Endophthalmitis
|
WikiDoc Resources for Endophthalmitis |
|
Articles |
|---|
|
Most recent articles on Endophthalmitis Most cited articles on Endophthalmitis |
|
Media |
|
Powerpoint slides on Endophthalmitis |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Endophthalmitis at Clinical Trials.gov Trial results on Endophthalmitis Clinical Trials on Endophthalmitis at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Endophthalmitis NICE Guidance on Endophthalmitis
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Endophthalmitis Discussion groups on Endophthalmitis Patient Handouts on Endophthalmitis Directions to Hospitals Treating Endophthalmitis Risk calculators and risk factors for Endophthalmitis
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Endophthalmitis |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
For more information on bacterial endophthalmitis, please click here
For more information on post-operative endophthalmitis, please click here
For more information on bleb-related endophthalmitis, please click here
For more information on post-traumatic endophthalmitis, please click here
For more information on endogenous endophthalmitis, please click here
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Sara Mehrsefat, M.D. [2]; Mohamed Moubarak, M.D. [3]
Overview
Endophthalmitis is an inflammation of the internal coats of the eye. It is a dreaded complication of all intraocular surgeries, particularly cataract surgery, with possible loss of vision. The most common etiology is infectious. Various bacteria and fungi have been isolated as the cause of infectious endophthalmitis. Other causes include penetrating trauma and retained intraocular foreign bodies.
Historical Perspective
Classification
Endophthalmitis may be classified according to causative organisms into 2 subtypes:
- Bacterial endophthalmitis
- Fungal endophthalmitis
Additionally, endophthalmitis may be classified as either endogenous or exogenous based on the route of infection.
- Exogenous endophthalmitis
- Endogenous endophthalmitis
Pathophysiology
Pathogenesis
Endophthalmitis is an ocular inflammation resulting from the introduction of an infectious agent, either bacterial or fungal, into the posterior segment of the eye. Infectious agents are introduced to the anterior and posterior segments of the eye exogenously or endogenously.[1][2]
Exogenous endophthalmitis occurs following a penetrating ocular injury or ocular surgery. Besides cataract (approximately 90% of all cases), nearly all other type of ocular surgery such as glaucoma, retinal, radial keratotomy, and intravitreal injections may be able to disturb the integrity of the eye globe and contaminate the aqueous humor and/or vitreous humor.[1][2][3]
Endogenous endophthalmitis is caused by the hematologic dissemination of an infection to the eyes. The most common extraocular foci of infection include liver abscess, pneumonia, and endocarditis. Endogenous endophthalmitis is commonly associated with immunosuppression or procedures that increase the risk for blood-borne infections such as diabetes, HIV, malignancy, intravenous drug use, transplantation, immunosuppressive therapy, and catheterization.[1][2][4]
Gross Pathology
On gross pathology, eyelid swelling, eyelid erythema, injected conjunctiva and sclera, hypopyon, chemosis, and mucopurulunt discharge are characteristic findings of bacterial endophthalmitis.
Microscopic Pathology
On microscopic histopathological analysis, infiltration of polymorphonuclear leukocytes or chronic inflammatory cells (depending on the duration of the inflammation) and destruction of ocular structures are characteristic findings of endophthalmitis.
Causes
Infectious
Common causes of endophthalmitis include:
- Bacterial
- Fungal
Drug-induced
Differentiating Endophthalmitis from Other Diseases
Post-operative endophthalmitis must be differentiated from:[1][5][6]
- Toxic anterior segment syndrome (TASS)
- Retained lens material
- Flare-up of pre-existing uveitis
- Dehemoglobinized vitreous hemorrhage
Bleb-related endophthalmitis must be differentiated from:[7]
- Blebitis (bleb-related endophthalmitis is characterized by severe loss of vision, marked pain, and presence of vitritis)
- Anterior uveitis
- Uveitis-glaucoma-hyphema syndrome
Epidemiology and Demographics
In the United States, post-cataract endophthalmitis is the most common form of endophthalmitis. The incidence of post-cataract endophthalmitis is estimated to range from 80 to 360 cases per 100,000 individuals.[8]
Risk Factors
Exogenous Endophthalmitis
Common risk factors in the development of exogenous endophthalmitis include:[2][9][2][10]
- Post-cataract
- Secondary intraocular lens placement
- Intra-ocular lenses (IOLs) with polypropylene
- Intracapsular cataract extraction
- Clear corneal incisions
- Post-traumatic
- Retained intraocular foreign bodies
- Injury in a rural setting
- Delay in repair more than 24 hours
- Bleb related
- Bleb leakage (increase the risk of bleb infection 26 fold)
- Inappropriate use of antifibrotic agents (such as 5-fluorouracil (5-FU) and mitomycin C (MMC))
- Inferior and nasal placement of bleb
- Bleb manipulation/trauma
Endogenous Endophthalmitis
Common risk factors in the development of endogenous endophthalmitis include:[1][2][4]
- Recent hospitalization
- Immunosuppression
Screening
There is no recommended screening guideline for endophthalmitis.[11]
Natural History, Complications, and Prognosis
Natural History
Endophthalmitis is a medical emergency. If left untreated, it may lead to panophthalmitis, corneal infiltration, corneal perforation, and permanent vision loss.
