Congenital CMV
To view the congenital infections main page Click here
|
WikiDoc Resources for Congenital CMV |
|
Articles |
|---|
|
Most recent articles on Congenital CMV Most cited articles on Congenital CMV |
|
Media |
|
Powerpoint slides on Congenital CMV |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Congenital CMV at Clinical Trials.gov Trial results on Congenital CMV Clinical Trials on Congenital CMV at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Congenital CMV NICE Guidance on Congenital CMV
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Congenital CMV Discussion groups on Congenital CMV Patient Handouts on Congenital CMV Directions to Hospitals Treating Congenital CMV Risk calculators and risk factors for Congenital CMV
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Congenital CMV |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Dima Nimri, M.D. [2]
Overview
Congenital CMV infection is the most common congenital infection worldwide. Its incidence ranges between 0.4% to 2.0% worldwide. The infection can be asymptomatic at birth, or can have severe symptoms such as microcephaly, SGA and hypotonia. One of the most common complications of congenital CMV infection is sensorineural hearing loss. There is no universal screening for pregnant women for CMV infection. Congenital CMV infection must be differentiated from other congenital infections (TORCH infections). The diagnosis is made by the typical findings on a prenatal ultrasound, along with isolation of the virus from fetal tissue. Treatment with antiviral medications improves auditory sequelae in these infants, but not the neurological outcome.
Historical Perspective
- In 1947, congenital CMV infection was described as inclusion disease of infancy.[1]
- In 1960, the term cytomegalovirus was proposed.[2]
- In 1971, prenatal diagnosis of congenital CMV was first reported by isolating CMV from amniotic fluid.[3]
Classification
Congenital CMV infection can be classified based on the initial presentation at birth:
- Asymptomatic congenital CMV infection
- Symptomatic congenital CMV infection
Pathophysiology
Pathogenesis
The pathogenesis of congenital CMV infection is largely unknown and poorly understood. However, the clinical manifestations are thought to arise as a result of direct injury to the fetal cells from CMV virus or due to decreased function of the placenta as a result of the infection.[4]
Microscopic Pathology
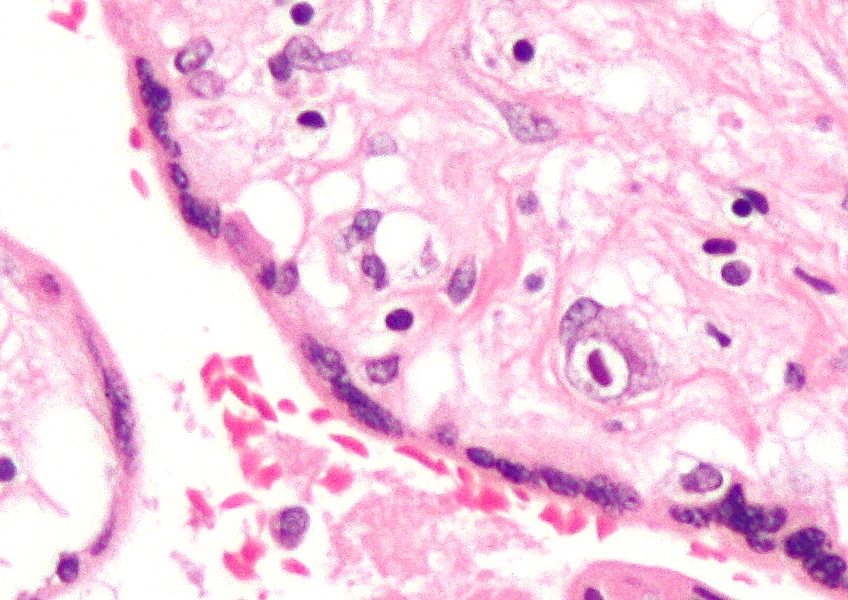
Causes
The cause of congenital CMV is cytomegalovirus. For more information about the causative agent, click here.
