Panitumumab
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Alberto Plate [2]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Black Box Warning
|
Warning: Dermatological Toxicity
See full prescribing information for complete Boxed Warning.
Dermatologic Toxicity:
|
Overview
Panitumumab is an Immunological Agent and Monoclonal Antibody that is FDA approved for the treatment of metastatic colorectal cancer with wild-type KRAS (exon 2 in codons 12 or 13) as first-line therapy in combination with FOLFOX, monotherapy following disease progression after prior treatment with fluoropyrimidine, oxaliplatin, and irinotecan-containing chemotherapy. There is a Black Box Warning for this drug as shown here. Common adverse reactions include rash with variable presentations, paronychia, fatigue, nausea, and diarrhea, stomatitis, mucosal inflammation, asthenia, paronychia, anorexia, hypomagnesemia, hypokalemia, acneiform dermatitis, pruritus, and dry skin.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Patient Selection
- Prior to initiation of treatment with Panitumumab, assess KRAS mutational status in colorectal tumors and confirm the absence of a KRAS mutation using an FDA-approved test. Information on FDA-approved tests for the detection of KRAS mutations in patients with metastatic colorectal cancer is available at: http://www.fda.gov/CompanionDiagnostics.
Recommended Dose
- The recommended dose of Panitumumab is 6 mg/kg, administered as an intravenous infusion over 60 minutes, every 14 days. If the first infusion is tolerated, administer subsequent infusions over 30 to 60 minutes. Administer doses higher than 1000 mg over 90 minutes [see Dosage and Administration (2.4)].
- Appropriate medical resources for the treatment of severe infusion reactions should be available during Panitumumab infusions.
Dose Modifications
- Reduce infusion rate by 50% in patients experiencing a mild or moderate (grade 1 or 2) infusion reaction for the duration of that infusion.
- Terminate the infusion in patients experiencing severe infusion reactions. Depending on the severity and/or persistence of the reaction, permanently discontinue Panitumumab.
Dose Modifications for Dermatologic Toxicity
- Upon first occurrence of a grade 3 (NCI-CTC/CTCAE) dermatologic reaction, withhold 1 to 2 doses of Panitumumab. If the reaction improves to < grade 3, reinitiate Panitumumab at the original dose.
- Upon the second occurrence of a grade 3 (NCI-CTC/CTCAE) dermatologic reaction, withhold 1 to 2 doses of Panitumumab. If the reaction improves to < grade 3, reinitiate Panitumumab at 80% of the original dose.
- Upon the third occurrence of a grade 3 (NCI-CTC/CTCAE) dermatologic reaction, withhold 1 to 2 doses of Panitumumab. If the reaction improves to < grade 3, reinitiate Panitumumab at 60% of the original dose.
- Upon the fourth occurrence of a grade 3 (NCI-CTC/CTCAE) dermatologic reaction, permanently discontinue Panitumumab.
- Permanently discontinue Panitumumab following the occurrence of a grade 4 dermatologic reaction or for a grade 3 (NCI-CTC/CTCAE) dermatologic reaction that does not recover after withholding 1 or 2 doses.
Preparation and Administration
- Do not administer Panitumumab as an intravenous push or bolus.
Preparation
Prepare the solution for infusion, using aseptic technique, as follows:
- Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration. *Although Panitumumab should be colorless, the solution may contain a small amount of visible translucent-to-white, amorphous, proteinaceous, panitumumab particulates (which will be removed by filtration; see below).
- Do not shake.
- Do not administer Panitumumab if discoloration is observed.
- Withdraw the necessary amount of Panitumumab for a dose of 6 mg/kg.
- Dilute to a total volume of 100 mL with 0.9% sodium chloride injection, USP. Doses higher than 1000 mg should be diluted to 150 mL with 0.9% sodium chloride injection, USP. Do not exceed a final concentration of 10 mg/mL.
- Mix diluted solution by gentle inversion. Do not shake.
Administration
- Administer using a low-protein-binding 0.2 μm or 0.22 μm in-line filter.
- Panitumumab must be administered via infusion pump.
- Flush line before and after Panitumumab administration with 0.9% sodium chloride injection, USP, to avoid mixing with other drug products or intravenous solutions. Do not mix Panitumumab with, or administer as an infusion with, other medicinal products. Do not add other medications to solutions containing panitumumab.
- Infuse doses of 1000 mg or lower over 60 minutes through a peripheral intravenous line or indwelling intravenous catheter. If the first infusion is tolerated, administer subsequent infusions over 30 to 60 minutes. Administer doses higher than 1000 mg over 90 minutes.
- Use the diluted infusion solution of Panitumumab within 6 hours of preparation if stored at room temperature, or within 24 hours of dilution if stored at 2° to 8°C (36º to 46ºF). DO NOT FREEZE.
- Discard any unused portion remaining in the vial.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Panitumumab in adult patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Panitumumab in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
There is limited information regarding Panitumumab FDA-Labeled Indications and Dosage (Pediatric) in the drug label.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Panitumumab in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Panitumumab in pediatric patients.
Contraindications
- None.
Warnings
|
Warning: Dermatological Toxicity
See full prescribing information for complete Boxed Warning.
Dermatologic Toxicity:
|
Dermatologic and Soft Tissue Toxicity
- In Study 1, dermatologic toxicities occurred in 90% of patients and were severe (NCI-CTC grade 3 and higher) in 15% of patients with mCRC receiving Panitumumab The clinical manifestations included, but were not limited to, acneiform dermatitis, pruritus, erythema, rash, skin exfoliation, paronychia, dry skin, and skin fissures.
