Pre-excitation syndrome: Difference between revisions
No edit summary |
|||
| Line 37: | Line 37: | ||
=== WPW Syndrome === | === WPW Syndrome === | ||
WPW is a combination of presence of congenital accessory pathways along with episodic tachyarrhythmias. The features of pre excitation are subtle and | WPW is a combination of presence of '''congenital accessory pathways along with episodic tachyarrhythmias'''. | ||
The features of pre excitation are subtle, intermittent and are aggravated by increase in vagal tone ( Valsalva maneuver, AV blockage by drugs). | |||
* ECG Features of WPW | * ECG Features of WPW | ||
| Line 49: | Line 51: | ||
== Pathophysiology [edit | edit source] == | |||
[[File:WPW-in-SR (1).jpg|thumb|332.986x332.986px|WPW Syndrome]]Pathophysiology of Pre-Excitation syndromes | |||
*[[Pre-excitation of the ventricles|Pre-excitation]] refers to the early activation of the ventricles as a result of impulses bypassing the AV node via an accessory pathway. The latter are abnormal conduction pathways formed during cardiac development. These can conduct impulses either towards ventricles ([[Anterograde conduction]], rarely seen) , Away from the ventricles (Retrograde conduction, in approx 15%), or in both the directions ( Majority of cases). | |||
*In [[Wolff-Parkinson-White syndrome|WPW]] syndrome which is a type of pre-excitation syndrome the abnormal conduction pathways are called [[Bundle of Kent]] or AV bypass tract. These accessory pathways facilitates formation of [[Tachyarrhythmias]] by mainly forming reentry circuit , termed as <u>AVRT</u>. Even the direct conduction through the accessory pathways from A to V ( Bypassing AV node) can result in the formation of [[Tachyarrhythmia|Tachyarrhythmias]], seen most frequently in A. Fib with RVR. | |||
<br /> | |||
==== <u>Atrioventricular Reentry Tachycardia's (AVRT)</u> ==== | |||
AVRT is a form of PSVT. Reentry circuit results from the combination of signal transduction from normal conduction system and accessory pathway. | |||
* During tachyarrythmias, the accessory pathway forms part of the reentry circuit that results in the disappearance of features of tachyarrythmias.. | |||
* AVRT are further divided into | |||
** Orthodromic or Antidromic conduction based on ECG morphology and direction of formation of re-entry circuit. | |||
<br /> | |||
====== AVRT with Orthodromic Conduction ====== | |||
In this the anterograde conduction occurs via the AV node and retrograde conduction occurs via accessory pathway. | |||
ECG features of AVRT with orthodromic conduction | |||
== | * Rate usually 200 – 300 bpm | ||
* P waves may be buried in QRS complex or retrograde | |||
* QRS Complex usually <120 ms unless pre-existing bundle branch block, or rate-related aberrant conduction | |||
* QRS Alternans – phasic variation in QRS amplitude associated with AVNRT and AVRT, distinguished from electrical alternans by a normal QRS amplitude | |||
* T wave inversion common | |||
* ST segment depression | |||
<blockquote><u>Treatment of orthodromic AVRT</u>: If patient is unstable( Low BP, Altered mental state, pulmonary edema)- Synchronised DC Cardioversion. In patients who are hemodynamically stable - Vagal manoeuvers, Adenosine, CCB and DC cardioversion on if pt not responding to medical therapy.</blockquote> | |||
==== AVRT with Antidromic Conduction ==== | |||
In antidromic AVRT anterograde conduction occurs via the accessory pathway with retrograde conduction via the AV node. Much less common than orthodromic AVRT occurring in ~5% of patients with WPW. | |||
ECG features of AVRT with antidromic conduction are: | |||
* Rate usually 200 – 300 bpm. | |||
* Wide QRS complexes due to abnormal ventricular depolarisation via accessory pathway. | |||
Treatment of antidromic AVRT | |||
* AVRT with antidromic conduction results in a wide complex tachycardia which may be mistaken for Ventricular Tachycardia. | |||
* For discussion on differentiating wide complex tachycardias see here, here, and here. | |||
* Stable patients may respond to drug therapy including amiodarone, procainamide or ibutilide, but may require DC cardioversion | |||
* In a haemodynamically unstable patient urgent synchronised DC cardioversion is required. | |||
* If in doubt treat as VT | |||
---- | |||
==== Atrial Fibrillation & Atrial Flutter in WPW ==== | |||
* Atrial fibrillation can occur in up to 20% of patients with WPW. | |||
* Atrial flutter can occur in up to 7% of patients with WPW. | |||
* The accessory pathway allows for rapid conduction directly to the ventricles bypassing the AV node. | |||
