Cordarone tablet warnings and precautions
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Ahmed Zaghw, M.D. [2]
Warnings
 |
Mortality
In the National Heart, Lung and Blood Institute's Cardiac Arrhythmia Suppression Trial (CAST), a long-term, multi-centered, randomized, double-blind study in patients with asymptomatic non-life-threatening ventricular arrhythmias who had had myocardial infarctions more than six days but less than two years previously, an excessive mortality or non-fatal cardiac arrest rate was seen in patients treated with encainide or flecainide (56/730) compared with that seen in patients assigned to matched placebo-treated groups (22/725). The average duration of treatment with encainide or flecainide in this study was ten months.
Cordarone therapy was evaluated in two multi-centered, randomized, double-blind, placebo-controlled trials involving 1202 (Canadian Amiodarone Myocardial Infarction Arrhythmia Trial; CAMIAT) and 1486 (European Myocardial Infarction Amiodarone Trial; EMIAT) post-MI patients followed for up to 2 years. Patients in CAMIAT qualified with ventricular arrhythmias, and those randomized to amiodarone received weight- and response-adjusted doses of 200 to 400 mg/day. Patients in EMIAT qualified with ejection fraction <40%, and those randomized to amiodarone received fixed doses of 200 mg/day. Both studies had weeks-long loading dose schedules. Intent-to-treat all-cause mortality results were as follows:
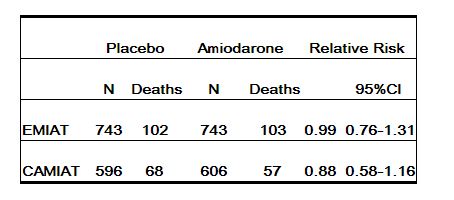 |
These data are consistent with the results of a pooled analysis of smaller, controlled studies involving patients with structural heart disease (including myocardial infarction).
Pulmonary Toxicity
There have been post-marketing reports of acute-onset (days to weeks) pulmonary injury in patients treated with oral Cordarone with or without initial I.V. therapy. Findings have included pulmonary infiltrates and/or mass on X-ray, pulmonary alveolar hemorrhage, pleural effusion, bronchospasm, wheezing, fever, dyspnea, cough, hemoptysis, and hypoxia. Some cases have progressed to respiratory failure and/or death. Post-marketing reports describe cases of pulmonary toxicity in patients treated with low doses of Cordarone; however, reports suggest that the use of lower loading and maintenance doses of Cordarone are associated with a decreased incidence of Cordarone-induced pulmonary toxicity.
Cordarone Tablets may cause a clinical syndrome of cough and progressive dyspnea accompanied by functional, radiographic, gallium-scan, and pathological data consistent with pulmonary toxicity, the frequency of which varies from 2 to 7% in most published reports, but is as high as 10 to 17% in some reports. Therefore, when Cordarone therapy is initiated, a baseline chest X-ray and pulmonary-function tests, including diffusion capacity, should be performed. The patient should return for a history, physical exam, and chest X-ray every 3 to 6 months.
Pulmonary toxicity secondary to Cordarone seems to result from either indirect or direct toxicity as represented by hypersensitivity pneumonitis (including eosinophilic pneumonia) or interstitial/alveolar pneumonitis, respectively.
Patients with preexisting pulmonary disease have a poorer prognosis if pulmonary toxicity develops.
Hypersensitivity pneumonitis usually appears earlier in the course of therapy, and rechallenging these patients with Cordarone results in a more rapid recurrence of greater severity.
Bronchoalveolar lavage is the procedure of choice to confirm this diagnosis, which can be made when a T suppressor/cytotoxic (CD8-positive) lymphocytosis is noted. Steroid therapy should be instituted and Cordarone therapy discontinued in these patients.
