Mitral stenosis resident survival guide: Difference between revisions
Rim Halaby (talk | contribs) |
Rim Halaby (talk | contribs) |
||
| (11 intermediate revisions by the same user not shown) | |||
| Line 1: | Line 1: | ||
<div style="width: 80%;"> | <div style="width: 80%;"> | ||
__NOTOC__ | __NOTOC__ | ||
{{CMG}}; {{AE}} {{TS}}; {{MM}}; {{AM}} | {{CMG}}; {{AE}} {{TS}}; {{MM}}; {{AM}}; {{Rim}} | ||
{| class="infobox" style="margin: 0 0 0 0; border: 0; float: right; width: 100px; background: #A8A8A8; position: fixed; top: 250px; right: 21px; border-radius: 0 0 10px 10px;" cellpadding="0" cellspacing="0"; | {| class="infobox" style="margin: 0 0 0 0; border: 0; float: right; width: 100px; background: #A8A8A8; position: fixed; top: 250px; right: 21px; border-radius: 0 0 10px 10px;" cellpadding="0" cellspacing="0"; | ||
| Line 11: | Line 11: | ||
! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide#Causes|Causes]] | ! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide#Causes|Causes]] | ||
|- | |- | ||
! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide# | ! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide#Stages|Stages]] | ||
|- | |- | ||
! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide#FIRE: Focused Initial Rapid Evaluation|FIRE]] | ! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide#FIRE: Focused Initial Rapid Evaluation|FIRE]] | ||
| Line 18: | Line 18: | ||
|- | |- | ||
! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide#Treatment|Treatment]] | ! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide#Treatment|Treatment]] | ||
: [[Mitral stenosis resident survival guide# | : [[Mitral stenosis resident survival guide#Medical Therapy|Medical Therapy]] | ||
: [[Mitral stenosis resident survival guide#Intervention|Intervention]] | |||
: [[Mitral stenosis resident survival guide# | |||
|- | |- | ||
! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide#Rheumatic Fever | ! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide#Secondary Prevention of Rheumatic Fever|Secondary Prevention of Rheumatic Fever]] | ||
|- | |- | ||
! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide#Do's|Do's]] | ! style="font-size: 80%; padding: 0 5px; background: #DCDCDC" align=left | [[Mitral stenosis resident survival guide#Do's|Do's]] | ||
| Line 42: | Line 41: | ||
Click '''[[Mitral stenosis causes|here]]''' for the complete list of causes | Click '''[[Mitral stenosis causes|here]]''' for the complete list of causes | ||
== | ==Stages== | ||
{| style=" | Shown below is a table depicting the 4 stages of mitral stenosis, adapted from 2014 AHA/ACC guidelines for management of valvular heart diseases.<ref name="pmid24589852">{{cite journal| author=Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP, Guyton RA et al.| title=2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. | journal=Circulation | year= 2014 | volume= | issue= | pages= | pmid=24589852 | doi=10.1161/CIR.0000000000000029 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=24589852 }} </ref> | ||
<span style="font-size:85%">'''Abbreviations:''' '''MS: ''' mitral stenosis; '''MVA: '''mitral valve area; '''PASP: ''' pulmonary artery systolic pressure</span> | |||
{|Class="wikitable" | |||
|- | |- | ||
|style=" | |style="background:#DCDCDC;"|'''Stage'''||style="background:#DCDCDC;"|'''Definition'''||style="background:#DCDCDC;"|'''Valve anatomy'''||style="background:#DCDCDC;"|'''Valve hemodynamics'''||style="background:#DCDCDC;"|'''Hemodynamic consequences'''||style="background:#DCDCDC;"|'''Symptoms''' | ||
|- | |- | ||
| | |'''A'''||At risk of [[MS]]||❑ Mild diastolic doming of mitral valve leaflets||❑ Normal transmitral velocity||Absent||Absent | ||
