Dysphagia causes
|
Dysphagia Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Dysphagia causes On the Web |
|
American Roentgen Ray Society Images of Dysphagia causes |
Please help WikiDoc by adding more content here. It's easy! Click here to learn about editing.
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Farman Khan, MD, MRCP [2] Kiran Singh, M.D. [3]
Overview
Life threatening causes of dysphagia include lead poisoning, rabies, and stroke. Other common causes of dysphagia include food impaction, gastroesophageal reflux, and pharyngitis.
Causes
Life Threatening Causes
Common Causes
Causes by Organ System
Causes in Alphabetical Order[1] [2]
{{columns-list|3|
- 10th cranial nerve disorder
- Aberrant subclavian artery
- Abscess
- Achalasia
- Achalasia-addisonian syndrome
- Achromatopsia
- Acoustic neuroma
- Adrenoleukodystrophy
- Aerophagia
- Agranulocytosis
- Alcoholism
- Allergic swelling
- Amyloidosis
- Amyotrophic Lateral Sclerosis
- Angina tonsillaris
- Anxiety disorders
- Aortic aneurysm
- Arizona bark scorpion poisoning
- Arnold-chiari malformation type 3
- Artemether and lumefantrin
- Aspiration of foreign body
- Autonomic nerve disorders
- Autonomic neuropathy
- Autosomal recessive spastic paraplegia, type 11
- Avellis syndrome
- Babinski–Nageotte syndrome
- Barret's syndrome
- Basal ganglia disease
- Basilar artery insufficiency syndrome
- Behcet's Syndrome
- Botulinum toxin
- Botulism
- Brainstem stroke
- Bronchial carcinoma
- Bulbar palsy
- Candidiasis
- Canomad syndrome
- Carcinoma of the vocal tract
- Carotid body tumor
- Carotid paraganglioma
- Cascade stomach
- Caustic esophagitis
- Central pontine myelinosis
- Central hypoglossal nerve paralysis
- Central vagal nucleus lesion
- Cerebellar stroke
- Cerebral palsy
- Cerebrovascular accident
- Chagas Disease
- Charge syndrome
- Chemical burns
- Chemotherapy
- Chordoma
- Chromosome 1p36 deletion syndrome
- Chromosome 22 ring
- Chromosome 22 trisomy mosaic
- Cobra poisoning
- Congenital bronchogenic cyst
- Connective tissue disease
- Crest syndrome
- Cricopharyngeal spasm
- Crisponi syndrome
- Crohn's disease of the esophagus
- Cushing's syndrome
- Cyclosporine toxicity
- Cytarabine
- Cytomegalovirus (CMV)
- Cytoplasmic body myopathy
- Dementia
- Dermatomyositis
- Diabetic neuropathy
- Diffuse esophageal spasm
- Diffuse idiopathic skeletal hyperostosis
- Diphtheria
- Distal myopathy 2
- Diverticulum
- Double aortic arch
- Dystonia
- Eagle syndrome
- Elongated styloid process
- Emanuel syndrome
- Enlarged aorta
- Enlarged left atrium
- Eosinophilic esophagitis
- Eosinophilic gastroenteritis
- Epiglottitis
- Epileptic encephalopathy, early infantile, 1
- Esophageal achalasia
- Esophageal atresia
- Esophageal cancer
- Esophageal cyst
- Esophageal Crohn's disease
- Esophageal diverticulum
- Eesophageal foreign body
- Esophageal moniliasis
- Esophageal ring
- Esophageal web
- Esophageal sarcoidosis
- Esophageal spasm
- Esophageal trauma
- Esophagotracheal fistula
- Esophageal web
- Esophagitis
- External esophageal compression
- Extreme spinal curvature
- Fibrosis
- Fluoridated toothpaste
- Food bolus
- Facial Onset Sensory Motor Neuropathy syndrome
- Franek-bocker-kahlen syndrome
- Frontotemporal dementia
- Functional disorders
- Gastric cancer
- Gastric volvulus
- Gastritis
- Gastroesophageal reflux
- Gastroparesis
- Gaucher disease
- Gastroparesis
- Global hystericus
- Globus syndrome
- Goiter
- Graft-versus-host disease
- Guillain-Barre Syndrome
- Herpangina
- Herpes simplex virus
- Hiatal hernia
- Huntington's chorea
- Huntington disease
- Hydroxocobalamin
- Hyperthyroidism
- Hypokalemia
- Hypomagnesemia primary
- Hypophosphatemia
- Hypothyroidism
- Idiopathic human immunodeficiency virus ulcers
- Impaired sensitivity in the larynx
- Inclusion body myositis
