Melasma
|
WikiDoc Resources for Melasma |
|
Articles |
|---|
|
Most recent articles on Melasma |
|
Media |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Melasma at Clinical Trials.gov Clinical Trials on Melasma at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Melasma
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Directions to Hospitals Treating Melasma Risk calculators and risk factors for Melasma
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Melasma |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-in-Chief: Niwat Polnikorn, M.D. Associate Editor(s)-in-Chief: Jesus Rosario Hernandez, M.D. [1].
Synonyms and keywords: Chloasma, mask of pregnancy.
Overview
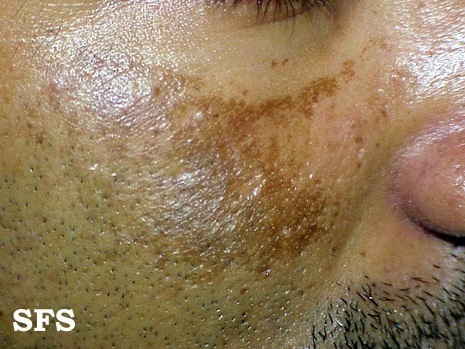
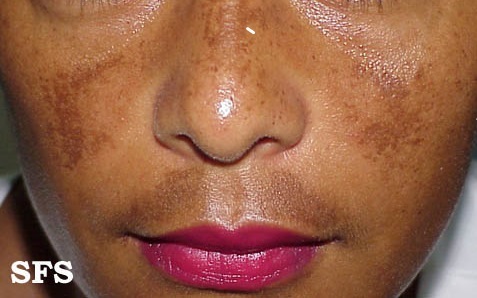
Melasma (also known as chloasma or the mask of pregnancy when present in pregnant women) is a tan or dark facial skin discoloration. Although it can affect anyone, melasma is particularly common in women, especially pregnant women and those who are taking oral contraceptives or hormone replacement therapy (HRT) medications.The ratio of female to male is 9:1 and is more common in yellow to brown skin color ( Fitzpatrick's skin photo type III to V) .The lesions usually develops in middle age and persists for many years. In post menopause women , the lesions usually fade spontaneously. Prolong exposure to sunlight is the most important etiologic factor. It is also prevalent in men and women of Native American descent (on the forearms) and in men and women of German/Russian Jewish descent (on the face).
Symptoms
The symptoms of melasma are brown to dark brown , irregular patches commonly found on the mid-face, upper cheek, nose, lips, upperlip, and forehead. Early lesions have well defined irregular margin,while older lesions tend to be grayish brown color with irregular and ill-defined border. These patches often develop gradually over time. clinically melasma had been divided into two clinical types 1) centro-facial and 2) zygoma types. Melasma does not cause any other symptoms beyond the cosmetic discoloration.
Cause
Melasma is thought to be the stimulation of melanocytes or pigment-producing cells by the female sex hormones estrogen and progesterone to produce more melanin pigments when the skin is exposed to sun. Women with a light brown skin type who are living in regions with intense sun exposure are particularly susceptible to developing this condition.
Genetic predisposition is also a major factor in determining whether someone will develop melasma.Recent study of pathology changes of melasma had revealed that majority of melasma also had increase in number of melanocytes. The average increase is about 30% together with proliferation of small blood vessels in the dermis . Melanin dropping into dermis together with presence of macrophages containing melanins (melanophages) are commonly found in long standing cases. These three findings may explain the chronicity of melasma. Proliferate and dilated blood vessels may contribute to chronicity by being the source of cytokines ,prostaglandins and leukotrienes that stimulate melanin synthesis.
The incidence of melasma also increases in patients with thyroid disease. It is thought that the overproduction of melanocyte-stimulating hormone (MSH) brought on by stress can cause outbreaks of this condition. Other rare causes of melasma include allergic reaction to medications and cosmetics. Drugs like conjugated estrogens causes melasma
Melasma Suprarenale (Latin - of the adrenals) is a symptom of Addison's disease, particularly when caused by pressure or minor injury to the skin, as discovered by Dr. FJJ Schmidt of Rotterdam in 1859.