Complications
Common complications of endophthalmitis include:
- Panophthalmitis
- Decrease or loss of vision
- Chronic pain
- Cataract development
- Retinal detachment
- Vitreous hemorrhage
- Hypotony and phthisis bulbi
Prognosis
Early diagnosis and treatment with antimicrobial therapy are fundamental to optimize visual outcome.[2]
Diagnosis
Endophthalmitis is a clinical diagnosis supported by culture of intra-ocular fluids.[1][2]
History and Symptoms
History
A history of recent intraocular surgery or penetrating ocular trauma is usually elicited. Endogenous endophthalmitis is more commonly seen in patients with immunocompromised states such as AIDS and also in diabetes.
Symptoms
The condition is usually accompanied by severe pain, loss of vision, and redness of the conjunctiva and the underlying episclera. Hypopyon may also be observed in endophthalmitis patients by a slit lamp examination.
Physical Examination
Laboratory Findings
Laboratory studies consistent with the diagnosis of post-cataract endophthalmitis include:[1][12][13]
- Culture and gram stain of aqueous humor as well as the vitreous humor
- Polymerase chain reaction (PCR) of aqueous humor as well as the vitreous humor
Imaging Findings
Other Diagnostic Studies
Slit Lamp Examination Findings
- Hypopyon ( >80% of cases)
- Anterior chamber and vitreous inflammation
- Cloudy cornea
- Clumps of exudate in the anterior chamber (around the pupillary margin)
- Cloudy cornea
- Decreased red reflex
-
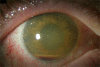
Anterior chamber inflammation, mild corneal edema, and hypopyon in bacterial endophthalmitis
-
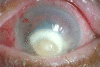
Exogenous fungal endophthalmitis with corneal ulcer
-
(A) Severe conjunctival injection, subconjunctival hemorrhage, corneal stromal edema, and hypopyon (B) Fundus photograph shows a mild pale color of optic disc & macular degeneration[14]
-
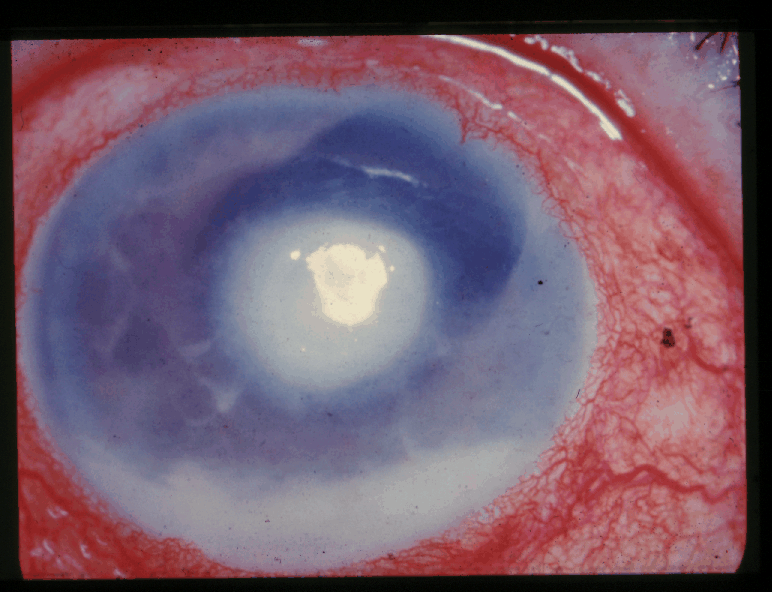
Corneal edema and severe anterior chamber exudation[15]
Treatment
Patients require urgent examination by an expert ophthalmologist and vitreo-retinal specialist who will determine the need for intravitreal injection of antibiotics and possible urgent pars plana vitrectomy. Enucleation may be required to remove a blind and painful eye. Systemic antibiotics are recommended in endogenous bacterial endophthalmitis because the source of the infection is extraocular. Immediate vitrectomy is often necessary
Medical Therapy
Antimicrobial Regimens
- Infectious endophthalmitis[1]
- 1. Causative pathogens
- 2. Empiric antimicrobial therapy
- Preferred regimen: Vancomycin 1 mg per 0.1 mL normal saline intravitreal injection, single dose AND Vancomycin 1 g IV bid for 2 weeks AND Ceftazidime 2.25 mg per 0.1 mL normal saline intravitreal injection, single dose AND Ceftazidime 1 g IV bid for 2 weeks AND Clindamycin 600-1200 mg IV bid to qid for 2 weeks
- Note (1): Re-injection should be considered if the infection does not improve beyond 48 hours of the first injection. Re-injection significantly increases the risk of retinal toxicity.
