COVID-19-associated coagulopathy
|
COVID-19 Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
COVID-19-associated coagulopathy On the Web |
|
American Roentgen Ray Society Images of COVID-19-associated coagulopathy |
|
Risk calculators and risk factors for COVID-19-associated coagulopathy |
For COVID-19 frequently asked inpatient questions, click here
For COVID-19 frequently asked outpatient questions, click here
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Ifrah Fatima, M.B.B.S[2]
Synonyms and keywords: Hematological findings and COVID-19, hypercoagulability in COVID-19, clotting disorder in COVID-19
Overview
Hypercoagulability is a major complication seen in as many as 31% of patients with COVID-19. It leads to many life-threatening outcomes with pulmonary embolism being the most common thrombotic complication. Fibrinogen and D-dimer levels are elevated. Coagulopathy in COVID-19 must be differentiated from other diseases that cause disseminated intravascular coagulation (DIC). Prophylactic anticoagulation with low molecular weight heparin is given to all inpatients in the absence of active bleeding. Full dose anticoagulation is done in patients with documented and confirmed venous thromboembolism (VTE) .
Historical Perspective
- The etiological agent is SARS-CoV-2, named for the similarity of its symptoms to those induced by the severe acute respiratory syndrome, causing coronavirus disease 2019 (COVID-19), is a virus identified as the cause of an outbreak of respiratory illness first detected in Wuhan, China.
- The growing number of patients however, suggest that human-to-human transmission is actively occurring.
- The outbreak was declared a Public Health Emergency of International Concern on 30 January 2020.
- On March 12, 2020, the World Health Organization declared the COVID-19 outbreak a pandemic.
Classification
- There is no established system for the classification of the hypercoagulability seen in COVID-19.
- The coagulopathy may be classified according to the type of vessels and organs involved into:
- To view the classification of COVID-19, click here.
Pathophysiology
- COVID-19 induces a hypercoagulable state in the body. An increased risk of mortality has been noted in patient’s with coagulopathy in COVID-19. It is thought that the coagulopathy in COVID-19 is the result of:[1]
- Virchow’s triad
- Vascular endothelial damage
- Endothelitis- direct invasion of endothelial cells by SARS-CoV-2 which exposes the vWF associated with a massive release of vWF, eventually activating the coagulation cascade.
- Complement mediated damage to pericytes
- Pro-inflammatory cytokines- IL-1, IL-6, and TNF- α, that activate the coagulation pathway and the fibrinolytic system.
- Stasis- Prolonged hospital admissions causing immobilization of the patient
- Hypercoagulabe state- Evidenced by elevated fibrinogen, prothrombotic factors and hyperviscosity
- Some patients have been found to have Lupus anticoagulant (anti-cardiolipin) and anti-β2GP1 antibodies that may be contributory.
Causes
- Coronavirus disease 2019 (COVID-19) is caused by a novel coronavirus called SARS-CoV-2 and is the cause of thrombocytopenia in COVID-19 infection.
- To view causes of COVID-19, click here.
Differentiating COVID-19 associated coagulopathy from other Diseases
- Coagulopathy in COVID-19 must be differentiated from other diseases that cause DIC which include the folowing:
- The main feature of COVID-19 coagulopathy is thrombosis while the acute phase of DIC presents with bleeding:
- Similar laboratory findings are marked increase in D-dimer and normal/slightly low platelets and prolonged PT.
- Findings distinct in COVID 19 are high fibrinogen and high factor VIII activity
- The scoring system of the International Society on Thrombosis and Hemostasis should be used to detect DIC (platelet count, PT, fibrinogen, D‐dimer, antithrombin and protein C activity monitoring), but the diagnosis and subsequent treatment should be done clinically.
To view the differential diagnosis of COVID-19, click here.
Epidemiology and Demographics
Incidence
- The incidence of venous thromboembolism in ICU patients with COVID-19 was analyzed in a study by Klok et al.
- It concluded that the cumulative incidence of acute pulmonary embolism (PE), deep vein thrombosis (DVT), ischemic stroke, MI, or systemic arterial embolism was 31%.
