Molluscum contagiosum differential diagnosis: Difference between revisions
Jump to navigation
Jump to search
No edit summary |
No edit summary |
||
| Line 11: | Line 11: | ||
*Other lesions that may be mistaken for molluscum contagiosum include flat warts, condyloma acuminatum, pyogenic granuloma , adnexal tumors, Langerhans cell histiocytosis , basal cell carcinoma , and amelanotic melanoma. Skin biopsy is useful for distinguishing molluscum contagiosum from other disorders. | *Other lesions that may be mistaken for molluscum contagiosum include flat warts, condyloma acuminatum, pyogenic granuloma , adnexal tumors, Langerhans cell histiocytosis , basal cell carcinoma , and amelanotic melanoma. Skin biopsy is useful for distinguishing molluscum contagiosum from other disorders. | ||
====Differential diagnosis of | ====Differential diagnosis of rash-like skin lesions==== | ||
{| class="wikitable sortable" | {| class="wikitable sortable" | ||
! style="width: 200px; background: #4479BA; text-align: center;" | {{fontcolor|#FFF|Disease}} | ! style="width: 200px; background: #4479BA; text-align: center;" | {{fontcolor|#FFF|Disease}} | ||
! style="width: 200px; background: #4479BA; text-align: center;" | {{fontcolor|#FFF|Features}} | ! style="width: 200px; background: #4479BA; text-align: center;" | {{fontcolor|#FFF|Features}} | ||
! | ! style="width: 200px; background: #4479BA; text-align: center;" | {{fontcolor|#FFF|Images}} | ||
|- | |- | ||
| style="background: #DCDCDC; padding: 5px;" |[[Cryptococcosis]] | | style="background: #DCDCDC; padding: 5px;" |[[Cryptococcosis]] | ||
| Line 26: | Line 26: | ||
[[File:Cryptococcosis05.jpeg|300px]] | [[File:Cryptococcosis05.jpeg|300px]] | ||
|- | |- | ||
| style="background: #DCDCDC; padding: 5px;" |[[ | | style="background: #DCDCDC; padding: 5px;" |[[Histoplasmosis]] | ||
| | | | ||
*Acquired via inhalation of airborne microconidia. | *Acquired via inhalation of airborne microconidia. | ||
| Line 44: | Line 44: | ||
|- | |- | ||
| style="background: #DCDCDC; padding: 5px;" |[[ | | style="background: #DCDCDC; padding: 5px;" |[[Condyloma acuminatum]] | ||
| | | | ||
*Spread through direct skin-to-skin contact during oral, genital, or anal sex with an infected partner. | *Spread through direct skin-to-skin contact during oral, genital, or anal sex with an infected partner. | ||
| Line 51: | Line 51: | ||
[[File:Condyloma acuminatum07.jpg|300px]] | [[File:Condyloma acuminatum07.jpg|300px]] | ||
|- | |- | ||
| style="background: #DCDCDC; padding: 5px;" |[[ | | style="background: #DCDCDC; padding: 5px;" |[[Pyogenic granuloma]] | ||
| | | | ||
* | * A vascular lesion that occurs on both mucosa and skin, and appears as an [[hyperplasia|overgrowth]] of tissue due to [[irritation]], [[physical trauma]] or [[hormones|hormonal]] factors.<ref name="Fitz2">Freedberg, et al. (2003). ''Fitzpatrick's Dermatology in General Medicine''. (6th ed.). McGraw-Hill. ISBN 0-07-138076-0.</ref><ref name="joralsci">{{cite journal | author = Jafarzadeh H, Sanatkhani M, Mohtasham N | title = Oral pyogenic granuloma: a review | journal = J Oral Sci | volume = 48 | issue = 4 | pages = 167–75 |date=December 2006 | pmid = 17220613 | doi = 10.2334/josnusd.48.167| url = http://joi.jlc.jst.go.jp/JST.JSTAGE/josnusd/48.167?from=PubMed| accessdate = 2009-01-04 | format = – <sup>[http://scholar.google.co.uk/scholar?hl=en&lr=&q=intitle%3AOral+pyogenic+granuloma%3A+a+review&as_publication=J+Oral+Sci&as_ylo=2006&as_yhi=2006&btnG=Search Scholar search]</sup>}} {{dead link|date=March 2009}}</ref> | ||
