Endometriosis echocardiography or ultrasound
|
Endometriosis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Endometriosis echocardiography or ultrasound On the Web |
|
American Roentgen Ray Society Images of Endometriosis echocardiography or ultrasound |
|
Risk calculators and risk factors for Endometriosis echocardiography or ultrasound |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Joseph Nasr, M.D.[2], Aravind Kuchkuntla, M.B.B.S[3]
Overview
Abdominal ultrasound in a patient with endometriosis is helpful in differentiating endometriosis from other cystic abnormalities. The endometrial lesions have increased vascularity and will demonstrate increased Doppler flow. Transvaginal ultrasound is more sensitive. Multiple international guidelines recommend transvaginal pelvic ultrasound as the initial diagnostic test for patients with pelvic pain and suspected endometriosis.[1]
Ultrasound
- Abdominal ultrasound is helpful in differentiating endometriosis from other cystic abnormalities. The endometrial lesions have increased vascularity and will demonstrate increased Doppler flow.[2]
- Transvaginal ultrasound is useful in the detection of deeply seated endometriosis and rectosigmoid endometriosis. Transvaginal ultrasound is more sensitive than abdominal ultrasound.[3]
- Key features of endometrioma are typically unilocular cysts but may be multilocular, containing thin or thick septations.
- Ultrasound may show mural nodules in the case of endometriosis. If these mural nodules are hyperechoic, these have a high predictive value for endometrioma over non-endometrial cancer.
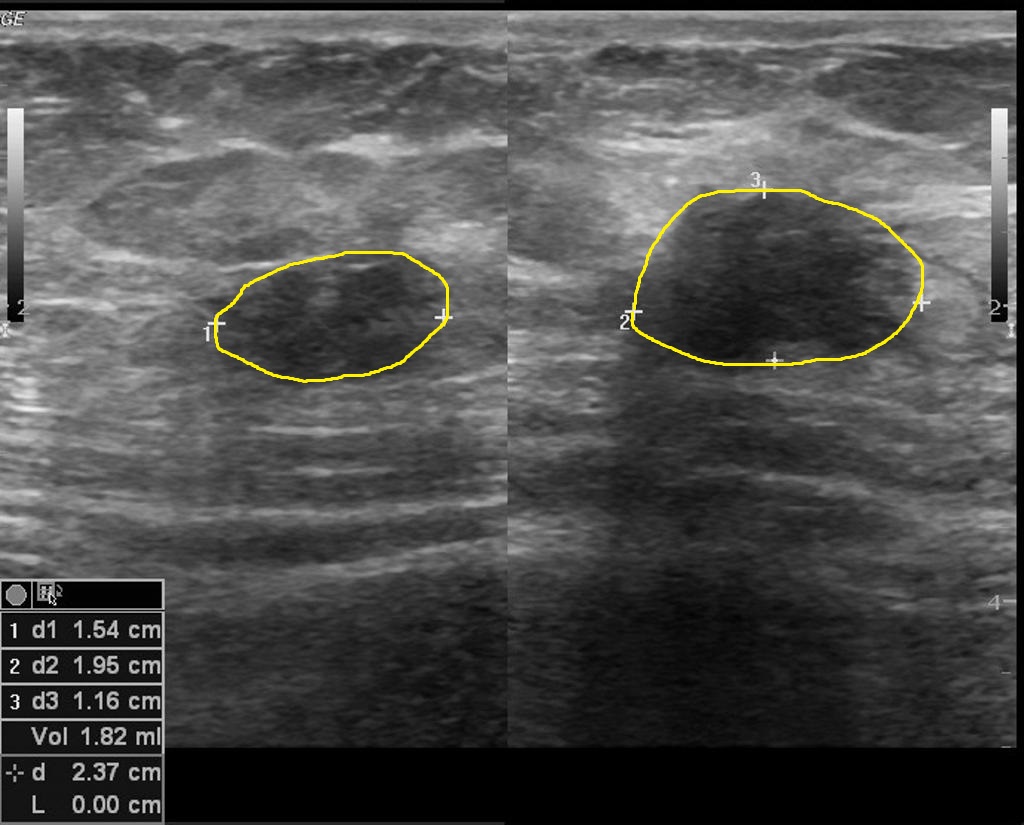
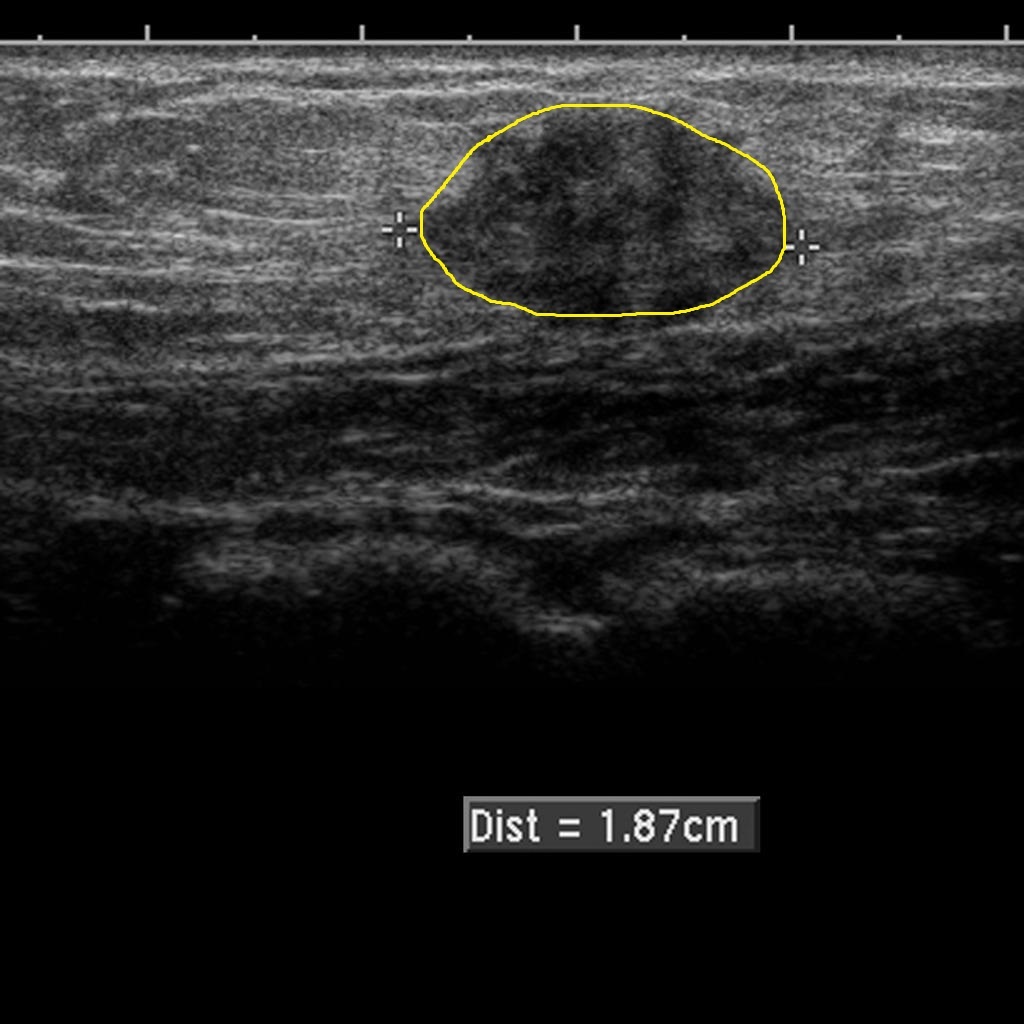
Diagnostic accuracy (transvaginal ultrasound compared with surgical visualization):
- Ovarian endometriomas: sensitivity 93% (95% CI, 87%–99%) and specificity 96% (95% CI, 92%–99%) (8 studies; n = 765).[4]
- Deep endometriosis: sensitivity 79% (95% CI, 69%–89%) (9 studies; n = 934).[4]
- Superficial peritoneal disease: sensitivity 65% (95% CI, 27%–100%).[4]