|- | |||
|'''B'''||Progressive [[MS]]|| ❑ Rheumatic valve changes characterized by commissural fusion and diastolic doming of [[mitral valve]]<br>❑ MVA > 1.5 cm<sup>2</sup> (planimetered)||❑ Increased transmitral flow velocities<br>❑ MVA > 1.5 cm<sup>2</sup> <br>❑ Pressure half time during diastole < 150 ms||❑ Mild to moderate [[left atrial]] enlargement<br>❑ Normal pulmonary pressure at rest ||None | |||
|- | |||
|'''C'''||Asymptomatic severe [[MS]]||❑ Rheumatic valve changes characterized by commissural fusion and diastolic doming of [[mitral valve]]<br> ❑ MVA ≤ 1.5 cm<sup>2</sup><br>❑ MVA ≤ 1 cm<sup>2</sup> in very severe [[MS]]|| ❑ MVA ≤ 1.5 cm<sup>2</sup> (planimetered)<br>❑ MVA ≤ 1 cm<sup>2</sup> (planimetered) in very severe [[MS]]<br>❑ Diastolic pressure half time ≥ 150 ms<br> ❑ Diastolic pressure half time ≥ 220 ms with very severe [[MS]]||❑ Severe [[left atrial]] enlargement<br>❑ PASP > 30 mm Hg||Absent | |||
|- | |||
|'''D'''||Symptomatic severe [[MS]]||❑ Rheumatic valve changes characterized by commissural fusion and diastolic doming of [[mitral valve]]<br> ❑ MVA ≤ 1.5 cm<sup>2</sup> (planimetered)||❑ MVA ≤ 1.5 cm<sup>2</sup><br>❑ MVA ≤ 1 cm<sup>2</sup> in very severe [[MS]]<br>❑ Diastolic pressure half time ≥ 150 ms<br> ❑ Diastolic pressure half time ≥ 220 ms with very severe [[MS]]||❑ Severe left atrial enlargement<br>❑ PASP > 30 mm Hg||❑ [[Dyspnea]] on exertion<br>❑ Decreased exercise tolerance | |||
|} | |} | ||
| Line 67: | Line 75: | ||
{{familytree | | | | | | | |!| | | | | | | | | | }} | {{familytree | | | | | | | |!| | | | | | | | | | }} | ||
{{familytree | | | | | | | A01 | | | | | | | | | | A01= <div style="text-align: left; width: 18em; padding: 1em;">'''Does the patient have any of the following findings of decompensated [[mitral stenosis]] that require urgent management?'''<br> | {{familytree | | | | | | | A01 | | | | | | | | | | A01= <div style="text-align: left; width: 18em; padding: 1em;">'''Does the patient have any of the following findings of decompensated [[mitral stenosis]] that require urgent management?'''<br> | ||
❑ [[Tachycardia]] <br> ❑ [[Hypotension]]<br> ❑ [[Dyspnea|Severe dyspnea]]<br> ❑ [[Loss of consciousness]]<br>❑ [[Chest pain]]</div>}} | ❑ [[Tachycardia]] <br> ❑ [[Hypotension]]<br> ❑ [[Dyspnea|Severe dyspnea]]<br> ❑ [[Loss of consciousness]]<br>❑ [[Chest pain]]<br>❑ Sudden [[weakness]] or [[paralysis]]</div>}} | ||
{{familytree | | | | |,|-|-|^|-|-|.| | | | |}} | {{familytree | | | | |,|-|-|^|-|-|.| | | | |}} | ||
{{familytree |boxstyle= padding: 0; background: #FA8072; text-align: center;| | | | B01 | | | | | B02 | | | |B01={{fontcolor|#F8F8FF|'''Yes'''}}| B02=<div style="text-align: center; background: #FFFFFF; height: 25px; line-height: 25px;">'''No'''</div>}} | {{familytree |boxstyle= padding: 0; background: #FA8072; text-align: center;| | | | B01 | | | | | B02 | | | |B01={{fontcolor|#F8F8FF|'''Yes'''}}| B02=<div style="text-align: center; background: #FFFFFF; height: 25px; line-height: 25px;">'''No'''</div>}} | ||
| Line 224: | Line 232: | ||
==Treatment== | ==Treatment== | ||
===Medical Therapy=== | |||
< | {{Family tree/start}} | ||
{{Family tree | A01 | | A01=<div style="float: left; text-align: left; padding:1em;"> | |||
'''Treatment of Acute Decompensation'''<br> | |||
❑ Digoxin <br> | |||
In the following cases:<br> | |||
:❑ Symptomatic [[right ventricular]] or [[left ventricular]] dysfunction ([[digitalis]] increases [[myocardial]] contractility) | |||