* Rapid ventricular rates may result in degeneration to VT or VF. | |||
ECG features of Atrial Fibrillation in WPW are: | |||
* Rate > 200 bpm | |||
* Irregular rhythm | |||
* Wide QRS complexes due to abnormal ventricular depolarisation via accessory pathway | |||
* QRS Complexes change in shape and morphology | |||
* Axis remains stable unlike Polymorphic VT | |||
''Atrial Flutter results in the same features as AF in WPW except the rhythm is regular and may be mistaken for VT.'' | |||
Treatment of AF with WPW | |||
* | * Treatment with AV nodal blocking drugs e.g. adenosine, calcium-channel blockers, beta-blockers may increase conduction via the accessory pathway with a resultant increase in ventricular rate and possible degeneration into VT or VF | ||
* In a haemodynamically unstable patient urgent synchronised DC cardioversion is required. | |||
* Medical treatment options in a stable patient include procainamide or ibutilide, although DC cardioversion may be preferred. | |||
<br /> | <br /> | ||
Revision as of 12:58, 2 June 2020
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Please Take Over This Page and Apply to be Editor-In-Chief for this topic: There can be one or more than one Editor-In-Chief. You may also apply to be an Associate Editor-In-Chief of one of the subtopics below. Please mail us [2] to indicate your interest in serving either as an Editor-In-Chief of the entire topic or as an Associate Editor-In-Chief for a subtopic. Please be sure to attach your CV and or biographical sketch.
Overview[edit | edit source]
Pre-excitation syndrome is a condition where the the ventricles of the heart become depolarized too early, which leads to their partially premature contraction. Normally, the atria (chambers taking venous blood) and the ventriculi (chambers pro-pulsing blood towards organs) are electrically isolated, and only electrical passage exists at "atrioventricular node". In all pre-excitation syndromes, there is at least one more conductive pathway is present. Physiologically, the electrical depolarization wave 'waits' in atrioventricular node to allow atria contract before ventriculi. However, there is no such property exists in abnormal pathway, so electrical stimulus passes to ventricle by this tracts far before normal atrioventricular-his system, and ventricles are depolarized (excited) before (pre-) normal conduction system. The term pre-excitation derives from this condition.
It is usually caused by a secondary conduction pathway (other than the bundle of His)
Classification[edit | edit source]
| Type | Conduction pathway | PR interval | QRS interval | Delta wave? |
| Wolff-Parkinson-White syndrome | Bundle of Kent (atria to ventricles) | short | long | yes |
| Lown-Ganong-Levine syndrome | "James bundle" (atria to bundle of His) | short | normal | no |
| Mahaim-type | Mahaim fibers | normal | long |
WPW Syndrome
WPW is a combination of presence of congenital accessory pathways along with episodic tachyarrhythmias.
The features of pre excitation are subtle, intermittent and are aggravated by increase in vagal tone ( Valsalva maneuver, AV blockage by drugs).
- ECG Features of WPW
- Shortened PR interval (Less than 120ms)
- Delta wave – slow/slurring in the rise of initial portion of the QRS
- Widening of QRS complex
- ST Segment and T wave discordant changes – i.e. in the opposite direction to the major component of the QRS complex
- WPW is mainly categorized as type A or B.
- Type A: positive delta wave in all precordial leads with R/S > 1 in V1
- Type B: negative delta wave in leads V1 and V2
Pathophysiology [edit | edit source]
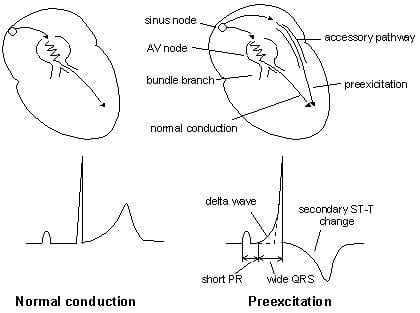
Pathophysiology of Pre-Excitation syndromes
- Pre-excitation refers to the early activation of the ventricles as a result of impulses bypassing the AV node via an accessory pathway. The latter are abnormal conduction pathways formed during cardiac development. These can conduct impulses either towards ventricles (Anterograde conduction, rarely seen) , Away from the ventricles (Retrograde conduction, in approx 15%), or in both the directions ( Majority of cases).
- In WPW syndrome which is a type of pre-excitation syndrome the abnormal conduction pathways are called Bundle of Kent or AV bypass tract. These accessory pathways facilitates formation of Tachyarrhythmias by mainly forming reentry circuit , termed as AVRT. Even the direct conduction through the accessory pathways from A to V ( Bypassing AV node) can result in the formation of Tachyarrhythmias, seen most frequently in A. Fib with RVR.