- Monitor patients who develop dermatologic or soft tissue toxicities while receiving Panitumumab for the development of inflammatory or infectious sequelae. Life-threatening and fatal infectious complications including necrotizing fasciitis, abscesses, and sepsis have been observed in patients treated with Panitumumab. Life-threatening and fatal bullous mucocutaneous disease with blisters, erosions, and skin sloughing has also been observed in patients treated with Panitumumab It could not be determined whether these mucocutaneous adverse reactions were directly related to EGFR inhibition or to idiosyncratic immune-related effects (eg, Stevens-Johnson syndrome or toxic epidermal necrolysis). Withhold or discontinue Panitumumab for dermatologic or soft tissue toxicity associated with severe or life-threatening inflammatory or infectious complications. Dose modifications for Panitumumab concerning dermatologic toxicity are provided.
Increased Tumor Progression, Increased Mortality, or Lack of Benefit in Patients with RAS- and KRAS-Mutant mCRC
- A predefined retrospective subset analysis of Study 3 further identified a shortening of progression-free survival (PFS) and overall survival (OS) in patients with RAS-mutant tumors who received Panitumumab and FOLFOX versus FOLFOX alone. Determination of RAS-mutant tumor status should be performed by an experienced laboratory.
- Determination of KRAS mutational status in colorectal tumors using an FDA-approved test indicated for this use is necessary for selection of patients for treatment with Panitumumab. Panitumumab is indicated only for the treatment of patients with KRAS wild-type mCRC. Panitumumab is not indicated for the treatment of patients with colorectal cancer that harbor somatic mutations in codons 12 and 13 (exon 2) as determined by an FDA-approved test for this use. In Study 3, 221 patients with KRAS-mutant mCRC tumors receiving Panitumumab in combination with FOLFOX experienced shorter OS compared to 219 patients receiving FOLFOX alone (HR = 1.16, 95% CI: 0.94-1.41). Perform the assessment for KRAS mutational status in colorectal cancer in laboratories with demonstrated proficiency in the specific technology being utilized. Improper assay performance can lead to unreliable test results. Refer to an FDA-approved test’s package insert for instructions on the identification of patients eligible for the treatment of Panitumumab.
Electrolyte Depletion/Monitoring
- Progressively decreasing serum magnesium levels leading to severe (grade 3-4) hypomagnesemia occurred in up to 7% (in Study 2) of patients across clinical trials. Monitor patients for hypomagnesemia and hypocalcemia prior to initiating Panitumumab treatment, periodically during Panitumumab treatment, and for up to 8 weeks after the completion of treatment. Other electrolyte disturbances, including hypokalemia, have also been observed. Replete magnesium and other electrolytes as appropriate.
Infusion Reactions
In Study 1, 4% of patients experienced infusion reactions and 1% of patients experienced severe infusion reactions (NCI-CTC grade 3-4).
- Infusion reactions, manifesting as fever, chills, dyspnea, bronchospasm, and hypotension, can occur following Panitumumab administration. Fatal infusion reactions occurred in postmarketing experience. Terminate the infusion for severe infusion reactions.
Acute Renal Failure in Combination with Chemotherapy
- Severe diarrhea and dehydration, leading to acute renal failure and other complications, have been observed in patients treated with Panitumumab in combination with chemotherapy.
Pulmonary Fibrosis/Interstitial Lung Disease (ILD)
- Fatal and nonfatal cases of interstitial lung disease (ILD) (1%) and pulmonary fibrosis have been observed in patients treated with Panitumumab. Pulmonary fibrosis occurred in less than 1% (2/1467) of patients enrolled in clinical studies of Panitumumab In the event of acute onset or worsening of pulmonary symptoms, interrupt Panitumumab therapy. Discontinue Panitumumab therapy if ILD is confirmed.
- In patients with a history of interstitial pneumonitis or pulmonary fibrosis, or evidence of interstitial pneumonitis or pulmonary fibrosis, the benefits of therapy with Panitumumab versus the risk of pulmonary complications must be carefully considered.
Photosensitivity
- Exposure to sunlight can exacerbate dermatologic toxicity. Advise patients to wear sunscreen and hats and limit sun exposure while receiving Panitumumab.
Ocular Toxicities
- Keratitis and ulcerative keratitis, known risk factors for corneal perforation, have been reported with Panitumumab use. Monitor for evidence of keratitis or ulcerative keratitis. Interrupt or discontinue Panitumumab therapy for acute or worsening keratitis.
Increased Mortality and Toxicity with Panitumumab in Combination with Bevacizumab and Chemotherapy
- In an interim analysis of an open-label, multicenter, randomized clinical trial in the first-line setting in patients with mCRC, the addition of Panitumumab to the combination of bevacizumab and chemotherapy resulted in decreased OS and increased incidence of NCI-CTC grade 3-5 (87% vs 72%) adverse reactions. NCI-CTC grade 3-4 adverse reactions occurring at a higher rate in Panitumumab-treated patients included rash/acneiform dermatitis (26% vs 1%), diarrhea (23% vs 12%), dehydration (16% vs 5%), primarily occurring in patients with diarrhea, hypokalemia (10% vs 4%), stomatitis/mucositis (4% vs < 1%), and hypomagnesemia (4% vs 0).
- NCI-CTC grade 3-5 pulmonary embolism occurred at a higher rate in Panitumumab-treated patients (7% vs 3%) and included fatal events in three (< 1%) Panitumumab-treated patients.
- As a result of the toxicities experienced, patients randomized to Panitumumab, bevacizumab, and chemotherapy received a lower mean relative dose intensity of each chemotherapeutic agent (oxaliplatin, irinotecan, bolus 5-FU, and/or infusional 5-FU) over the first 24 weeks on study compared with those randomized to bevacizumab and chemotherapy.