* | *Involve the gums, the skin and [[nasal septum]], and has also been found far from the head such as in the thigh.<ref name="Nthumba">{{cite journal |author=Nthumba PM |title=Giant pyogenic granuloma of the thigh: a case report |journal=J Med Case Reports |volume=2 |issue= 1|pages=95 |year=2008 |pmid=18377654 |pmc=2329656 |doi=10.1186/1752-1947-2-95 |url=http://www.jmedicalcasereports.com/content/2//95}}</ref> | ||
| | | | ||
[[File:Granuloma pyogenic 16.jpeg|300px]] | [[File:Granuloma pyogenic 16.jpeg|300px]] | ||
| Line 60: | Line 60: | ||
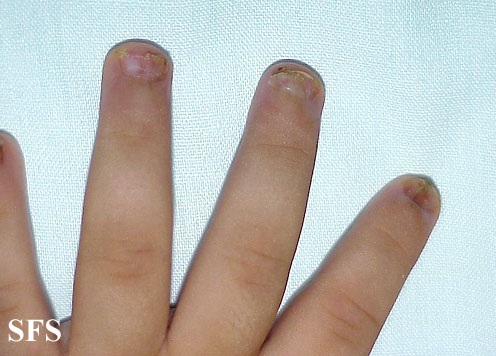
| style="background: #DCDCDC; padding: 5px;" |[[Langerhans cell histiocytosis]] | | style="background: #DCDCDC; padding: 5px;" |[[Langerhans cell histiocytosis]] | ||
| | | | ||
* | *Result of either a true [[neoplastic]] process or a reactive [[immune]] condition.<ref name="pmid25281259">{{cite journal| author=DiCaprio MR, Roberts TT| title=Diagnosis and Management of Langerhans Cell Histiocytosis. | journal=J Am Acad Orthop Surg | year= 2014 | volume= 22 | issue= 10 | pages= 643-652 | pmid=25281259 | doi=10.5435/JAAOS-22-10-643 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=25281259 }} </ref><ref name="pmid25310214">{{cite journal| author=Grana N| title=Langerhans cell histiocytosis. | journal=Cancer Control | year= 2014 | volume= 21 | issue= 4 | pages= 328-34 | pmid=25310214 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=25310214 }} </ref><ref name="pmid26414464">{{cite journal| author=Harmon CM, Brown N| title=Langerhans Cell Histiocytosis: A Clinicopathologic Review and Molecular Pathogenetic Update. | journal=Arch Pathol Lab Med | year= 2015 | volume= 139 | issue= 10 | pages= 1211-4 | pmid=26414464 | doi=10.5858/arpa.2015-0199-RA | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=26414464 }} </ref> | ||
*Common symptoms of Langerhans cell histiocytosis include [[bone]] pain, [[rash]], [[fever]], and [[failure to thrive]].<ref name="wiki">Langerhans cell histiocytosis. Wikipedia (2015) https://en.wikipedia.org/wiki/Langerhans_cell_histiocytosis Accessed on February, 2 2016</ref><ref name="radio">Langerhans cell histiocytosis. Radiopeadia (2015) http://radiopaedia.org/articles/langerhans-cell-histiocytosis Accessed on February, 3 2016</ref><ref name="PDQ">Langerhans Cell Histiocytosis Treatment (PDQ®): Health Professional Version. National Cancer Institute (2015) http://www.cancer.gov/types/langerhans/hp/langerhans-treatment-pdq Accessed on February, 3 2016</ref> | *Common symptoms of Langerhans cell histiocytosis include [[bone]] pain, [[rash]], [[fever]], and [[failure to thrive]].<ref name="wiki">Langerhans cell histiocytosis. Wikipedia (2015) https://en.wikipedia.org/wiki/Langerhans_cell_histiocytosis Accessed on February, 2 2016</ref><ref name="radio">Langerhans cell histiocytosis. Radiopeadia (2015) http://radiopaedia.org/articles/langerhans-cell-histiocytosis Accessed on February, 3 2016</ref><ref name="PDQ">Langerhans Cell Histiocytosis Treatment (PDQ®): Health Professional Version. National Cancer Institute (2015) http://www.cancer.gov/types/langerhans/hp/langerhans-treatment-pdq Accessed on February, 3 2016</ref> | ||
