Lower gastrointestinal bleeding pathophysiology: Difference between revisions
Aditya Ganti (talk | contribs) |
Aditya Ganti (talk | contribs) |
||
| (33 intermediate revisions by 3 users not shown) | |||
| Line 4: | Line 4: | ||
==Overview== | ==Overview== | ||
[[Superior mesenteric artery]] and [[inferior mesenteric artery]] are the two major [[blood vessels]] that supply [[lower gastrointestinal tract]]. Disruption of blood vessel junction, formed by these two vessels, by any of the disease process results in bleeding. [[Diverticulosis]] is the most common etiology of lower GI bleeding accounting for 30% of all cases, followed by [[Anorectal|ano-rectal disease]], [[ischemia]] of bowel, [[inflammatory bowel disease]] ([[Inflammatory bowel disease|IBD]]), [[Colorectal cancer|neoplasia]], and [[Angiodysplasia|arteriovenous (AV) malformations]]. The characteristic gross and microscopic findings of lower [[Gastrointestinal tract|gastrointestinal tracts]] depends upon the underlying pathology. | |||
==Pathophysiology== | ==Pathophysiology== | ||
===Blood supply=== | ===Blood supply=== | ||
* The | * [[Superior mesenteric artery]] and [[inferior mesenteric artery]] are the two major [[blood vessels]] that supply [[lower gastrointestinal tract]].<ref name="pmid11355897">{{cite journal |vauthors=Geboes K, Geboes KP, Maleux G |title=Vascular anatomy of the gastrointestinal tract |journal=Best Pract Res Clin Gastroenterol |volume=15 |issue=1 |pages=1–14 |year=2001 |pmid=11355897 |doi=10.1053/bega.2000.0152 |url=}}</ref><ref name="pmid26140727">{{cite journal |vauthors=Granger DN, Holm L, Kvietys P |title=The Gastrointestinal Circulation: Physiology and Pathophysiology |journal=Compr Physiol |volume=5 |issue=3 |pages=1541–83 |year=2015 |pmid=26140727 |doi=10.1002/cphy.c150007 |url=}}</ref><ref name="urlThe Gastrointestinal Circulation - NCBI Bookshelf">{{cite web |url=https://www.ncbi.nlm.nih.gov/books/NBK53092/ |title=The Gastrointestinal Circulation - NCBI Bookshelf |format= |work= |accessdate=}}</ref> | ||
* This vascular arcade runs in the mesentery close to the bowel | * The [[superior mesenteric artery]] and [[inferior mesenteric artery]] are interconnected through a branch of anastomosis between various branches which are collectively called as [[Marginal artery of the colon|marginal artery]] of Drummond. | ||
* This [[vascular]] arcade runs in the [[mesentery]] close to the [[bowel]]. | |||
{| border="1" cellpadding="5" cellspacing="0" align="center" |class="wikitable" | {| border="1" cellpadding="5" cellspacing="0" align="center" |class="wikitable" | ||
! colspan="2" align="center" style="background:#4479BA; color: #FFFFFF;" |Lower GI Tract | ! colspan="2" align="center" style="background:#4479BA; color: #FFFFFF;" |Lower GI Tract | ||
| Line 16: | Line 15: | ||
! align="center" style="background:#4479BA; color: #FFFFFF;" |Venous Drainage | ! align="center" style="background:#4479BA; color: #FFFFFF;" |Venous Drainage | ||
|- | |- | ||
| style="padding: 5px 5px; background: #DCDCDC;" align="center" |Midgut | | style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Midgut]] | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="left" | | | style="padding: 5px 5px; background: #F5F5F5;" align="left" | | ||
* Distal duodenum | * [[Duodenum|Distal duodenum]] | ||
* Ileum | * [[Jejunum]] | ||
* Appendix | * [[Ileum]] | ||
* Cecum | * [[Appendix]] | ||
* Ascending colon | * [[Cecum]] | ||
* Hepatic flexure | * [[Ascending colon]] | ||
* Proximal transverse colon | * [[Hepatic flexure]] | ||
* [[Transverse colon|Proximal transverse colon]] | |||
| style="padding: 5px 5px; background: #F5F5F5;" align="left" | | | style="padding: 5px 5px; background: #F5F5F5;" align="left" | | ||
* Superior mesenteric artery (SMA) | * [[Superior mesenteric artery]] ([[Superior mesenteric artery|SMA]]) | ||
** [[Ileocolic artery]] | |||
** [[Right colic artery]] | |||
** [[Middle colic artery|Middle colic branches]] | |||
| style="padding: 5px 5px; background: #F5F5F5;" align="left" | | | style="padding: 5px 5px; background: #F5F5F5;" align="left" | | ||
* | * [[Superior mesenteric vein]] | ||
|- | |- | ||
| style="padding: 5px 5px; background: #DCDCDC;" align="center" |Hindgut | | style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Hindgut]] | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="left" | | | style="padding: 5px 5px; background: #F5F5F5;" align="left" | | ||
* Distal one-third of the transverse colon | * [[Distal]] one-third of the [[transverse colon]] | ||
* Splenic flexure | * [[Splenic flexure]] | ||
* Descending colon | * [[Descending colon]] | ||
* Sigmoid colon | * [[Sigmoid colon]] | ||
* | * [[Rectum]] | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="left" | | | style="padding: 5px 5px; background: #F5F5F5;" align="left" | | ||
* Inferior mesenteric artery (IMA) | * [[Inferior mesenteric artery]] ([[Inferior mesenteric artery|IMA]]) | ||
** [[Left colic artery]] | |||
** [[Sigmoid arteries|Sigmoid artery]] | |||
** [[Superior rectal artery|Superior rectal branches]] | |||
| style="padding: 5px 5px; background: #F5F5F5;" align="left" | | | style="padding: 5px 5px; background: #F5F5F5;" align="left" | | ||
* Portal system '''<sup>ɸ</sup>''' | * [[Portal venous system|Portal system]] '''<sup>ɸ</sup>''' | ||
