Alopecia areata
Template:DiseaseDisorder infobox Template:Search infobox Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Jesus Rosario Hernandez, M.D. [2]
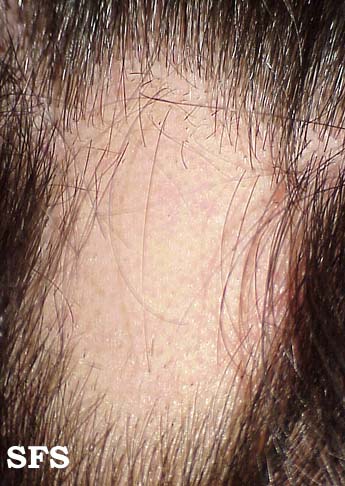
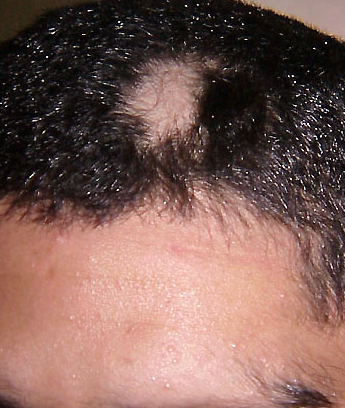
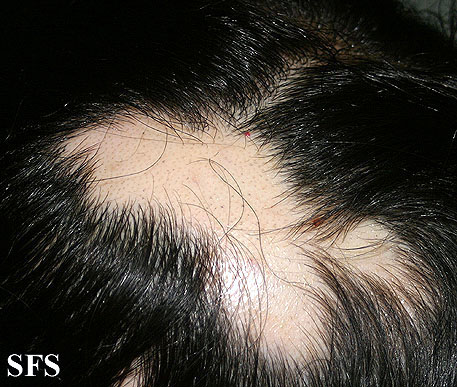
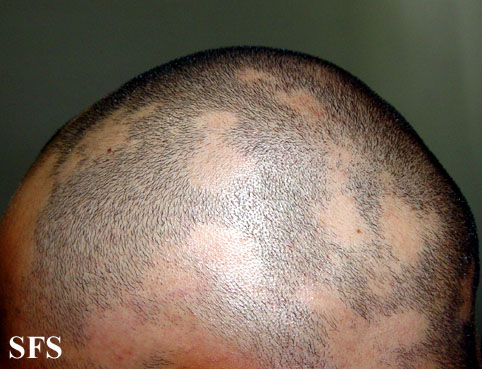
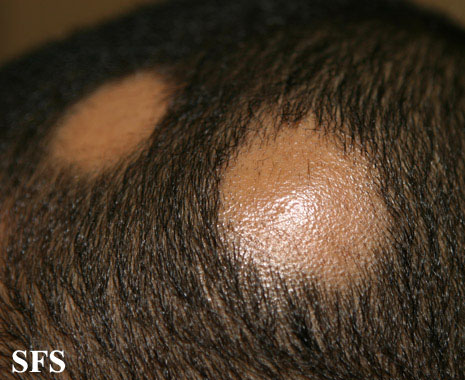
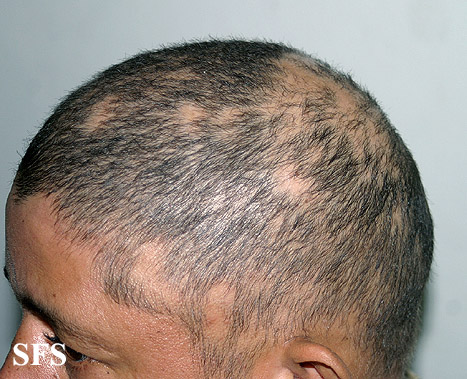
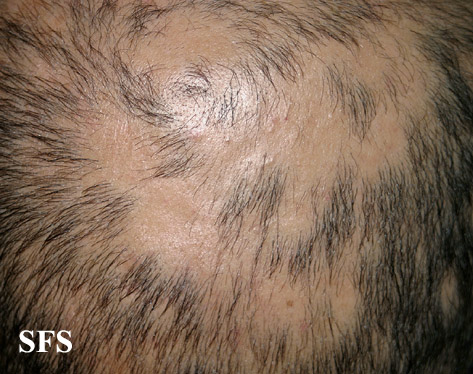
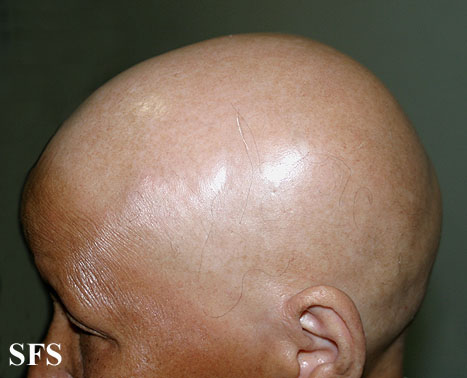
Alopecia areata (AA) is a form of hair loss from areas of the body, usually from the scalp.[1] Because it causes bald spots on the head, especially in the first stages, it is sometimes called spot baldness. In 1%–2% of cases, the condition can spread to the entire scalp (Alopecia totalis) or to the entire epidermis (Alopecia universalis).