*scaly erythematous lesions located on the scalp and extremities, localized [[bone]] [[tenderness]], and [[hepatosplenomegaly]].<ref name="PDQ">Langerhans Cell Histiocytosis Treatment (PDQ®): Health Professional Version. National Cancer Institute (2015) http://www.cancer.gov/types/langerhans/hp/langerhans-treatment-pdq Accessed on February, 3 2016</ref><ref name="wiki">Langerhans cell histiocytosis. Wikipedia (2015) https://en.wikipedia.org/wiki/Langerhans_cell_histiocytosis Accessed on February, 2 2016</ref> | *scaly erythematous lesions located on the scalp and extremities, localized [[bone]] [[tenderness]], and [[hepatosplenomegaly]].<ref name="PDQ">Langerhans Cell Histiocytosis Treatment (PDQ®): Health Professional Version. National Cancer Institute (2015) http://www.cancer.gov/types/langerhans/hp/langerhans-treatment-pdq Accessed on February, 3 2016</ref><ref name="wiki">Langerhans cell histiocytosis. Wikipedia (2015) https://en.wikipedia.org/wiki/Langerhans_cell_histiocytosis Accessed on February, 2 2016</ref> | ||
| Line 66: | Line 66: | ||
[[File:Langerhans cell histiocytosis08.jpg|300px]] | [[File:Langerhans cell histiocytosis08.jpg|300px]] | ||
|- | |- | ||
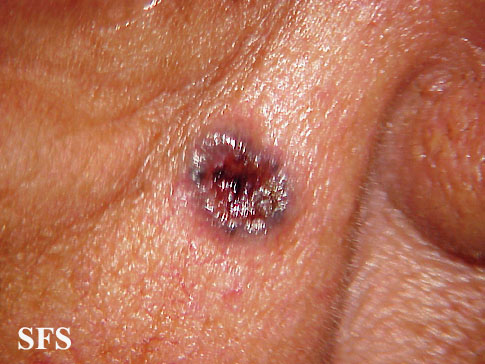
| style="background: #DCDCDC; padding: 5px;" | | | style="background: #DCDCDC; padding: 5px;" |Basal cell carcinoma | ||
| | | | ||
* | * Develop in the basal cell layer of the skin. | ||
* Cumulative DNA damage leads to mutations, after sunlight exposure. | * Cumulative DNA damage leads to mutations, after sunlight exposure. | ||
* | * Skin growths on sun-exposed skin | ||
| | | | ||
[[File:Basal cell carcinoma 01.jpeg|300px]] | [[File:Basal cell carcinoma 01.jpeg|300px]] | ||
|- | |- | ||
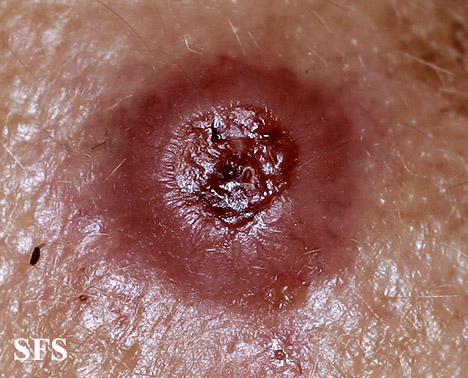
| | | style="background: #DCDCDC; padding: 5px;" |[[Amelanotic melanoma]] | ||
| | | | ||
* Amelanotic or hypomelanotic lesions or maybe nodular and desmoplastic subtypes | * Amelanotic or hypomelanotic lesions or maybe nodular and desmoplastic subtypes | ||
* Lesions may present as pink or red macules, plaques, or nodules, often with well-defined borders | * Lesions may present as pink or red macules, plaques, or nodules, often with well-defined borders | ||
* | * Often clinically confused with benign lesions | ||
| | | | ||
[[File:Melanoma 08.jpg|300px]] | [[File:Melanoma 08.jpg|300px]] | ||
Revision as of 14:10, 12 June 2017
|
Molluscum contagiosum Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Mahshid Mir, M.D. [2], João André Alves Silva, M.D. [3]
Overview
Molluscum contagiosum must be differentiated from other diseases that cause infection of the skin and of the mucous membranes, including chickenpox, herpes zoster, erythema multiforme, among others.
