Pneumothorax pathophysiology
|
Pneumothorax Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Pneumothorax pathophysiology On the Web |
|
American Roentgen Ray Society Images of Pneumothorax pathophysiology |
|
Risk calculators and risk factors for Pneumothorax pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Feham Tariq, MD [2], Hamid Qazi, MD, BSc [3]
Overview
Pneumothorax is air in the pleural space under pressure resulting in lung collapse.The pathophysiology of each type depends on the underlying disease/etiology. Primary spontaneous pneumothorax most commonly results from the bleb (small air-filled lesions under pleural surface) rupture allowing the air to leak into the pleural space. A subclass of primary spontaneous pneumothorax is isolated familial primary spontaneous pneumothorax which is genetically associated with folliculin gene mutation. Secondary spontaneous pneumothorax occurs subsequent to underlying lung pathology such as obstructive lung disease, cystic fibrosis, diffuse parenchymal lung disease and lung cancer. In tension pneumothorax, the underlying pathophysiology most commonly is chest trauma forming a one-way valve in the pleura whereby air enters the pleural space when the pleural pressure is negative during inspiration. Pneumothorax can also result from several interventional procedures which cause penetrating or non-penetrating injury to the pleura resutling in abrupt increase in the alveolar pressure and hence, lead to alveolar rupture forming a communication with the pleura.
Pathophysiology
Anatomy and physiology of the thoracic cavity
The normal anatomy and physiology of thoracic cavity is as follows:
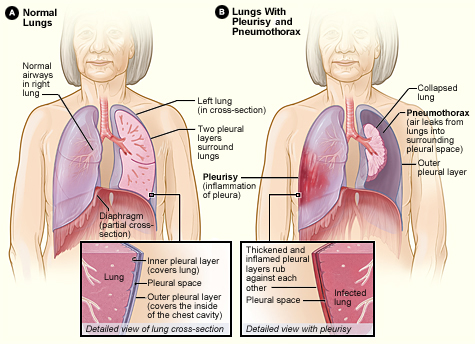
- Thoracic cavity is defined as the space inside the chest that contains the heart, lungs, and, several major blood vessels.[1][2][3]
- On either side of the cavity, a pleural membrane covers the outside surface of the lung (visceral pleura) and also lines the inside of the chest wall (parietal pleura).
- The two layers are separated by a small amount of lubricating serous fluid known as the pleural fluid.
- The lungs are fully inflated within the cavity as the pressure inside the airways is higher than the pressure inside the pleural space.
