Ponatinib hydrochloride
{{DrugProjectFormSinglePage |authorTag=Kiran Singh, M.D. [1] |genericName=ponatinib hydrochloride |aOrAn=a |drugClass=tyrosine kinase inhibitor |indicationType=treatment |indication=chronic myeloid leukemia |hasBlackBoxWarning=Yes |adverseReactions=hypertension, abdominal pain, constipation |blackBoxWarningTitle=WARNING: VASCULAR OCCLUSION, HEART FAILURE, AND HEPATOTOXICITY |blackBoxWarningBody=Vascular Occlusion:
- Arterial and venous thrombosis and occlusions have occurred in at least 27% of Iclusig treated patients, including fatal myocardial infarction, stroke, stenosis of large arterial vessels of the brain, severe peripheral vascular disease, and the need for urgent revascularization procedures. Patients with and without cardiovascular risk factors, including patients age 50 years or younger, experienced these events.
- Monitor for evidence of thromboembolism and vascular occlusion. Interrupt or stop Iclusig immediately for vascular occlusion. A benefit-risk consideration should guide a decision to restart Iclusig therapy.
Heart Failure:
- Heart failure, including fatalities, occurred in 8% of Iclusig-treated patients. Monitor cardiac function. Interrupt or stop Iclusig for new or worsening heart failure.
Hepatotoxicity:
- Hepatotoxicity, liver failure and death have occurred in Iclusig-treated patients. Monitor hepatic function. Interrupt Iclusig if hepatotoxicity is suspected.
|fdaLIADAdult===Indications==
Iclusig (ponatinib) is a kinase inhibitor indicated for the:
- Treatment of adult patients with T315I-positive chronic myeloid leukemia (CML) (chronic phase, accelerated phase, or blast phase) or T315I-positive Philadelphia chromosome positive acute lymphoblastic leukemia (Ph+ALL).
- Treatment of adult patients with chronic phase, accelerated phase, or blast phase chronic myeloid leukemia or Ph+ ALL for whom no other tyrosine kinase inhibitor (TKI) therapy is indicated.
- These indications are based upon response rate. There are no trials verifying an improvement in disease-related symptoms or increased survival with Iclusig.
Dosing
Recommended Dosing
- The optimal dose of ponatinib hydrochloride has not been identified. In clinical trials, the starting dose of ponatinib hydrochloride was 45 mg administered orally once daily. However, 59% of the patients required dose reductions to 30 mg or 15 mg once daily during the course of therapy.
- Start dosing with 45 mg once daily. Consider reducing the dose of ponatinib hydrochloride for chronic phase (CP) CML and accelerated phase (AP) CML patients who have achieved a major cytogenetic response.
- Consider discontinuing ponatinib hydrochloride if response has not occurred by 3 months (90 days).
- Ponatinib hydrochloride may be taken with or without food. Tablets should be swallowed whole.
Dose Modifications for Myelosuppression
- Suggested dose modifications for neutropenia (ANC* less than 1.0 × 109/L) and thrombocytopenia (platelet less than 50 × 109/L) that are unrelated to leukemia are summarized in Table 1.

Dose Modifications for Non-Hematologic Adverse Reactions
- If a serious non-hematologic adverse reaction occurs, modify the dose or interrupt treatment. Do not restart Iclusig in patients with arterial or venous occlusive reactions unless the potential benefit outweighs the risk of recurrent arterial or venous occlusions and the patient has no other treatment options. For serious reactions other than arterial or venous occlusion, do not restart ponatinib hydrochlorideuntil the serious event has resolved or the potential benefit of resuming therapy is judged to outweigh the risk.
Hepatic Toxicity
Recommended modifications for hepatic toxicity are summarized in Table 2.

Pancreatitis and Elevation of Lipase
Recommended modifications for pancreatic adverse reactions are summarized in Table 3.

Dose Modification for Use With Strong CYP3A Inhibitors
The recommended dose should be reduced to 30 mg once daily when administering ponatinib hydrochloride with strong CYP3A inhibitors.
Dose Modification for Use in Patients with Hepatic Impairment
The recommended starting dose is 30 mg once daily in patients with hepatic impairment (Child-Pugh A, B, or C)
DOSAGE FORMS AND STRENGTHS
- 15 mg and 45 mg round, white, film-coated tablets.
|offLabelAdultGuideSupport=There is limited information regarding Off-Label Guideline-Supported Use of Ponatinib hydrochloride in adult patients. |offLabelAdultNoGuideSupport=There is limited information regarding Off-Label Non–Guideline-Supported Use of Ponatinib hydrochloride in adult patients.
|fdaLIADPed=There is limited information regarding FDA-Labeled Use of Ponatinib hydrochloride in pediatric patients.
|offLabelPedGuideSupport=There is limited information regarding Off-Label Guideline-Supported Use of Ponatinib hydrochloride in pediatric patients.
|offLabelPedNoGuideSupport=There is limited information regarding Off-Label Non–Guideline-Supported Use of Ponatinib hydrochloride in pediatric patients.
|contraindications=* None
|warnings=Vascular Occlusion
- Arterial and venous thrombosis and occlusions, including fatal myocardial infarction, stroke, stenosis of large arterial vessels of the brain, severe peripheral vascular disease, and the need for urgent revascularization procedures have occurred in at least 27% of ponatinib hydrochloride-treated patients from the phase 1 and phase 2 trials. Ponatinib hydrochloride can cause fatal and life-threatening vascular occlusion within 2 weeks of starting treatment. Ponatinib hydrochloride can also cause recurrent or multi-site vascular occlusion.
- In the dose-escalation (phase 1) clinical trial, 48% (31/65) of patients with CML or Ph+ ALL developed vascular occlusive events. The median time to onset of the first vascular occlusion event was 5 months. Ponatinib hydrochloride can cause fatal and life-threatening vascular occlusion in patients treated at dose levels as low as 15 mg per day.