Differentiating Congenital CMV from Other Congenital Infections
The most important congenital infections, which can be transmitted vertically from mother to fetus are the TORCH infections. These infections have overlapping features and hence, must be differentiated from congenital CMV infection:[5]
| Congenital Infection | Cardiac Findings | Skin Findings | Ocular Findings | Hepatosplenomegaly | Hydrocephaly | Microcephaly | Intracranial Calcifications | Hearing deficits |
|---|---|---|---|---|---|---|---|---|
| Cytomegalovirus (CMV) | ✔ | ✔ | — | ✔ | Periventricular calcifications | ✔ | ||
| Toxoplasmosis | — | ✔ | ✔ | ✔ | Diffuse intracranial calcifications | — | ||
| Treponema pallidum | — | ✔ | — | — | — | — | ||
| Rubella | ✔ | ✔ | ✔ | — | ✔ | |||
| Herpes simplex virus (HSV) | ✔ | ✔ | ✔ | — | ✔ | |||
| Parvovirus B19 | ✔ | — | — | — | — |
Epidemiology and Demographics
Epidemiology
Incidence
The worldwide incidence of congenital CMV infection ranges between 400 to 2,000 per 100,000 cases.[6][7][8][9][10][11][10][12][13][14]
Demographics
Race
Congenital CMV infection is more common among non-whites.[10]
Socioeconomic Status
Congenital CMV infection is more common among low socioeconomic status.[10]
Risk Factors
Risk factors to congenital CMV infection include:[10]
- Non-white race
- Low socioeconomic status (SES)
- Maternal seroconversion during pregnancy
- Preterm delivery[15][16][17]
- NICU admission[15][16][18][19]
Screening
There are no screening recommendations for congenital CMV.[20]
Natural History, Complications and Prognosis
Natural History
Treatment of congenital CMV infection can only improve hearing outcomes. Depending of the initial presentation at birth and severity of symptoms, the natural history of the disease can have severe and debilitating long-term complications.
Complications
Common Complications
Common complications in infants with congenital CMV infection include:[21]
Less Common Complications
Less common complications of congenital CMV infection include:[21]
Prognosis
The prognosis of congenital CMV infection is usually poor with development of long-term complications, such as hearing loss and developmental delay.
History and Symptoms
Symptoms in the Mother
Mothers with primary or recurrent CMV infection are usually asymptomatic, although those with primary infection are more likely to be symptomatic than those with a recurrent infection. Signs and symptoms of CMV infection in pregnant women include:[6][22][23][24]
- Fever: elevated temperature
- Pharyngitis: sore throat
- Fatigue
- Myalgia: muscle aches
- Hepatosplenomegaly
- Cervical adenopathy
Symptoms in the Neonate
Infants with congenital CMV can be asymptomatic at birth. However, one or more of these symptoms may be present:[4][6][14][25][26][27][28][29][30]
- SGA: small size for gestational age
- Microcephaly: small head size
- Sensorineural hearing loss: inattention to sounds, which may be suggestive of deafness
- Cataracts: cloudiness of the corneas
- Petechiae and purpura: skin rash at birth
- Jaundice: yellow discoloration of skin and eyes
- Lethargy
- Poor sucking when feeding
- Hypotonia: floppiness of the baby and low muscle tone
Physical Examination
Physical examination findings in infants with congenital CMV infection include:[4][6][14][25][26][27][28][29][30]
| Organ System | Findings | Suggestive of | ||
|---|---|---|---|---|
| General Appearance | Small for gestational age (SGA) | |||
| Skin | Skin lesions of several sizes (petechiae and purpura) | Thrombocytopenic purpura | ||
| Yellow discoloration of the skin and mucous membranes | Obstructive jaundice | |||
| Eyes | Small eyes | Microphthalmia | ||
| Clouding of the corneas | Cataracts | |||
| Chorioretinitis | ||||
| Yellow discoloration of the sclera | Obstructive jaundice | |||
| Ears | Sensorineural hearing loss | |||
| Heart | Myocarditis | |||
| Abdomen | Hepatosplenomegaly (HSM) | |||
| Neurological | Small head circumference | Microcephaly | ||
| Seizures | ||||
Laboratory Investigations
Laboratory findings in infants with congenital CMV infection include:[14][21][26][30][31][32]
- Elevated liver transaminases (AST and ALT)
- Elevated levels of direct and indirect serum bilirubin
- Low platelet levels (thrombocytopenia)
Electrocardiogram
There are no ECG findings in infants with congenital CMV, unless they have associated myocarditis.