:❑ [[Atrial fibrillation]] ([[digitalis]] slows the ventricular response which prolongs the diastolic filling time)<ref name="pmid11907022">{{cite journal| author=Boon NA, Bloomfield P| title=The medical management of valvar heart disease. | journal=Heart | year= 2002 | volume= 87 | issue= 4 | pages= 395-400 | pmid=11907022 | doi= | pmc=PMC1767079 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=11907022 }} </ref> | |||
❑ Diuretics (In the following cases fluid overload)<br> | |||
❑ Low sodium diet <br> | |||
❑ Activity restriction <br> | |||
'''Systemic Embolization Prevention'''<ref name="pmid24589852">{{cite journal| author=Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP, Guyton RA et al.| title=2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. | journal=Circulation | year= 2014 | volume= | issue= | pages= | pmid=24589852 | doi=10.1161/CIR.0000000000000029 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=24589852 }} </ref> <br> | |||
In the following cases:<br> | |||
{{ | ❑ Paroxysmal, persistent, or permanent [[atrial fibrillation]] ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class I, Level of Evidence B]]) <br> | ||
❑ Prior [[embolization]] event ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class I, Level of Evidence B]]) <br> | |||
| | ❑ [[Left atrial]] thrombus ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class I, Level of Evidence B]]) <br> | ||
| | |||
| | |||
'''Rate Control'''<ref name="pmid24589852">{{cite journal| author=Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP, Guyton RA et al.| title=2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. | journal=Circulation | year= 2014 | volume= | issue= | pages= | pmid=24589852 | doi=10.1161/CIR.0000000000000029 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=24589852 }} </ref><br> | |||
In the following cases:<br> | |||
❑ [[Atrial fibrillation]] associated with fast ventricular response ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class IIa, Level of Evidence C]]) | |||
<br> | ❑ Normal [[sinus rhythm]] plus symptoms associated with exercise ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class IIb, Level of Evidence B]]) </div>}} | ||
{{Family tree/end}} | |||
{{ | |||
===Summary | ===Intervention=== | ||
Shown below is an algorithm depicting the indications for mitral stenosis intervention according to the 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease.<ref name="pmid24589852">{{cite journal| author=Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP, Guyton RA et al.| title=2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. | journal=Circulation | year= 2014 | volume= | issue= | pages= | pmid=24589852 | doi=10.1161/CIR.0000000000000029 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=24589852 }} </ref> | |||
<span style="font-size:85%">'''Abbreviations:''' '''AF''': [[atrial fibrillation]]; '''MR:''' [[mitral regurgitation]]; '''MS:''' [[mitral stenosis]]; '''MVA:''' mitral valve area ; '''PCWP:''' [[pulmonary capillary wedge pressure]]; '''PMBC:''' [[percutaneous mitral balloon commissurotomy]]; '''T<sub>1/2</sub>:''' pressure half-time</span> | <span style="font-size:85%">'''Abbreviations:''' '''AF''': [[atrial fibrillation]]; '''MR:''' [[mitral regurgitation]]; '''MS:''' [[mitral stenosis]]; '''MVA:''' mitral valve area ; '''PCWP:''' [[pulmonary capillary wedge pressure]]; '''PMBC:''' [[percutaneous mitral balloon commissurotomy]]; '''T<sub>1/2</sub>:''' pressure half-time</span> | ||
| Line 284: | Line 284: | ||
{{Familytree/end}} | {{Familytree/end}} | ||
==Rheumatic Fever | ==Secondary Prevention of Rheumatic Fever== | ||
