Dobutamine
{{DrugProjectFormSinglePage |authorTag=Alejandro Lemor, M.D. [1] |genericName=dobutamine |aOrAn=an |drugClass=adrenergic receptor agonist |indication=decreased cardiac output and heart failure |adverseReactions=hypertension, tachyarrhythmia, angina, and headache |blackBoxWarningTitle=TITLE |blackBoxWarningBody=Condition Name: (Content) |fdaLIADAdult======Decreased Cardiac Output=====
- Inotropic support in the short-term treatment of adults with cardiac decompensation due to depressed contractility resulting either from organic heart disease or from cardiac surgical procedures
- Dosing Information
- Initial dose: 0.5 to 1 mcg/kg/min
- Maintenance dose: 2 to 40 mcg/kg/min
Heart Failure
- Dosing Information
- Initial dose: 0.5 to 1 mcg/kg/min
- Maintenance dose: 2 to 40 mcg/kg/min
|offLabelAdultGuideSupport=There is limited information regarding Off-Label Guideline-Supported Use of Dobutamine in adult patients. |offLabelAdultNoGuideSupport======Acute myocardial infarction=====
- Dosing Information
- Infusion 7.7 mcg/kg/minute[1]
Bradyarrhythmia - Heart block
- Dosing Information
- 5-15 mcg/kg/m2[2]
Cardiac MRI
- Dosing Information
- 10 mcg/kg/min IV 5 min prior to and during MRI. [3]
Cardiac ventriculography
- Dosing Information
- 5 mcg/kg/min[4]
Severity Assessment of Mitral Valve Stenosis
- Dosing Information
- 5-20 mcg/kg/min every 3 min [5]
PET heart study
- Dosing Information
- 5 to 40 mcg/kg/min[6]
Shock in Pulmonary Embolism
- Dosing Information
- 8.3 mcg/kg/min[7]
Septic shock
- Dosing Information
- 10 mcg/kg/min [8]
Stress Photon Emission Computerized Tomography,
- Dosing Information
Stress echocardiography
Toxic shock syndrome
- Dosing Information
- Initial dose: 2.0 mcg/kg/min
- Maintenance dose: increase 2.0 mcg/kg/min every 20 minutes
|offLabelPedGuideSupport=There is limited information regarding Off-Label Guideline-Supported Use of Dobutamine in pediatric patients. |offLabelPedNoGuideSupport======Septic shock=====
- Dosing Information
- 7.5 mcg/kg/min [11]
Stress echocardiography
- Dosing Information
- up to 30 mcg/kg/min [12]
|contraindications=* Patients with idiopathic hypertrophic subaortic stenosis.
- Patients who have shown previous manifestations of hypersensitivity to dobutamine.
|warnings=====Increase in Heart Rate or Blood Pressure====
- Dobutamine hydrochloride may cause a marked increase in heart rate or blood pressure, especially systolic pressure.
- Approximately 10% of patients in clinical studies have had rate increases of 30 beats/minute or more, and about 7.5% have had a 50 mm Hg or greater increase in systolic pressure. Usually, reduction of dosage promptly reverses these effects.
- Because dobutamine hydrochloride facilitates atrioventricular conduction, patients with atrial fibrillation are at risk of developing rapid ventricular response.
- Patients with pre-existing hypertension appear to face an increased risk of developing an exaggerated pressor response.
Ectopic Activity
- Dobutamine hydrochloride may precipitate or exacerbate ventricular ectopic activity, but it rarely has caused ventricular tachycardia.
Hypersensitivity
- Reactions suggestive of hypersensitivity associated with administration of Dobutamine Injection, USP, including skin rash, fever, eosinophilia, and bronchospasm, have been reported occasionally.
- Dobutamine Injection, USP contains sodium metabisulfite, a sulfite that may cause allergic-type reactions, including anaphylactic symptoms and life-threatening or less severe asthmatic episodes, in certain susceptible people.
- The overall prevalence of sulfite sensitivity in the general population is unknown and probably low. Sulfite sensitivity is seen more frequently in asthmatic than in nonasthmatic people.
|clinicalTrials=====Cardiovascular====
Tachycardia
- An increase in heart rate of 5 to 15 beats/minute has been noted in most patients.
- The effect is dose related.
Hypertension
- A 10- to 20-mm increase in systolic blood pressure has been noted in most patients.
- The effect is dose related.
Ventricular Ectopic Activity
- Approximately 5% of patients have had increased premature ventricular beats during infusions.
