Differentiating psoriasis from other diseases: Difference between revisions
Usama Talib (talk | contribs) No edit summary |
No edit summary |
||
| Line 26: | Line 26: | ||
**[[Seborrheic dermatitis]] | **[[Seborrheic dermatitis]] | ||
{| class="wikitable" | {| class="wikitable" | ||
!Disease | !Disease | ||
!Rash Characteristics | !Rash Characteristics | ||
| Line 33: | Line 32: | ||
!Rash Appearance | !Rash Appearance | ||
|- | |- | ||
|[[Cutaneous T cell lymphoma]]/[[Mycosis fungoides]]<ref name="urlMycosis Fungoides and the Sézary Syndrome Treatment (PDQ®)—Patient Version - National Cancer Institute">{{cite web |url=https://www.cancer.gov/types/lymphoma/patient/mycosis-fungoides-treatment-pdq |title=Mycosis Fungoides and the Sézary Syndrome Treatment (PDQ®)—Patient Version - National Cancer Institute |format= |work= |accessdate=}}</ref> | |[[Cutaneous T cell lymphoma]]/[[Mycosis fungoides]]<ref name="urlMycosis Fungoides and the Sézary Syndrome Treatment (PDQ®)—Patient Version - National Cancer Institute">{{cite web |url=https://www.cancer.gov/types/lymphoma/patient/mycosis-fungoides-treatment-pdq |title=Mycosis Fungoides and the Sézary Syndrome Treatment (PDQ®)—Patient Version - National Cancer Institute |format= |work= |accessdate=}}</ref> | ||
| | | | ||
| Line 101: | Line 99: | ||
[[Image:PLEVA2.jpg|200px|courtesy http://www.regionalderm.com]] | [[Image:PLEVA2.jpg|200px|courtesy http://www.regionalderm.com]] | ||
|- | |- | ||
|[[Nummular dermatitis]]<ref name="pmid23517392">{{cite journal |vauthors=Jiamton S, Tangjaturonrusamee C, Kulthanan K |title=Clinical features and aggravating factors in nummular eczema in Thais |journal=Asian Pac. J. Allergy Immunol. |volume=31 |issue=1 |pages=36–42 |year=2013 |pmid=23517392 |doi= |url=}}</ref> | |[[Nummular dermatitis]]<ref name="pmid23517392">{{cite journal |vauthors=Jiamton S, Tangjaturonrusamee C, Kulthanan K |title=Clinical features and aggravating factors in nummular eczema in Thais |journal=Asian Pac. J. Allergy Immunol. |volume=31 |issue=1 |pages=36–42 |year=2013 |pmid=23517392 |doi= |url=}}</ref> | ||