|- | |- | ||
| colspan="4" style="padding: 5px 5px; background: #F5F5F5;" align="center" |ɸ -Except lower rectum, which drains into the systemic circulation. | | colspan="4" style="padding: 5px 5px; background: #F5F5F5;" align="center" |ɸ -Except [[Rectum|lower rectum]], which drains into the [[systemic circulation]]. | ||
|} | |} | ||
| Line 48: | Line 54: | ||
===Pathogenesis=== | ===Pathogenesis=== | ||
The pathogenesis of lower gastrointestinal bleeding can be discussed based on the etiology. Diverticulosis is the most common etiology of lower GI bleeding accounting for 30% of all cases, followed by anorectal disease, ischemia, inflammatory bowel disease (IBD), neoplasia and arteriovenous (AV) malformations. | The pathogenesis of lower gastrointestinal bleeding can be discussed based on the etiology. [[Diverticulosis]] is the most common etiology of lower GI bleeding accounting for 30% of all cases, followed by [[anorectal]] disease, [[ischemia]], [[inflammatory bowel disease]] ([[Inflammatory bowel disease|IBD]]), [[Colorectal cancer|neoplasia]], and [[Angiodysplasia|arteriovenous (AV) malformations]]. | ||
*'''<u>Diverticulosis</u>''' | *'''<u>[[Diverticulosis]]</u>''' | ||
**The colonic wall weakens with age and results in the formation of | **The [[Intestinal wall|colonic wall]] weakens with age and results in the formation of sac-like protrusions known as [[Diverticulum|diverticula]].<ref name="pmid20011269">{{cite journal |vauthors=Hobson KG, Roberts PL |title=Etiology and pathophysiology of diverticular disease |journal=Clin Colon Rectal Surg |volume=17 |issue=3 |pages=147–53 |year=2004 |pmid=20011269 |pmc=2780060 |doi=10.1055/s-2004-832695 |url=}}</ref><ref name="pmid20011276">{{cite journal |vauthors=Maykel JA, Opelka FG |title=Colonic diverticulosis and diverticular hemorrhage |journal=Clin Colon Rectal Surg |volume=17 |issue=3 |pages=195–204 |year=2004 |pmid=20011276 |pmc=2780065 |doi=10.1055/s-2004-832702 |url=}}</ref><ref name="pmid17468551">{{cite journal |vauthors=Comparato G, Pilotto A, Franzè A, Franceschi M, Di Mario F |title=Diverticular disease in the elderly |journal=Dig Dis |volume=25 |issue=2 |pages=151–9 |year=2007 |pmid=17468551 |doi=10.1159/000099480 |url=}}</ref><ref name="pmid20676256">{{cite journal |vauthors=Matrana MR, Margolin DA |title=Epidemiology and pathophysiology of diverticular disease |journal=Clin Colon Rectal Surg |volume=22 |issue=3 |pages=141–6 |year=2009 |pmid=20676256 |pmc=2780269 |doi=10.1055/s-0029-1236157 |url=}}</ref> | ||
**These protrusions generally occur at the junction of blood vessel penetrating through the mucosa and circular muscle fibers of the colon. | **These protrusions generally occur at the junction of [[blood vessel]] penetrating through the [[mucosa]] and circular [[muscle fibers]] of the [[colon]]. | ||
** | **[[Hemorrhage]] results from rupture of the intramural branches ([[vasa recta]]) of the [[marginal artery]] at the dome of a [[diverticulum]] and can give rise to a massive, life-threatening LGIB. | ||
[[Image:Sigmoid diverticulum (diagram).jpg|thumb|center|400px|Diagram of sigmoid diverticulum<br>Source:By Anpol42 (Own work) [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)], via Wikimedia Commons]] | [[Image:Sigmoid diverticulum (diagram).jpg|thumb|center|400px|Diagram of sigmoid diverticulum<br>Source:By Anpol42 (Own work) [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)], via Wikimedia Commons]] | ||
*'''<u>Anorectal disease</u>''' | *'''<u>Anorectal disease</u>''' | ||
:*Hemorrhoids | :*Hemorrhoids are defined as [[Swelling (medical)|swelling]] and [[inflammation]] of [[veins]] in the [[Rectum|rectal]] and [[Anus|anal region]] | ||
:* | :*Hemorrhoids can be either internal or external based on their relation to dentate line. | ||
:* | :*The first step in the pathogenesis of either type of hemorrhoids is weakening of the surrounding connective tissue and vein wall.<ref name="pmid22563187">{{cite journal |vauthors=Lohsiriwat V |title=Hemorrhoids: from basic pathophysiology to clinical management |journal=World J. Gastroenterol. |volume=18 |issue=17 |pages=2009–17 |year=2012 |pmid=22563187 |pmc=3342598 |doi=10.3748/wjg.v18.i17.2009 |url=}}</ref><ref name="pmid22379400">{{cite journal |vauthors=Sanchez C, Chinn BT |title=Hemorrhoids |journal=Clin Colon Rectal Surg |volume=24 |issue=1 |pages=5–13 |year=2011 |pmid=22379400 |pmc=3140328 |doi=10.1055/s-0031-1272818 |url=}}</ref><ref name="pmid22563187">{{cite journal |vauthors=Lohsiriwat V |title=Hemorrhoids: from basic pathophysiology to clinical management |journal=World J. Gastroenterol. |volume=18 |issue=17 |pages=2009–17 |year=2012 |pmid=22563187 |pmc=3342598 |doi=10.3748/wjg.v18.i17.2009 |url=}}</ref> | ||
*'''<u>Mesenteric Ischemia</u>''' | :*Weakening of blood vessels can result in bleeding under pressure. | ||
:*Mesenteric ischemia results when there is inadequate blood supply at the level of the small intestine. | :*An anal fissure can be defined as disruption or tear in the mucosal surface of the skin. | ||