- Patients with and without cardiovascular risk factors, including patients age 50 years or younger, experienced these events. Vascular occlusion adverse events were more frequent with increasing age and in patients with prior history of ischemia, hypertension, diabetes, or hyperlipidemia (see TABLE 4).

Arterial Occlusion and Thrombosis
- Arterial occlusion and thrombosis occurred in at least 20% (91/449) of ponatinib hydrochloride-treated patients with some patients experiencing events of more than one type. Patients have required revascularization procedures (cerebrovascular, coronary, and peripheral arterial) due to vascular occlusion from ponatinib hydrochloride.
- Cardiac vascular occlusion, including fatal and life-threatening myocardial infarction and coronary artery occlusion has occurred in 12% (55/449) of ponatinib hydrochloride-treated patients. Patients have developed heart failure concurrent or subsequent to the myocardial ischemic event.
- Cerebrovascular occlusion, including fatal stroke, has occurred in 6% (27/449) of ponatinib hydrochloride-treated patients. Ponatinib hydrochloride can cause stenosis over multiple segments in major arterial vessels that supply the brain (e.g., carotid, vertebral, middle cerebral artery).
- Peripheral arterial occlusive events, including fatal mesenteric artery occlusion and life-threatening peripheral arterial disease, have occurred in 8% (36/449) of ponatinib hydrochloride-treated patients. Patients have developed digital or distal extremity necrosis and have required amputations.
- Clinicians should consider whether the benefits of ponatinib hydrochloride treatment are expected to exceed the risks of therapy. In patients suspected of developing arterial thrombotic events, interrupt or stop ponatinib hydrochloride. A benefit-risk consideration should guide a decision to restart ponatinib hydrochloride therapy. .
Venous Thromboembolism
- Venous thromboembolic events occurred in 5% (23/449) of ponatinib hydrochloride-treated patients, including deep venous thrombosis (8 patients), pulmonary embolism (6 patients), superficial thrombophlebitis (3 patients), and retinal vein thrombosis (2 patients). Consider dose modification or discontinuation of ponatinib hydrochloride in patients who develop serious venous thromboembolism
Heart Failure
Fatal and serious heart failure or left ventricular dysfunction occurred in 5% of ponatinib hydrochloride-treated patients (N =22). Eight percent of patients (N= 35) experienced any grade of heart failure or left ventricular dysfunction. Monitor patients for signs or symptoms consistent with heart failure and treat as clinically indicated, including interruption of ponatinib hydrochloride. Consider discontinuation of ponatinib hydrochloride in patients who develop serious heart failure.
Hepatotoxicity
- Ponatinib hydrochloride can cause hepatotoxicity, including liver failure and death. Fulminant hepatic failure leading to death occurred in an ponatinib hydrochloride-treated patient within one week of starting ponatinib hydrochloride. Two additional fatal cases of acute liver failure also occurred. The fatal cases occurred in patients with blast phase (BP) CML or Ph+ ALL. Severe hepatotoxicity occurred in all disease cohorts.
- The incidence of aspartate aminotransferase (ALT) or alanine aminotransferase (AST) elevation was 56% (all grades) and 8% (grade 3 or 4). Ponatinib hydrochloride treatment may result in elevation in ALT, AST, or both. ALT or AST elevation was not reversed by the date of last follow-up in 5% of patients.
- Monitor liver function tests at baseline, then at least monthly or as clinically indicated. Interrupt, reduce or discontinue ponatinib hydrochloride as clinically indicated.
Hypertension
- Treatment-emergent hypertension occurred in 67% of patients (300/449). Eight patients (2%) treated with ponatinib hydrochloride in clinical trials experienced treatment-emergent symptomatic hypertension as a serious adverse reaction, including hypertensive crisis. Patients may require urgent clinical intervention for hypertension associated with confusion, headache, chest pain, or shortness of breath. In patients with baseline systolic BP<140 mm Hg and baseline diastolic BP<90mm Hg, 78% (220/282) experienced treatment-emergent hypertension; 49% (139/282) developed Stage 1 hypertension (defined as systolic BP≥140 mm Hg or diastolic BP≥90 mm Hg) while 29% developed Stage 2 hypertension (defined as systolic BP≥160 mm Hg or diastolic BP≥100 mm Hg). In 131 patients with Stage 1 hypertension at baseline, 61% (80/131) developed Stage 2 hypertension. Monitor and manage blood pressure elevations during ponatinib hydrochloride use and treat hypertension to normalize blood pressure. Interrupt, dose reduce, or stop ponatinib hydrochloride if hypertension is not medically controlled.
Pancreatitis
- Clinical pancreatitis occurred in 6% (28/449) of patients (5% grade 3) treated with ponatinib hydrochloride. Pancreatitis resulted in discontinuation or treatment interruption in 6% of patients (25/449). Twenty-two of the 28 cases of pancreatitis resolved within 2 weeks with dose interruption or reduction. The incidence of treatment-emergent lipase elevation was 41%.
- Check serum lipase every 2 weeks for the first 2 months and then monthly thereafter or as clinically indicated. Consider additional serum lipase monitoring in patients with a history of pancreatitis or alcohol abuse. Dose interruption or reduction may be required. In cases where lipase elevations are accompanied by abdominal symptoms, interrupt treatment with ponatinib hydrochloride and evaluate patients for pancreatitis. Do not consider restarting ponatinib hydrochloride until patients have complete resolution of symptoms and lipase levels are less than 1.5 × ULN.
Neuropathy
- Peripheral and cranial neuropathy have occurred in ponatinib hydrochloride-treated patients. Overall, 13% (59/449) of ponatinib hydrochloride-treated patients experienced a peripheral neuropathy event of any grade (2%, grade 3/4). In clinical trials, the most common peripheral neuropathies reported were peripheral neuropathy (4%, 18/449), paresthesia (4%, 17/449), hypoesthesia (2%, 11/449), and hyperesthesia (1%, 5/449). Cranial neuropathy developed in 1% (6/449) of ponatinib hydrochloride-treated patients (<1% grade 3/4).