- The incidence of most common thrombotic complication was pulmonary embolism seen in 81% of patients. All these patients were on at least standard doses of thromboprophylaxis. [2]
- The cumulative incidence of venous thromboembolism (VTE) were 16% (95% CI, 10-22) at 7 days, 33% (95% CI, 23-43) at 14 days and 42% (95% CI 30-54) at 21 days.
- Comparatively, the cumulative incidence of venous thromboembolism (VTE) was higher in the ICU patients - 26% (95% CI, 17-37) at 7 days, 47% (95% CI, 34-58) at 14 days and 59% (95% CI, 42-72) at 21 days) than on the floor.
To view the epidemiology and demographics for COVID-19, click here.
Age
- There is insufficient information regarding age-specific prevalence or incidence of COVID-19-associated coagulopathy.
Gender
- There is insufficient information regarding gender-specific prevalence or incidence of COVID-19-associated coagulopathy.
Race
- There is insufficient information regarding race-specific prevalence or incidence of COVID-19-associated coagulopathy.
Risk Factors
Common hypothesized risk factors for coagulopathy in COVID-19 pneumonia based on studies include:
Other general risk factors for venous thromboembolism (VTE) are:
To view the risk factors of COVID-19, click here.
Screening
- Every patient with COVID-19 infection admitted to the hospital should have a baseline of basic blood investigations such as
- Complete blood count (CBC)
- Platelet count
- Prothrombin Time (PT), Activated partial thromboplastin time (aPTT)
- Fibrinogen
- D-dimer
- C-reactive protein
- Routine screening with imaging is not done as there is no evidence to indicate an improvement in clinical outcomes.
- Depending on the clinical state of the patient and suspicion for the development of VTE or arterial thrombi, repeat testing and further imaging investigations are done.
To view screening for COVID-19, click here.
Natural History, Complications, and Prognosis
Natural History
- If left untreated, patients with coagulopathy may progress to develop VTE, arterial thrombosis, or microvascular thrombosis and ultimately succumb to death.
Complications
- Thrombotic complications : [1]
- Deep Vein Thrombosis
- Pulmonary Embolism
- Ischemic stroke
- Myocardial infarction
- Ischemic limbs
- Systemic arterial events
- Clotting of central venous catheters, dialysis catheters, and dialysis filters
- Independent predictors of thrombotic complications seen were:
- Age
- Coagulopathy (defined as spontaneous prolongation of the prothrombin time > 3 s or activated partial thromboplastin time > 5 s)
- Active cancer
Prognosis
Prognosis depends on numerous factors:
- Increased D-dimer levels- poor prognosis
- Increased fibrin degradation product (FDP) levels [3]
- ICU admission
To view natural history, complications, and prognosis of COVID-19, click here.
Diagnosis
Diagnostic Study of Choice
- The diagnosis of coagulopathy in COVID-19 is based mainly on the laboratory findings showing a pro-coagulant profile.
- The pre-test probability of DVT and PE can be calculated using the Wells' criteria
- Computed Tomography with pulmonary angiography (CTPA) is the diagnostic test of choice. Ventilation/Perfusion scan may also be done, but may not be of much yield in patients with COVID-19.
- To view the study of choice for diagnosis of COVID-19, click here.
History and Symptoms
The symptoms depend on the vessels and the organ systems involved.
Pulmonary Embolism- Many symptoms of PE overlap with the respiratory symptoms seen in COVID-19.
- Maybe asymptomatic
- Dyspnea
- Chest pain
- Cough
- Some other rare presentations include- hemoptysis, shock, hypotension, death.
A positive history of the following is suggestive of and contributory-
- Immobilization or prolonged hospitalization
- Recent surgery
- Trauma
- Obesity
- History of previous venous thromboembolism (VTE)
- Malignancy
- Stroke with hemiplegia or immobility
- Age >65 years
Deep Vein Thrombosis
Arterial thrombosis involving various systems show the following symptoms:
- Ischemic Stroke: various focal neurological deficits depending on the large artery involved
- Myocardial infarction: Chest pain radiating to left arm and neck, sweating, dyspnea
- Acute ischemic limb: pain, pallor, poikilothermia, pulselessness, paresthesia, paralysis
To view the history and symptoms of COVID-19, click here.