:*2 or more vessels (celiac, SMA, or IMA) must be involved for | :*During defecation, due to increased pressure which can exaggerate the tears may present as bright red rectal bleeding with severe periodic pain.<ref name="pmid3140330">{{cite journal |vauthors=Holland RA, Rimes AF, Comis A, Tyndale-Biscoe CH |title=Oxygen carriage and carbonic anhydrase activity in the blood of a marsupial, the Tammar wallaby (Macropus eugenii), during early development |journal=Respir Physiol |volume=73 |issue=1 |pages=69–86 |year=1988 |pmid=3140330 |doi= |url=}}</ref> | ||
:* | *'''<u>[[Mesenteric ischemia|Mesenteric Ischemia]]</u>''' | ||
:* | :*[[Mesenteric ischemia]] results when there is inadequate blood supply at the level of the [[small intestine]].<ref name="pmid9146726">{{cite journal |vauthors=Krupski WC, Selzman CH, Whitehill TA |title=Unusual causes of mesenteric ischemia |journal=Surg. Clin. North Am. |volume=77 |issue=2 |pages=471–502 |year=1997 |pmid=9146726 |doi= |url=}}</ref><ref name="pmid21326562">{{cite journal |vauthors=Walker TG |title=Mesenteric ischemia |journal=Semin Intervent Radiol |volume=26 |issue=3 |pages=175–83 |year=2009 |pmid=21326562 |pmc=3036494 |doi=10.1055/s-0029-1225662 |url=}}</ref><ref name="pmid18625147">{{cite journal |vauthors=Berland T, Oldenburg WA |title=Acute mesenteric ischemia |journal=Curr Gastroenterol Rep |volume=10 |issue=3 |pages=341–6 |year=2008 |pmid=18625147 |doi= |url=}}</ref><ref name="pmid26909235">{{cite journal |vauthors=Mastoraki A, Mastoraki S, Tziava E, Touloumi S, Krinos N, Danias N, Lazaris A, Arkadopoulos N |title=Mesenteric ischemia: Pathogenesis and challenging diagnostic and therapeutic modalities |journal=World J Gastrointest Pathophysiol |volume=7 |issue=1 |pages=125–30 |year=2016 |pmid=26909235 |pmc=4753178 |doi=10.4291/wjgp.v7.i1.125 |url=}}</ref> | ||
*'''<u>Ischemic Colitis</u>''' | :*2 or more vessels ([[Celiac artery|celiac]], [[Superior mesenteric artery|SMA]], or [[Inferior mesenteric artery|IMA]]) must be involved for bleeding to occur. | ||
:*Ischemic colitis is | :*Decreased blood supply can occur due to obstruction of blood vessel either by emobolus or due to vasoconstriction effect of drugs. | ||
:*Decreased blood supply initiates necrosis of mucosal surface of intestine. | |||
:*The | :*unopposed blood deprivation leads to trans-mural necrosis and ultimately sloughing of the tissues with associated bleeding. | ||
:* | *'''<u>[[Ischemic colitis|Ischemic Colitis]]</u>''' | ||
:*Ischemic colitis is a condition in which injury of the [[large intestine]] results from decreased blood supply.<ref name="pmid26034405">{{cite journal |vauthors=FitzGerald JF, Hernandez Iii LO |title=Ischemic colitis |journal=Clin Colon Rectal Surg |volume=28 |issue=2 |pages=93–8 |year=2015 |pmid=26034405 |pmc=4442720 |doi=10.1055/s-0035-1549099 |url=}}</ref><ref name="pmid19109863">{{cite journal |vauthors=Theodoropoulou A, Koutroubakis IE |title=Ischemic colitis: clinical practice in diagnosis and treatment |journal=World J. Gastroenterol. |volume=14 |issue=48 |pages=7302–8 |year=2008 |pmid=19109863 |pmc=2778113 |doi= |url=}}</ref><ref name="pmid25504381">{{cite journal |vauthors=Rania H, Mériam S, Rym E, Hyafa R, Amine A, Najet BH, Lassad G, Mohamed TK |title=Ischemic colitis in five points: an update 2013 |journal=Tunis Med |volume=92 |issue=5 |pages=299–303 |year=2014 |pmid=25504381 |doi= |url=}}</ref> | |||
*'''<u>Inflammatory Bowel Disease</u>''' | :*The [[Colon (anatomy)|colon]] is most commonly involved due the presence of water shed areas ( splenic flexure and hepatic flexure). | ||
:*Similar to mesentric ischemia bleeding occurs due to necrosis and sloughing of mucosal membrane. | |||
: | *'''<u>Inflammatory Bowel Disease</u>'''<ref name="pmid28261018">{{cite journal |vauthors=Kim DH, Cheon JH |title=Pathogenesis of Inflammatory Bowel Disease and Recent Advances in Biologic Therapies |journal=Immune Netw |volume=17 |issue=1 |pages=25–40 |year=2017 |pmid=28261018 |pmc=5334120 |doi=10.4110/in.2017.17.1.25 |url=}}</ref><ref name="pmid11781268">{{cite journal |vauthors=Hendrickson BA, Gokhale R, Cho JH |title=Clinical aspects and pathophysiology of inflammatory bowel disease |journal=Clin. Microbiol. Rev. |volume=15 |issue=1 |pages=79–94 |year=2002 |pmid=11781268 |pmc=118061 |doi= |url=}}</ref> | ||
**'''[[Crohn's disease]]''' | |||
:*In ulcerative colitis T cells cytotoxic to the colonic epithelium accumulate in the lamina propria, accompanied by B cells that secrete immunoglobulin G (IgG) and IgE. | ***In [[Crohn's disease]], [[T cell]] activation stimulates [[Interleukin 12|interleukin (IL)-12]] and [[Tumor necrosis factor alpha|tumor necrosis factor (TNF)-α]], resulting in [[chronic]] [[inflammation]] and tissue injury.