Streptococcus pneumoniae infection
For patient information click here
| Streptococcus pneumoniae | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
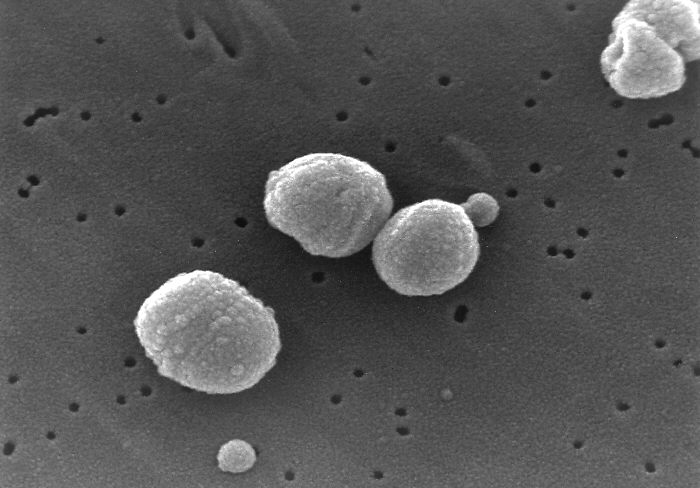 SEM micrograph of S. pneumoniae.
| ||||||||||||||
| Scientific classification | ||||||||||||||
| ||||||||||||||
| Binomial name | ||||||||||||||
| Streptococcus pneumoniae (Klein 1884) Chester 1901 |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Streptococcus pneumoniae, or pneumococcus, is a Gram-positive, alpha-hemolytic diplococcus bacterium and a member of the genus Streptococcus.[1] A significant human pathogen, S. pneumoniae was recognized as a major cause of pneumonia in the late 19th century and is the subject of many humoral immunity studies.
Despite the name, the organism causes many types of infection other than pneumonia, including acute sinusitis, otitis media, meningitis, osteomyelitis, septic arthritis, endocarditis, peritonitis, pericarditis, cellulitis, and brain abscess.
S. pneumoniae is the most common cause of bacterial meningitis in adults and children, and is one of the top two isolates found in otitis media.[2] Pneumococcal pneumonia is more common in the very young and the very old.
S. pneumoniae can be differentiated from Streptococcus viridans, which is also alpha hemolytic, using an optochin test, as S. pneumoniae is optochin sensitive. The encapsulated, gram-positive coccoid bacteria have a distinctive morphology on gram stain, the so-called, "lancet shape." It has a polysaccharide capsule that acts as a virulence factor for the organism; 91 different capsular types are known, and these types differ in virulence, prevalence, and extent of drug resistance.
History
In 1881, the organism, then known as the pneumococcus for its role as an etiologic agent of pneumonia, was first isolated simultaneously and independently by the U.S Army physician George Sternberg and the French chemist Louis Pasteur.
The organism was termed Diplococcus pneumoniae from 1926 because of its characteristic appearance in Gram-stained sputum. It was renamed Streptococcus pneumoniae in 1974 because of its growth in chains in liquid media.
S. pneumoniae played a central role in demonstrating that genetic material consists of DNA. In 1928, Frederick Griffith demonstrated transformation of live, harmless pneumococcus into a lethal form by co-inoculating the live pneumococci into a mouse along with heat-killed, virulent pneumococci. In 1944, Oswald Avery, Colin MacLeod, and Maclyn McCarty demonstrated that the transforming factor in Griffith's experiment was DNA, not protein as was widely believed at the time.[3] Avery's work marked the birth of the molecular era of genetics.[4]
Pathogenesis
S. pneumoniae is normally found in the nasopharynx of 5-10% of healthy adults, and 20-40% of healthy children.[1] It can be found in higher amounts in certain environments, especially those where people are spending a great deal of time in close proximity to each other (day cares, army barracks). It attaches to nasopharyngeal cells through interaction of bacterial surface adhesins. This normal colonization can become infectious if the organisms are carried into areas such as the Eustachian tube or nasal sinuses where it can cause otitis media and sinusitis, respectively. Pneumonia occurs if the organisms are inhaled into the lungs and not cleared (again, viral infection, or smoking-induced ciliary paralysis might be contributing factors). Once the organism makes its way to a site where it is not normally found, it activates the complement protein group, stimulates cytokine production, and attracts white blood cells (specifically neutrophils). The organism's polysaccharide capsule makes it resistant to phagocytosis, and if there is no pre-existing anticapsular antibody, alveolar macrophages cannot adequately kill the pneumococci. The organism spreads to the blood stream (where it can cause bacteremia) and is carried to the meninges, joint spaces, bones, and peritoneal cavity, and may result in meningitis, brain abscess, septic arthritis, or osteomyelitis.
