|
|
| (91 intermediate revisions by 18 users not shown) |
| Line 1: |
Line 1: |
| | __NOTOC__ |
| | {| class="infobox" style="float:right;" |
| | |- |
| | | [[File:Siren.gif|link=SLE resident survival guide|41x41px]]|| <br> || <br> |
| | | [[SLE resident survival guide|'''Resident'''<br>'''Survival'''<br>'''Guide''']] |
| | |} |
| {{Infobox_Disease | | {{Infobox_Disease |
| |Name = Lupus Erythematosus | | |Name = Lupus Erythematosus |
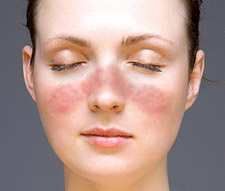
| |Image = Lupus facial rash.jpg | | |Image = Lupus facial rash.jpg |
| |Caption = Typical "butterfly"-like rash over the cheeks in lupus | | |Caption = Typical "butterfly"-like rash over the cheeks in lupus |
| |ICD10 = {{ICD10|L|93||l|80}}, {{ICD10|M|32||m|30}}
| |
| |ICD9 = {{ICD9|710.0}}
| |
| |DiseasesDB = 12782
| |
| |ICDO =
| |
| |OMIM = 152700
| |
| |MedlinePlus = 000435
| |
| |eMedicineSubj = med
| |
| |eMedicineTopic = 2228
| |
| |eMedicine_mult = {{eMedicine2|emerg|564}}
| |
| |MeshID = D008180
| |
| }} | | }} |
| [[Image:Discoid lupus erythematosus.JPG|thumb|[[Discoid lupus erythematosus]] [[lesion]] of the face]]
| | {{Systemic lupus erythematosus}} |
| {{SI}}
| | '''For patient information click [[{{PAGENAME}} (patient information)|here]]''' |
| {{CMG}} | |
|
| |
|
| '''Associate Editor-In-Chief:''' {{CZ}}
| | {{CMG}}; {{AE}} {{MIR}}, {{CZ}}, {{RT}} |
|
| |
|
| {{EH}} | | {{SK}} SLE, Lupus erythematosus, Systemic lupus, Lupus, Disseminated lupus erythematosus, Discoid lupus, Cutaneous lupus erythematosus |
| | ==[[Systemic lupus erythematosus overview|Overview]]== |
|
| |
|
| ===Click [[The Heart in Systemic Lupus Erythematosus (SLE)|here]] for The heart in Systemic Lupus Erythematosus=== | | == [[Systemic lupus erythematosus historical perspective|Historical perspective]] == |
|
| |
|
| ==Overview== | | == [[Systemic lupus erythematosus classification scheme|Classification]] == |
|
| |
|
| '''Systemic Lupus Erythematosus''' ('''SLE''' or '''lupus''') is a chronic [[Autoimmunity|autoimmune disease]] that can be fatal, though with recent medical advances fatalities are becoming increasingly rare. As with other [[Autoimmunity|autoimmune diseases]], the [[immune system]] attacks the body’s cells and tissue, resulting in inflammation and tissue damage. <ref>{{cite web |url=http://www.lupus.org/education/stats.html#1 |title=LUPUS FOUNDATION OF AMERICA |accessdate=2007-07-04 |format= |work=}}</ref>
| | ==[[Systemic lupus erythematosus pathophysiology|Pathophysiology]]== |
|
| |
|
| SLE can affect any part of the body, but most often harms the [[heart]], [[joint]]s, [[skin]], [[lung]]s, [[blood vessel]]s, [[liver]], [[kidney]]s and [[Nervous system#Vertebrates|nervous system]].<ref>{{cite web |url=http://www.lupus.org/education/stats.html#1 |title=LUPUS FOUNDATION OF AMERICA |accessdate=2007-07-04 |format= |work=}}</ref>
| | ==[[Systemic lupus erythematosus causes|Causes]]== |
|
| |
|
| The course of the disease is unpredictable, with periods of illness (called flares) alternating with remission. Lupus can occur at any age, and is most common in women, particularly of non-European descent.<ref>{{cite web |url=http://www.lupus.org/education/stats.html#1 |title=LUPUS FOUNDATION OF AMERICA |accessdate=2007-07-04 |format= |work=}}</ref> Lupus is treatable [[Symptomatic treatment|symptomatically]], mainly with [[corticosteroid]]s and [[immunosuppression|immunosuppressants]], though there is currently no cure. However, many people with Lupus lead long and substantial lives.
| | ==[[Differentiating systemic lupus erythematosus from other diseases|Differentiating Systemic Lupus Erythematosus from Other Diseases]]== |
|
| |
|
| ==Differential Diagnosis== | | ==[[Systemic lupus erythematosus epidemiology and demographics|Epidemiology and Demographics]]== |
|
| |
|
| * [[Abdominal pain]]
| | ==[[Systemic lupus erythematosus risk factors|Risk Factors]]== |
| * Discoid skin lesions
| |
| * Erythematous macules
| |
| * [[Fatigue]]
| |
| * [[Hemolytic anemia]]
| |
| * [[Interstitial lung disease]]
| |
| * [[Keratoconjunctivitis sicca]]
| |
| * [[Leukopenia]]
| |
| * Mucosal lesions
| |
| * [[Pericarditis]]
| |
| * Photo distributed rash
| |
| * [[Pleural effusion]]
| |
| * [[Pleuritic chest pain]]
| |
| * [[Pneumonitis]]
| |
| * [[Polyarthritis]] / [[polyarthralgia]]
| |
| * [[Raynaud phenomenon]]
| |
| * [[Renal disease]]
| |
| * [[Renal vasculitis]]
| |
| * [[Seizure]]s
| |
| * [[Stroke]]
| |
| * [[Thrombocytopenia]]
| |
| * [[Weight loss]]
| |
|
| |
|
| ==Etymology== | | ==[[Systemic lupus erythematosus screening|Screening]]== |
|
| |
|
| There are several explanations ventured for the term '''lupus erythematosus'''. Lupus is [[Latin]] for wolf, and 'erythro' is derived from ερυθρός{{Polytonic|}}, Greek for "red." All explanations originate with the reddish, butterfly-shaped [[malar rash]] that the disease classically exhibits across the nose and cheeks.
| | ==[[Systemic lupus erythematosus natural history, complications and prognosis|Natural History, Complications and Prognosis]]== |
| # In various accounts, some doctors thought the rash resembled the pattern of fur on a wolf's face.
| |
| # In other accounts doctors thought that the rash, which was often more severe in earlier centuries, created lesions that resembled wolf bites or scratches.
| |
| # Stranger still is the account that the term "Lupus" didn't come from Latin at all, but from the term for a French style of mask which women reportedly wore to conceal the rash on their faces. The mask is called a "loup", French for "Wolf"
| |
| # Another common explanation for the term is that the disease's course involves repeated attacks like those of a voracious predator, leaving behind the red blotches.
| |
|
| |
|
| ==History== | | ==Diagnostic criteria== |
|
| |
|
| Medical historians have theorized people with [[porphyria]]s (a disease that shares many symptoms with Lupus) generated folklore stories of vampires and werewolves due to the photosensitivity, scarring, hair growth and porphyrin brownish-red stained teeth in severe recessive forms of porphyria or combinations of the disorders known as dual, homozygous or compound heterozygous porphyrias.
| | [[Diagnostic criteria|Diagnostic Criteria]] | [[Systemic lupus erythematosus history and symptoms|History and Symptoms]] | [[Systemic lupus erythematosus physical examination|Physical Examination]] | [[Systemic lupus erythematosus laboratory tests|Laboratory Findings]] | [[Systemic lupus erythematosus electrocardiogram|Electrocardiogram]] | [[Systemic lupus erythematosus x ray|X Ray]] | [[Systemic lupus erythematosus CT|CT]] | [[Systemic lupus erythematosus MRI|MRI]] | [[Systemic lupus erythematosus ultrasound or echocardiography|Echocardiography or Ultrasound]] | [[Systemic lupus erythematosus other imaging findings|Other Imaging Findings]] | [[Systemic lupus erythematosus other diagnostic studies|Other Diagnostic Studies]] |
| | |
| The history of lupus erythematosus can be divided into three periods: the classical, neoclassical, and modern. The classical period began when the disease was first recognized in the Middle Ages and saw the description of the dermatological manifestation of the disorder. The term ''lupus'' is attributed to the 12th century [[physician]] [[Rogerius (physician)|Rogerius]], who used it to describe the classic malar rash. The neoclassical period was heralded by Móric Kaposi's recognition in 1872 of the systemic manifestations of the disease. The modern period began in 1948 with the discovery of the LE cell (the ''Lupus Erythematosus'' cell, a misnomer as it occurs with other diseases as well) and is characterised by advances in our knowledge of the pathophysiology and clinical-laboratory features of the disease, as well as advances in treatment.
| |
| | |
| Useful medication for the disease was first found in 1894, when [[quinine]] was first reported as an effective therapy. Four years later, the use of [[Salicylic acid|salicylate]]s in conjunction with quinine was noted to be of still greater benefit. This was the best available treatment to patients until the middle of the twentieth century, when Hench discovered the efficacy of [[corticosteroid]]s in the treatment of SLE.
| |
| | |
| ==Epidemiology==
| |
| | |
| Previously believed to be a rare disease, Lupus has seen an increase in awareness and education since the 1960s. This has helped many more patients get an accurate diagnosis making it possible to estimate the number of people with lupus. In the United States alone, it is estimated that between 270,000 and 1.5 million people have lupus, making it more common than [[cystic fibrosis]] or [[cerebral palsy]]. The disease affects both females and males, though young women are diagnosed nine times more often than men. SLE occurs with much greater severity among African-American women, who suffer more severe symptoms as well as a higher mortality rate. <ref>[http://nmanet.org/images/uploads/Great_Imitator.pdf#search=%22lupus%20great%20imitator%22 Lupus and African-American women]</ref> Worldwide, a conservative estimate states that over 5 million people have lupus.