<ref name="pmid4447044">{{cite journal |vauthors=Woźniak-Parnowska W, Werakso B |title=[Comparative studies of microbiological purity of ointments by the direct culture method and use of membrane filters] |language=Polish |journal=Acta Pol Pharm |volume=31 |issue=6 |pages=819–23 |year=1974 |pmid=4447044 |doi= |url=}}</ref><ref name="pmid24395894">{{cite journal |vauthors=Mazal J |title=Crohn disease: pathophysiology, diagnosis, and treatment |journal=Radiol Technol |volume=85 |issue=3 |pages=297–316; quiz 317–20 |year=2014 |pmid=24395894 |doi= |url=}}</ref><ref name="pmid2694136">{{cite journal |vauthors=Jewell DP |title=Aetiology and pathogenesis of ulcerative colitis and Crohn's disease |journal=Postgrad Med J |volume=65 |issue=768 |pages=718–9 |year=1989 |pmid=2694136 |pmc=2429831 |doi= |url=}}</ref><ref name="pmid16819502">{{cite journal |vauthors=Sartor RB |title=Mechanisms of disease: pathogenesis of Crohn's disease and ulcerative colitis |journal=Nat Clin Pract Gastroenterol Hepatol |volume=3 |issue=7 |pages=390–407 |year=2006 |pmid=16819502 |doi=10.1038/ncpgasthep0528 |url=}}</ref><ref name="pmid15656711">{{cite journal |vauthors=Head K, Jurenka JS |title=Inflammatory bowel disease. Part II: Crohn's disease--pathophysiology and conventional and alternative treatment options |journal=Altern Med Rev |volume=9 |issue=4 |pages=360–401 |year=2004 |pmid=15656711 |doi= |url=}}</ref><ref name="pmid24415861">{{cite journal |vauthors=Zhang YZ, Li YY |title=Inflammatory bowel disease: pathogenesis |journal=World J. Gastroenterol. |volume=20 |issue=1 |pages=91–9 |year=2014 |pmid=24415861 |pmc=3886036 |doi=10.3748/wjg.v20.i1.91 |url=}}</ref> | ||
:*This results in inflammation of the crypts of Lieberkuhn, with abscesses and pseudopolyps | ***TNF-alpha induces expression of adhesion factors that allow for inflammatory cells to infiltrate and activates macrophages resulting in granuloma formations | ||
:* | ***The inflammatory response invades through the entire thickness of the bowel wall weakening the surrounding blood vessels resulting in bleeding. | ||
:* '''<u>Ulcerative colitis</u>''' | |||
:** In [[ulcerative colitis]], [[T cells]], [[cytotoxic]] to the colonic epithelium, accumulate in the [[lamina propria]], accompanied by [[B cells]] that secrete [[immunoglobulin G]] ([[Immunoglobulin G|IgG]]) and [[Immunoglobulin E|IgE]].<ref name="pmid16819502">{{cite journal |vauthors=Sartor RB |title=Mechanisms of disease: pathogenesis of Crohn's disease and ulcerative colitis |journal=Nat Clin Pract Gastroenterol Hepatol |volume=3 |issue=7 |pages=390–407 |year=2006 |pmid=16819502 |doi=10.1038/ncpgasthep0528 |url=}}</ref><ref name="pmid27914657">{{cite journal |vauthors=Ungaro R, Mehandru S, Allen PB, Peyrin-Biroulet L, Colombel JF |title=Ulcerative colitis |journal=Lancet |volume=389 |issue=10080 |pages=1756–1770 |year=2017 |pmid=27914657 |doi=10.1016/S0140-6736(16)32126-2 |url=}}</ref><ref name="pmid11830216">{{cite journal |vauthors=Farrell RJ, Peppercorn MA |title=Ulcerative colitis |journal=Lancet |volume=359 |issue=9303 |pages=331–40 |year=2002 |pmid=11830216 |doi=10.1016/S0140-6736(02)07499-8 |url=}}</ref><ref name="pmid1516252">{{cite journal |vauthors=Rönnblom LE, Janson ET, Perers A, Oberg KE, Alm GV |title=Characterization of anti-interferon-alpha antibodies appearing during recombinant interferon-alpha 2a treatment |journal=Clin. Exp. Immunol. |volume=89 |issue=3 |pages=330–5 |year=1992 |pmid=1516252 |pmc=1554468 |doi= |url=}}</ref> | |||
:** This results in [[inflammation]] of the [[crypts of Lieberkuhn]], with [[abscesses]] and [[pseudopolyps]] along with | |||
:** rupturing of minute [[blood vessels]] in [[mucosa]] resulting in bleeding. | |||
*'''<u>Neoplasia</u>''' | *'''<u>Neoplasia</u>''' | ||
**Colon cancer arises mostly due to sporadic mutations that originates from the [[epithelial cells]] of [[colon]] or [[rectum]]. | |||
**Genetic instability/mutation results in [[Epigenetic|epigenetic alteration]], [[chronic inflammation]], [[oxidative stress]], and intestinal [[microbiota]].<ref name="pmid12702969">{{cite journal |vauthors=Itzkowitz S |title=Colon carcinogenesis in inflammatory bowel disease: applying molecular genetics to clinical practice |journal=J. Clin. Gastroenterol. |volume=36 |issue=5 Suppl |pages=S70–4; discussion S94–6 |year=2003 |pmid=12702969 |doi= |url=}}</ref><ref name="pmid21530747">{{cite journal |vauthors=Ullman TA, Itzkowitz SH |title=Intestinal inflammation and cancer |journal=Gastroenterology |volume=140 |issue=6 |pages=1807–16 |year=2011 |pmid=21530747 |doi=10.1053/j.gastro.2011.01.057 |url=}}</ref><ref name="pmid19589728">{{cite journal |vauthors=Kraus S, Arber N |title=Inflammation and colorectal cancer |journal=Curr Opin Pharmacol |volume=9 |issue=4 |pages=405–10 |year=2009 |pmid=19589728 |doi=10.1016/j.coph.2009.06.006 |url=}}</ref> | |||
**As [[tumor]] tends to grow slowly it invades the surrounding tissue disrupting the normal blood vessels along with it. | |||
**This is responsible for slow occult bleeding that is found positive on FOBT. | |||
*'''<u>AV Malformation/Angiodysplasia</u>''' | *'''<u>AV Malformation/Angiodysplasia</u>''' | ||
:*In AV malformation | :*In [[Arteriovenous malformations|AV malformation]] abnormal connections occur between [[arteries]] and [[veins]].<ref name="pmid8389094">{{cite journal |vauthors=Foutch PG |title=Angiodysplasia of the gastrointestinal tract |journal=Am. J. Gastroenterol. |volume=88 |issue=6 |pages=807–18 |year=1993 |pmid=8389094 |doi= |url=}}</ref><ref name="pmid9048468">{{cite journal |vauthors=Dodda G, Trotman BW |title=Gastrointestinal angiodysplasia |journal=J Assoc Acad Minor Phys |volume=8 |issue=1 |pages=16–9 |year=1997 |pmid=9048468 |doi= |url=}}</ref><ref name="pmid1744847">{{cite journal |vauthors=Kheterpal S |title=Angiodysplasia: a review |journal=J R Soc Med |volume=84 |issue=10 |pages=615–8 |year=1991 |pmid=1744847 |pmc=1295562 |doi= |url=}}</ref><ref name="pmid311247">{{cite journal |vauthors=Athanasoulis CA, Galdabini JJ, Waltman AC, Novelline RA, Greenfield AJ, Ezpeleta ML |title=Angiodysplasia of the colon: a cause of rectal bleeding |journal=Cardiovasc Radiol |volume=1 |issue=1 |pages=3–13 |year=1977 |pmid=311247 |doi= |url=}}</ref><ref name="pmid24138285">{{cite journal |vauthors=Sami SS, Al-Araji SA, Ragunath K |title=Review article: gastrointestinal angiodysplasia - pathogenesis, diagnosis and management |journal=Aliment. Pharmacol. Ther. |volume=39 |issue=1 |pages=15–34 |year=2014 |pmid=24138285 |doi=10.1111/apt.12527 |url=}}</ref> | ||
