Fractional flow reserve
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor-In-Chief: Priyantha Ranaweera, M.D. Alberto Castro Molina, M.D.
Synonyms and Keywords: FFR, coronary fractional flow reserve
Overview
While coronary angiography assess the extent and the structural severity of fixed coronary stenoses, angiography does not provide functional information regarding flow limitations. While exercise tolerance testing may provide this functional information, only a quarter to a third of patients undergoing cardiac catheterization may have undergone stress test before cardiac catheterization. Thus there is the need for diagnostic studies to assess the functional significance of stenoses in the cardiac catheterization laboratory. While intervention in a critically narrowed lesion is appropriate, a considerable number of lesions are of “intermediate” severity on coronary angiography. Assessment of fractional flow reserve (FFR) may improve the ability to assess the functinal consequences of such lesions in the cardiac catheterization laboratory [1].
Definition
Fractional flow reserve is defined as the fraction of maximal achievable blood flow that can still be maintained to the myocardium despite the presence of a stenosis.
FFR = Pd/Pa ( Pd = pressure distal to the lesion measured by the pressure wire, Pa = pressure at the tip of the guide/catheter)
This measure is a surrogate marker of relative ischemia during exercise.
Physiologic Basis for FFR Measurements
- During maximal hyperemia the FFR can be calculated by dividing the distal pressure by proximal pressure.
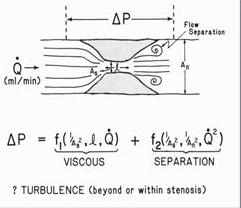
- Pressure drop across a lesion is proportional to:
- length of the lesion
- flow across the lesion.
- It is inversely related to:
- square root of the area of the stenosis.

FFR Vs Coronary flow reserve CFR
The FFR assesse the significance of epicardial stenosis independent of the distal vascular bed, where as the CFR is a measure of the distal vascular bed which may be affected by conditions such as hypertension and diabetes.
FFR - 0.75 threshold/cut off
Pijls, et al. in a landmark study validated the clinical use of FFR against ischemai on nuclear imaging studies. A threshold of 0.75 is associated with a sensitivity of 90% and a specificity of 100% [2].
Setting up the equipment
- Open the Radi wire from the packet and flush it with saline. Do not pull it out of the protective tubing.
- Zero the arterial and distal pressure ports. ( Pa and Pd). (If the pressure tracings need to be displayed in the cardiac cath lab display rather than on the Radi console display, then connect the two connector cables from the Radi console to the cath lab system.)
- Do ACT ( Do not introduce the guide wire in to the coronary artery until the ACT > 200)
- After confirming an ACT > 200 secs, equlize the pressure with the Radi wire at the tip of the guide.
- Cross the lesion with the pre-planned wire. (The Radi wire can be used for lesions that are easy to cross)
- Obsreve the FFR at rest.
- Induced coronary hyperemia.
- Measure FFR
- Could also perform pull back FFR if use the iv route for drugs.
Inducing maximum coronary hyperemia
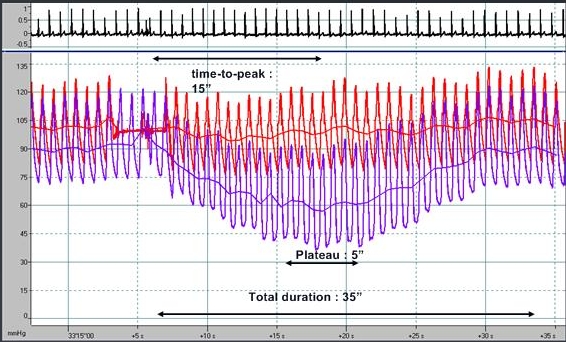
This can be done either by delivering one or more of intracoronary boluses of adenosine (20 mcg dose, peaks in 5 seconds), or using 140 mcg/kg/min over two minutes intravenously from the antecubital fossa or up to 180 mcg/kg/min intravenously from the femoral vein.