Epidemiology
The condition affects 1%–2% of the population,[2] occurring in both males and females.[1]
Alopecia areata occurs in people who are apparently healthy and have no skin disorder.[3] Initial presentation most commonly occurs in the late teenage years, early childhood, or young adulthood, but can happen with people of all ages.[1]
Types

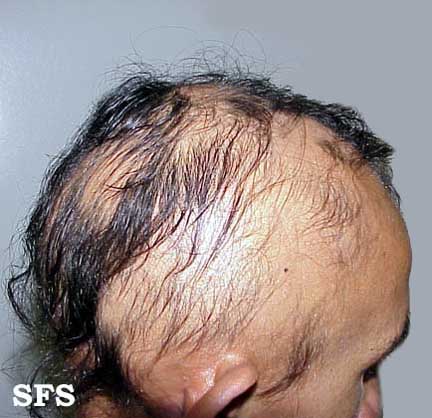
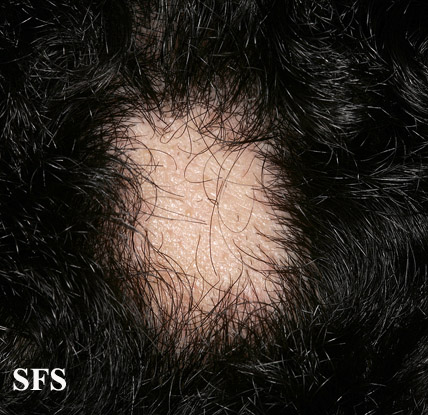
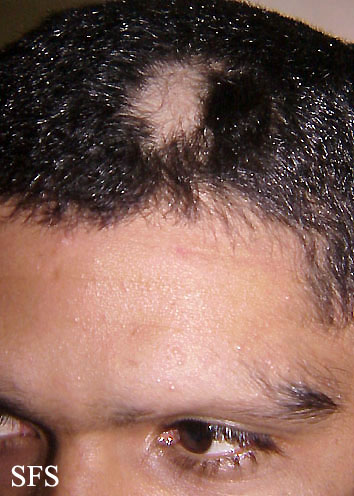
The most common type of alopecia areata occurs when hair is lost in one or more spots on the scalp.[1]
- Hair may also be lost more diffusely over the whole scalp, in which case the condition is called diffuse alopecia areata.[1]
- Alopecia areata monolocularis describes baldness in only one spot. It may occur anywhere on the head.
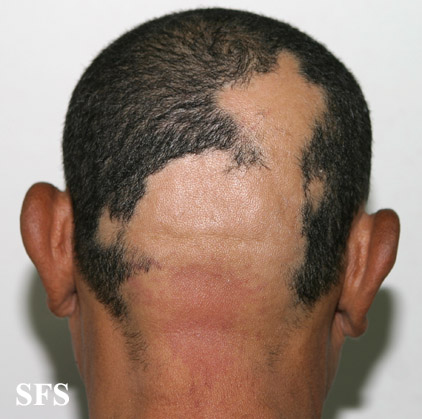
- Alopecia areata multilocularis refers to multiple areas of hair loss.