Differential Diagnosis
Different rash-like conditions can be confused with molluscum contagiosum and are thus included in its differential diagnosis. The various conditions that should be differentiated from molluscum contagiosum include:[1][2][3][4][5][6][7]
- Skin lesions due to cryptococcosis, histoplasmosis, or Penicillium marneffei infection may resemble molluscum lesions.
- Other lesions that may be mistaken for molluscum contagiosum include flat warts, condyloma acuminatum, pyogenic granuloma , adnexal tumors, Langerhans cell histiocytosis , basal cell carcinoma , and amelanotic melanoma. Skin biopsy is useful for distinguishing molluscum contagiosum from other disorders.
Differential diagnosis of rash-like skin lesions
| Disease | Features | Images |
|---|---|---|
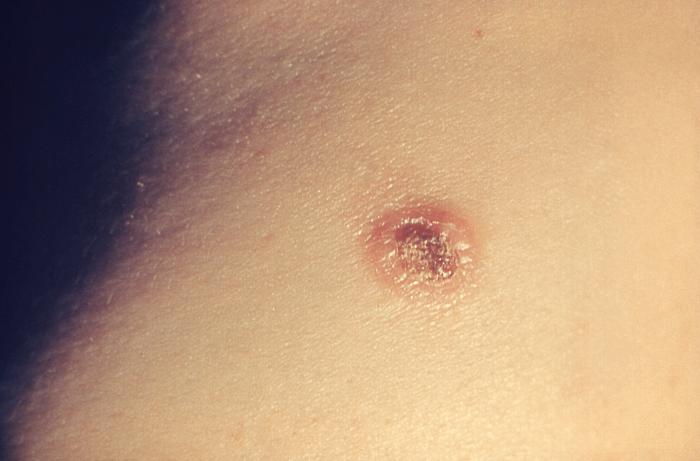
| Cryptococcosis |
|
|
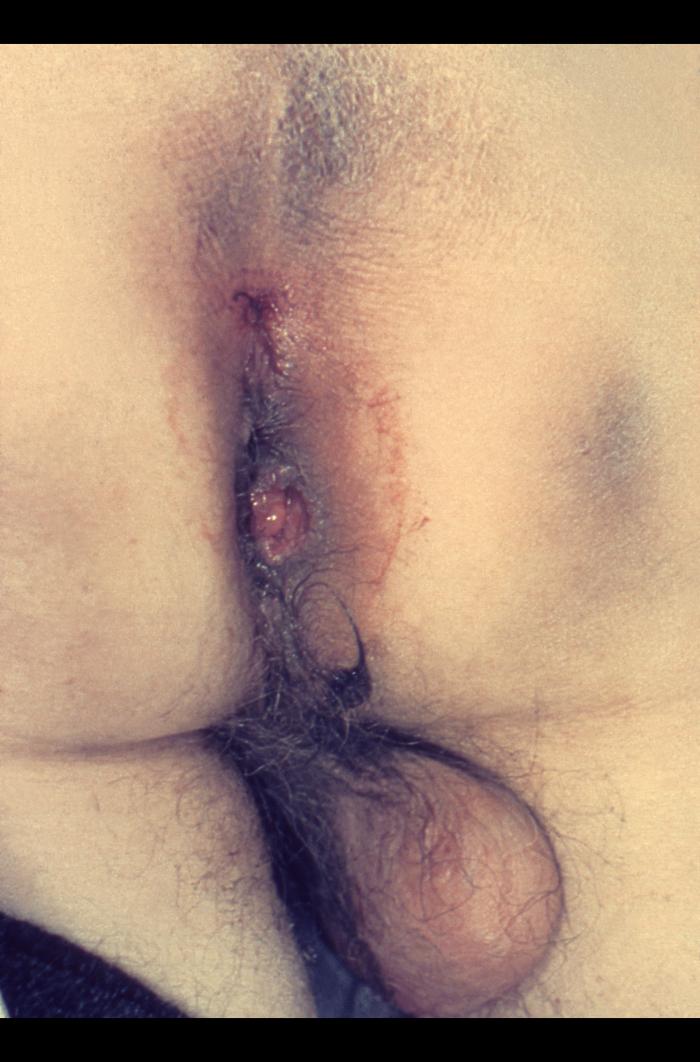
| Histoplasmosis |
|
|
| Penicillium marneffei |
|
|
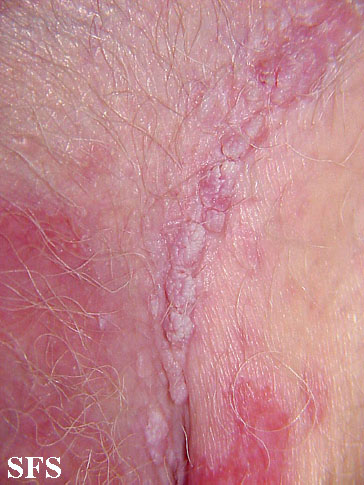
| Condyloma acuminatum |
|
|