| | | | ||
| Line 125: | Line 122: | ||
[[Image:Nummular_dermatitis_eczematous.jpg|200px]] | [[Image:Nummular_dermatitis_eczematous.jpg|200px]] | ||
|- | |- | ||
|[[Secondary syphilis]]<ref name="urlSTD Facts - Syphilis">{{cite web |url=https://www.cdc.gov/std/syphilis/stdfact-syphilis.htm |title=STD Facts - Syphilis |format= |work= |accessdate=}}</ref> | |[[Secondary syphilis]]<ref name="urlSTD Facts - Syphilis">{{cite web |url=https://www.cdc.gov/std/syphilis/stdfact-syphilis.htm |title=STD Facts - Syphilis |format= |work= |accessdate=}}</ref> | ||
| | | | ||
| Line 147: | Line 143: | ||
[[Image:Secondary_Syphilis.jpg|200px]] | [[Image:Secondary_Syphilis.jpg|200px]] | ||
|- | |- | ||
|[[Bowen’s disease]]<ref name="pmid28523295">{{cite journal |vauthors=Neagu TP, Ţigliş M, Botezatu D, Enache V, Cobilinschi CO, Vâlcea-Precup MS, GrinŢescu IM |title=Clinical, histological and therapeutic features of Bowen's disease |journal=Rom J Morphol Embryol |volume=58 |issue=1 |pages=33–40 |year=2017 |pmid=28523295 |doi= |url=}}</ref> | |[[Bowen’s disease]]<ref name="pmid28523295">{{cite journal |vauthors=Neagu TP, Ţigliş M, Botezatu D, Enache V, Cobilinschi CO, Vâlcea-Precup MS, GrinŢescu IM |title=Clinical, histological and therapeutic features of Bowen's disease |journal=Rom J Morphol Embryol |volume=58 |issue=1 |pages=33–40 |year=2017 |pmid=28523295 |doi= |url=}}</ref> | ||
| | | | ||
| Line 171: | Line 166: | ||
[[Image:Bowen.jpg|200px]] | [[Image:Bowen.jpg|200px]] | ||
|- | |- | ||