- Note (2): In addition to intravitreal and systemic antibiotic therapy, vitrectomy is usually necessary
- Note (3): Intravitreal and intravenous Amphotericin B may be added to the regimen if fungal endophthalmitis is suspected
- 3. Pathogen-directed antimicrobial therapy
- 3.1 Bacillus spp.
- Preferred regimen: Vancomycin 1 mg per 0.1 mL normal saline intravitreal injection, single dose AND Vancomycin 1 g IV bid for 2 weeks AND Clindamycin 600-1200 mg IV bid to qid for 2 weeks
- Note: In addition to antimicrobial therapy, vitrectomy is usually necessary
- 3.2 Non-Bacillus gram-positive bacteria
- Preferred regimen: Vancomycin 1 mg per 0.1 mL normal saline intravitreal injection, single dose AND Vancomycin 1 g IV bid for 2 weeks
- Note: In addition to antimicrobial therapy, vitrectomy is usually necessary
- 3.3 Gram-negative bacteria
- Preferred regimen: Ceftazidime 2.25 mg per 0.1 mL normal saline intravitreal injection, single dose AND Ceftazidime 1 g IV bid for 2 weeks
- Note: In addition to antimicrobial therapy, vitrectomy is usually necessary
- 3.4 Candida spp.
- Preferred regimen: (Fluconazole 400-800 mg IV/PO qd for 6-12 weeks OR Voriconazole 400 mg IV/PO bid for 2 doses followed by 200-300 mg IV/PO bid for 6-12 weeks OR Amphotericin B 0.7-1.0 mg/kg IV qd for 6-12 weeks) AND Amphotericin B 5-10 microgram in 0.1 mL in normal saline intravitreal injection, single dose
- Note (1): In addition to antimicrobial therapy, vitrectomy is usually necessary
- 3.5 Aspergillus spp.
- Preferred regimen: Amphotericin B 5-10 microgram in 0.1 mL normal saline intravitreal injection, single dose AND Dexamethasone 400 microgram intravitreal injection, single dose
- Note (1): In addition to antimicrobial therapy, vitrectomy is usually necessary
- Note (2): Repeat antimicrobial regimen in 2 days post-vitrectomy
- 4. Special Considerations
- 4.1 Endogenous endophthalmitis
- 4.1.1 Empiric antimicrobial therapy
- Preferred regimen: Vancomycin 1 mg per 0.1 mL normal saline intravitreal injection, single dose AND Vancomycin 1 g IV bid for 2 weeks AND Ceftazidime 2.25 mg per 0.1 mL normal saline intravitreal injection, single dose AND Ceftazidime 1 g IV bid for 2 weeks AND Clindamycin 600-1200 mg IV bid to qid for 2 weeks
- Note (1): Re-injection should be considered if the infection does not improve beyond 48 hours of the first injection. Re-injection significantly increases the risk of retinal toxicity.