:*The lack of capillary buffers | :*This connections results in blood flow from high pressure arteries to low pressure veins without buffering effects of capillaries. | ||
:*In Angiodysplasia | :*The lack of [[capillary]] buffers makes the [[vessels]] weak due to increased blood flow and ultimately bleeding. | ||
:* | :*In [[Angiodysplasia]], with age the connective tissue of the blood vessels become weak. | ||
:*With mild increase in pressure leads to disrupture of vessels leading to painless bleeding. | |||
==Associated Conditions== | ==Associated Conditions== | ||
Other diseases that are commonly associated with lower gastrointestinal bleeding include: | |||
*Aortoenteric [[fistula]] | |||
*[[Abdominal aortic aneurysm|Abdominal aortic aneurysms]] | |||
*[[Peutz-Jeghers syndrome]] | |||
*[[Klippel-Trenaunay-Weber syndrome]] | |||
*[[Hereditary hemorrhagic telangiectasia]] | |||
*[[Neurofibromatosis]] | |||
*[[Blue rubber bleb syndrome]] | |||
==Gross Pathology== | ==Gross and Microscopic Pathology== | ||
{| class="wikitable" | |||
!Disease | |||
!Gross Pathology | |||
!Microscopic Pathology | |||
|- | |||
|[[Diverticulosis]]<ref name="pmid15115923">{{cite journal |vauthors=West AB, Losada M |title=The pathology of diverticulosis coli |journal=J. Clin. Gastroenterol. |volume=38 |issue=5 Suppl 1 |pages=S11–6 |year=2004 |pmid=15115923 |doi= |url=}}</ref> | |||
| | |||
* Numerous visible flask like protrusions along the [[intestinal wall]]. | |||
* Thick and corrugated circular [[muscle fibers]] with mucosal folds. | |||
| | |||
* Numerous [[Inflammatory cells|cells of inflammation]] | |||
* [[Ganglion cells|Intramucosal ganglion cells]] | |||
* [[Lymphoid]] infiltrate | |||
* [[Cryptitis|Mild cryptitis]] | |||
* [[Paneth cells|Paneth cell metaplasia]] | |||
* [[Ulcers]] | |||
|- | |||
|[[Angiodysplasia]]<ref name="pmid4029903">{{cite journal |vauthors=Stamm B, Heer M, Bühler H, Ammann R |title=Mucosal biopsy of vascular ectasia (angiodysplasia) of the large bowel detected during routine colonoscopic examination |journal=Histopathology |volume=9 |issue=6 |pages=639–46 |year=1985 |pmid=4029903 |doi= |url=}}</ref> | |||
| | |||
* Tortuous dilatation of multiple small [[submucosal]] and [[mucosal]] blood vessels. | |||
| | |||
* Clusters of numerous dilated and thin-walled [[vessels]] in [[mucosa]] and [[Submucosal|submucosa]]. | |||
* Erosion of surrounding [[mucosa]] | |||
|- | |||
|[[Hemorrhoids]]<ref name="pmid22563187">{{cite journal |vauthors=Lohsiriwat V |title=Hemorrhoids: from basic pathophysiology to clinical management |journal=World J. Gastroenterol. |volume=18 |issue=17 |pages=2009–17 |year=2012 |pmid=22563187 |pmc=3342598 |doi=10.3748/wjg.v18.i17.2009 |url=}}</ref> | |||
| | |||
* Tortuous superficial dilatations of multiple blood vessels. | |||
| | |||
* Dilated, thick-walled, [[congested]] [[submucosal]] [[vessels]] | |||
* [[Papillary]] [[endothelial]] [[hyperplasia]] | |||
* [[Superficial]] [[ulcerations]] | |||
* [[Pagetoid]] dyskeratosis | |||
|- | |||
|[[Mesenteric ischemia]] <ref name="pmid1731389">{{cite journal |vauthors=Mitsudo S, Brandt LJ |title=Pathology of intestinal ischemia |journal=Surg. Clin. North Am. |volume=72 |issue=1 |pages=43–63 |year=1992 |pmid=1731389 |doi= |url=}}</ref> | |||
| | |||
* [[Hemorrhagic]] [[Infarction|infarctions]] | |||
== | * [[Ulcerations]] | ||
* [[Strictures]] | |||
| | |||
* [[Hemorrhage]] in [[lamina propria]] | |||
* [[Necrosis]] of superficial [[epithelial cells]] | |||
* Deep crypts | |||
* [[Fibrosis]] | |||
|- | |||
|[[Ischemic colitis]]<ref name="pmid1731389">{{cite journal |vauthors=Mitsudo S, Brandt LJ |title=Pathology of intestinal ischemia |journal=Surg. Clin. North Am. |volume=72 |issue=1 |pages=43–63 |year=1992 |pmid=1731389 |doi= |url=}}</ref> | |||
| | |||
* Discrete or [[serpiginous]] [[ulcerations]] | |||
* [[Pseudopolyps]] | |||
* [[Hemorrhagic]] [[Infarction|infarctions]] | |||
* Frank blood or dark mucus in lumen | |||
* [[Strictures]] | |||
| | |||
* [[Necrotizing]] [[phlebitis]] | |||
* Multiple thrombi | |||
* [[Ulcerations]] | |||
* [[Granulation tissue]] extending into surrounding [[submucosa]] and smooth muscle fibers. | |||
|- | |||
|[[Crohn's disease]]<ref name="pmid1089084">{{cite journal |vauthors=Price AB, Morson BC |title=Inflammatory bowel disease: the surgical pathology of Crohn's disease and ulcerative colitis |journal=Hum. Pathol. |volume=6 |issue=1 |pages=7–29 |year=1975 |pmid=1089084 |doi= |url=}}</ref><ref name="pmid9537465">{{cite journal |vauthors=Wright CL, Riddell RH |title=Histology of the stomach and duodenum in Crohn's disease |journal=Am. J. Surg. Pathol. |volume=22 |issue=4 |pages=383–90 |year=1998 |pmid=9537465 |doi= |url=}}</ref> | |||
| | |||
* Creeping fat | |||
* Thick/rubbery [[intestinal wall]] | |||