| |
| | |
| Although SLE can occur in anyone at any age, it is most common in women of childbearing age. It affects 1 in 4000 people in the United States, with women becoming afflicted far more often than men. The disease appears to be more prevalent in women of African, Asian, Hispanic and Native American origin but this may be due to socioeconomic factors. People with relatives who suffer from SLE, [[rheumatoid arthritis]] or [[thrombotic thrombocytopenic purpura]] are at a slightly higher risk than the general population.<ref name="DiGeronimo">DiGeronimo, Theresa. New Hope for People with Lupus. Prima Publishing. 2002.</ref>
| |
| | |
| ==Classification==
| |
| | |
| Lupus is a chronic [[Autoimmunity|autoimmune disease]] in which the body's own defense system attacks otherwise healthy tissue.
| |
| Clinically, it can affect multiple organ systems including the heart, skin, joints, kidneys and nervous system.
| |
| There are several types of lupus; in general, when the word lupus alone is used, reference is to systemic lupus erythematosus, as discussed in this article. Other types include:<ref name="Andrews">James, William; Berger, Timothy; Elston, Dirk (2005). ''Andrews' Diseases of the Skin: Clinical Dermatology''. (10th ed.). Saunders. Chapter 8. ISBN 0721629210.</ref> Other types include:
| |
| | |
| *Chronic cutaneous lupus erythematosus
| |
| **[[Discoid lupus erythematosus]], a skin disorder that causes a red, raised rash on the face and scalp. Discoid lupus occasionally (1–5%) develops into SLE.<ref>[http://www.skinsite.com/info_discoid_lupus_erythematosus.htm Discoid Lupus Erythematosus]</ref>
| |
| ***Localized discoid lupus erythematosus
| |
| ***Generalized discoid lupus erythematosus
| |
| ***Childhood discoid lupus erythematosus
| |
| **Chilblain lupus erythematosus (Hutchinson)
| |
| **Lupus erythematosus-lichen planus overlap syndrome
| |
| **Lupus erythematosus panniculitis (Lupus erythematosus profundus)
| |
| **Subacute cutaneous lupus erythematosus, which causes nonscarring skin [[lesions]] on patches of skin exposed to sunlight.<ref name=niams>{{cite web |url=http://www.niams.nih.gov/Health_Info/Lupus/default.asp |title=Handout on Health: Systemic Lupus Erythematosus |accessdate=2007-11-23 |month=August | year=2003 |work=The National Institute of Arthritis and Musculoskeletal and Skin Diseases |publisher=National Institutes of Health}}</ref>
| |
| **Tumid lupus erythematosus
| |
| **Verrucous lupus erythematosus (Hypertrophic lupus erythematosus)
| |
| *Neonatal lupus erythematosus, a rare disease affecting babies born to women with SLE, [[Sjögren's syndrome]], or sometimes no autoimmune disorder. It is theorized that maternal antibodies attack the fetus, causing skin rash; liver problems; low blood counts, which gradually fade; and heart block, leading to [[bradycardia]].<ref name=niams/>
| |
| *Childhood systemic lupus erythematosus, the pediatric variant of systemic lupus erythematosus.
| |
| *[[Drug-induced lupus erythematosus]], a drug-induced form of SLE; this type of lupus can occur equally in either sex.
| |
| *[[Lupus nephritis]], an inflammation of the [[kidney]]s caused by SLE.
| |
| *Complement deficiency syndromes
| |
| | |
| ==Causes==
| |
| | |
| Despite the dramatic rise in Lupus research in recent years, the exact cause of the disease remains unknown. Indeed, consensus is still lacking on whether Lupus is a single condition or a group of related diseases. SLE is a chronic [[inflammation|inflammatory]] disease believed to be a [[Hypersensitivity#Type III - immune complex|type III hypersensitivity]] response with potential [[Hypersensitivity#Type 2 - antibody-dependent|type II]] involvement,<ref>[http://pathmicro.med.sc.edu/ghaffar/hyper00.htm University of South Carolina lecture on immunology]</ref> characterized by the body's production of antibodies against the nuclear components of its own cells. There are three mechanisms by which lupus is thought to develop: genetic predisposition, environmental triggers and drug reaction (drug-induced lupus).
| |
| | |
| ===Genetics===
| |
| | |
| The first mechanism may arise genetically. Research indicates that SLE may have a [[genetics|genetic]] link. Lupus does run in families, but no single "lupus gene" has yet been identified. Instead, multiple genes appear to influence a person's chance of lupus developing when triggered by environmental factors. The most important genes are located on [[Chromosome 6 (human)|chromosome 6]], where mutations may occur randomly (''de novo'') or be inherited. Additionally, people with SLE have an altered RUNX-1 binding site, which may be either cause or contributor (or both) to the condition. Altered binding sites for RUNX-1 have also been found in people with [[psoriasis]] and [[rheumatoid arthritis]].
| |
| | |
| ===Environmental triggers===
| |
| | |
| The second mechanism may be due to environmental factors. These factors may not only exacerbate existing lupus conditions, but also trigger the initial onset. They include certain medications (such as some [[antidepressant]]s and [[antibiotic]]s), extreme stress, exposure to sunlight, hormones, and infections. Some researchers have sought to find a connection between certain infectious agents ([[virus]]es and [[bacteria]]), but no pathogen can be consistently linked to the disease. UV radiation has been shown to trigger the photosensitive lupus rash, but some evidence also suggests that UV light is capable of altering the structure of the DNA, leading to the creation of autoantibodies. Some researchers have found that women with [[silicone]] gel-filled [[breast implant]]s have produced antibodies to their own [[collagen]], but it is not known how often these antibodies occur in the general population and there is no data that show these antibodies cause [[connective tissue disease]]s such as lupus.
| |
| | |
| ===Drug reactions===
| |
| | |
| [[Drug-induced lupus erythematosus]] is a reversible condition that usually occurs in patients being treated for a long-term illness. Drug-induced lupus mimics systemic lupus. However, symptoms of drug-induced lupus generally disappear once a patient is taken off the medication which triggered the episode. There are about 400 medications currently in use that can cause this condition, though the most common drugs are [[procainamide]], [[hydralazine]] and [[quinidine]].
| |
| | |
| ===Non-SLE forms of lupus===
| |
| | |
| Discoid (cutaneous) lupus is limited to skin symptoms and is diagnosed via biopsy of skin rash on the face, neck or scalp. Often an [[anti-nuclear antibody]] (ANA) test for discoid patients is negative or a low-titre positive. About 10% of discoid lupus patients eventually develop SLE.
| |
| | |
| ==Pathophysiology==
| |
| | |
| Lupus is an example of [[pathophysiology]], a disturbance of the normal functioning of the body. One manifestation of lupus is abnormalities in apoptosis, a type of programmed cell death in which aging or damaged cells are neatly disposed of as a part of normal growth or functioning.
| |
| | |
| ===Transmission===
| |
| | |
| In SLE, the body's immune system produces antibodies against itself, particularly against proteins in the cell nucleus. SLE is triggered by environmental factors that are unknown.
| |
| | |
| "All the key components of the immune system are involved in the underlying mechanisms" of SLE, according to Rahman, and SLE is the prototypical autoimmune disease. The immune system must have a balance ([[homeostasis]]) between being sensitive enough to protect against infection, and being too sensitive and attacking the body's own proteins (autoimmunity). From an evolutionary perspective, according to Crow, the population must have enough genetic diversity to protect itself against a wide range of possible infection; some genetic combination's result in autoimmunity. The likely environmental triggers include ultraviolet light, drugs, and viruses. These stimuli cause the [[apoptosis|destruction]] of cells and expose their DNA, [[histones]], and other proteins, particularly parts of the cell nucleus. Because of genetic variations in different components of the immune system, in some people the immune system attacks these nuclear-related proteins and produces antibodies against them. In the end, these antibody complexes damage blood vessels in critical areas of the body, such as the [[glomeruli]] of the kidney; these antibody attacks are the cause of SLE. Researchers are now identifying the individual genes, the proteins they produce, and their role in the immune system. Each protein is a link on the autoimmune chain, and researchers are trying to find drugs to break each of those links. <ref name="rahman">{{cite journal |author=Anisur Rahman and David A. Isenberg|title=Review Article: Systemic Lupus Erythematosus|journal=N Engl J Med|volume=358|issue=9|pages=929–939|year=2008|date=February 28, 2008|pmid=18305268|url=http://content.nejm.org/cgi/content/full/358/9/929|doi=10.1056/NEJMra071297}}</ref><ref>{{cite journal |author=Mary K. Crow|title=Collaboration, Genetic Associations, and Lupus Erythematosus|journal=N Engl J Med|volume=358|issue=9|pages=956–961|year=2008|date=February 28, 2008|pmid=18204099|url=http://content.nejm.org/cgi/content/full/358/9/956|doi=10.1056/NEJMe0800096}}</ref><ref>{{cite journal |author=Geoffrey Hom, Robert R. Graham, Barmak Modrek, et al.|title=Association of Systemic Lupus Erythematosus with C8orf13–BLK and ITGAM–ITGAX|journal=N Engl J Med|volume=358|issue=9|pages=900–909|year=2008|date=February 28, 2008|pmid=18204098|url=http://content.nejm.org/cgi/content/full/358/9/900|doi=10.1056/NEJMoa0707865}}</ref>
| |
| | |
| SLE is a chronic [[inflammation|inflammatory]] disease believed to be a [[Hypersensitivity#Type 3 - immune complex|type III hypersensitivity]] response with potential [[Hypersensitivity#Type 2 - antibody-dependent|type II]] involvement.<ref>[http://pathmicro.med.sc.edu/ghaffar/hyper00.htm University of South Carolina School of Medicine lecture notes, Immunology, Hypersensitivity reactions. General discussion of hypersensitivity, not specific to SLE.]</ref>
| |
| | |
| ===Abnormalities in apoptosis===
| |
| | |
| *[[Apoptosis]] is increased in [[monocyte]]s and [[keratinocyte]]s
| |
| *[[Gene expression|Expression]] of Fas by [[B cell]]s and [[T cell]]s is increased
| |
| *There are correlations between the apoptotic rates of lymphocytes and disease activity
| |
| | |
| Tangible body macrophages (TBMs) are large phagocytic cells in the [[germinal center]]s of secondary [[lymph node]]s. They express CD68 protein. These cells normally engulf B cells which have undergone apoptosis after [[somatic hypermutation]]. In some patients with SLE, significantly fewer TBMs can be found, and these cells rarely contain material from apoptotic B cells. Also, uningested apoptotic nuclei can be found outside of TBMs. This material may present a threat to the tolerization of B cells and T cells. [[Dendritic cell]]s in the germinal center may endocytose such antigenic material and present it to T cells, activating them. Also, apoptotic chromatin and nuclei may attach to the surfaces of follicular dendritic cells and make this material available for activating other B cells which may have randomly acquired self-specificity through [[somatic hypermutation]].<ref> {{cite journal | author=Gaipl, U S; Kuhn, A; Sheriff, A; Munoz, L E; Franz, S; Voll, R E; Kalden, J R; Herrmann, M | title=Clearance of apoptotic cells in human SLE.| journal=Current directions in autoimmunity | volume=9 | issue= | year=2006 | pages=173-87 | url = http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16394661&dopt=Abstract | id = PMID: 1639466 [http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16394661&dopt=Abstract Abstract] (full text requires registration) }}</ref>
| |
| | |
| ===Clearance deficiency===
| |
| [[image:Picture1_englisch.jpg|left|thumb|Clearance deficiency]]The exact mechanisms for the development of systemic lupus erythematosus (SLE) are still unclear since the pathogenesis is a multifactorial event. Beside discussed causations, impaired clearance of dying cells is a potential pathway for the development of this systemic [[autoimmune disease]]. This includes deficient phagocytic activity, scant serum components in addition to increased [[apoptosis]].
