COVID-19-associated seizure
|
COVID-19 Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
COVID-19-associated seizure On the Web |
|
American Roentgen Ray Society Images of COVID-19-associated seizure |
|
Risk calculators and risk factors for COVID-19-associated seizure |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Mandana Safakhah, MD[2]
Synonyms and keywords:
Overview
Coronaviruses impacts are not always restricted to respiratory system and they have potential for neuroinvasion under specific circumstances. Neurological manifestations such as dizziness,headache ,anosmia as well as case reports with encephalitis ,stroke,epileptic seizures associated with covid-19, have been reported.
Historical Perspective
- two male patients, non-epileptic were hospitalised with covid-19 signs and symptoms, March 2020 ,Ohio, U.S.A. During their hospital stay they developed encephalopathy and seizures, controlled by levetiracetam
- A women with the past medical history of seizure following herpetic encephalitis ,presented with a sudden focal myoclonus and positive test for covid 19 in Italy, 23rd of april 2020.[1]
- Also, a cohort multicentre study was done in China, April 2020, demonstrating that COVID 19 doesn't increase the risk of symptomatic seizure in patients hospitalized with the acute respiratory phase of COVID 19.Although ,some seizure-like reactions are seen because of acute reaction to stress or hypocalcemia .[2]
Classification
There isn't any established classification for covid-19 associated seizure.
Pathophysiology
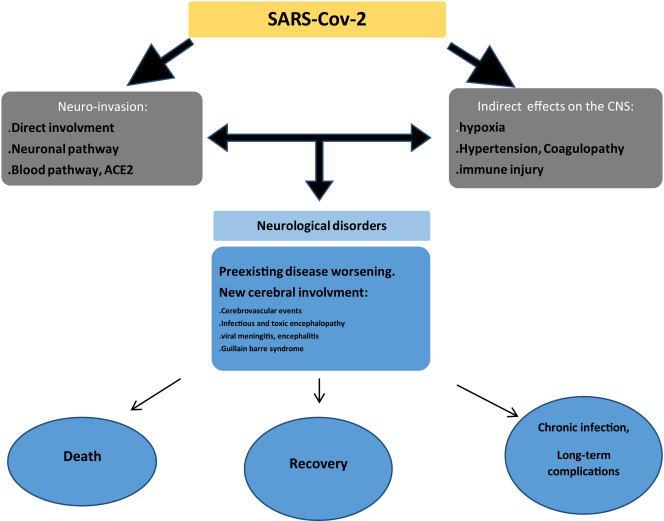
Although there are some evidences suggesting covid -19 may affect CNS through two direct ways:haematogenous and neuronal retrograde dissemination through olfactory bulb ,the exact neurotropic mechanisms of this virus are yet to be known.[3] on the other hand, there are some slim evidences supporting the multifactorial origin of covid-19 associated seizure including:
- blood brain barrier breakdown due to cytokine reaction as a part of viral infection
- Entry into to glial cells and neurons via ACE2 receptor and CNS attack
- Impairment of gas exchange in lungs and leading to anaemia ,hence increasing anaerobic metabolites in brain resulting cellular and interstitial oedema
- Prolonged prothrombin time induced by covid-19 may lead to cerebral hemorrhage
Causes
The aetiology of seizure regardless whether it is covid-19 or not ,is divided into two categories:
- 'Provoked seizures : these seizures usually have a temporary trigger such as CNS infection,electrolytes disturbance, withdrawal syndrome,sepsis ,fever, sleep deprivation and stroke.
- Unprovoked seizures: In this catrgory ,there isn't any obvious cause or precipitating factor .[5]
Differentiating COVID-19-associated seizure from other Diseases
Apart from the viral cause of the seizure, the differential diagnosis for this disease is usually based on the presenting symptoms as below:
- Generalized convulsive movements:Epilepsy-syncope with secondary jerking movement-Involuntary movement disorders and other neurological conditions
- Drop attack:Epilepsy-Cardiac-Brainstem abnormalities-vertebrobasilar ischemia-Idiopathic
- Transient focal motor and sensory attack :tics-tonic spasms of multiple
- Facial muscles and eye movement:partial seizures-movement disorder-Other neurological conditions.[6]
Epidemiology and Demographics
By now there isn't any sufficient evidence for demographic and epidemiologic data about covid- 19 associated seizure.
Risk Factors
There are no established risk factors for covid-19 associated seizure.
Screening
There is insufficient evidence to recommend routine screening for covid-19 associated seizure.