Chest X-Ray
Infants with congenital CMV have a normal chest x-ray, unless they have associated myocarditis.
CT
The following CT scan findings may be seen in patients with congenital CMV:[21][33][34][35]
- Microcephaly
- Intracerebral calcifications
- Ventriculomegaly
- Cortical atrophy
- White matter abnormalities
- Cerebellar hypoplasia
MRI
MRI findings are similar to those seen on CT scan.[21][33][34][35][36]
Echocardiography
Echocardiography findings in infants with congenital CMV may be seen if they have associated myocarditis.
Ultrasound
Prenatal Ultrasound
Various findings may be seen during a routine prenatal ultrasound in a suspected case of congenital CMV infection. However, none of these findings are specific.[6][37][38][39][40][41][42][43][44][45][46][47][48][49][50]
| Anomaly | Possible Findings |
|---|---|
| Amniotic Fluid | |
| Placenta |
|
| General Fetal |
|
| Brain |
|
| Heart | |
| Gastrointestinal/ Abdominal |
|
Other Diagnostic Studies
Serology in Mother
The following antibodies can be ordered in a pregnant woman to check the immunity status of the mother:[51]
- IgM antibodies against CMV: detection of anti-CMV IgM antibodies alone is not a reliable means for diagnosis, because there is a high false-positive rate
- IgG antibodies against CMV: IgG antibodies alone do not eliminate the potential for congenital CMV infection, as some infections can result from re-infection with a different strain of CMV, as well as reactivation of the latent virus
- IgG avidity against CMV: it is a more reliable measure to detect a primary infection, as it is a measure of antibody maturity
Isolation of the Virus in the Fetus or Infant
CMV virus can be isolated or cultured from the following:[52]
- Detection of viral DNA by PCR in amniotic fluid
- Isolation of the CMV virus by culture in amniotic fluid
- Measurement of CMV viral load in amniotic fluid or fetal blood
- Detection of CMV virus or viral antigens in newborn samples of urine or saliva
Medical Therapy
Medical therapy in infants with congenital CMV infection should only be targeted towards symptomatic patients. One of the following regimens may be followed:[53][54][55][56]
- IV Ganciclovir: should be administered to neonates with life-threatening complications. The drug is administered intravenously at a dose of 6mg/kg per dose every 12 hours. Patients are usually maintained on this drug for 2-6 weeks and can be switched to oral Valganciclovir if they are stable.
- Oral Valganciclovir: usually administered to clinically stable neonates. The drug is given at a dose of 16mg/kg every 12 hours, usually for a period of 6 months.
- Antiviral drugs are thought to improve auditory outcomes in infants with congenital CMV infection. However, they have no impact on neurological outcome.
- Antiviral drugs should not be administered to asymptomatic infants.
Surgery
There is no role for surgery in the treatment of congenital CMV.