- Infantile striato-thalamic degeneration
- Infectious esophagitis
- Intramural pseudodiverticulosis
- Ixabepilone
- Laryngeal cancer
- Laryngeal papillomatosis
- Lead poisoning
- Leiomyoma
- Lhermitte-cornil-quesnel syndrome
- Lissencephaly, type 1, x-linked
- Ludwig's angina
- Lyme disease
- Lymph granulomatosis
- Lymphadenopathy
- Medication-induced esophagitis
- Metabolic encephalopathies
- Microcephaly brain defect spasticity hypernatremia
- Mitochondrial neurogastrointestinal encephalopathy syndrome
- Mitral valve stenosis
- Mononucleosis
- Motor neuron disease
- Mucositis
- Multiple Sclerosis
- Multiple system atrophy
- Mumps
- Muscular dystrophy, Duchenne and Becker type
- Myasthenia Gravis
- Congenital myasthenic syndrome
- Myoneurogastrointestinal encephalopathy syndrome
- Myopathy
- Myotonic dystrophy
- Nasopharyngeal carcinoma
- Neck cancer
- Nemaline myopathy1
- Neonatal tetanus
- Neoplastic (external compression)
- Neuroferritinopathy
- Neuroleptics
- Neurosarcoidosis
- Nutcracker esophagus
- Oculopharyngeal muscular dystrophy
- Odontoma
- Ondine's curse
- Opitz-frias syndrome
- Oral candidiasis
- Oral cavity tumor
- Oral pharyngeal disorders
- Oral submucous fibrosis
- Oropharyngeal cancer
- Osteophytes
- Palate cancer
- Palatoplegia
- Pallidopyramidal syndrome
- Paracoccidioidomycosis
- Paraganglioma
- Paraneoplastic limbic encephalitis
- Paraneoplastic syndrome
- Parkinson's Disease
- Peptic esophagitis
- Peptic stricture
- Pergolide
- Pericarditis
- Peripheral neuropathy
- Peripheral tongue paralysis
- Pharyngitis
- Pharynx cancer
- Pierre Robin syndrome
- Pill esophagitis
- Pill injury
- Pleuritis
- Plummer-Vinson Syndrome
- Polio
- Poliomyelitis
- Polyradiculitis
- Pontocerebellar hypoplasia type 2a
- Post surgery (laryngeal, esophageal, gastric)
- Post polio syndrome
- Primary lateral sclerosis, adult
- Primary motility disorders
- Pseudoachalasia
- Pseudoadrenoleukodystrophy
- Pseudobulbar paralysis
- Pyloric stenosis
- Quinsy
- Rabies
- Radiation esophagitis
- Radiation therapy
- Recent tracheotomy
- Reflux esophagitis
- Retropharyngeal abscess
- Rheumatoid Arthritis
- Riedel thyroiditis
- Riociguat
- Rumination disorder
- Sarcoidosis
- Sargramostim
- Scarlet Fever
- Schatzki ring
- Scleroderma
- Secondary motility disorders
- Sensory ataxic neuropathy, dysarthria, and ophthalmoparesis
- Shy-Drager Syndrome
- Small cell lung cancer
- Spastic paraplegia 11, autosomal recessive
- Spinal muscular atrophy type I
- Spinocerebellar ataxia 17
- Spinocerebellar ataxia 22
- Spinocerebellar ataxia, autosomal recessive 1
- Stevens-Johnson Syndrome
- Stomach cancer
- Stomatitis
- Striatonigral degeneration infantile
- Stroke
- Stuve-wiedemann dysplasia
- Subacute granulomatous thyroiditis
- Subacute thyroiditis
- Supraglottic laryngeal cancer
- Syphilis
- Syringobulbia
- Systemic Lupus Erythematosus
- Systemic sclerosis
- Tardive dyskinesia
- Tetanus
- Throat cancer
- Thyroglossal tract cyst
- Thyroid cancer, anaplastic
- Thyrotoxicosis
- Tiagabine
- Tongue cancer
- Tongue conditions
- [[The tongue is a muscular hydrostat on the floor of the mouth of most vertebrates that manipulates food for mastication. It is the primary organ of taste (gustation), as much of its upper surface is covered in taste buds. The tongue's upper surface is also covered in numerous lingual papillae. It is sensitive and kept moist by saliva, and is richly supplied with nerves and blood vessels. In humans a secondary function of the tongue is phonetic articulation. The tongue also serves as a natural means of cleaning the teeth.[3] The ability to perceive different tastes is not localised in different parts of the tongue, as is widely believed.[4] This error arose because of misinterpretation of some 19th-century research (see tongue map).