- The effect is dose related.
Hypotension
- Precipitous decreases in blood pressure have occasionally been described in association with dobutamine therapy.
- Decreasing the dose or discontinuing the infusion typically results in rapid return of blood pressure to baseline values.
- In rare cases, however, intervention may be required and reversibility may not be immediate.
Reactions at Sites of Intravenous Infusion
- Phlebitis has occasionally been reported.
- Local inflammatory changes have been described following inadvertent infiltration.
- Isolated cases of cutaneous necrosis (destruction of skin tissue) have been reported.
Miscellaneous Uncommon Effects
The following adverse effects have been reported in 1% to 3% of patients:
- Nausea
- Headache
- Angina
- Nonspecific chest pain
- Palpitations
- Shortness of breath
- Isolated cases of thrombocytopenia have been reported.
Administration of dobutamine, like other catecholamines, can produce a mild reduction in serum potassium concentration, rarely to hypokalemic levels.
Longer-Term Safety
- Infusions of up to 72 hours have revealed no adverse effects other than those seen with shorter infusions
|drugInteractions=* Animal studies indicate that dobutamine may be ineffective if the patient has recently received a β-blocking drug. In such a case, the peripheral vascular resistance may increase.
- Preliminary studies indicate that the concomitant use of dobutamine and nitroprusside results in a higher cardiac output and, usually, a lower pulmonary wedge pressure than when either drug is used alone.
- There was no evidence of drug interactions in clinical studies in which dobutamine was administered concurrently with other drugs, including digitalis preparations, furosemide, spironolactone, lidocaine, nitroglycerin, isosorbide dinitrate, morphine, atropine, heparin, protamine, potassium chloride, folic acid, and acetaminophen.
|FDAPregCat=B |useInPregnancyFDA=Reproduction studies performed in rats at doses up to the normal human dose (10 mcg/kg/min for 24 h, total daily dose of 14.4 mg/kg), and in rabbits at doses up to twice the normal human dose, have revealed no evidence of harm to the fetus due to dobutamine hydrochloride. There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed. |AUSPregCat=B2 |useInPregnancyAUS=Drugs which have been taken by only a limited number of pregnant women and women of childbearing age, without an increase in the frequency of malformation or other direct or indirect harmful effects on the human fetus having been observed. Studies in animals are inadequate or may be lacking, but available data show no evidence of an increased occurrence of fetal damage. |useInLaborDelivery=The effect of dobutamine hydrochloride on labor and delivery is unknown. |useInNursing=It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when dobutamine hydrochloride is administered to a nursing woman. If a mother requires dobutamine hydrochloride treatment, breastfeeding should be discontinued for the duration of treatment. |useInPed=The safety and effectiveness of Dobutamine Injection, USP for use in pediatric patients have not been studied. |administration=* Intravenous

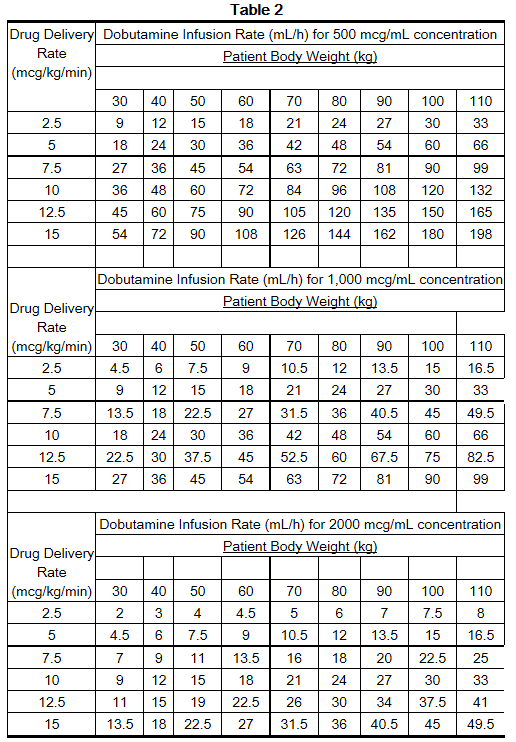
- The rate of administration and the duration of therapy should be adjusted according to the patient's response as determined by heart rate, presence of ectopic activity, blood pressure, urine flow, and, whenever possible, measurement of central venous or pulmonary wedge pressure and cardiac output.
- Concentrations of up to 5,000 mcg/mL have been administered to humans (250 mg/50 mL). The final volume administered should be determined by the fluid requirements of the patient.
- Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
|monitoring=====General====
- During the administration of dobutamine Injection, USP, as with any adrenergic agent, ECG and blood pressure should be continuously monitored. In addition, pulmonary wedge pressure and cardiac output should be monitored whenever possible to aid in the safe and effective infusion of dobutamine hydrochloride.
- Hypovolemia should be corrected with suitable volume expanders before treatment with dobutamine hydrochloride is instituted.
- No improvement may be observed in the presence of marked mechanical obstruction, such as severe valvular aortic stenosis.
Usage Following Acute Myocardial Infarction
- Clinical experience with dobutamine hydrochloride following myocardial infarction has been insufficient to establish the safety of the drug for this use.
- There is concern that any agent that increases contractile force and heart rate may increase the size of an infarction by intensifying ischemia, but it is not known whether dobutamine hydrochloride does so.
Laboratory Tests
- Dobutamine, like other β2-agonists, can produce a mild reduction in serum potassium concentration, rarely to hypokalemic levels.
- Accordingly, consideration should be given to monitoring serum potassium.
|IVCompat=* At the time of administration, Dobutamine Injection, USP must be further diluted in an I.V. container to at least a 50 mL solution using one of the following intravenous solutions as a diluent: 5% Dextrose Injection, USP; 5% Dextrose and 0.45% Sodium Chloride Injection, USP; 5% Dextrose and 0.9% Sodium Chloride Injection, USP; 10% Dextrose Injection, USP; Isolyte® M with 5% Dextrose Injection; Lactated Ringer's Injection; 5% Dextrose in Lactated Ringer's Injection; Normosol®-M in D5-W; 20% Osmitrol® in Water for Injection; 0.9% Sodium Chloride Injection, USP; or Sodium Lactate Injection, USP.
- Intravenous solutions should be used within 24 hours.
|overdose=* Overdoses of dobutamine have been reported rarely. The following is provided to serve as a guide if such an overdose is encountered.
Signs and Symptoms
- Toxicity from dobutamine is usually due to excessive cardiac β-receptor stimulation.
- The duration of action of dobutamine is generally short (T1/2 = 2 minutes) because it is rapidly metabolized by catechol-O-methyltransferase.
- The symptoms of toxicity may include anorexia, nausea, vomiting, tremor, anxiety, palpitations, headache, shortness of breath, and anginal and nonspecific chest pain.
- The positive inotropic and chronotropic effects of dobutamine on the myocardium may cause hypertension, tachyarrhythmias, myocardial ischemia, and ventricular fibrillation.
- Hypotension may result from vasodilation.
Management
- The initial actions to be taken in a dobutamine overdose are discontinuing administration, establishing an airway, and ensuring oxygenation and ventilation.
- Resuscitative measures should be initiated promptly. Severe ventricular tachyarrhythmias may be successfully treated with propranolol or lidocaine.
- Hypertension usually responds to a reduction in dose or discontinuation of therapy.
- Protect the patient's airway and support ventilation and perfusion.
- If needed, meticulously monitor and maintain, within acceptable limits, the patient's vital signs, blood gases, serum electrolytes, etc. If the product is ingested, unpredictable absorption may occur from the mouth and the gastrointestinal tract.
- Absorption of drugs from the gastrointestinal tract may be decreased by giving activated charcoal, which, in many cases, is more effective than emesis or lavage; consider charcoal instead of or in addition to gastric emptying.
- Repeated doses of charcoal over time may hasten elimination of some drugs that have been absorbed.
- Safeguard the patient's airway when employing gastric emptying or charcoal.
- Forced diuresis, peritoneal dialysis, hemodialysis, or charcoal hemo-perfusion have not been established as beneficial for an overdose of dobutamine.