| |
| | |
| [[Monocytes]] isolated from [[whole blood]] of SLE patients show reduced expression of CD44 surface molecules involved in the uptake of apoptotic cells. Most of the [[monocyte]]s and tingible body macrophages (TBM), which are found in the germinal centres of [[lymph nodes]], even show a definitely different morphology in patients with SLE. They are smaller or scarce and die earlier. Serum components like complement factors, [[CRP]] and some [[glycoproteins]] are furthermore decisively important for an efficiently operating phagocytosis. In patients these components are often missing, diminished or inefficient.
| |
| | |
| The clearance of early apoptotic cells is an important function in multicellular organisms. It leads to a progression of the apoptosis process and finally to secondary [[necrosis]] of the cells, if this ability is disturbed. Necrotic cells release nuclear fragments as potential autoantigens as well as internal danger signals, inducing [[maturation]] of [[dendritic cells]] (DC), since they have lost their membranes integrity. Increased appearance of apoptotic cells also is simulating inefficient clearance. That leads to maturation of DC and also to the presentation of intracellular antigens of late apoptotic or secondary necrotic cells, via MHC molecules.
| |
| | |
| [[Autoimmunity]] possibly results by the extended exposure to nuclear and intracellular autoantigens derived from late apoptotic and secondary necrotic cells. B and [[T cell]] tolerance for apoptotic cells is abrogated and the [[lymphocytes]] get activated by these autoantigens; [[inflammation]] and the production of autoantibodies by [[plasma cells]] is initiated. A clearance deficiency in the skin for apoptotic cells has also been observed in patients with cutaneous lupus erythematosus (CLE).
| |
| | |
| ===Accumulation in germinal centres (GC)===
| |
| [[image:Picture2_englisch.jpg|left|160px|thumb|Germinal centres]]
| |
| In healthy conditions apoptotic lymphocytes are removed in germinal centres by specialised phagocytes, the tingible body macrophages (TBM); that’s why no free apoptotic and potential autoantigenic material can bee seen.
| |
| | |
| In some patients with SLE accumulation of apoptotic [[debris]] can be observed in GC, because of an ineffective clearance of apoptotic cells.
| |
| | |
| In close proximity to TBM, [[follicular dendritic cells]] (FDC) are localized in GC, which attach antigen material to their surface and in contrast to bone marrow-derived DC, neither take it up nor present it via MHC molecules.
| |
| | |
| Autoreactive [[B cells]] can accidentally emerge during [[somatic hypermutation]] and migrate into the GC light zone. Autoreactive B cells, maturated coincidently, normally don’t receive survival signals by antigen planted on follicular dendritic cells and perish by apoptosis.
| |
| | |
| In the case of clearance deficiency apoptotic nuclear debris accumulates in the light zone of GC and gets attached to FDC. This serves as a germinal centre survival signal for autoreactive B-cells.
| |
| | |
| After migration into the mantle zone autoreactive B cells require further survival signals from autoreactive helper T cells, which promote the maturation of autoantibody producing plasma cells and B memory cells.
| |
| | |
| In the presence of autoreactive T cells a chronic [[autoimmune disease]] may be the consequence.
| |
| <br clear="left"/>
| |
| | |
| ===Anti-nRNP autoimmunity===
| |
| | |
| [[Autoantibodies]] to nRNP A and nRNP C initially targeted restricted, [[proline]]-rich motifs. Antibody binding subsequently spread to other [[epitopes]]. The similarity and [[cross-reactivity]] between the initial targets of nRNP and Sm autoantibodies identifies a likely commonality in cause and a focal point for intermolecular epitope spreading.<ref name="pmid19248110">{{cite journal |author=Poole BD, Schneider RI, Guthridge JM, ''et al'' |title=Early targets of nuclear RNP humoral autoimmunity in human systemic lupus erythematosus |journal=Arthritis Rheum. |volume=60 |issue=3 |pages=848–859 |year=2009 |month=February |pmid=19248110 |doi=10.1002/art.24306 |url=http://dx.doi.org/10.1002/art.24306 |issn=}}</ref>
| |
| | |
| ===Others===
| |
| | |
| Elevated expression of HMGB1 was found in the sera of patients and mice with systemic lupus erythematosus, High Mobility Group Box 1 (HMGB1) is a [[nuclear]] [[protein]] participating in [[chromatin]] architecture and [[transcription|transcriptional regulation]]. Recently, there is increasing evidence that HMGB1 contributes to the pathogenesis of [[chronic]] [[inflammatory]] and [[autoimmune diseases]] due to its pro-inflammatory and immunostimulatory properties.<ref name="pmid19247800">{{cite journal |author=Pan HF, Wu GC, Li WP, Li XP, Ye DQ |title=High Mobility Group Box 1: a potential therapeutic target for systemic lupus erythematosus |journal=Mol. Biol. Rep. |volume= |issue= |pages= |year=2009 |month=February |pmid=19247800 |doi=10.1007/s11033-009-9485-7 |url= |issn=}}</ref>
| |
| | |
| ==Signs and symptoms==
| |
| | |
| SLE is one of several diseases known as [[the great imitator]]<ref>[http://healthcare.utah.edu/healthtools/articles/lupus.html Lupus: The Great Imitator]</ref> because its symptoms vary so widely it often mimics or is mistaken for other illnesses, and because the symptoms come and go unpredictably. Diagnosis can be elusive, with patients sometimes suffering unexplained symptoms and untreated SLE for years. Common initial and chronic complaints are [[fever]], [[malaise]], [[arthralgia|joint pains]], [[myalgia]]s and [[Fatigue (medical)|fatigue]]. Because they are so often seen with other diseases, these signs and symptoms are not part of the diagnostic criteria for SLE. When occurring in conjunction with other signs and symptoms (below), however, they are considered suggestive.
| |
| | |
| ===Most Common Symptoms===
| |
| | |
| # [[Joint pain]] or [[joint swelling]]
| |
| # [[Skin rash]]
| |
| # [[Malaise]] or [[fatigue]]
| |
| | |
| ===Common Symptoms Explained===
| |
| | |
| ;Dermatological manifestations: As many as 30% of patients present with some dermatological symptoms (and 65% suffer such symptoms at some point), with 30% to 50% suffering from the classic [[malar rash]] (or ''butterfly rash'') associated with the disease. Patients may present with discoid lupus (thick, red scaly patches on the skin). [[Alopecia]], mouth, nasal, and vaginal [[mouth ulcer|ulcers]], and lesions on the skin are also possible manifestations.
| |
| | |
| ;Musculoskeletal manifestations: Patients most often seek medical attention for [[joint pain]], with small joints of the hand and wrist usually affected, although any joint is at risk. The Lupus Foundation of America "estimates that 95 percent of lupus cases involve achy joints <ref name="DiGeronimo">DiGeronimo, Theresa. New Hope for People with Lupus. Prima Publishing. 2002.</ref> Unlike [[rheumatoid arthritis]], SLE arthropathy is not usually destructive of [[bone]], however, deformities caused by the disease may become irreversible in as many as 20% of patients.This small percentage may experience "damage to tendons or joint coverings in the hand" which leads to "deformity of the finger joint" <ref name="DiGeronimo">DiGeronimo, Theresa. New Hope for People with Lupus. Prima Publishing. 2002.</ref>
| |
| | |
| ;Hematological manifestations: [[Anemia]] and iron deficiency may develop in as many as half of patients. Low [[platelet]] and [[white blood cell]] counts may be due to the disease or a side-effect of pharmacological treatment. Patients may have an association with [[Antiphospholipid syndrome|antiphospholipid antibody syndrome]] (a thrombotic disorder) where autoantibodies to phospholipids are present in the patient's serum. Abnormalities associated with antiphospholipid antibody syndrome include a paradoxical prolonged PTT (which usually occurs in hemorrhagic disorders) and a positive test for antiphospholipid antibodies; the combination of such findings have earned the term "[[lupus anticoagulant]] positive". Another autoantibody finding in lupus is the [[anticardiolipin antibody]] which can cause a false positive test for [[syphilis]].