Structure
The tongue is a muscular structure that forms part of the floor of the oral cavity. The left and right sides of the tongue are separated by the lingual septum. The human tongue is divided into anterior and posterior parts. The anterior part is the visible part situated at the front and makes up roughly two-thirds the length of the tongue. The posterior part is the part closest to the throat, roughly one-third of its length. These parts differ in terms of their embryological development and nerve supply. The two parts of the tongue are divided by the terminal sulcus.[5]:989–990
The anterior tongue is, at its apex, thin and narrow, it is directed forward against the lingual surfaces of the lower incisor teeth. The posterior part is, at its root, directed backward, and connected with the hyoid bone by the hyoglossi and genioglossi muscles and the hyoglossal membrane, with the epiglottis by three folds (glossoepiglottic) of mucous membrane, with the soft palate by the glossopalatine arches, and with the pharynx by the superior pharyngeal constrictor muscle and the mucous membrane. It also forms the anterior wall of the oropharynx.
In phonetics and phonology, a distinction is made between the tip of the tongue and the blade (the portion just behind the tip). Sounds made with the tongue tip are said to be apical, while those made with the tongue blade are said to be laminal.
Muscles
The eight muscles of the human tongue are classified as either intrinsic or extrinsic. The four intrinsic muscles act to change the shape of the tongue, and are not attached to any bone. The four extrinsic muscles act to change the position of the tongue, and are anchored to bone.
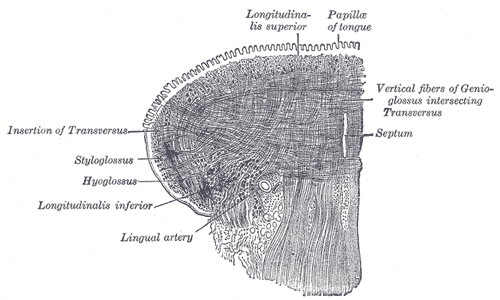
-
Coronal section of tongue, showing intrinsic muscles
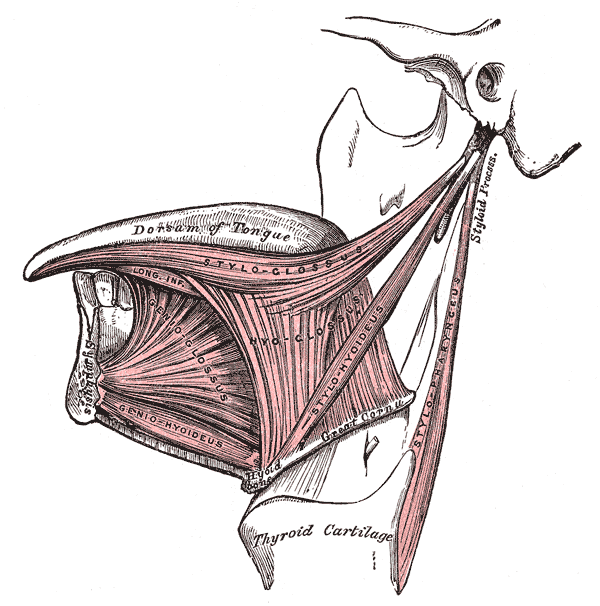
-
Lateral view of the tongue, with extrinsic muscles highlighted.
Extrinsic
The extrinsic muscles originate from bone and extend to the tongue. Their main functions are altering the tongue's position allowing for protrusion, retraction, and side-to-side movement.[5]:991
- Genioglossus, which arises from the mandible and protrudes the tongue. It is also known as the "safety muscle" of the tongue since it is the only muscle having the forward action.
- Hyoglossus, which arises from the hyoid bone and depresses the tongue
- Styloglossus, which arises from the styloid process of the temporal bone and elevates and retracts the tongue
- Palatoglossus, which arises from the palatine aponeurosis, and depresses the soft palate, moves the palatoglossal fold towards the midline, and elevates the back of the tongue.
Intrinsic
Four paired intrinsic muscles of the tongue originate and insert within the tongue, running along its length. These muscles alter the shape of the tongue by: lengthening and shortening it, curling and uncurling its apex and edges, and flattening and rounding its surface. This provides shape, and helps facilitate speech, swallowing, and eating.[5]:991
- The superior longitudinal muscle runs along the superior surface of the tongue under the mucous membrane, and elevates, assists in retraction of, or deviates the tip of the tongue. It originates near the epiglottis, the hyoid bone, from the median fibrous septum.