Examples of FFR Measurements
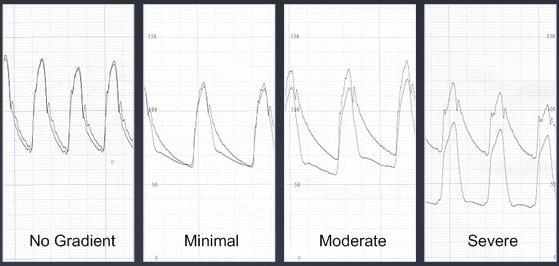
Different types of tracings
As the lesion progresses in severity, the pressure drops first in diastole, and then both in systole and diastole.
FFR correlation with IVUS
Using FFR as the gold standard for lesion severity, Brigouri et al demonstrated
- Optimal sensitivity (sens) and specificity (spec) of IVUS to discriminate significant from non-significant stenoses when area stenosis was >70% (sen 100%, spec 68%)
- Cut-off values fitted to a FFR of <0.75
- MLD <1.8 mm (sen 100%, spec 66%),
- MLA <4.0 mm2 (sens 92%, spec 56%)
- (All lesions with area stenosis <70%had FFR >0.75 but 50% of lesions with area stenosis >70% had FFR <0.75) [3].
FFR in clinical decision making
The Outcomes of Lesions that are not Hemodynamically Significant by FFR: The DEFER Trial
The DEFER trial demonstrated that among intermediate lesions that were not hemodynamically significant (i.e. the FFR was greater than 0.75), there was no impact on clinical outcomes (Death or death / MI). Furthermore the risk of adverse events was quite low and mortality attributable to these lesions was under 1% per year[4].
In the DEFER trial, a total of 325 patients undergoing PCI of an intermediate lesion were randomized to deferral of the PCI if the FFR was > 0.75 (n=91) or performance of a PCI (n=90) even though the lesion was not functionally significant. In other words this trial test what would happen if lesions that are not functionally significant either are or are not dilated. If the FFR was < 0.75, the lesion was dilated.
At 5 years, the survival did not differ between those patients who had a a PCI versus those who did not have a PCI (the deferred group) of a stenosis that was not associated with ischemia. Likewise there was no difference in the risk of death or MI or the number of patients who were free of chest pain on follow-up between the two groups. The risk of cardiovascular death was less than 1% per year in vessels that were either treated or untreated and was not affected by stenting.
The Role of FFR in Selecting Which Lesions to Dilate in the Patient with Multivessel Disease: Results of the FAME Trial
The FAME trial randomized 1005 patients with multivessel disease (excluding those with left main disease or STEMI) who were undergoing intracoronary stent implantation to one of the two following strategies[5][6]:
- Drug-eluting stent implantation guided by angiography alone in which case all significant lesions were stented versus
- Drug-eluting stent implantation guided by FFR measurements in addition to angiography. patients who were randomly assigned to the FFR strategy had stents implanted in those lesions with an FFR of 0.80 or less.
Patients in the FFR guided strategy had fewer stents placed than those in the strategy relying upon angiography alone (2.7±1.2 versus 1.9±1.3 stents, p<0.001). At one year, the primary end point of death, nonfatal myocardial infarction, and repeat revascularization was observed in 18.3% of patients in the angiography group versus 13.2% patients) in the angiography plus FFR group (P=0.02). there was no difference in the incidence of survival free from angina at one year: 78% of patients in the angiography group versus 81% of patients in the FFR group (P=0.20). The risk of death was 3.0% vs 1.8% (p=0.19). The risk of death or MI was 11.1% in the angiography group versus 7.3% in the FFR group (p=0.04). The number of patients who were event free and free of angina were 73% in the FFR group and 67.6% in the angiography group (p=0.07). Procedure costs and the use of contrast was lower in the FFR group as well. It should be noted that only 63% of lesions that were measured had an FFR less than 0.80.
The authors speculate that the results of COURAGE and SYNTAX might have been different had stenting been performed with FFR guidance in which case only those lesions that were ischemic would have been treated. THE FFR cutpointis 075 to 0.80 and FAME used the higher end of this range to that fewer lesions were left unrevascularized.
