Diabetic foot pathophysiology: Difference between revisions
No edit summary |
No edit summary |
||
| Line 2: | Line 2: | ||
{{Diabetic foot}} | {{Diabetic foot}} | ||
{{CMG}} {{AE}} {{VVS}} | {{CMG}} {{AE}} {{VVS}} | ||
==Overview== | |||
== Pathophysiology== | == Pathophysiology== | ||
Diabetic foot is an umbrella term for foot problems in patients with [[diabetes mellitus]]. Due to [[artery|arterial]] abnormalities and [[diabetic neuropathy]] and delayed wound healing, [[infection]] or [[gangrene]] of the foot is relatively common. The key components of diabetic foot are [[neuropathy]], [[angiopathy]] and [[trauma]]. <ref name="pmid12039404">{{cite journal| author=Assal JP, Mehnert H, Tritschler HJ, Sidorenko A, Keen H, Hellmut Mehnert Award Workshop Participants| title=On your feet! Workshop on the diabetic foot. | journal=J Diabetes Complications | year= 2002 | volume= 16 | issue= 2 | pages= 183-94 | pmid=12039404 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=12039404 }} </ref> | Diabetic foot is an umbrella term for foot problems in patients with [[diabetes mellitus]]. Due to [[artery|arterial]] abnormalities and [[diabetic neuropathy]] and delayed wound healing, [[infection]] or [[gangrene]] of the foot is relatively common. The key components of diabetic foot are [[neuropathy]], [[angiopathy]] and [[trauma]]. <ref name="pmid12039404">{{cite journal| author=Assal JP, Mehnert H, Tritschler HJ, Sidorenko A, Keen H, Hellmut Mehnert Award Workshop Participants| title=On your feet! Workshop on the diabetic foot. | journal=J Diabetes Complications | year= 2002 | volume= 16 | issue= 2 | pages= 183-94 | pmid=12039404 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=12039404 }} </ref> | ||
| Line 35: | Line 38: | ||
==References== | ==References== | ||
{{reflist|2}} | {{reflist|2}} | ||
{{ | |||
{{ | {{WikiDoc Help Menu}} | ||
{{WikiDoc Sources}} | |||
[[Category:Emergency medicine]] | [[Category:Emergency medicine]] | ||
[[Category:Endocrinology]] | [[Category:Endocrinology]] | ||
[[Category:Primary care]] | [[Category:Primary care]] | ||
[[Category:Needs overview]] | [[Category:Needs overview]] | ||
Revision as of 20:05, 22 July 2016
|
Diabetic foot Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Diabetic foot pathophysiology On the Web |
|
American Roentgen Ray Society Images of Diabetic foot pathophysiology |
|
Risk calculators and risk factors for Diabetic foot pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Vishnu Vardhan Serla M.B.B.S. [2]
Overview
Pathophysiology
Diabetic foot is an umbrella term for foot problems in patients with diabetes mellitus. Due to arterial abnormalities and diabetic neuropathy and delayed wound healing, infection or gangrene of the foot is relatively common. The key components of diabetic foot are neuropathy, angiopathy and trauma. [1]
Neuropathy
The most important cause of diabetic foot is neuropathy. This presence, to some extent, is more than half of the patients with diabetes older than 60 years old. Peripheral neuropathy usually is profound at the point where it leads to the formation of a foot ulcer. What causes neuropathy and why it occurs is not fully known. It is most likely caused by a combination of factors such as; high blood glucose, reactive oxygen species, vasculopathy, reduced oxygenation of the nerves, inflammation, autoimmunity in diabetes, genetic factors, mechanical injury, smoking and alcohol abuse.
Generalized symmetric distal polyneuropathy is the most common and widely recognized form of diabetic neuropathy leading to diabetic foot ulcer. It may be either sensory or motor, and involves small fibers, large fibers or both. The clinical manifestations are divided into the three types of sensory, motor and autonomic neuropathy. Motor neuropathy causes wasting of small muscles of the feet with hammer toes and weakness of hands and feet.