|drugBox={{Drugbox2 | verifiedrevid = 459442789 | IUPAC_name = (RS)-4-(2-{[4-(4-hydroxyphenyl)butan-2-yl]amino}ethyl)benzene-1,2-diol | image = Dobutamine skeletal.png | imagename = 1 : 1 mixture (racemate) | drug_name = Dobutamine
| tradename = | Drugs.com = Monograph | MedlinePlus = a682861 | pregnancy_category = B | legal_status = Rx-only | routes_of_administration = Intravenous
| bioavailability = | protein_bound = | metabolism = | elimination_half-life = 2 minutes
| CASNo_Ref =
| CAS_number_Ref =
| CAS_number = 34368-04-2
| ATC_prefix = C01
| ATC_suffix = CA07
| ATC_supplemental =
| PubChem = 36811
| IUPHAR_ligand = 535
| DrugBank_Ref =
| DrugBank = DB00841
| ChemSpiderID_Ref =
| ChemSpiderID = 33786
| UNII_Ref =
| UNII = 0WR771DJXV
| KEGG_Ref =
| KEGG = D03879
| ChEBI_Ref =
| ChEBI = 4670
| ChEMBL_Ref =
| ChEMBL = 926
| C=18 | H=23 | N=1 | O=3
| molecular_weight = 301.38 g/mol
| smiles = Oc1ccc(cc1O)CCNC(C)CCc2ccc(O)cc2
| InChI = 1/C18H23NO3/c1-13(2-3-14-4-7-16(20)8-5-14)19-11-10-15-6-9-17(21)18(22)12-15/h4-9,12-13,19-22H,2-3,10-11H2,1H3
| InChIKey = JRWZLRBJNMZMFE-UHFFFAOYAV
| StdInChI_Ref =
| StdInChI = 1S/C18H23NO3/c1-13(2-3-14-4-7-16(20)8-5-14)19-11-10-15-6-9-17(21)18(22)12-15/h4-9,12-13,19-22H,2-3,10-11H2,1H3
| StdInChIKey_Ref =
| StdInChIKey = JRWZLRBJNMZMFE-UHFFFAOYSA-N
| synonyms = Dobutrex, Inotrex
}}
|mechAction=Dobutamine hydrochloride is a direct-acting inotropic agent whose primary activity results from stimulation of the β receptors of the heart while producing comparatively mild chronotropic, hypertensive, arrhythmogenic, and vasodilative effects. It does not cause the release of endogenous norepinephrine, as does dopamine. In animal studies, dobutamine hydrochloride produces less increase in heart rate and less decrease in peripheral vascular resistance for a given inotropic effect than does isoproterenol.
In patients with depressed cardiac function, both dobutamine hydrochloride and isoproterenol increase the cardiac output to a similar degree. In the case of dobutamine hydrochloride, this increase is usually not accompanied by marked increases in heart rate (although tachycardia is occasionally observed), and the cardiac stroke volume is usually increased. In contrast, isoproterenol increases the cardiac index primarily by increasing the heart rate while stroke volume changes little or declines.
Facilitation of atrioventricular conduction has been observed in human electrophysiologic studies and in patients with atrial fibrillation.
Systemic vascular resistance is usually decreased with administration of dobutamine hydrochloride. Occasionally, minimum vasoconstriction has been observed.
Most clinical experience with dobutamine hydrochloride is short-term − not more than several hours in duration. In the limited number of patients who were studied for 24, 48, and 72 hours, a persistent increase in cardiac output occurred in some, whereas output returned toward baseline values in others.
|structure=

- Dobutamine Hydrochloride, USP is chemically designated (±)-4-2-3-(ρ-hydroxyphenyl)-1-methylpropyl] amino]ethyl]-pyrocatechol hydrochloride.
- It is a synthetic catecholamine.
- Molecular Weight: 337.85
- Molecular Formula: C18H23NO3 • HCl
|PK=The onset of action of dobutamine is within 1 to 2 minutes; however, as much as 10 minutes may be required to obtain the peak effect of a particular infusion rate.