- Note (2): In addition to intravitreal and systemic antibiotic therapy, vitrectomy is usually necessary
- Note (3): Intravitreal and intravenous Amphotericin B may be added to the regimen if fungal endophthalmitis is suspected
- 4.2 Bleb-related endophthalmitis
- 4.2.1 Empiric antimicrobial therapy
- Preferred regimen: Vancomycin 1 mg per 0.1 mL normal saline intravitreal injection, single dose AND Vancomycin 1 g IV bid for 2 weeks AND Ceftazidime 2.25 mg per 0.1 mL normal saline intravitreal injection, single dose AND Ceftazidime 1 g IV bid for 2 weeks AND Clindamycin 600-1200 mg IV bid to qid for 2 weeks
- Note (1): Re-injection should be considered if the infection does not improve beyond 48 hours of the first injection. Re-injection significantly increases the risk of retinal toxicity.
- Note (2): In addition to intravitreal and systemic antibiotic therapy, vitrectomy is usually necessary
- 4.3 Post-operative endophthalmitis
- 4.3.1 Empiric antimicrobial therapy
- Preferred regimen: Vancomycin 1 mg per 0.1 mL normal saline intravitreal injection, single dose AND Ceftazidime 2.25 mg per 0.1 mL normal saline intravitreal injection, single dose
- Note (1): In addition to intravitreal antibiotic therapy, vitrectomy is necessary
- Note (2): If there is no improvement in 48 h, a repeat intravitreal injection may be administered
- Note (3): Late post-operative endophthalmitis is often caused by Propionibacterium acnes (several years post-op)
- 4.3.2 Pathogen-directed antimicrobial therapy
- 4.3.2.1 Gram-positive bacteria
- Preferred regimen: Vancomycin 1 mg per 0.1 mL normal saline intravitreal injection, single dose
- 4.3.2.2 Gram-negative bacteria
- Preferred regimen: Amikacin 0.4 mg per 0.1 mL normal saline intravitreal injection, single dose
- Note: Intravitreal amikacin is associated with the development of retinal microvasculitis
- 4.4 Post-traumatic endophthalmitis
- 4.4.1 Empiric antimicrobial therapy
- Preferred regimen: Vancomycin 1 mg per 0.1 mL normal saline intravitreal injection, single dose AND Ceftazidime 2.25 mg per 0.1 mL normal saline intravitreal injection, single dose AND Amphotericin B 5-10 microgram in 0.1 mL in normal saline intravitreal injection, single dose
- Note (1): Removal of foreign bodies and debridement of necrotic tissue is necessary
- Note (2): In addition to antimicrobial therapy, vitrectomy is necessary
- Note (3): Systemic broad spectrum antibiotics are recommended in post-traumatic endophthalmitis
Surgery
Vitrectomy
Vitrectomy surgically debrides the vitreous humor, similarly to draining an abscess, and is the fastest way of clearing the infection in eyes with fulminant endophthalmitis.[1][12][16]
Prevention
Primary prevention
Common effective measures for the primary prevention of endophthalmitis include:[17]
- Proper sterile preparation of the surgical site
- Sterile preparation of the skin surrounding the surgical eye with Povidone-Iodine 10%
- Povidone-Iodine 5% onto the ocular surface (3-5 minutes prior to surgery)
- Removal of foreign bodies and debridement of necrotic tissue after penetrating eye injury
- Intracameral or intravitreal antibiotic injection after penetrating eye injury
- Effective treatment of underlying medical conditions
Secondary prevention
There are no secondary preventive measures available for post-operative endophthalmiatis, endophthalmiatis is a medical emergency.
External links
- Peters JR. "Endophthalmitis." eMedicine.com. Accessed September 28, 2006.
- Wu L. "Endophthalmitis, Fungal." eMedicine.com. Accessed September 28, 2006.
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 Durand ML (2013). "Endophthalmitis". Clin Microbiol Infect. 19 (3): 227–34. doi:10.1111/1469-0691.12118. PMC 3638360. PMID 23438028.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Kernt M, Kampik A (2010). "Endophthalmitis: Pathogenesis, clinical presentation, management, and perspectives". Clin Ophthalmol. 4: 121–35. PMC 2850824. PMID 20390032.
- ↑ Keay L, Gower EW, Cassard SD, Tielsch JM, Schein OD (2012). "Postcataract surgery endophthalmitis in the United States: analysis of the complete 2003 to 2004 Medicare database of cataract surgeries". Ophthalmology. 119 (5): 914–22. doi:10.1016/j.ophtha.2011.11.023. PMC 3343208. PMID 22297029.