Interstitial/alveolar pneumonitis may result from the release of oxygen radicals and/or phospholipidosis and is characterized by findings of diffuse alveolar damage, interstitial pneumonitis or fibrosis in lung biopsy specimens. Phospholipidosis (foamy cells, foamy macrophages), due to inhibition of phospholipase, will be present in most cases of Cordarone-induced pulmonary toxicity; however, these changes also are present in approximately 50% of all patients on Cordarone therapy. These cells should be used as markers of therapy, but not as evidence of toxicity. A diagnosis of Cordarone-induced interstitial/alveolar pneumonitis should lead, at a minimum, to dose reduction or, preferably, to withdrawal of the Cordarone to establish reversibility, especially if other acceptable antiarrhythmic therapies are available. Where these measures have been instituted, a reduction in symptoms of amiodarone-induced pulmonary toxicity was usually noted within the first week, and a clinical improvement was greatest in the first two to three weeks. Chest X-ray changes usually resolve within two to four months. According to some experts, steroids may prove beneficial. Prednisone in doses of 40 to 60 mg/day or equivalent doses of other steroids have been given and tapered over the course of several weeks depending upon the condition of the patient. In some cases rechallenge with Cordarone at a lower dose has not resulted in return of toxicity.
In a patient receiving Cordarone, any new respiratory symptoms should suggest the possibility of pulmonary toxicity, and the history, physical exam, chest X-ray, and pulmonary-function tests (with diffusion capacity) should be repeated and evaluated. A 15% decrease in diffusion capacity has a high sensitivity but only a moderate specificity for pulmonary toxicity; as the decrease in diffusion capacity approaches 30%, the sensitivity decreases but the specificity increases. A gallium-scan also may be performed as part of the diagnostic workup.
Fatalities, secondary to pulmonary toxicity, have occurred in approximately 10% of cases. However, in patients with life-threatening arrhythmias, discontinuation of Cordarone therapy due to suspected drug-induced pulmonary toxicity should be undertaken with caution, as the most common cause of death in these patients is sudden cardiac death. Therefore, every effort should be made to rule out other causes of respiratory impairment (i.e., congestive heart failure with Swan-Ganz catheterization if necessary, respiratory infection, pulmonary embolism, malignancy, etc.) before discontinuing Cordarone in these patients. In addition, bronchoalveolar lavage, transbronchial lung biopsy and/or open lung biopsy may be necessary to confirm the diagnosis, especially in those cases where no acceptable alternative therapy is available.
If a diagnosis of Cordarone-induced hypersensitivity pneumonitis is made, Cordarone should be discontinued, and treatment with steroids should be instituted. If a diagnosis of Cordarone-induced interstitial/alveolar pneumonitis is made, steroid therapy should be instituted and, preferably, Cordarone discontinued or, at a minimum, reduced in dosage. Some cases of Cordarone-induced interstitial/alveolar pneumonitis may resolve following a reduction in Cordarone dosage in conjunction with the administration of steroids. In some patients, rechallenge at a lower dose has not resulted in return of interstitial/alveolar pneumonitis; however, in some patients (perhaps because of severe alveolar damage) the pulmonary lesions have not been reversible.
Worsened Arrhythmia
Cordarone, like other antiarrhythmics, can cause serious exacerbation of the presenting arrhythmia, a risk that may be enhanced by the presence of concomitant antiarrhythmics. Exacerbation has been reported in about 2 to 5% in most series, and has included new ventricular fibrillation, incessant ventricular tachycardia, increased resistance to cardioversion, and polymorphic ventricular tachycardia associated with QTc prolongation (Torsade de Pointes [TdP]). In addition, Cordarone has caused symptomatic bradycardia or sinus arrest with suppression of escape foci in 2 to 4% of patients.
Fluoroquinolones, macrolide antibiotics, and azoles are known to cause QTc prolongation. There have been reports of QTc prolongation, with or without TdP, in patients taking amiodarone when fluoroquinolones, macrolide antibiotics, or azoles were administered concomitantly. (See "Drug Interactions, Other reported interactions with amiodarone").
The need to co-administer amiodarone with any other drug known to prolong the QTc interval must be based on a careful assessment of the potential risks and benefits of doing so for each patient.