By not dilating and stenting lesions that appear to be severe angiographically but are not associated with ischemia, you avoid the placement of a stent which could result in a risk of thrombosis or restenosis in a lesion that was not associated with ischemia. The FAME authors concluded that "Routine measurement of FFR in patients with multivessel coronary artery disease who are undergoing PCI with drug-eluting stents significantly reduces the rate of the composite end point of death, nonfatal myocardial infarction, and repeat revascularization at 1 year."
The Role of FFR in Left Main Coronary Artery Disease (LMCA)
In a small non-randomized study, 30 patients who had a hemodynamically significant FFR of <0.75 underwent coronary artery bypass grafting, and an accompanying 24 patients who had a non-hemodynamically significant FFR > 0.75 were managed medically. There was no difference in clinical outcomes between these two groups[7]. In this very small study no patients in the medically managed group died or had AMI.
Likewise, in a small study of 51 patients, FFR measurenet was helpful to identify patients with intermediate left main disease in whom deferral of surgical revascularization was associated with excellent survival and low event rates[8].
The Role of FFR in Acute Coronary Syndromes
The utility of FFR during the course of an acute coronary syndrome is unclear.
In patients with previous myocardial infarction (defined as > 6 days before FFR is performed), FFR has been closely related to abnormalities on SPECT imaging (sensitivity of 82%, specificity of 87%) [9]. Patients with a higher LVEF had higher FFRs independent of the lumen diameters. FFR may be helpful in identifying those patients who may benefit from revascularization > 6 days after an MI.
The Role of FFR in Serial Lesions
Serial lesions may limit the maximal hyperemia achievable in each of the stenoses. The interaction and significance of serial stenoses depends upon their sequence, the distance between them, their severity, the length of the stenoses, and the flow down the artery. A pullback can be performed, and the lesion with the greatest gradient can be dilated first. The gradient can then be checked again to determine if any of the remaining lesions need to be dilated as well.
The Role of FFR in Lesions Involving Bifurcations and Sidebranches
In one small study, measurement of FFR among jailed side branch lesions was shown to be both safe and feasible. This study demonstrated that most of these lesions did not have functional significance, despite morphologic appearance[10].
FFR Measurement In Renal Artery Stenosis
Using PressureWire and vasodilatory stimulus, and during diagnositc catheterization, pressure measurement and calculation of Pd/Pa ratio can be used to guide treatment of renal artery stenosis. The cutoff value is found to be a Pd/Pa ratio of 0.90[11].
FFR and Procedural Time Saved
Using FFR for decision making was shown to cut down the overall hospital stay with better outcomes when compared to using angiography alone to guide angiographic findings [12].
Cost-Effectiveness of FFR
Using FFR for decision making was shown to cut down the overall cost with better outcomes when compared to using angiography alone to guide PCI [12].
Precautions
- Ensure that there is no pressure gradient between the pressure wire (placed at the tip of the guide) and the guiding catheter. The pressures should be equalized at the onset.
- The two pressures should be compared and noted before inducing coronary hyperemia.
- Use a standard wire first to cross difficult lesions. The pressure wire may not be the most suitable in complex lesions.
- Pressure wire may track under a plaque and cause a dissection.
- Repeated attempts in trying to negotiate tortuous anatomy may cause trauma to intact endothelium and promote thrombosis and dissection.
