Hyperpigmentation
| Hyperpigmentation | |
| DiseasesDB | 24638 |
|---|---|
| MeSH | D017495 |
|
WikiDoc Resources for Hyperpigmentation |
|
Articles |
|---|
|
Most recent articles on Hyperpigmentation Most cited articles on Hyperpigmentation |
|
Media |
|
Powerpoint slides on Hyperpigmentation |
|
Evidence Based Medicine |
|
Cochrane Collaboration on Hyperpigmentation |
|
Clinical Trials |
|
Ongoing Trials on Hyperpigmentation at Clinical Trials.gov Trial results on Hyperpigmentation Clinical Trials on Hyperpigmentation at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Hyperpigmentation NICE Guidance on Hyperpigmentation
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Hyperpigmentation Discussion groups on Hyperpigmentation Patient Handouts on Hyperpigmentation Directions to Hospitals Treating Hyperpigmentation Risk calculators and risk factors for Hyperpigmentation
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Hyperpigmentation |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]Associate Editor(s)-in-Chief: Luke Rusowicz-Orazem, B.S.
Overview
In dermatology, hyperpigmentation is the darkening of an area of skin or nails caused by increased melanin.
Causes
Common Causes
- Acanthosis nigricans
- Acne
- Addison's disease
- Adrenal insufficiency
- Adrenocorticotrophic hormone
- Alkaptonuria
- Angioma
- Antimalarials
- Arsenic trioxide
- Arsenicals
- Atopic dermatitis
- Atrophoderma of pasini and pierini
- Autoimmune adrenalitis
- Basal cell papilloma
- Birthmark
- Bleomycin
- Blue nevus
- Carbon monoxide toxicity
- Cardiofaciocutaneous syndrome
- Carney myxoma-endocrine complex
- Carotenemia
- Celiac disease
- Chemical poisoning
- Chloasma
- Chondrodysplasia punctata 2, x-linked dominant
- Chromosome 14 trisomy syndrome
- Chromosome 14q deletion syndrome
- Chronic renal failure
- Classic childhood adrenoleukodystrophy
- Cutaneomeningospinal angiomatosis
- Cutaneous t-cell lymphoma
- Cyclophosphamide
- Dermatitis herpetiformis
- Dermatofibroma
- Dermatopathia pigmentosa reticularis
- Dermatosis papulosa nigra
- Eczema
- Elevated melanin synthesis
- Excessive acth production
- Excessive exposure to sunlight
- Fanconi anaemia
- Freckles
- Gaucher's disease
- Glucocorticoid deficiency
- Gold salts
- Haematoma
- Haemochromatosis
- Hay-wells syndrome
- Hereditary acth resistance
- Hereditary sensory and autonomic neuropathy type 3
- Hidrotic ectodermal dysplasia
- Hydroxyurea
- Hypercarotinemia
- Incontinentia pigmenti
- Jaundice
- Kindler-weary bullous acrokeratosis poikiloderma
- Kwashiorkor
- Laser surgery
- Laugier-hunziker syndrome
- Lichen planus
- Lichen simplex chronicus
- Linea nigra
- Mccune-albright syndrome
- Melanoderma
- Melanoma
- Melarsoprol
- Melasma
- Microcephalic osteodysplastic primordial dwarfism, type 2
- Minocycline
- Moles
- Mongolian blue spots
- Multiple lentigines syndrome
- Naegeli-franceschetti-jadassohn syndrome
- Nelson's syndrome
- Neurocutaneous melanosis
- Nevus flammeus
- Nevus of ota
- Nevus spilus
- Onchocerciasis
- Parry-romberg syndrome
- Peplomycin
- Peutz-jeghers syndrome
- Photocontact dermatitis
- Phytophotodermatitis
- Pigmented hairy epidermal nevus
- Pigmented naevus
- Poems syndrome
- Polidocanol
- Polycystic ovary syndrome
- Porphyria cutanea tarda type 1
- Porphyria cutanea tarda type 2
- Prednisolone
- Primary biliary cirrhosis
- Proteus syndrome
- Psoriasis
- Scleredema adultorum
- Scleroderma
- Selenium
- Sertaconazole
- Siltuximab
- Silver poisoning
- Skin tag
- Smoker's melanosis
- Spitz nevus
- Tinea nigra
- Tinea versicolor
- Urod-related porphyria cutanea tarda
- Varicose veins
- Variegate porphyria
- Yemenite deaf-blind hypopigmentation syndrome
Causes by Organ System
Causes in Alphabetical Order
- Acanthosis nigricans
- Acne
- Addison's disease
- Adrenal insufficiency
- Adrenocorticotrophic hormone
- Alkaptonuria
- Angioma
- Antimalarials
- Arsenic trioxide
- Arsenicals
- Atopic dermatitis
- Atrophoderma of pasini and pierini
- Autoimmune adrenalitis
- Basal cell papilloma
- Berardinelli-seip congenital lipodystrophy, type 1
- Berardinelli-seip congenital lipodystrophy, type 2
- Birthmark
- Bleomycin
- Blue nevus
- Busulphan
- Canada-cronkhite syndrome
- Carbon monoxide toxicity