A careful assessment of the potential risks and benefits of administering Cordarone must be made in patients with thyroid dysfunction due to the possibility of arrhythmia breakthrough or exacerbation of arrhythmia in these patients.
Implantable Cardiac Devices
In patients with implanted defibrillators or pacemakers, chronic administration of antiarrhythmic drugs may affect pacing or defibrillating thresholds. Therefore, at the inception of and during amiodarone treatment, pacing and defibrillation thresholds should be assessed.
Thyrotoxicosis
Cordarone-induced hyperthyroidism may result in thyrotoxicosis and/or the possibility of arrhythmia breakthrough or aggravation. There have been reports of death associated with amiodarone-induced thyrotoxicosis. IF ANY NEW SIGNS OF ARRHYTHMIA APPEAR, THE POSSIBILITY OF HYPERTHYROIDISM SHOULD BE CONSIDERED (see"PRECAUTIONS, Thyroid Abnormalities").
Liver Injury
Elevations of hepatic enzyme levels are seen frequently in patients exposed to Cordarone and in most cases are asymptomatic. If the increase exceeds three times normal, or doubles in a patient with an elevated baseline, discontinuation of Cordarone or dosage reduction should be considered. In a few cases in which biopsy has been done, the histology has resembled that of alcoholic hepatitis or cirrhosis. Hepatic failure has been a rare cause of death in patients treated with Cordarone.
Loss of Vision
Cases of optic neuropathy and/or optic neuritis, usually resulting in visual impairment, have been reported in patients treated with amiodarone. In some cases, visual impairment has progressed to permanent blindness. Optic neuropathy and/or neuritis may occur at any time following initiation of therapy. A causal relationship to the drug has not been clearly established. If symptoms of visual impairment appear, such as changes in visual acuity and decreases in peripheral vision, prompt ophthalmic examination is recommended. Appearance of optic neuropathy and/or neuritis calls for re-evaluation of Cordarone therapy. The risks and complications of antiarrhythmic therapy with Cordarone must be weighed against its benefits in patients whose lives are threatened by cardiac arrhythmias. Regular ophthalmic examination, including funduscopy and slit-lamp examination, is recommended during administration of Cordarone. (See "ADVERSE REACTIONS").
Neonatal Hypo- or Hyperthyroidism
Cordarone can cause fetal harm when administered to a pregnant woman. Although Cordarone use during pregnancy is uncommon, there have been a small number of published reports of congenital goiter/hypothyroidism and hyperthyroidism. If Cordarone is used during pregnancy, or if the patient becomes pregnant while taking Cordarone, the patient should be apprised of the potential hazard to the fetus.
In general, Cordarone Tablets should be used during pregnancy only if the potential benefit to the mother justifies the unknown risk to the fetus.
In pregnant rats and rabbits, amiodarone HCl in doses of 25 mg/kg/day (approximately 0.4 and 0.9 times, respectively, the maximum recommended human maintenance dose*) had no adverse effects on the fetus. In the rabbit, 75 mg/kg/day (approximately 2.7 times the maximum recommended human maintenance dose*) caused abortions in greater than 90% of the animals. In the rat, doses of 50 mg/kg/day or more were associated with slight displacement of the testes and an increased incidence of incomplete ossification of some skull and digital bones; at 100 mg/kg/day or more, fetal body weights were reduced; at 200 mg/kg/day, there was an increased incidence of fetal resorption. (These doses in the rat are approximately 0.8, 1.6 and 3.2 times the maximum recommended human maintenance dose.*) Adverse effects on fetal growth and survival also were noted in one of two strains of mice at a dose of 5 mg/kg/day (approximately 0.04 times the maximum recommended human maintenance dose*).
- 600 mg in a 50 kg patient (doses compared on a body surface area basis)
Precautions
Impairment of Vision
Optic Neuropathy and/or Neuritis
Cases of optic neuropathy and optic neuritis have been reported (see "WARNINGS").