Shown below is the table depicting the secondary prophylaxis of [[rheumatic fever]].<ref name="pmid19246689">{{cite journal| author=Gerber MA, Baltimore RS, Eaton CB, Gewitz M, Rowley AH, Shulman ST et al.| title=Prevention of rheumatic fever and diagnosis and treatment of acute Streptococcal pharyngitis: a scientific statement from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee of the Council on Cardiovascular Disease in the Young, the Interdisciplinary Council on Functional Genomics and Translational Biology, and the Interdisciplinary Council on Quality of Care and Outcomes Research: endorsed by the American Academy of Pediatrics. | journal=Circulation | year= 2009 | volume= 119 | issue= 11 | pages= 1541-51 | pmid=19246689 | doi=10.1161/CIRCULATIONAHA.109.191959 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=19246689 }} </ref> | ===Indications=== | ||
Shown below is the table depicting the indication for secondary prophylaxis of [[rheumatic fever]].<ref name="pmid19246689">{{cite journal| author=Gerber MA, Baltimore RS, Eaton CB, Gewitz M, Rowley AH, Shulman ST et al.| title=Prevention of rheumatic fever and diagnosis and treatment of acute Streptococcal pharyngitis: a scientific statement from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee of the Council on Cardiovascular Disease in the Young, the Interdisciplinary Council on Functional Genomics and Translational Biology, and the Interdisciplinary Council on Quality of Care and Outcomes Research: endorsed by the American Academy of Pediatrics. | journal=Circulation | year= 2009 | volume= 119 | issue= 11 | pages= 1541-51 | pmid=19246689 | doi=10.1161/CIRCULATIONAHA.109.191959 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=19246689 }} </ref> | |||
{| style=" | {| style="cellpadding=0; cellspacing= 0; width: 600px;" | ||
|- | |- | ||
| style="font-size: | | style="padding: 0 5px; font-size: 100%; background: #4682B4; color: #FFFFFF;" align=center | '''Indications'''|| style="padding: 0 5px; font-size: 100%; background: #4682B4; color: #FFFFFF;" align=center | '''Duration of prophylaxis''' | ||
|- | |- | ||
| style="font-size: | |style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left | ▸ '''''[[Rheumatic fever]] with [[carditis]] and persistent [[valvular heart disease]] || style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left |▸ '''''10 years or until the patient is 40 years (whichever is longer)''''' ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class I, Level of Evidence C]]) | ||
|- | |- | ||
|style="font-size: | |style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left | ▸ '''''[[Rheumatic fever]] with [[carditis]] but no [[valvular heart disease]] || style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left |▸ '''''10 years or until the patient is 21 years (whichever is longer)''''' ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class I, Level of Evidence C]]) | ||
|- | |- | ||
|style="font-size: | |style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left | ▸ '''''[[Rheumatic fever]] without [[carditis]] || style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left |▸ '''''5 years or until the patient is 21 years (whichever is longer)''''' ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class I, Level of Evidence C]]) | ||
|- | |- | ||
|} | |} | ||
|} | |||
< | ===Antibiotic Regimens=== | ||