Physical Examination
Pulmonary Embolism Physical examination of patients with Pulmonary Embolism is usually remarkable for-
Deep Vein Thrombosis Physical examination of patients with Deep Vein Thrombosis includes-
- Unilateral swelling/edema with a difference in diameters
- Warmth
- Tenderness
- Dilated veins
- Homan's sign may also be seen but is unreliable.
Arterial thrombosis-
- Ischemic Stroke- Focal neurological deficits depending on the vessel involved
- Myocardial Infarction- uncomfortable appearing patient with diaphoresis
- Ischemic Limb- pallor, poikilothermia, pulselessness, paresthesia, paralysis
To view the complete physical examination in COVID-19, click here.
Laboratory Findings
An elevated concentration of serum/blood pro-coagulant factors is diagnostic of coagulopathy associated with COVID-19. Laboratory findings consistent with the diagnosis of COVID-19 associated coagulopathy include:
- Coagulation testing- Pro-coagulant profile
- Platelet Counts- Normal or increased
- Prothrombin time (PT) and activated partial thromboplastin time (aPTT)- normal or slightly prolonged
- Fibrinogen- increased
- D-dimer- increased
- Factor VIII activity- increased
- VWF antigen- increased
- Protein C, Protein S, Antithrombin III - slightly decreased
TEG findings:
- Reaction time (R) - decreased
- Clot formation time (K)- decreased
- Maximum amplitude (MA)- increased
- Clot lysis at 30 minutes (LY30)- decreased
To view the laboratory findings on COVID-19, click here.
Electrocardiogram
An ECG may be helpful in the diagnosis of pulmonary embolism or myocardial infacrctioncaused due to hypercoagulability in COVID-19.
- Findings on an ECG suggestive of/diagnostic of pulmonary embolism include tachycardia and S1Q3T3 pattern.
- Findings on an ECG suggestive of/diagnostic of myocardial infarction include STE elevation in various leads.
- To view the electrocardiogram findings on COVID-19, click here.
X-ray
There are no specific x-ray findings associated with PE. However, an x-ray may be helpful in ruling out other causes with similar symptoms like pneumonia, cardiogenic causes of dyspnea, and pneumothorax.
- To view the x-ray finidings on COVID-19, click here.
Echocardiography or Ultrasound
- Echocardiography may be helpful in the diagnosis of pulmonary embolism.
- Compressive Ultrasound may be helpful in the diagnosis of deep vein thrombosis
- To view the echocardiographic findings on COVID-19, click here.
CT scan
CTPA and Ventilation Perfusion(V/Q) Scan
- Prompt diagnosis of PE in COVID-19 patient is difficult in this regard that various symptoms of COVID-19 overlap with that of pulmonary embolism. American Society of Hematology provides the following guidelines regarding the diagnosis of pulmonary embolism:
- Normal d-dimers level in a patient with low to moderate pretest probability is sufficient to rule out the diagnosis of PE. D-dimers level is usually elevated in COVID-19 patients. This is not applicable to a patient with a high pretest probability.
- Inpatient with suspected PE with symptoms like hypotension, tachycardia, and sudden drop in oxygen saturation with a high pretest probability of PE, computed tomography with pulmonary angiography is used for the diagnosis. Contraindication to the use of CTPA warrants investigation with ventilation/perfusion scan.