|[[Exanthematous pustulosis]]<ref name="pmid26354880">{{cite journal |vauthors=Szatkowski J, Schwartz RA |title=Acute generalized exanthematous pustulosis (AGEP): A review and update |journal=J. Am. Acad. Dermatol. |volume=73 |issue=5 |pages=843–8 |year=2015 |pmid=26354880 |doi=10.1016/j.jaad.2015.07.017 |url=}}</ref> | |[[Exanthematous pustulosis]]<ref name="pmid26354880">{{cite journal |vauthors=Szatkowski J, Schwartz RA |title=Acute generalized exanthematous pustulosis (AGEP): A review and update |journal=J. Am. Acad. Dermatol. |volume=73 |issue=5 |pages=843–8 |year=2015 |pmid=26354880 |doi=10.1016/j.jaad.2015.07.017 |url=}}</ref> | ||
| | | | ||
| Line 188: | Line 182: | ||
[[Image:Acute_generalized_exanthematous_pustulosis.jpg|200px]] | [[Image:Acute_generalized_exanthematous_pustulosis.jpg|200px]] | ||
|- | |- | ||
|[[Lichen planus|Hypertrophic lichen planus]]<ref name="pmid27222766">{{cite journal |vauthors=Ankad BS, Beergouder SL |title=Hypertrophic lichen planus versus prurigo nodularis: a dermoscopic perspective |journal=Dermatol Pract Concept |volume=6 |issue=2 |pages=9–15 |year=2016 |pmid=27222766 |pmc=4866621 |doi=10.5826/dpc.0602a03 |url=}}</ref> | |[[Lichen planus|Hypertrophic lichen planus]]<ref name="pmid27222766">{{cite journal |vauthors=Ankad BS, Beergouder SL |title=Hypertrophic lichen planus versus prurigo nodularis: a dermoscopic perspective |journal=Dermatol Pract Concept |volume=6 |issue=2 |pages=9–15 |year=2016 |pmid=27222766 |pmc=4866621 |doi=10.5826/dpc.0602a03 |url=}}</ref> | ||
| | | | ||
| Line 202: | Line 195: | ||
[[Image:Lichen_planus2.JPG|200px]] | [[Image:Lichen_planus2.JPG|200px]] | ||
|- | |- | ||
|Sneddon–Wilkinson disease<ref name="pmid9564592">{{cite journal |vauthors=Lutz ME, Daoud MS, McEvoy MT, Gibson LE |title=Subcorneal pustular dermatosis: a clinical study of ten patients |journal=Cutis |volume=61 |issue=4 |pages=203–8 |year=1998 |pmid=9564592 |doi= |url=}}</ref> | |Sneddon–Wilkinson disease<ref name="pmid9564592">{{cite journal |vauthors=Lutz ME, Daoud MS, McEvoy MT, Gibson LE |title=Subcorneal pustular dermatosis: a clinical study of ten patients |journal=Cutis |volume=61 |issue=4 |pages=203–8 |year=1998 |pmid=9564592 |doi= |url=}}</ref> | ||