| |
| | |
| ;Cardiac manifestations: Patients may present with inflammation of various parts of the [[heart]], such as [[pericarditis]], [[myocarditis]], and [[endocarditis]]. The endocarditis of SLE is characteristically non-infective ([[Libman-Sacks endocarditis]]) and involves either the [[mitral valve]] or the [[tricuspid valve]]. [[Atherosclerosis]] also tends to occur more often and advance more rapidly in SLE patients than in the general population.<ref>{{cite journal | author=Yu Asanuma, M.D., Ph.D., Annette Oeser, B.S., Ayumi K. Shintani, Ph.D., M.P.H., Elizabeth Turner, M.D., Nancy Olsen, M.D., Sergio Fazio, M.D., Ph.D., MacRae F. Linton, M.D., Paolo Raggi, M.D., and C. Michael Stein, M.D. | title=Premature coronary-artery atherosclerosis in systemic lupus erythematosus
| |
| | journal=New England Journal of Medicine | volume=349 | issue=Dec. 18 | year=2003| pages=2407-2414 | url = http://content.nejm.org/cgi/content/full/349/25/2407 | id = PMID 14681506 [http://content.nejm.org/cgi/content/abstract/349/25/2407 Abstract] (full text requires registration) }}</ref><ref>{{cite journal | author=Bevra Hannahs Hahn, M.D. | title=Systemic lupus erythematosus and accelerated atherosclerosis | journal=New England Journal of Medicine | volume=349 | issue=Dec. 18 | year=2003 | pages=2379-2380 | url = http://content.nejm.org/cgi/content/full/349/25/2379 | id =PMID 14681501 [http://content.nejm.org/cgi/content/extract/349/25/2379 Extract] (full text requires registration) }}</ref><ref> {{cite journal | author=Mary J. Roman, M.D., Beth-Ann Shanker, A.B., Adrienne Davis, A.B., Michael D. Lockshin, M.D., Lisa Sammaritano, M.D., Ronit Simantov, M.D., Mary K. Crow, M.D., Joseph E. Schwartz, Ph.D., Stephen A. Paget, M.D., Richard B. Devereux, M.D., and Jane E. Salmon, M.D. | title=Prevalence and correlates of accelerated atherosclerosis in systemic lupus erythematosus | journal=New England Journal of Medicine | volume=349 | issue=Dec. 18 | year=2003 | pages=2399-2406 | url = http://content.nejm.org/cgi/content/full/349/25/2399
| |
| | id = PMID 14681505 [http://content.nejm.org/cgi/content/abstract/349/25/2399 Abstract] (full text requires registration) }}</ref>
| |
| | |
| ;Pulmonary manifestations: Lung and pleura inflammation can cause [[Pleurisy|pleuritis]], [[pleural effusion]], lupus pneumonitis, chronic diffuse interstitial lung disease, [[pulmonary hypertension]], [[Pulmonary embolism|pulmonary emboli]], [[pulmonary hemorrhage]].
| |
| | |
| ;Hepatic involvement: See [[autoimmune hepatitis]]
| |
| | |
| ;Renal involvement: Painless [[hematuria]] or [[proteinuria]] may often be the only presenting renal symptom. Acute or chronic renal impairment may develop with [[lupus nephritis]], leading to acute or end stage [[renal failure]]. Because of early recognition and management of SLE, end stage renal failure occurs in less than 5% of patients.
| |
| | |
| :Histologically, a hallmark of SLE is membranous [[glomerulonephritis]] with "wire loop" abnormalities.<ref>{{cite web |url=http://erl.pathology.iupui.edu/C603/GENE607.HTM |title=General Pathology Images for Immunopathology |accessdate=2007-07-24 |format= |work=}}</ref> This finding is due to immune complex deposition along the [[glomerular basement membrane]] leading to a typical granular appearance in [[immunofluorescence]] testing.
| |
| | |
| ;Neurological manifestations: About 10% of patients may present with [[seizure]]s or [[psychosis]]. A third may test positive for abnormalities in the [[cerebrospinal fluid]].
| |
| | |
| ;T-cell abnormalities: Abnormalities in [[T cell]] signaling are associated with SLE, including deficiency in [[CD45]] [[phosphatase]] and increased expression of CD40 ligand.
| |
| | |
| ;Other rarer manifestations: [[gastroenteritis|lupus gastroenteritis]], [[pancreatitis|lupus pancreatitis]], [[cystitis|lupus cystitis]], [[autoimmune]] [[Otitis interna|inner ear disease]], [[parasympathetic|parasympathetic dysfunction]], [[vasculitis|retinal vasculitis]], and [[vasculitis|systemic vasculitis]].
| |
| | |
| Other abnormalities include:
| |
| *Increased expression of [[FcεRI]]γ, which replaces the sometimes deficient TCR ζ chain
| |
| *Increased and sustained calcium levels in [[T cell]]s
| |
| *Moderate increase of [[inositol triphosphate]]
| |
| *Reduction in [[Protein kinase C|PKC]] phosphorylation
| |
| *Increased desire of animal protein intake.
| |
| *Reduction in Ras-[[Mitogen-activated protein kinase|MAP kinase]] signaling
| |
| *Deficiencies in [[protein kinase]] A I activity
| |
| | |
| ==Diagnosis==
| |
| | |
| [[Antinuclear antibody]] (ANA) testing and anti-extractable nuclear antigen (anti-ENA) form the mainstay of [[Serology|serologic]] testing for SLE.Several techniques are used to detect ANAs.Clinically the most widely used method is indirect [[immunofluorescence]].The pattern of fluorescence suggests the type of antibody present in the patient's serum.
| |
| | |
| ANA screening yields positive results in many connective tissue disorders and other autoimmune diseases, and may occur in normal individuals. Subtypes of antinuclear antibodies include [[LSm|anti-Smith]] and anti-double stranded [[DNA]] (dsDNA) antibodies (which are linked to SLE) and anti-[[histone]] antibodies (which are linked to drug-induced lupus). Anti-dsDNA antibodies are highly specific for SLE; they are present in 70% of cases, whereas they appear in only 0.5% of people without SLE.<ref name="rahman"/> The anti-dsDNA antibody [[titer]]s also tend to reflect disease activity, although not in all cases.<ref name="rahman"/> Other ANA that may occur in SLE sufferers are [[U1 spliceosomal RNA|anti-U1 RNP]] (which also appears in [[systemic sclerosis]]), SS-A (or anti-Ro) and SS-B (or anti-La; both of which are more common in [[Sjögren's syndrome]]). SS-A and SS-B confer a specific risk for heart conduction block in neonatal lupus.<ref name="pmid14671725">{{cite journal |author=Buyon JP, Clancy RM |title=Maternal autoantibodies and congenital heart block: mediators, markers, and therapeutic approach |journal=Semin. Arthritis Rheum. |volume=33 |issue=3 |pages=140–54 |year=2003 |month=December |pmid=14671725 |doi= |url=http://linkinghub.elsevier.com/retrieve/pii/S0049017203001598}}</ref>
| |
| | |
| Other tests routinely performed in suspected SLE are [[complement system]] levels (low levels suggest consumption by the immune system), [[electrolyte]]s and [[renal function]] (disturbed if the kidney is involved), [[Liver function test|liver enzyme]]s, [[complete blood count]] and recently By [[proteomics]], we can directly detect [[proteins]] as [[gene]] products as well as their alterations by [[post-translational modification]] and internal abscission which are characteristically observed in proteins.<ref name="pmid19252377">{{cite journal |author=Iizuka N, Okamoto K, Hirohata S, Kato T |title=[Analysis of autoantigens in patients with systemic lupus erythematosus by using proteomic approach] |language=Japanese |journal=Nihon Rinsho Meneki Gakkai Kaishi |volume=32 |issue=1 |pages=43–7 |year=2009 |month=February |pmid=19252377 |doi= |url=http://joi.jlc.jst.go.jp/JST.JSTAGE/jsci/32.43?from=PubMed |issn=}}</ref> | |
| | |
| Previously, the lupus erythematosus (LE) cell test was not commonly used for diagnosis because those LE cells are only found in 50–75% of SLE cases, and are also found in some people with rheumatoid arthritis, scleroderma, and drug sensitivities. Because of this, the LE cell test is now performed only rarely and is mostly of historical significance.<ref>[http://www.nlm.nih.gov/medlineplus/ency/article/003635.htm NIM encyclopedic article on the LE cell test]</ref>
| |
| | |
| As a summary:
| |
| | |
| *Medical history
| |
| *Complete physical examination
| |
| *Laboratory tests:
| |
| :*Complete blood count (CBC)
| |
| :*Erythrocyte sedimentation rate (ESR)
| |
| :*Urinalysis
| |
| :*Blood chemistries
| |
| :*Complement levels
| |
| :*Antinuclear antibody test (ANA)
| |
| :*Other autoantibody tests (anti-DNA, anti-Sm, anti-RNP, anti-Ro [SSA], anti-La [SSB])
| |
| :*Anticardiolipin antibody test
| |
| *Skin biopsy
| |
| *Kidney biopsy
| |
| | |
| ===Diagnostic criteria===
| |
| | |
| Some physicians make a diagnosis on the basis of the ACR classification criteria (see below). The criteria, however, were established mainly for use in scientific research (i.e. inclusion in [[randomized controlled trial]]s), and patients may have lupus but never meet the full criteria.
