Lyme disease primary prevention
|
Lyme disease Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Lyme disease primary prevention On the Web |
|
American Roentgen Ray Society Images of Lyme disease primary prevention |
|
Risk calculators and risk factors for Lyme disease primary prevention |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Anmol Pitliya, M.B.B.S. M.D.[2]Ilan Dock, B.S.
Overview
Primary prevention of Lyme disease involves tick control and reducing exposure to ticks. The tick should be removed with proper technique so as to decrease the risk of infection. A Lyme disease vaccine used in the past is no longer available.
Primary Prevention
Tick control
- Tick control can help prevent many tick-borne diseases including Lyme disease, human granulomatous anaplasmosis (HGA), babesiosis, and others.
- Use of acaricidal sprays on vegetation where ticks live is consistently most effective method.
- Acaricides are pesticides that kill members of the arachnid subclass Acari, which includes ticks and mites.
- Examples of acaricides include:[1][2][3]
- A single spray during the spring has shown to reduce the density of the nymphal stage of I. scapularis significantly, ranging from 67.9% for carbaryl to 97.4% for chlorpyrifos.[1]
- Evidence suggests that removal and controlled burning of vegetation (foilage and leaf litter) results in reduction in the density of the nymph stage of I. scapularis ranging from 72.7 to 100%.[4][5]
- Permethrin-impregnated cotton balls:[6]
- Permethrin-impregnated cotton balls in an applicator tube are placed outdoors.
- Fibers from the tube are carried to nests by white-footed mice, which are the principle reservoir host of B. burgdorferi.
- Exposure to permethrin kills all ticks infesting these mice.
- This method was a success in the coastal New England area.
- These permethrin-impregnated cotton balls are available commercially as 'Damminix tick tubes'.
- However, this method was found ineffective in New York and Connecticut.[7][8]
Minimizing tick exposure
The best way to prevent Lyme disease is to avoid tick infested areas, but it is unreasonable to assume that a person can completely eliminate activities that may result in tick exposure. Therefore, preventive measures should emphasize personal protection when exposed to natural areas where ticks are present:[9]
- Frequently check skin and clothes to identify ticks and remove before infection can be transmitted.
- Wear light-colored clothing that allows you to see ticks that are crawling on clothing.
- Use long sleeved shirts tucked into pants and tuck pant legs into socks so that ticks cannot crawl up the inside the pant legs.
- Apply repellents to discourage tick attachment.[10]
- Permethrin
- Repellents containing permethrin can be sprayed on boots and clothing, and will last for several days.
- N,N-diethyl-3-methylbenzamide (DEET)
- Repellents containing DEET can be applied to the skin, but will last only a few hours before reapplication is necessary.
- Use DEET with caution on children. DEET is appears to be safe when used as directed.[11]
- Application of large amounts of DEET on children has been associated with adverse reactions.[12]
- DEET should be avoided on face, hands, and irritated or abraded skin.
- DEET should be washed off with soap and water upon returning indoors.
- Permethrin
- Conduct a body check upon return from potentially tick-infested areas by searching the entire body for ticks. Use a hand-held or full-length mirror to view all parts of the body. Remove any tick found on the body.
- Parents should check their children for ticks, especially in the hair, when returning from potentially tick-infested areas.
- Ticks may also be carried into the household on clothing and pets and only attach later, so both should be examined carefully to exclude ticks.[13]
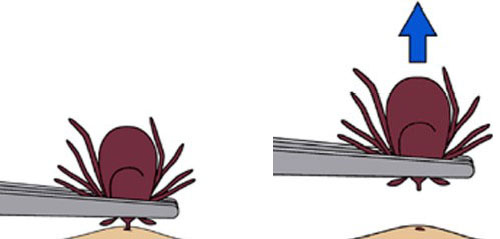
The best way to remove a tick
Note:
|
 |
Vaccination
- A vaccine called Lymerix against a North American strain of the spirochetal bacteria was available from 1998 to 2002.
- It was produced by GlaxoSmithKline (GSK) and was based on the outer surface protein A (Osp-A) of Borrelia. Osp-A causes the human immune system to create antibodies that attack that protein.
- A group of patients who were administered Lymerix developed arthritis, muscle pain, and other troubling symptoms post-vaccination.[15]
- It was later learned that patients with the genetic allele HLA-DR4 were susceptible to T-cell cross-reactivity between epitopes of OspA and lymphocyte function-associated antigen in these patients, causing an autoimmune reaction.[16]
- New vaccines are being researched using outer surface protein C (Osp-C) and glycolipoprotein as methods of immunization.[17][18]
References
- ↑ 1.0 1.1 Curran KL, Fish D, Piesman J (1993). "Reduction of nymphal Ixodes dammini (Acari: Ixodidae) in a residential suburban landscape by area application of insecticides". J Med Entomol. 30 (1): 107–13. PMID 8433317.