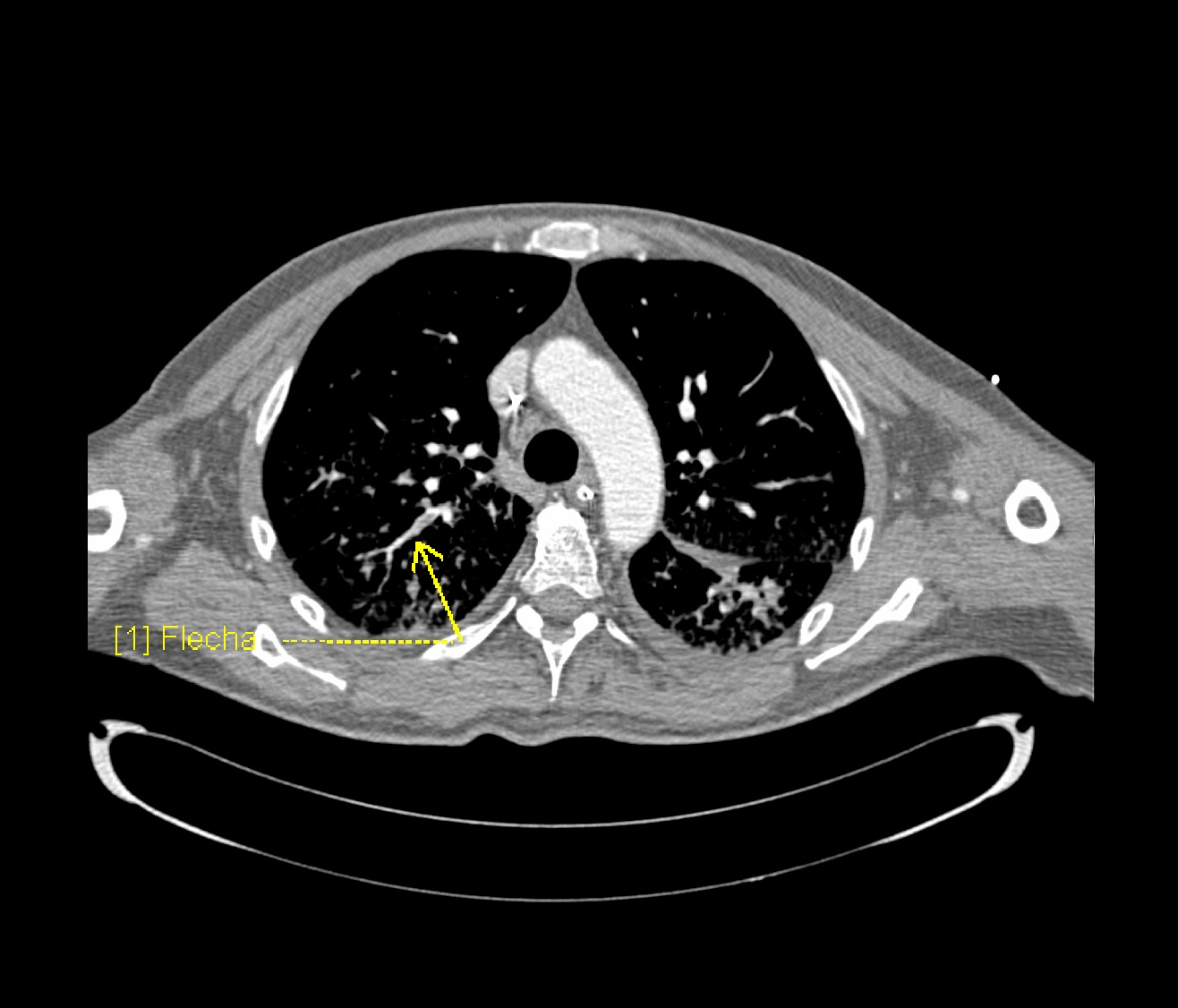
To view the CT scan findings on COVID-19, click here.
MRI
- There are no MRI findings associated with coagulopathy of COVID-19 unless it is used to diagnose and evaluate an ischemic stroke caused by it.
- To view the MRI findings on COVID-19, click here.
Other Imaging Findings
There are no other imaging findings associated with coagulopathy of COVID-19
Other Diagnostic Studies
- To view other diagnostic studies for COVID-19, click here.
Treatment
Medical Therapy
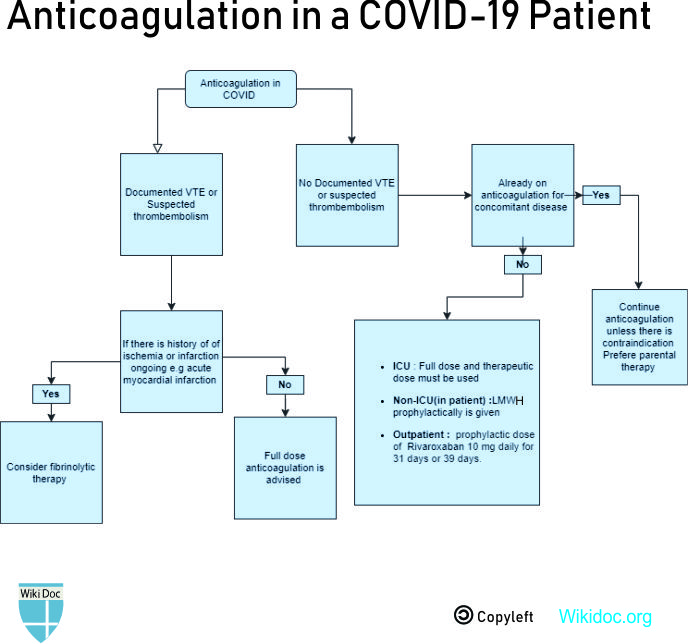
Prophylactic dose of anticoagulation
- Drug- LMWH is preferred over unfractionated heparin to reduce contact with the patient. Unfractionated heparin may be used in case of unavailability or severe renal impairment.