- The inferior longitudinal muscle lines the sides of the tongue, and is joined to the styloglossus muscle.
- The vertical muscle is located in the middle of the tongue, and joins the superior and inferior longitudinal muscles.
- The transverse muscle divides the tongue at the middle, and is attached to the mucous membranes that run along the sides.
Blood supply
The tongue receives its blood supply primarily from the lingual artery, a branch of the external carotid artery. The lingual veins, drain into the internal jugular vein. The floor of the mouth also receives its blood supply from the lingual artery.[5]:993–994 There is also a secondary blood supply to the tongue from the tonsillar branch of the facial artery and the ascending pharyngeal artery.
An area in the neck sometimes called Pirogov's triangle is formed by the intermediate tendon of the digastric muscle, the posterior border of the mylohyoid muscle, and the hypoglossal nerve.[6][7] The lingual artery is a good place to stop severe hemorrage from the tongue.
Innervation
Innervation of the tongue consists of motor fibers, special sensory fibers for taste, and general sensory fibers for sensation.[5]:994–5
- Motor supply for all intrinsic and extrinsic muscles of the tongue is supplied by efferent motor nerve fibers from the hypoglossal nerve (CN XII), with the exception of the palatoglossus. The palatoglossus is innervated by the vagus nerve (CN X).[5]:995
Innervation of taste and sensation is different for the anterior and posterior part of the tongue because they are derived from different embryological structures (pharyngeal arch 1 and pharyngeal arch 3 and 4, respectively).[8]
- Anterior two thirds of tongue (anterior to the vallate papillae):
- Taste: chorda tympani branch of the facial nerve (CN VII) via special visceral afferent fibers
- Sensation: lingual branch of the mandibular division (V3) of the trigeminal nerve (CN V) via general somatic afferent fibers
- Posterior one third of tongue:
- Taste and sensation: glossopharyngeal nerve (CN IX) via a mixture of special and general visceral afferent fibers
Histology
The tongue is covered with numerous taste buds, and filiform, fungiform, vallate and foliate, lingual papillae.[5]:990
Length
The average length of the human tongue from the oropharynx to the tip is 10cms in length.[9]
Development
The anterior tongue is derived primarily from the first pharyngeal arch. The posterior tongue is derived primarily from the third pharyngeal arch. The second arch however has a substantial contribution during fetal development, but this later atrophies. The fourth arch may also contribute, depending upon how the boundaries of the tongue are defined.
The terminal sulcus, which separates the anterior and posterior tongue, is shaped like a V, with the tip of the V situated posteriorly. At the apex is the foramen caecum, which is the point where the embryological thyroid begins to descend.[5]:990
Function
Taste
Chemicals that stimulate taste receptor cells are known as tastants. Once a tastant is dissolved in saliva, it can make contact with the plasma membrane of the gustatory hairs, which are the sites of taste transduction.[10]
The tongue is equipped with many taste buds on its dorsal surface, and each taste bud is equipped with taste receptor cells that can sense particular classes of tastes. Distinct types of taste receptor cells respectively detect substances that are sweet, bitter, salty, sour, spicy, or taste of umami.[11] Umami receptor cells are the least understood and accordingly are the type most intensively under research.[12]
Mastication
The tongue is also used for crushing food against the hard palate, during mastication. The epithelium on the tongue’s upper, or dorsal surface is keratinised. Consequently, the tongue can grind against the hard palate without being itself damaged or irritated.[13]
Swallowing
Speech
Clinical relevance
Disease
After the gums, the tongue is the second most common soft tissue site for various pathologies in the oral cavity.[medical citation needed] Examples of pathological conditions of the tongue include glossitis (e.g. geographic tongue, median rhomboid glossitis), burning mouth syndrome, oral hairy leukoplakia, oral candidiasis and squamous cell carcinoma.[14] Food debris, desquamated epithelial cells and bacteria often form a visible tongue coating.[15] This coating has been identified as a major contributing factor in bad breath (halitosis),[15] which can be managed by brushing the tongue gently with a toothbrush or using special oral hygiene instruments such as tongue scrapers or mouth brushes.[16]
Medical delivery
The sublingual region underneath the front of the tongue is a location where the oral mucosa is very thin, and underlain by a plexus of veins. This is an ideal location for introducing certain medications to the body. The sublingual route takes advantage of the highly vascular quality of the oral cavity, and allows for the speedy application of medication into the cardiovascular system, bypassing the gastrointestinal tract. This is the only convenient and efficacious route of administration (apart from I.V. administration) of nitroglycerin to a patient suffering chest pain from angina pectoris.