Shown below is the table depicting the antibiotic regimens for secondary prophylaxis of [[rheumatic fever]].<ref name="pmid19246689">{{cite journal| author=Gerber MA, Baltimore RS, Eaton CB, Gewitz M, Rowley AH, Shulman ST et al.| title=Prevention of rheumatic fever and diagnosis and treatment of acute Streptococcal pharyngitis: a scientific statement from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee of the Council on Cardiovascular Disease in the Young, the Interdisciplinary Council on Functional Genomics and Translational Biology, and the Interdisciplinary Council on Quality of Care and Outcomes Research: endorsed by the American Academy of Pediatrics. | journal=Circulation | year= 2009 | volume= 119 | issue= 11 | pages= 1541-51 | pmid=19246689 | doi=10.1161/CIRCULATIONAHA.109.191959 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=19246689 }} </ref> | |||
{| style="cellpadding=0; cellspacing= 0; width: 600px;" | {| style="cellpadding=0; cellspacing= 0; width: 600px;" | ||
|- | |- | ||
| style="padding: 0 5px; font-size: 100%; background: # | | style="padding: 0 5px; font-size: 100%; background: #4682B4; color: #FFFFFF;" align=center | '''Antibiotics'''|| style="padding: 0 5px; font-size: 100%; background: #4682B4; color: #FFFFFF;" align=center | '''Dosage''' | ||
|- | |||
|- | |||
| style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left | '''''[[Penicillin G benzathine]]''''' <br> ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class I, Level of Evidence A]])||style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left| ▸ '''''Weight >27 Kg (60 lb): 1.2 million units IM every day for 4 weeks'''''<br>▸ '''''Weight ≤27 Kg (60 lb): 600,000 units IM every day for 4 weeks''''' | |||
|- | |- | ||
| style="font-size: | |style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left |'''''[[Penicillin V]]''''' <br> ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class I, Level of Evidence B]])|| style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left |▸ '''''200 mg orally twice a day''''' | ||
|- | |- | ||
|style="font-size: | |style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left|'''''[[Sulfadiazine]]''''' <br> ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class I, Level of Evidence B]])|| style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left|▸ '''''Weight >27 Kg (60 lb): 1 g orally once a day''''' <br> ▸ '''''Weight ≤27 Kg (60 lb): o.5 g orally once a day''''' | ||
|- | |- | ||
|style="font-size: | |style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left|'''''[[Macrolide]] or [[azalide]] antibiotics (in patients allergic to [[penicillin]])''''' <br> ([[ACC AHA guidelines classification scheme#Classification of Recommendations|Class I, Level of Evidence C]])|| style="font-size: 100; padding: 0 5px; background: #B8B8B8" align=left|▸ '''''Varies''''' | ||
|- | |- | ||
|} | |} | ||
Latest revision as of 22:36, 22 July 2014
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Twinkle Singh, M.B.B.S. [2]; Mohamed Moubarak, M.D. [3]; Amr Marawan, M.D. [4]; Rim Halaby, M.D. [5]
| Mitral Stenosis Resident Survival Guide Microchapters |
|---|
| Overview |
| Causes |
| Stages |
| FIRE |
| Diagnosis |
| Treatment |
| Secondary Prevention of Rheumatic Fever |
| Do's |
Overview
Mitral stenosis refers to abnormal narrowing of mitral orifice, which leads to obstruction of blood flow from left atrium to left ventricle most commonly as a complication of rheumatic fever. The most common presentations of mitral stenosis are dyspnea, orthopnea, paroxysmal nocturnal dyspnea, and peripheral edema. Mitral stenosis has a characteristic low-pitched, rumbling diastolic murmur, heard best at the apex during physical examination. The definitive therapy for mitral stenosis include percutaneous balloon valvotomy, surgical mitral valve repair, or mitral valve replacement.
Causes
Life Threatening Causes
Life-threatening causes include conditions which may result in death or permanent disability within 24 hours if left untreated.