Adverse Reactions
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates in the clinical trials of a drug cannot be directly compared to rates in clinical trials of another drug and may not reflect the rates observed in practice. The adverse reaction information from clinical studies does, however, provide a basis for identifying the adverse events that appear to be related to drug use and for approximating rates.
- Safety data are presented from two clinical trials in which patients received Panitumumab: Study 1, an open-label, multinational, randomized, controlled, monotherapy clinical trial (N = 463) evaluating Panitumumab with best supportive care (BSC) versus BSC alone in patients with EGFR-expressing mCRC and Study 3, a randomized, controlled trial (N = 1183) in patients with mCRC that evaluated Panitumumab in combination with FOLFOX chemotherapy versus FOLFOX chemotherapy alone. Safety data for Study 3 are limited to 656 patients with wild-type KRAS mCRC.
Panitumumab Monotherapy
- In Study 1, the most common adverse reactions (≥ 20%) with Panitumumab were skin rash with variable presentations, paronychia, fatigue, nausea, and diarrhea.
- The most common (> 5%) serious adverse reactions in the Panitumumab arm were general physical health deterioration and intestinal obstruction. The most frequently reported adverse reactions for Panitumumab leading to withdrawal were general physical health deterioration (n = 2) and intestinal obstruction (n = 2).
For Study 1, the data described in Table 1 and in other sections below, except where noted, reflect exposure to Panitumumab administered to patients with mCRC as a single agent at the recommended dose and schedule (6 mg/kg every 2 weeks).
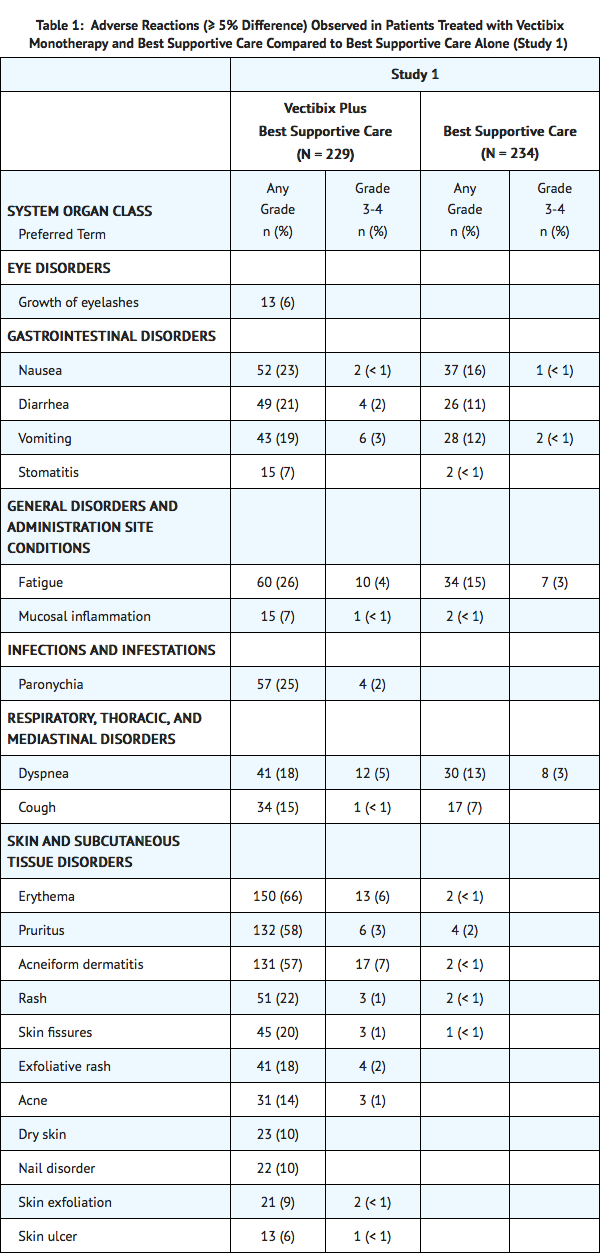
- Adverse reactions in Study 1 that did not meet the threshold criteria for inclusion in Table 1 were conjunctivitis (4.8% vs < 1%), dry mouth (4.8% vs 0%), pyrexia (16.6% vs 13.2%), chills (3.1% vs < 1%), pustular rash (4.4% vs 0%), papular rash (1.7% vs 0%), dehydration (2.6% vs 1.7%), epistaxis (3.9% vs 0%), and pulmonary embolism (1.3% vs 0%).
- In Study 1, dermatologic toxicities occurred in 90% of patients receiving Panitumumab. Skin toxicity was severe (NCI-CTC grade 3 and higher) in 15% of patients. Ocular toxicities occurred in 16% of patients and included, but were not limited to, conjunctivitis (5%). One patient experienced an NCI-CTC grade 3 event of mucosal inflammation. The incidence of paronychia was 25% and was severe in 2% of patients.
- In Study 1 (N = 229), median time to the development of dermatologic, nail, or ocular toxicity was 12 days after the first dose of Panitumumab the median time to most severe skin/ocular toxicity was 15 days after the first dose of Panitumumab and the median time to resolution after the last dose of Panitumumab was 98 days. Severe toxicity necessitated dose interruption in 11% of Panitumumab-treated patients.
- Subsequent to the development of severe dermatologic toxicities, infectious complications, including sepsis, septic death, necrotizing fasciitis, and abscesses requiring incisions and drainage were reported.