Primary Prevention
- The following measures are recommended by the CDC to decrease the risk of congenital CMV among pregnant women or young women planning on becoming pregnant:[6]
- Thoroughly washing hands with soap and warm water after activities such as changing diapers, feeding or bathing a young child, wiping a child's nose or handling a child's toys
- Avoid sharing food, drinks or utensils with young children
- Avoid sharing a toothbrush with young children
- Avoid contact with saliva when kissing a young child
- Clean surfaces that come in contact with a child's urine and saliva
- Treatment of a pregnant woman with primary CMV infection with CMV hyperimmune globulin (HIG) has been tried, but its efficacy has not been proven.[57]
Secondary Prevention
Secondary prevention in infants with congenital CMV is aimed at long-term follow-up to detect any late-onset complications, such as developmental delay and sensorineural hearing loss. In addition, measures such as physical and occupational therapy, as well as audiology amplification should be implemented.[57]
References
- ↑ KALFAYAN B (1947). "Inclusion disease of infancy". Arch Pathol (Chic). 44 (5): 467–76. PMID 20273212.
- ↑ Congenital CMV infection https://www.kaleidahealth.org/childrens/grandrounds/pdfs/grand_Rounds_111309.pdf. Accessed on Feb 8, 2017
- ↑ Lazzarotto T, Guerra B, Spezzacatena P, Varani S, Gabrielli L, Pradelli P, Rumpianesi F, Banzi C, Bovicelli L, Landini MP (1998). "Prenatal diagnosis of congenital cytomegalovirus infection". J. Clin. Microbiol. 36 (12): 3540–4. PMC 105236. PMID 9817869.
- ↑ 4.0 4.1 4.2 McMullan BJ, Palasanthiran P, Jones CA, Hall BM, Robertson PW, Howard J, Rawlinson WD (2011). "Congenital cytomegalovirus--time to diagnosis, management and clinical sequelae in Australia: opportunities for earlier identification". Med. J. Aust. 194 (12): 625–9. PMID 21692718.
- ↑ Neu N, Duchon J, Zachariah P (2015). "TORCH infections". Clin Perinatol. 42 (1): 77–103, viii. doi:10.1016/j.clp.2014.11.001. PMID 25677998.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 Naing ZW, Scott GM, Shand A, Hamilton ST, van Zuylen WJ, Basha J, Hall B, Craig ME, Rawlinson WD (2016). "Congenital cytomegalovirus infection in pregnancy: a review of prevalence, clinical features, diagnosis and prevention". Aust N Z J Obstet Gynaecol. 56 (1): 9–18. doi:10.1111/ajo.12408. PMID 26391432.
- ↑ Balasubramaniam V, Sinniah M, Tan DS, Redzwan G, Lo'man SG (1994). "The role of cytomegalovirus (CMV) infection in congenital diseases in Malaysia". Med. J. Malaysia. 49 (2): 113–6. PMID 8090088.
- ↑ Dar L, Pati SK, Patro AR, Deorari AK, Rai S, Kant S, Broor S, Fowler KB, Britt WJ, Boppana SB (2008). "Congenital cytomegalovirus infection in a highly seropositive semi-urban population in India". Pediatr. Infect. Dis. J. 27 (9): 841–3. doi:10.1097/INF.0b013e3181723d55. PMID 18645544.
- ↑ Mussi-Pinhata MM, Yamamoto AY, Moura Brito RM, de Lima Isaac M, de Carvalho e Oliveira PF, Boppana S, Britt WJ (2009). "Birth prevalence and natural history of congenital cytomegalovirus infection in a highly seroimmune population". Clin. Infect. Dis. 49 (4): 522–8. doi:10.1086/600882. PMC 2778219. PMID 19583520.
- ↑ 10.0 10.1 10.2 10.3 10.4 Kenneson A, Cannon MJ (2007). "Review and meta-analysis of the epidemiology of congenital cytomegalovirus (CMV) infection". Rev. Med. Virol. 17 (4): 253–76. doi:10.1002/rmv.535. PMID 17579921.
- ↑ Dollard SC, Grosse SD, Ross DS (2007). "New estimates of the prevalence of neurological and sensory sequelae and mortality associated with congenital cytomegalovirus infection". Rev. Med. Virol. 17 (5): 355–63. doi:10.1002/rmv.544. PMID 17542052.