The plasma half-life of dobutamine hydrochloride in humans is 2 minutes. The principal routes of metabolism are methylation of the catechol and conjugation. In human urine, the major excretion products are the conjugates of dobutamine and 3-O-methyl dobutamine. The 3-O-methyl derivative of dobutamine is inactive. |nonClinToxic=====Carcinogenesis, Mutagenesis, Impairment of Fertility ==== Studies to evaluate the carcinogenic or mutagenic potential of dobutamine hydrochloride, or its potential to affect fertility, have not been conducted. |howSupplied=Dobutamine Injection, USP is supplied in 20 mL single-dose glass vials containing 250 mg dobutamine, as the hydrochloride packaged in individual cartons or in a tray of 10. |storage=Store at 20 to 25°C (68° to 77°F) |alcohol=Alcohol-Dobutamine interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication. |brandNames=Dobutrex |lookAlike=* Dobutamine - Dopamine |nlmPatientInfo=(Link to patient information page) |drugShortage=Drug Shortage }} {{#subobject:
|Label Page=Dobutamine |Label Name=Dobutamine label.jpg
}}
{{#subobject:
|Label Page=Dobutamine |Label Name=Dobutamine FDA panel.png
}}
- ↑ N. A. Awan, M. K. Evenson, K. E. Needham, J. M. Beattie & D. T. Mason (1983). "Effect of combined nitroglycerin and dobutamine infusion in left ventricular dysfunction". American heart journal. 106 (1 Pt 1): 35–40. PMID 6408917. Unknown parameter
|month=ignored (help) - ↑ A. Masoni, P. Alboni, C. Malacarne & L. Codeca (1979). "Effects of dobutamine on electrophysiological properties of the specialized conduction system in man". Journal of electrocardiology. 12 (4): 361–370. PMID 512532. Unknown parameter
|month=ignored (help) - ↑ F. M. Baer, P. Theissen, C. A. Schneider, E. Voth, U. Sechtem, H. Schicha & E. Erdmann (1998). "Dobutamine magnetic resonance imaging predicts contractile recovery of chronically dysfunctional myocardium after successful revascularization". Journal of the American College of Cardiology. 31 (5): 1040–1048. PMID 9562005. Unknown parameter
|month=ignored (help) - ↑ N. Takeyasu, S. Watanabe, R. Ajisaka, K. Eda, M. Toyama, K. Sakamoto, T. Saito, T. Yamanouchi, T. Masuoka, T. Takeda, Y. Itai, Y. Sugishita & I. Yamaguchi (2000). "Low-dose dobutamine radionuclide ventriculography for prediction of myocardial viability: quantitative analysis of regional left ventricular function". Clinical cardiology. 23 (6): 409–414. PMID 10875029. Unknown parameter
|month=ignored (help) - ↑ M. H. Hwang, I. Pacold, Z. E. Piao, R. Engelmeier, P. J. Scanlon & H. S. Loeb (1986). "The usefulness of dobutamine in the assessment of the severity of mitral stenosis". American heart journal. 111 (2): 312–316. PMID 3946174. Unknown parameter
|month=ignored (help) - ↑ S. Severi, R. Underwood, R. H. Mohiaddin, H. Boyd, M. Paterni & P. G. Camici (1995). "Dobutamine stress: effects on regional myocardial blood flow and wall motion". Journal of the American College of Cardiology. 26 (5): 1187–1195. doi:10.1016/0735-1097(95)00319-3. PMID 7594031. Unknown parameter
|month=ignored (help) - ↑ F. Jardin, B. Genevray, D. Brun-Ney & A. Margairaz (1985). "Dobutamine: a hemodynamic evaluation in pulmonary embolism shock". Critical care medicine. 13 (12): 1009–1012. PMID 4064710. Unknown parameter
|month=ignored (help) - ↑ J. Berre, D. De Backer, J. J. Moraine, C. Melot, R. J. Kahn & J. L. Vincent (1997). "Dobutamine increases cerebral blood flow velocity and jugular bulb hemoglobin saturation in septic patients". Critical care medicine. 25 (3): 392–398. PMID 9118652. Unknown parameter
|month=ignored (help) - ↑ A. Elhendy, F. B. Sozzi, R. Valkema, R. T. van Domburg, J. J. Bax & J. R. Roelandt (2000). "Dobutamine technetium-99m tetrofosmin SPECT imaging for the diagnosis of coronary artery disease in patients with limited exercise capacity". Journal of nuclear cardiology : official publication of the American Society of Nuclear Cardiology. 7 (6): 649–654. doi:10.1067/mnc.2000.109660. PMID 11144480. Unknown parameter
|month=ignored (help) - ↑ C. J. Jr Fisher, Z. Horowitz & T. E. Albertson (1985). "Cardiorespiratory failure in toxic shock syndrome: effect of dobutamine". Critical care medicine. 13 (3): 160–165. PMID 3971725. Unknown parameter
|month=ignored (help) - ↑ R. M. Perkin, D. L. Levin, R. Webb, A. Aquino & J. Reedy (1982). "Dobutamine: a hemodynamic evaluation in children with shock". The Journal of pediatrics. 100 (6): 977–983. PMID 7086606. Unknown parameter
|month=ignored (help) - ↑ N. Noto, M. Ayusawa, K. Karasawa, H. Yamaguchi, N. Sumitomo, T. Okada & K. Harada (1996). "Dobutamine stress echocardiography for detection of coronary artery stenosis in children with Kawasaki disease". Journal of the American College of Cardiology. 27 (5): 1251–1256. doi:10.1016/0735-1097(95)00570-6. PMID 8609352. Unknown parameter
|month=ignored (help)