Lupus nephritis pathophysiology
| https://https://www.youtube.com/watch?v=HwzNQ4Oav00&t=4s |350}} |
|
Lupus nephritis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Lupus nephritis pathophysiology On the Web |
|
American Roentgen Ray Society Images of Lupus nephritis pathophysiology |
|
Risk calculators and risk factors for Lupus nephritis pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Cafer Zorkun, M.D., Ph.D. [2], Raviteja Guddeti, M.B.B.S. [3]
Overview
Pathophysiology
Systemic lupus erythematosus (SLE, or lupus) is an autoimmune disease. This means there is a problem with the body's immune system.
Normally, the immune system helps protect the body from harmful substances. But in patients with an autoimmune disease, the immune system cannot tell the difference between harmful substances and healthy ones. As a result, the immune system attacks otherwise healthy cells and tissue.
Overview
The exact pathogenesis of [disease name] is not fully understood.
OR
It is thought that [disease name] is the result of / is mediated by / is produced by / is caused by either [hypothesis 1], [hypothesis 2], or [hypothesis 3].
OR
[Pathogen name] is usually transmitted via the [transmission route] route to the human host.
OR
Following transmission/ingestion, the [pathogen] uses the [entry site] to invade the [cell name] cell.
OR
[Disease or malignancy name] arises from [cell name]s, which are [cell type] cells that are normally involved in [function of cells].
OR
The progression to [disease name] usually involves the [molecular pathway].
OR
The pathophysiology of [disease/malignancy] depends on the histological subtype.
Pathophysiology
Pathogenesis
Immune system, genetic, and environmental factors are considered in the pathogenesis of SLE.
- Immune system [1]:
- Plasma cells and B lymphocytes:
Numbers of plasma cells(PC) are high in the kidney medulla of patients with severe lupus nephritis( LN). PCs and B cells produce auto antibodies. Increased number and activation of B cells may cause worsening proteinuria and severe damage.
B cells in LN patients have more MicroRNAs (miRNAs) which modulate gene expression [2]. Over expression of the miR-30a could lower the level of Lyn (type of protein tyrosine kinases), and lower level of Lyn may cause deposition of immune complexes in the kidney [3][4].
- Macrophages:
Increase expression of Sialoadhesin (Sn), a macrophage-restricted adhesion molecule may play a role in causing sever LN [5].
- Inflammatory cytokines:
Tumor necrosis factor (TNF) is a cytokine (cell signaling protein) that play role in inflammation process. One of the sub types of TNF is TNF-like weak inducer of apoptosis (TWEAK) which has an important role in causing LN [6].
Fn14 ( TWEAK receptor) is interacted with TWEAK on renal mesangial, endothelial, tubular cells and podocytes [7]. This interactions produce multiple inflammatory mediators which lead to LN.
- It is understood that [disease name] is the result of / is mediated by / is produced by / is caused by either [hypothesis 1], [hypothesis 2], or [hypothesis 3].
- [Pathogen name] is usually transmitted via the [transmission route] route to the human host.
- Following transmission/ingestion, the [pathogen] uses the [entry site] to invade the [cell name] cell.
- [Disease or malignancy name] arises from [cell name]s, which are [cell type] cells that are normally involved in [function of cells].
- The progression to [disease name] usually involves the [molecular pathway].
- The pathophysiology of [disease/malignancy] depends on the histological subtype.
Genetics
- [Disease name] is transmitted in [mode of genetic transmission] pattern.
- Genes involved in the pathogenesis of [disease name] include [gene1], [gene2], and [gene3].
- The development of [disease name] is the result of multiple genetic mutations.