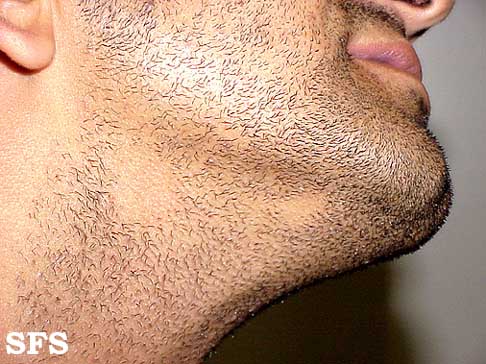
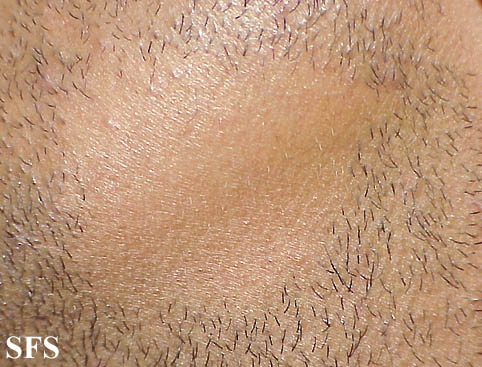
- The disease may be limited only to the beard, in which case it is called Alopecia areata barbae.[1]
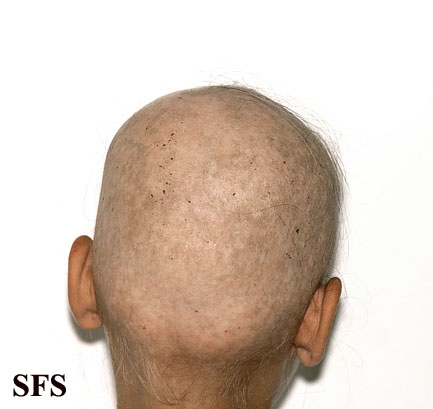
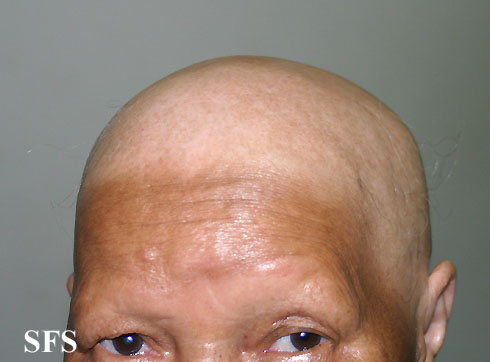
- If the patient loses all the hair on his/her scalp, the disease is then called Alopecia areata totalis.
- If all body hair, including pubic hair, is lost, the diagnosis then becomes Alopecia areata universalis.[4]
Alopecia areata totalis and universalis are rare.[4]
Causes
Alopecia areata is not contagious.[1] It occurs more frequently in people who have affected family members, suggesting that heredity may be a factor.[1] In addition, it is slightly more likely to occur in people who have relatives with autoimmune diseases.[4]
The condition is thought to be an autoimmune disorder in which the body attacks its own hair follicles and suppresses or stops hair growth.[1] There is evidence that T cell lymphocytes cluster around these follicles, causing inflammation and subsequent hair loss. An unknown environmental trigger such as emotional stress or a pathogen is thought to combine with hereditary factors to cause the condition.[3] There are a few recorded cases of babies being born with congenital alopecia areata; however, these are not cases of autoimmune disease because an infant is born without a fully developed immune system.
As with most autoimmune diseases, alopecia areata is associated with increased risk of developing other autoimmune diseases, specifically systemic lupus erythematosus or SLE.