Contemporary guideline updates on fractional flow reserve
Fractional flow reserve in chronic coronary disease
- In patients with chronic coronary disease and angina or an anginal equivalent, no previous evaluation for ischemia, and angiographically intermediate stenoses, invasive physiologic lesion assessment with fractional flow reserve (FFR) or a validated nonhyperemic pressure ratio such as instantaneous wave-free ratio (iFR) is recommended before proceeding with percutaneous coronary intervention (PCI).[13]
- This strategy is intended to determine whether an angiographically intermediate lesion is truly ischemia-producing and to guide revascularization more appropriately than angiography alone.[13]
Contemporary ischemic threshold
- Although historical validation studies established the physiologic basis of FFR, contemporary trials and guideline-based strategies commonly use an FFR threshold of 0.80 or less to define a hemodynamically significant stenosis when guiding revascularization decisions.[14][15]
FFR and coronary CT
- Several controlled studies cited in the 2023 chronic coronary disease guideline reported high diagnostic sensitivity of noninvasive fractional flow reserve derived from coronary computed tomography angiography (FFR-CT) when compared with invasive FFR.[13]
- FFR-CT may complement coronary CT angiography in selected patients when anatomic stenosis severity alone is insufficient to establish functional significance.[13]
FFR in ischemia with nonobstructive coronary arteries
- In the contemporary diagnostic framework for microvascular angina and ischemia with nonobstructive coronary arteries (INOCA), absence of obstructive coronary artery disease may be defined by <50% diameter reduction or FFR >0.80.[13]
- Invasive coronary physiology testing is feasible and safe in selected patients with suspected INOCA and may help define specific endotypes of ischemia.[13]
FFR in acute coronary syndromes
- The role of FFR in acute coronary syndromes continues to evolve and is most often discussed in the setting of multivessel disease and nonculprit lesion assessment.[14]
- The 2025 acute coronary syndromes guideline cites the FAMOUS-NSTEMI trial, in which 350 patients with non-ST-segment elevation acute coronary syndrome and multivessel disease were randomized to FFR-guided PCI if FFR ≤0.80 or angiography-guided PCI; an FFR-guided strategy reduced the number of revascularization procedures at 1 year.[14]
- The same guideline cites prior ACS studies evaluating physiology-guided assessment of nonculprit lesions, but overall evidence remains more nuanced in ACS than in stable chronic coronary disease.[14]
FFR-guided complete revascularization after myocardial infarction
- In the FULL REVASC trial, patients with ST-segment elevation myocardial infarction (STEMI) or very-high-risk non-ST-segment elevation myocardial infarction (NSTEMI) and multivessel disease who underwent culprit-lesion PCI were randomized to FFR-guided complete revascularization of nonculprit lesions or culprit-lesion-only PCI.[15]
- In patients with visually graded 90% to 99% nonculprit stenoses, FFR was recommended but not mandated, and an FFR value of 0.80 or less was considered clinically significant for ischemia.[15]
- Among patients assigned to FFR-guided complete revascularization, 40% had all nonculprit lesions deferred because the FFR value was 0.81 or greater.[15]
- At a median follow-up of 4.8 years, FFR-guided complete revascularization did not reduce the composite of death from any cause, myocardial infarction, or unplanned revascularization when compared with culprit-lesion-only PCI.[15]
- These findings support the concept that physiology-guided complete revascularization in ACS is more selective than angiography-guided treatment alone, but they also underscore that its prognostic benefit in the setting of acute myocardial infarction is not uniform across trials.[15][14]
2025 ACC/AHA/ACEP/NAEMSP/SCAI acute coronary syndromes guideline recommendations relevant to FFR