- ↑ Waters A, Jennings K, Fitzpatrick E, Coughlan S, Molloy EJ, De Gascun CF, Hall WW, Knowles SJ (2014). "Incidence of congenital cytomegalovirus infection in Ireland: implications for screening and diagnosis". J. Clin. Virol. 59 (3): 156–60. doi:10.1016/j.jcv.2013.12.007. PMID 24461765.
- ↑ Cannon MJ, Schmid DS, Hyde TB (2010). "Review of cytomegalovirus seroprevalence and demographic characteristics associated with infection". Rev. Med. Virol. 20 (4): 202–13. doi:10.1002/rmv.655. PMID 20564615.
- ↑ 14.0 14.1 14.2 14.3 Istas AS, Demmler GJ, Dobbins JG, Stewart JA (1995). "Surveillance for congenital cytomegalovirus disease: a report from the National Congenital Cytomegalovirus Disease Registry". Clin. Infect. Dis. 20 (3): 665–70. PMID 7756493.
- ↑ 15.0 15.1 Mussi-Pinhata MM, Yamamoto AY, do Carmo Rego MA, Pinto PC, da Motta MS, Calixto C (2004). "Perinatal or early-postnatal cytomegalovirus infection in preterm infants under 34 weeks gestation born to CMV-seropositive mothers within a high-seroprevalence population". J. Pediatr. 145 (5): 685–8. doi:10.1016/j.jpeds.2004.07.025. PMID 15520780.
- ↑ 16.0 16.1 Panhani S, Heinonen KM (1994). "Screening for congenital cytomegalovirus infection among preterm infants born before the 34th gestational week in Finland". Scand. J. Infect. Dis. 26 (4): 375–8. PMID 7984966.
- ↑ Yamamoto AY, Mussi-Pinhata MM, Cristina P, Pinto G, Moraes Figueiredo LT, Jorge SM (2001). "Congenital cytomegalovirus infection in preterm and full-term newborn infants from a population with a high seroprevalence rate". Pediatr. Infect. Dis. J. 20 (2): 188–92. PMID 11224840.
- ↑ Santos DV, Souza MM, Gonçalves SH, Cotta AC, Melo LA, Andrade GM, Brasileiro-Filho G (2000). "Congenital cytomegalovirus infection in a neonatal intensive care unit in brazil evaluated by PCR and association with perinatal aspects". Rev. Inst. Med. Trop. Sao Paulo. 42 (3): 129–32. PMID 10887370.
- ↑ MacDonald H, Tobin J (1978). "Congenital cytomegalovirus infection: a collaborative study on epidemiological, clinical and laboratory findings". Dev Med Child Neurol. 20 (4): 471–82. PMID 211063. Vancouver style error: initials (help)
- ↑ U.S. Preventive Services Task Force https://www.uspreventiveservicestaskforce.org/BrowseRec/Search?s=congenital+cytomegalovirus. Accessed on Feb 6, 2016
- ↑ 21.0 21.1 21.2 21.3 21.4 Boppana SB, Fowler KB, Vaid Y, Hedlund G, Stagno S, Britt WJ, Pass RF (1997). "Neuroradiographic findings in the newborn period and long-term outcome in children with symptomatic congenital cytomegalovirus infection". Pediatrics. 99 (3): 409–14. PMID 9041297.
- ↑ Stagno S, Pass RF, Cloud G, Britt WJ, Henderson RE, Walton PD, Veren DA, Page F, Alford CA (1986). "Primary cytomegalovirus infection in pregnancy. Incidence, transmission to fetus, and clinical outcome". JAMA. 256 (14): 1904–8. PMID 3020264.
- ↑ Griffiths PD, Baboonian C (1984). "A prospective study of primary cytomegalovirus infection during pregnancy: final report". Br J Obstet Gynaecol. 91 (4): 307–15. PMID 6324849.
- ↑ Nigro G, Anceschi MM, Cosmi EV (2003). "Clinical manifestations and abnormal laboratory findings in pregnant women with primary cytomegalovirus infection". BJOG. 110 (6): 572–7. PMID 12798474.