- Of the patients who developed neuropathy, 31% (20/65) developed neuropathy during the first month of treatment. Monitor patients for symptoms of neuropathy, such as hypoesthesia, hyperesthesia, paresthesia, discomfort, a burning sensation, neuropathic pain or weakness. Consider interrupting ponatinib hydrochloride and evaluate if neuropathy is suspected.
Ocular Toxicity
- Serious ocular toxicities leading to blindness or blurred vision have occurred in ponatinib hydrochloride-treated patients. Retinal toxicities including macular edema, retinal vein occlusion, and retinal hemorrhage occurred in 3% of ponatinib hydrochloride-treated patients. Conjunctival or corneal irritation, dry eye, or eye pain occurred in 13% of patients. Visual blurring occurred in 6% of patients. Other ocular toxicities include cataracts, glaucoma, iritis, iridocyclitis, and ulcerative keratitis. Conduct comprehensive eye exams at baseline and periodically during treatment.
Hemorrhage
- Serious bleeding events, including fatalities, occurred in 5% (22/449) of patients treated with ponatinib hydrochloride. Hemorrhage occurred in 24% of patients. The incidence of serious bleeding events was higher in patients with AP-CML, BP-CML, and Ph+ ALL. Cerebral hemorrhage and gastrointestinal hemorrhage were the most commonly reported serious bleeding events. Most hemorrhagic events, but not all, occurred in patients with grade 4 thrombocytopenia . Interrupt ponatinib hydrochloride for serious or severe hemorrhage and evaluate.
Fluid Retention
- Fluid retention events judged as serious occurred in 3% (13/449) of patients treated with ponatinib hydrochloride. One instance of brain edema was fatal. Serious fluid retention events in more than 1 patient included: pericardial effusion (6/449, 1%), pleural effusion (5/449, 1%), and ascites (2/449, <1%).
- In total, fluid retention occurred in 23% of the patients. The most common fluid retention events were peripheral edema (16%), pleural effusion (7%), and pericardial effusion (3%).
- Monitor patients for fluid retention and manage patients as clinically indicated. Interrupt, reduce, or discontinue ponatinib hydrochloride as clinically indicated.
Cardiac Arrhythmias
- Symptomatic bradyarrhythmias that led to a requirement for pacemaker implantation occurred in 1% (3/449) of ponatinib hydrochloride-treated patients. The cardiac rhythms (1 case each) identified were complete heart block, sick sinus syndrome, and atrial fibrillation with bradycardia and pauses. Advise patients to report signs and symptoms suggestive of slow heart rate (fainting, dizziness, or chest pain). Interrupt ponatinib hydrochloride and evaluate.
- Supraventricular tachyarrhythmias occurred in 5% (25/449) of ponatinib hydrochloride-treated patients. Atrial fibrillation was the most common supraventricular tachyarrhythmia and occurred in 20 patients. The other supraventricular tachyarrhythmias were atrial flutter (4 patients), supraventricular tachycardia (4 patients), and atrial tachycardia (1 patient). For 13 patients, the event led to hospitalization. Advise patients to report signs and symptoms of rapid heart rate (palpitations, dizziness). Interrupt ponatinib hydrochloride and evaluate.
Myelosuppression
- Severe (grade 3 or 4) myelosuppression occurred in 48% (215/449) of patients treated with ponatinib hydrochloride. The incidence of these events was greater in patients with AP-CML, BP-CML, and Ph+ALL than in patients with CP-CML. Obtain complete blood counts every 2 weeks for the first 3 months and then monthly or as clinically indicated, and adjust the dose as recommended.
Tumor Lysis Syndrome
- Two patients (<1%) treated with ponatinib hydrochloride developed serious tumor lysis syndrome. Both cases occurred in patients with advanced CML. Hyperuricemia occurred in 7% (30/449) of patients; the majority had CP-CML (19 patients). Due to the potential for tumor lysis syndrome in patients with advanced disease (AP-CML, BP-CML, or Ph+ ALL), ensure adequate hydration and treat high uric acid levels prior to initiating therapy with ponatinib hydrochloride.
Compromised Wound Healing and Gastrointestinal Perforation
- No formal studies of the effect of ponatinib hydrochloride on wound healing have been conducted. Based on the mechanism of action, ponatinib hydrochloride could compromise wound healing. Serious gastrointestinal perforation (fistula) occurred in one patient 38 days post-cholecystectomy.
- Interrupt ponatinib hydrochloride for at least 1 week prior to major surgery. The decision when to resume ponatinib hydrochloride after surgery should be based on clinical judgment of adequate wound healing.
Embryo-Fetal Toxicity
- Ponatinib hydrochloride can cause fetal harm when administered to a pregnant woman based on its mechanism of action and findings in animals. Ponatinib caused embryo-fetal toxicity in rats at exposures lower than human exposures at the recommended human dose. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential hazard to the fetus. Advise women to avoid pregnancy while taking ponatinib hydrochloride
|clinicalTrials=* Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
- The following adverse reactions are discussed in greater detail in other sections of the prescribing information:
- Vascular Occlusion
- Heart Failure
- Hepatotoxicity
- Hypertension
- Pancreatitis
- Neuropathy
- Ocular Toxicity
- Hemorrhage
- Fluid Retention
- Cardiac Arrhythmias
- Myelosuppression
- The adverse reactions described in this section were identified in a single-arm, open-label, international, multicenter trial in 449 patients with CML or Ph+ ALL whose disease was considered to be resistant or intolerant to prior tyrosine kinase inhibitor (TKI) therapy including those with the BCR-ABL T315I mutation. All patients received a starting dose of 45 mg ponatinib hydrochloride once daily. At the time of analysis, the median duration of treatment with ponatinib hydrochloride was 337 days in patients with CP-CML, 362 days in patients with AP-CML, 89 days in patients with BP-CML, and 81 days in patients with Ph+ ALL. The median dose intensity was 37 mg or 83% of the expected 45 mg dose. The events of arterial ischemia, cardiac failure, and peripheral neuropathy reported in Tables 5 and 6 below include data from an additional 13 months of follow-up (median duration of treatment CP-CML: 672 days, AP-CML: 590 days, BP-CML: 89 days, Ph+ ALL: 81 days).