The following recommendations from the 2025 ACC/AHA/ACEP/NAEMSP/SCAI Guideline for the Management of Patients With Acute Coronary Syndromes are relevant to contemporary use of fractional flow reserve in acute coronary syndromes, particularly in the setting of multivessel coronary artery disease and assessment of nonculprit lesions.[14]
Management of multivessel CAD in STEMI
| Class I |
| "1. In selected, hemodynamically stable patients with ST-segment elevation myocardial infarction and multivessel disease (MVD), after successful PCI of the infarct-related artery, PCI of significantly stenosed noninfarct-related arteries is recommended to reduce the risk of death or myocardial infarction and improve angina-related quality of life (QOL). (Level of Evidence: A)"[14] |
| Class IIa |
| "1. In appropriate patients with ST-segment elevation myocardial infarction and complex MVD, after successful PCI of the infarct-related artery, elective coronary artery bypass grafting surgery for significantly stenosed noninfarct-related arteries involving the left anterior descending artery or left main disease is reasonable to reduce the risk of cardiovascular events. (Level of Evidence: C-EO)"[14] |
| Class IIb |
| "1. In selected hemodynamically stable patients with ST-segment elevation myocardial infarction and low-complexity MVD (those not intended for CABG surgery), multivessel PCI of significantly stenosed noninfarct-related arteries at the time of primary PCI may be preferred over a staged approach to reduce the risk of cardiovascular events. (Level of Evidence: B-R)"[14] |
Management of multivessel CAD in NSTE-ACS
| Class I |
| "1. In patients with non-ST-segment elevation acute coronary syndrome with MVD, the mode of revascularization (coronary artery bypass grafting or multivessel PCI) should be based on the disease complexity and patient’s comorbidities. (Level of Evidence: C-EO)"[14] |
| "2. In stable patients with non-ST-segment elevation acute coronary syndrome with MVD but without left main stenosis who are not intended for CABG surgery and undergoing culprit-lesion PCI, PCI of significant nonculprit lesions (at the time of the index procedure or as a staged procedure) is recommended to reduce the risk of major adverse cardiovascular events (MACE). (Level of Evidence: B-R)"[14] |
| Class IIb |
| "1. In patients with non-ST-segment elevation acute coronary syndrome in whom multivessel PCI is being considered, physiological assessment of a nonculprit stenosis may be considered to guide revascularization decisions. (Level of Evidence: B-R)"[14] |
2011, 2009 and 2005 ACCF/AHA/SCAI Guidelines for Percutaneous Coronary Intervention (DO NOT EDIT)[16][17][18]
Fractional Flow Reserve (DO NOT EDIT)[16]
| Class IIa |
| "1. Fractional flow reserve is reasonable to assess angiographic intermediate coronary lesions (50% to 70% diameter stenosis) and can be useful for guiding revascularization decisions in patients with sudden ischemic heart disease (SIHD).[5][19][4][20][21] (Level of Evidence: A)" |
Use of Fractional Flow Reserve (DO NOT EDIT)[17]
| Class III (Harm) |
| "1. Routine assessment with intracoronary physiological measurements such as coronary pressure (FFR) or Doppler ultrasound to assess the severity of angiographic disease in concordant vascular distribution in patients with angina and a positive, unequivocal noninvasive functional study is not recommended. (Level of Evidence: C) " |
| Class IIa |
|
"1.Coronary pressure (fractional flow reserve [FFR]) or Doppler velocimetry can be useful to determine whether PCI of a specific coronary lesion is warranted. FFR or Doppler velocimetry can also be useful as an alternative to performing noninvasive functional testing (eg, when the functional study is absent or ambiguous) to determine whether an intervention is warranted. It is reasonable to use intracoronary physiological measurements (coronary pressure [FFR][5][22][23][24][25][26][27][28][29][2][30] (Level of Evidence: A) or Doppler velocimetry (Level of Evidence: C) in the assessment of the effects of intermediate coronary stenoses (30% to 70% luminal narrowing) in patients with anginal symptoms. " |
Coronary Artery Pressure and Flow:Use of Fractional Flow Reserve and Coronary Vasodilatory Reserve (DO NOT EDIT)[18]
| Class IIb |
