Achilles tendon
|
WikiDoc Resources for Achilles tendon |
|
Articles |
|---|
|
Most recent articles on Achilles tendon Most cited articles on Achilles tendon |
|
Media |
|
Powerpoint slides on Achilles tendon |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Achilles tendon at Clinical Trials.gov Trial results on Achilles tendon Clinical Trials on Achilles tendon at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Achilles tendon NICE Guidance on Achilles tendon
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Achilles tendon Discussion groups on Achilles tendon Patient Handouts on Achilles tendon Directions to Hospitals Treating Achilles tendon Risk calculators and risk factors for Achilles tendon
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Achilles tendon |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Overview
The Achilles tendon (or occasionally Achilles’ tendon) also known as the calcaneal tendon or the tendocalcaneous is a tendon of the posterior leg. It serves to attach the gastrocnemius (calf) and soleus muscles to the calcaneus (heel) bone.
Anatomy
The Achilles tendon is the tendonous extension of three muscles in the lower leg: gastrocnemius, soleus, and plantaris. In humans, the tendon passes behind the ankle. It is the thickest and strongest tendon in the body. It is about 15 cm long, and begins near the middle of the leg, but receives fleshy fibers on its anterior surface, almost to its lower end. Gradually becoming contracted below, it is inserted into the middle part of the posterior surface of the calcaneus, a bursa being interposed between the tendon and the upper part of this surface. The tendon spreads out somewhat at its lower end, so that its narrowest part is about 4 cm. above its insertion. It is covered by the fascia and the integument, and stands out prominently behind the bone; the gap is filled up with areolar and adipose tissue. Along its lateral side, but superficial to it, is the small saphenous vein. The achilles' muscle reflex tests the integrity of the S1 spinal root.
Nomenclature
The oldest-known written record of the tendon being named for Achilles is in 1693 by the Flemish/Dutch anatomist Philip Verheyen. In his widely used text Corporis Humani Anatomia, Chapter XV, page 328, he described the tendon's location and said that it was commonly called "the cord of Achilles" ("quae vulgo dicitur chorda Achillis").
The name Achilles' heel comes from Greek mythology. His mother, the goddess Thetis, received a prophecy of her son's death. In order to protect him, she dipped him into the River Styx, which protected his entire body from harm. However, in order to dip him into the river, she needed to grab onto his heel. During the Trojan War Achilles was struck on his unprotected heel by a poisoned arrow, which killed him.
Because eponyms have no relationship to the subject matter anatomical eponyms are being replaced by descriptive terms. The current terminology for Achilles tendon is calcaneal tendon.
Role in disease
Achilles tendinitis is inflammation of the tendon, generally due to overuse of the affected limb or as part of a strain injury. More common is Achilles tendinosis, a degenerative condition with inflammation of the tendon, often accompanied by pain and swelling of the surrounding tissue and paratendon. Maffulli et al. suggested that the clinical label of tendinopathy should be given to the combination of tendon pain, swelling and impaired performance. Achilles tendon rupture is a partial or complete break in the tendon; it requires immobilisation or surgery. Xanthoma can develop in the Achilles tendon in patients with familial hypercholesterolemia.
Treatment of Achilles tendon damage
Initial treatment of damage to the tendon is generally nonoperative. Orthotics can produce early relief to the tendon by the correction of malalignments, non-steroidal anti-inflammatory drugs (NSAIDs) are generally to be avoided as they make the more-common tendinopathy (degenerative) injuries worse; though they may very occasionally be indicated for the rarer tendinitis (inflammatory) injuries. Physiotherapy by eccentric calf stretching under resistance is commonly recommended, usually in conjunction with podiatric insoles or heel cushioning. According to reports by Hakan Alfredson, M.D., and associates of clinical trials in Sweden, the pain in Achilles tendinopathy arises from the nerves associated with neovascularization and can be effectively treated with 1-4 small injections of a sclerosant. In a cross-over trial, 19 of 20 of his patients were successfully treated with this sclerotherapy.
Where tendon rupture is concerned, there are three main types of treatment: the open and the percutaneous operative methods, and nonoperative approaches.
Additional images
-
The popliteal, posterior tibial, and peroneal arteries.
-
Back of left lower extremity.
-
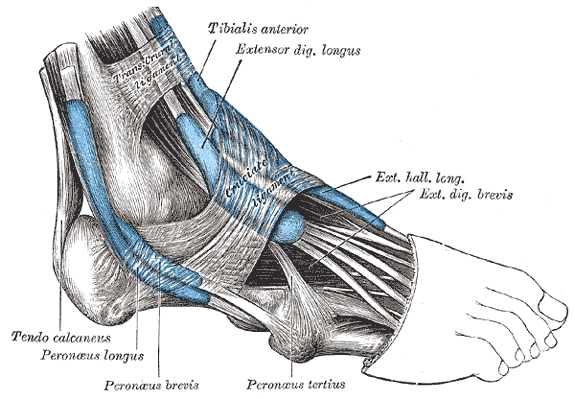
The mucous sheaths of the tendons around the ankle. Lateral aspect.
-
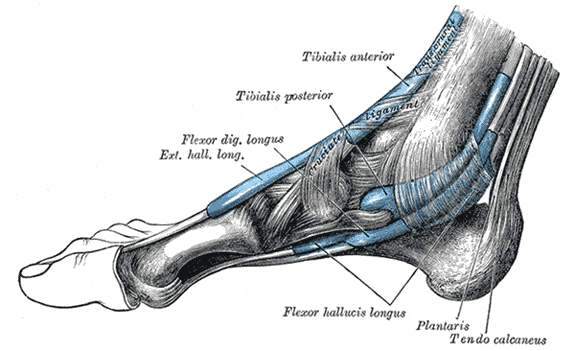
The mucous sheaths of the tendons around the ankle. Medial aspect.