Sensory neuropathy causes:
- Impaired vibration perception and position sense
- Depressed tendon reflexes
- Dull, crushing or cramp-like pain in the bones of the feet
- Sensory ataxia
- Shortening of the achilles tendon
- Abnormal thresholds for warm thermal perception
- Decreased neurovascular function
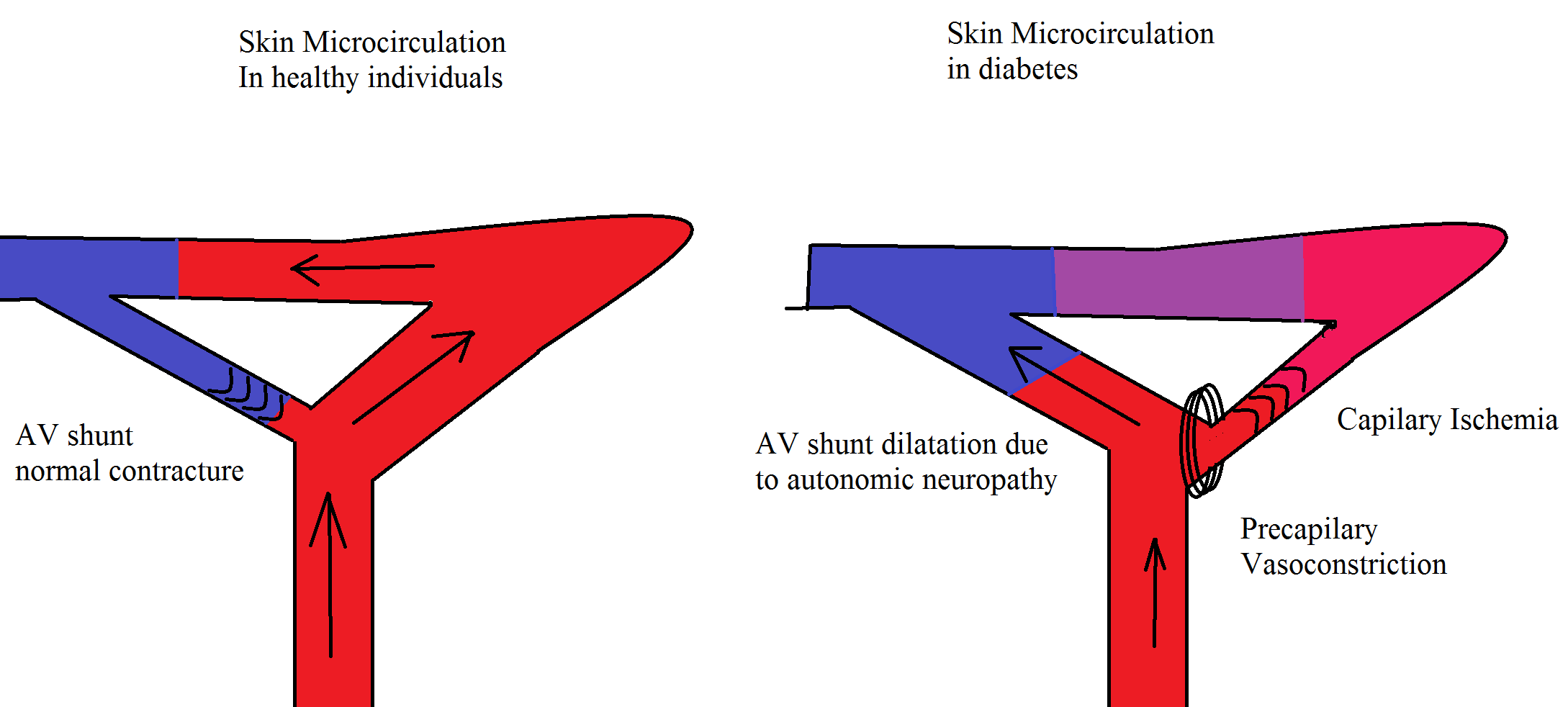
Autonomic neuropathy is the increased or decreased blood flow to the foot (hot foot) with an increased risk of charcot neuroarthropathy, decreased sweating, dry skin, impaired vasomotion and blood flow. These lead to cold feet which ultimately result into the loss of skin integrity, providing a vulnerable site for infection [2].
Angiopathy
Micro and macrovascular complications are the leading cause of diabetic complications. Atherosclerosis occurs due to inflammation, which leads to the accumulation of foam cells. The vascular changes which are responsible for foot problems include stiff arteries due to calcification of the smooth muscle cells in the arterial wall (mediasclerosis). It is usually discovered by an impaired ankle brachial index (ABI). The resting ABI is the ratio of the blood pressure in the lower legs to the blood pressure in the arms. The ABI is calculated by dividing the systolic blood pressure at the ankle by the systolic blood pressures in the arm. It is a non-invasive method to assess the lower extremity arterial system and to detect the presence of arterial occlusion disease. In severe cases, it leads to ischemic foot problems, which the only treatment is vascular surgery. Even in neuropathic foot ulcers, the non healing wounds are the result of impaired blood supply to the tissue. Decreasing the central blood pressure by antihypertensive drugs may be deleterious for these patients[2]. Microvascular complications cause skin damage, infection and impaired wound healing. Once a foot ulcer develops, peripheral vascular disease is the most important factor which may contribute to adverse outcomes. Vascular complications are like a positive feedback which worsen the skin and nerve damage in diabetes [3]
Trauma
Trauma is frequently the trigger of foot ulcer as repetitive trauma and pressure to the area prevent healing. Excessive plantar pressure is related to limited joint mobility and to foot deformities (Charcot foot, hammer toe). Limited joint mobility and abnormal foot biomechanisms have been associated with an increased risk of ulceration. It could also be the result of poor vision and sensory neuropathy so that the patients does not feel the pain, nor do they see the ulcer. Loss of balance can also make patients more susceptible to falls. [2]
References
- ↑ Assal JP, Mehnert H, Tritschler HJ, Sidorenko A, Keen H, Hellmut Mehnert Award Workshop Participants (2002). "On your feet! Workshop on the diabetic foot". J Diabetes Complications. 16 (2): 183–94. PMID 12039404.
- ↑ 2.0 2.1 2.2 Alexiadou K, Doupis J (2012). "Management of diabetic foot ulcers". Diabetes Ther. 3 (1): 4. doi:10.1007/s13300-012-0004-9. PMID 22529027.
- ↑ Venermo M, Vikatmaa P, Terasaki H, Sugano N (2012). "Vascular laboratory for critical limb ischaemia". Scand J Surg. 101 (2): 86–93. PMID 22623440.