Atrioventricular Reentry Tachycardia's (AVRT)
AVRT is a form of PSVT. Reentry circuit results from the combination of signal transduction from normal conduction system and accessory pathway.
- During tachyarrythmias, the accessory pathway forms part of the reentry circuit that results in the disappearance of features of tachyarrythmias..
- AVRT are further divided into
- Orthodromic or Antidromic conduction based on ECG morphology and direction of formation of re-entry circuit.
AVRT with Orthodromic Conduction
In this the anterograde conduction occurs via the AV node and retrograde conduction occurs via accessory pathway.
ECG features of AVRT with orthodromic conduction
- Rate usually 200 – 300 bpm
- P waves may be buried in QRS complex or retrograde
- QRS Complex usually <120 ms unless pre-existing bundle branch block, or rate-related aberrant conduction
- QRS Alternans – phasic variation in QRS amplitude associated with AVNRT and AVRT, distinguished from electrical alternans by a normal QRS amplitude
- T wave inversion common
- ST segment depression
Treatment of orthodromic AVRT: If patient is unstable( Low BP, Altered mental state, pulmonary edema)- Synchronised DC Cardioversion. In patients who are hemodynamically stable - Vagal manoeuvers, Adenosine, CCB and DC cardioversion on if pt not responding to medical therapy.
AVRT with Antidromic Conduction
In antidromic AVRT anterograde conduction occurs via the accessory pathway with retrograde conduction via the AV node. Much less common than orthodromic AVRT occurring in ~5% of patients with WPW.
ECG features of AVRT with antidromic conduction are:
- Rate usually 200 – 300 bpm.
- Wide QRS complexes due to abnormal ventricular depolarisation via accessory pathway.
Treatment of antidromic AVRT
- AVRT with antidromic conduction results in a wide complex tachycardia which may be mistaken for Ventricular Tachycardia.
- For discussion on differentiating wide complex tachycardias see here, here, and here.
- Stable patients may respond to drug therapy including amiodarone, procainamide or ibutilide, but may require DC cardioversion
- In a haemodynamically unstable patient urgent synchronised DC cardioversion is required.
- If in doubt treat as VT
Atrial Fibrillation & Atrial Flutter in WPW
- Atrial fibrillation can occur in up to 20% of patients with WPW.
- Atrial flutter can occur in up to 7% of patients with WPW.
- The accessory pathway allows for rapid conduction directly to the ventricles bypassing the AV node.
- Rapid ventricular rates may result in degeneration to VT or VF.
ECG features of Atrial Fibrillation in WPW are:
- Rate > 200 bpm
- Irregular rhythm
- Wide QRS complexes due to abnormal ventricular depolarisation via accessory pathway
- QRS Complexes change in shape and morphology
- Axis remains stable unlike Polymorphic VT
Atrial Flutter results in the same features as AF in WPW except the rhythm is regular and may be mistaken for VT.
Treatment of AF with WPW
- Treatment with AV nodal blocking drugs e.g. adenosine, calcium-channel blockers, beta-blockers may increase conduction via the accessory pathway with a resultant increase in ventricular rate and possible degeneration into VT or VF
- In a haemodynamically unstable patient urgent synchronised DC cardioversion is required.
- Medical treatment options in a stable patient include procainamide or ibutilide, although DC cardioversion may be preferred.
Clinical Features[edit | edit source]
- People with Pre- Excitation syndromes are usually asymptomatic , however the individual may experience following symptoms
- Palpitations
- Dizziness or lightheadedness.
- Shortness of breath.
- Chest pain
- Fatigue.
- Anxiety.
- Fainting
- Difficulty breathing
Differentiating [disease name] from other Diseases[edit | edit source]
- Pre-Excitation syndrome must be differentiated from other diseases. The conditions that needs to be ruled out while making the diagnosis are:
- [Differential dx1]
- [Differential dx2]
- [Differential dx3]
Epidemiology and Demographics[edit | edit source]
- The prevalence of [disease name] is approximately [number or range] per 100,000 individuals worldwide.
- In [year], the incidence of [disease name] was estimated to be [number or range] cases per 100,000 individuals in [location].
Age[edit | edit source]
- Patients of all age groups may develop [disease name].
- [Disease name] is more commonly observed among patients aged [age range] years old.
- [Disease name] is more commonly observed among [elderly patients/young patients/children].
Gender[edit | edit source]
- [Disease name] affects men and women equally.
- [Gender 1] are more commonly affected with [disease name] than [gender 2].
- The [gender 1] to [Gender 2] ratio is approximately [number > 1] to 1.
Race[edit | edit source]
- There is no racial predilection for [disease name].
- [Disease name] usually affects individuals of the [race 1] race.