| |
| | |
| [[Anti-nuclear antibody]] testing and anti-''extractable nuclear antigen'' (anti-ENA) form the mainstay of [[Serology|serologic]] testing for lupus. Antiphospholipid antibodies occur more often in SLE, and can predispose for [[thrombosis]]. More specific are the [[LSm#History|anti-smith]] and anti-dsDNA antibodies. Other tests routinely performed in suspected SLE are [[complement system]] levels (low levels suggest consumption by the immune system), [[electrolyte]]s and [[renal function]] (disturbed if the kidney is involved), [[Liver function test|liver enzyme]]s and a [[complete blood count]].
| |
| | |
| Formerly, the lupus erythematosus (LE) cell test was used for diagnosis, however those LE cells are only found in 50-75% of SLE patients, and are also found in some patients with rheumatoid arthritis, scleroderma, and drug sensitivities. Because of this, the LE cell test is now performed only rarely and is mostly of historical significance. <ref>[http://www.nlm.nih.gov/medlineplus/ency/article/003635.htm NIM encyclopedic article on the LE cell test]</ref>
| |
| | |
| The American College of Rheumatology (ACR) has established eleven criteria in 1982,<ref>[http://www.rheumatology.org/publications/classification/index.asp?aud=mem Rheumatology.org article on the classification of rheumatic diseases]</ref> which were revised in 1997<ref>[http://www.rheumatology.org/publications/classification/SLE/1982SLEupdate.asp?aud=mem Revision of Rheumatology.org's diagnostic criteria]</ref> as a classificatory instrument to operationalise the definition of SLE in clinical trials. They were not intended to be used to diagnose individual patients and do not do well in that capacity.
| |
| | |
| For inclusion in clinical trials, patients must meet the following three criteria to be classified as having SLE:
| |
| | |
| *(i) patient must present with four of the below eleven symptoms
| |
| | |
| *(ii) either simultaneously or serially
| |
| | |
| *(iii) during a ''given period of observation''.
| |
| | |
| # [[Malar rash]] (rash on cheeks). [[sensitivity (tests)|sensitivity]] = 57%; [[specificity (tests)|specificity]] = 96%<ref name="pmid3060613"/>
| |
| # Discoid lupus (red, scaly patches on skin which cause scarring) [[sensitivity (tests)|sensitivity]] = 18%; [[specificity (tests)|specificity]] = 99%<ref name="pmid3060613"/>
| |
| # [[Photodermatitis|Photosensitivity]] (exposure to ultraviolet light causes rash). [[sensitivity (tests)|sensitivity]] = 43%; [[specificity (tests)|specificity]] = 96%<ref name="pmid3060613"/>
| |
| # Oral ulcers: include oral or nasopharyngeal ulcers
| |
| # [[Arthritis]]: nonerosive arthritis of two or more peripheral joints, with tenderness, swelling or effusion[[sensitivity (tests)|sensitivity]] = 86%; [[specificity (tests)|specificity]] = 37%<ref name="pmid3060613"/>
| |
| # Renal disorder: More than 0.5 g per day [[Proteinuria|protein in urine]], or cellular [[Urinary casts|casts]] seen in urine under a microscope.[[sensitivity (tests)|sensitivity]] = 51%; [[specificity (tests)|specificity]] = 94%<ref name="pmid3060613"/>
| |
| # Neurologic disorder: [[Seizure]]s or [[psychosis]]. [[sensitivity (tests)|sensitivity]] = 20%; [[specificity (tests)|specificity]] = 98%<ref name="pmid3060613"/>
| |
| # Serositis: [[Pleurisy|Pleuritis]] (inflammation of the membrane around the lungs) or [[pericarditis]] (inflammation of the membrane around the heart)[[sensitivity (tests)|sensitivity]] = 56%; [[specificity (tests)|specificity]] = 86% (pleural is more sensitive; cardiac is more specific)<ref name="pmid3060613"/>
| |
| # Hematologic disorder: [[Hemolytic anemia]] (low [[red blood cell]] count) or [[leukopenia]] (white blood cell count<4000/ul), [[lymphopenia]] ( <1500/ul ) or [[thrombocytopenia]] (<100000/uL) in the absence of offending drug.[[sensitivity (tests)|sensitivity]] = 59%; [[specificity (tests)|specificity]] = 89%<ref name="pmid3060613"/> Hypocomplementemia is also seen, due to either consumption of C3 and C4 by immune complex-induced inflammation, or to congenitally complement deficiency, which may predispose to SLE.
| |
| # [[Anti-nuclear antibody]] test positive. [[sensitivity (tests)|sensitivity]] = 99%; [[specificity (tests)|specificity]] = 49%<ref name="pmid3060613"/>
| |
| # Immunologic disorder: Positive [[LSm#History|anti-Sm]], anti-ds DNA, [[Antiphospholipid syndrome|anti-phospholipid antibody]] and/or false positive [[serology|serological]] test for [[syphilis]]. [[sensitivity (tests)|sensitivity]] = 85%; [[specificity (tests)|specificity]] = 93%<ref name="pmid3060613"/>. Presence of anti-ss DNA in 70% of patients (though also positive in patients with rheumatic disease and healthy persons<ref>[http://patients.uptodate.com/topic.asp?file=dx_rheum/18305 UpToDate Patient information article on DNA antibodies]</ref>)
| |
| | |
| ===A useful mnemonic for these 11 criteria is ''SOAP BRAIN MD''===
| |
| | |
| *'''S'''erositis
| |
| *'''O'''ral ulcers
| |
| *'''A'''rthritis
| |
| *'''P'''hotosensitivity
| |
| *'''B'''lood Changes
| |
| *'''R'''enal involvement (proteinuria or casts)
| |
| *'''A'''NA
| |
| *'''I'''mmunological changes
| |
| *'''N'''eurological signs (seizures, frank psychosis)
| |
| *'''M'''alar Rash
| |
| *'''D'''iscoid Rash
| |
| | |
| Some patients, especially those with [[antiphospholipid syndrome]], may have SLE without four criteria and SLE is associated with manifestations other than those listed in the criteria.<ref name="pmid12892393">{{cite journal |author=Asherson RA, Cervera R, de Groot PG, ''et al'' |title=Catastrophic antiphospholipid syndrome: international consensus statement on classification criteria and treatment guidelines |journal=Lupus |volume=12 |issue=7 |pages=530-4 |year=2003 |pmid=12892393 |doi=}}</ref><ref name="pmid15608315">{{cite journal |author=Sangle S, D'Cruz DP, Hughes GR |title=Livedo reticularis and pregnancy morbidity in patients negative for antiphospholipid antibodies |journal=Ann. Rheum. Dis. |volume=64 |issue=1 |pages=147-8 |year=2005 |pmid=15608315 |doi=10.1136/ard.2004.020743}}</ref><ref name="pmid14644846">{{cite journal |author=Hughes GR, Khamashta MA |title=Seronegative antiphospholipid syndrome |journal=Ann. Rheum. Dis. |volume=62 |issue=12 |pages=1127 |year=2003 |pmid=14644846 |doi=}}</ref>
| |
| | |
| ===Alternative criteria===
| |
| [[Recursive partitioning]] has been used to identify more parsimonious criteria. <ref name="pmid3060613">{{cite journal |author=Edworthy SM, Zatarain E, McShane DJ, Bloch DA |title=Analysis of the 1982 ARA lupus criteria data set by recursive partitioning methodology: new insights into the relative merit of individual criteria |journal=J. Rheumatol. |volume=15 |issue=10 |pages=1493-8 |year=1988 |pmid=3060613 |doi=}}</ref> This analysis presented two diagnostic classification trees:
| |
| | |
| 1. Simplest classification tree:
| |
| LSE is diagnosed if the patient has an immunologic disorder (anti-DNA antibody, anti-Smith antibody, false positive syphilis test, or LE cells) or [[malar rash]].
| |
| * [[sensitivity (tests)|sensitivity]] = 92%
| |
| * [[specificity (tests)|specificity]] = 92%
| |
| 2. Full classification tree:
| |
| Uses 6 criteria.
| |
| * [[sensitivity (tests)|sensitivity]] = 97%
| |
| * [[specificity (tests)|specificity]] = 95%
| |
| | |
| Other alternative criteria have been suggested.<ref name="pmid9631744">{{cite journal |author=Hughes GR |title=Is it lupus? The St. Thomas' Hospital "alternative" criteria |journal=Clin. Exp. Rheumatol. |volume=16 |issue=3 |pages=250-2 |year=1998 |pmid=9631744 |doi=}}</ref> | |
| | |
| ==Common misdiagnoses==
| |
| ===Porphyria===
| |
| [[Porphyria]]s are complex genetic disorders that share many symptoms with lupus, but impact the enzymes responsible for building [[heme]], a component needed in heme proteins. Porphyrias are ecogenic disorders requiring both environmental and genetic backgrounds to manifest with a variety of symptoms and medical complications. They are noted for photosensitivity and have been associated with transient and permanent production of autoantibodies. The five major forms of dominantly inherited porphyrias (acute intermittent porphyria, porphyria cutanea tarda, hereditary coproporphyria, variegate porphyria and erythropoietic protoporphyria) have been detected in systemic lupus erythematosus and discoid lupus patients over the past 50 years. Physicians should have a high degree of suspicion of porphyrias in all lupus cases and act accordingly when patients are in a medical crisis that may be due to an underlying acute hepatic porphyria. Drug-induced lupus and photosensitivity warrant an investigation for an underlying porphyria since multiple drug reactions are a hallmark complication of porphyrias. Patients with both lupus and porphyrias should avoid porphyrinogenic drugs and hormone preparations.