- Cardiofaciocutaneous syndrome
- Carney myxoma-endocrine complex
- Carotenemia
- Celiac disease
- Chemical poisoning
- Chemotherapy
- Chloasma
- Chondrodysplasia punctata 2, x-linked dominant
- Chromosome 14 trisomy syndrome
- Chromosome 14q deletion syndrome
- Chronic renal failure
- Cigarette smoke
- Cisplatin
- Classic childhood adrenoleukodystrophy
- Combined oral contraceptive pill
- Congenital erythropoeitic porphyria
- Congenital lipomatous overgrowth
- Craniolenticulosutural dysplasia
- Cronkite-canada syndrome
- Cushing's disease
- Cutaneomeningospinal angiomatosis
- Cutaneous t-cell lymphoma
- Cyclophosphamide
- Dermatitis herpetiformis
- Dermatofibroma
- Dermatopathia pigmentosa reticularis
- Dermatosis papulosa nigra
- Dexamethasone
- Dihydroxyacetone
- Dowling-degos syndrome
- Doxycycline
- Dyschromatosis universalis hereditaria
- Dyskeratosis congenita, autosomal dominant
- Dyskeratosis congenita, x-linked
- Eczema
- Elevated melanin synthesis
- Emtricitabine
- Epidermal nevus
- Erythema dyschromicum perstans
- Erythrokeratoderma variabilis
- Erythromelanosis follicularis faciei et colli
- Excessive acth production
- Excessive exposure to sunlight
- Fanconi anaemia
- Freckles
- Gaucher's disease
- Glucocorticoid deficiency
- Gold salts
- Haematoma
- Haemochromatosis
- Hay-wells syndrome
- Hereditary acth resistance
- Hereditary sensory and autonomic neuropathy type 3
- Hidrotic ectodermal dysplasia
- Humeroradioulnar synostosis
- Hydroxyurea
- Hypercarotinemia
- Hypomelanosis
- Hypothyroidism
- Incontinentia pigmenti
- Indinavir
- Insulin resistance
- Jaundice
- Kindler-weary bullous acrokeratosis poikiloderma
- Kwashiorkor
- Laser surgery
- Laugier-hunziker syndrome
- Lichen planus
- Lichen simplex chronicus
- Linea nigra
- Lison syndrome
- Lupus
- Macular amyloidosis
- Malassezia furfur
- Mastocytosis
- Mccune-albright syndrome
- Melanoderma
- Melanoma
- Melarsoprol
- Melasma
- Microcephalic osteodysplastic primordial dwarfism, type 2
- Minocycline
- Moles
- Mongolian blue spots
- Multiple lentigines syndrome
- Naegeli-franceschetti-jadassohn syndrome
- Nelson's syndrome
- Neurocutaneous melanosis
- Nevus flammeus
- Nevus of ota
- Nevus spilus
- Onchocerciasis
- Parry-romberg syndrome
- Peplomycin
- Peutz-jeghers syndrome
- Photocontact dermatitis
- Phytophotodermatitis
- Pigmented hairy epidermal nevus
- Pigmented naevus
- Poems syndrome
- Poikiloderma
- Poikiloderma of civatte
- Polidocanol
- Polycystic ovary syndrome
- Porphyria cutanea tarda type 1
- Porphyria cutanea tarda type 2
- Prednisolone
- Pregnancy
- Primary biliary cirrhosis
- Proteus syndrome
- Psoriasis
- Radiotherapy
- Rapadilino syndrome
- Reticulate acropigmentation
- Retigabine
- Retinol
- Riehl's melanosis
- Ringworm
- Rothmund-thomson syndrome
- Salicylic acid
- Schimke immunoosseous dysplasia
- Scleredema adultorum
- Scleroderma
- Selenium
- Sertaconazole
- Siltuximab
- Silver poisoning
- Skin tag
- Smoker's melanosis
- Spitz nevus
- Spondylohypoplasia arthrogryposis popliteal pterygium
- Stomach cancer
- Sunitinib malate
- Systemic sclerosis
- Tattoo
- Thiazides
- Thrombophlebitis
- Tinea nigra
- Tinea versicolor
- Urod-related porphyria cutanea tarda
- Varicose veins
- Variegate porphyria
- Vascular malformations
- Visceral leishmaniasis
- Vitreoretinochoroidopathy dominant
- Whipple's disease
- Whyte murphy syndrome
- Wolcott-rallison syndrome
- Yemenite deaf-blind hypopigmentation syndrome
Treatment
Treatment of hyperpigmentation may include hydroquinone, kojic acid, azelaic acid, ascorbic acid, tretinoin (Retinol), topical glucocorticoids, and licorice extract. Note that all treatments will fail if the affected area is exposed to the sun and if there is not adequate UVA/UVB protection.
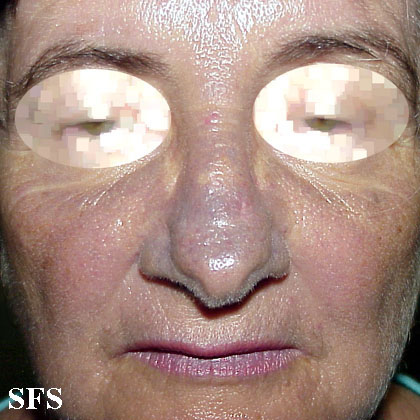
Physical examination for hyperpigmentation due to Amiodarone
-
Hyperpigmentation Due To Amiodarone.
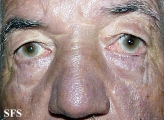
With permission of Dermatology Atlas -
Hyperpigmentation Due To Amiodarone.
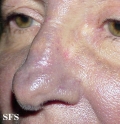
With permission of Dermatology Atlas -
Hyperpigmentation Due To Amiodarone.
With permission of Dermatology Atlas
See also
References
| Wikimedia Commons has media related to Acne. |