Common Causes
Click here for the complete list of causes
Stages
Shown below is a table depicting the 4 stages of mitral stenosis, adapted from 2014 AHA/ACC guidelines for management of valvular heart diseases.[2]
Abbreviations: MS: mitral stenosis; MVA: mitral valve area; PASP: pulmonary artery systolic pressure
| Stage | Definition | Valve anatomy | Valve hemodynamics | Hemodynamic consequences | Symptoms |
| A | At risk of MS | ❑ Mild diastolic doming of mitral valve leaflets | ❑ Normal transmitral velocity | Absent | Absent |
| B | Progressive MS | ❑ Rheumatic valve changes characterized by commissural fusion and diastolic doming of mitral valve ❑ MVA > 1.5 cm2 (planimetered) |
❑ Increased transmitral flow velocities ❑ MVA > 1.5 cm2 ❑ Pressure half time during diastole < 150 ms |
❑ Mild to moderate left atrial enlargement ❑ Normal pulmonary pressure at rest |
None |
| C | Asymptomatic severe MS | ❑ Rheumatic valve changes characterized by commissural fusion and diastolic doming of mitral valve ❑ MVA ≤ 1.5 cm2 ❑ MVA ≤ 1 cm2 in very severe MS |
❑ MVA ≤ 1.5 cm2 (planimetered) ❑ MVA ≤ 1 cm2 (planimetered) in very severe MS ❑ Diastolic pressure half time ≥ 150 ms ❑ Diastolic pressure half time ≥ 220 ms with very severe MS |
❑ Severe left atrial enlargement ❑ PASP > 30 mm Hg |
Absent |
| D | Symptomatic severe MS | ❑ Rheumatic valve changes characterized by commissural fusion and diastolic doming of mitral valve ❑ MVA ≤ 1.5 cm2 (planimetered) |
❑ MVA ≤ 1.5 cm2 ❑ MVA ≤ 1 cm2 in very severe MS ❑ Diastolic pressure half time ≥ 150 ms ❑ Diastolic pressure half time ≥ 220 ms with very severe MS |
❑ Severe left atrial enlargement ❑ PASP > 30 mm Hg |
❑ Dyspnea on exertion ❑ Decreased exercise tolerance |
FIRE: Focused Initial Rapid Evaluation
A Focused Initial Rapid Evaluation (FIRE) should be performed to identify patients in need of immediate intervention.
Boxes in the red color signify that an urgent management is needed.
Identify cardinal findings that increase the pretest probability of mitral stenosis ❑ Mid diastolic murmur
| |||||||||||||||||||||||||||||||||||||||||||||
Does the patient have any of the following findings of decompensated mitral stenosis that require urgent management? ❑ Tachycardia ❑ Hypotension ❑ Severe dyspnea ❑ Loss of consciousness ❑ Chest pain ❑ Sudden weakness or paralysis | |||||||||||||||||||||||||||||||||||||||||||||
| Yes | No | ||||||||||||||||||||||||||||||||||||||||||||
What is the complication of mitral stenosis that is causing decompensation? | |||||||||||||||||||||||||||||||||||||||||||||
❑ Suspect in case of:
| ❑ Suspect in case of palpitations ❑ Order an ECG immediately looking for | ❑ Suspect in case of:
| Pulmonary hypertension ± right sided heart failure ❑ Suspect in case of severe dyspnea ❑ Increased jugular venous pressure immediately ❑ Hepatomegaly ± pulsatile liver | ||||||||||||||||||||||||||||||||||||||||||
❑ Treat the complications of mitral stenosis that lead to decompensation ❑ Order a TTE to evaluate the severity of the mitral stenosis | |||||||||||||||||||||||||||||||||||||||||||||
Complete Diagnostic Approach
A complete diagnostic approach should be carried out after a focused initial rapid evaluation is conducted and following initiation of any urgent intervention.[2].
