Tricuspid valve
|
WikiDoc Resources for Tricuspid valve |
|
Articles |
|---|
|
Most recent articles on Tricuspid valve Most cited articles on Tricuspid valve |
|
Media |
|
Powerpoint slides on Tricuspid valve |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Tricuspid valve at Clinical Trials.gov Trial results on Tricuspid valve Clinical Trials on Tricuspid valve at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Tricuspid valve NICE Guidance on Tricuspid valve
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Tricuspid valve Discussion groups on Tricuspid valve Patient Handouts on Tricuspid valve Directions to Hospitals Treating Tricuspid valve Risk calculators and risk factors for Tricuspid valve
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Tricuspid valve |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Basir Gill, M.B.B.S, M.D.[2]
Overview
The tricuspid valve is on the right side of the heart, between the right atrium and the right ventricle, and it is the largest valve of the heart.[1][2] The normal tricuspid valve has four main components: the annulus, leaflets, chordae tendineae, and papillary muscles.[3] Tricuspid valves may also occur with two or four leaflets, and the number may change during life (Van Pragh, 1998).
Valve Morphology
The anatomy of tricuspid valve is designed to prevent blood from returning to the right atrium when the right ventricle contracts. Its morphology is classified into four types:[4]
- Type I: Three leaflets (most common variant overall)
- Type II: Two leaflets
- Type III: Four Leaflets. Further divided into IIIA, IIIB (second most common variant overall) and IIIC subtypes based on location of the fourth cusp.
- Typer IV: More than four leaflets
Annulus
The annulus is a D-shaped fibrous ring that conforms to the muscular movements during a cardiac cycle. It acts as a tether for the leaflets. [3]
Leaflets and Cusps
For the most common-three leaflet morphology, the largest cusp is interposed between the atrioventricular orifice and the conus arteriosus and is termed the anterior or infundibular cusp. A second, the posterior or marginal cusp, is in relation to the right margin of the ventricle. A third, the medial or septal cusp, to the ventricular septum.
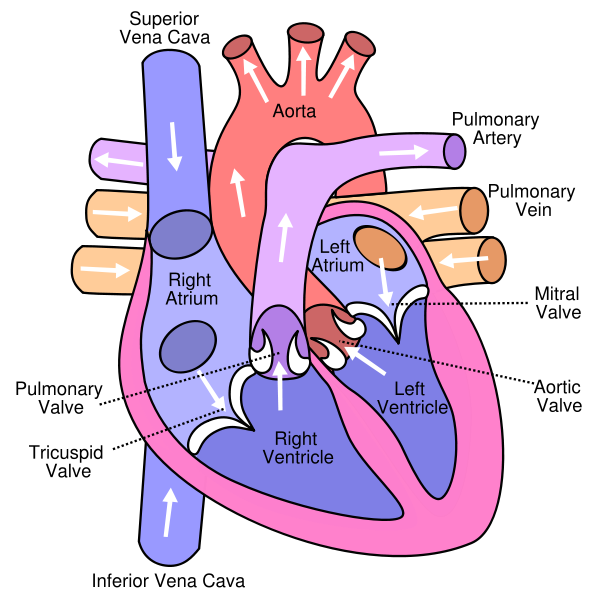
-
Anterior (frontal) view of the opened heart. White arrows indicate normal blood flow. (Tricuspid valve labeled at bottom left.)
Pathology
A small amount of leakage or regurgitation is not uncommon in the tricuspid valve. It is a common valve to be infected (endocarditis) in IV drug users.[5][6] Although it is not a common site of endocarditis, patients with a small VSD usually develop endocarditis of the tricuspid valve.
The tricuspid valve can be affected by rheumatic fever which can cause tricuspid stenosis or tricuspid insufficiency (also called tricuspid regurgitation).
Some patients are born with congenital abnormalities of the tricuspid valve. Congenital apical displacement of the tricuspid valve is called Ebstein's anomaly and typically causes significant tricuspid regurgitation.