| "1. Intracoronary physiologic measurements may be considered for the evaluation of the success of PCI in restoring flow reserve and to predict the risk of restenosis. (Level of Evidence: C) " |
| "2. Intracoronary physiologic measurements may be considered for the evaluation of patients with anginal symptoms without an apparent angiographic culprit lesion. (Level of Evidence: C) " |
References
- ↑ Pijls NH (2004). "Optimum guidance of complex PCI by coronary pressure measurement". Heart. 90 (9): 1085–93. doi:10.1136/hrt.2003.032151. PMC 1768417. PMID 15310716. Unknown parameter
|month=ignored (help) - ↑ 2.0 2.1 Pijls NH, De Bruyne B, Peels K; et al. (1996). "Measurement of fractional flow reserve to assess the functional severity of coronary-artery stenoses". N. Engl. J. Med. 334 (26): 1703–8. PMID 8637515. Unknown parameter
|month=ignored (help) - ↑ Briguori C, Anzuini A, Airoldi F; et al. (2001). "Intravascular ultrasound criteria for the assessment of the functional significance of intermediate coronary artery stenoses and comparison with fractional flow reserve". Am. J. Cardiol. 87 (2): 136–41. PMID 11152827. Unknown parameter
|month=ignored (help) - ↑ 4.0 4.1 Pijls NH, van Schaardenburgh P, Manoharan G; et al. (2007). "Percutaneous coronary intervention of functionally nonsignificant stenosis: 5-year follow-up of the DEFER Study". J. Am. Coll. Cardiol. 49 (21): 2105–11. doi:10.1016/j.jacc.2007.01.087. PMID 17531660. Unknown parameter
|month=ignored (help) - ↑ 5.0 5.1 5.2 Tonino PA, De Bruyne B, Pijls NH, Siebert U, Ikeno F, van' t Veer M; et al. (2009). "Fractional flow reserve versus angiography for guiding percutaneous coronary intervention". N Engl J Med. 360 (3): 213–24. doi:10.1056/NEJMoa0807611. PMID 19144937. Review in: Ann Intern Med. 2009 May 19;150(10):JC5-7
- ↑ van Nunen LX, Zimmermann FM, Tonino PA, Barbato E, Baumbach A, Engstrøm T; et al. (2015). "Fractional flow reserve versus angiography for guidance of PCI in patients with multivessel coronary artery disease (FAME): 5-year follow-up of a randomised controlled trial". Lancet. 386 (10006): 1853–60. doi:10.1016/S0140-6736(15)00057-4. PMID 26333474.
- ↑ Bech GJ, Droste H, Pijls NH; et al. (2001). "Value of fractional flow reserve in making decisions about bypass surgery for equivocal left main coronary artery disease". Heart. 86 (5): 547–52. PMID 11602550. Unknown parameter
|month=ignored (help) - ↑ Lindstaedt M, Yazar A, Germing A; et al. (2006). "Clinical outcome in patients with intermediate or equivocal left main coronary artery disease after deferral of surgical revascularization on the basis of fractional flow reserve measurements". Am. Heart J. 152 (1): 156.e1–9. doi:10.1016/j.ahj.2006.03.026. PMID 16824848. Unknown parameter
|month=ignored (help) - ↑ De Bruyne B, Pijls NH, Bartunek J; et al. (2001). "Fractional flow reserve in patients with prior myocardial infarction". Circulation. 104 (2): 157–62. PMID 11447079. Unknown parameter
|month=ignored (help) - ↑ Koo BK, Kang HJ, Youn TJ; et al. (2005). "Physiologic assessment of jailed side branch lesions using fractional flow reserve". J. Am. Coll. Cardiol. 46 (4): 633–7. doi:10.1016/j.jacc.2005.04.054. PMID 16098427. Unknown parameter
|month=ignored (help) - ↑ De Bruyne B, Manoharan G, Pijls NH; et al. (2006). "Assessment of renal artery stenosis severity by pressure gradient measurements". J. Am. Coll. Cardiol. 48 (9): 1851–5. doi:10.1016/j.jacc.2006.05.074. PMID 17084261. Unknown parameter
|month=ignored (help) - ↑ 12.0 12.1 Leesar MA, Abdul-Baki T, Akkus NI, Sharma A, Kannan T, Bolli R (2003). "Use of fractional flow reserve versus stress perfusion scintigraphy after unstable angina. Effect on duration of hospitalization, cost, procedural characteristics, and clinical outcome". J. Am. Coll. Cardiol. 41 (7): 1115–21. PMID 12679210. Unknown parameter
|month=ignored (help) - ↑ 13.0 13.1 13.2 13.3 13.4 13.5 Virani SS, Newby LK, Arnold SV; et al. (2023). "2023 AHA/ACC/ACCP/ASPC/NLA/PCNA Guideline for the Management of Patients With Chronic Coronary Disease: A Report of the American Heart Association/American College of Cardiology Joint Committee on Clinical Practice Guidelines". J Am Coll Cardiol. 82 (9): 833–955. doi:10.1016/j.jacc.2023.04.003.