- ↑ 25.0 25.1 Boppana SB, Ross SA, Fowler KB (2013). "Congenital cytomegalovirus infection: clinical outcome". Clin. Infect. Dis. 57 Suppl 4: S178–81. doi:10.1093/cid/cit629. PMC 4471438. PMID 24257422.
- ↑ 26.0 26.1 26.2 Boppana SB, Pass RF, Britt WJ, Stagno S, Alford CA (1992). "Symptomatic congenital cytomegalovirus infection: neonatal morbidity and mortality". Pediatr. Infect. Dis. J. 11 (2): 93–9. PMID 1311066.
- ↑ 27.0 27.1 Boppana SB, Fowler KB, Britt WJ, Stagno S, Pass RF (1999). "Symptomatic congenital cytomegalovirus infection in infants born to mothers with preexisting immunity to cytomegalovirus". Pediatrics. 104 (1 Pt 1): 55–60. PMID 10390260.
- ↑ 28.0 28.1 Morita M, Morishima T, Yamazaki T, Chiba S, Kawana T (1998). "Clinical survey of congenital cytomegalovirus infection in Japan". Acta Paediatr Jpn. 40 (5): 432–6. PMID 9821701.
- ↑ 29.0 29.1 WELLER TH, HANSHAW JB (1962). "Virologic and clinical observations on cytomegalic inclusion disease". N. Engl. J. Med. 266: 1233–44. doi:10.1056/NEJM196206142662401. PMID 14040222.
- ↑ 30.0 30.1 30.2 Kylat RI, Kelly EN, Ford-Jones EL (2006). "Clinical findings and adverse outcome in neonates with symptomatic congenital cytomegalovirus (SCCMV) infection". Eur. J. Pediatr. 165 (11): 773–8. doi:10.1007/s00431-006-0172-6. PMID 16835757.
- ↑ Dreher AM, Arora N, Fowler KB, Novak Z, Britt WJ, Boppana SB, Ross SA (2014). "Spectrum of disease and outcome in children with symptomatic congenital cytomegalovirus infection". J. Pediatr. 164 (4): 855–9. doi:10.1016/j.jpeds.2013.12.007. PMC 3982912. PMID 24433826.
- ↑ Rivera LB, Boppana SB, Fowler KB, Britt WJ, Stagno S, Pass RF (2002). "Predictors of hearing loss in children with symptomatic congenital cytomegalovirus infection". Pediatrics. 110 (4): 762–7. PMID 12359792.
- ↑ 33.0 33.1 Noyola DE, Demmler GJ, Nelson CT, Griesser C, Williamson WD, Atkins JT, Rozelle J, Turcich M, Llorente AM, Sellers-Vinson S, Reynolds A, Bale JF, Gerson P, Yow MD (2001). "Early predictors of neurodevelopmental outcome in symptomatic congenital cytomegalovirus infection". J. Pediatr. 138 (3): 325–31. doi:10.1067/mpd.2001.112061. PMID 11241037.
- ↑ 34.0 34.1 Fink KR, Thapa MM, Ishak GE, Pruthi S (2010). "Neuroimaging of pediatric central nervous system cytomegalovirus infection". Radiographics. 30 (7): 1779–96. doi:10.1148/rg.307105043. PMID 21057120.
- ↑ 35.0 35.1 Alarcon A, Martinez-Biarge M, Cabañas F, Hernanz A, Quero J, Garcia-Alix A (2013). "Clinical, biochemical, and neuroimaging findings predict long-term neurodevelopmental outcome in symptomatic congenital cytomegalovirus infection". J. Pediatr. 163 (3): 828–34.e1. doi:10.1016/j.jpeds.2013.03.014. PMID 23587436.