Panitumumab in Combination with FOLFOX Chemotherapy
- The most commonly reported adverse reactions (≥ 20%) in patients with wild-type KRAS mCRC receiving Panitumumab (6 mg/kg every 2 weeks) and FOLFOX therapy (N = 322) in Study 3 were diarrhea, stomatitis, mucosal inflammation, asthenia, paronychia, anorexia, hypomagnesemia, hypokalemia, rash, acneiform dermatitis, pruritus, and dry skin (Table 2). Serious adverse reactions (≥ 2% difference between treatment arms) in Panitumumab-treated patients with wild-type KRAS mCRC were diarrhea and dehydration. The commonly reported adverse reactions (≥ 1%) leading to discontinuation in patients with wild-type KRAS mCRC receiving Panitumumab were rash, paresthesia, fatigue, diarrhea, acneiform dermatitis, and hypersensitivity. One grade 5 adverse reaction, hypokalemia, occurred in a patient who received Panitumumab.
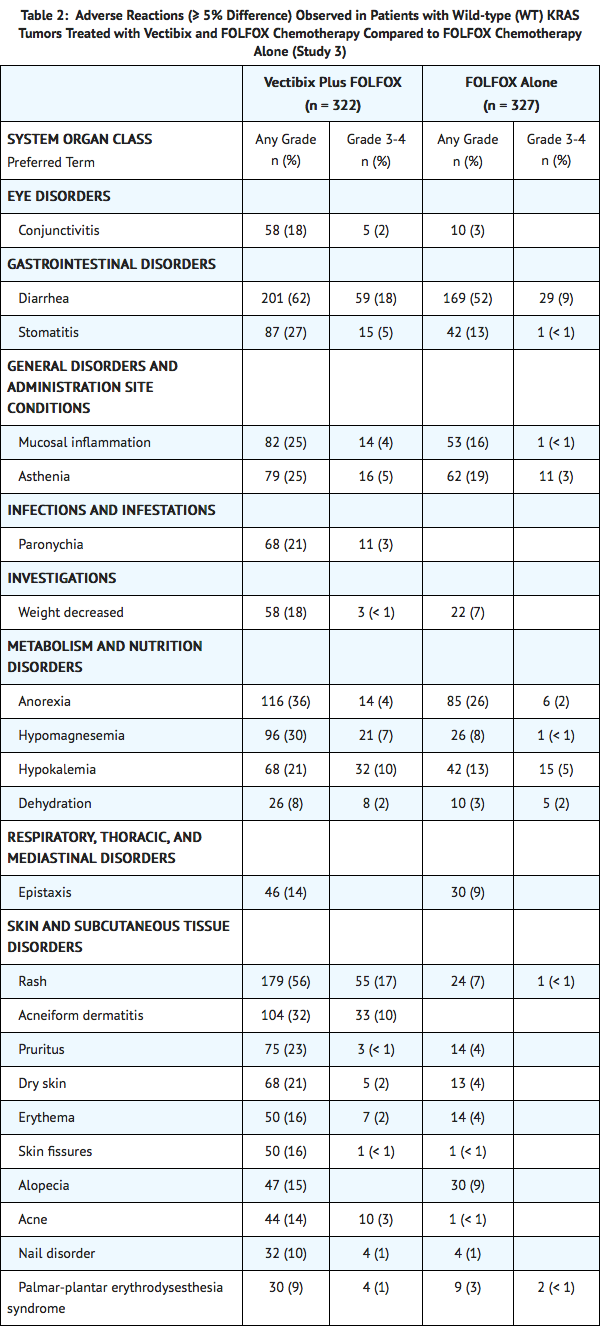
- Adverse reactions that did not meet the threshold criteria for inclusion in Table 2 were abdominal pain (28% vs 23%), localized infection (3.7% vs < 1%), cellulitis (2.5% vs 0%), hypocalcemia (5.6% vs 2.1%), and deep vein thrombosis (5.3% vs 3.1%).
Infusion Reactions
- Infusional toxicity manifesting as fever, chills, dyspnea, bronchospasm or hypotension was assessed within 24 hours of an infusion during the clinical study. Vital signs and temperature were measured within 30 minutes prior to initiation and upon completion of the Panitumumab infusion. The use of premedication was not standardized in the clinical trials. Thus, the utility of premedication in preventing the first or subsequent episodes of infusional toxicity is unknown. Across clinical trials of Panitumumab monotherapy, 3% (24/725) experienced infusion reactions of which < 1% (3/725) were severe (NCI-CTC grade 3-4). In one patient, Panitumumab was permanently discontinued for a serious infusion reaction.
Immunogenicity
- As with all therapeutic proteins, there is potential for immunogenicity. The immunogenicity of Panitumumab has been evaluated using two different screening immunoassays for the detection of binding anti-panitumumab antibodies: an acid dissociation bridging enzyme-linked immunosorbent assay (ELISA) detecting high-affinity antibodies and a Biacore® biosensor immunoassay detecting both high- and low-affinity antibodies. For patients whose sera tested positive in screening immunoassays, an in vitro biological assay was performed to detect neutralizing antibodies.
- Monotherapy: The incidence of binding anti-panitumumab antibodies (excluding preexisting and transient positive patients) was 0.4% (5/1123) as detected by the acid dissociation ELISA and 3.2% (36/1123) as detected by the Biacore® assay. The incidence of neutralizing anti-panitumumab antibodies (excluding preexisting and transient positive patients) was 0.8% (9/1123). There was no evidence of altered pharmacokinetic or safety profiles in patients who developed antibodies to Panitumumab.
- In combination with chemotherapy: The incidence of binding anti-panitumumab antibodies (excluding preexisting positive patients) was 0.9% (12/1297) as detected by the acid dissociation ELISA and 0.7% (9/1296) as detected by the Biacore® assay. The incidence of neutralizing anti-panitumumab antibodies (excluding preexisting positive patients) was 0.2% (2/1297). No evidence of an altered safety profile was found in patients who developed antibodies to Panitumumab.
