Herpes simplex anogenital infection
| Anogenital herpesviral infection | |
 | |
|---|---|
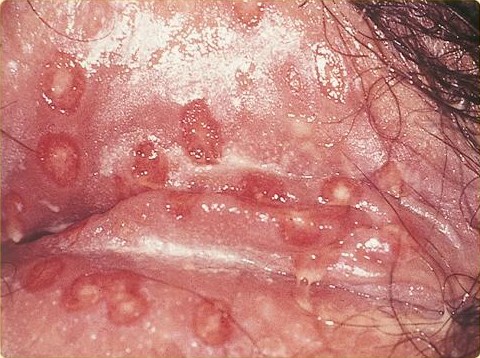
| Genital herpes in a female |
|
Herpes simplex Microchapters |
|
Patient Information |
|
Classification |
|
Herpes simplex anogenital infection On the Web |
|
Risk calculators and risk factors for Herpes simplex anogenital infection |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-In-Chief: Cafer Zorkun, M.D., Ph.D. [2]; Lakshmi Gopalakrishnan, M.B.B.S.
Overview
HSV-2 is widespread, affecting an estimated 1 in 4 females and 1 in 5 males in the United States. Most young, sexually active patients who have genital, anal, or perianal ulcers have either genital herpes or syphilis. The frequency of each condition differs by geographic area and population; however, genital herpes is the most prevalent of these diseases.
Initial Presentation
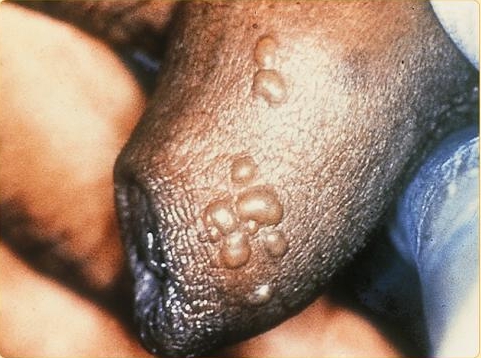
- Clusters of inflammed papules and vesicles on the outer surface of the genitals represent the typical symptoms of a primary HSV-1 or HSV-2 genital infection.
- These usually appear 4–7 days after sexual exposure to HSV for the first time,[1] and may resemble cold sores.[2]
- In males, the lesions occur on the shaft of the penis or other parts of the genital region, on the inner thigh, buttocks, or anus.
- In females, lesions appear on or near the pubis, labia, clitoris, vulva, buttocks or anus.[2]
- Other common symptoms include pain, itching, and burning.
- Less frequent, yet still common, symptoms include discharge from the penis or vagina, fever, headache, muscle pain (myalgia), swollen and enlarged lymph nodes and malaise.[1]
- Women often experience additional symptoms that include painful urination (dysuria) and cervicitis, while herpetic proctitis (inflammation of the anus and rectum) is common for individuals participating in anal intercourse.[1]
Disease Progression
After 2–3 weeks, existing lesions progress into ulcers and then crust and heal, although lesions on mucosal surfaces may never form crusts.[1] The virus is not removed from the body by immune system, but enters nerve ganglia that serve the infected dermatome where it becomes dormant.[1]
Recurrence
- Many HSV infected people experience a recurrence within the first year of infection, when the virus reactivates from its latent state.[1]
- Development of lesions follows prodrome - which warns of a recurrence and includes tingling (paresthesia), itching, and pain where lumbosacral nerves innervate the skin by hours to days.
- In some individuals, starting to take antiviral treatment when prodrome is experienced can reduce the appearance and duration of lesions.
- Fewer lesions are likely to develop that cause less pain and heal faster (5–10 days without antiviral treatment) than during the primary infection.[1]
- Subsequent outbreaks tend to be periodic or episodic, occur on average four to five times a year when not using antiviral therapy, and may be triggered by stress, illness, fatigue, menstruation.
Treatment
- Although certain therapies can prevent outbreaks or reduce the risk of transmission to partners, no cure is yet available.[1][2]
- You can more detail about treatment strategies for primary infection here and for recurrent disease here.
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Gupta R, Warren T, Wald A (2007) Genital herpes. Lancet 370 (9605):2127-37. DOI:10.1016/S0140-6736(07)61908-4 PMID: 18156035
- ↑ 2.0 2.1 2.2 "STD Facts - Genital Herpes". Retrieved 2008-02-22.