- The inhaled air does not enter the pleural space as there is no natural connections between them as well as the pressure of gases in the blood stream is too low for them to be forced into the pleural space.
- The pleural pressure is negative with respect to atmospheric pressure during spontaneous breathing.
- Air can enter the pleural space through the following mechanisms:[4][5][6]
Pathogenesis
The pathophysiology of pneumothorax depends on the underlying disease causing it.
Primary spontaneous pneumothorax
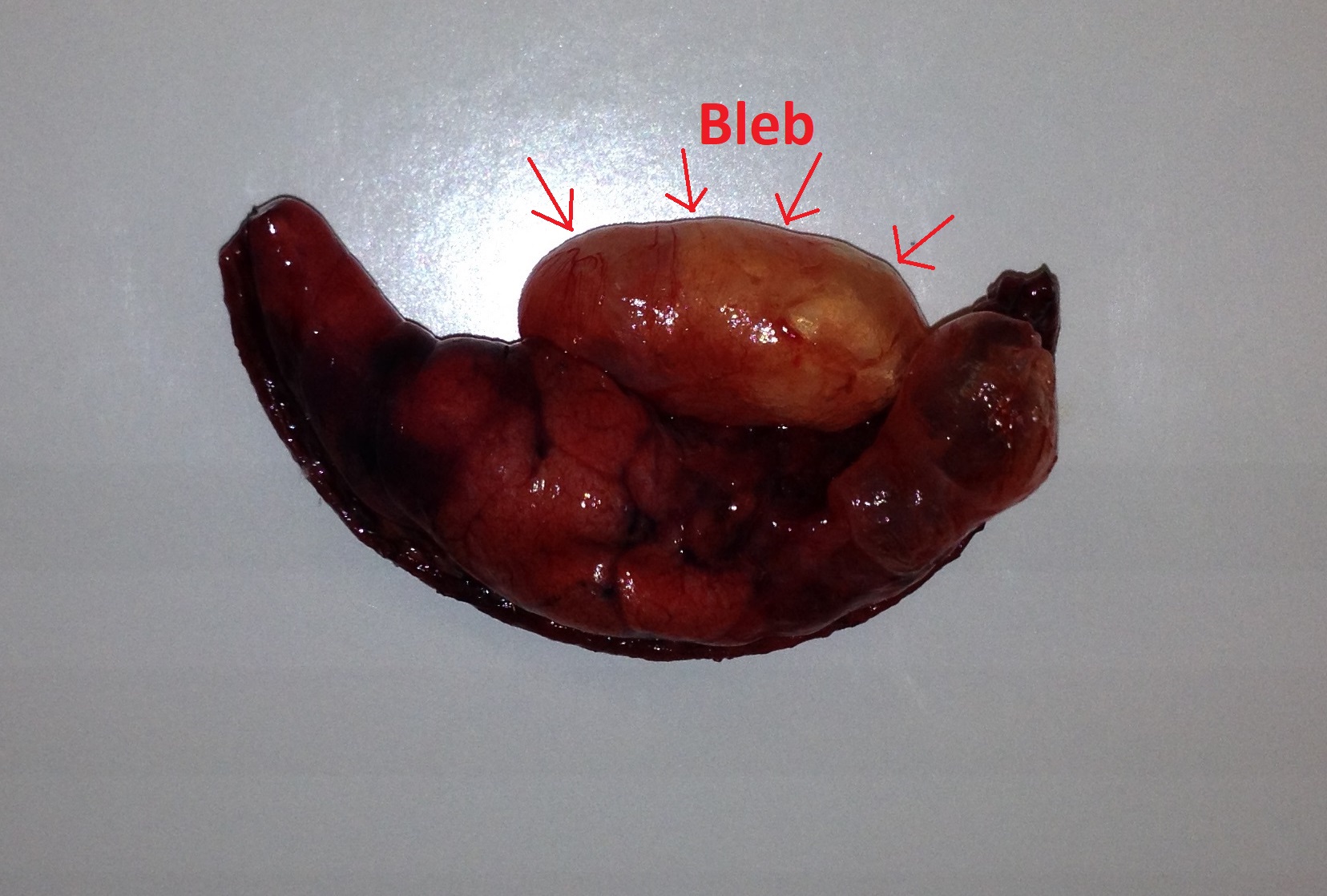
- The most common underlying pathology of primary spontaneous pneumothorax is an apical subpleural bleb (small air-filled lesions under the pleural surface).[7]
- In addition, smoking causes inflammation and obstruction of the small airways, which is responsible for the increased risk of primary spontaneous pneumothorax in smokers.
Secondary spontaneous pneumothorax
- Pneumothorax due to underlying lung disease is secondary spontaneous pneumothorax.
Tension pneumothorax
- Tension pneumothorax develops when a disruption involves the visceral pleura, parietal pleura, or the tracheobronchial tree.[8][9]
- The disruption occurs when a one-way valve forms, allowing air inflow into the pleural space, and prohibiting air outflow.
- The volume of this nonabsorbable intrapleural air increases with each inspiration.
- As a result, pressure rises within the affected hemithorax; ipsilateral lung collapses and causes hypoxia.
- Further pressure causes the mediastinum shift toward the contralateral side and compresses both, the contralateral lung and the vasculature entering the right atrium of the heart.
- This leads to worsening hypoxia and compromised venous return.
Iatrogenic pneumothorax
Following procedures commonly cause iatrogenic pneumothorax:[10][11]
- Central cannulation[12]
- Transthoracic needle aspiration
- Thoracocentesis
- Mechanical ventilation
- Thoracic acupuncture[13][14]
- Transbronchial lung biopsy or transpleural intervention
- Intravenous drug abusers using neck veins
- Aggressive cardiopulmonary resuscitation
Mechanism of injury:
- Iatrogenic pneumothorax causes penetrating or non-penetrating injury to the pleura resulting in abrupt increase in the alveolar pressure, which can lead to alveolar rupture.