- The detection of antibody formation is highly dependent on the sensitivity and specificity of the assay. Additionally, the observed incidence of antibody (including neutralizing antibody) positivity in an assay may be influenced by several factors, including assay methodology, sample handling, timing of sample collection, concomitant medications, and underlying disease. For these reasons, comparison of the incidence of antibodies to panitumumab with the incidence of antibodies to other products may be misleading.
Postmarketing Experience
The following adverse reactions have been identified during post-approval use of Panitumumab Because these reactions are reported in a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Skin and subcutaneous tissue disorders: Skin necrosis, angioedema, life-threatening and fatal bullous mucocutaneous disease.
- Immune system disorders: Infusion reaction.
- Eye disorders: Keratitis/ulcerative keratitis.
Drug Interactions
- No formal drug-drug interaction studies have been conducted between Panitumumab and oxaliplatin or fluoropyrimidine.
Use in Specific Populations
Pregnancy
- There are no studies of Panitumumab in pregnant women. Reproduction studies in cynomolgus monkeys treated with 1.25 to 5 times the recommended human dose of panitumumab resulted in significant embryolethality and abortions; however, no other evidence of teratogenesis was noted in offspring. Panitumumab should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
- Based on animal models, EGFR is involved in prenatal development and may be essential for normal organogenesis, proliferation, and differentiation in the developing embryo. Human IgG is known to cross the placental barrier; therefore, panitumumab may be transmitted from the mother to the developing fetus, and has the potential to cause fetal harm when administered to pregnant women.
- Women who become pregnant during Panitumumab treatment are encouraged to enroll in Amgen’s Pregnancy Surveillance Program. Patients or their physicians should call 1-800-77-AMGEN (1-800-772-6436) to enroll.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Panitumumab in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Panitumumab during labor and delivery.
Nursing Mothers
- It is not known whether panitumumab is excreted into human milk; however, human IgG is excreted into human milk. Published data suggest that breast milk antibodies do not enter the neonatal and infant circulation in substantial amounts. Because many drugs are excreted into human milk and because of the potential for serious adverse reactions in nursing infants from Panitumumab a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother. If nursing is interrupted, based on the mean half-life of panitumumab, nursing should not be resumed earlier than 2 months following the last dose of Panitumumab.
- Women who are nursing during Panitumumab treatment are encouraged to enroll in Amgen’s Lactation Surveillance Program. Patients or their physicians should call 1-800-77-AMGEN (1-800-772-6436) to enroll.
Pediatric Use
- The safety and effectiveness of Panitumumab have not been established in pediatric patients. The pharmacokinetic profile of Panitumumab has not been studied in pediatric patients.
Geriatic Use
- Of the 737 patients who received Panitumumab monotherapy in Study 1 and 2, 36% were 65 and over while 8% were 75 and over. No overall differences in safety or efficacy were observed in elderly patients (≥ 65 years of age) treated with Panitumumab monotherapy.
- Of the 322 patients in Study 3 who received Panitumumab plus FOLFOX, 128 (40%) were 65 and over while 8% were 75 and over. Patients older than 65 years of age experienced an increased incidence of serious adverse events (52% vs 36%) and an increased incidence of serious diarrhea (15% vs 5%) as compared to younger patients.
Gender
There is no FDA guidance on the use of Panitumumab with respect to specific gender populations.
Race
There is no FDA guidance on the use of Panitumumab with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Panitumumab in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Panitumumab in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Panitumumab in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Panitumumab in patients who are immunocompromised.
Administration and Monitoring
Administration
There is limited information regarding Panitumumab Administration in the drug label.
Monitoring
There is limited information regarding Panitumumab Monitoring in the drug label.
IV Compatibility
There is limited information regarding the compatibility of Panitumumab and IV administrations.
Overdosage
- Doses up to approximately twice the recommended therapeutic dose (12 mg/kg) resulted in adverse reactions of skin toxicity, diarrhea, dehydration, and fatigue.
Pharmacology
Panitumumab?
| |
| Therapeutic monoclonal antibody | |
| Source | u |
| Target | EGFR |
| Identifiers | |
| CAS number | |
| ATC code | L01 |
| PubChem | ? |
| DrugBank | |
| Chemical data | |
| Formula | Template:OrganicBox atomTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox |
| Mol. mass | ? |
| Pharmacokinetic data | |
| Bioavailability | ? |
| Metabolism | ? |
| Half life | ∼9.4 days (range: 4-11 days) |
| Excretion | ? |
| Therapeutic considerations | |
| Pregnancy cat. |
? |
| Legal status |
Template:Unicode Prescription only |
| Routes | intravenous |
Mechanism of Action
- The EGFR is a transmembrane glycoprotein that is a member of a subfamily of type I receptor tyrosine kinases, including EGFR, HER2, HER3, and HER4. EGFR is constitutively expressed in normal epithelial tissues, including the skin and hair follicle. EGFR is overexpressed in certain human cancers, including colon and rectum cancers. Interaction of EGFR with its normal ligands (eg, EGF, transforming growth factor-alpha) leads to phosphorylation and activation of a series of intracellular proteins, which in turn regulate transcription of genes involved with cellular growth and survival, motility, and proliferation. Signal transduction through the EGFR results in activation of the wild-type KRAS protein. However, in cells with activating KRAS somatic mutations, the KRAS-mutant protein is continuously active and appears independent of EGFR regulation.
- Panitumumab binds specifically to EGFR on both normal and tumor cells, and competitively inhibits the binding of ligands for EGFR. Nonclinical studies show that binding of panitumumab to the EGFR prevents ligand-induced receptor autophosphorylation and activation of receptor-associated kinases, resulting in inhibition of cell growth, induction of apoptosis, decreased proinflammatory cytokine and vascular growth factor production, and internalization of the EGFR. In vitro assays and in vivo animal studies demonstrate that panitumumab inhibits the growth and survival of selected human tumor cell lines expressing EGFR.