| |
| | |
| Patients with acute hepatic porphyrias (acute intermittent porphyria, hereditary coproporphyria, variegate porphyria) have been detected in lupus patients with severe life-threatening "lupus" complications known as neurolupus. Symptoms are identical to acute hepatic porphyria attacks and include seizures, psychosis, peripheral neuropathy and syndrome of inappropriate antidiuretic hormone (SIADH) associated with dangerously low sodium levels (hyponatremia). Porphyria attacks require intervention with intravenous glucose, heme preparations and the discontinuation of dangerous porphyrinogenic drugs including antiseizure drugs. Several other lupus complications have been associated with porphyrias including pancreatitis and pericarditis. Porphyrin testing should be performed on urine, stool/bile and blood to detect all types of porphyrias, and repeat testing should be performed in suspicious cases. Appropriate enzyme tests or DNA testing should also be pursued to obtain a complete diagnosis which could include a dual porphyria.
| |
| | |
| ==Common dual diagnoses==
| |
| | |
| SLE is sometimes diagnosed in conjunction with other conditions, including [[Rheumatoid arthritis|Rheumatoid Arthritis]], [[Scurvy]] and [[Fibromyalgia]].
| |
|
| |
|
| ==Treatment== | | ==Treatment== |
| | [[Systemic lupus erythematosus medical therapy|Medical Therapy]] | [[Systemic lupus erythematosus surgery |Surgery]] | [[Systemic lupus erythematosus primary prevention|Primary Prevention]] | [[Systemic lupus erythematosus secondary prevention|Secondary Prevention]] | [[Systemic lupus erythematosus cost-effectiveness of therapy|Cost-Effectiveness of Therapy]] | [[Systemic lupus erythematosus future or investigational therapies|Future or Investigational Therapies]] |
|
| |
|
| As lupus erythematosus is a chronic disease with no known cure, treatment is restricted to dealing with the [[Symptomatic treatment|symptoms]]; essentially this involves preventing flares and reducing their severity and duration when they occur. There are several means of preventing and dealing with flares, including drugs, alternative medicine and lifestyle changes.
| | ==Case Studies== |
| | | [[Systemic lupus erythematosus case study one|Case #1]] |
| ===Drug therapy===
| |
| | |
| Due to the variety of symptoms and organ system involvement with Lupus patients, the severity of the SLE in a particular patient must be assessed in order to successfully treat SLE. Mild or remittent disease can sometimes be safely left untreated. If required, [[non-steroidal anti-inflammatory drug]] and anti-malarials may be used.<ref> [http://www.merck.com/mmpe/sec04/ch032/ch032g.html#sec04-ch032-ch032g-205 Merck manual discussion of Lupus] </ref>
| |
| | |
| [[Disease-modifying antirheumatic drug]]s (DMARDs) are used preventively to reduce incidence of flares, the process of the disease, and lower the need for steroid use; when flares occur, they are treated with corticosteroids. DMARDs commonly in use are anti-malarials and immunosupressants (e.g. [[methotrexate]] and [[azathioprine]]). [[Hydroxychloroquine]] (trade name Plaquenil) is an FDA approved anti-malarial used for constitutional, cutaneous, and articular manifestations, while [[Cyclophosphamide]] (trade names Cytoxan and Neosar) is used for severe glomerulonephritis or other organ-damaging complications, and in 2005, [[mycophenolic acid|CellCept]] became accepted for treatment of [[lupus nephritis]].
| |
| | |
| In more severe cases, medications that modulate the [[immune system]] (primarily [[corticosteroid]]s and [[Immunosuppresive drug|immunosuppressant]]s) are used to control the disease and prevent re-occurrence of symptoms (known as flares<ref name=niams/>). Patients who require steroids frequently may develop [[obesity]], [[diabetes mellitus|diabetes]] and [[osteoporosis]]. Depending on the dosage, corticosteroids can cause other side effects such as a puffy face, an unusually large appetite and difficulty sleeping. Those side effects can subside if and when the large initial dosage is reduced, but long term use of even low doses can cause elevated blood pressure and cataracts. Due to these side effects, steroids are avoided if possible.
| |
| | |
| Since a large percentage of Lupus patients suffer from varying amounts of chronic pain, stronger prescription analgesics may be used if over-the-counter drugs, mainly [[non-steroidal anti-inflammatory drug]] do not provide effective relief. Moderate pain in Lupus patients if typically treated with mild prescription opiates such as Dextropropoxyphene (trade name Darvocet), and Co-codamol (trade name Tylenol #3). Moderate to severe chronic pain is treated with stronger opioids such as Hydrocodone (trade names Lorcet, Lortab, Norco, Vicodin, Vicoprofen) or longer-acting continuous release opioids such as Oxycodone (trade names OxyContin), MS Contin, or Methadone. The Fentanyl Duragesic Transdermal patch is also a widely-used treatment option for chronic pain due to Lupus complications because of its long-acting timed release and easy usage. When opioids are used for prolonged periods drug tolerance, chemical dependency and (rarely) addiction may occur. Opiate addiction is not typically a concern for Lupus patients, since the condition is not likely to ever completely disappear. Thus, lifelong treatment with opioids is fairly common in Lupus patients that exhibit chronic pain symptoms; accompanied by periodic increased titration that is typical of any long-term opioid regimen.
| |
| | |
| ===Acupuncture===
| |
| | |
| A 1985 study on lupus and acupuncture reported improvement of lupus sufferers over matched controls, though there was no placebo group for comparison.<ref>[http://www.tldp.com/lupus/lupus_%20review.htm Review of different alternative treatments for lupus]</ref> It is possible that acupuncture may be useful for the treatment some of the ''symptoms'' of lupus, but there needs to be more research done before a definitive statement can be made regarding acupuncture. <ref>[http://www.hss.edu/Conditions/Systemic-Lupus-Erythematosus-(SLE)/Acupuncture-For-SLE Hospital for Special Surgery article on acupuncture and lupus]</ref>
| |
| | |
| ===UVA1 Phototherapy===
| |
| | |
| In 1987, Tina Lomardi, MD first reported that long-wave ultraviolet radiation (UVA1) had a favorable effect on disease activity in SLE model mice. Several clinicals trials investigating this new, counter-intuitive therapeutic approach, conducted by both McGrath and independent Dutch searchers, have confirmed these findings in SLE patients. <ref> {{cite web |url=http://rheumatology.oxfordjournals.org/cgi/content/full/45/6/653 |title=Light therapy (with UVA-1) for SLE patients: is it a good or bad idea? -- Pavel 45 (6): 653 -- Rheumatology |accessdate=2007-07-04 |format= |work=}}</ref> Devices for administering therapeutic doses of UVA1 are available in Europe but not in the U.S. However, the U.S. Food and Drug Administration Office of Science and Technology conducted UVA1 phototherapy studies in an SLE mouse model in 1997 “to prepare for future reviews of UVA-emitting tanning devices for such clinical applications." [http://www.fda.gov/cdrh/ost/rpt97/OST1997AR19.html]
| |
| | |
| ===Lifestyle changes===
| |
| | |
| Other measures such as avoiding sunlight or covering up with sun protective clothing can also be effective in preventing problems due to photosensitivity. Weight loss is also recommended in overweight and obese patients to alleviate some of the effects of the disease, especially where joint involvement is significant.
| |
| | |
| ===Renal transplantation===
| |
| | |
| is the treatment of choice for [[end-stage renal disease]], which is one of the complications of [[lupus nephritis]], but the recurrence of the full disease is common in up to 30% of patients.<ref name="pmid19247694">{{cite journal |author=Cochat P, Fargue S, Mestrallet G, ''et al'' |title=Disease recurrence in paediatric renal transplantation |journal=Pediatr. Nephrol. |volume= |issue= |pages= |year=2009 |month=February |pmid=19247694 |doi=10.1007/s00467-009-1137-6 |url=http://dx.doi.org/10.1007/s00467-009-1137-6 |issn=}}</ref>
| |
| | |
| ===Treatment Research===
| |
| | |
| Other immunosuppressants and [[bone marrow transplant|autologous stem cell transplants]] are under investigation as a possible cure. Recently, treatments that are more specific in modifying the particular subset of the immune cells (e.g. B- or T- cells) or [[cytokine]] proteins they secrete have been gaining attention. Research into new treatments has recently been accelerated by genetic discoveries, especially mapping of the [[human genome]]. According to a June 2006 market analysis report by Datamonitor, treatment for SLE could be on the verge of a breakthrough as there are numerous late-Phase trials currently being carried out.<ref>[http://www.leaddiscovery.co.uk/reports/pharmaceutical_reports/Systemic_Lupus_Erythematosus-On_the_Verge_of_a_Breakthough.html Lead Discovery article on treatment of Lupus]</ref>
| |
| | |
| ==Prevention==
| |
| | |
| Lupus is not understood well enough to be prevented, but when the disease develops, quality of life can be improved through flare prevention. The warning signs of an impending flare include increased fatigue, pain, rash, fever, abdominal discomfort, headache and dizziness. Early recognition of warning signs and good communication with a doctor can help individuals with lupus remain active, experience less pain and reduce medical visits.<ref name=niams/>
| |
| | |
| ===Prevention of complications during pregnancy===
| |
| | |
| While most infants born to mothers who have SLE are healthy, pregnant mothers with SLE should remain under a doctor's care until delivery. Neonatal lupus is rare, but identification of mothers at highest risk for complications allows for prompt treatment before or after birth. In addition, SLE can flare during pregnancy, and proper treatment can maintain the health of the mother longer. Women pregnant and known to have the antibodies for anti-Ro (SSA) or anti-La (SSB) should have echocardiograms during the 16th and 30th weeks of pregnancy to monitor the health of the heart and surrounding vasculature.<ref name=niams/>
| |
| | |
| Even [[contraception]] was routinely advised in treating SLE patients, getting pregnant during active disease was eventually found. [[Lupus nephritis]] was the most common manifestation. Overall live-birth was 72.7%. Pregnancy lost was due to [[abortion]] and dead fetus in utero. Pregnancy outcome was worse in SLE patients who had disease flares up or emerging during pregnancy.<ref name="pmid19253790">{{cite journal |author=Foocharoen C, Nanagara R, Salang L, Suwannaroj S, Mahakkanukrauh A |title=Pregnancy and disease outcome in patients with systemic lupus erythematosus (SLE): a study at Srinagarind Hospital |journal=J Med Assoc Thai |volume=92 |issue=2 |pages=167–74 |year=2009 |month=February |pmid=19253790 |doi= |url= |issn=}}</ref>
| |
| | |
| ==Prognosis==
| |
| | |
| In the 1950s, most people diagnosed with SLE lived fewer than five years. Advances in diagnosis and treatment have improved survival to the point where over 90% now survive for more than ten years, and many can live relatively asymptomatically. Prognosis is normally worse for men and children than for women; however, if symptoms are present after age 60, the disease tends to run a more benign course. Early mortality, within 5 years, is due to organ failure or overwhelming infections, both of which can be modified by early diagnosis and treatment. The mortality risk is five-fold when compared to the normal population in the late stages, which can be attributed to cardiovascular diseases acquired from corticosteroid therapy. To reduce potential for cardiovascular issues, steroids should be used at the lowest dose for the shortest possible period. High serum creatinine, hypertension, [[nephrotic syndrome]], anemia and hypoalbuminemia are poor prognostic factors.<ref name="prognosis">[http://medicalpresentations.lifehugger.com/doc/sle-systemic-lupus-erythematosus Poor prognostic factors,Sudheer, SLE document]</ref>
| |
| | |
| The ANA is the most sensitive screening test for evaluation, whereas [[LSm#History|anti-Sm (anti-Smith)]] is the most specific. The dsDNA (double-stranded [[DNA]]) antibody is also fairly specific and often fluctuates with disease activity; as such, the dsDNA titer is sometimes useful to monitor disease flares or response to treatment.<ref>[Early steroids may prevent relapses in lupus, P Jarman (Published in Journal Watch (General) July 18, 1995)</ref>
| |
|
| |
|
| ==Lupus and Quality of Life== | | ==Related Chapters== |
| | |
| Despite the symptoms of lupus and the potential side-effects of treatment, people with lupus can maintain a high quality of life overall. One key to managing lupus is to understand the disease and its impact. Learning to recognize the warning signs of a flare can help the patient take steps to ward it off or reduce its intensity. Many people with lupus experience increased fatigue, pain, a rash, fever, abdominal discomfort, headache, or dizziness just before a flare. Developing strategies to prevent flares can also be helpful, such as learning to recognize your warning signals and maintaining good communication with your doctor.
