Varicose veins: Difference between revisions
No edit summary |
No edit summary |
||
| Line 4: | Line 4: | ||
Image = Varicose-veins.jpg| | Image = Varicose-veins.jpg| | ||
Caption = | | Caption = | | ||
}} | }} | ||
{{SI}} | {{SI}} | ||
Revision as of 17:18, 7 February 2013
| Varicose veins | |
 |
|---|
|
WikiDoc Resources for Varicose veins |
|
Articles |
|---|
|
Most recent articles on Varicose veins Most cited articles on Varicose veins |
|
Media |
|
Powerpoint slides on Varicose veins |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Varicose veins at Clinical Trials.gov Trial results on Varicose veins Clinical Trials on Varicose veins at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Varicose veins NICE Guidance on Varicose veins
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Varicose veins Discussion groups on Varicose veins Patient Handouts on Varicose veins Directions to Hospitals Treating Varicose veins Risk calculators and risk factors for Varicose veins
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Varicose veins |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [7]
Synonyms and keywords: Varicosities; venous insufficiency; phlebectasia
Overview
Varicose veins are veins that have become enlarged and twisted. The term commonly refers to the veins on the leg, although varicose veins occur elsewhere. Veins have leaflet valves to prevent blood from flowing backwards (retrograde). Leg muscles pump the veins to return blood to the heart. When veins become enlarged, the leaflets of the valves no longer meet properly, and the valves don't work. A common cause of valve failure is Deep Vein Thrombosis (DVT), which can cause permanent damage to the valves. The blood collects in the veins and they enlarge even more. Varicose veins are common in the superficial veins of the legs, which are subject to high pressure when standing. Besides cosmetic problems, varicose veins are often painful, especially when standing or walking. They often itch, and scratching them can cause ulcers. Serious complications are rare. Non-surgical treatments include sclerotherapy, elastic stockings, elevating the legs, and exercise. The traditional surgical treatment has been vein stripping to remove the affected veins. Newer surgical treatments are less invasive (see radiofrequency ablation) and are slowly replacing traditional surgical treatments. Since most of the blood in the legs is returned by the deep veins, and the superficial veins only return about 10%, they can be removed or ablated without serious harm.[1]
Causes
Varicose veins are more common in women than in men, and are linked with heredity[2]. Other related factors are pregnancy, obesity, menopause, aging, prolonged standing, leg injury and abdominal straining. Varicose veins are bulging veins that are larger than spider veins, typically 3 mm or more in diameter.[3] Varicose veins are distinguished from reticular veins (blue veins) and telangiectasias (spider veins) which also involve valvular insufficiency,[4] by the size and location of the veins.
Symptoms
- Aching, heavy legs (often worse at night and after exercise)
- Ankle swelling
- A brownish-blue shiny skin discoloration around the veins
- Skin over the vein may become dry, itchy and thin, leading to eczema (venous eczema)
- The skin may darken (stasis dermatitis), because of the waste products building up in the legs
- Minor injuries to the area may bleed more than normal and/or take a long time to heal
- Rarely, there is a large amount of bleeding from a ruptured vein
- In some people the skin above the ankle may shrink (lipodermatosclerosis) because the fat underneath the skin becomes hard.
- Restless Leg Syndrome[5]. Restless Leg Syndrome appears to be a common overlapping clinical syndrome in patients with varicose veins and other chronic venous insufficiency.
-
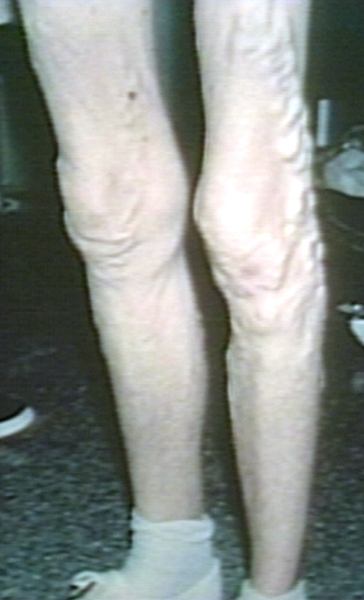
Varicose veins
(Image courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA)
Treatment
Conservative treatment
The symptoms of varicose veins can be controlled to an extent with the following:
- Elevating the legs often provides temporary symptomatic relief.
- "Advice about regular exercise sounds sensible but is not supported by any evidence."[6]
- The wearing of graduated compression stockings with a pressure of 30–40 mmHg has been shown to correct the swelling, nutritional exchange, and improve the microcirculation in legs affected by varicose veins.[7] They also often provide relief from the discomfort associated with this disease. Caution should be exercised in their use in patients with concurrent arterial disease.