* [[Strictures]] (string sign on barium enema) | |||
* Skip areas | |||
* [[Aphthous ulcers|Aphthous mucosal ulcers]] | |||
| | |||
* Superficial or deep [[ulcerations]] | |||
* [[Granulation tissue]] extending into surrounding [[submucosa]] and smooth muscle fibers. | |||
* Transmural inflammation with lymphoid aggregates | |||
* [[Goblet cells]] | |||
* Focal [[neutrophils]] in [[epithelium]] | |||
* [[Lymphoid]] aggregates | |||
* [[Plasmacytosis]] | |||
* Edematous [[mucosa]] and [[submucosa]] | |||
|- | |||
|[[Ulcerative colitis]]<ref name="pmid24942757">{{cite journal |vauthors=DeRoche TC, Xiao SY, Liu X |title=Histological evaluation in ulcerative colitis |journal=Gastroenterol Rep (Oxf) |volume=2 |issue=3 |pages=178–92 |year=2014 |pmid=24942757 |pmc=4124271 |doi=10.1093/gastro/gou031 |url=}}</ref> | |||
| | |||
* Deep fissuring [[ulcerations]] | |||
* [[Hemorrhagic]] [[mucosa]] | |||
* [[Pseudopolyps]] | |||
| | |||
* [[Mononuclear cells|Mononuclear]] inflammatory infiltrate in [[lamina propria]] | |||
* [[Crypt (anatomy)|Crypt]] [[abscesses]] | |||
* [[Granulation tissue]] extending into surrounding [[submucosa]] and smooth muscle fibers. | |||
* [[Submucosal]] [[fibrosis]] | |||
* [[Schwann cell]] [[proliferation]] | |||
|} | |||
==References== | ==References== | ||
Latest revision as of 22:47, 28 December 2017
|
Lower gastrointestinal bleeding Microchapters |
|
Differentiating Lower gastrointestinal bleeding from other Diseases |
|---|
|
Diagnosis |
|
Treatment |
|
Management |
|
Surgery |
|
Case Studies |
|
Lower gastrointestinal bleeding pathophysiology On the Web |
|
American Roentgen Ray Society Images of Lower gastrointestinal bleeding pathophysiology |
|
Risk calculators and risk factors for Lower gastrointestinal bleeding pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Aditya Ganti M.B.B.S. [2]
Overview
Superior mesenteric artery and inferior mesenteric artery are the two major blood vessels that supply lower gastrointestinal tract. Disruption of blood vessel junction, formed by these two vessels, by any of the disease process results in bleeding. Diverticulosis is the most common etiology of lower GI bleeding accounting for 30% of all cases, followed by ano-rectal disease, ischemia of bowel, inflammatory bowel disease (IBD), neoplasia, and arteriovenous (AV) malformations. The characteristic gross and microscopic findings of lower gastrointestinal tracts depends upon the underlying pathology.
Pathophysiology
Blood supply
- Superior mesenteric artery and inferior mesenteric artery are the two major blood vessels that supply lower gastrointestinal tract.[1][2][3]
- The superior mesenteric artery and inferior mesenteric artery are interconnected through a branch of anastomosis between various branches which are collectively called as marginal artery of Drummond.
- This vascular arcade runs in the mesentery close to the bowel.
| Lower GI Tract | Arterial Supply | Venous Drainage | |
|---|---|---|---|
| Midgut | |||
| Hindgut |
|
||
| ɸ -Except lower rectum, which drains into the systemic circulation. | |||

Source: By Anpol42 (Own work) [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)], via Wikimedia Commons
Pathogenesis
The pathogenesis of lower gastrointestinal bleeding can be discussed based on the etiology. Diverticulosis is the most common etiology of lower GI bleeding accounting for 30% of all cases, followed by anorectal disease, ischemia, inflammatory bowel disease (IBD), neoplasia, and arteriovenous (AV) malformations.
- Diverticulosis
- The colonic wall weakens with age and results in the formation of sac-like protrusions known as diverticula.[4][5][6][7]
- These protrusions generally occur at the junction of blood vessel penetrating through the mucosa and circular muscle fibers of the colon.
- Hemorrhage results from rupture of the intramural branches (vasa recta) of the marginal artery at the dome of a diverticulum and can give rise to a massive, life-threatening LGIB.
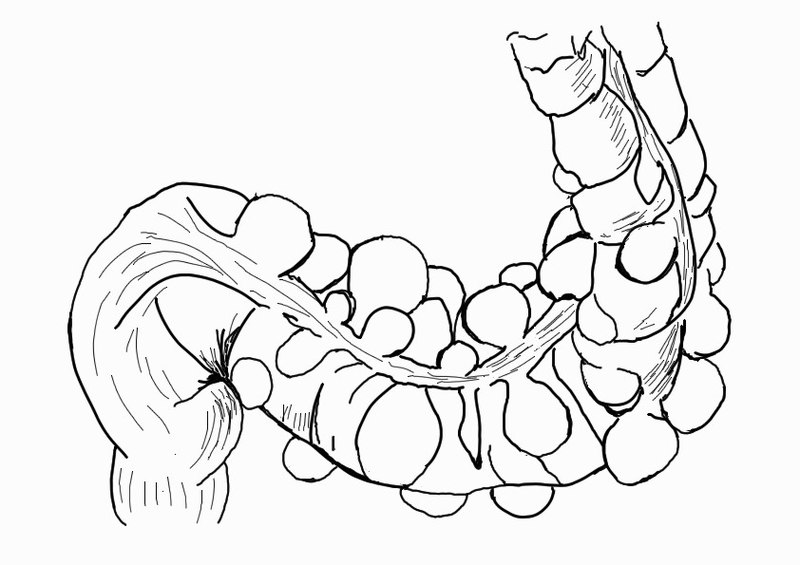
Source:By Anpol42 (Own work) [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)], via Wikimedia Commons
- Anorectal disease
- Hemorrhoids are defined as swelling and inflammation of veins in the rectal and anal region
- Hemorrhoids can be either internal or external based on their relation to dentate line.
- The first step in the pathogenesis of either type of hemorrhoids is weakening of the surrounding connective tissue and vein wall.[8][9][8]
- Weakening of blood vessels can result in bleeding under pressure.
- An anal fissure can be defined as disruption or tear in the mucosal surface of the skin.
- During defecation, due to increased pressure which can exaggerate the tears may present as bright red rectal bleeding with severe periodic pain.[10]
- Mesenteric ischemia results when there is inadequate blood supply at the level of the small intestine.[11][12][13][14]
- 2 or more vessels (celiac, SMA, or IMA) must be involved for bleeding to occur.
- Decreased blood supply can occur due to obstruction of blood vessel either by emobolus or due to vasoconstriction effect of drugs.
- Decreased blood supply initiates necrosis of mucosal surface of intestine.
- unopposed blood deprivation leads to trans-mural necrosis and ultimately sloughing of the tissues with associated bleeding.