Corneal Microdeposits
Corneal microdeposits appear in the majority of adults treated with Cordarone. They are usually discernible only by slit-lamp examination, but give rise to symptoms such as visual halos or blurred vision in as many as 10% of patients. Corneal microdeposits are reversible upon reduction of dose or termination of treatment. Asymptomatic microdeposits alone are not a reason to reduce dose or discontinue treatment (see "ADVERSE REACTIONS").
Neurologic
Chronic administration of oral amiodarone in rare instances may lead to the development of peripheral neuropathy that may resolve when amiodarone is discontinued, but this resolution has been slow and incomplete.
Photosensitivity
Cordarone has induced photosensitization in about 10% of patients; some protection may be afforded by the use of sun-barrier creams or protective clothing. During long-term treatment, a blue-gray discoloration of the exposed skin may occur. The risk may be increased in patients of fair complexion or those with excessive sun exposure, and may be related to cumulative dose and duration of therapy.
Thyroid Abnormalities
Cordarone inhibits peripheral conversion of thyroxine (T4) to triiodothyronine (T3) and may cause increased thyroxine levels, decreased T3 levels, and increased levels of inactive reverse T3 (rT3) in clinically euthyroid patients. It is also a potential source of large amounts of inorganic iodine. Because of its release of inorganic iodine, or perhaps for other reasons, Cordarone can cause either hypothyroidism or hyperthyroidism. Thyroid function should be monitored prior to treatment and periodically thereafter, particularly in elderly patients, and in any patient with a history of thyroid nodules, goiter, or other thyroid dysfunction. Because of the slow elimination of Cordarone and its metabolites, high plasma iodide levels, altered thyroid function, and abnormal thyroid-function tests may persist for several weeks or even months following Cordarone withdrawal.
Hypothyroidism has been reported in 2 to 4% of patients in most series, but in 8 to 10% in some series. This condition may be identified by relevant clinical symptoms and particularly by elevated serum TSH levels. In some clinically hypothyroid amiodarone-treated patients, free thyroxine index values may be normal. Hypothyroidism is best managed by Cordarone dose reduction and/or thyroid hormone supplement. However, therapy must be individualized, and it may be necessary to discontinue Cordarone® Tablets in some patients.
Hyperthyroidism occurs in about 2% of patients receiving Cordarone, but the incidence may be higher among patients with prior inadequate dietary iodine intake. Cordarone-induced hyperthyroidism usually poses a greater hazard to the patient than hypothyroidism because of the possibility of thyrotoxicosis and/or arrhythmia breakthrough or aggravation, all of which may result in death. There have been reports of death associated with amiodarone-induced thyrotoxicosis. IF ANY NEW SIGNS OF ARRHYTHMIA APPEAR, THE POSSIBILITY OF HYPERTHYROIDISM SHOULD BE CONSIDERED.
Hyperthyroidism is best identified by relevant clinical symptoms and signs, accompanied usually by abnormally elevated levels of serum T3 RIA, and further elevations of serum T4, and a subnormal serum TSH level (using a sufficiently sensitive TSH assay). The finding of a flat TSH response to TRH is confirmatory of hyperthyroidism and may be sought in equivocal cases. Since arrhythmia breakthroughs may accompany Cordarone-induced hyperthyroidism, aggressive medical treatment is indicated, including, if possible, dose reduction or withdrawal of Cordarone.
The institution of antithyroid drugs, β-adrenergic blockers and/or temporary corticosteroid therapy may be necessary. The action of antithyroid drugs may be especially delayed in amiodarone-induced thyrotoxicosis because of substantial quantities of preformed thyroid hormones stored in the gland. Radioactive iodine therapy is contraindicated because of the low radioiodine uptake associated with amiodarone-induced hyperthyroidism. Cordarone-induced hyperthyroidism may be followed by a transient period of hypothyroidism (see "WARNINGS, Thyrotoxicosis").
When aggressive treatment of amiodarone-induced thyrotoxicosis has failed or amiodarone cannot be discontinued because it is the only drug effective against the resistant arrhythmia, surgical management may be an option. Experience with thyroidectomy as a treatment for amiodarone-induced thyrotoxicosis is limited, and this form of therapy could induce thyroid storm. Therefore, surgical and anesthetic management require careful planning.