- ↑ Capretti MG, Lanari M, Tani G, Ancora G, Sciutti R, Marsico C, Lazzarotto T, Gabrielli L, Guerra B, Corvaglia L, Faldella G (2014). "Role of cerebral ultrasound and magnetic resonance imaging in newborns with congenital cytomegalovirus infection". Brain Dev. 36 (3): 203–11. doi:10.1016/j.braindev.2013.04.001. PMID 23647916.
- ↑ Enders G, Bäder U, Lindemann L, Schalasta G, Daiminger A (2001). "Prenatal diagnosis of congenital cytomegalovirus infection in 189 pregnancies with known outcome". Prenat. Diagn. 21 (5): 362–77. doi:10.1002/pd.59. PMID 11360277.
- ↑ Twickler DM, Perlman J, Maberry MC (1993). "Congenital cytomegalovirus infection presenting as cerebral ventriculomegaly on antenatal sonography". Am J Perinatol. 10 (5): 404–6. doi:10.1055/s-2007-994773. PMID 8240605.
- ↑ Abdel-Fattah SA, Bhat A, Illanes S, Bartha JL, Carrington D (2005). "TORCH test for fetal medicine indications: only CMV is necessary in the United Kingdom". Prenat. Diagn. 25 (11): 1028–31. doi:10.1002/pd.1242. PMID 16231309.
- ↑ Guerra B, Simonazzi G, Puccetti C, Lanari M, Farina A, Lazzarotto T, Rizzo N (2008). "Ultrasound prediction of symptomatic congenital cytomegalovirus infection". Am. J. Obstet. Gynecol. 198 (4): 380.e1–7. doi:10.1016/j.ajog.2007.09.052. PMID 18191802.
- ↑ Benoist G, Salomon LJ, Jacquemard F, Daffos F, Ville Y (2008). "The prognostic value of ultrasound abnormalities and biological parameters in blood of fetuses infected with cytomegalovirus". BJOG. 115 (7): 823–9. doi:10.1111/j.1471-0528.2008.01714.x. PMID 18485159.
- ↑ Picone O, Teissier N, Cordier AG, Vauloup-Fellous C, Adle-Biassette H, Martinovic J, Senat MV, Ayoubi JM, Benachi A (2014). "Detailed in utero ultrasound description of 30 cases of congenital cytomegalovirus infection". Prenat. Diagn. 34 (6): 518–24. doi:10.1002/pd.4340. PMID 24532345.
- ↑ Azam AZ, Vial Y, Fawer CL, Zufferey J, Hohlfeld P (2001). "Prenatal diagnosis of congenital cytomegalovirus infection". Obstet Gynecol. 97 (3): 443–8. PMID 11239654.
- ↑ Liesnard C, Donner C, Brancart F, Gosselin F, Delforge ML, Rodesch F (2000). "Prenatal diagnosis of congenital cytomegalovirus infection: prospective study of 237 pregnancies at risk". Obstet Gynecol. 95 (6 Pt 1): 881–8. PMID 10831985.
- ↑ La Torre R, Nigro G, Mazzocco M, Best AM, Adler SP (2006). "Placental enlargement in women with primary maternal cytomegalovirus infection is associated with fetal and neonatal disease". Clin. Infect. Dis. 43 (8): 994–1000. doi:10.1086/507634. PMID 16983610.
- ↑ Simonazzi G, Guerra B, Bonasoni P, Pilu G, Lazzarotto T, Santini D, Rizzo N (2010). "Fetal cerebral periventricular halo at midgestation: an ultrasound finding suggestive of fetal cytomegalovirus infection". Am. J. Obstet. Gynecol. 202 (6): 599.e1–5. doi:10.1016/j.ajog.2009.12.021. PMID 20227051.
- ↑ Malinger G, Lev D, Zahalka N, Ben Aroia Z, Watemberg N, Kidron D, Sira LB, Lerman-Sagie T (2003). "Fetal cytomegalovirus infection of the brain: the spectrum of sonographic findings". AJNR Am J Neuroradiol. 24 (1): 28–32. PMID 12533323.