- Adverse reactions reported in more than 10% of all patients treated with ponatinib hydrochloride in this trial are presented in Table 5. Overall, the most common non-hematologic adverse reactions (≥ 20%) were hypertension, rash, abdominal pain, fatigue, headache, dry skin, constipation, arthralgia, nausea, and pyrexia.
- The rates of treatment-emergent adverse events resulting in discontinuation were 13% in CP-CML, 11% in AP-CML, 15% in BP-CML, and 9% in Ph+ ALL. The most common adverse events that led to treatment discontinuation were thrombocytopenia (4%) and infections (1%).
- Dose modifications (dose delays or dose reductions) due to adverse reactions occurred in 74% of the patients. The most common adverse reactions (≥5%) that led to dose modifications include thrombocytopenia (30%), neutropenia (13%), lipase increased (12%), rash (11%), abdominal pain (11%), pancreatitis (6%), and ALT, AST, or GGT increased (6%).


Laboratory Abnormalities
- Myelosuppression was commonly reported in all patient populations. The frequency of grade 3 or 4 thrombocytopenia, neutropenia, and anemia was higher in patients with AP-CML, BP-CML, and Ph+ ALL than in patients with CP-CML

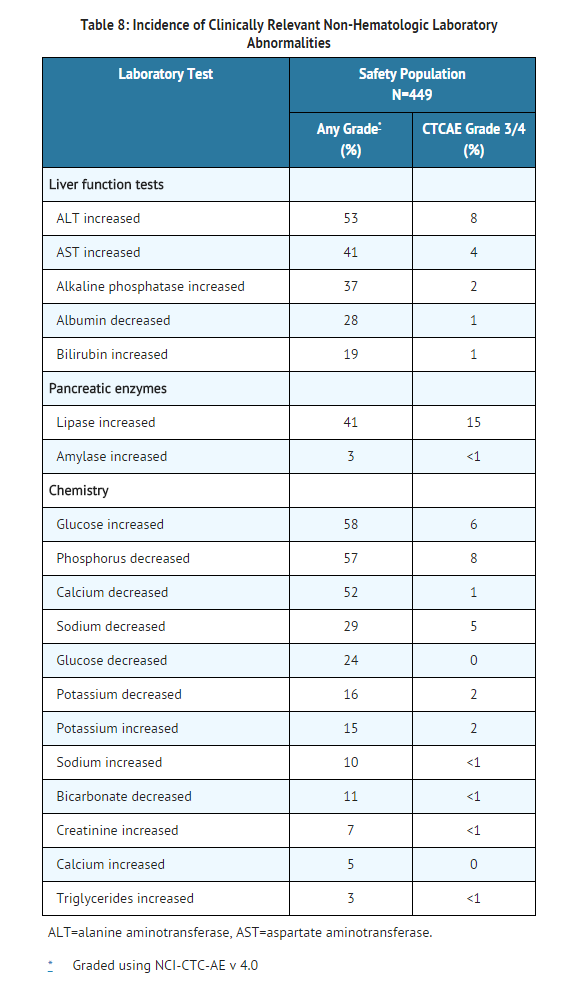
|postmarketing=There is limited information regarding Postmarketing Experience of Ponatinib hydrochloride in the drug label. |drugInteractions=* Based on in vitro studies, ponatinib is a substrate of CYP3A and to a lesser extent CYP2C8 and CYP2D6. Ponatinib also inhibits the P-glycoprotein (P-gp), ATP-binding cassette G2 (ABCG2) [also known as BCRP], and bile salt export pump (BSEP) transporter systems in vitro.
Drugs That Are Strong Inhibitors of CYP3A Enzymes
- In a drug interaction study in healthy volunteers, co-administration of ponatinib hydrochloride with ketoconazole increased plasma ponatinib AUC0-inf and Cmax by 78% and 47%, respectively. When administering ponatinib hydrochloride with strong CYP3A inhibitors (e.g., boceprevir, clarithromycin, conivaptan, grapefruit juice, indinavir, itraconazole, ketoconazole, lopinavir/ritonavir, nefazodone, nelfinavir, posaconazole, ritonavir, saquinavir, telaprevir, telithromycin, voriconazole), the recommended starting dose should be reduced. Patients taking concomitant strong CYP3A inhibitors may be at increased risk for adverse reactions.
Drugs That Are Strong Inducers of CYP3A Enzymes
- Coadministration of strong CYP3A inducers (e.g., carbamazepine, phenytoin, rifampin, and St. John's Wort) with ponatinib hydrochloride should be avoided unless the benefit outweighs the risk of decreased ponatinib exposure. Monitor patients for reduced efficacy. Selection of concomitant medication with no or minimal CYP3A induction potential is recommended. In a drug interaction study in healthy volunteers, co-administration of ponatinib hydrochloride following multiple doses of rifampin resulted in decreased ponatinib AUC0-inf and Cmax values by 62% and 42%, respectively.
Drugs That Elevate Gastric pH
- Ponatinib hydrochloride may be co-administered with gastric pH-elevating medications. In a drug interaction study in healthy volunteers, co-administration of ponatinib hydrochloride following multiple doses of lansoprazole resulted in a minimal (6%) decrease in ponatinib exposure.