Structure
There is limited information regarding Panitumumab Structure in the drug label.
Pharmacodynamics
There is limited information regarding Panitumumab Pharmacodynamics in the drug label.
Pharmacokinetics
- Panitumumab administered as a single agent exhibits nonlinear pharmacokinetics.
- Following single-dose administrations of panitumumab as 1-hour infusions, the area under the concentration-time curve (AUC) increased in a greater than dose-proportional manner, and clearance (CL) of panitumumab decreased from 30.6 to 4.6 mL/day/kg as the dose increased from 0.75 to 9 mg/kg. However, at doses above 2 mg/kg, the AUC of panitumumab increased in an approximately dose-proportional manner.
- Following the recommended dose regimen (6 mg/kg given once every 2 weeks as a 1-hour infusion), panitumumab concentrations reached steady-state levels by the third infusion with mean (± SD) peak and trough concentrations of 213 ± 59 and 39 ± 14 mcg/mL, respectively. The mean (± SD) AUC0-tau and CL were 1306 ± 374 mcg•day/mL and 4.9 ± 1.4 mL/kg/day, respectively. The elimination half-life was approximately 7.5 days (range: 3.6 to 10.9 days).
- A population pharmacokinetic analysis was performed to explore the potential effects of selected covariates on panitumumab pharmacokinetics. Results suggest that age (21-88 years), gender, race (15% nonwhite), mild-to-moderate renal dysfunction, mild-to-moderate hepatic dysfunction, and EGFR membrane-staining intensity (1+, 2+, and 3+) in tumor cells had no apparent impact on the pharmacokinetics of panitumumab.
- No formal pharmacokinetic studies of panitumumab have been conducted in patients with renal impairment or hepatic impairment.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
- No carcinogenicity or mutagenicity studies of panitumumab have been conducted. It is not known if panitumumab can impair fertility in humans. Prolonged menstrual cycles and/or amenorrhea occurred in normally cycling, female cynomolgus monkeys treated weekly with 1.25 to 5 times the recommended human dose of panitumumab (based on body weight). Menstrual cycle irregularities in panitumumab-treated female monkeys were accompanied by both a decrease and delay in peak progesterone and 17β-estradiol levels. Normal menstrual cycling resumed in most animals after discontinuation of panitumumab treatment. A no-effect level for menstrual cycle irregularities and serum hormone levels was not identified. The effects of panitumumab on male fertility have not been studied. However, no adverse effects were observed microscopically in reproductive organs from male cynomolgus monkeys treated for 26 weeks with panitumumab at doses of up to approximately 5-fold the recommended human dose (based on body weight).
Animal Toxicology and/or Pharmacology
- Weekly administration of panitumumab to cynomolgus monkeys for 4 to 26 weeks resulted in dermatologic findings, including dermatitis, pustule formation and exfoliative rash, and deaths secondary to bacterial infection and sepsis at doses of 1.25 to 5-fold higher (based on body weight) than the recommended human dose.
Reproductive and Developmental Toxicology
- Pregnant cynomolgus monkeys were treated weekly with panitumumab during the period of organogenesis (gestation day [GD] 20-50). While no panitumumab was detected in serum of neonates from panitumumab-treated dams, anti-panitumumab antibody titers were present in 14 of 27 offspring delivered at GD 100. There were no fetal malformations or other evidence of teratogenesis noted in the offspring. However, significant increases in embryolethality and abortions occurred at doses of approximately 1.25 to 5 times the recommended human dose (based on body weight).
Clinical Studies
Recurrent or Refractory mCRC
- The safety and efficacy of Panitumumab was demonstrated in Study 1, an open-label, multinational, randomized, controlled trial of 463 patients with EGFR-expressing, metastatic carcinoma of the colon or rectum, and in Study 2, an open-label, multicenter, multinational, randomized trial of 1010 patients with wild-type KRAS mCRC.
Study 1
- Patients in Study 1 were required to have progressed on or following treatment with a regimen(s) containing a fluoropyrimidine, oxaliplatin, and irinotecan; progression was confirmed by an independent review committee (IRC) masked to treatment assignment for 76% of the patients. Patients were randomized (1:1) to receive panitumumab at a dose of 6 mg/kg given once every 2 weeks plus BSC (N = 231) or BSC alone (N = 232) until investigator-determined disease progression. Randomization was stratified based on Eastern Cooperative Oncology Group (ECOG) performance status (PS) (0 and 1 vs 2) and geographic region (Western Europe, Eastern/Central Europe, or other). Upon investigator-determined disease progression, patients in the BSC-alone arm were eligible to receive panitumumab and were followed until disease progression was confirmed by the IRC.
- Based upon IRC determination of disease progression, a statistically significant prolongation in PFS was observed in patients receiving panitumumab compared to those receiving BSC alone. The mean PFS was 96 days in the panitumumab arm and 60 days in the BSC-alone arm.
- The study results were analyzed in the wild-type KRAS subgroup where KRAS status was retrospectively determined using archived paraffin-embedded tumor tissue. KRAS mutation status was determined in 427 patients (92%); of these, 243 (57%) had no detectable KRAS mutations in either codons 12 or 13. The hazard ratio for PFS in patients with wild-type KRAS mCRC was 0.45 (95% CI: 0.34-0.59) favoring the panitumumab arm. The response rate was 17% for the panitumumab arm and 0% for BSC. There were no differences in OS; 77% of patients in the BSC arm received panitumumab at the time of disease progression.