- [Race 2] individuals are less likely to develop [disease name].
Risk Factors[edit | edit source]
- Common risk factors in the development of [disease name] are [risk factor 1], [risk factor 2], [risk factor 3], and [risk factor 4].
Natural History, Complications and Prognosis[edit | edit source]
- The majority of patients with [disease name] remain asymptomatic for [duration/years].
- Early clinical features include [manifestation 1], [manifestation 2], and [manifestation 3].
- If left untreated, [#%] of patients with [disease name] may progress to develop [manifestation 1], [manifestation 2], and [manifestation 3].
- Common complications of [disease name] include [complication 1], [complication 2], and [complication 3].
- Prognosis is generally [excellent/good/poor], and the [1/5/10year mortality/survival rate] of patients with [disease name] is approximately [#%].
Diagnosis[edit | edit source]
Diagnostic Criteria[edit | edit source]
- The diagnosis of [disease name] is made when at least [number] of the following [number] diagnostic criteria are met:
- [criterion 1]
- [criterion 2]
- [criterion 3]
- [criterion 4]
Symptoms[edit | edit source]
- [Disease name] is usually asymptomatic.
- Symptoms of [disease name] may include the following:
- [symptom 1]
- [symptom 2]
- [symptom 3]
- [symptom 4]
- [symptom 5]
- [symptom 6]
Physical Examination[edit | edit source]
- Patients with [disease name] usually appear [general appearance].
- Physical examination may be remarkable for:
- [finding 1]
- [finding 2]
- [finding 3]
- [finding 4]
- [finding 5]
- [finding 6]
Laboratory Findings[edit | edit source]
- There are no specific laboratory findings associated with [disease name].
- A [positive/negative] [test name] is diagnostic of [disease name].
- An [elevated/reduced] concentration of [serum/blood/urinary/CSF/other] [lab test] is diagnostic of [disease name].
- Other laboratory findings consistent with the diagnosis of [disease name] include [abnormal test 1], [abnormal test 2], and [abnormal test 3].
Imaging Findings[edit | edit source]
- There are no [imaging study] findings associated with [disease name].
- [Imaging study 1] is the imaging modality of choice for [disease name].
- On [imaging study 1], [disease name] is characterized by [finding 1], [finding 2], and [finding 3].
- [Imaging study 2] may demonstrate [finding 1], [finding 2], and [finding 3].
Other Diagnostic Studies[edit | edit source]
- [Disease name] may also be diagnosed using [diagnostic study name].
- Findings on [diagnostic study name] include [finding 1], [finding 2], and [finding 3].
Treatment[edit | edit source]
Medical Therapy[edit | edit source]
- There is no treatment for [disease name]; the mainstay of therapy is supportive care.
- The mainstay of therapy for [disease name] is [medical therapy 1] and [medical therapy 2].
- [Medical therapy 1] acts by [mechanism of action 1].
- Response to [medical therapy 1] can be monitored with [test/physical finding/imaging] every [frequency/duration].
Surgery[edit | edit source]
- Surgery is the mainstay of therapy for [disease name].
- [Surgical procedure] in conjunction with [chemotherapy/radiation] is the most common approach to the treatment of [disease name].
- [Surgical procedure] can only be performed for patients with [disease stage] [disease name].
Prevention[edit | edit source]
- There are no primary preventive measures available for [disease name].
- Effective measures for the primary prevention of [disease name] include [measure1], [measure2], and [measure3].
- Once diagnosed and successfully treated, patients with [disease name] are followed-up every [duration]. Follow-up testing includes [test 1], [test 2], and [test 3].
Pre-excitation syndrome is a condition where the the ventricles of the heart become depolarized too early, which leads to their partially premature contraction. Normally, the atria (chambers taking venous blood) and the ventriculi (chambers pro-pulsing blood towards organs) are electrically isolated, and only electrical passage exists at "atrioventricular node". In all pre-excitation syndromes, there is at least one more conductive pathway is present. Physiologically, the electrical depolarization wave 'waits' in atrioventricular node to allow atria contract before ventriculi. However, there is no such property exists in abnormal pathway, so electrical stimulus passes to ventricle by this tracts far before normal atrioventricular-his system, and ventricules are depolarized (excited) before (pre-) normal conduction system. The term pre-excitation derives from this condition.
It is usually caused by a secondary conduction pathway (other than the bundle of His):
| Type | Conduction pathway | PR interval | QRS interval | Delta wave? |
| Wolff-Parkinson-White syndrome | Bundle of Kent (atria to ventricles) | short | long | yes |
| Lown-Ganong-Levine syndrome | "James bundle" (atria to bundle of His) | short | normal | no |
| Mahaim-type | Mahaim fibers | normal | long | yes |