Drugs That Are Substrates of the P-gp or ABCG2 Transporter Systems
- In vitro studies demonstrate that ponatinib hydrochloride inhibits the P-gp and ABCG2 transporter systems. The effect of coadministration of ponatinib hydrochloride with sensitive substrates of the P-gp (e.g., aliskiren, ambrisentan, colchicine, dabigatran etexilate, digoxin, everolimus, fexofenadine, imatinib, lapatinib, maraviroc, nilotinib, posaconazole, ranolazine, saxagliptin, sirolimus, sitagliptin, tolvaptan, topotecan) and ABCG2 (e.g., methotrexate, mitoxantrone, imatinib, irinotecan, lapatinib, rosuvastatin, sulfasalazine, topotecan) transporter systems on exposure of these substrates has not been evaluated in clinical studies.
|useInPregnancyFDA=Pregnancy Category D
Risk Summary
- Based on its mechanism of action and findings in animals, ponatinib hydrochloride can cause fetal harm when administered to a pregnant woman. There are no adequate and well-controlled studies with ponatinib hydrochloride in pregnant women. Advise women to avoid becoming pregnant while taking ponatinib hydrochloride. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential hazard to a fetus.
Animal Data
- Ponatinib was studied for effects on embryo-fetal development in pregnant rats given oral doses of 0.3, 1, and 3 mg/kg/day during organogenesis. At the maternally toxic dose of 3 mg/kg/day (equivalent to the AUC in patients receiving the recommended dose of 45 mg/day), ponatinib caused embryo-fetal toxicity as shown by increased resorptions, reduced body weight, external alterations, multiple soft tissue and skeletal alterations, and reduced ossification. Embryo-fetal toxicities also were observed at 1 mg/kg/day (approximately 24% the AUC in patients receiving the recommended dose) and involved multiple fetal soft tissue and skeletal alterations, including reduced ossification.
|useInPregnancyAUS=* Australian Drug Evaluation Committee (ADEC) Pregnancy Category
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Ponatinib hydrochloride in women who are pregnant. |useInLaborDelivery=There is no FDA guidance on use of Ponatinib hydrochloride during labor and delivery. |useInNursing=* It is unknown whether ponatinib is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from ponatinib, a decision should be made whether to discontinue nursing or to discontinue ponatinib hydrochloride, taking into account the importance of the drug to the mother. |useInPed=* The safety and efficacy of ponatinib hydrochloride in patients less than 18 years of age have not been established. |useInGeri=* One hundred and fifty-five of 449 patients (35%) in the clinical trial of ponatinib hydrochloride were 65 years of age and over. In patients with CP-CML, patients of age ≥ 65 years had a lower major cytogenetic response rate (38%) as compared with patients < 65 years of age (64%). In patients with AP-CML, BP-CML, and Ph+ ALL, patients of age ≥ 65 years had a higher major hematologic response rate (47%) as compared with patients < 65 years of age (40%). Forty-six percent of patients ≥ 65 years had vascular occlusion events. Patients of age ≥ 65 years are more likely to experience adverse reactions including vascular occlusion decreased platelet count, peripheral edema, increased lipase, dyspnea, asthenia, muscle spasms, and decreased appetite. In general, dose selection for an elderly patient should be cautious, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy. |useInGender=There is no FDA guidance on the use of Ponatinib hydrochloride with respect to specific gender populations. |useInRace=There is no FDA guidance on the use of Ponatinib hydrochloride with respect to specific racial populations. |useInRenalImpair=* Ponatinib hydrochloride has not been studied in patients with renal impairment. Although renal excretion is not a major route of ponatinib elimination, the potential for moderate or severe renal impairment to affect hepatic elimination has not been determined. |useInHepaticImpair=* Administer ponatinib hydrochloride at a dose of 30 mg once daily in patients with hepatic impairment (Child-Pugh A, B, or C).
- In a single-dose (30 mg) pharmacokinetic (PK) study; compared to subjects with normal liver function, no major differences in ponatinib PK were observed in subjects with hepatic impairment (Child-Pugh A, B, or C). However, there was an increased overall incidence of adverse reactions (e.g., gastrointestinal disorders, including a case of severe pancreatitis) in the subjects with hepatic impairment following the single 30 mg dose compared to subjects with normal liver function. The safety of multiple ponatinib doses, or doses higher than 30 mg have not been studied in patients with hepatic
|useInReproPotential=There is no FDA guidance on the use of Ponatinib hydrochloride in women of reproductive potentials and males. |useInImmunocomp=There is no FDA guidance one the use of Ponatinib hydrochloride in patients who are immunocompromised. |administration=* Oral |monitoring=There is limited information regarding Monitoring of Ponatinib hydrochloride in the drug label. |IVCompat=There is limited information regarding IV Compatibility of Ponatinib hydrochloride in the drug label. |overdose=* Overdoses with ponatinib hydrochloride were reported in clinical trials. One patient was accidentally administered the entire contents of a bottle of study medication via nasogastric tube. The investigator estimated that the patient received 540 mg of ponatinib hydrochloride. Two hours after the overdose, the patient had an uncorrected QT interval of 520 ms. Subsequent ECGs showed normal sinus rhythm with uncorrected QT intervals of 480 and 400 ms. The patient died 9 days after the overdose from pneumonia and sepsis. Another patient accidentally self-administered 165 mg on cycle 1 day 2. The patient experienced fatigue and non-cardiac chest pain on day 3. Multiple doses of 90 mg per day for 12 days in a patient resulted in pneumonia, systemic inflammatory response, atrial fibrillation, and a moderate pericardial effusion.
- In the event of an overdose of ponatinib hydrochloride, stop ponatinib hydrochloride, observe the patient and provide appropriate supportive treatment.