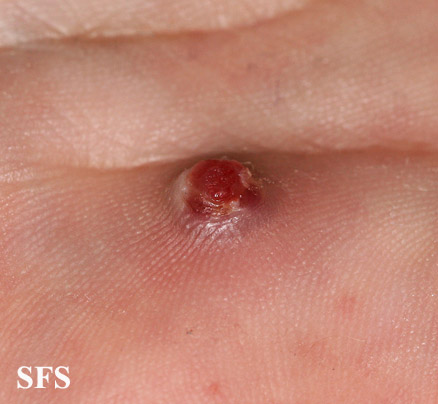
| Pyogenic granuloma |
|
|
| Langerhans cell histiocytosis |
|
|
| Basal cell carcinoma |
|
|
| Amelanotic melanoma |
|
| Disease | Features |
|---|---|
| Impetigo | |
| Insect bites |
|
| Kawasaki disease |
|
| Measles |
|
| Monkeypox |
|
| Rubella |
|
| Atypical measles |
|
| Coxsackievirus |
|
| Acne |
|
| Syphilis | It commonly presents with gneralized systemic symptoms such as malaise, fatigue, headache and fever. Skin eruptions may be subtle and asymptomatic It is classically described as:
|
| Molluscum contagiosum |
|
| Mononucleosis |
|
| Toxic erythema | |
| Rat-bite fever | |
| Parvovirus B19 | |
| Cytomegalovirus |
|
| Scarlet fever |
|
| Rocky Mountain spotted fever |
|
| Stevens-Johnson syndrome |
|
| Varicella-zoster virus | |
| Chickenpox |
|
| Meningococcemia | |
| Rickettsial pox | |
| Meningitis |
|
References
- ↑ Hartman-Adams H, Banvard C, Juckett G (2014). "Impetigo: diagnosis and treatment". Am Fam Physician. 90 (4): 229–35. PMID 25250996.