- ↑ Stafford KC (1991). "Effectiveness of carbaryl applications for the control of Ixodes dammini (Acari: Ixodidae) nymphs in an endemic residential area". J Med Entomol. 28 (1): 32–6. PMID 1903451.
- ↑ Schulze TL, Jordan RA, Hung RW, Taylor RC, Markowski D, Chomsky MS (2001). "Efficacy of granular deltamethrin against Ixodes scapularis and Amblyomma americanum (Acari: Ixodidade) nymphs". J Med Entomol. 38 (2): 344–6. PMID 11296847.
- ↑ Stafford KC, Ward JS, Magnarelli LA (1998). "Impact of controlled burns on the abundance of Ixodes scapularis (Acari: Ixodidae)". J Med Entomol. 35 (4): 510–3. PMID 9701937.
- ↑ Schulze TL, Jordan RA, Hung RW (1995). "Suppression of subadult Ixodes scapularis (Acari: Ixodidae) following removal of leaf litter". J Med Entomol. 32 (5): 730–3. PMID 7473629.
- ↑ Deblinger RD, Rimmer DW (1991). "Efficacy of a permethrin-based acaricide to reduce the abundance of Ixodes dammini (Acari: Ixodidae)". J Med Entomol. 28 (5): 708–11. PMID 1941940.
- ↑ Daniels TJ, Fish D, Falco RC (1991). "Evaluation of host-targeted acaricide for reducing risk of Lyme disease in southern New York state". J Med Entomol. 28 (4): 537–43. PMID 1941916.
- ↑ Stafford KC (1992). "Third-year evaluation of host-targeted permethrin for the control of Ixodes dammini (Acari: Ixodidae) in southeastern Connecticut". J Med Entomol. 29 (4): 717–20. PMID 1495085.
- ↑ Wormser GP, Dattwyler RJ, Shapiro ED, Halperin JJ, Steere AC, Klempner MS; et al. (2006). "The clinical assessment, treatment, and prevention of lyme disease, human granulocytic anaplasmosis, and babesiosis: clinical practice guidelines by the Infectious Diseases Society of America". Clin Infect Dis. 43 (9): 1089–134. doi:10.1086/508667. PMID 17029130.
- ↑ Fradin MS (1998). "Mosquitoes and mosquito repellents: a clinician's guide". Ann Intern Med. 128 (11): 931–40. PMID 9634433.
- ↑ Carroll JF, Klun JA, Debboun M (2005). "Repellency of deet and SS220 applied to skin involves olfactory sensing by two species of ticks". Med Vet Entomol. 19 (1): 101–6. doi:10.1111/j.0269-283X.2005.00559.x. PMID 15752184.
- ↑ Centers for Disease Control (CDC) (1989). "Seizures temporally associated with use of DEET insect repellent--New York and Connecticut". MMWR Morb Mortal Wkly Rep. 38 (39): 678–80. PMID 2506420.
- ↑ General Tick Disease Information. Centers for Disease Control and Prevention (2015). http://www.cdc.gov/ticks/symptoms.html Accessed on December 30, 2015
- ↑ Tick Removal. Centers for Disease Control and Prevention (2015). http://www.cdc.gov/ticks/removing_a_tick.html Accessed on December 30, 2015
- ↑ Safety/Efficacy concerns re: Lyme vaccine: LYMErix Controversy LymeInfo.net
- ↑ Willett TA, Meyer AL, Brown EL, Huber BT (2004). "An effective second-generation outer surface protein A-derived Lyme vaccine that eliminates a potentially autoreactive T cell epitope". Proc. Natl. Acad. Sci. U.S.A. 101 (5): 1303–8. doi:10.1073/pnas.0305680101. PMID 14742868.
- ↑ Earnhart CG, Marconi RT (2007). "OspC phylogenetic analyses support the feasibility of a broadly protective polyvalent chimeric Lyme disease vaccine". Clin. Vaccine Immunol. 14 (5): 628–34. doi:10.1128/CVI.00409-06. PMID 17360854.
- ↑ Pozsgay V, Kubler-Kielb J (2007). "Synthesis of an experimental glycolipoprotein vaccine against Lyme disease". Carbohydr. Res. 342 (3–4): 621–6. doi:10.1016/j.carres.2006.11.014. PMID 17182019.