- Once the alveolus is ruptured, air enters the interstitial space and dissects toward either the visceral pleura or the mediastinum.
- A pneumothorax occurs when either the visceral or the mediastinal pleura ruptures that allows air to enter the pleural space.
Genetics
Genetic association of familial primary sponatneous pneumothorax
The genetic association of familial primary sponatneous pneumothorax is as follows:[15][16][17][18][19][20]
- Primary spontaneous pneumothorax can result as a mutation in the FLCN (folliculin) gene.
- This gene codes for a protein called folliculin.
- It is produced by the cells lining the alveoli of the lung.
- Folliculin is found in the connective tissue cells that allow the lungs to contract and expand while breathing.
- It plays a role in repairing the lung tissue after damage.
- Nonsense mutation in the folliculin gene results in isolated familial sponataneous primary pneumothorax.[21]
- Altered folliculin protein can trigger the inflammatory process within the lung tissue that can alter and damage the tissue, resulting in blebs formation.
Associated Conditions
Pneumothorax is associated with the following conditions:[22][23]
- Homocystinuria
- Marfan's syndrome
- For Marfan's syndrome genetics, please click here.
- Iatrogenic buffalo chest syndrome
Gross Pathology
On gross pathology, pneumothorax has the following findings:[24][25]
- Pleuropulmonary adhesions
Microscopic Pathology
- The microscopic findings associated with pneumothorax are as follows:[26]
- Pleural fibrosis with mesothelial thickening and hyperplasia.
- Lymphocytes, eosinophils, mesothelial thickening, and proliferation of the pleura.

References
- ↑ Grundy S, Bentley A, Tschopp JM (2012). "Primary spontaneous pneumothorax: a diffuse disease of the pleura". Respiration. 83 (3): 185–9. doi:10.1159/000335993. PMID https://www.ncbi.nlm.nih.gov/pubmed/22343477 Check
|pmid=value (help). - ↑ Lee SC, Cheng YL, Huang CW, Tzao C, Hsu HH, Chang H (2008). "Simultaneous bilateral primary spontaneous pneumothorax". Respirology. 13 (1): 145–8. doi:10.1111/j.1440-1843.2007.01168.x. PMID 18197926.
- ↑ Bintcliffe, O.; Maskell, N. (2014). "Spontaneous pneumothorax". BMJ. 348 (may08 1): g2928–g2928. doi:10.1136/bmj.g2928. ISSN 1756-1833.
- ↑ Tschopp JM, Rami-Porta R, Noppen M, Astoul P (2006). "Management of spontaneous pneumothorax: state of the art". Eur Respir J. 28 (3): 637–50. doi:10.1183/09031936.06.00014206. PMID 16946095.
- ↑ Grundy, Seamus; Bentley, Andrew; Tschopp, Jean-Marie (2012). "Primary Spontaneous Pneumothorax: A Diffuse Disease of the Pleura". Respiration. 83 (3): 185–189. doi:10.1159/000335993. ISSN 1423-0356.
- ↑ Barton ED, Rhee P, Hutton KC, Rosen P (1997). "The pathophysiology of tension pneumothorax in ventilated swine". J Emerg Med. 15 (2): 147–53. PMID 9144053.
- ↑ Yazkan R, Han S (2010). "Pathophysiology, clinical evaluation and treatment options of spontaneous pneumothorax". Tuberk Toraks. 58 (3): 334–43. PMID 21038147.
- ↑ Nelson D, Porta C, Satterly S, Blair K, Johnson E, Inaba K; et al. (2013). "Physiology and cardiovascular effect of severe tension pneumothorax in a porcine model". J Surg Res. 184 (1): 450–7. doi:10.1016/j.jss.2013.05.057. PMID 23764307.
- ↑ Plewa MC, Ledrick D, Sferra JJ (1995). "Delayed tension pneumothorax complicating central venous catheterization and positive pressure ventilation". Am J Emerg Med. 13 (5): 532–5. PMID 7662057.
- ↑ Kornbau C, Lee KC, Hughes GD, Firstenberg MS (2015). "Central line complications". Int J Crit Illn Inj Sci. 5 (3): 170–8. doi:10.4103/2229-5151.164940. PMC 4613416. PMID 26557487.