Society and culture
Figures of speech
The tongue can be used as a metonym for language, as in the phrase mother tongue. Many languages[17] have the same word for "tongue" and "language".
A common temporary failure in word retrieval from memory is referred to as the tip-of-the-tongue phenomenon. The expression tongue in cheek refers to a statement that is not to be taken entirely seriously – something said or done with subtle ironic or sarcastic humour. A tongue twister is a phrase made specifically to be very difficult to pronounce. Aside from being a medical condition, "tongue-tied" means being unable to say what you want to due to confusion or restriction. The phrase "cat got your tongue" refers to when a person is speechless. To "bite one's tongue" is a phrase which describes holding back an opinion to avoid causing offence. A "slip of the tongue" refers to an unintentional utterance, such as a Freudian slip. Speaking in tongues is a common phrase used to describe glossolalia, which is to make smooth, language-resembling sounds that is no true spoken language itself. A deceptive person is said to have a forked tongue, and a smooth-talking person said to have a silver tongue.
Gestures
Sticking one's tongue out at someone is considered a childish gesture of rudeness and/or defiance in many countries; the act may also have sexual connotations, depending on the way in which it is done. However, in Tibet it is considered a greeting.[18] In 2009, a farmer from Fabriano, Italy was convicted and fined by the country's highest court for sticking his tongue out at a neighbor with whom he had been arguing. Proof of the affront had been captured with a cell phone camera.[19] Blowing a raspberry can also be meant as a gesture of derision.[citation needed]
Body art
Being a cultural custom for long time, tongue piercing and splitting has become quite common in western countries in recent decades, with up to one-fifth of young adults having at least one piece of body art in the tongue.[20]
As food
The tongues of some animals are consumed and sometimes considered delicacies. Hot tongue sandwiches are frequently found on menus in Kosher delicatessens in America. Taco de lengua (lengua being Spanish for tongue) is a taco filled with beef tongue, and is especially popular in Mexican cuisine. As part of Colombian gastronomy, Tongue in Sauce (Lengua en Salsa), is a dish prepared by frying the tongue, adding tomato sauce, onions and salt. Tongue can also be prepared as birria. Pig and beef tongue are consumed in Chinese cuisine. Duck tongues are sometimes employed in Szechuan dishes, while lamb's tongue is occasionally employed in Continental and contemporary American cooking. Fried cod "tongue" is a relatively common part of fish meals in Norway and Newfoundland. In Argentina and Uruguay cow tongue is cooked and served in vinegar (lengua a la vinagreta). In the Czech Republic and Poland, a pork tongue is considered a delicacy, and there are many ways of preparing it. In Eastern Slavic countries, pork and beef tongues are commonly consumed, boiled and garnished with horseradish or jelled; beef tongues fetch a significantly higher price and are considered more of a delicacy. In Alaska, cow tongues are among the more common.
Tongues of seals and whales have been eaten, sometimes in large quantities, by sealers and whalers, and in various times and places have been sold for food on shore.[21]
History
Etymology
The word tongue derives from the Old English tunge, which comes from Proto-Germanic *tungōn.[22] It has cognates in other Germanic languages — for example tonge in West Frisian, tong in Dutch/Afrikaans, Zunge in German, tunge in Danish/Norwegian and tunga in Icelandic/Faroese/Swedish. The ue ending of the word seems to be a fourteenth-century attempt to show "proper pronunciation", but it is "neither etymological nor phonetic".[22] Some used the spelling tunge and tonge as late as the sixteenth century.
Other animals

Most vertebrate animals have tongues. In mammals such as dogs and cats, the tongue is often used to clean the fur and body. The tongues of these species have a very rough texture which allows them to remove oils and parasites. A dog's tongue also acts as a heat regulator. As a dog increases its exercise the tongue will increase in size due to greater blood flow. The tongue hangs out of the dog's mouth and the moisture on the tongue will work to cool the bloodflow.[23][24]
Some animals have tongues that are specially adapted for catching prey. For example, chameleons, frogs, and anteaters have prehensile tongues.