Abbreviations: AF: Atrial fibrillation; PMBC: Percutaneous mitral ballon commissurotomy; TR: Tricuspid regurgitation; S1: First heart sound; P2: Pulmonary component of second heart sound; EKG: Electrocardiogram; TTE: Transthoracic echocardiography; MS: Mitral stenosis
Characterize the symptoms: ❑ Exercise intolerance ❑ Respiratory infections | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Examine the patient: Appearance of the patient Vital signs ❑ Pulse
Neck:
Extremities: Abdominal examination: Cardiovascular examination: Auscultation
{{#ev:youtube|HW2pk1icYdM|250}} | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Order tests: ❑ Transthoracic echocardiography
❑ Exercise testing with Doppler or invasive hemodynamic assessment in case of discrepancy between resting Doppler echocardiographic findings and clinical symptoms or signs
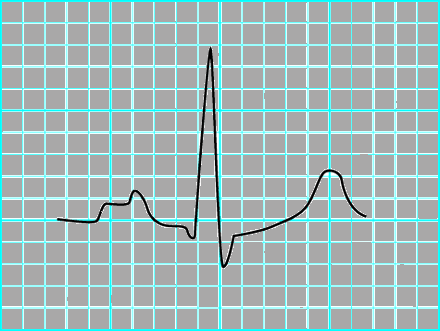
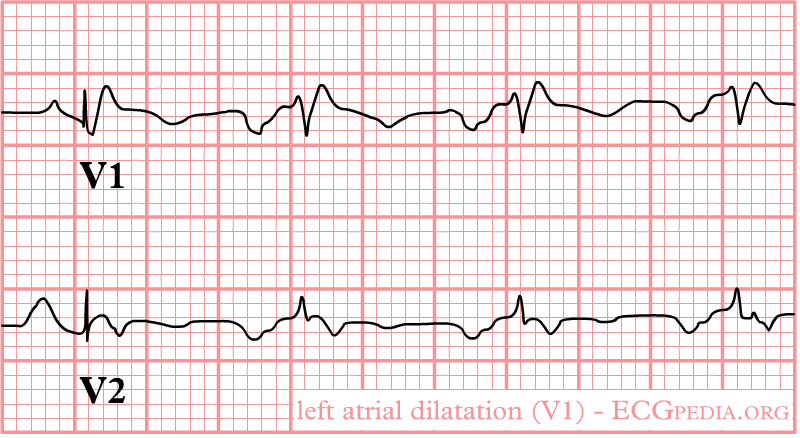
❑ EKG
Click here for the rest of the EKG findings in right ventricular hypertrophy
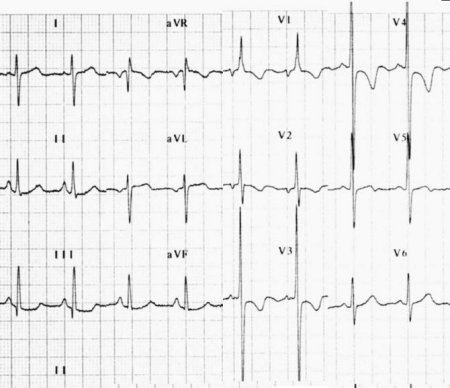
Shown below an ECG depicting right axis deviation
Shown below an ECG depicting atrial fibrillation
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Classify mitral stenosis based on the following findings on TTE: ❑ Valve anatomy ❑ Valve hemodynamics gradient ❑ Hemodynamic consequences | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Treatment
Medical Therapy
Treatment of Acute Decompensation
❑ Diuretics (In the following cases fluid overload)
| |||||||
Intervention
Shown below is an algorithm depicting the indications for mitral stenosis intervention according to the 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease.[2]
Abbreviations: AF: atrial fibrillation; MR: mitral regurgitation; MS: mitral stenosis; MVA: mitral valve area ; PCWP: pulmonary capillary wedge pressure; PMBC: percutaneous mitral balloon commissurotomy; T1/2: pressure half-time
Determine the severity of rheumatic mitral stenosis (MS) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Very severe MS ❑ MVA ≤1 cm2 ❑ T1/2 ≥220 ms | Severe MS ❑ MVA ≤1.5 cm2 ❑ T1/2 ≥150 ms | Progressive MS MVA >1.5 cm2 T1/2 <150 ms | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Is the patient symptomatic? | Is the patient symptomatic? | Is the patient symptomatic? | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| No ( Stage C) | Yes (Stage D) | No (Stage C) | Yes With no other cause for the symptoms | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Is there a new onset of AF? | Order an exercise treadmill test | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| No | Yes | Yes | No | Yes | No | Is PCWP> 25 mm Hg? | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| No | Yes | Yes | No | Yes | No | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Periodic monitoring | PMBC (Class IIa) | PMBC (Class I) | Mitral valve surgery (Class I) | PMBC (Class IIb) | Periodic monitoring | PMBC (Class IIb) | Periodic monitoring | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Secondary Prevention of Rheumatic Fever
Indications
Shown below is the table depicting the indication for secondary prophylaxis of rheumatic fever.[4]
| Indications | Duration of prophylaxis |
| ▸ Rheumatic fever with carditis and persistent valvular heart disease | ▸ 10 years or until the patient is 40 years (whichever is longer) (Class I, Level of Evidence C) |
