Multiple sclerosis classification: Difference between revisions
No edit summary |
|||
| Line 3: | Line 3: | ||
{{CMG}} | {{CMG}} | ||
==Classification== | ==Classification== | ||
| Line 25: | Line 24: | ||
{{reflist|2}} | {{reflist|2}} | ||
[[Category:Primary care]] | |||
[[Category:Autoimmune diseases]] | |||
[[Category:Neurological disorders]] | |||
[[Category:multiple sclerosis]] | |||
[[Category:Neurology]] | |||
[[Category:Orthopedics]] | |||
[[Category:Disease]] | |||
[[Category:Needs overview]] | |||
{{WH}} | {{WH}} | ||
{{WS}} | {{WS}} | ||
Revision as of 18:10, 30 April 2013
|
Multiple sclerosis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Multiple sclerosis classification On the Web |
|
American Roentgen Ray Society Images of Multiple sclerosis classification |
|
Risk calculators and risk factors for Multiple sclerosis classification |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [2]
Classification
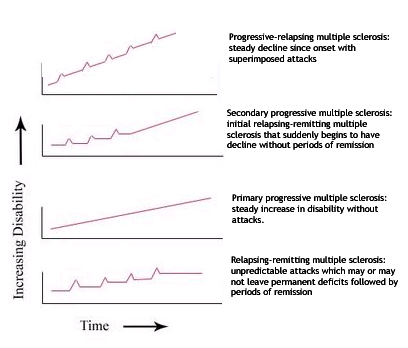
The course of MS is difficult to predict, and the disease may at times either lie dormant or progress steadily. Several subtypes, or patterns of progression, have been described. Subtypes use the past course of the disease in an attempt to predict the future course. Subtypes are important not only for prognosis but also for therapeutic decisions. In 1996 the United States National Multiple Sclerosis Society standardized the following four subtype definitions:[1]
- Relapsing-remitting
- Relapsing-remitting describes the initial course of 85% to 90% of individuals with MS. This subtype is characterized by unpredictable attacks (relapses) followed by periods of months to years of relative quiet (remission) with no new signs of disease activity. Deficits suffered during the attacks may either resolve or may be permanent. When deficits always resolve between attacks, this is referred to as "benign" MS.
- Secondary progressive
- Secondary progressive describes around 80% of those with initial relapsing-remitting MS, who then begin to have neurologic decline between their acute attacks without any definite periods of remission. This decline may include new neurologic symptoms, worsening cognitive function, or other deficits. Secondary progressive is the most common type of MS and causes the greatest amount of disability.
- Primary progressive
- Primary progressive describes the approximately 10% of individuals who never have remission after their initial MS symptoms. Decline occurs continuously without clear attacks. The primary progressive subtype tends to affect people who are older at disease onset.
- Progressive relapsing
- Progressive relapsing describes those individuals who, from the onset of their MS, have a steady neurologic decline but also suffer superimposed attacks; and is the least common of all subtypes
Nevertheless the earliest clinical presentation of relapsing-remitting MS (RRMS) is the clinically isolated syndrome (CIS). In CIS, there is a subacute attack suggestive of demyelination but the person does not fullfill the criteria for multiple sclerosis.[2] Several studies have shown that starting treatment with interferons during the initial attack can decrease the chance that a patient will develop MS.[3][4][5]
Special cases of the disease with non-standard behavior have also been described although many researchers believe they are different diseases. These cases are sometimes referred to as borderline forms of multiple sclerosis and are Neuromyelitis optica (NMO), Balo concentric sclerosis, Schilder's diffuse sclerosis and Marburg multiple sclerosis.[6]
References
- ↑ Lublin FD; Reingold SC. Defining the clinical course of multiple sclerosis: results of an international survey. National Multiple Sclerosis Society (USA) Advisory Committee on Clinical Trials of New Agents in Multiple Sclerosis. Neurology 1996 Apr;46(4):907-11. PMID 8780061
- ↑ Miller D, Barkhof F, Montalban X, Thompson A, Filippi M (2005). "Clinically isolated syndromes suggestive of multiple sclerosis, part I: natural history, pathogenesis, diagnosis, and prognosis". Lancet neurology. 4 (5): 281–8. doi:10.1016/S1474-4422(05)70071-5. PMID 15847841.
- ↑ Jacobs LD; Beck RW; Simon JH; Kinkel RP; Brownscheidle CM; Murray TJ; Simonian NA; Slasor PJ; Sandrock AW. Intramuscular interferon beta-1a therapy initiated during a first demyelinating event in multiple sclerosis. CHAMPS Study Group. N Engl J Med 2000 September 28;343(13):898–904. PMID 11006365
- ↑ Comi G; Filippi M; Barkhof F; Durelli L; Edan G; Fernandez O; Hartung H; Seeldrayers P; Sorensen PS; Rovaris M; Martinelli V; Hommes OR.Effect of early interferon treatment on conversion to definite multiple sclerosis: a randomised study.Lancet 2001 May 19;357(9268):1576–82. PMID 11377645
- ↑ Kappos L, Freedman MS, Polman CH; et al. (2007). "Effect of early versus delayed interferon beta-1b treatment on disability after a first clinical event suggestive of multiple sclerosis: a 3-year follow-up analysis of the BENEFIT study". Lancet. 370 (9585): 389–97. doi:10.1016/S0140-6736(07)61194-5. PMID 17679016.
- ↑ Borderline forms of MS, Fontaine, B., Federation de Neurologie, INSERM U546, Groupe Hospitalier, Faculte de Medecine Pitie-Salpetriere, Paris [1]