Natural History, Complications, and Prognosis
The global case fatality rate is currently estimated to be 4.6% according to WHO , 9th,June.[7] Also neurological complications of covid-19 .The covid-19 fatality rate depends on several factors such as:
- patient demographics
- availability of health care
- test limitation
Also , the more comorbidities the patient has ,the poorer covid-19 clinical output. Some of the prognostic factor of covid-19 are listed as below:
- Above 65 years old
- smoking
- male sex
- elevated inflammatory markers
- elevated D-Dimer
- elevated interleukin 6
- thrombocytopenia
- high neutrophil to lymphocyte ratio
- higher acute physiology and chronic health evaluation score.[8]
Diagnosis
Diagnostic Study of Choice
History and Symptoms
History
- Neurotropism is one common feature of coronaviruses[10][11].
- COVID-19 document CNS manifestations in 25% of the patients, headache (13%), dizziness (17%), impaired consciousness (8%), acute cerebrovascular problems (3%), ataxia (0.5), and seizures (0.5%).
Symptoms
- General symptoms or warning signs of a seizure can include:
- Staring
- Jerking movements of the arms and legs
- Stiffening of the body
- Loss of consciousness
- Breathing problems or stopping breathing
- Loss of bowel or bladder control
- Falling suddenly for no apparent reason, especially when associated with loss of consciousness
- Not responding to noise or words for brief periods
- Appearing confused or in a haze
- Nodding your head rhythmically, when associated with loss of awareness or loss of consciousness
- Periods of rapid eye blinking and staring
Physical Examination
Patients with [disease name] usually appear [general appearance]. Physical examination of patients with [disease name] is usually remarkable for [finding 1], [finding 2], and [finding 3].
OR
Common physical examination findings of [disease name] include [finding 1], [finding 2], and [finding 3].
OR
The presence of [finding(s)] on physical examination is diagnostic of [disease name].
OR
The presence of [finding(s)] on physical examination is highly suggestive of [disease name].
Laboratory Findings
An elevated/reduced concentration of serum/blood/urinary/CSF/other [lab test] is diagnostic of [disease name].
OR
Laboratory findings consistent with the diagnosis of [disease name] include [abnormal test 1], [abnormal test 2], and [abnormal test 3].
OR
[Test] is usually normal among patients with [disease name].
OR
Some patients with [disease name] may have elevated/reduced concentration of [test], which is usually suggestive of [progression/complication].
OR
There are no diagnostic laboratory findings associated with [disease name].
Electrocardiogram
There are no ECG findings associated with [disease name].
OR
An ECG may be helpful in the diagnosis of [disease name]. Findings on an ECG suggestive of/diagnostic of [disease name] include [finding 1], [finding 2], and [finding 3].
X-ray
There are no x-ray findings associated with [disease name].
OR
An x-ray may be helpful in the diagnosis of [disease name]. Findings on an x-ray suggestive of/diagnostic of [disease name] include [finding 1], [finding 2], and [finding 3].
OR
There are no x-ray findings associated with [disease name]. However, an x-ray may be helpful in the diagnosis of complications of [disease name], which include [complication 1], [complication 2], and [complication 3].
Echocardiography or Ultrasound
There are no echocardiography/ultrasound findings associated with [disease name].
OR
Echocardiography/ultrasound may be helpful in the diagnosis of [disease name]. Findings on an echocardiography/ultrasound suggestive of/diagnostic of [disease name] include [finding 1], [finding 2], and [finding 3].
OR
There are no echocardiography/ultrasound findings associated with [disease name]. However, an echocardiography/ultrasound may be helpful in the diagnosis of complications of [disease name], which include [complication 1], [complication 2], and [complication 3].
CT scan
There are no CT scan findings associated with [disease name].
OR
[Location] CT scan may be helpful in the diagnosis of [disease name]. Findings on CT scan suggestive of/diagnostic of [disease name] include [finding 1], [finding 2], and [finding 3].
OR
There are no CT scan findings associated with [disease name]. However, a CT scan may be helpful in the diagnosis of complications of [disease name], which include [complication 1], [complication 2], and [complication 3].
MRI
There are no MRI findings associated with [disease name].
OR
[Location] MRI may be helpful in the diagnosis of [disease name]. Findings on MRI suggestive of/diagnostic of [disease name] include [finding 1], [finding 2], and [finding 3].
OR
There are no MRI findings associated with [disease name]. However, a MRI may be helpful in the diagnosis of complications of [disease name], which include [complication 1], [complication 2], and [complication 3].
Other Imaging Findings
There are no other imaging findings associated with [disease name].
OR
[Imaging modality] may be helpful in the diagnosis of [disease name]. Findings on an [imaging modality] suggestive of/diagnostic of [disease name] include [finding 1], [finding 2], and [finding 3].