| | | | ||
| Line 219: | Line 211: | ||
[[Image:Snedden.jpg|200px]] | [[Image:Snedden.jpg|200px]] | ||
|- | |- | ||
|[[Parapsoriasis|Small plaque parapsoriasis]]<ref name="pmid7026622">{{cite journal |vauthors=Lambert WC, Everett MA |title=The nosology of parapsoriasis |journal=J. Am. Acad. Dermatol. |volume=5 |issue=4 |pages=373–95 |year=1981 |pmid=7026622 |doi= |url=}}</ref> | |[[Parapsoriasis|Small plaque parapsoriasis]]<ref name="pmid7026622">{{cite journal |vauthors=Lambert WC, Everett MA |title=The nosology of parapsoriasis |journal=J. Am. Acad. Dermatol. |volume=5 |issue=4 |pages=373–95 |year=1981 |pmid=7026622 |doi= |url=}}</ref> | ||
| | | | ||
| Line 233: | Line 224: | ||
[[Image:Small_plaque_parapsoriasis.jpg|200px|courtesy http://www.regionalderm.com]] | [[Image:Small_plaque_parapsoriasis.jpg|200px|courtesy http://www.regionalderm.com]] | ||
|- | |- | ||
|[[Intertrigo]]<ref name="pmid16156342">{{cite journal |vauthors=Janniger CK, Schwartz RA, Szepietowski JC, Reich A |title=Intertrigo and common secondary skin infections |journal=Am Fam Physician |volume=72 |issue=5 |pages=833–8 |year=2005 |pmid=16156342 |doi= |url=}}</ref> | |[[Intertrigo]]<ref name="pmid16156342">{{cite journal |vauthors=Janniger CK, Schwartz RA, Szepietowski JC, Reich A |title=Intertrigo and common secondary skin infections |journal=Am Fam Physician |volume=72 |issue=5 |pages=833–8 |year=2005 |pmid=16156342 |doi= |url=}}</ref> | ||
| | | | ||
| Line 252: | Line 242: | ||
[[Image:Axillary_intertrigo.png|200px]] | [[Image:Axillary_intertrigo.png|200px]] | ||
|- | |- | ||
