Oral candidiasis physical examination
Jump to navigation
Jump to search
|
Oral candidiasis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Oral candidiasis physical examination On the Web |
|
American Roentgen Ray Society Images of Oral candidiasis physical examination |
|
Risk calculators and risk factors for Oral candidiasis physical examination |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1];Associate Editor(s)-in-Chief: Ahmed Younes M.B.B.CH [2]
Overview
Oral candidiasis usually appears as thick white curdy deposits. Underlying mucosa may appear inflamed (red and possibly slightly raised).
Physical examination
The appearance of lesions on physical examination varies according to the subtype of oral candidiasis.
Pseudomembranous oropharyngeal candidiasis:
- Candida lesions appear as white plaques on the mouth and tongue.
- Trying to remove the patches with tongue depressor will leave an erythematous area and sometimes bleeding (which differentiates it from lichen planus).[1]
Atrophic oropharyngeal candidiasis:
- It’s also called denture stomatitis.[2]
- On inspection, lesions appear as erythematous areas with no white plaques.
- Lesions are usually found in the site of the fitting contact of the dental dentures (hence its name).
Hyperplastic oropharyngeal candidiasis (candidal leukoplakia):
- Plaques are usually found on both sides of the buccal mucosa (less often on the tongue)[3]
- Appear as rough irregular nodular lesions on an erythematous base
- Non homogenous (speckled) leukoplakias are seen frequently
Chronic mucocutaneous candidiasis:
- This syndrome is characterized by recurrent or persistent candidal infection in the mouth, tongue, scalp and nails.
- Due to chronicity of the infection, it’s usually associated with disfigurement and thickness of the affected areas. Nails appear brittle and broken.
- In rare cases, condition might progress into systemic candidiasis (usually if accompanied by another immunocompromisation).[4]
- Patients frequently have accompanying autoimmune disorders as hypopararthyroidism, diabetes or Grave’s disease.
Videos
{{#ev:youtube|0Ld4bOPN-AI}}
Gallery
-
Oral manifestations of HIV infection and AIDS. Chronic oral candidiasis in patient with AIDS. Image courtesy of Professor Peter Anderson DVM PhD and published with permission. © PEIR, University of Alabama at Birmingham, Department of Pathology
-
Soft palate showing extensive oral candidiasis in patient with AIDS. Image courtesy of Professor Peter Anderson DVM PhD and published with permission. © PEIR, University of Alabama at Birmingham, Department of Pathology
-
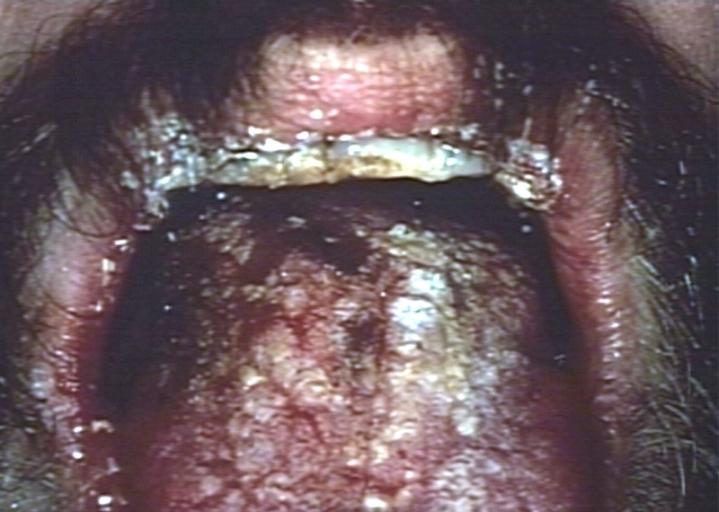
Patient with swollen gingivae was diagnosed with oral moniliasis secondary to monocytic leukemia. From Public Health Image Library (PHIL). [5]
References
- ↑ Akpan A, Morgan R (2002). "Oral candidiasis". Postgrad Med J. 78 (922): 455–9. PMC 1742467. PMID 12185216.
- ↑ Budtz-Jørgensen E (1981). "Oral mucosal lesions associated with the wearing of removable dentures". J. Oral Pathol. 10 (2): 65–80. PMID 6792333.
- ↑ Sitheeque MA, Samaranayake LP (2003). "Chronic hyperplastic candidosis/candidiasis (candidal leukoplakia)". Crit. Rev. Oral Biol. Med. 14 (4): 253–67. PMID 12907694.
- ↑ Kirkpatrick CH (2001). "Chronic mucocutaneous candidiasis". Pediatr. Infect. Dis. J. 20 (2): 197–206. PMID 11224843.
- ↑ "Public Health Image Library (PHIL)".


![Patient with swollen gingivae was diagnosed with oral moniliasis secondary to monocytic leukemia. From Public Health Image Library (PHIL). [5]](/images/c/cb/Moniliasis03.jpeg)