Ceftaroline clinical studies
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1];Associate Editor(s)-in-Chief: Abdurahman Khalil, M.D. [2]
Acute Bacterial Skin and Skin Structure Infections (ABSSSI)
A total of 1396 adults with clinically documented complicated skin and skin structure infection were enrolled in two identical randomized, multi-center, multinational, double-blind, non-inferiority trials (Trials 1 and 2) comparing Teflaro (600 mg administered IV over 1 hour every 12 hours) to vancomycin plus aztreonam (1 g vancomycin administered IV over 1 hour followed by 1 g aztreonam administered IV over 1 hour every 12 hours). Treatment duration was 5 to 14 days. A switch to oral therapy was not allowed. The Modified Intent-to-Treat (MITT) population included all patients who received any amount of study drug according to their randomized treatment group. The CE population included patients in the MITT population who demonstrated sufficient adherence to the protocol.
To evaluate the treatment effect of ceftaroline, an analysis was conducted in 797 patients with ABSSSI (such as deep/extensive cellulitis or a wound infection [surgical or traumatic]) for whom the treatment effect of antibacterials may be supported by historical evidence. This analysis evaluated responder rates based on achieving both cessation of lesion spread and absence of fever on Trial Day 3 in the following subgroup of patients:
Patients with lesion size ≥ 75 cm2and having one of the following infection types:
Major abscess with ≥ 5 cm of surrounding erythema Wound infection Deep/extensive cellulitis
The results of this analysis are shown inTable 8.
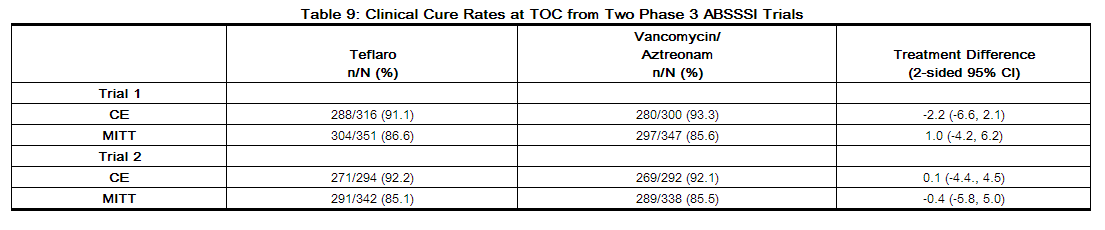
The protocol-specified analyses included clinical cure rates at the Test of Cure (TOC) (visit 8 to 15 days after the end of therapy) in the co-primary CE and MITT populations (Table 9) and clinical cure rates at TOC by pathogen in the Microbiologically Evaluable (ME) population (Table 10). However, there are insufficient historical data to establish the magnitude of drug effect for antibacterial drugs compared with placebo at a TOC time point. Therefore, comparisons of Teflaro to vancomycin plus aztreonam based on clinical response rates at TOC can not be utilized to establish non-inferiority.
Community-Acquired Bacterial Pneumonia (CABP)
A total of 1231 adults with a diagnosis of CABP were enrolled in two randomized, multi-center, multinational, double-blind, non-inferiority trials (Trials 1 and 2) comparing Teflaro (600 mg administered IV over 1 hour every 12 hours) with ceftriaxone (1 g ceftriaxone administered IV over 30 minutes every 24 hours). In both treatment groups of CABP Trial 1, two doses of oral clarithromycin (500 mg every 12 hours), were administered as adjunctive therapy starting on Study Day 1. No adjunctive macrolide therapy was used in CABP Trial 2. Patients with known or suspected MRSA were excluded from both trials. Patients with new or progressive pulmonary infiltrate(s) on chest radiography and signs and symptoms consistent with CABP with the need for hospitalization and IV therapy were enrolled in the trials. Treatment duration was 5 to 7 days. A switch to oral therapy was not allowed. Among all subjects who received any amount of study drug in the two CABP trials, the 30-day all-cause mortality rates were 11/609 (1.8%) for the Teflaro group vs. 12/610 (2.0%) for the ceftriaxone group, and the difference in mortality rates was not statistically significant.
To evaluate the treatment effect of ceftaroline, an analysis was conducted in CABP patients for whom the treatment effect of antibacterials may be supported by historical evidence. The analysis endpoint required subjects to meet sign and symptom criteria at Day 4 of therapy: a responder had to both (a) be in stable condition according to consensus treatment guidelines of the Infectious Diseases Society of America and American Thoracic Society, based on temperature, heart rate, respiratory rate, blood pressure, oxygen saturation, and mental status;4(b) show improvement from baseline on at least one symptom of cough, dyspnea, pleuritic chest pain, or sputum production, while not worsening on any of these four symptoms. The analysis used a microbiological intent-to-treat population (mITT population) containing only subjects with a confirmed bacterial pathogen at baseline. Results for this analysis are presented inTable 11.
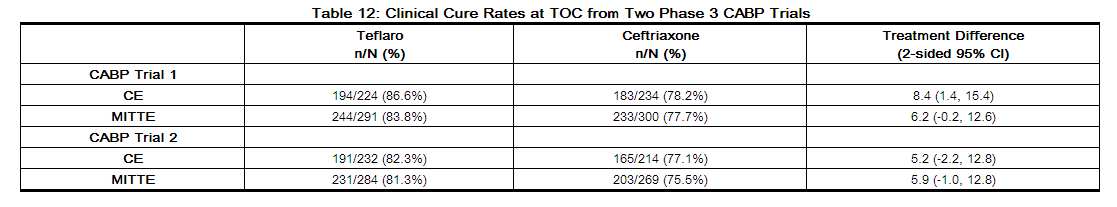
The protocol-specified analyses included clinical cure rates at the TOC (8 to 15 days after the end of therapy) in the co-primary Modified Intent-to-Treat Efficacy (MITTE) and CE populations (Table 12) and clinical cure rates at TOC by pathogen in the Microbiologically Evaluable (ME) population (Table 13). However, there are insufficient historical data to establish the magnitude of drug effect for antibacterials drugs compared with placebo at a TOC time point. Therefore, comparisons of Teflaro to ceftriaxone based on clinical response rates at TOC cannot be utilized to establish non-inferiority. Neither trial established that Teflaro was statistically superior to ceftriaxone in terms of clinical response rates. The MITTE population included all patients who received any amount of study drug according to their randomized treatment group and were in PORT (Pneumonia Outcomes Research Team) Risk Class III or IV. The CE population included patients in the MITTE population who demonstrated sufficient adherence to the protocol.
References
http://www.accessdata.fda.gov/drugsatfda_docs/label/2011/200327s001lbl.pdf