Other Diagnostic Studies
There are no other diagnostic studies associated with [disease name].
OR
[Diagnostic study] may be helpful in the diagnosis of [disease name]. Findings suggestive of/diagnostic of [disease name] include [finding 1], [finding 2], and [finding 3].
OR
Other diagnostic studies for [disease name] include [diagnostic study 1], which demonstrates [finding 1], [finding 2], and [finding 3], and [diagnostic study 2], which demonstrates [finding 1], [finding 2], and [finding 3].
Treatment
Medical Therapy
There is no treatment for [disease name]; the mainstay of therapy is supportive care.
OR
Supportive therapy for [disease name] includes [therapy 1], [therapy 2], and [therapy 3].
OR
The majority of cases of [disease name] are self-limited and require only supportive care.
OR
[Disease name] is a medical emergency and requires prompt treatment.
OR
The mainstay of treatment for [disease name] is [therapy].
OR
The optimal therapy for [malignancy name] depends on the stage at diagnosis.
OR
[Therapy] is recommended among all patients who develop [disease name].
OR
Pharmacologic medical therapy is recommended among patients with [disease subclass 1], [disease subclass 2], and [disease subclass 3].
OR
Pharmacologic medical therapies for [disease name] include (either) [therapy 1], [therapy 2], and/or [therapy 3].
OR
Empiric therapy for [disease name] depends on [disease factor 1] and [disease factor 2].
OR
Patients with [disease subclass 1] are treated with [therapy 1], whereas patients with [disease subclass 2] are treated with [therapy 2].
Surgery
Surgical intervention is not recommended for the management of [disease name].
OR
Surgery is not the first-line treatment option for patients with [disease name]. Surgery is usually reserved for patients with either [indication 1], [indication 2], and [indication 3]
OR
The mainstay of treatment for [disease name] is medical therapy. Surgery is usually reserved for patients with either [indication 1], [indication 2], and/or [indication 3].
OR
The feasibility of surgery depends on the stage of [malignancy] at diagnosis.
OR
Surgery is the mainstay of treatment for [disease or malignancy].
Primary Prevention
There are no established measures for the primary prevention of [disease name].
OR
There are no available vaccines against [disease name].
OR
Effective measures for the primary prevention of [disease name] include [measure1], [measure2], and [measure3].
OR
[Vaccine name] vaccine is recommended for [patient population] to prevent [disease name]. Other primary prevention strategies include [strategy 1], [strategy 2], and [strategy 3].
Secondary Prevention
There are no established measures for the secondary prevention of [disease name].
OR
Effective measures for the secondary prevention of [disease name] include [strategy 1], [strategy 2], and [strategy 3].
References
- ↑ {{https://www.seizure-journal.com/article/S1059-1311(20)30115-1/fulltext}}
- ↑ {{https://onlinelibrary.wiley.com/doi/full/10.1111/epi.16524}}
- ↑ {{https://pubmed.ncbi.nlm.nih.gov/32458193/}}
- ↑ {{https://www.sciencedirect.com/science/article/pii/S1878875020311645#sec3}}
- ↑ {{https://www.ncbi.nlm.nih.gov/books/NBK430765/}}
- ↑ {{https://www.nice.org.uk/guidance/CG20/documents/appendix-a-a-differential-diagnosis-first-consultation2}}
- ↑ Template:Https://bestpractice.bmj.com/topics/en-gb/3000168/prognosis
- ↑ Template:Https://bestpractice.bmj.com/topics/en-gb/3000168/prognosis
- ↑ Haines S, Caccamo A, Chan F, Galaso G, Catinchi A, Gupta PK (2020). "Practical Considerations When Performing Neurodiagnostic Studies on Patients with COVID-19 and Other Highly Virulent Diseases". Neurodiagn J. 60 (2): 78–95. doi:10.1080/21646821.2020.1756132. PMC 7212538 Check
|pmc=value (help). PMID 32374647 Check|pmid=value (help). - ↑ Bohmwald K, Gálvez NMS, Ríos M, Kalergis AM (2018). "Neurologic Alterations Due to Respiratory Virus Infections". Front Cell Neurosci. 12: 386. doi:10.3389/fncel.2018.00386. PMC 6212673. PMID 30416428.
- ↑ Li YC, Bai WZ, Hashikawa T (2020). "The neuroinvasive potential of SARS-CoV2 may play a role in the respiratory failure of COVID-19 patients". J Med Virol. 92 (6): 552–555. doi:10.1002/jmv.25728. PMC 7228394 Check
|pmc=value (help). PMID 32104915 Check|pmid=value (help).