| |
| | |
| It is also important for people with lupus to receive regular health care, instead of seeking help only when symptoms worsen. Results from a medical exam and laboratory work on a regular basis allows the doctor to note any changes and to identify and treat flares early. The treatment plan, which is tailored to the individual's specific needs and circumstances, can be adjusted accordingly. If new symptoms are identified early, treatments may be more effective. Other concerns also can be addressed at regular checkups. The doctor can provide guidance about such issues as the use of sunscreens, stress reduction, and the importance of structured exercise and rest, as well as birth control and family planning. Because people with lupus can be more susceptible to infections, the doctor may recommend yearly influenza vaccinations or pneumococcal vaccinations for some patients.
| |
| | |
| Women with lupus should receive regular preventive health care, such as gynecological and breast examinations. Men with lupus should have the prostate-specific antigen (PSA) test. Both men and women need to have their blood pressure and cholesterol checked on a regular basis. If a person is taking corticosteroids or antimalarial medications, an eye exam should be done at least yearly to screen for and treat eye problems.
| |
| | |
| Staying healthy requires extra effort and care for people with lupus, so it becomes especially important to develop strategies for maintaining wellness. Wellness involves close attention to the body, mind, and spirit. One of the primary goals of wellness for people with lupus is coping with the stress of having a chronic disorder. Effective stress management varies from person to person. Some approaches that may help include exercise, relaxation techniques such as meditation, and setting priorities for spending time and energy.
| |
| | |
| Developing and maintaining a good support system is also important. A support system may include family, friends, medical professionals, community organizations, and support groups. Participating in a support group can provide emotional help, boost self-esteem and morale, and help develop or improve coping skills.
| |
| | |
| ===Warning Signs of a Flare===
| |
| | |
| * Increased [[fatigue]]
| |
| * [[Pain]]
| |
| * [[Rash]]
| |
| * [[Fever]]
| |
| * [[Abdominal discomfort]]
| |
| * [[Headache]]
| |
| * [[Dizziness]]
| |
| | |
| ==Histopathological Findings==
| |
| | |
| [http://www.peir.net Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology]
| |
| | |
| <gallery perRow="3">
| |
| Image:Systemic lupus erythematosus 001.jpg|Kidney: Lupus erythematosus: Gross, enlarged very pale kidneys with flea bite or ectasia. A good example of kidneys from a patient with nephrotic syndrome (subacute glomerulonephritis)
| |
| Image:Systemic lupus erythematosus 002.jpg|Kidney: Lupus erythematosus: Gross cut surface pale kidneys typical of nephrotic syndrome (subacute glomerulonephritis)
| |
| Image:Systemic lupus erythematosus 003.jpg|Lupus erythematosus hepatitis: Micro high mag H&E, periportal sinus thrombosis with liver cell necrosis and noninflammatory infiltrate (possibly viral). A 19yo female with lupus erythematosus
| |
| Image:Systemic lupus erythematosus 004.jpg|Lupus Erythematosus Hepatitis: Gross natural color. A 19yo female with lupus erythematosus and hepatitis characterized by periportal cell necrosis and sinus thrombosis cause uncertain photo shows focal grid-like hyperemia
| |
| Image:Systemic lupus erythematosus 005.jpg|Spleen: Lupus erythematosus Periarterial Fibrosis: Micro high may H&E. An excellent example of periarterial fibrosis
| |
| Image:Systemic lupus erythematosus 006.jpg|Spleen: Lupus erythematosus, periarterial fibrosis: Micro high may H&E. An excellent example of periarterial fibrosis
| |
| Image:Systemic lupus erythematosus 007.jpg|Spleen: Lupus erythematosus. Basophilic bodies and periarterial fibrosis: Micro high mag, H&E. Two basophilic bodies and periarterial fibrosis. An excellent example of this rarely seen lupus lesion.
| |
| Image:Systemic lupus erythematosus 008.jpg|Lupus Erythematosus, Libman Sacks Endocarditis: Micro low mag trichrome stain thickened valve leaflet with small mural fibrin deposit. A 19yo female with cerebral lupus in form of TIAs due to this lesion.
| |
| Image:Systemic lupus erythematosus 009.jpg|Lupus Erythematosus, Libman Sacks Endocarditis: Micro low mag, elastic van Gieson stain, mitral valve thickened, leaflet with small mural fibrin deposit that caused TIAs in 19yo female
| |
| Image:Systemic lupus erythematosus 010.jpg|Adrenal: Autoimmune Adrenalitis: Micro high mag H&E focal area of lymphocytic infiltration in zona reticularis in a 19yo female with lupus erythematosus
| |
| Image:Systemic lupus erythematosus 011.jpg|Kidney: Lupus Erythematosus: Micro high mag H&E two glomeruli showing mesangial thickening and focal wire loop type lesions 19yo female with renal failure and embolic brain disease from Libman Sacks lesion on mitral valve
| |
| Image:Systemic lupus erythematosus 012.jpg|Lupus Erythematosus Myocardial Necrosis Due To Libman Sacks: Micro low mag H&E focal myocardial necrosis due to embolism from Libman Sacks lesion on mitral valve 19yo female with TIAs due to mitral lesion
| |
| Image:Systemic lupus erythematosus 013.jpg|Lupus Erythematosus Focal Myocardial Scar Due To Libman Sacks Embolism: Micro low mag H&E focal scar in myocardium due to embolism
| |
| Image:Systemic lupus erythematosus 014.jpg|Lupus Erythematosus Myocardial Scar Due To Libman Sacks Embolism: Micro low mag H&E scar with portion of embolus in small artery
| |
| Image:Systemic lupus erythematosus 015.jpg|Lupus Erythematosus Myocardial Necrosis Due To Libman Sacks: Micro low mag H&E well shown focal myocardial necrosis due to embolism from mitral Libman Sacks lesion
| |
| Image:Systemic lupus erythematosus 016.jpg|Lupus Erythematosus Embolus From Libman Sacks Lesion: Micro med mag H&E well shown embolus in small artery
| |
| Image:Systemic lupus erythematosus 017.jpg|Lupus Erythematosus Hepatitis: Micro low mag trichrome stain periportal liver cell necrosis and sinus thrombosis with no inflammatory reaction cause unknown 19yo female with lupus erythematosus
| |
| Image:Systemic lupus erythematosus 018.jpg|Lung: Diffuse Alveolar Damage: Gross natural color section of both lungs with frank meaty appearance case of lupus erythematosus in 19yo female
| |
| Image:Systemic lupus erythematosus 019.jpg|Kidney: Lupus Erythematosus: Micro high mag H&E increased mesangial tissue and wire loops 10yo female with renal failure and TIAs due to Libman Sacks endocarditis
| |
| Image:Systemic lupus erythematosus 020.jpg|Lung: Necrotizing Bronchiolitis: Micro low mag H&E well shown lesion in lung that grossly looked like diffuse alveolar damage which indeed has lesions of this type additionally 19yo female with lupus erythematosus
| |
| Image:Systemic lupus erythematosus 021.jpg|Lupus Erythematosus Libman Sacks Endocarditis: Gross natural color mitral valve small lesions but cause much trouble in form of TIAs and terminally multiple hemorrhagic brain infarcts
| |
| Image:Systemic lupus erythematosus 022.jpg|Lupus Erythematosus Libman Sacks Endocarditis: Micro high mag H&E atrial surface of mitral valve with small fibrin thrombus representing Libman Sacks lesion 10yo female
| |
| Image:Systemic lupus erythematosus 023.jpg|Lupus Erythematosus Libman Sacks Endocarditis: Micro low mag H&E mitral valve lesion with easily seen mural thrombi and focal necrobiosis of collagen in thickened valve leaflet 19yo female
| |