Many species of fish have small folds at the base of their mouths that might informally be called tongues, but they lack a muscular structure like the true tongues found in most tetrapods.[25][26]
Other animals may have organs that are analogous to tongues, such as a butterfly's proboscis or a radula on a mollusc, but these are not homologous with the tongues found in vertebrates, and often have little resemblance in function, for example, butterflies do not lick with their proboscides; they suck through them, and the proboscis is not a single organ, but two jaws held together to form a tube.[27]
Additional Images
-
The human tongue
See also
References
- ↑ Sailer, Christian, Wasner, Susanne. Differential Diagnosis Pocket. Hermosa Beach, CA: Borm Bruckmeir Publishing LLC, 2002:77 ISBN 1591032016
- ↑ Kahan, Scott, Smith, Ellen G. In A Page: Signs and Symptoms. Malden, Massachusetts: Blackwell Publishing, 2004:68 ISBN 140510368X
- ↑ Maton, Anthea; Hopkins, Jean; McLaughlin, Charles William; Johnson, Susan; Warner, Maryanna Quon; LaHart, David; Wright, Jill D. (1993). Human Biology and Health. Englewood Cliffs, New Jersey, USA: Prentice Hall. ISBN 0-13-981176-1.
- ↑ The Taste Map: All Wrong, Scientific American, March 18, 2001.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 Drake, Richard L.; Vogl, Wayne; Tibbitts, Adam W.M. Mitchell; illustrations by Richard; Richardson, Paul (2005). Gray's anatomy for students. Philadelphia: Elsevier/Churchill Livingstone. ISBN 978-0-8089-2306-0.
- ↑ Pirogov's triangle
- ↑ Jamrozik, T.; Wender, W. (January 1952). "Topographic anatomy of lingual arterial anastomoses; Pirogov-Belclard's triangle". Folia Morphologica. 3 (1): 51–62. PMID 13010300.
- ↑ PhD, Dr Ronald W. Dudek (2014). BRS Embryology (Sixth ed.). LWW. ISBN 9781451190380.
- ↑ Kerrod, Robin (1997). MacMillan's Encyclopedia of Science. 6. Macmillan Publishing Company, Inc. ISBN 0-02-864558-8.
- ↑ Tortora. Principles of Anatomy and Physiology 12th edition, chapter 17, p.602.
- ↑ Silverhorn. Human Physiology: An integrated approach 5th edition, chapter 10, p.352.
- ↑ Schacter, Daniel L., Daniel Todd. Gilbert, and Daniel M. Wegner. "Sensation and Perception." Psychology. 2nd ed. New York: Worth, 2009. 166. Print.
- ↑ Atkinson. "Anatomy for dental students 4th edition.
- ↑ Lam, L.; Logan, R. M.; Luke, C. (March 2006). "Epidemiological analysis of tongue cancer in South Australia for the 24-year period, 1977-2001". Aust Dent J. 51 (1): 16–22. doi:10.1111/j.1834-7819.2006.tb00395.x. PMID 16669472.
- ↑ 15.0 15.1 (editors) Newman MG, Takei HH, Klokkevold PR, Carranza FA (2012). Carranza's clinical periodontology (11th ed.). St. Louis, Mo.: Elsevier/Saunders. pp. 84–96. ISBN 978-1-4377-0416-7.
- ↑ Outhouse, TL; Al-Alawi, R; Fedorowicz, Z; Keenan, JV (Apr 19, 2006). "Tongue scraping for treating halitosis". The Cochrane database of systematic reviews (2): CD005519. doi:10.1002/14651858.CD005519.pub2. PMID 16625641.
- ↑ Afrikaans tong; Danish tunge; Albanian gjuha; Armenian lezu (լեզու); Greek glóssa (γλώσσα); Irish teanga; Manx çhengey; Latin and Italian lingua; Catalan llengua; French langue; Portuguese língua; Spanish lengua; Romanian limba; Bulgarian ezik (език); Polish język; Russian yazyk (язык); Czech and Slovak jazyk; Slovene, Bosnian, Croatian, and Serbian jezik; Kurdish ziman (زمان); Persian and Urdu zabān (زبان); Arabic lisān (لسان); Aramaic liššānā (ܠܫܢܐ/לשנא); Hebrew lāšon (לָשׁוֹן); Maltese ilsien; Estonian keel; Finnish kieli; Hungarian nyelv; Azerbaijani and Turkish dil; Kazakh and Khakas til (тіл)
- ↑ Bhuchung K Tsering (27 December 2007). "Tibetan culture in the 21st century". Retrieved 13 February 2012.