|[[Langerhans cell histiocytosis]]<ref name="pmid18577030">{{cite journal |vauthors=Satter EK, High WA |title=Langerhans cell histiocytosis: a review of the current recommendations of the Histiocyte Society |journal=Pediatr Dermatol |volume=25 |issue=3 |pages=291–5 |year=2008 |pmid=18577030 |doi=10.1111/j.1525-1470.2008.00669.x |url=}}</ref> | |[[Langerhans cell histiocytosis]]<ref name="pmid18577030">{{cite journal |vauthors=Satter EK, High WA |title=Langerhans cell histiocytosis: a review of the current recommendations of the Histiocyte Society |journal=Pediatr Dermatol |volume=25 |issue=3 |pages=291–5 |year=2008 |pmid=18577030 |doi=10.1111/j.1525-1470.2008.00669.x |url=}}</ref> | ||
| | | | ||
| Line 269: | Line 258: | ||
[[Image:Langerhan_cell_histiocytosis.jpg|200px|courtesy http://www.regionalderm.com ]] | [[Image:Langerhan_cell_histiocytosis.jpg|200px|courtesy http://www.regionalderm.com ]] | ||
|- | |- | ||
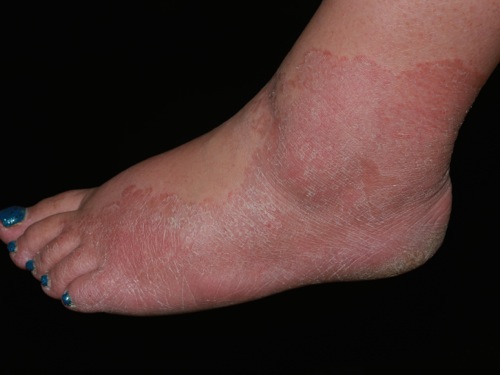
|[[Tinea manuum]]/pedum/capitis<ref name="pmid15050029">{{cite journal |vauthors=Al Hasan M, Fitzgerald SM, Saoudian M, Krishnaswamy G |title=Dermatology for the practicing allergist: Tinea pedis and its complications |journal=Clin Mol Allergy |volume=2 |issue=1 |pages=5 |year=2004 |pmid=15050029 |pmc=419368 |doi=10.1186/1476-7961-2-5 |url=}}</ref> | |[[Tinea manuum]]/pedum/capitis<ref name="pmid15050029">{{cite journal |vauthors=Al Hasan M, Fitzgerald SM, Saoudian M, Krishnaswamy G |title=Dermatology for the practicing allergist: Tinea pedis and its complications |journal=Clin Mol Allergy |volume=2 |issue=1 |pages=5 |year=2004 |pmid=15050029 |pmc=419368 |doi=10.1186/1476-7961-2-5 |url=}}</ref> | ||
| | | | ||
| Line 286: | Line 274: | ||
[[Image:Tinea_pedis.jpg|200px]] | [[Image:Tinea_pedis.jpg|200px]] | ||
|- | |- | ||
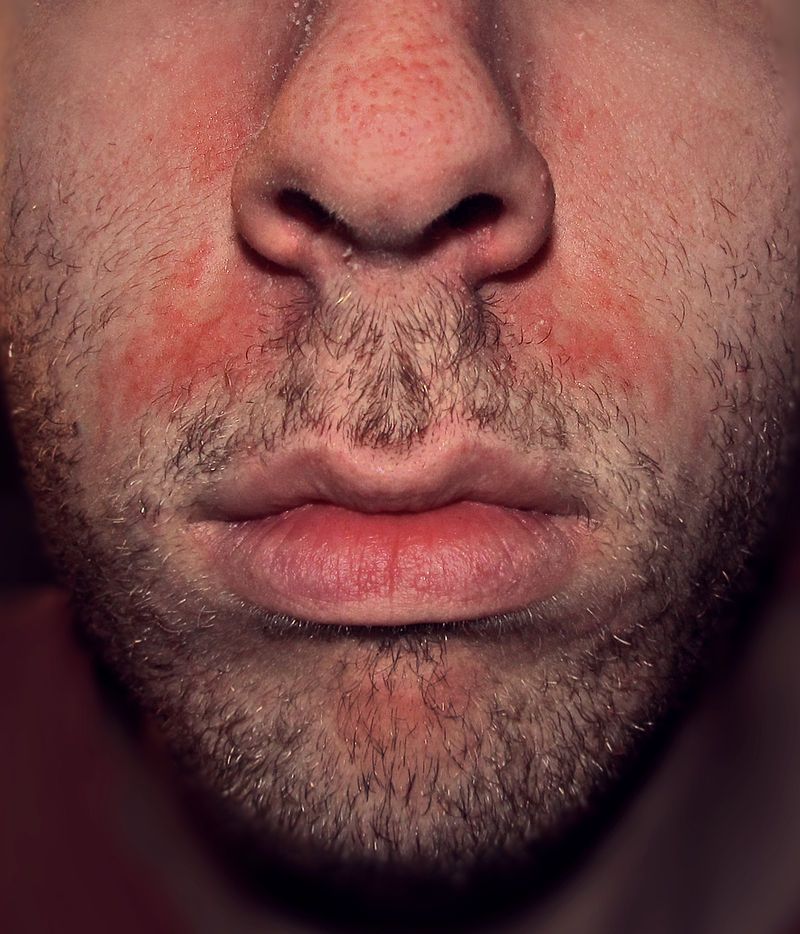
|[[Seborrheic dermatitis]] | |[[Seborrheic dermatitis]] | ||
| | | | ||
Revision as of 01:35, 2 July 2017