Medications
Diagnosis
Melasma is usually diagnosed visually or with assistance of a Wood's lamp (340 - 400 nm wavelength). Under Wood's lamp, excess melanin in the epidermis can be distinguished from that of the dermis. By this technique melasma can be divided into two types 1) epidermal 2) mixed (epidermal+ dermal). This diffentiation is important for planning of management.
Physical examination
Gallery
Head
Treatment
The discoloration usually disappears spontaneously over a period of several months after giving birth or stopping the oral contraceptives or hormone replacement therapy. In cases without definite causes, the lesions may persist for many years. In cases that severity of lesions justify the treatment, the following are the common treatment methods available: 1) Avoiding of exposure to strong sunlight (ultraviolet range ) with UVA-blocker sunscreen (320-400 nm) prevention. Since UVA is the most important wavelength of sunlight that stimulate hyperpigmentation. The over the counter UVA-sunscreen with PA more than +++ and SPF more than 30 is recommended. 2)Reduction of melanin synthesis, the most commonly use drug is hydroquinone 2-4% . To enhance effectiveness ,4% hydroquinone is combined with tretinoin(0.05%) and steroids(fluocinolone acetonide 0.01%) and has been named Kligman's formula. This formula had been proved to be the most effective in clearing of epidermal melasma. More than 60% will have complete clearing by three months. The problem of this formula is its long term side effects.At present Tri-Luma TM (Galderma,USA) is the only one triple drugs approved by USA-FDA for treatment of melasma. Hydroquinone has been associated with many complictions in dark skin patients i.e. contact dermatitis, exogenous ochronosis, confetti-like hypopigmentation and rebound hyperpigmentation. Others topical treatments that had been used for treatments include arbutin, kojic acid, licorice extract, azelaic acid, vitamin C, soy, green tea , decapeptides, ,glove extract etc. The results were inferior to Kligman's formular but claimed to have lower incidence of complications. Many of these products are ingredients of over the counter whitening creams. In some countries hydroquinone has not been approved , because of concern of mutagenic and toxicity e.g. Japan. The second technique for treatment of melasma is by enhancing peeling of epithelial cells by chemicals e.g. retinoic acid, glycolic , salycylic acid. Facial peels with glycolic or alpha hydroxy acids are popular in many countries. For mixed type with dermal melanophages and dilated blood vessels, usually resisted to topical treatments. These types are justified for method with deeper effects to melanocytes and melanophages. Recently two laser systems have been shown to be effective for treatment of deep lesions of melasma 1) flat beam, high energy Q-switched NdYAG (1064 nm)(Medlite c6/Revlite, Hoya-Conbio,USA) 2) Fractional Erbium Glass (1550 nm) laser. The first technique originate from Asia where mixed melasma are more common. The technique has been called "Laser toning" which work by superficial vaporization of epidermis, fragmentation and dispersion of melanins in melanocytes and melanophages and reduction of melanocytes. Thesecond technique works by partial reduction of epidermal melanocytes and transepidermal elimination of dermal melanins. Both technique needs mutiple treatments until the lesions fade. Intense pulse light (IPL) or frequency-doubled Q-switched NdYAG laser ( 532 nm) which was effective for superficial hyperpigmentation often resulted in transient improvemnt with rapid recurrence or worsening of lesions.In Asia , many doctors are treating melasma with oral tranexamic acid 1-2 Gram/day. This medicine has not been approved for this condition. The most serious complication of this medicine is thromboembolism. Prolong use of this medicine should be discouraged. Recently intradermal injection of 4% tranexamic acid had been reported to be effective treatment of melasma. After multiple laser treatments and hyperpigmentation decrease to close to normal skin colour, topical maintainance with effective medication should be administered . Cure may be unlikely for melasma, life long sunlight protection and topical antioxidants with safe antimelanin synthesis has to be applied as long as possible.