Because ultrasound does not have 100% sensitivity (particularly for superficial peritoneal lesions), absence of ultrasound findings does not exclude endometriosis.[4]
Augmented pelvic ultrasound
A Society of Radiologists in Ultrasound consensus describes “augmented pelvic ultrasound” to improve detection of deep endometriosis.[5]
Key augmented ultrasound features include:
- “Kissing ovaries,” which may suggest deep endometriosis.
- Absent uterine sliding against the rectosigmoid, which may suggest adhesions and deep endometriosis.[5]
- In a prospective observational study of 273 patients undergoing laparoscopic surgery, augmented pelvic ultrasound for deep endometriosis had sensitivity 88.4% (95% CI, 83.2%–92.4%) and specificity 78.8% (95% CI, 67.0%–87.9%).[6]
References
- ↑ Singh SS, Allaire C, Al-Nourhji O, et al. Guideline No. 449: diagnosis and impact of endometriosis—a canadian guideline. J Obstet Gynaecol Can. 2024;46(5):102450. doi:10.1016/j.jogc.2024.102450
- ↑ Grasso RF, Di Giacomo V, Sedati P, Sizzi O, Florio G, Faiella E; et al. (2010). "Diagnosis of deep infiltrating endometriosis: accuracy of magnetic resonance imaging and transvaginal 3D ultrasonography". Abdom Imaging. 35 (6): 716–25. doi:10.1007/s00261-009-9587-7. PMID 19924468.
- ↑ Dueholm M, Lundorf E (2007). "Transvaginal ultrasound or MRI for diagnosis of adenomyosis". Curr Opin Obstet Gynecol. 19 (6): 505–12. doi:10.1097/GCO.0b013e3282f1bf00. PMID 18007126.
- ↑ 4.0 4.1 4.2 4.3 Nisenblat V, Bossuyt PM, Farquhar C, Johnson N, Hull ML. Imaging modalities for the non-invasive diagnosis of endometriosis. Cochrane Database Syst Rev. 2016;2(2):CD009591. doi:10.1002/14651858.CD009591.pub2
- ↑ 5.0 5.1 Young SW, Jha P, Chamié L, et al. Society of Radiologists in Ultrasound consensus on routine pelvic US for endometriosis. Radiology. 2024;311(1):e232191. doi:10.1148/radiol.232191
- ↑ Leonardi M, Uzuner C, MestdaghW, et al. Diagnostic accuracy of transvaginal ultrasound for detection of endometriosis using International Deep Endometriosis Analysis (IDEA) approach: prospective international pilot study. Ultrasound Obstet Gynecol. 2022;60(3):404-413. doi:10.1002/uog.24936