The symptoms of varicose veins can be controlled to an extent with either of the following:
- Anti-inflammatory medication such as ibuprofen or aspirin can be used as part of treatment for superficial thrombophlebitis along with graduated compression hosiery – but there is a risk of intestinal bleeding. In extensive superficial thrombophlebitis, consideration should be given to anti-coagulation, thrombectomy or sclerotherapy of the involved vein.
- Diosmin 95 is a dietary supplement distributed in the U.S. by Nutratech, Inc. The U.S. Food and Drug Administration does not approve dietary supplements, and concluded that there was an "inadequate basis for reasonable expectation of safety." [8] [9]
Surgical treatment
Several techniques have been performed for over a century, from the more invasive named "saphenous stripping" up to mini invasives like superficial phlectomies and CHIVA cure.
Stripping
Stripping consists in a removal of all the saphena vein main trunk from the groin down to the ankle.The complications include deep vein thrombosis (5.3%),[10] pulmonary embolism (0.06%), and wound complications including infection (2.2%). For traditional surgery, reported recurrence rates, which have been tracked for 10 years, range from 5-60%. In addition, since stripping removes the saphenous main trunks, they are no longer availlable for venous by-pass in the future (coronary and/or leg artery vital disease)[11]
CHIVA
CHIVA is the acronym for Conservative and Haemodynamic cure of Incompetent Varicose veins in Ambulatory patients translated from the French cure "Conservatrice et Hémodynamique de l'Insuffisance Veineuse en Ambulatoire"[12] published in France in 1988.
- Pathophysiological principles
CHIVA relies on an hemodynamic impairment assessed by data and evidences depicted through Ultrasound dynamic venous investigations. According to this new concept, the clinical symptoms of venous insufficiency are not the cause but the consequence of various abnormalities of the venous system. For example,a varicose vein being overloaded, may be dilated not only because of valvular incompetence (the most frequent) but because of a venous block (thombosis) or arterio-venous fistulae...and so the treatment has to be tailord according the hemodynamic feature.
- Procedure and outcomes
It generally consists in 1 to 4 small incisions under local anaestesia in order to disconnect the varicose veins from the abnormal flow due to valvular incompetence which dilates them.[13] The patient is dismissed the same day. This method leads to an improvement of the venous function in order to:
- Cure the symptoms of venous insufficiency as varicose veins, legs swelling, ulcers.[14][15]
- Prevent varicose recurrence due to progressive enlargement of collateral veins which replace and overtake the destroyed veins: CHIVA vs Stripping: varicose recurrence divided by 2 to 5 at 10 years.[16]
- Preserve the superficial venous capital for unpredictable but possible need for coronary or leg artery vital by-pass which increases with ageing.
- Consequences
To be achieved properly,CHIVA method needs a comprehensive knowledge of both hemodynamics and Ultrasound venous investigation.
Non-surgical treatment
Sclerotherapy
A commonly performed non-surgical treatment for varicose and "spider" leg veins is sclerotherapy. It has been used in the treatment of varicose veins for over 150 years.[17] Sclerotherapy is often used for telangiectasias (spider veins) and varicose veins that persist or recur after vein stripping.[18][19]
Sclerotherapy can also be performed using microfoam sclerosants under ultrasound guidance to treat larger varicose veins, including the greater and short saphenous veins.[20][21] A study by Kanter and Thibault in 1996 reported a 76% success rate at 24 months in treating saphenofemoral junction and great saphenous vein incompetence with STS 3% solution.[22] A Cochrane Collaboration review[23] concluded sclerotherapy was better than surgery in the short term (1 year) for its treatment success, complication rate and cost, but surgery was better after 5 years, although the research is weak.[24]
A Health Technology Assessment found that sclerotherapy provided less benefit than surgery, but is likely to provide a small benefit in varicose veins without reflux.[25] Complications of sclerotherapy are rare but can include blood clots and ulceration. Anaphylactic reactions are "extraordinarily rare but can be life-threatening," and doctors should have resuscitation equipment ready.[26] There has been one reported case of stroke after ultrasound guided sclerotherapy when an unusually large dose of sclerosant foam was injected.
Endovenous laser and radiofrequency ablation
The Australian Medical Services Advisory Committee (MSAC) in 2008 has determined that endovenous laser treatment for varicose veins "appears to be more effective in the short term, and at least as effective overall, as the comparative procedure of junction ligation and vein stripping for the treatment of varicose veins."[27] It also found in its assessment of available literature, that "occurrence rates of more severe complications such as DVT, nerve injury and paraesthesia, post-operative infections and haematomas, appears to be greater after ligation and stripping than after EVLT". Complications for endovenous laser treatment include minor skin burns (0.4%)[28] and temporary paraesthesia (2.1%).[28] The longest study of endovenous laser ablation is 39 months.