- ↑ 4.0 4.1 Wong JS, Chan TK, Lee HM, Chee SP (2000). "Endogenous bacterial endophthalmitis: an east Asian experience and a reappraisal of a severe ocular affliction". Ophthalmology. 107 (8): 1483–91. PMID 10919895.
- ↑ Kutty PK, Forster TS, Wood-Koob C, Thayer N, Nelson RB, Berke SJ; et al. (2008). "Multistate outbreak of toxic anterior segment syndrome, 2005". J Cataract Refract Surg. 34 (4): 585–90. doi:10.1016/j.jcrs.2007.11.037. PMID 18361979.
- ↑ Cutler Peck CM, Brubaker J, Clouser S, Danford C, Edelhauser HE, Mamalis N (2010). "Toxic anterior segment syndrome: common causes". J Cataract Refract Surg. 36 (7): 1073–80. doi:10.1016/j.jcrs.2010.01.030. PMID 20610082.
- ↑ Mac, Ivan, and Joern B. Soltau. "Glaucoma-filtering bleb infections." Current opinion in ophthalmology 14.2 (2003): 91-94.
- ↑ Aaberg TM, Flynn HW, Schiffman J, Newton J (1998). "Nosocomial acute-onset postoperative endophthalmitis survey. A 10-year review of incidence and outcomes". Ophthalmology. 105 (6): 1004–10. doi:10.1016/S0161-6420(98)96000-6. PMID 9627649.
- ↑ Taban M, Behrens A, Newcomb RL, Nobe MY, Saedi G, Sweet PM; et al. (2005). "Acute endophthalmitis following cataract surgery: a systematic review of the literature". Arch Ophthalmol. 123 (5): 613–20. doi:10.1001/archopht.123.5.613. PMID 15883279.
- ↑ Essex RW, Yi Q, Charles PG, Allen PJ (2004). "Post-traumatic endophthalmitis". Ophthalmology. 111 (11): 2015–22. doi:10.1016/j.ophtha.2003.09.041. PMID 15522366.
- ↑ U.S. Preventive Services Task Force http://www.uspreventiveservicestaskforce.org/BrowseRec/Search?s=endophthalmitis Accessed on August 5, 2016
- ↑ 12.0 12.1 Barza M, Pavan PR, Doft BH, Wisniewski SR, Wilson LA, Han DP; et al. (1997). "Evaluation of microbiological diagnostic techniques in postoperative endophthalmitis in the Endophthalmitis Vitrectomy Study". Arch Ophthalmol. 115 (9): 1142–50. PMID 9298055.
- ↑ Seal D, Reischl U, Behr A, Ferrer C, Alió J, Koerner RJ; et al. (2008). "Laboratory diagnosis of endophthalmitis: comparison of microbiology and molecular methods in the European Society of Cataract & Refractive Surgeons multicenter study and susceptibility testing". J Cataract Refract Surg. 34 (9): 1439–50. doi:10.1016/j.jcrs.2008.05.043. PMID 18721702.
- ↑ Seo SW, Chung IY, Kim E, Park JM (2008). "A case of postoperative Sphingomonas paucimobilis endophthalmitis after cataract extraction". Korean J Ophthalmol. 22 (1): 63–5. doi:10.3341/kjo.2008.22.1.63. PMC 2629956. PMID 18323709.
- ↑ Jaru-Ampornpan P, Agarwal A, Midha NK, Kim SJ (2011). "Traumatic Endophthalmitis due to Cellulosimicrobium cellulans". Case Rep Ophthalmol Med. 2011: 469607. doi:10.1155/2011/469607. PMC 3350247. PMID 22606461.
- ↑ "Results of the Endophthalmitis Vitrectomy Study. A randomized trial of immediate vitrectomy and of intravenous antibiotics for the treatment of postoperative bacterial endophthalmitis. Endophthalmitis Vitrectomy Study Group". Arch Ophthalmol. 113 (12): 1479–96. 1995. PMID 7487614.
- ↑ Kelkar A, Kelkar J, Amuaku W, Kelkar U, Shaikh A (2008). "How to prevent endophthalmitis in cataract surgeries?". Indian J Ophthalmol. 56 (5): 403–7. PMC 2636140. PMID 18711270.
![Corneal edema and severe anterior chamber exudation[15]](/images/c/c4/IndianJOphthalmol-55-464-g001.gif)