- Ischemic colitis is a condition in which injury of the large intestine results from decreased blood supply.[15][16][17]
- The colon is most commonly involved due the presence of water shed areas ( splenic flexure and hepatic flexure).
- Similar to mesentric ischemia bleeding occurs due to necrosis and sloughing of mucosal membrane.
- Inflammatory Bowel Disease[18][19]
- Crohn's disease
- In Crohn's disease, T cell activation stimulates interleukin (IL)-12 and tumor necrosis factor (TNF)-α, resulting in chronic inflammation and tissue injury.[20][21][22][23][24][25]
- TNF-alpha induces expression of adhesion factors that allow for inflammatory cells to infiltrate and activates macrophages resulting in granuloma formations
- The inflammatory response invades through the entire thickness of the bowel wall weakening the surrounding blood vessels resulting in bleeding.
- Crohn's disease
- Ulcerative colitis
- In ulcerative colitis, T cells, cytotoxic to the colonic epithelium, accumulate in the lamina propria, accompanied by B cells that secrete immunoglobulin G (IgG) and IgE.[23][26][27][28]
- This results in inflammation of the crypts of Lieberkuhn, with abscesses and pseudopolyps along with
- rupturing of minute blood vessels in mucosa resulting in bleeding.
- Ulcerative colitis
- Neoplasia
- Colon cancer arises mostly due to sporadic mutations that originates from the epithelial cells of colon or rectum.
- Genetic instability/mutation results in epigenetic alteration, chronic inflammation, oxidative stress, and intestinal microbiota.[29][30][31]
- As tumor tends to grow slowly it invades the surrounding tissue disrupting the normal blood vessels along with it.
- This is responsible for slow occult bleeding that is found positive on FOBT.
- AV Malformation/Angiodysplasia
- In AV malformation abnormal connections occur between arteries and veins.[32][33][34][35][36]
- This connections results in blood flow from high pressure arteries to low pressure veins without buffering effects of capillaries.
- The lack of capillary buffers makes the vessels weak due to increased blood flow and ultimately bleeding.
- In Angiodysplasia, with age the connective tissue of the blood vessels become weak.
- With mild increase in pressure leads to disrupture of vessels leading to painless bleeding.
Associated Conditions
Other diseases that are commonly associated with lower gastrointestinal bleeding include:
- Aortoenteric fistula
- Abdominal aortic aneurysms
- Peutz-Jeghers syndrome
- Klippel-Trenaunay-Weber syndrome
- Hereditary hemorrhagic telangiectasia
- Neurofibromatosis
- Blue rubber bleb syndrome
Gross and Microscopic Pathology
| Disease | Gross Pathology | Microscopic Pathology |
|---|---|---|
| Diverticulosis[37] |
|
|
| Angiodysplasia[38] |
|
|
| Hemorrhoids[8] |
|
|
| Mesenteric ischemia [39] |
| |
| Ischemic colitis[39] |
|
|
| Crohn's disease[40][41] |
|
|
| Ulcerative colitis[42] |
|
|
References
- ↑ Geboes K, Geboes KP, Maleux G (2001). "Vascular anatomy of the gastrointestinal tract". Best Pract Res Clin Gastroenterol. 15 (1): 1–14. doi:10.1053/bega.2000.0152. PMID 11355897.
- ↑ Granger DN, Holm L, Kvietys P (2015). "The Gastrointestinal Circulation: Physiology and Pathophysiology". Compr Physiol. 5 (3): 1541–83. doi:10.1002/cphy.c150007. PMID 26140727.
- ↑ "The Gastrointestinal Circulation - NCBI Bookshelf".
- ↑ Hobson KG, Roberts PL (2004). "Etiology and pathophysiology of diverticular disease". Clin Colon Rectal Surg. 17 (3): 147–53. doi:10.1055/s-2004-832695. PMC 2780060. PMID 20011269.
- ↑ Maykel JA, Opelka FG (2004). "Colonic diverticulosis and diverticular hemorrhage". Clin Colon Rectal Surg. 17 (3): 195–204. doi:10.1055/s-2004-832702. PMC 2780065. PMID 20011276.
- ↑ Comparato G, Pilotto A, Franzè A, Franceschi M, Di Mario F (2007). "Diverticular disease in the elderly". Dig Dis. 25 (2): 151–9. doi:10.1159/000099480. PMID 17468551.
- ↑ Matrana MR, Margolin DA (2009). "Epidemiology and pathophysiology of diverticular disease". Clin Colon Rectal Surg. 22 (3): 141–6. doi:10.1055/s-0029-1236157. PMC 2780269. PMID 20676256.
- ↑ 8.0 8.1 8.2 Lohsiriwat V (2012). "Hemorrhoids: from basic pathophysiology to clinical management". World J. Gastroenterol. 18 (17): 2009–17. doi:10.3748/wjg.v18.i17.2009. PMC 3342598. PMID 22563187.
- ↑ Sanchez C, Chinn BT (2011). "Hemorrhoids". Clin Colon Rectal Surg. 24 (1): 5–13. doi:10.1055/s-0031-1272818. PMC 3140328. PMID 22379400.
- ↑ Holland RA, Rimes AF, Comis A, Tyndale-Biscoe CH (1988). "Oxygen carriage and carbonic anhydrase activity in the blood of a marsupial, the Tammar wallaby (Macropus eugenii), during early development". Respir Physiol. 73 (1): 69–86. PMID 3140330.
- ↑ Krupski WC, Selzman CH, Whitehill TA (1997). "Unusual causes of mesenteric ischemia". Surg. Clin. North Am. 77 (2): 471–502. PMID 9146726.
- ↑ Walker TG (2009). "Mesenteric ischemia". Semin Intervent Radiol. 26 (3): 175–83. doi:10.1055/s-0029-1225662. PMC 3036494. PMID 21326562.
- ↑ Berland T, Oldenburg WA (2008). "Acute mesenteric ischemia". Curr Gastroenterol Rep. 10 (3): 341–6. PMID 18625147.
- ↑ Mastoraki A, Mastoraki S, Tziava E, Touloumi S, Krinos N, Danias N, Lazaris A, Arkadopoulos N (2016). "Mesenteric ischemia: Pathogenesis and challenging diagnostic and therapeutic modalities". World J Gastrointest Pathophysiol. 7 (1): 125–30. doi:10.4291/wjgp.v7.i1.125. PMC 4753178. PMID 26909235.