Diagnosis
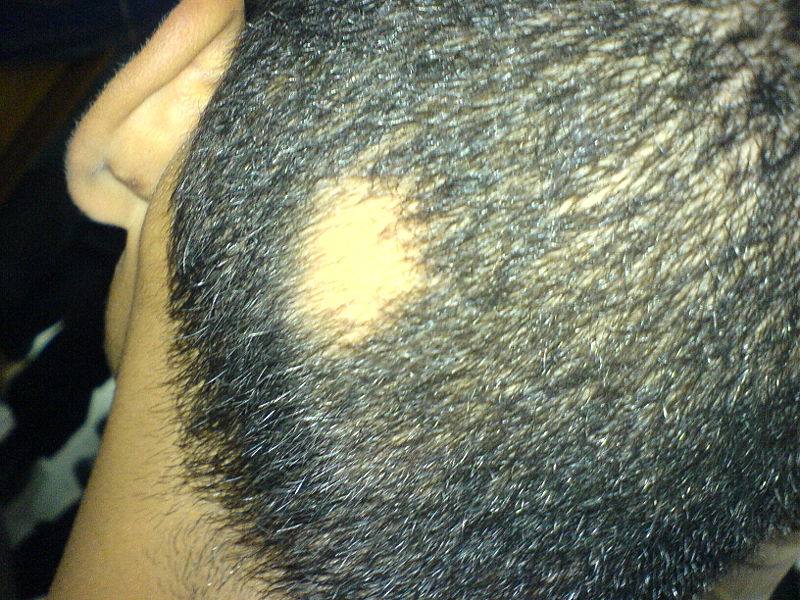
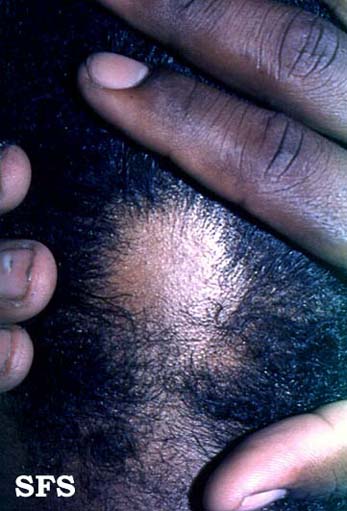
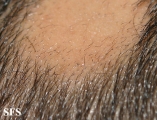
First symptoms are small, soft, bald patches which can take just about any shape but are most usually round. It most often affects the scalp and beard but may occur on any hair-bearing part of the body.[3] There may be different skin areas with hair loss and regrowth in the same body at the same time. It may also go into remission for a time, or permanently.
The area of hair loss may tingle or be very slightly painful.[5]
The hair tends to fall out over a short period of time, with the loss commonly occurring more on one side of the scalp than the other.[1]
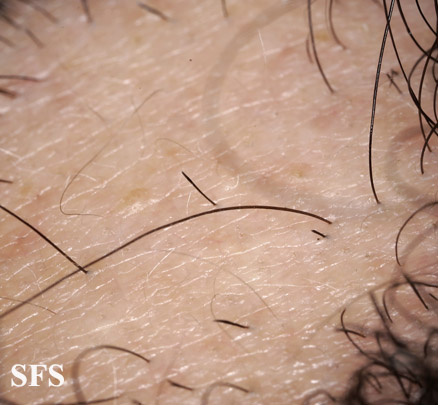
Another presentation of the condition are exclamation point hairs. Exclamation point hairs are hairs that become narrower along the length of the strand closer to the base, producing a characteristic "exclamation point" appearance.[1]
One diagnostic technique applied by medical professionals is to gently tug at a handful of hair along the edge of a patch with less strength than would be required to pull out healthy hair. In healthy hair, no hair should fall out or ripped hair should be distributed evenly across the tugged portion of the scalp. In cases of alopecia, hair will tend to pull out easier along the edge of the patch where the follicles are already being attacked by the body's immune system than away from the patch where they are still healthy. Professionals usually remind patients that the hair that is pulled out would eventually fall naturally. The test is conducted only once to identify the condition and rule out a simple localized hair loss condition.