Study 2
- Study 2 was an open-label, multicenter, multinational, randomized (1:1) clinical trial, stratified by region (North America, Western Europe, and Australia versus rest of the world) and ECOG PS (0 and 1 vs 2) in patients with wild-type KRAS mCRC. A total of 1010 patients who received prior treatment with irinotecan, oxaliplatin, and a thymidylate synthase inhibitor were randomized to receive Panitumumab 6 mg/kg intravenously over 60 minutes every 14 days or cetuximab 400 mg/m2 intravenously over 120 minutes on day 1 followed by 250 mg/m2 intravenously over 60 minutes every 7 days. The trial excluded patients with clinically significant cardiac disease and interstitial lung disease. The major efficacy analysis tested whether the OS of Panitumumab was noninferior to cetuximab. Data for investigator-assessed PFS and objective response rate (ORR) were also collected. The criteria for noninferiority was for Panitumumab to retain at least 50% of the OS benefit of cetuximab based on an OS hazard ratio of 0.55 from the NCIC CTG CO.17 study relative to BSC.
- In Study 2, 37% of patients were women, 52% were white, 45% were Asian, and 1.3% were Hispanic or Latino. Thirty-one percent of patients were enrolled at sites in North America, Western Europe, or Australia. ECOG performance was 0 in 32% of patients, 1 in 60% of patients, and 2 in 8% of patients. Median age was 61 years. More patients (62%) had colon cancer than rectal cancer (38%). Most patients (74%) had not received prior bevacizumab.
- The key efficacy analysis for Study 2 demonstrated that Panitumumab was statistically significantly noninferior to cetuximab for OS.
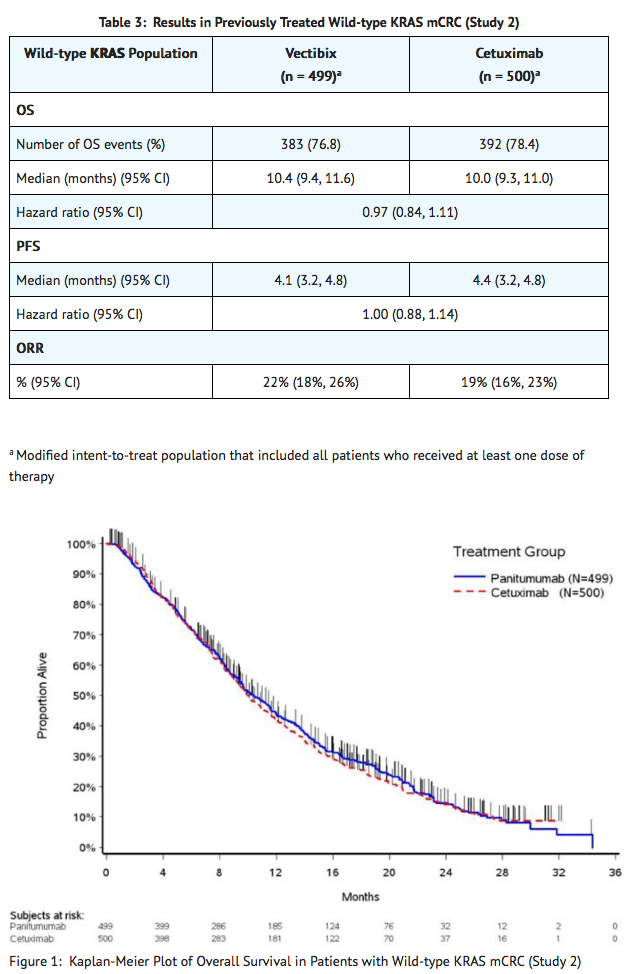
First-line in Combination with FOLFOX Chemotherapy
Study 3
- Study 3 was a multicenter, open-label trial that randomized (1:1) patients with mCRC who were previously untreated in the metastatic setting and who had received no prior oxaliplatin to receive Panitumumab every 14 days in combination with FOLFOX or to FOLFOX alone every 14 days. Panitumumab was administered at 6 mg/kg over 60 minutes prior to administration of chemotherapy. The FOLFOX regimen consisted of oxaliplatin 85 mg per m2 IV infusion over 120 minutes and leucovorin (dl-racemic) 200 mg per m2 intravenous infusion over 120 minutes at the same time on day 1 using a Y-line, followed on day 1 by 5-FU 400 mg per m2 intravenous bolus. The 5FU bolus was followed by a continuous infusion of 5-FU 600 mg per m2 over 22 hours. On day 2, patients received leucovorin 200 mg per m2 followed by the bolus dose (400 mg per m2) and continuous infusion of 5FU (600 mg per m2) over 22 hours. Study 3 excluded patients with known central nervous system metastases, clinically significant cardiac disease, interstitial lung disease, or active inflammatory bowel disease. The prespecified major efficacy measure was PFS in patients (n = 656) with wild-type KRAS mCRC as assessed by a blinded independent central review of imaging. Other key efficacy measures included OS and ORR.
- In Study 3, in the wild-type KRAS group, 64% of patients were men, 92% white, 2% black, and 4% Hispanic or Latino. Sixty-six percent of patients had colon cancer and 34% had rectal cancer. ECOG performance was 0 in 56% of patients, 1 in 38% of patients, and 2 in 6% of patients. Median age was 61.5 years.