|
Psoriasis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Differentiating psoriasis from other diseases On the Web |
|
American Roentgen Ray Society Images of Differentiating psoriasis from other diseases |
|
Risk calculators and risk factors for Differentiating psoriasis from other diseases |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Syed Hassan A. Kazmi BSc, MD [2]
Overview
Psoriasis must be differentiated from other diseases that cause erythematous, scaly rash such as Cutaneous T cell lymphoma/mycosis fungoides, pityriasis rosea, pityriasis rubra pilaris, pityriasis lichenoides chronica, nummular dermatitis, secondary syphilis, bowen’s disease, exanthematous pustulosis, hypertrophic lichen planus, Sneddon–Wilkinson disease, small plaque parapsoriasis, intertrigo, langerhans cell histiocytosis, dyshidrotic dermatitis, tinea manuum/pedum/capitis and seborrheic dermatitis.
Differentiating Psoriasis from other Diseases
- Psoriasis must be differentiated from other diseases causing papulosquamous or erythematosquamous rash especially when the psoriatic lesions are localized in particular sites for example, palms, soles, scalp, body folds, penis and nails.
- The differentials include:
- Cutaneous T cell lymphoma/mycosis fungoides
- Pityriasis rosea
- Pityriasis rubra pilaris
- Pityriasis lichenoides chronica
- Nummular dermatitis
- Secondary syphilis
- Bowen’s disease
- Exanthematous pustulosis
- Hypertrophic lichen planus
- Sneddon–Wilkinson disease
- Small plaque parapsoriasis
- Intertrigo
- Langerhans cell histiocytosis
- Dyshidrotic dermatitis
- Tinea manuum/pedum/capitis
- Seborrheic dermatitis
| Disease | Rash Characteristics | Signs and Symptoms | Associated Conditions | Rash Appearance |
|---|---|---|---|---|
| Cutaneous T cell lymphoma/Mycosis fungoides[1] |
|
|
|
|
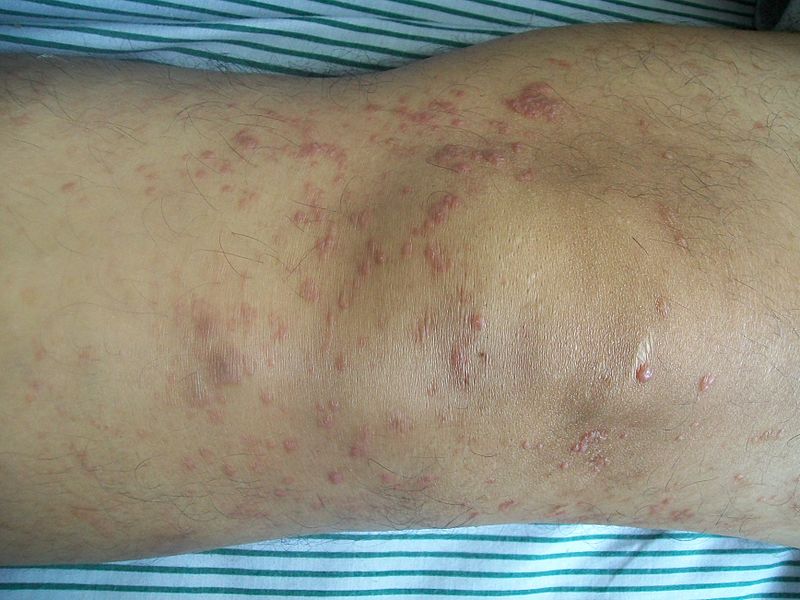