Nails may have pitting or trachyonychia.[3]
Physical examination
Gallery
Head
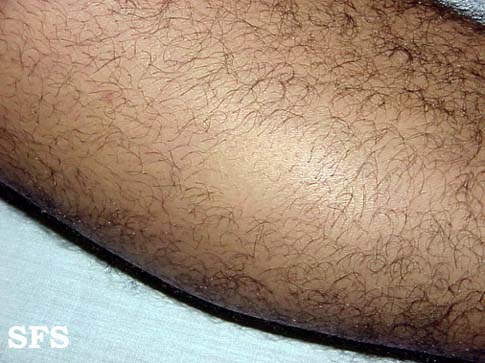
Extremities
Treatment
Since the exact mechanisms are not ultimately understood, there is no known cure to date.
About 50% of patients' hair will regrow in one year without any treatment.[1] If the affected region is small, it is reasonable to observe the progression of the illness as the problem often spontaneously regresses and the hair grows back. In 90% of cases, the hair will, ultimately, grow back. In the other 10%, only some or no hair will regrow.
In cases where there is severe hair loss, there has been limited success treating alopecia areata with clobetasol or fluocinonide, steroid injections, or cream. Steroid injections are commonly used in sites where there are small areas of hair loss on the head or especially where eyebrow hair has been lost. Some other medications used are minoxidil, irritants (anthralin or topical coal tar), and topical immunotherapy cyclosporine, each of which are sometimes used in different combinations.
Oral corticosteroids decrease the hair loss, but only for the period during which they are taken, and these drugs have adverse side effects.[3]
Initial stages may be kept from increasing by applying topical corticosteroids. However, topical corticosteroids frequently fail to enter the skin deeply enough to affect the hair bulbs, which are the treatment target.[3]
Hair implants may help covering bald spots, but cannot guarantee satisfactory outcome, since the bald areas might expand.
Wigs can be prescribed if patients, especially female patients, mention social discomfort.
Prognosis
In most cases that begin with a small number of patches of hair loss, hair grows back after a few months to a year.[5] In cases with a greater number of patches, hair can either grow back or progress to alopecia totalis or, in rare cases, universalis.[5]
Effects of alopecia areata are mainly psychological (loss of self image due to hair loss). However, patients also tend to have a slightly higher incidence of asthma, allergies, atopic dermal ailments, and even hypothyroidism. Loss of hair also means that the scalp burns more easily in the sun. Loss of nasal hair increases severity of hay fever and similar allergic conditions. Patients may also have aberrant nail formation because keratin forms both hair and nails.
Episodes of alopecia areata before puberty predispose chronic recurrence of the condition.[3] Pitting of the fingernails can hint at a more severe or prolonged course.
Hair may grow back and then fall out again later.[4]
Psychosocial issues
Alopecia can certainly be the cause of psychological stress. Because hair loss can lead to significant appearance changes, individuals may experience social phobia, anxiety, and depression. In severe cases where the chance of hair regrowth is slim, individuals need to adapt to the condition, rather than look for a cure. There is currently little provision for psychological treatment for people afflicted with alopecia.
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 Zoe Diana Draelos (August 30, 2007), Alopecia Areata. MedicineNet.com. Retrieved on December 2, 2007.
- ↑ Dudda-Subramanya R, Alexis AF, Siu K, Sinha AA (2007). "Alopecia areata: genetic complexity underlies clinical heterogeneity". European journal of dermatology : EJD. 17 (5): 367–74. doi:10.1684/ejd.2007.0231. PMID 17673378.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 Alopecia (Baldness) Merck.com. Retrieved on December 2, 2007.
- ↑ 4.0 4.1 4.2 4.3 Skin Conditions: Alopecia Areata. WebMD. Retrieved on December 2, 2007.
- ↑ 5.0 5.1 5.2 American Osteopathic College of Dermatology. Alopecia Areata. Dermatologic Disease Database. Aocd.org. Retrieved on December 3, 2007.
External links
- Template:DMOZ
- National Institute of Arthritis and Musculoskeletal and Skin Diseases at NIH
- Medical Images of Alopecia Areata
de:Haarausfall
it:Alopecia areata
lt:Židininis nuplikimas
nl:Alopecia areata
no:Alopecia areata
sv:Alopecia areata