- ↑ FitzGerald JF, Hernandez Iii LO (2015). "Ischemic colitis". Clin Colon Rectal Surg. 28 (2): 93–8. doi:10.1055/s-0035-1549099. PMC 4442720. PMID 26034405.
- ↑ Theodoropoulou A, Koutroubakis IE (2008). "Ischemic colitis: clinical practice in diagnosis and treatment". World J. Gastroenterol. 14 (48): 7302–8. PMC 2778113. PMID 19109863.
- ↑ Rania H, Mériam S, Rym E, Hyafa R, Amine A, Najet BH, Lassad G, Mohamed TK (2014). "Ischemic colitis in five points: an update 2013". Tunis Med. 92 (5): 299–303. PMID 25504381.
- ↑ Kim DH, Cheon JH (2017). "Pathogenesis of Inflammatory Bowel Disease and Recent Advances in Biologic Therapies". Immune Netw. 17 (1): 25–40. doi:10.4110/in.2017.17.1.25. PMC 5334120. PMID 28261018.
- ↑ Hendrickson BA, Gokhale R, Cho JH (2002). "Clinical aspects and pathophysiology of inflammatory bowel disease". Clin. Microbiol. Rev. 15 (1): 79–94. PMC 118061. PMID 11781268.
- ↑ Woźniak-Parnowska W, Werakso B (1974). "[Comparative studies of microbiological purity of ointments by the direct culture method and use of membrane filters]". Acta Pol Pharm (in Polish). 31 (6): 819–23. PMID 4447044.
- ↑ Mazal J (2014). "Crohn disease: pathophysiology, diagnosis, and treatment". Radiol Technol. 85 (3): 297–316, quiz 317–20. PMID 24395894.
- ↑ Jewell DP (1989). "Aetiology and pathogenesis of ulcerative colitis and Crohn's disease". Postgrad Med J. 65 (768): 718–9. PMC 2429831. PMID 2694136.
- ↑ 23.0 23.1 Sartor RB (2006). "Mechanisms of disease: pathogenesis of Crohn's disease and ulcerative colitis". Nat Clin Pract Gastroenterol Hepatol. 3 (7): 390–407. doi:10.1038/ncpgasthep0528. PMID 16819502.
- ↑ Head K, Jurenka JS (2004). "Inflammatory bowel disease. Part II: Crohn's disease--pathophysiology and conventional and alternative treatment options". Altern Med Rev. 9 (4): 360–401. PMID 15656711.
- ↑ Zhang YZ, Li YY (2014). "Inflammatory bowel disease: pathogenesis". World J. Gastroenterol. 20 (1): 91–9. doi:10.3748/wjg.v20.i1.91. PMC 3886036. PMID 24415861.
- ↑ Ungaro R, Mehandru S, Allen PB, Peyrin-Biroulet L, Colombel JF (2017). "Ulcerative colitis". Lancet. 389 (10080): 1756–1770. doi:10.1016/S0140-6736(16)32126-2. PMID 27914657.
- ↑ Farrell RJ, Peppercorn MA (2002). "Ulcerative colitis". Lancet. 359 (9303): 331–40. doi:10.1016/S0140-6736(02)07499-8. PMID 11830216.
- ↑ Rönnblom LE, Janson ET, Perers A, Oberg KE, Alm GV (1992). "Characterization of anti-interferon-alpha antibodies appearing during recombinant interferon-alpha 2a treatment". Clin. Exp. Immunol. 89 (3): 330–5. PMC 1554468. PMID 1516252.
- ↑ Itzkowitz S (2003). "Colon carcinogenesis in inflammatory bowel disease: applying molecular genetics to clinical practice". J. Clin. Gastroenterol. 36 (5 Suppl): S70–4, discussion S94–6. PMID 12702969.
- ↑ Ullman TA, Itzkowitz SH (2011). "Intestinal inflammation and cancer". Gastroenterology. 140 (6): 1807–16. doi:10.1053/j.gastro.2011.01.057. PMID 21530747.
- ↑ Kraus S, Arber N (2009). "Inflammation and colorectal cancer". Curr Opin Pharmacol. 9 (4): 405–10. doi:10.1016/j.coph.2009.06.006. PMID 19589728.
- ↑ Foutch PG (1993). "Angiodysplasia of the gastrointestinal tract". Am. J. Gastroenterol. 88 (6): 807–18. PMID 8389094.
- ↑ Dodda G, Trotman BW (1997). "Gastrointestinal angiodysplasia". J Assoc Acad Minor Phys. 8 (1): 16–9. PMID 9048468.
- ↑ Kheterpal S (1991). "Angiodysplasia: a review". J R Soc Med. 84 (10): 615–8. PMC 1295562. PMID 1744847.
- ↑ Athanasoulis CA, Galdabini JJ, Waltman AC, Novelline RA, Greenfield AJ, Ezpeleta ML (1977). "Angiodysplasia of the colon: a cause of rectal bleeding". Cardiovasc Radiol. 1 (1): 3–13. PMID 311247.
- ↑ Sami SS, Al-Araji SA, Ragunath K (2014). "Review article: gastrointestinal angiodysplasia - pathogenesis, diagnosis and management". Aliment. Pharmacol. Ther. 39 (1): 15–34. doi:10.1111/apt.12527. PMID 24138285.
- ↑ West AB, Losada M (2004). "The pathology of diverticulosis coli". J. Clin. Gastroenterol. 38 (5 Suppl 1): S11–6. PMID 15115923.
- ↑ Stamm B, Heer M, Bühler H, Ammann R (1985). "Mucosal biopsy of vascular ectasia (angiodysplasia) of the large bowel detected during routine colonoscopic examination". Histopathology. 9 (6): 639–46. PMID 4029903.
- ↑ 39.0 39.1 Mitsudo S, Brandt LJ (1992). "Pathology of intestinal ischemia". Surg. Clin. North Am. 72 (1): 43–63. PMID 1731389.
- ↑ Price AB, Morson BC (1975). "Inflammatory bowel disease: the surgical pathology of Crohn's disease and ulcerative colitis". Hum. Pathol. 6 (1): 7–29. PMID 1089084.
- ↑ Wright CL, Riddell RH (1998). "Histology of the stomach and duodenum in Crohn's disease". Am. J. Surg. Pathol. 22 (4): 383–90. PMID 9537465.
- ↑ DeRoche TC, Xiao SY, Liu X (2014). "Histological evaluation in ulcerative colitis". Gastroenterol Rep (Oxf). 2 (3): 178–92. doi:10.1093/gastro/gou031. PMC 4124271. PMID 24942757.