- ↑ 14.00 14.01 14.02 14.03 14.04 14.05 14.06 14.07 14.08 14.09 14.10 14.11 Rao SV, O’Donoghue ML, Ruel M, Rab T, Tamis-Holland JE, Alexander JH, Baber U, Baker H, Cohen MG, Cruz-Ruiz M, Davis LL, de Lemos JA, DeWald TA, Elgendy IY, Feldman DN, Goyal A, Isiadinso I, Menon V, Morrow DA, Mukherjee D, Platz E, Promes SB, Sandner S, Sandoval Y, Schunder R, Shah B, Stopyra JP, Talbot AW, Taub PR, Williams MS (2025). "2025 ACC/AHA/ACEP/NAEMSP/SCAI Guideline for the Management of Patients With Acute Coronary Syndromes: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines". Circulation. 151: e771–e862. doi:10.1161/CIR.0000000000001309.
- ↑ 15.0 15.1 15.2 15.3 15.4 15.5 Böhm F, Mogensen B, Engstrøm T; et al. (2024). "FFR-Guided Complete or Culprit-Only PCI in Patients with Myocardial Infarction". N Engl J Med. 390 (16): 1481–1492. doi:10.1056/NEJMoa2314149.
- ↑ 16.0 16.1 Levine GN, Bates ER, Blankenship JC, Bailey SR, Bittl JA, Cercek B, Chambers CE, Ellis SG, Guyton RA, Hollenberg SM, Khot UN, Lange RA, Mauri L, Mehran R, Moussa ID, Mukherjee D, Nallamothu BK, Ting HH (2011). "2011 ACCF/AHA/SCAI Guideline for Percutaneous Coronary Intervention: Executive Summary A Report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines and the Society for Cardiovascular Angiography and Interventions" (PDF). Journal of the American College of Cardiology. 58 (24): 2550–83. doi:10.1016/j.jacc.2011.08.006. PMID 22070837. Retrieved 2011-12-08. Text "PDF" ignored (help); Unknown parameter
|month=ignored (help) - ↑ 17.0 17.1 Kushner FG, Hand M, Smith SC, King SB, Anderson JL, Antman EM, Bailey SR, Bates ER, Blankenship JC, Casey DE, Green LA, Hochman JS, Jacobs AK, Krumholz HM, Morrison DA, Ornato JP, Pearle DL, Peterson ED, Sloan MA, Whitlow PL, Williams DO (2009). "2009 focused updates: ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction (updating the 2004 guideline and 2007 focused update) and ACC/AHA/SCAI guidelines on percutaneous coronary intervention (updating the 2005 guideline and 2007 focused update) a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines". Journal of the American College of Cardiology. 54 (23): 2205–41. doi:10.1016/j.jacc.2009.10.015. PMID 19942100. Retrieved 2011-12-06. Unknown parameter
|month=ignored (help) - ↑ 18.0 18.1 Smith SC, Feldman TE, Hirshfeld JW, Jacobs AK, Kern MJ, King SB; et al. (2006). "ACC/AHA/SCAI 2005 guideline update for percutaneous coronary intervention: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (ACC/AHA/SCAI Writing Committee to Update 2001 Guidelines for Percutaneous Coronary Intervention)". Circulation. 113 (7): e166–286. doi:10.1161/CIRCULATIONAHA.106.173220. PMID 16490830.