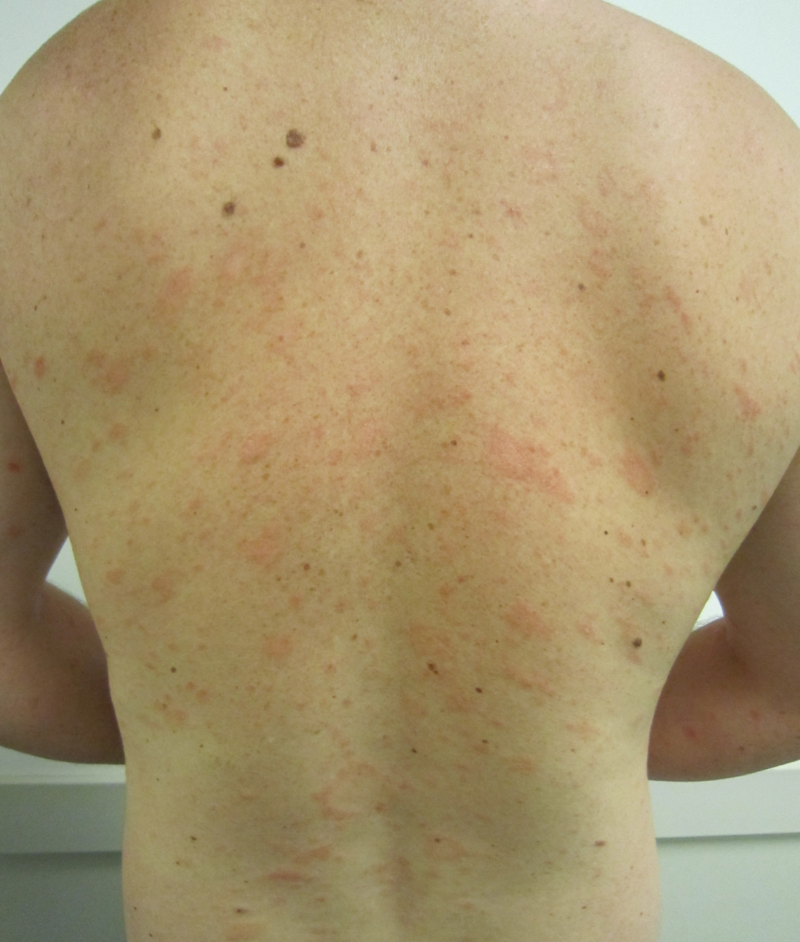
| Pityriasis rosea[2] |
|
|
||
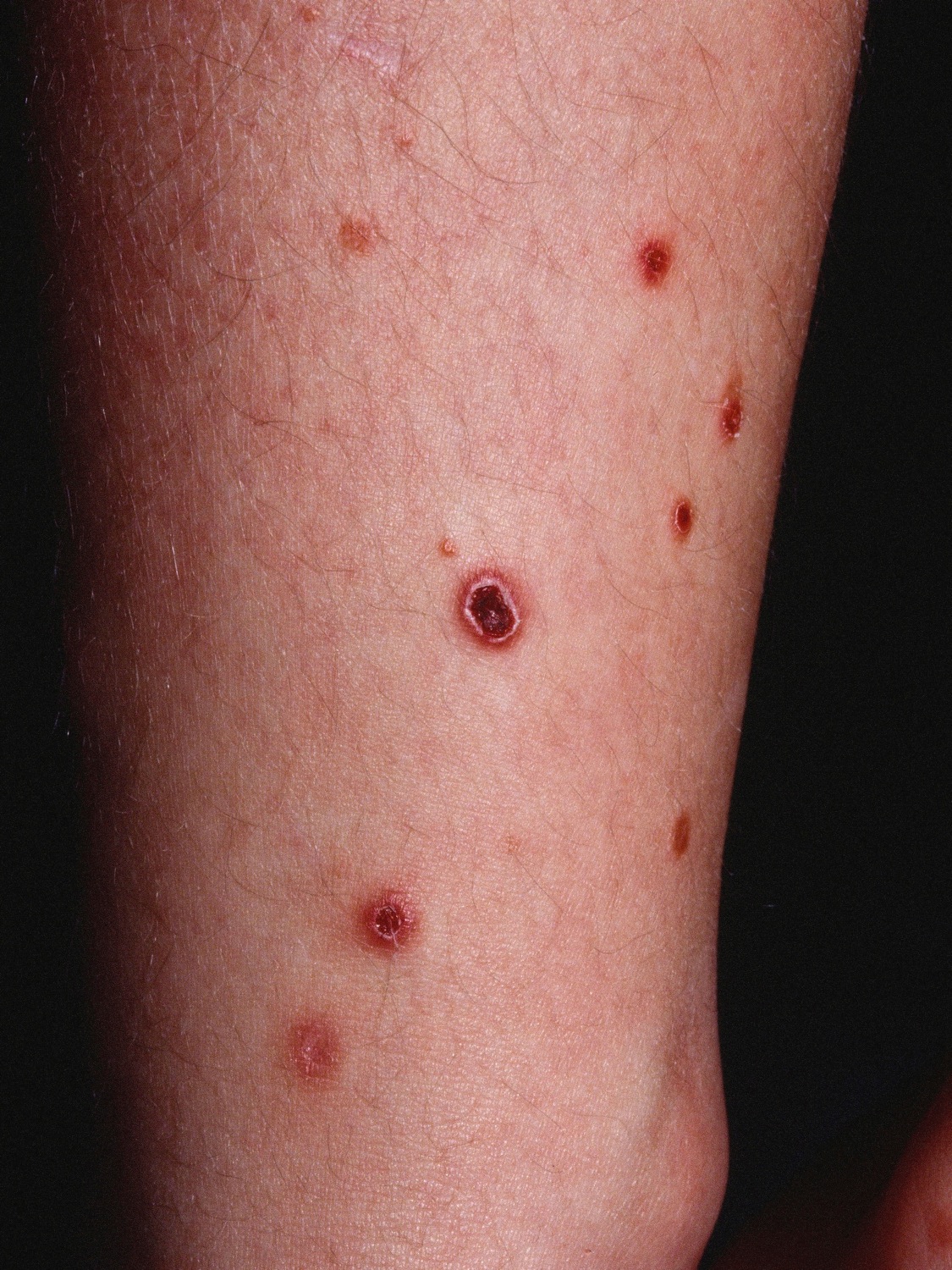
| Pityriasis lichenoides chronica |
|
|
||
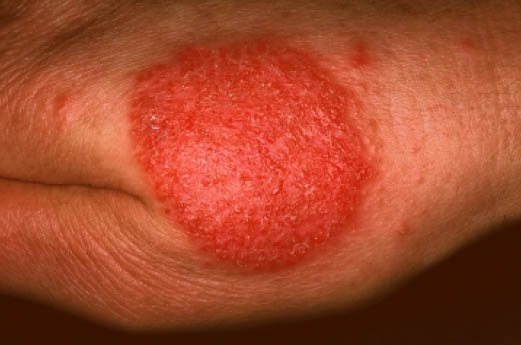
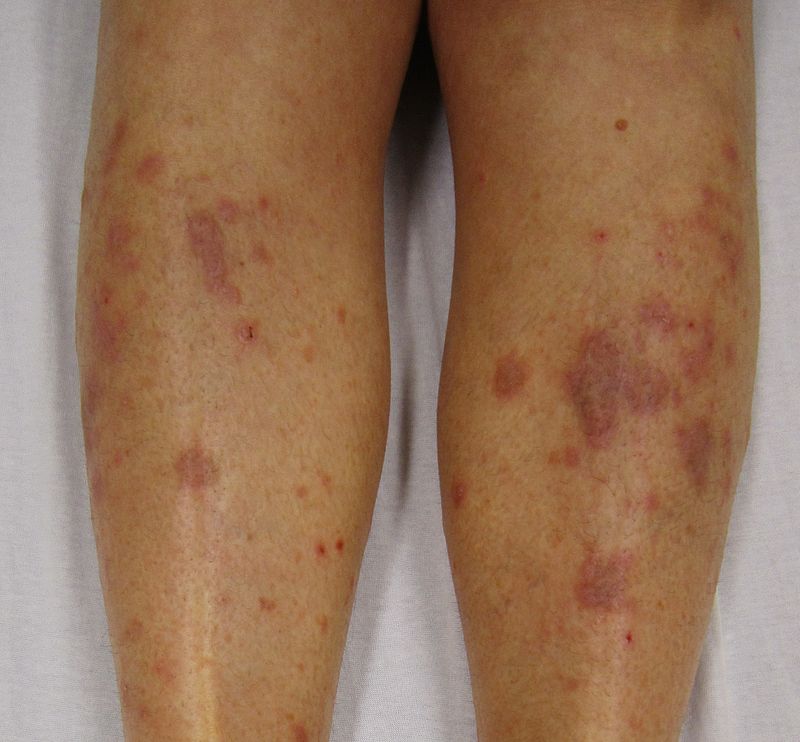
| Nummular dermatitis[5] |
|
|
|
|
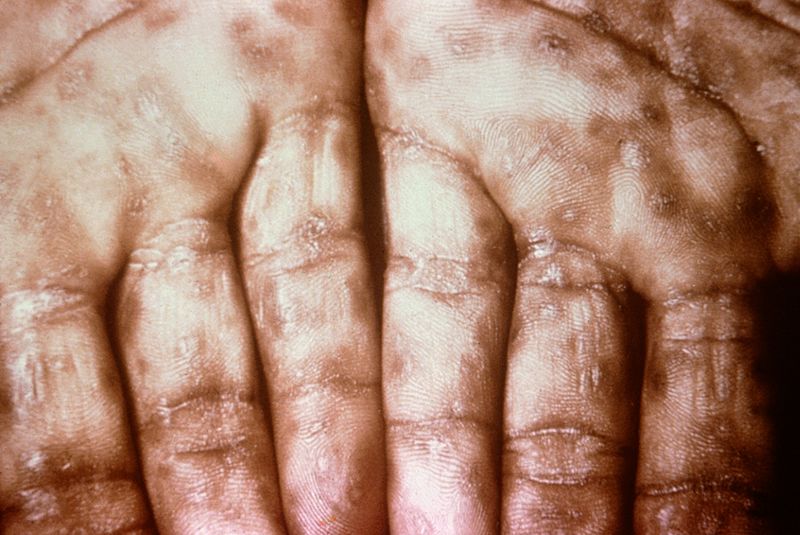
| Secondary syphilis[6] |
|
|
|
|
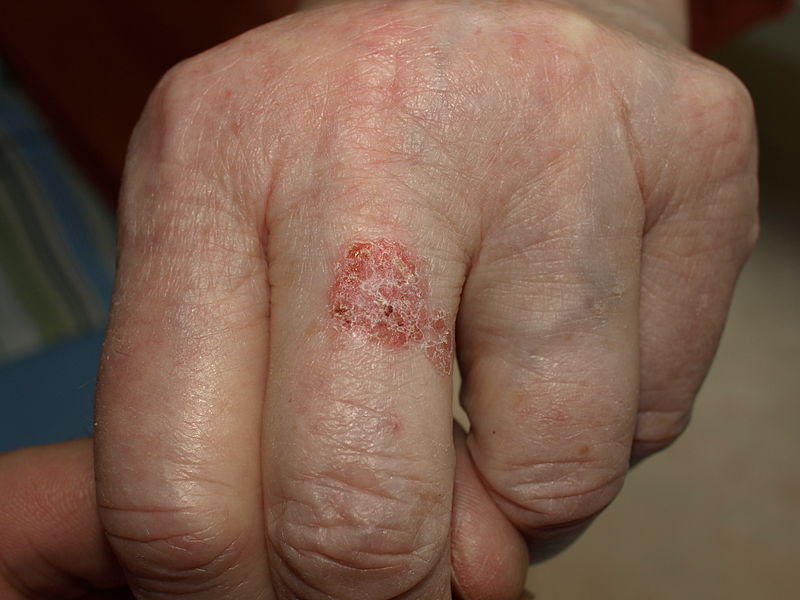
| Bowen’s disease[7] |
|
|
|
|
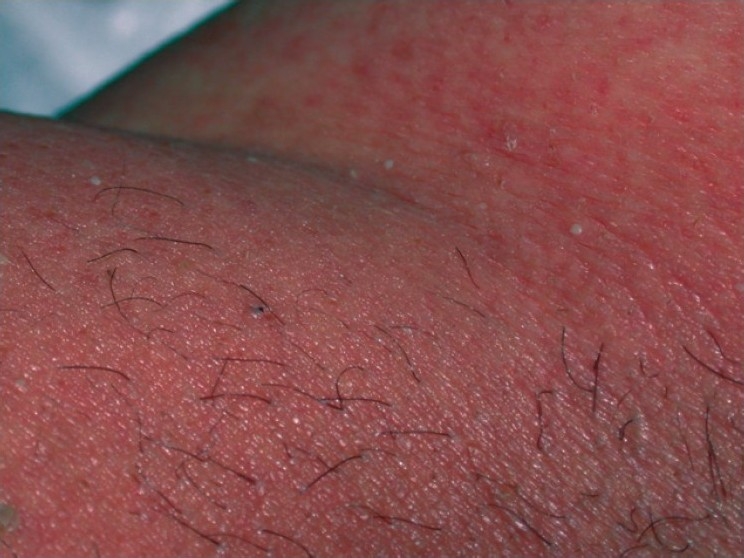
| Exanthematous pustulosis[9] |
|
|
||
| Hypertrophic lichen planus[11] |
|
|
|
|
| Sneddon–Wilkinson disease[13] |
|
|
||
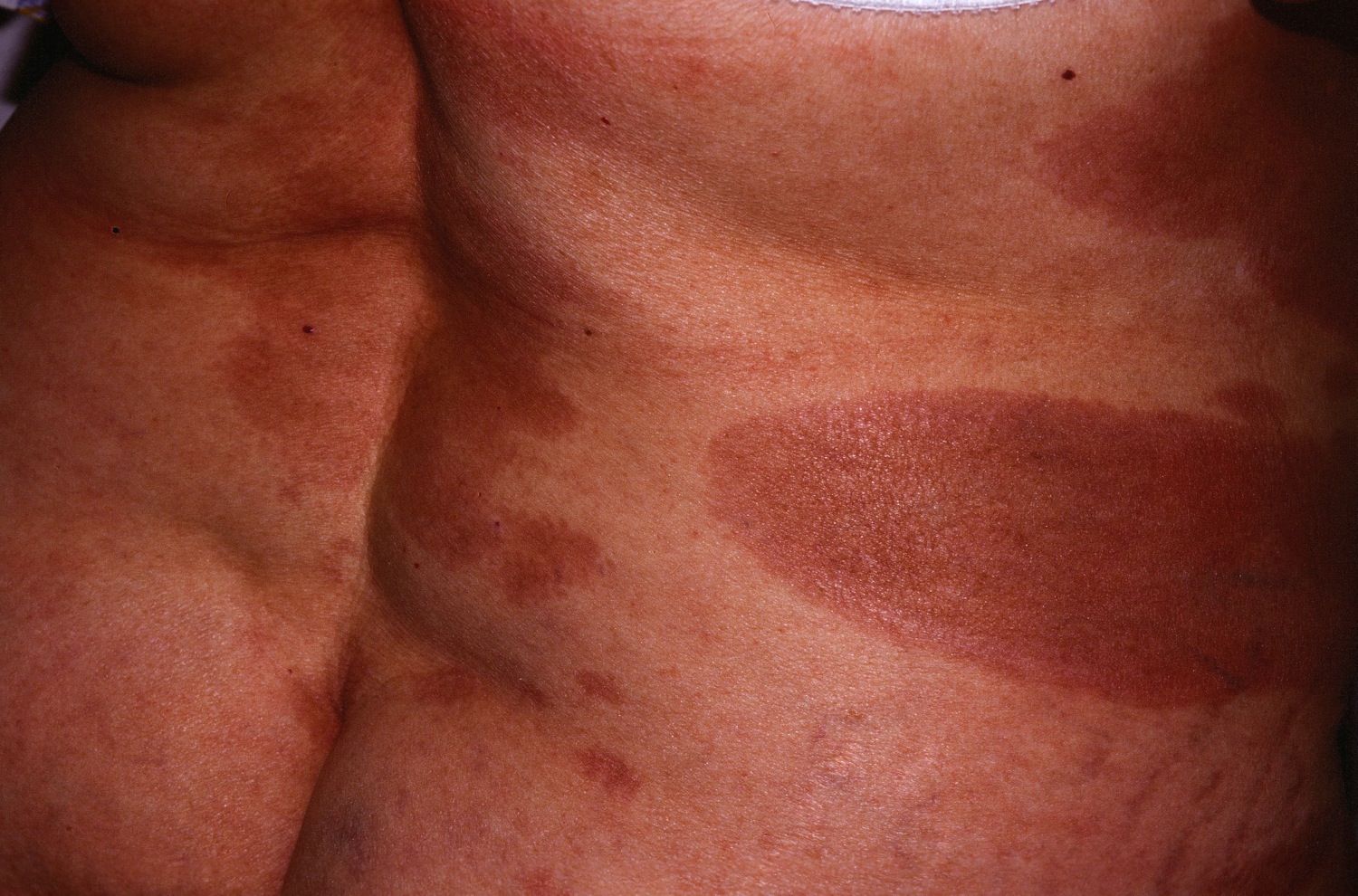
| Small plaque parapsoriasis[17] |
|
|
|
|
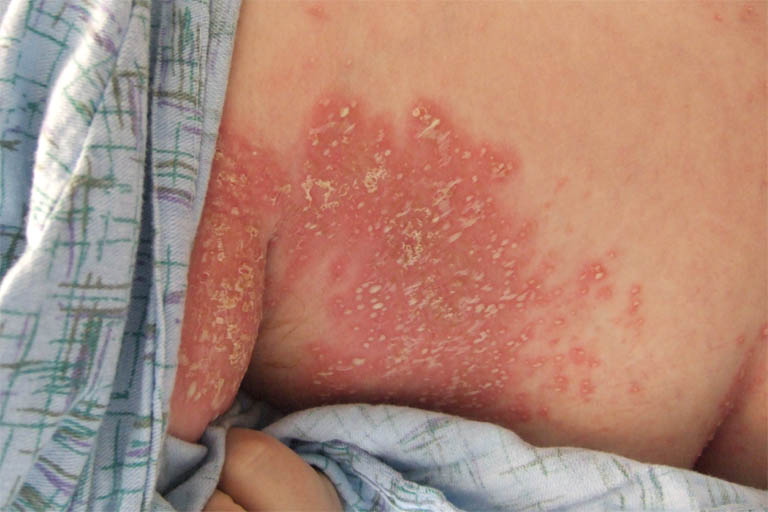
| Intertrigo[19] |
|
|
||
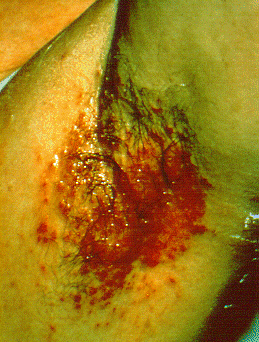
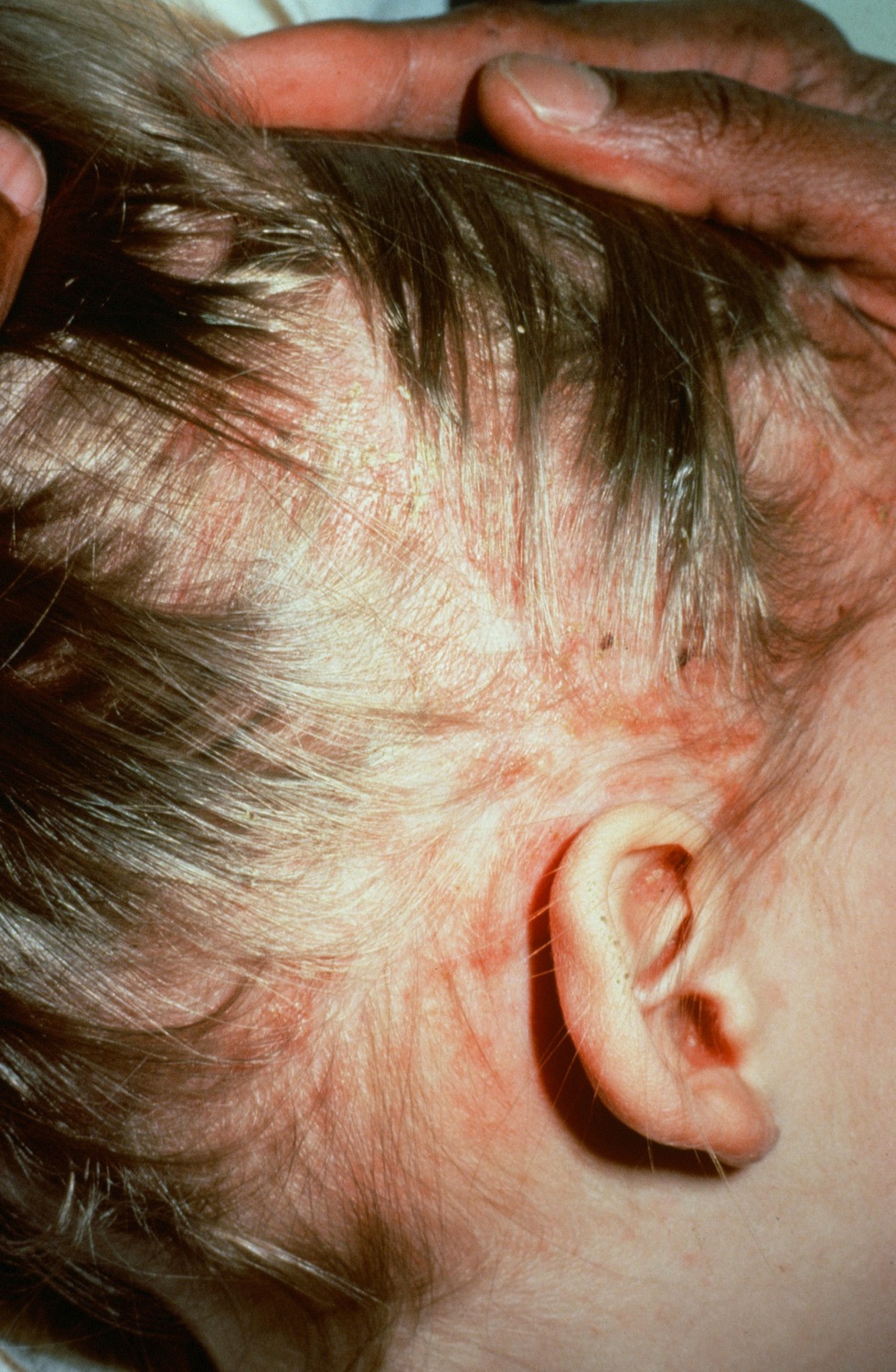
| Langerhans cell histiocytosis[20] |
|
|
|
|
| Tinea manuum/pedum/capitis[24] |
|
|
|
|
| Seborrheic dermatitis |
|
References
- ↑ "Mycosis Fungoides and the Sézary Syndrome Treatment (PDQ®)—Patient Version - National Cancer Institute".
- ↑ Mahajan K, Relhan V, Relhan AK, Garg VK (2016). "Pityriasis Rosea: An Update on Etiopathogenesis and Management of Difficult Aspects". Indian J Dermatol. 61 (4): 375–84. doi:10.4103/0019-5154.185699. PMC 4966395. PMID 27512182.
- ↑ Prantsidis A, Rigopoulos D, Papatheodorou G, Menounos P, Gregoriou S, Alexiou-Mousatou I, Katsambas A (2009). "Detection of human herpesvirus 8 in the skin of patients with pityriasis rosea". Acta Derm. Venereol. 89 (6): 604–6. doi:10.2340/00015555-0703. PMID 19997691.
- ↑ Smith KJ, Nelson A, Skelton H, Yeager J, Wagner KF (1997). "Pityriasis lichenoides et varioliformis acuta in HIV-1+ patients: a marker of early stage disease. The Military Medical Consortium for the Advancement of Retroviral Research (MMCARR)". Int. J. Dermatol. 36 (2): 104–9. PMID 9109005.