Associated Conditions
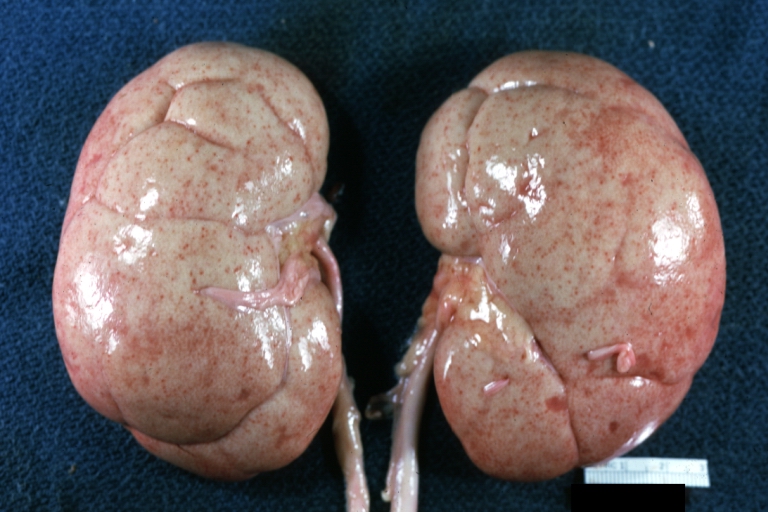
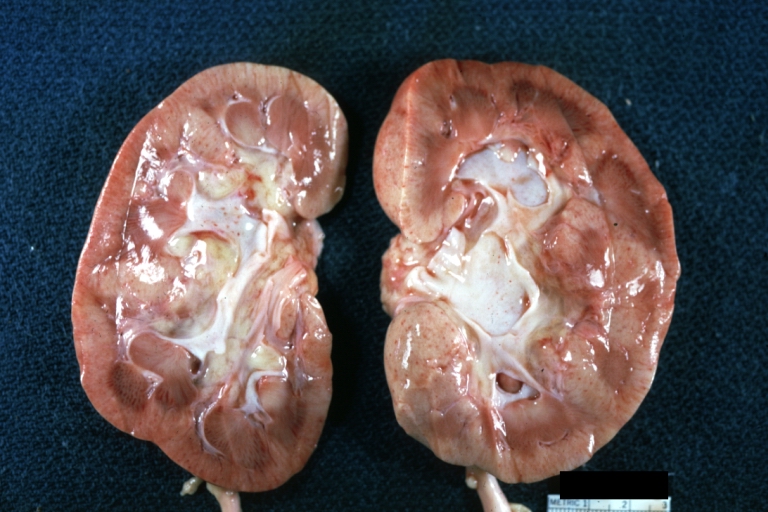
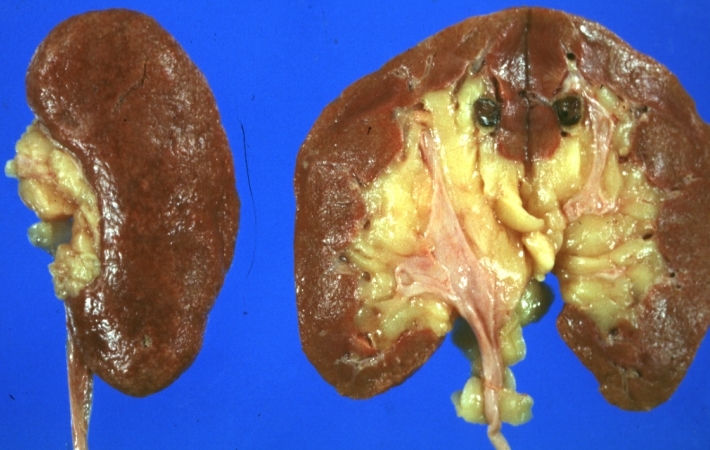
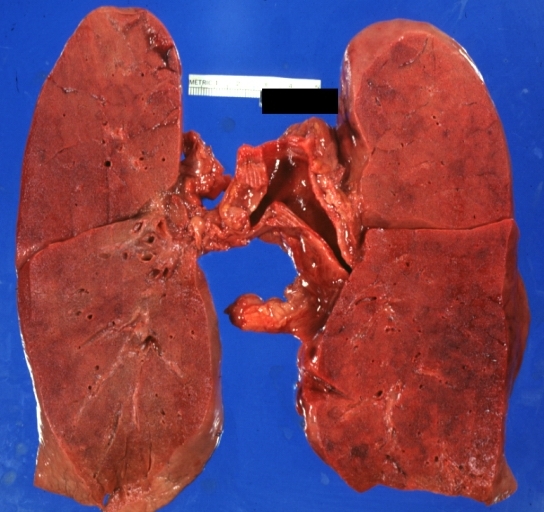
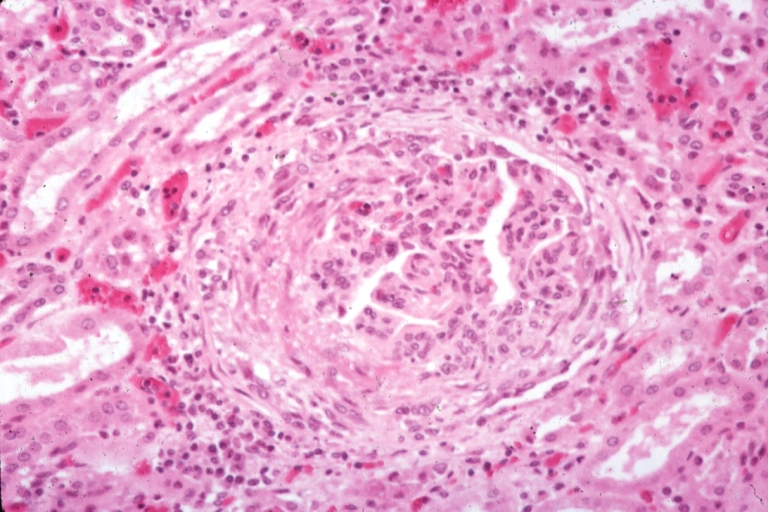
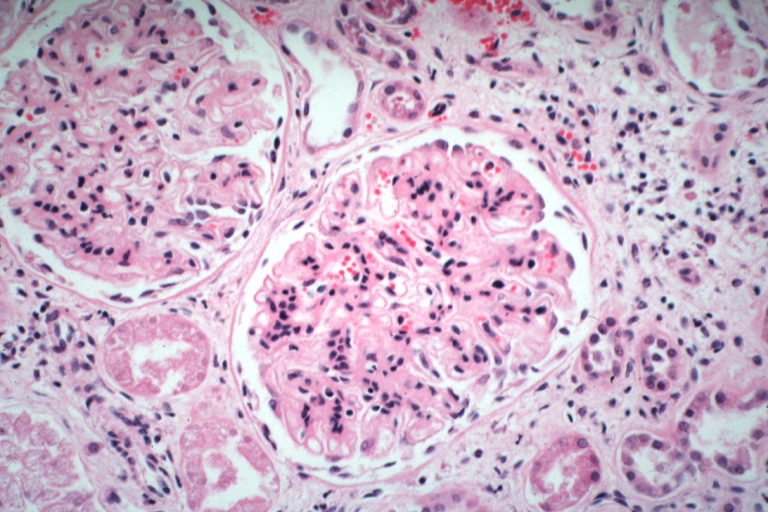
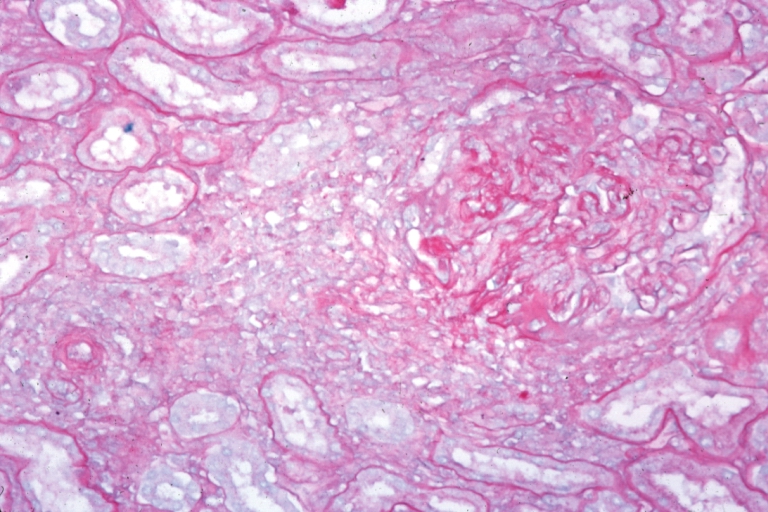
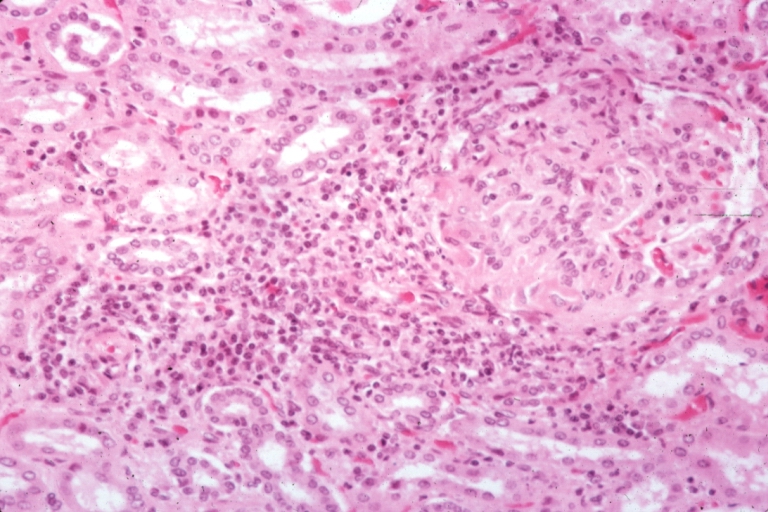
Gross Pathology
- On gross pathology, [feature1], [feature2], and [feature3] are characteristic findings of [disease name].
Microscopic Pathology
- On microscopic histopathological analysis, [feature1], [feature2], and [feature3] are characteristic findings of [disease name].
Videos
{{#ev:youtube|Tw07BFaDEo0}}
References
- ↑ Schwartz N, Goilav B, Putterman C (September 2014). "The pathogenesis, diagnosis and treatment of lupus nephritis". Curr Opin Rheumatol. 26 (5): 502–9. doi:10.1097/BOR.0000000000000089. PMC 4221732. PMID 25014039.