S. pneumoniae has several virulence factors, including the polysaccharide capsule mentioned earlier, that help it evade a host's immune system. It has pneumococcal surface proteins that inhibit complement-mediated opsonization, and it secretes IgA1 protease that will destroy secretory IgA produced by the body.
The risk of pneumococcal infection is much increased in persons with impaired IgG synthesis, impaired phagocytosis, or defective clearance of pneumococci. In particular, the absence of a functional spleen, through congenital asplenia, splenectomy, or sickle-cell disease predisposes one to a more severe course of infection (Overwhelming post-splenectomy infection) and prevention measures are indicated (see asplenia).
Virulence Factors
S. pneumoniae expresses different virulence factors on its cell surface and inside the organism. These virulence factors contribute to some of the clinical manifestations during infection with S. pneumoniae.
- Polysaccharide capsule -prevents phagocytosis by host immune cells by inhibiting C3b opsonization of the bacterial cells
- Pneumolysin (Ply) -a 53-kDa protein that can cause lysis of host cells and activate complement
- Autolysin (LytA) -activation of this protein lyses the bacteria releasing its internal contents (i.e. pneumolysin)
- Hydrogen peroxide - causes damage to host cells (can cause apoptosis in neuronal cells during meningitis) and has bactericidal effects against competing bacteria (Staphylococcus aureus)[5]
- Pili - hair-like structures that extend from the surface of many strains of S. pneumoniae. They contribute to colonization of upper respiratory tract and increase the formation of large amounts of TNF by the immune system during sepsis, raising the possibility of septic shock[6]
- Choline binding protein A (CbpA) -an adhesin that can interact with carbohydrates on the cell surface of pulmonary epithelial cells
- Protective Antigen (PspA) -can inhibit complement-mediated opsonization of pneumococci
Humoral immunity
In the 19th century, it was demonstrated that immunization of rabbits with killed pneumococci protected them against subsequent challenge with viable pneumococci. Serum from immunized rabbits or from humans who had recovered from pneumococcal pneumonia also conferred protection. In the 20th century, the efficacy of immunization was demonstrated in South African miners.
It was discovered that the pneumococcus's capsule made it resistant to phagocytosis, and in the 1920s it was shown that an antibody specific for capsular polysaccharide aided the killing of S. pneumoniae. In 1936, a pneumococcal capsular polysaccharide vaccine was used to abort an epidemic of pneumococcal pneumonia. In the 1940s, experiments on capsular transformation by pneumococci first identified DNA as the material that carries genetic information.
In 1900, it was recognized that different serovars of pneumococci exist, and that immunization with a given serovar did not protect against infection with other serovars. Since then over ninety serovars have been discovered, each with a unique polysaccharide capsule which can be identified by the quellung reaction. Because some of these serovars cause disease more commonly than others, it is possible to provide reasonable protection by immunizing with less than 90 serovars; the current vaccine contains 23 serovars (i.e., it is "23-valent").
The serovars are numbered according to two systems: the American system, which numbers them in the order in which they were discovered, and the Danish system which groups them according to antigenic similarities.
Diagnosis
Depending on the nature of infection, an appropriate sample is collected for laboratory identification. Pneumococci are typically gram positive, cocci, seen in pairs or chains. When cultured on blood agar plates with added optochin antibiotic disk, they show alpha-hemolytic colonies and a clear zone of inhibition around the disk meaning they're sensitive to the antibiotic. Pneumococci are also bile soluble. Just like other streptococci, it's catalase negative. Quellung test to identify specific capsular polysaccharides may also be done.