The first endovascular tricuspid valve implant was performed by physicians at the Cleveland Clinic. [7]
Images
Images shown below are Courtesy of Professor Peter Anderson DVM PhD and Published with permission. © PEIR, University of Alabama at Birmingham, Department of Pathology
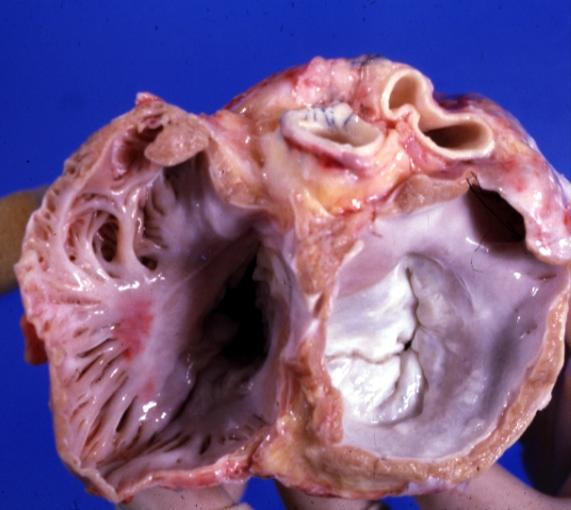
-
Mitral and tricuspid valves from atria. Normal valvular anatomy
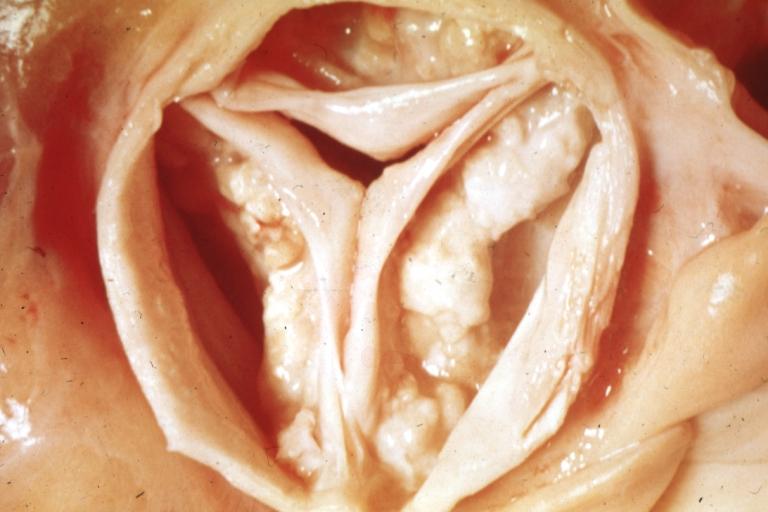
-
Tricuspid valve. A close look up.
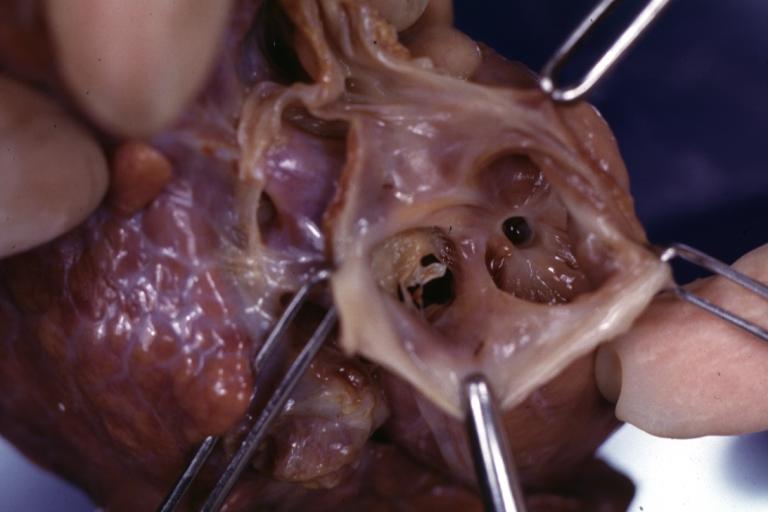
-
Tricuspid valve in an infant with hypoplastic right ventricle
References
- ↑ Dahou, A., Levin, D., Reisman, M., & Hahn, R. T. (2019). Anatomy and physiology of the tricuspid valve. JACC. Cardiovascular Imaging, 12(3), 458–468. https://doi.org/10.1016/j.jcmg.2018.07.032
- ↑ Hahn, R. T., Waxman, A. B., Denti, P., & Delhaas, T. (2019). Anatomic relationship of the complex tricuspid valve, right ventricle, and pulmonary vasculature: A review: A review. JAMA Cardiology, 4(5), 478–487. https://doi.org/10.1001/jamacardio.2019.0535
- ↑ 3.0 3.1 Dahou, A., Levin, D., Reisman, M., & Hahn, R. T. (2019). Anatomy and physiology of the tricuspid valve. JACC. Cardiovascular Imaging, 12(3), 458–468. https://doi.org/10.1016/j.jcmg.2018.07.032
- ↑ Hahn, R. T., Weckbach, L. T., Noack, T., Hamid, N., Kitamura, M., Bae, R., Lurz, P., Kodali, S. K., Sorajja, P., Hausleiter, J., & Nabauer, M. (2021). Proposal for a standard echocardiographic tricuspid valve nomenclature. JACC. Cardiovascular Imaging, 14(7), 1299–1305. https://doi.org/10.1016/j.jcmg.2021.01.012
- ↑ Demin AA, Drobysheva VP, Vel'ter OIu (2000). "[Infectious endocarditis in intravenous drug abusers]". Klinicheskaia meditsina (in Russian). 78 (8): 47–51. PMID 11019526.
- ↑ Butany J, Dev V, Leong SW, Soor GS, Thangaroopan M, Borger MA (2006). "Infective endocarditis of the tricuspid valve". Journal of cardiac surgery. 21 (6): 603–4. PMID 17073968.
- ↑ http://www.universitycircle.org/content/healthcare.asp