical calcineurin inhibitors in cutaneous lupus erythematosus". Arch. Dermatol. Res. 301 (1): 93–8. doi:10.1007/s00403-008-0894-6. PMID 18797893.
- ↑ BJORNBERG A, HELLGREN L (1963). "Treatment of chronic discoid lupus erythematosus with fluocinolone acetonide ointment". Br. J. Dermatol. 75: 156–60. PMID 13971327.
- ↑ Ritschel WA, Hammer GV, Thompson GA (1978). "Pharmacokinetics of antimalarials and proposals for dosage regimens". Int J Clin Pharmacol Biopharm. 16 (9): 395–401. PMID 359493.
- ↑ Schwartz N, Goilav B, Putterman C (2014). "The pathogenesis, diagnosis and treatment of lupus nephritis". Curr Opin Rheumatol. 26 (5): 502–9. doi:10.1097/BOR.0000000000000089. PMC 4221732. PMID 25014039.
- ↑ Hogan J, Appel GB (2013). "Update on the treatment of lupus nephritis". Curr. Opin. Nephrol. Hypertens. 22 (2): 224–30. doi:10.1097/MNH.0b013e32835d921c. PMID 23328501.
- ↑ 60.0 60.1 Tunnicliffe DJ, Singh-Grewal D, Kim S, Craig JC, Tong A (2015). "Diagnosis, Monitoring, and Treatment of Systemic Lupus Erythematosus: A Systematic Review of Clinical Practice Guidelines". Arthritis Care Res (Hoboken). 67 (10): 1440–52. doi:10.1002/acr.22591. PMID 25778500.