Indications-
- All inpatients in the absence of active bleeding
- To be held only if platelet counts fall below 25 x 109/L, or fibrinogen less than 0.5 g/L
- In case of a history of heparin-induced thrombocytopenia(HIT), fondaparinux is used.
Intermediate or therapeutic dose anticoagulation
- Drug and dose- eg, Enoxaparin 40 to 60 mg once daily
Indications-
- Critically ill patients or ICU patients
- According to a study, a better prognosis was seen in patients who met the SIC (Sepsis-induced coagulopathy) criteria or had marked elevated D-dimer levels and were put on anticoagulant therapy(mainly with low molecular weight heparin) [4]
Therapeutic/ full-dose anticoagulation
- Drug and dose- eg, enoxaparin 1 mg/kg every 12 hours
Indications-
- Suspected VTE/PE
- Confirmed VTE/PE
- Clotting in catheters, or extracorporeal circuits like ECMO and CRRT. [5]
Post-discharge thromboprophylaxis
- Drug and dose- Regulatory-approved regimen
- Betrixaban 160 mg on day 1, followed by 80 mg once daily for 35-42 days
- Rivaroxaban 10 mg daily for 31-39 days
Indications-
- Patients with documented VTE require thromboprophylaxis for up to 90 days after discharge.
- Some patients who do not have VTE but require extended thromboprophylaxis include- acute medical illness, older age, immobilization, recent surgery, or trauma. Most of these criteria are met by patients with COVID-19, and they require thromboprophylaxis for up to 90 days after discharge.
Bleeding in COVID-19
- Transfusion and replacement; discontinuation or reversal of anticoagulation are the mainstay of treatment
- Transfuse platelets if the platelet count is less than 50 x 109/L
- Administer plasma if the INR is above 1.8
- Order fibrinogen concentrate or cryoprecipitate if the fibrinogen level is less than 1.5 g/L
- To view medical treatment for COVID-19, click here.
References
- ↑ 1.0 1.1 Becker RC (2020). "COVID-19 update: Covid-19-associated coagulopathy". J Thromb Thrombolysis. doi:10.1007/s11239-020-02134-3. PMC 7225095 Check
|pmc=value (help). PMID 32415579 Check|pmid=value (help). - ↑ 2.0 2.1 Klok FA, Kruip MJHA, van der Meer NJM, Arbous MS, Gommers DAMPJ, Kant KM; et al. (2020). "Incidence of thrombotic complications in critically ill ICU patients with COVID-19". Thromb Res. 191: 145–147. doi:10.1016/j.thromres.2020.04.013. PMC 7146714 Check
|pmc=value (help). PMID 32291094 Check|pmid=value (help). - ↑ Tang N, Li D, Wang X, Sun Z (2020). "Abnormal coagulation parameters are associated with poor prognosis in patients with novel coronavirus pneumonia". J Thromb Haemost. 18 (4): 844–847. doi:10.1111/jth.14768. PMC 7166509 Check
|pmc=value (help). PMID 32073213 Check|pmid=value (help). - ↑ Tang N, Bai H, Chen X, Gong J, Li D, Sun Z (2020). "Anticoagulant treatment is associated with decreased mortality in severe coronavirus disease 2019 patients with coagulopathy". J Thromb Haemost. 18 (5): 1094–1099. doi:10.1111/jth.14817. PMID 32220112 Check
|pmid=value (help). - ↑ Akima S, McLintock C, Hunt BJ (2020). "RE: ISTH interim guidance to recognition and management of coagulopathy in COVID-19". J Thromb Haemost. doi:10.1111/jth.14853. PMID 32302442 Check
|pmid=value (help).