- ↑ Sticking out your tongue ruled illegal
- ↑ Liran, Levin; Yehuda, Zadik; Tal, Becker (December 2005). "Oral and dental complications of intra-oral piercing". Dent Traumatol. 21 (6): 341–3. doi:10.1111/j.1600-9657.2005.00395.x. PMID 16262620.
|access-date=requires|url=(help) - ↑ CHARLES BOARDMAN HAWES. Whaling. Doubleday, 1924
- ↑ 22.0 22.1 Online Etymology Dictionary
- ↑ A dog's tongue
- ↑ Krönert, H.; Pleschka, K. (January 1976). "Lingual blood flow and its hypothalamic control in the dog during panting". Pflügers Archiv European Journal of Physiology. 367 (1): 25–31. doi:10.1007/BF00583652. ISSN 0031-6768.
|access-date=requires|url=(help) - ↑ Romer, Alfred Sherwood; Parsons, Thomas S. (1977). The Vertebrate Body. Philadelphia, PA: Holt-Saunders International. pp. 298–299. ISBN 0-03-910284-X.
- ↑ Kingsley, John Sterling (1912). Comparative anatomy of vertebrates. P. Blackiston's Son & Co. pp. 217–220. ISBN 1-112-23645-7.
- ↑ Richards, O. W.; Davies, R. G. (1977). Imms' General Textbook of Entomology: Volume 1: Structure, Physiology and Development Volume 2: Classification and Biology. Berlin: Springer. ISBN 0-412-61390-5.
External links
| Wikimedia Commons has media related to tongue. |
| Wikiquote has quotations related to: Dysphagia causes |
| File:Wiktionary-logo-en-v2.svg | Look up dysphagia causes in Wiktionary, the free dictionary. |
Template:Mouth anatomy Template:Gustatory system Template:Taste
Lua error in Module:Authority_control at line 788: attempt to index field 'wikibase' (a nil value).
- Tonsillar cancer
- Tonsillar abscess
- Typhoid fever angina
- Ulcer
- Upper oesophageal sphincter dysfunction
- Vagal paraganglioma
- Vascular abnormality
- Vascular ring with right aortic arch
- Vincent's angina
- Wallenberg's syndrome
- Wiedemann–Rautenstrauch syndrome
- Wilson disease
- Zenker's Diverticulum
}}
Common Causes of Oropharyngeal Dysphagia
- A stroke can trigger a rapid onset of dysphagia with a high occurrence of aspiration. The function of normal swallowing may or may not return completely following an acute phase lasting approximately 6 weeks. [1]
- Parkinson's disease can cause "multiple prepharyngeal, pharyngeal, and esophageal abnormalities". The severity of the disease most often correlates with the severity of the swallowing disorder.[1]
- Neurologic disorders such as stroke, Parkinson's disease, amyotrophic lateral sclerosis, Bell's palsy, or myasthenia gravis can cause weakness of facial and lip muscles that are involved in coordinated mastication as well as weakness of other important muscles of mastication and swallowing.
- Oculopharyngeal muscular dystrophy is a genetic disease with palpebral ptosis, oropharyngeal dysphagia, and proximal limb weakness.
- Decrease in salivary flow, which can lead to dry mouth or xerostomia, can be due to Sjogren's syndrome, anticholinergics, antihistamines, or certain antihypertensives and can lead to incomplete processing of food bolus.
- Xerostomia can reduce the volume and increase the viscosity of oral secretions making bolus formation difficult as well as reducing the ability to initate and swallow the bolus[1]
- Dental problems can lead to inadequate chewing.
- Abnormality in oral mucosa such as from mucositis, aphthous ulcers, or herpetic lesions can interfere with bolus processing.
- Mechanical obstruction in the oropharynx may be due to malignancies, cervical rings or webs, or cervical osteophytes.
- Increased upper esophageal sphincter tone can be due to Parkinson's disease which leads to incomplete opening of the UES. This may lead to formation of a Zenker's diverticulum.
- Pharyngeal pouches typically cause difficulty in swallowing after the first mouthful of food, with regurgitation of the pouch contents. These pouches are also marked by malodorous breath due to decomposing foods residing in the pouches. (See Zenker's diverticulum)
- Dysphagia is often a side effect of surgical procedures like anterior cervical spine surgery, carotid endarterectomy, head and neck resection, oral surgeries like removal of the tongue, and parietal laryngectomies [1]
- Radiotherapy, used to treat head and neck cancer, can cause tissue fibrosis in the irradiated areas. Fibrosis of tongue and larynx lead to reduced tongue base retraction and laryngeal elevation during swallowing[1]
- Infection may cause pharyngitis which can prevent swallowing due to pain.