- ↑ Mehta N, Chen KK, Kroumpouzos G (2016). "Skin disease in pregnancy: The approach of the obstetric medicine physician". Clin Dermatol. 34 (3): 320–6. doi:10.1016/j.clindermatol.2016.02.003. PMID 27265069.
- ↑ Moore, Zack S; Seward, Jane F; Lane, J Michael (2006). "Smallpox". The Lancet. 367 (9508): 425–435. doi:10.1016/S0140-6736(06)68143-9. ISSN 0140-6736.
- ↑ Ibrahim F, Khan T, Pujalte GG (2015). "Bacterial Skin Infections". Prim Care. 42 (4): 485–99. doi:10.1016/j.pop.2015.08.001. PMID 26612370.
- ↑ Ramoni S, Boneschi V, Cusini M (2016). "Syphilis as "the great imitator": a case of impetiginoid syphiloderm". Int J Dermatol. 55 (3): e162–3. doi:10.1111/ijd.13072. PMID 26566601.
- ↑ Kimura U, Yokoyama K, Hiruma M, Kano R, Takamori K, Suga Y (2015). "Tinea faciei caused by Trichophyton mentagrophytes (molecular type Arthroderma benhamiae ) mimics impetigo : a case report and literature review of cases in Japan". Med Mycol J. 56 (1): E1–5. doi:10.3314/mmj.56.E1. PMID 25855021.
- ↑ CEDEF (2012). "[Item 87--Mucocutaneous bacterial infections]". Ann Dermatol Venereol. 139 (11 Suppl): A32–9. doi:10.1016/j.annder.2012.01.002. PMID 23176858.
- ↑ Freedberg, et al. (2003). Fitzpatrick's Dermatology in General Medicine. (6th ed.). McGraw-Hill. ISBN 0-07-138076-0.
- ↑ Jafarzadeh H, Sanatkhani M, Mohtasham N (December 2006). "Oral pyogenic granuloma: a review" (– Scholar search). J Oral Sci. 48 (4): 167–75. doi:10.2334/josnusd.48.167. PMID 17220613. Retrieved 2009-01-04.[dead link]
- ↑ Nthumba PM (2008). "Giant pyogenic granuloma of the thigh: a case report". J Med Case Reports. 2 (1): 95. doi:10.1186/1752-1947-2-95. PMC 2329656. PMID 18377654.
- ↑ DiCaprio MR, Roberts TT (2014). "Diagnosis and Management of Langerhans Cell Histiocytosis". J Am Acad Orthop Surg. 22 (10): 643–652. doi:10.5435/JAAOS-22-10-643. PMID 25281259.
- ↑ Grana N (2014). "Langerhans cell histiocytosis". Cancer Control. 21 (4): 328–34. PMID 25310214.
- ↑ Harmon CM, Brown N (2015). "Langerhans Cell Histiocytosis: A Clinicopathologic Review and Molecular Pathogenetic Update". Arch Pathol Lab Med. 139 (10): 1211–4. doi:10.5858/arpa.2015-0199-RA. PMID 26414464.
- ↑ 14.0 14.1 Langerhans cell histiocytosis. Wikipedia (2015) https://en.wikipedia.org/wiki/Langerhans_cell_histiocytosis Accessed on February, 2 2016
- ↑ Langerhans cell histiocytosis. Radiopeadia (2015) http://radiopaedia.org/articles/langerhans-cell-histiocytosis Accessed on February, 3 2016
- ↑ 16.0 16.1 Langerhans Cell Histiocytosis Treatment (PDQ®): Health Professional Version. National Cancer Institute (2015) http://www.cancer.gov/types/langerhans/hp/langerhans-treatment-pdq Accessed on February, 3 2016