Treatment
Historically, treatment relied primarily on β-lactam antibiotics. In the 1960s, nearly all strains of S. pneumoniae were susceptible to penicillin, but since that time, there has been an increasing prevalence of penicillin resistance, especially in areas of high antibiotic use. A varying proportion of strains may also be resistant to cephalosporins, macrolides (such as erythromycin), tetracycline, clindamycin and the quinolones. Penicillin-resistant strains are more likely to be resistant to other antibiotics. Most isolates remain susceptible to vancomycin, though its use in a β-lactam-susceptible isolate is less desirable because of tissue distribution of the drug and concerns of development of vancomycin resistance. More advanced beta-lactam antibiotics (cephalosporins) are commonly used in combination with other drugs to treat meningitis and community-acquired pneumonia. In adults, recently developed fluoroquinolones such as levofloxacin and moxifloxacin are often used to provide empiric coverage for patients with pneumonia. Susceptibility testing should be routine, with empiric antibiotic treatment guided by resistance patterns in the community in which the organism was acquired, pending the results. There is currently debate as to how relevant the results of susceptibility testing are to clinical outcome.[7][8] There is slight clinical evidence that penicillins may act synergistically with macrolides to improve outcomes.[9]
Prevention
Vaccination in the USA
In the USA, a heptavalent pneumococcal conjugate vaccine vaccine (PCV 7) (e.g. Prevnar) is recommended since 2000 for all children aged 2-23 months and for at-risk children aged 24-59 months. The normally 4-doses series is given at 2, 4, 6 & 12 - 14 months of age. Protection is good against deep pneumococcal infections (especially septicemia and meningitis). Similar 9- and 13-valent vaccines are being tested. Yet, if the child is exposed to a serotype of pneumococcus that is not contained in the vaccine, he/she is not afforded any protection. This limitation, and the ability of capsular-polysaccharide conjugate vaccines to promote the spread of non-covered serotypes, has led to research into vaccines that would provide species-wide protection.
Pneumococcal polysaccharide vaccine (Pneumovax™ is one brand) gives at least 85% protection in those under 55 years of age for five years or longer. Immunization is suggested for those at highest risk of infection, including those 65 years or older, and generally should be a single lifetime dose (high risk side effects if repeated). The standard 23-valent vaccines are ineffective for children under two years old.
The current guidelines of the American College of Physicians call for administration of the immunization between ages 2 and 65 when indicated, or at age 65. If someone received the immunization before age 60, the guidelines call for a one-time revaccination.
Revaccination at periodic intervals is also indicated for those with other conditions such as asplenia or nephrotic syndrome.
Vaccination in the UK
It was announced in February 2006 that the UK government would introduce vaccination with the conjugate vaccine in children aged 2, 4 and 13 months.[10][11] This is expected to start on September 4,2006 and is to include changes to the immunisation programme in general.[12]
Vaccination Worldwide
Pneumococcal vaccines Accelerated Development and Introduction Plan (PnemoADIP) is a program to accelerate the evaluation and access to new pneumococcal vaccines in the developing world. PneumoADIP is funded by the Global Alliance for Vaccines and Immunization (GAVI). Thirty GAVI countries have expressed interest in participating by 2010. PneumoADIP aims to save 5.4 million children by 2030.[13]
Vaccine research
There is currently research into producing vaccines than can be given into the nose rather than by injection.[14] [15] It is believed that this improves vaccine efficacy and also avoids the need for injection.
The development of serotype-specific anticapsular monoclonal antibodies has also been an area of vaccine research in recent years. These antibodies have been shown to prolong survival in a mouse model of pneumococcal infection characterized by a reduction in bacterial loads and a suppression of the host inflammatory response.[16][17]
Interaction with Haemophilus influenzae
Both H. influenzae and S. pneumoniae can be found in the human upper respiratory system. A study of competition in a laboratory revealed that, in a petrì dish, S. pneumoniae always overpowered H. influenzae by attacking it with a hydrogen peroxide and stripping off surface molecules that H. influenzae needs for survival.
When both bacteria are placed together into a nasal cavity, within 2 weeks, only H. influenzae survives. When both are placed separately into a nasal cavity, each one survives. Upon examining the upper respiratory tissue from mice exposed to both bacteria, an extraordinarily large number of neutrophils immune cells were found. In mice exposed to only one bacteria, the cells were not present
Lab tests show that neutrophils that were exposed to already dead H. influenzae were more aggressive in attacking S. pneumoniae than unexposed neutrophils. Exposure to killed H. influenzae had no effect on live H. influenzae.
Two scenarios may be responsible for this response:
- When H. influenzae is attacked by S. pneumoniae, it signals the immune system to attack the S. pneumoniae
- The combination of the two species together sets off an immune system alarm that is not set off by either species individually.
It is unclear why H. influenzae is not affected by the immune system response.[18]
References
- ↑ 1.0 1.1 Ryan KJ; Ray CG (editors) (2004). Sherris Medical Microbiology (4th ed. ed.). McGraw Hill. ISBN 0-8385-8529-9.