- ↑ He L, Hannon GJ (July 2004). "MicroRNAs: small RNAs with a big role in gene regulation". Nat. Rev. Genet. 5 (7): 522–31. doi:10.1038/nrg1379. PMID 15211354.
- ↑ Yu CC, Yen TS, Lowell CA, DeFranco AL (January 2001). "Lupus-like kidney disease in mice deficient in the Src family tyrosine kinases Lyn and Fyn". Curr. Biol. 11 (1): 34–8. PMID 11166177.
- ↑ Liu Y, Dong J, Mu R, Gao Y, Tan X, Li Y, Li Z, Yang G (June 2013). "MicroRNA-30a promotes B cell hyperactivity in patients with systemic lupus erythematosus by direct interaction with Lyn". Arthritis Rheum. 65 (6): 1603–11. doi:10.1002/art.37912. PMID 23450709.
- ↑ Biesen R, Demir C, Barkhudarova F, Grün JR, Steinbrich-Zöllner M, Backhaus M, Häupl T, Rudwaleit M, Riemekasten G, Radbruch A, Hiepe F, Burmester GR, Grützkau A (April 2008). "Sialic acid-binding Ig-like lectin 1 expression in inflammatory and resident monocytes is a potential biomarker for monitoring disease activity and success of therapy in systemic lupus erythematosus". Arthritis Rheum. 58 (4): 1136–45. doi:10.1002/art.23404. PMID 18383365.
- ↑ Lu J, Kwan BC, Lai FM, Choi PC, Tam LS, Li EK, Chow KM, Wang G, Li PK, Szeto CC (May 2011). "Gene expression of TWEAK/Fn14 and IP-10/CXCR3 in glomerulus and tubulointerstitium of patients with lupus nephritis". Nephrology (Carlton). 16 (4): 426–32. doi:10.1111/j.1440-1797.2011.01449.x. PMID 21303425.
- ↑ Campbell S, Burkly LC, Gao HX, Berman JW, Su L, Browning B, Zheng T, Schiffer L, Michaelson JS, Putterman C (February 2006). "Proinflammatory effects of TWEAK/Fn14 interactions in glomerular mesangial cells". J. Immunol. 176 (3): 1889–98. PMID 16424220.