- Medications can cause central nervous system effects that can result in an oropharyngeal dysphagia. Examples: sedatives, hypnotic agents, anticonvulsants, antihistamines, neuroleptics, barbiturates, and antiseizure medication. Medications can also cause peripheral nervous system effects resulting in an oropharyngeal dysphagia. Examples: corticosteroids, tetracycline, L-tryptophan, and anticholinergics[1]
Common Causes of Esophageal Dysphagia
- Peptic stricture, or narrowing of the esophagus, is usually a complication of acid reflux, most commonly due to gastroesophageal reflux (GERD). These patients are usually older and have had GERD for a long time. Acid reflux can also be due to other causes, such as Zollinger-Ellison syndrome, NG tube placement, and scleroderma. Other non-acid related causes of peptic strictures include infectious esophagitis, ingestion of chemical irritant, pill irritation, and radiation. Peptic stricture is a progressive mechanical dysphagia, meaning patients will complain of initial intolerance to solids followed by inability to tolerate liquids. Usually the threshold to solid intolerance is 13 mm of the esophageal lumen. Symptoms relating to the underlying cause of the stricture usually will also be present.
- Esophageal cancer also presents with progressive mechanical dysphagia. Patients usually come with rapidly progressive dysphagia first with solids then with liquids, weight loss (> 10 kg), and anorexia (loss of appetite). Esophageal cancer usually affects the elderly. Esophageal cancers can be either squamous cell carcinoma or adenocarcinoma. Adenocarcinoma is the most prevalent in the US and is associated with patients with chronic GERD who has developed Barrett's esophagus (intestinal metaplasia of esophageal mucosa). Squamous cell carcinoma is more prevalent in Asia and is associated with tobacco smoking and alcohol use.
- Esophageal rings and webs, are actual rings and webs of tissue that may occlude the esophageal lumen.
- Rings --- Also known as Schatzki rings from the discoverer, these rings are usually mucosal rings rather than muscular rings, and are located near the gastroesophageal junction at the squamo-columnar junction. Presence of multiple rings may suggest eosinophilic esophagitis. Rings cause intermittent mechanical dysphagia, meaning patients will usually present with transient discomfort and regurgitation while swallowing solids and then liquids, depending on the constriction of the ring.
- Webs --- Usually squamous mucosal protrusion into the esophageal lumen, especially anterior cervical esophagus behind the cricoid area. Patients are usually asymptomatic or have intermittent dysphagia. An important association of esophageal webs is to the Plummer-Vinson syndrome in iron deficiency, in which case patients will also have anemia, koilonychia, fatigue, and other symptoms of anemia.
- Achalasia is an idiopathic motility disorder characterized by failure of lower esophageal sphincter (LES) relaxation as well as loss of peristalsis in the distal esophagus, which is mostly smooth muscle. Both of these features impair the ability of the esophagus to empty contents into the stomach. Patients usually complain of dysphagia to both solids and liquids. Dysphagia to liquids, in particular, is a characteristic of achalasia. Other symptoms of achalasia include regurgitation, night coughing, chest pain, weight loss, and heartburn. The combination of achalasia, adrenal insufficiency, and alacrima (lack of tear production) in children is known as the triple A (Allgrove) syndrome. In most cases the cause is unknown (idiopathic), but in some regions of the world, achalasia can also be caused by Chagas disease due to infection by Trypanosoma cruzi.
- Scleroderma is a disease characterized by atrophy and sclerosis of the gut wall, most commonly of the distal esophagus (~90%). Consequently, the lower esophageal sphincter cannot close and this can lead to severe gastroesophageal reflux disease (GERD). Patients typically present with progressive dysphagia to both solids and liquids secondary to motility problems or peptic stricture from acid reflux.
- Spastic motility disorders include diffuse esophageal spasm (DES), nutcracker esophagus, hypertensive lower esophageal sphincter, and nonspecific spastic esophageal motility disorders (NEMD).
- DES can be caused by many factors that affect muscular or neural functions, including acid reflux, stress, hot or cold food, or carbonated drinks. Patients present with intermittent dysphagia, chest pain, or heartburn.
- Diverticulum
- Aberrant subclavian artery, or (dysphagia lusoria)
- Cervical osteophytes
- Enlarged aorta
- Enlarged left atrium
- Mediastinal tumor
References
- CS1 maint: Multiple names: authors list
- CS1 maint: Extra text: authors list
- Pages using citations with accessdate and no URL
- Pages with script errors
- Pages with broken file links
- All articles with unsourced statements
- Articles with unsourced statements from July 2013
- Articles with invalid date parameter in template
- Articles with unsourced statements from September 2015
- Commons category link is locally defined
- Commons category link is on Wikidata using P373
- Sensory organs
- Gustatory system
- Tongue
- Digestive system
- Human mouth anatomy
- Crowdiagnosis
- Geriatrics
- Gastroenterology
- Otolaryngology
- Primary care