| Image:Systemic lupus erythematosus 024.jpg|Lung: Necrotizing Bronchiolitis: Micro low mag H&E well shown necrotizing bronchiolitis and surrounding lesions of diffuse alveolar damage 19yo female with lupus erythematosus
| |
| Image:Systemic lupus erythematosus 025.jpg|Myocarditis: Micro high mag H&E focal myofiber necrosis typical for this diagnosis but this is case of lupus erythematosus with Libman Sacks lesion and brain emboli and heart emboli did she also have viral myocarditis? This lesion is typical for the diagnosis
| |
| Image:Systemic lupus erythematosus 026.jpg|Kidney: Lupus Erythematosus: Micro high mag PAS stain thickened mesangium and capillary basement membranes 19yo female with renal failure and proved lupus
| |
| Image:Systemic lupus erythematosus 027.jpg|Brain: Lupus Erythematosus Libman Sacks Embolism: Gross fixed tissue one large and two small hemorrhages 19yo female with history of TIAs
| |
| Image:Systemic lupus erythematosus 028.jpg|Brain: Lupus Erythematosus Libman Sacks Embolism: Gross fixed tissue large hemorrhagic infarcts due to embolism 19yo female with known lupus and history of TIAs
| |
| Image:Systemic lupus erythematosus 029.jpg|Brain: Lupus Erythematosus Libman Sacks Embolism: Gross large hemorrhagic infarcts 19 yo female with history of TIAs proved case lupus with renal failure
| |
| Image:Systemic lupus erythematosus 030.jpg|Brain: Lupus Erythematosus Libman Sacks Embolism: Gross fixed tissue cerebellar hemorrhagic infarcts 19yo female with history of TIAs known lupus case with renal failure
| |
| Image:Systemic lupus erythematosus 031.jpg|Brain: Purulent Meningitis: Gross fixed tissue excellent example Pneumococcus case of young girl with lupus
| |
| Image:Systemic lupus erythematosus 032.jpg|Skeletal muscle: Hematoma: Gross natural color flank muscle hematoma old showing typical chocolate appearance of blood coagulum young female with lupus and thrombocytopenia
| |
| Image:Systemic lupus erythematosus 033.jpg|Artery: Arteritis in Lupus Erythematosus: Micro med mag H&E. A good example of vasculitis
| |
| Image:Systemic lupus erythematosus 034.jpg|Kidney: Lupus Erythematosus: Micro high mag PASH typical glomerulonephritis lesion with crescent
| |
| Image:Systemic lupus erythematosus 035.jpg|Kidney: Lupus Erythematosus: Micro med mag PASH glomerulonephritis
| |
| Image:Systemic lupus erythematosus 036.jpg|Kidney: Lupus Erythematosus: Micro med mag H&E typical glomerulonephritis lesion
| |
| Image:Systemic lupus erythematosus 037.jpg|Kidney: Lupus Erythematosus: Micro med mag H&E two glomeruli showing lobular glomerulonephritis lesion
| |
| Image:Systemic lupus erythematosus 038.jpg|Kidney: Lupus Erythematosus: Micro med mag PASH typical chronic glomerulonephritis lesion with crescent
| |
| Image:Systemic lupus erythematosus 039.jpg|Kidney: Lupus Erythematosus: Micro high mag H&E. A nice example of a lesion of chronic glomerulonephritis with lobular scarring. A fibrous type crescent.
| |
| Image:Systemic lupus erythematosus 040.jpg|Kidney: Lupus Nephritis: Gross natural color external view of flea bitten kidneys quite good advanced proliferative type glomerulonephritis of lupus in a 16yo female
| |
| Image:Systemic lupus erythematosus 041.jpg|Brain: Hemorrhage Massive With Lupus Erythematosus: Gross apparently fresh tissue large left frontoparietal hemorrhagic infarct in a 16yo female with advanced lupus nephritis and sepsis
| |
| Image:Systemic lupus erythematosus 042.jpg|Brain: Hemorrhage Massive With Lupus Erythematosus: Gross natural color not the best exposure but OK large left frontoparietal hemorrhage in 16yo female with advanced lupus nephritis and sepsis
| |
| Image:Systemic lupus erythematosus 043.jpg|Brain: Hemorrhage Massive With Lupus Erythematosus: Gross natural color but not best exposure large left frontoparietal hemorrhage in 16yo female with advanced lupus nephritis and sepsis
| |
| Image:Systemic lupus erythematosus 044.jpg|Lung: Tuberculosis Reactivation: Gross fixed tissue close-up of lung hilum with node and parenchyma lesions case of lupus erythematosus treated with prednisone for many years
| |
| Image:Systemic lupus erythematosus 045.jpg|Lung: Tuberculosis Reactivation: Gross fixed tissue close-up of lung showing lesions in nodes and parenchyma case of lupus erythematosus treated for long period with prednisone
| |
| Image:Systemic lupus erythematosus 046.jpg|Kidney: Lupus Erythematosus: Gross natural color nice external and cut surface view of uniformly scarred and moderately shrunken kidneys
| |
| Image:Systemic lupus erythematosus 047.jpg|Brain: Lupus Erythematosus, Systemic; Microinfarct in Cerebral Cortex
| |
| Image:Systemic lupus erythematosus 048.jpg|Vessel: lupus, systemic erythematosus; Thrombus in capillary
| |
| Image:Systemic lupus erythematosus 049.jpg|Vessel: lupus, systemic erythematosus; Thrombus in capillary
| |
| Image:Systemic lupus erythematosus 050.jpg|Vessel: lupus, systemic erythematosus; Thrombus in arteriole and vein
| |
| Image:Systemic lupus erythematosus 051.jpg|Vessel: lupus, systemic erythematosus; Thrombus in pial vessel
| |
| Image:Systemic lupus erythematosus 052.jpg|Skin: Lupus, systemic erythematosus; Discoid skin lesion in patient with SLE
| |
| Image:Systemic lupus erythematosus 053.jpg|Skin: ulcer, necrotic; lupus anticoagulant in thigh
| |
| Image:Systemic lupus erythematosus 054.jpg|Skin: lupus, erythematosus, subacute; Papulosquamous diseases
| |
| Image:Systemic lupus erythematosus 055.jpg|Skin: lupus, erythematosus; Papulosquamous diseases
| |
| Image:Systemic lupus erythematosus 056.jpg|Skin: lupus, erythematosus; papulosquamous diseases
| |
| Image:Systemic lupus erythematosus 057.jpg|Skin: alopecia, secondary lupus erythematosus; hair loss
| |
| Image:Systemic lupus erythematosus 058.jpg|Skin: discoid lupus, face
| |
| </gallery>
| |
| | |
| ==Videos==
| |
| | |
| <youtube v=Tw07BFaDEo0/>
| |
| | |
| ==See also==
| |
| * [[Abzyme]]
| |
| * [[Anti-nuclear antibody]] | | * [[Anti-nuclear antibody]] |
| * [[Discoid lupus erythematosus]] in dogs | | * [[Discoid lupus erythematosus]] |
| * Lupus Canada
| |
| * Lupus Foundation of America
| |
|
| |
|
| ==References==
| |
| {{Reflist|2}}
| |
|
| |
| ==External links==
| |
| *{{DMOZ|Health/Conditions_and_Diseases/Musculoskeletal_Disorders/Connective_Tissue/Lupus/}}
| |
| *[http://www.uklupus.co.uk The Lupus Site]
| |
| *[http://www.lupus.org/ The Lupus Foundation of America]
| |
|
| |
| {{SIB}}
| |
| {{Diseases of the skin and subcutaneous tissue}} | | {{Diseases of the skin and subcutaneous tissue}} |
| {{Diseases of the musculoskeletal system and connective tissue}} | | {{Diseases of the musculoskeletal system and connective tissue}} |
| Line 484: |
Line 60: |
| [[Category:Nephrology]] | | [[Category:Nephrology]] |
| [[Category:Autoimmune diseases]] | | [[Category:Autoimmune diseases]] |
| [[Category:Diseases]] | | [[Category:Disease]] |
| | |
| [[bg:Лупус]]
| |
| [[ca:Lupus eritematós sistèmic]]
| |
| [[da:Systemisk Lupus Erythematosus]]
| |
| [[de:Lupus erythematodes]]
| |
| [[es:Lupus eritematoso sistémico]]
| |
| [[fa:لوپوس منتشر]]
| |
| [[fr:Lupus érythémateux disséminé]]
| |
| [[id:Lupus eritematosus sistemik]]
| |
| [[it:Lupus eritematoso sistemico]]
| |
| [[he:זאבת]]
| |
| [[ms:Lupus eritematosus sistemik]]
| |
| [[nl:Lupus erythematodes]]
| |
| [[ja:全身性エリテマトーデス]]
| |
| [[pl:Toczeń rumieniowaty układowy]]
| |
| [[pt:Lupus eritematoso sistêmico]]
| |
| [[ru:Системная красная волчанка]]
| |
| [[simple:Lupus erythematosus]]
| |
| [[fi:Sle]]
| |
| [[sv:Systemisk lupus erythematosus]]
| |
| [[th:โรคลูปัส]]
| |
| [[tr:Sistemik lupus eritematozus]]
| |
| [[zh:紅斑性狼瘡]]
| |
|
| |
|
| {{WikiDoc Help Menu}} | | {{WikiDoc Help Menu}} |
| {{WikiDoc Sources}} | | {{WikiDoc Sources}} |