|mechAction=* Ponatinib is a kinase inhibitor. Ponatinib inhibited the in vitro tyrosine kinase activity of ABL and T315I mutant ABL with IC50 concentrations of 0.4 and 2.0 nM, respectively. Ponatinib inhibited the in vitro activity of additional kinases with IC50 concentrations between 0.1 and 20 nM, including members of the VEGFR, PDGFR, FGFR, EPH receptors and SRC families of kinases, and KIT, RET, TIE2, and FLT3. Ponatinib inhibited the in vitro viability of cells expressing native or mutant BCR-ABL, including T315I. In mice, treatment with ponatinib reduced the size of tumors expressing native or T315I mutant BCR-ABL when compared to controls. |structure=* ponatinib hydrochloride (ponatinib) is a kinase inhibitor. The chemical name for ponatinib hydrochloride is 3-(imidazo[1,2-b]pyridazin-3-ylethynyl)-4-methyl-N-{4-[(4-methylpiperazin-1-yl)methyl]-3-(trifluoromethyl)phenyl}benzamide hydrochloride. The molecular formula is C29H28ClF3N6O which corresponds to a formula weight of 569.02 g/mol. Its structure is shown below:

- Ponatinib HCl is an off-white to yellow powder with pKa of 2.77 and 7.8. The solubility of ponatinib in pH 1.7, 2.7, and 7.5 buffers is 7790 mcg/ml, 3.44 mcg/ml, and 0.16 mcg/ml, respectively, indicating a decrease in solubility with increasing pH. Ponatinib hydrochloride tablets are available as white, round, film-coated tablets for oral administration. Each tablet contains ponatinib hydrochloride equivalent to 15 or 45 mg ponatinib with the following inactive ingredients: lactose monohydrate, microcrystalline cellulose, sodium starch glycolate (type B), colloidal silicon dioxide, magnesium stearate and a tablet coating. The tablet coating consists of talc, polyethylene glycol, polyvinyl alcohol, and titanium dioxide.
|PD=* In a cell-based assay, ponatinib concentrations of 20 nM (10.65 ng/mL) were sufficient to suppress most BCR-ABL mutant clones. However, ponatinib concentrations of 40 nM (21.3 ng/mL) were required to suppress T315I mutants. The median and range of steady-state Cmax and trough (Cmin) concentrations of ponatinib following 29 days of once-daily dosing of 15 mg, 30 mg and 45 mg are listed in Table 9.

- Concentrations of ponatinib shown in cell-based assays to suppress unmutated BCR-ABL and most mutant BCR-ABL clones may be achieved at once daily dosing of 15 mg or 30 mg.
- The dose intensity-safety relationship indicated that there are significant increases in grade ≥ 3 adverse events (hypertension, thrombocytopenia, pancreatitis, neutropenia, rash, ALT increase, AST increase, lipase increase, myelosuppression) over the dose range of 15 to 45 mg once-daily.
- In vitro, there was no significant inhibition of platelet aggregation with ponatinib at concentrations seen clinically and up to 0.7 μg/mL (1.23 μM).
Cardiac Electrophysiology
- A QT assessment was performed in 39 patients with cancer who received 30 mg, 45 mg, or 60 mg ponatinib hydrochloride once daily. No large changes in the mean QTc interval (i.e., > 20 ms) from baseline were detected in the study. However, a small increase in the mean QTc interval (i.e., < 10 ms) cannot be excluded because of study design limitations.
|PK=* The geometric mean (CV%) Cmax and AUC(0-τ) of ponatinib hydrochloride 45 mg daily at presumed steady state in patients with advanced hematologic malignancies were 73 ng/mL (74%) and 1253 ng•hr/mL (73%), respectively. Ponatinib administered as an investigational capsule formulation to patients with cancer exhibited approximately dose proportional increases in both Cmax and AUC over the dose range of 15 to 60 mg. A dose intensity safety analysis showed a significant increase in grade 3 or higher adverse reactions (i.e., thrombocytopenia, neutropenia, rash, ALT elevation, AST elevation, pancreatitis, and lipase elevation) with an increase in dose intensity.
Absorption
- The absolute bioavailability of ponatinib is unknown. Peak concentrations of ponatinib are observed within 6 hours after ponatinib hydrochloride oral administration. Following ingestion of either a high-fat or low-fat meal by 22 healthy volunteers, plasma ponatinib exposures (AUC and Cmax) were not different when compared to fasting conditions.
Distribution
- Ponatinib is greater than 99% bound to plasma proteins in vitro. There was no plasma protein binding displacement of ponatinib (145 nM) in vitro by other highly protein bound medications (ibuprofen, nifedipine, propranolol, salicylic acid, and warfarin). The geometric mean (CV%) apparent steady state volume of distribution is 1223 liters (102%) following oral administration of ponatinib hydrochloride 45 mg once daily for 28 days in patients with cancer. Ponatinib is a weak substrate for both P-gp and ABCG2 in vitro. Ponatinib is not a substrate for organic anion transporting polypeptides (OATP1B1, OATP1B3) and organic cation transporter 1 (OCT1) in vitro.
Metabolism
- At least 64% of a ponatinib dose undergoes phase I and phase II metabolism. CYP3A4 and to a lesser extent CYP2C8, CYP2D6 and CYP3A5 are involved in the phase I metabolism of ponatinib in vitro. Ponatinib is also metabolized by esterases and/or amidases.
Elimination
- The geometric mean (range) terminal elimination half-life of ponatinib was approximately 24 (12 to 66) hours following ponatinib hydrochloride 45 mg oral administration once daily for 28 days in patients with cancer. Exposure increased by approximately 90% (median) [range: 20% to 440%] between the first dose and presumed steady state. Ponatinib is mainly eliminated via feces. Following a single oral dose of [14C]-labeled ponatinib, approximately 87% of the radioactive dose is recovered in the feces and approximately 5% in the urine.
Drug Interactions
Coadministration of Ponatinib and CYP3A Inhibitors
- Coadministration of a single 15 mg oral dose of ponatinib in the presence of ketoconazole (400 mg daily), a strong CYP3A inhibitor, to 22 healthy volunteers, increased the AUC0-inf and Cmax of ponatinib by 78% and 47%, respectively, when compared to administration of ponatinib alone.
Coadministration of Ponatinib and CYP3A Inducers
- Co-administration of a single 45 mg dose of ponatinib in the presence of rifampin (600 mg daily), a strong CYP3A inducer, to 19 healthy volunteers, decreased the AUC0-inf and Cmax of ponatinib by 62% and 42%, respectively, when compared to administration of ponatinib alone.
Coadministration With Other CYP Substrates
- In vitro studies indicate that ponatinib does not inhibit the metabolism of substrates for CYP1A2, CYP2B6, CYP2C8, CYP2C9, CYP2C19, CYP3A, or CYP2D6 and does not induce the metabolism of substrates for CYP1A2, CYP2B6, or CYP3A.