- ↑ Peuker E (2004). "Case report of tension pneumothorax related to acupuncture". Acupunct Med. 22 (1): 40–3. PMID 15077937.
- ↑ Kumar M, Singh A, Sidhu KS, Kaur A (2016). "Malposition of Subclavian Venous Catheter Leading to Chest Complications". J Clin Diagn Res. 10 (5): PD16–8. doi:10.7860/JCDR/2016/19399.7860. PMC 4948479. PMID 27437303.
- ↑ Juss JK, Speed CA, Warrington J, Mahadeva R (2008). "Acupuncture induced pneumothorax - a case report". Acupunct Med. 26 (3): 193–6. PMID 18818566.
- ↑ Ramnarain D, Braams R (2002). "[Bilateral pneumothorax in a young woman after acupuncture]". Ned Tijdschr Geneeskd. 146 (4): 172–5. PMID 11845568.
- ↑ Chiu HT, Garcia CK (2006). "Familial spontaneous pneumothorax". Curr Opin Pulm Med. 12 (4): 268–72. doi:10.1097/01.mcp.0000230630.73139.f0. PMID 16825879.
- ↑ Bintcliffe O, Maskell N (2014). "Spontaneous pneumothorax". BMJ. 348: g2928. doi:10.1136/bmj.g2928. PMID 24812003.
- ↑ Wakai A (2008). "Spontaneous pneumothorax". BMJ Clin Evid. 2008. PMC 2907964. PMID 19450320.
- ↑ Wakai AP (2011). "Spontaneous pneumothorax". BMJ Clin Evid. 2011. PMC 3275306. PMID 21477390.
- ↑ Andrivet P, Djedaini K, Teboul JL, Brochard L, Dreyfuss D (1995). "Spontaneous pneumothorax. Comparison of thoracic drainage vs immediate or delayed needle aspiration". Chest. 108 (2): 335–9. PMID 7634863.
- ↑ Lippert HL, Lund O, Blegvad S, Larsen HV (1991). "Independent risk factors for cumulative recurrence rate after first spontaneous pneumothorax". Eur Respir J. 4 (3): 324–31. PMID 1864347.
- ↑ Graham RB, Nolasco M, Peterlin B, Garcia CK (2005). "Nonsense mutations in folliculin presenting as isolated familial spontaneous pneumothorax in adults". Am J Respir Crit Care Med. 172 (1): 39–44. doi:10.1164/rccm.200501-143OC. PMID 15805188.
- ↑ Ray A, Gupta M (2017). "Iatrogenic buffalo-chest syndrome". Indian J Radiol Imaging. 27 (2): 254–255. doi:10.4103/0971-3026.209202. PMC 5510326. PMID 28744089.
- ↑ Reading M (2015). "Bilateral pneumothoraces secondary to a Buffalo chest". Aust Crit Care. 28 (1): 10, discussion 54-5. PMID 25879087.
- ↑ Khan, Omar A.; Tsang, Geoffrey M.; Barlow, Clifford W.; Amer, Khalid M. (2006). "Routine Histological Analysis of Resected Lung Tissue in Primary Spontaneous Pneumothorax—Is It Justified?". Heart, Lung and Circulation. 15 (2): 137–138. doi:10.1016/j.hlc.2005.10.007. ISSN 1443-9506.
- ↑ Schneider, Frank; Murali, Rajmohan; Veraldi, Kristen L.; Tazelaar, Henry D.; Leslie, Kevin O. (2014). "Approach to Lung Biopsies From Patients With Pneumothorax". Archives of Pathology & Laboratory Medicine. 138 (2): 257–265. doi:10.5858/arpa.2013-0091-RA. ISSN 0003-9985.
- ↑ Ayed, Adel K.; Chandrasekaran, Chezhian; Sukumar, Murugan (2006). "Video-assisted thoracoscopic surgery for primary spontaneous pneumothorax: clinicopathological correlation". European Journal of Cardio-Thoracic Surgery. 29 (2): 221–225. doi:10.1016/j.ejcts.2005.11.005. ISSN 1010-7940.