- ↑ Sampath V, Narendran V, Donovan EF, Stanek J, Schleiss MR (2005). "Nonimmune hydrops fetalis and fulminant fatal disease due to congenital cytomegalovirus infection in a premature infant". J Perinatol. 25 (9): 608–11. doi:10.1038/sj.jp.7211357. PMID 16123790.
- ↑ Dogan Y, Yuksel A, Kalelioglu IH, Has R, Tatli B, Yildirim A (2011). "Intracranial ultrasound abnormalities and fetal cytomegalovirus infection: report of 8 cases and review of the literature". Fetal. Diagn. Ther. 30 (2): 141–9. doi:10.1159/000330636. PMID 21952353.
- ↑ Pereira L, Petitt M, Fong A, Tsuge M, Tabata T, Fang-Hoover J, Maidji E, Zydek M, Zhou Y, Inoue N, Loghavi S, Pepkowitz S, Kauvar LM, Ogunyemi D (2014). "Intrauterine growth restriction caused by underlying congenital cytomegalovirus infection". J. Infect. Dis. 209 (10): 1573–84. doi:10.1093/infdis/jiu019. PMC 3997585. PMID 24403553.
- ↑ Bialas KM, Swamy GK, Permar SR (2015). "Perinatal cytomegalovirus and varicella zoster virus infections: epidemiology, prevention, and treatment". Clin Perinatol. 42 (1): 61–75, viii. doi:10.1016/j.clp.2014.10.006. PMC 4328139. PMID 25677997.
- ↑ Ross SA, Novak Z, Pati S, Boppana SB (2011). "Overview of the diagnosis of cytomegalovirus infection". Infect Disord Drug Targets. 11 (5): 466–74. PMC 3730495. PMID 21827433.
- ↑ Kimberlin DW, Lin CY, Sánchez PJ, Demmler GJ, Dankner W, Shelton M, Jacobs RF, Vaudry W, Pass RF, Kiell JM, Soong SJ, Whitley RJ (2003). "Effect of ganciclovir therapy on hearing in symptomatic congenital cytomegalovirus disease involving the central nervous system: a randomized, controlled trial". J. Pediatr. 143 (1): 16–25. PMID 12915819.
- ↑ Oliver SE, Cloud GA, Sánchez PJ, Demmler GJ, Dankner W, Shelton M, Jacobs RF, Vaudry W, Pass RF, Soong SJ, Whitley RJ, Kimberlin DW (2009). "Neurodevelopmental outcomes following ganciclovir therapy in symptomatic congenital cytomegalovirus infections involving the central nervous system". J. Clin. Virol. 46 Suppl 4: S22–6. doi:10.1016/j.jcv.2009.08.012. PMC 2805252. PMID 19766534.
- ↑ Acosta EP, Brundage RC, King JR, Sánchez PJ, Sood S, Agrawal V, Homans J, Jacobs RF, Lang D, Romero JR, Griffin J, Cloud G, Whitley R, Kimberlin DW (2007). "Ganciclovir population pharmacokinetics in neonates following intravenous administration of ganciclovir and oral administration of a liquid valganciclovir formulation". Clin. Pharmacol. Ther. 81 (6): 867–72. doi:10.1038/sj.clpt.6100150. PMID 17392728.
- ↑ Amir J, Wolf DG, Levy I (2010). "Treatment of symptomatic congenital cytomegalovirus infection with intravenous ganciclovir followed by long-term oral valganciclovir". Eur. J. Pediatr. 169 (9): 1061–7. doi:10.1007/s00431-010-1176-9. PMID 20232081.
- ↑ 57.0 57.1 James SH, Kimberlin DW (2016). "Advances in the prevention and treatment of congenital cytomegalovirus infection". Curr. Opin. Pediatr. 28 (1): 81–5. doi:10.1097/MOP.0000000000000305. PMC 4908547. PMID 26709686.