There have been postmarketing reports of thyroid nodules/thyroid cancer in patients treated with Cordarone. In some instances hyperthyroidism was also present (see "WARNINGS" and "ADVERSE REACTIONS").
Surgery
Volatile Anesthetic Agents: Close perioperative monitoring is recommended in patients undergoing general anesthesia who are on amiodarone therapy as they may be more sensitive to the myocardial depressant and conduction effects of halogenated inhalational anesthetics.
Hypotension Postbypass: Rare occurrences of hypotension upon discontinuation of cardiopulmonary bypass during open-heart surgery in patients receiving Cordarone have been reported. The relationship of this event to Cordarone therapy is unknown.
Adult Respiratory Distress Syndrome (ARDS): Postoperatively, occurrences of ARDS have been reported in patients receiving Cordarone therapy who have undergone either cardiac or noncardiac surgery. Although patients usually respond well to vigorous respiratory therapy, in rare instances the outcome has been fatal. Until further studies have been performed, it is recommended that FiO2 and the determinants of oxygen delivery to the tissues (e.g., SaO2, PaO2) be closely monitored in patients on Cordarone.
Corneal Refractive Laser Surgery
Patients should be advised that most manufacturers of corneal refractive laser surgery devices contraindicate that procedure in patients taking Cordarone.
Information for Patients
Patients should be instructed to read the accompanying Medication Guide each time they refill their prescription. Thecomplete text of the Medication Guide is reprinted at the end of this document.
Laboratory Tests
Elevations in liver enzymes (SGOT and SGPT) can occur. Liver enzymes in patients on relatively high maintenance doses should be monitored on a regular basis. Persistent significant elevations in the liver enzymes or hepatomegaly should alert the physician to consider reducing the maintenance dose of Cordarone or discontinuing therapy.
Cordarone alters the results of thyroid-function tests, causing an increase in serum T4 and serum reverse T3, and a decline in serum T3 levels. Despite these biochemical changes, most patients remain clinically euthyroid.
Electrolyte Disturbances
Since antiarrhythmic drugs may be ineffective or may be arrhythmogenic in patients with hypokalemia, any potassium or magnesium deficiency should be corrected before instituting and during Cordarone therapy. Use caution when coadministering Cordarone with drugs which may induce hypokalemia and/or hypomagnesemia.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Amiodarone HCl was associated with a statistically significant, dose-related increase in the incidence of thyroid tumors (follicular adenoma and/or carcinoma) in rats. The incidence of thyroid tumors was greater than control even at the lowest dose level tested, i.e., 5 mg/kg/day (approximately 0.08 times the maximum recommended human maintenance dose*). Mutagenicity studies (Ames, micronucleus, and lysogenic tests) with Cordarone were negative. In a study in which amiodarone HCl was administered to male and female rats, beginning 9 weeks prior to mating, reduced fertility was observed at a dose level of 90 mg/kg/day (approximately 1.4 times the maximum recommended human maintenance dose*).
- 600 mg in a 50 kg patient (dose compared on a body surface area basis)
Pregnancy: Pregnancy Category D
See "WARNINGS, Neonatal Hypo- or Hyperthyroidism".
Labor and Delivery
It is not known whether the use of Cordarone during labor or delivery has any immediate or delayed adverse effects. Preclinical studies in rodents have not shown any effect of Cordarone on the duration of gestation or on parturition.
Nursing Mothers
Cordarone and one of its major metabolites, desethylamiodarone (DEA), are excreted in human milk, suggesting that breast-feeding could expose the nursing infant to a significant dose of the drug. Nursing offspring of lactating rats administered Cordarone have been shown to be less viable and have reduced body-weight gains. Therefore, when Cordarone therapy is indicated, the mother should be advised to discontinue nursing.
Pediatric Use
The safety and effectiveness of Cordarone Tablets in pediatric patients have not been established.
Geriatric Use
Clinical studies of Cordarone Tablets did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.[1]
References
Adapted from the FDA Package Insert.