Coadministration With Substrates of Transporters
- In vitro, ponatinib is an inhibitor of P-gp and ABCG2, and BSEP.
- In vitro, ponatinib did not inhibit the human organic anion transporting polypeptides OATP1B1 or OATP1B3, or the organic cation transporters OCT1, OCT2, OAT1, and OAT3.
Coadministration of Ponatinib and Gastric pH elevating Medications
- The aqueous solubility of ponatinib is pH dependent, with higher pH resulting in lower solubility [see DESCRIPTION (11)]. Co-administration of a single 45 mg dose of ponatinib in the presence of lansoprazole (60 mg daily), a proton pump inhibitor, to 18 healthy volunteers decreased the AUC0-inf and Cmax of ponatinib by 6% and 25%, respectively, when compared to administration of ponatinib alone.
Pharmacokinetics in Specific Populations
Hepatic Impairment
- A single 30 mg oral dose of ponatinib was administered to subjects with normal liver function (N=8) and to subjects with mild [Child-Pugh A (N=6)], moderate [Child-Pugh B (N=6)], and severe [Child-Pugh C (N=4)] hepatic impairment. Compared to subjects with normal liver function, there was no trend of increased ponatinib exposure in subjects with hepatic impairment. There was an increased incidence of adverse reactions in patients with hepatic impairment compared to subjects with normal liver function.
Renal Impairment
- Ponatinib hydrochloride has not been studied in patients with renal impairment. Although renal excretion is not a major route of ponatinib elimination, the potential for moderate or severe renal impairment to affect hepatic elimination has not been determined.
|nonClinToxic=Carcinogenesis, Mutagenesis, Impairment of Fertility
- Carcinogenicity studies have not been performed with ponatinib.
- Ponatinib was not mutagenic in a bacterial mutagenesis (Ames) assay, was not clastogenic in a chromosome aberration assay in human lymphocytes, nor was it clastogenic in an in vivo mouse micronucleus assay at oral doses up to 2000 mg/kg.
- Ponatinib may impair male and female fertility. Fertility studies using ponatinib were not conducted. However, ponatinib effects on male and female reproductive organs observed during general toxicology studies included degeneration of epithelium of the testes in rats and monkeys and follicular atresia in the monkey ovary with associated endometrial atrophy. Effects seen in rats were at exposures approximating the AUC in patients receiving the recommended dose of 45 mg/day and in monkeys were approximately 4 times the AUC in patients.
|clinicalStudies=* The safety and efficacy of ponatinib hydrochloride in patients with CML and Ph+ ALL whose disease was considered to be resistant or intolerant to prior tyrosine kinase inhibitor (TKI) therapy were evaluated in a single-arm, open-label, international, multicenter trial. Efficacy results described below should be interpreted within the context of updated safety information.
- All patients were administered a starting dose of 45 mg of ponatinib hydrochloride once daily. Patients were assigned to one of six cohorts based on disease phase (chronic phase CML [CP-CML]; accelerated phase CML [AP-CML]; or blast phase CML /Philadelphia-positive acute lymphoblastic leukemia [BP-CML/Ph+ ALL]), resistance or intolerance (R/I) to prior TKI therapy, and the presence of the T315I mutation.
- Resistance in CP-CML while on prior TKI therapy, was defined as failure to achieve either a complete hematologic response (by 3 months), a minor cytogenetic response (by 6 months), or a major cytogenetic response (by 12 months). Patients with CP-CML who experienced a loss of response or development of a kinase domain mutation in the absence of a complete cytogenetic response or progression to AP-CML or BP-CML at any time on prior TKI therapy were also considered resistant. Resistance in AP-CML, BP-CML, and Ph+ ALL was defined as failure to achieve either a major hematologic response (by 3 months in AP-CML, and by 1 month in BP-CML and Ph+ ALL), loss of major hematologic response (at any time), or development of a kinase domain mutation in the absence of a complete major hematologic response while on prior TKI therapy.
- Intolerance was defined as the discontinuation of prior TKI therapy due to toxicities despite optimal management in the absence of a complete cytogenetic response in patients with CP-CML or major hematologic response for patients with AP-CML, BP-CML, or Ph+ ALL.
- The primary efficacy endpoint in CP-CML was major cytogenetic response (MCyR), which included complete and partial cytogenetic responses (CCyR and PCyR). The primary efficacy endpoint in AP-CML, BP-CML, and Ph+ ALL was major hematologic response (MaHR), defined as either a complete hematologic response (CHR) or no evidence of leukemia (NEL).
- The trial enrolled 449 patients, of which 444 were eligible for efficacy analysis: 267 patients with CP-CML (R/I Cohort: n=203, T315I: n=64), 83 patients with AP-CML, 62 patients with BP-CML, and 32 patients with Ph+ ALL. Five patients were not eligible for efficacy analysis due to lack of confirmation of T315I mutation status, and these patients had not received prior dasatinib or nilotinib.
- At the time of analysis, the median follow-up was 10 months (minimum of 6 months of follow-up for all ongoing patients). Baseline demographic characteristics are described in Table 10.

At the time of analysis, the median duration of ponatinib hydrochloride treatment was 281 days in patients with CP-CML, 286 days in patients with AP-CML, 89 days in patients with BP-CML, and 81 days in patients with Ph+ ALL. Efficacy results are summarized in Table 11, and Table 12.

In patients with CP-CML patients who achieved MCyR, the median time to MCyR was 84 days (range: 49 to 334 days). At the time of analysis, the median durations of MCyR had not yet been reached.

- The median time to MaHR in patients with AP-CML, BP-CML, and Ph+ ALL was 21 days (range: 12 to 176 days), 29 days (range 12 to 113 days), and 20 days (range: 11 to 168 days), respectively. The median duration of MaHR for patients with AP-CML, BP-CML, and Ph+ ALL was 9.5 months (range: 1.1 to 17.7 months), 4.7 months (range: 1.8 to 14.1+ months), and 3.2 months (range: 1.8 to 8.8+ months), respectively.