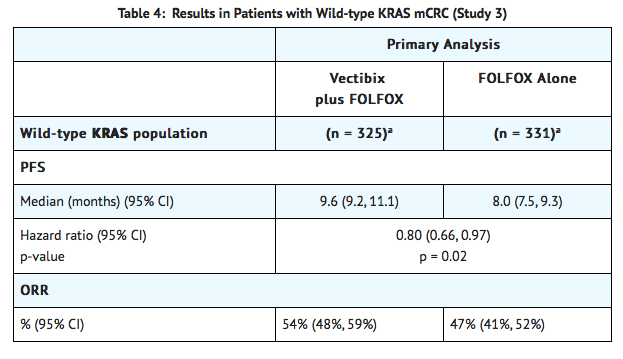
KRAS-Mutant Subgroup
- In Study 3, among patients with KRAS-mutant tumors, median PFS was 7.3 months (95% CI: 6.3, 8.0) among 221 patients receiving Panitumumab plus FOLFOX versus 8.8 months (95% CI: 7.7, 9.4) among patients who received FOLFOX alone (HR = 1.29, 95% CI: 1.04, 1.62). Median OS was 15.5 months (95% CI: 13.1, 17.6) among patients receiving Panitumumab plus FOLFOX versus 19.3 months (95% CI: 16.5, 21.8) among patients who received FOLFOX alone (HR = 1.24, 95% CI: 0.98, 1.57).
Exploratory Analysis of OS
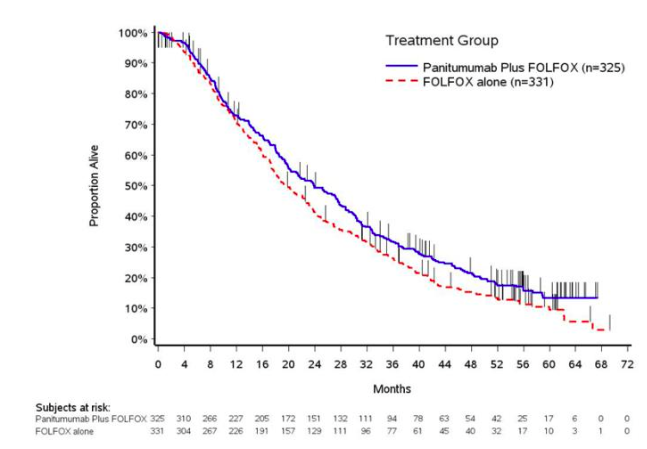
- An exploratory analysis of OS with updated information based on events in 82% of patients with wild-type KRAS mCRC estimated the treatment effect of Panitumumab plus FOLFOX compared with FOLFOX alone on OS (Figure 2). Median OS among 325 patients with wild-type KRAS mCRC who received Panitumumab plus FOLFOX was 23.8 months (95% CI: 20.0, 27.7) versus 19.4 months (95% CI: 17.4, 22.6) among 331 patients who received FOLFOX alone (HR = 0.83, 95% CI: 0.70, 0.98).
How Supplied
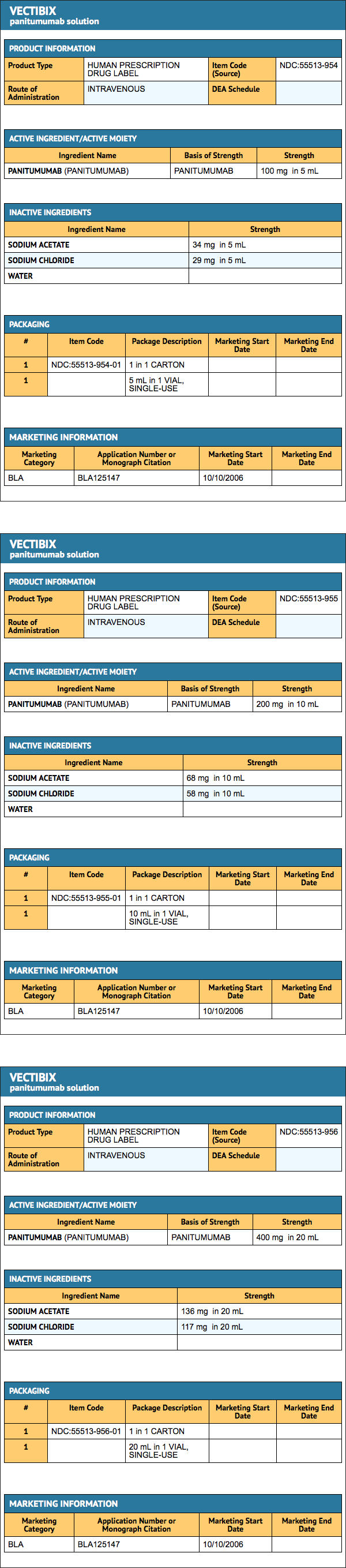
- Panitumumab is supplied as a sterile, colorless, preservative-free solution containing 20 mg/mL Panitumumab (panitumumab) in a single-use vial.
- Panitumumab is provided as one vial per carton:
- Each 5 mL single-use vial contains 100 mg of panitumumab in 5 mL (20 mg/mL) (NDC 55513-954-01).
- Each 10 mL single-use vial contains 200 mg of panitumumab in 10 mL (20 mg/mL) (NDC 55513-955-01).
- Each 20 mL single-use vial contains 400 mg of panitumumab in 20 mL (20 mg/mL) (NDC 55513-956-01).
Storage
Store vials in the original carton under refrigeration at 2º to 8ºC (36º to 46ºF) until time of use. Protect from direct sunlight. DO NOT FREEZE. Since Panitumumab does not contain preservatives, any unused portion remaining in the vial must be discarded.
The diluted infusion solution of Panitumumab should be used within 6 hours of preparation if stored at room temperature, or within 24 hours of dilution if stored at 2° to 8°C (36º to 46ºF). DO NOT FREEZE.
Images
Drug Images
{{#ask: Page Name::Panitumumab |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Panitumumab |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
There is limited information regarding Panitumumab Patient Counseling Information in the drug label.
Precautions with Alcohol
- Alcohol-Panitumumab interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
Look-Alike Drug Names
There is limited information regarding Panitumumab Look-Alike Drug Names in the drug label.
Price
References
The contents of this FDA label are provided by the National Library of Medicine.