- ↑ Dagan R. "Treatment of acute otitis media - challenges in the era of antibiotic resistance". Vaccine. 19 Suppl 1: S9–S16. PMID 11163457.
- ↑ Avery OT, MacLeod CM, and McCarty M (1944). "Studies on the chemical nature of the substance inducing transformation of pneumococcal types." J Exp Med 79:137-158.
- ↑ Lederberg J (1994). "The transformation of genetics by DNA: an anniversary celebration of Avery, MacLeod and McCarty (1944)". Genetics. 136 (2): 423–6. PMID 8150273.
- ↑ Pericone, Christopher D., Overweg, Karin, Hermans, Peter W. M., Weiser, Jeffrey N. (2000). "Inhibitory and Bactericidal Effects of Hydrogen Peroxide Production by Streptococcus pneumoniae on Other Inhabitants of the Upper Respiratory Tract". Infect Immun. 68 (7): 3990–3997. PMID 10858213.
- ↑ Barocchi M, Ries J, Zogaj X, Hemsley C, Albiger B, Kanth A, Dahlberg S, Fernebro J, Moschioni M, Masignani V, Hultenby K, Taddei A, Beiter K, Wartha F, von Euler A, Covacci A, Holden D, Normark S, Rappuoli R, Henriques-Normark B (2006). "A pneumococcal pilus influences virulence and host inflammatory responses". Proc Natl Acad Sci U S A. 103 (8): 2857–2862. PMID 16481624.
- ↑ Peterson LR (2006). "Penicillins for treatment of pneumococcal pneumonia: does in vitro resistance really matter?". Clin Infect Dis. 42 (2): 224–33. PMID 16355333.
- ↑ Tleyjeh IM, Tlaygeh HM, Hejal R, Montori VM, Baddour LM (2006). "The impact of penicillin resistance on short-term mortality in hospitalized adults with pneumococcal pneumonia: a systematic review and meta-analysis". Clin Infect Dis. 42 (6): 788–97. PMID 16477555.
- ↑ Martínez JA, Horcajada JP, Almela M; et al. (2003). "Addition of a Macrolide to a β-Lactam based empirical antibiotic regimen is associated with lower in-hospital mortality for patients with bacteremic pneumococcal pneumonia". Clin Infect Dis. 36: 389–395. doi:10.1086/367541. PMID 12567294.
- ↑ "Children to be given new vaccine" BBC News, February 08, 2006, retrieved August 25, 2006
- ↑ "Pneumococcal vaccine added to the childhood immunisation programme" February 08, 2006
- ↑ "Changes to the immunisation programme in the UK" Meningitis Research Foundation, retrieved August 25, 2006
- ↑ "PneumoADIP website"
- ↑ Hanniffy SB, Carter AT, Hitchin E, Wellsa JM. (2007). "Mucosal delivery of a Pneumococcal vaccine using Lactococcus lactis affords protection against respiratory infection". J Infect Dis. 195: 185–193.
- ↑ Malley R. Lipsitch M, Stack A, Saladino R, Fleisher G, Pelton S, Thompson C, Briles D, Anderson P. (2001). "Intranasal immunization with killed unencapsulated whole cells prevents colonization and invasive disease by capsulated pneumococci". Infect Immun. 69: 4870–4873.
- ↑ Burns T, Abadi M, Pirofski L (2005). "Modulation of the lung inflammatory response to serotype 8 pneumococcal infection by a human immunoglobulin m monoclonal antibody to serotype 8 capsular polysaccharide". Infect Immun. 73 (8): 4530–8. PMID 16040964.
- ↑ Fabrizio K, Groner A, Boes M, Pirofski L. "A Human Monoclonal IgM Reduces Bacteremia and Inflammation in a Mouse Model of Systemic Pneumococcal Infection". Clin Vaccine Immunol. PMID 17301214.
- ↑ Lysenko ES, Ratner AJ, Nelson AL, Weiser JN (2005). "The role of innate immune responses in the outcome of interspecies competition for colonization of mucosal surfaces". PLoS Pathog. 1 (1): e1. PMID 16201010. Full text
ca:Pneumococ de:Pneumokokken it:Streptococcus pneumoniae lt:Streptococcus pneumoniae nl:Pneumokok no:Pneumokokk sr:Пнеумококе fi:Streptococcus pneumoniae uk:Streptococcus pneumoniae