Ponatinib hydrochloride tablets are available in the following configurations:
Iclusig tablets should be stored at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30° C (59° to 86° F) [see USP Controlled Room Temperature]. Keep away from children. |howSupplied=* Iclusig tablets are available in the following configurations:
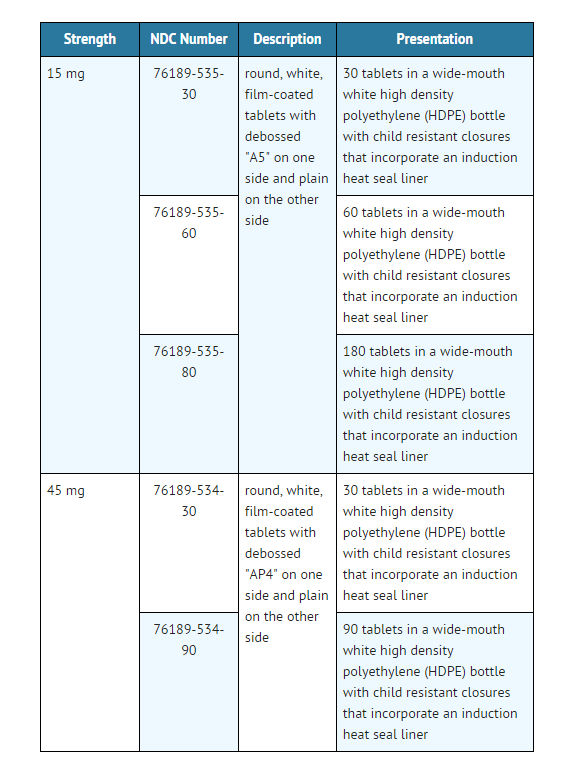
|storage=* Iclusig tablets should be stored at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30° C (59° to 86° F) [see USP Controlled Room Temperature]. Keep away from children.
|packLabel=


|fdaPatientInfo=Advise patients of the following and provide a copy of the Medication Guide:
Vascular Occlusions
Inform patients that serious arterial thromboses (including arterial stenosis sometimes requiring revascularization) and venous thromboembolism events have occurred. Advise patients to immediately contact their health care provider with any symptoms suggestive of a blood clot such as chest pain, shortness of breath, weakness on one side of the body, speech problems, leg pain, or leg swelling.
Heart Failure and Cardiac Arrhythmias
- Inform patients of the possibility of heart failure, and abnormally slow or fast heart rates. Advise patients to contact their health care provider if they experience symptoms such as shortness of breath, chest pain, palpitations, dizziness, or fainting.
Hepatotoxicity
- Inform patients of the possibility of developing liver function abnormalities and serious hepatic toxicity. Advise patients to immediately contact their health care provider if signs of liver failure occur, including jaundice, anorexia, bleeding or bruising.
Hypertension
- Inform patients of the possibility of new or worsening of existing hypertension. Advise patients to contact their health care provider for elevated blood pressure or if symptoms of hypertension occur including headache, dizziness, chest pain, or shortness of breath.
Pancreatitis
- Inform patients of the possibility of developing pancreatitis that may be accompanied by nausea, vomiting, abdominal pain, or abdominal discomfort, and to promptly report these symptoms.
Neuropathy
- Inform patients of the possibility of developing peripheral or cranial neuropathy while being treated with Iclusig. Advise patients to report symptoms of neuropathy, such as hypoesthesia, hyperesthesia, paresthesia, discomfort, a burning sensation, neuropathic pain, or weakness.
Ocular Toxicity
- Inform patients of the possibility of ocular toxicity while being treated with Iclusig. Advise patients to report symptoms of ocular toxicity, such as blurred vision, dry eye, or eye pain.
Hemorrhage
- Inform patients of the possibility of serious bleeding and to immediately contact their health care provider with any signs or symptoms suggestive of hemorrhage such as unusual bleeding or easy bruising.
Fluid Retention
- Inform patients of the possibility of developing fluid retention and to contact their health care provider for symptoms such as leg swelling, abdominal swelling, weight gain, or shortness of breath.
Myelosuppression
- Inform patients of the possibility of developing low blood cell counts; inform patients to report immediately should fever develop, particularly in association with any suggestion of infection.
Compromised Wound Healing and Gastrointestinal Perforation
- Advise patients to inform their health care provider if they plan to undergo a surgical procedure or had recent surgery.
- Inform patients that cases of gastrointestinal perforation have been reported .
Embryo-Fetal Toxicity
- Inform patients that Iclusig can cause fetal harm when administered to a pregnant woman. Advise women of the potential hazard to a fetus and to avoid becoming pregnant .
Instructions for Taking Iclusig
- Advise patients to take Iclusig exactly as prescribed and not to change their dose or to stop taking Iclusig unless they are told to do so by their health care provider. Iclusig may be taken with or without food. Iclusig tablets should be swallowed whole. Patients should not crush or dissolve the tablets.
- Patients should not take two doses at the same time to make up for a missed dose.
Lactose
- Inform patients that Iclusig contains 121 mg of lactose monohydrate in a 45 mg daily dose.
|alcohol=* Alcohol-Ponatinib hydrochloride interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
|brandNames=*Iclusig |drugShortage= }} {{#subobject:
|Page Name=Ponatinib hydrochloride
|Pill Name=No image.jpg
|Drug Name=
|Pill Ingred=|+sep=;
|Pill Imprint=
|Pill Dosage={{{dosageValue}}} {{{dosageUnit}}}
|Pill Color=|+sep=;
|Pill Shape=
|Pill Size (mm)=
|Pill Scoring=
|Pill Image=
|Drug Author=
|NDC=
}}
{{#subobject:
|Label Page=Ponatinib hydrochloride |Label Name=File:Ponatinib medication guide.png
}}