Crohn's disease pathophysiology
|
Crohn's disease |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Crohn's disease pathophysiology On the Web |
|
American Roentgen Ray Society Images of Crohn's disease pathophysiology |
|
Risk calculators and risk factors for Crohn's disease pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Pathophysiology
Genetics
Mutations in the CARD15 gene (also known as the NOD2 gene) are associated with Crohn's disease[1] and with susceptibility to certain phenotypes of disease location and activity.[2] In earlier studies, only two genes were linked to Crohn's, but scientists now believe there are over eight genes that show genetics play a crucial role in the disease.
Abnormalities in the immune system have often been invoked as being causes of Crohn's disease. It has been hypothesized that Crohn's disease involves augmentation of the Th1 of cytokine response in inflammation.[3] The most recent gene to be implicated in Crohn's disease is ATG16L1, which may reduce the effectiveness of autophagy, and hinder the body's ability to attack invasive bacteria.[4]
Gross Pathology
There are certain characteristic features of the pathology seen that point toward Crohn's disease. Crohn's disease shows a transmural pattern of inflammation, meaning that the inflammation may span the entire depth of the intestinal wall. Grossly, ulceration is an outcome seen in highly active disease. There is usually an abrupt transition between unaffected tissue and the ulcer.
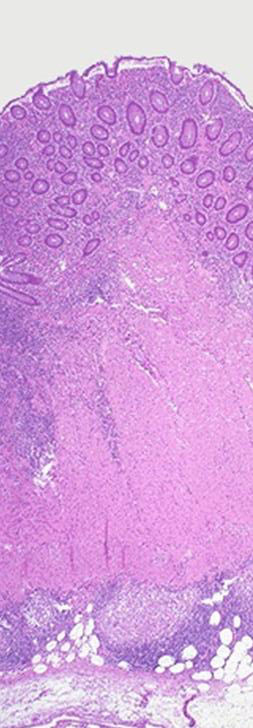
Microscopic Pathology
Under a microscope, biopsies of the affected colon may show mucosal inflammation. Transmural inflammation results in formation of lymphoid aggregates throughout the wall of the colon. This inflammation is characterized by focal infiltration of neutrophils, a type of inflammatory cell, into the epithelium. This typically occurs in the area overlying lymphoid aggregates. These neutrophils, along with mononuclear cells, may infiltrate into the crypts leading to inflammation (crypititis) or abscess (crypt abscess). Granulomas, aggregates of macrophage derivatives known as giant cells, are found in 50% of cases and are most specific for Crohn's disease. The granulomas of Crohn's disease do not show "caseation", a cheese-like appearance on microscopic examination that is characteristic of granulomas associated with infections such as tuberculosis. Biopsies may also show chronic mucosal damage as evidenced by blunting of the intestinal villi, atypical branching of the crypts, and change in the tissue type (metaplasia). One example of such metaplasia, Paneth cell metaplasia, involves development of Paneth cells (typically found in the small intestine) in other parts of the gastrointestinal system.[5]
References
- ↑ Ogura Y, Bonen DK, Inohara N, et al. A frameshift mutation in NOD2 associated with susceptibility to Crohn's disease. Nature. 2001 May 31;411(6837):603-6.
- ↑ Cuthbert A, Fisher S, Mirza M; et al. (2002). "The contribution of NOD2 gene mutations to the risk and site of disease in inflammatory bowel disease". Gastroenterology. 122 (4): 867–74. PMID 11910337.
- ↑ Cobrin GM, Abreu MT. Defects in mucosal immunity leading to Crohn's disease. Immunol Rev. 2005 Aug;206:277-95. PMID 16048555
- ↑ Prescott NJ, Fisher SA, Franke A, Hampe J, Onnie CM, Soars D, Bagnall R, Mirza MM, Sanderson J, Forbes A, Mansfield JC, Lewis CM, Schreiber S, Mathew CG. A nonsynonymous SNP in ATG16L1 predisposes to ileal Crohn's disease and is independent of CARD15 and IBD5. Gastroenterology. 2007 May;132(5):1665-71. PMID: 17484864.
- ↑ Crawford JM. "The Gastrointestinal tract, Chapter 17". In Cotran RS, Kumar V, Robbins SL. Robbins Pathologic Basis of Disease: 5th Edition. W.B. Saunders and Company, Philadelphia, 1994.