- ↑ Hamilos M, Muller O, Cuisset T, Ntalianis A, Chlouverakis G, Sarno G, Nelis O, Bartunek J, Vanderheyden M, Wyffels E, Barbato E, Heyndrickx GR, Wijns W, De Bruyne B (2009). "Long-term clinical outcome after fractional flow reserve-guided treatment in patients with angiographically equivocal left main coronary artery stenosis". Circulation. 120 (15): 1505–12. doi:10.1161/CIRCULATIONAHA.109.850073. PMID 19786633. Retrieved 2011-12-09. Unknown parameter
|month=ignored (help) - ↑ Pijls NH, Fearon WF, Tonino PA, Siebert U, Ikeno F, Bornschein B, van't Veer M, Klauss V, Manoharan G, Engstrøm T, Oldroyd KG, Ver Lee PN, MacCarthy PA, De Bruyne B (2010). "Fractional flow reserve versus angiography for guiding percutaneous coronary intervention in patients with multivessel coronary artery disease: 2-year follow-up of the FAME (Fractional Flow Reserve Versus Angiography for Multivessel Evaluation) study". Journal of the American College of Cardiology. 56 (3): 177–84. doi:10.1016/j.jacc.2010.04.012. PMID 20537493. Retrieved 2011-12-09. Unknown parameter
|month=ignored (help) - ↑ Tonino PA, Fearon WF, De Bruyne B, Oldroyd KG, Leesar MA, Ver Lee PN, Maccarthy PA, Van't Veer M, Pijls NH (2010). "Angiographic versus functional severity of coronary artery stenoses in the FAME study fractional flow reserve versus angiography in multivessel evaluation". Journal of the American College of Cardiology. 55 (25): 2816–21. doi:10.1016/j.jacc.2009.11.096. PMID 20579537. Retrieved 2011-12-09. Unknown parameter
|month=ignored (help) - ↑ Bech GJ, De Bruyne B, Bonnier HJ, et al. Long-term follow-up after deferral of percutaneous transluminal coronary angioplasty of intermediate stenosis on the basis of coronary pressure measurement. J Am Coll Cardiol. 1998; 31: 841–7.
- ↑ Berger A, Botman KJ, MacCarthy PA, et al. Long-term clinical outcome after fractional flow reserve-guided percutaneous coronary intervention in patients with multivessel disease. J Am Coll Cardiol. 2005; 46: 438–42.
- ↑ Botman KJ, Pijls NH, Bech JW, et al. Percutaneous coronary intervention or bypass surgery in multivessel disease? A tailored approach based on coronary pressure measurement. Catheter Cardiovasc Interv. 2004; 63: 184–91.
- ↑ Caymaz O, Fak AS, Tezcan H, et al. Correlation of myocardial fractional flow reserve with thallium-201 SPECT imaging in intermediate-severity coronary artery lesions. J Invasive Cardiol. 2000; 12: 345–50.
- ↑ Chamuleau SA, Meuwissen M, Koch KT, et al. Usefulness of fractional flow reserve for risk stratification of patients with multivessel coronary artery disease and an intermediate stenosis. Am J Cardiol. 2002; 89: 377–80.
- ↑ Christou MA, Siontis GC, Katritsis DG, et al. Meta-analysis of fractional flow reserve versus quantitative coronary angiography and noninvasive imaging for evaluation of myocardial ischemia. Am J Cardiol. 2007; 99: 450–6.
- ↑ Costa MA, Sabate M, Staico R, et al. Anatomical and physiologic assessments in patients with small coronary artery disease: final results of the Physiologic and Anatomical Evaluation Prior to and After Stent Implantation in Small Coronary Vessels (PHANTOM) trial. Am Heart J. 2007; 153: 296–7.
- ↑ Courtis J, Rodes-Cabau J, Larose E, et al. Comparison of medical treatment and coronary revascularization in patients with moderate coronary lesions and borderline fractional flow reserve measurements. Catheter Cardiovasc Interv. 2008; 71: 541–8.
- ↑ Verna E, Lattanzio M, Ghiringhelli S, et al. Performing versus deferring coronary angioplasty based on functional evaluation of vessel stenosis by pressure measurements: a clinical outcome study. J Cardiovasc Med (Hagerstown). 2006; 7: 169–75.