| ▸ Rheumatic fever with carditis but no valvular heart disease | ▸ 10 years or until the patient is 21 years (whichever is longer) (Class I, Level of Evidence C) |
| ▸ Rheumatic fever without carditis | ▸ 5 years or until the patient is 21 years (whichever is longer) (Class I, Level of Evidence C) |
Antibiotic Regimens
Shown below is the table depicting the antibiotic regimens for secondary prophylaxis of rheumatic fever.[4]
| Antibiotics | Dosage |
| Penicillin G benzathine (Class I, Level of Evidence A) |
▸ Weight >27 Kg (60 lb): 1.2 million units IM every day for 4 weeks ▸ Weight ≤27 Kg (60 lb): 600,000 units IM every day for 4 weeks |
| Penicillin V (Class I, Level of Evidence B) |
▸ 200 mg orally twice a day |
| Sulfadiazine (Class I, Level of Evidence B) |
▸ Weight >27 Kg (60 lb): 1 g orally once a day ▸ Weight ≤27 Kg (60 lb): o.5 g orally once a day |
| Macrolide or azalide antibiotics (in patients allergic to penicillin) (Class I, Level of Evidence C) |
▸ Varies |
Do's
- Perform transesophageal echocardiography (TEE) in patients considered for PMBC to rule out left atrial thrombus and to determine mitral regurgitation severity.
- Perform exercise testing or invasive hemodynamic testing, when clinical signs and symptoms don't co-relate with echocardiographic findings.
- Perform mitral valve surgery in stage C and stage D mitral stenosis, if patient is undergoing cardiac surgery for some other indication.
- Perform mitral valve surgery in moderate mitral stenosis (mitral valve area: 1.6 - 2 cm2) if the patient is undergoing cardiac surgery for other indications.
- Perform mitral valve surgery with excision of left atrial appendage in stage C and stage D mitral stenosis patients who have had recurrent embolic events despite being on anticoagulation therapy.
- Perform TTE every 3-5 years in asymptomatic stage B MS patients and every 1-2 years in asymptomatic stage C MS patients who have mitral valve area 1-1.5 cm2 .
- Perform TTE once every year in asymptomatic stage C MS patients who have mitral valve area < 1 cm2.
- In cases of senile calcific mitral stenosis, intervention is done only when symptoms are severe and cannot be controlled with heart rate control and diuretics.
References
- ↑ Tadele, H.; Mekonnen, W.; Tefera, E. (2013). "Rheumatic mitral stenosis in Children: more accelerated course in sub-Saharan Patients". BMC Cardiovasc Disord. 13 (1): 95. doi:10.1186/1471-2261-13-95. PMID 24180350. Unknown parameter
|month=ignored (help) - ↑ 2.0 2.1 2.2 2.3 2.4 Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP, Guyton RA; et al. (2014). "2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines". Circulation. doi:10.1161/CIR.0000000000000029. PMID 24589852.
- ↑ Boon NA, Bloomfield P (2002). "The medical management of valvar heart disease". Heart. 87 (4): 395–400. PMC 1767079. PMID 11907022.
- ↑ 4.0 4.1 Gerber MA, Baltimore RS, Eaton CB, Gewitz M, Rowley AH, Shulman ST; et al. (2009). "Prevention of rheumatic fever and diagnosis and treatment of acute Streptococcal pharyngitis: a scientific statement from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee of the Council on Cardiovascular Disease in the Young, the Interdisciplinary Council on Functional Genomics and Translational Biology, and the Interdisciplinary Council on Quality of Care and Outcomes Research: endorsed by the American Academy of Pediatrics". Circulation. 119 (11): 1541–51. doi:10.1161/CIRCULATIONAHA.109.191959. PMID 19246689.