- ↑ Jiamton S, Tangjaturonrusamee C, Kulthanan K (2013). "Clinical features and aggravating factors in nummular eczema in Thais". Asian Pac. J. Allergy Immunol. 31 (1): 36–42. PMID 23517392.
- ↑ "STD Facts - Syphilis".
- ↑ Neagu TP, Ţigliş M, Botezatu D, Enache V, Cobilinschi CO, Vâlcea-Precup MS, GrinŢescu IM (2017). "Clinical, histological and therapeutic features of Bowen's disease". Rom J Morphol Embryol. 58 (1): 33–40. PMID 28523295.
- ↑ Murao K, Yoshioka R, Kubo Y (2014). "Human papillomavirus infection in Bowen disease: negative p53 expression, not p16(INK4a) overexpression, is correlated with human papillomavirus-associated Bowen disease". J. Dermatol. 41 (10): 878–84. doi:10.1111/1346-8138.12613. PMID 25201325.
- ↑ Szatkowski J, Schwartz RA (2015). "Acute generalized exanthematous pustulosis (AGEP): A review and update". J. Am. Acad. Dermatol. 73 (5): 843–8. doi:10.1016/j.jaad.2015.07.017. PMID 26354880.
- ↑ Schmid S, Kuechler PC, Britschgi M, Steiner UC, Yawalkar N, Limat A, Baltensperger K, Braathen L, Pichler WJ (2002). "Acute generalized exanthematous pustulosis: role of cytotoxic T cells in pustule formation". Am. J. Pathol. 161 (6): 2079–86. doi:10.1016/S0002-9440(10)64486-0. PMC 1850901. PMID 12466124.
- ↑ Ankad BS, Beergouder SL (2016). "Hypertrophic lichen planus versus prurigo nodularis: a dermoscopic perspective". Dermatol Pract Concept. 6 (2): 9–15. doi:10.5826/dpc.0602a03. PMC 4866621. PMID 27222766.
- ↑ Shengyuan L, Songpo Y, Wen W, Wenjing T, Haitao Z, Binyou W (2009). "Hepatitis C virus and lichen planus: a reciprocal association determined by a meta-analysis". Arch Dermatol. 145 (9): 1040–7. doi:10.1001/archdermatol.2009.200. PMID 19770446.
- ↑ Lutz ME, Daoud MS, McEvoy MT, Gibson LE (1998). "Subcorneal pustular dermatosis: a clinical study of ten patients". Cutis. 61 (4): 203–8. PMID 9564592.
- ↑ Kasha EE, Epinette WW (1988). "Subcorneal pustular dermatosis (Sneddon-Wilkinson disease) in association with a monoclonal IgA gammopathy: a report and review of the literature". J. Am. Acad. Dermatol. 19 (5 Pt 1): 854–8. PMID 3056995.
- ↑ Delaporte E, Colombel JF, Nguyen-Mailfer C, Piette F, Cortot A, Bergoend H (1992). "Subcorneal pustular dermatosis in a patient with Crohn's disease". Acta Derm. Venereol. 72 (4): 301–2. PMID 1357895.
- ↑ Sauder MB, Glassman SJ (2013). "Palmoplantar subcorneal pustular dermatosis following adalimumab therapy for rheumatoid arthritis". Int. J. Dermatol. 52 (5): 624–8. doi:10.1111/j.1365-4632.2012.05707.x. PMID 23489057.
- ↑ Lambert WC, Everett MA (1981). "The nosology of parapsoriasis". J. Am. Acad. Dermatol. 5 (4): 373–95. PMID 7026622.
- ↑ Väkevä L, Sarna S, Vaalasti A, Pukkala E, Kariniemi AL, Ranki A (2005). "A retrospective study of the probability of the evolution of parapsoriasis en plaques into mycosis fungoides". Acta Derm. Venereol. 85 (4): 318–23. doi:10.1080/00015550510030087. PMID 16191852.
- ↑ Janniger CK, Schwartz RA, Szepietowski JC, Reich A (2005). "Intertrigo and common secondary skin infections". Am Fam Physician. 72 (5): 833–8. PMID 16156342.
- ↑ Satter EK, High WA (2008). "Langerhans cell histiocytosis: a review of the current recommendations of the Histiocyte Society". Pediatr Dermatol. 25 (3): 291–5. doi:10.1111/j.1525-1470.2008.00669.x. PMID 18577030.
- ↑ Stull MA, Kransdorf MJ, Devaney KO (1992). "Langerhans cell histiocytosis of bone". Radiographics. 12 (4): 801–23. doi:10.1148/radiographics.12.4.1636041. PMID 1636041.
- ↑ Sholl LM, Hornick JL, Pinkus JL, Pinkus GS, Padera RF (2007). "Immunohistochemical analysis of langerin in langerhans cell histiocytosis and pulmonary inflammatory and infectious diseases". Am. J. Surg. Pathol. 31 (6): 947–52. doi:10.1097/01.pas.0000249443.82971.bb. PMID 17527085.
- ↑ Grois N, Pötschger U, Prosch H, Minkov M, Arico M, Braier J, Henter JI, Janka-Schaub G, Ladisch S, Ritter J, Steiner M, Unger E, Gadner H (2006). "Risk factors for diabetes insipidus in langerhans cell histiocytosis". Pediatr Blood Cancer. 46 (2): 228–33. doi:10.1002/pbc.20425. PMID 16047354.
- ↑ Al Hasan M, Fitzgerald SM, Saoudian M, Krishnaswamy G (2004). "Dermatology for the practicing allergist: Tinea pedis and its complications". Clin Mol Allergy. 2 (1): 5. doi:10.1186/1476-7961-2-5. PMC 419368. PMID 15050029.
- ↑ Schwartz RA, Janusz CA, Janniger CK (2006). "Seborrheic dermatitis: an overview". Am Fam Physician. 74 (1): 125–30. PMID 16848386.
- ↑ Misery L, Touboul S, Vinçot C, Dutray S, Rolland-Jacob G, Consoli SG, Farcet Y, Feton-Danou N, Cardinaud F, Callot V, De La Chapelle C, Pomey-Rey D, Consoli SM (2007). "[Stress and seborrheic dermatitis]". Ann Dermatol Venereol (in French). 134 (11): 833–7. PMID 18033062.