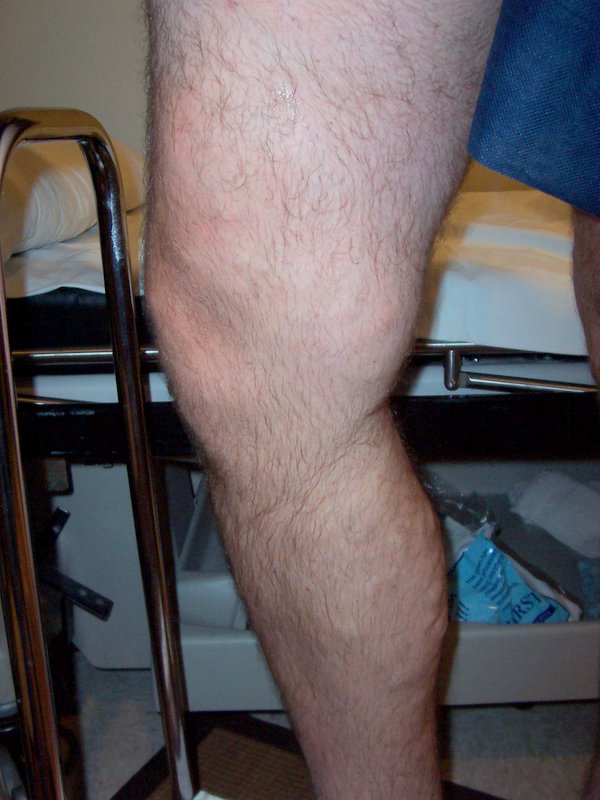
-
Varicose veins after EVLT
Two prospective randomized trials found speedier recovery and fewer complications after radiofrequency obliteration (AKA radiofrequency ablation) compared to open surgery.[29][30] Myers[31] wrote that open surgery for small saphenous vein reflux is obsolete. Myers said these veins should be treated with endovenous techniques, citing high recurrence rates after surgical management, and risk of nerve damage up to 15%. In comparison, radiofrequency ablation has been shown to control 80% of cases of small saphenous vein reflux at 4 years, said Myers. Complications for radiofrequency ablation include burns, paraesthesia, clinical phlebitis, and slightly higher rates of deep vein thrombosis (0.57%) and pulmonary embolism (0.17%).One 3-year study compared radiofrequency, with a recurrence rate of 33%, to open surgery, which had a recurrence rate of 23%.
Endovenous laser and radiofrequency ablation require specialized training for doctors and expensive equipment. Endovenous laser treatment is performed as an outpatient procedure and does not require the use of an operating theatre, nor does the patient need a general anaesthetic. Doctors must use ultrasound during the procedure to see what they are doing. Some practitioners also perform phlebectomy or ultrasound guided sclerotherapy at the time of endovenous treatment. Follow-up treatment to smaller branch varicose veins is often needed in the weeks after the initial procedure.
Other treatments are:
- ambulatory phlebectomy
- laser vein removal
- vein ligation
Complications
Most varicose veins are relatively benign, but severe varicosities can lead to major complications, due to the poor circulation through the affected limb.
- Pain, heaviness, inability to walk or stand for long hours thus hindering work
- Skin conditions / Dermatitis which could predispose skin loss
- Bleeding : life threatening bleed from injury to the varicose vein
- Ulcer : non healing varicose ulcer could threaten limb amputation.
- Development of carcinoma or sarcoma in longstanding venous ulcers. There have been over 100 reported cases of malignant transformation and the rate is reported as 0.4% to 1%.[32]
- Coagulation of blood in varicose veins cause superficial thrombosis, deep vein thrombosis (DVT), Pulmonary Embolism (PE) & could precipitate stroke in the rare case of predisposed individuals (that is, patients with patent foramen ovale).
External links
- Varicose Veins and varicosities
- Varicose Vein overview
- NHS Direct - Varicose Veins
- Varicose Veins Society for Vascular Surgery patient pages. Good illustrations.
- Varicose Vein Treatment in Australasia Information from the Australasian College of Phlebology Website
- Venous disease forum Blog for physicians to collaborate on vein disease treatment
- Varicose veins: Operation Script on Wikisurgery.
- Varicose veins: Information for patients on Wikisurgery
References
- ↑ Merck Manual Home Edition, 2nd ed.[1]
- ↑ Ng M, Andrew T, Spector T, Jeffery S (2005). "Linkage to the FOXC2 region of chromosome 16 for varicose veins in otherwise healthy, unselected sibling pairs". J Med Genet. 42 (3): 235–9. PMID 15744037.
- ↑ NHS Direct[2]
- ↑ Weiss R A, Weiss M A, Doppler Ultrasound Findings in Reticular Veins of the Thigh Subdermic Lateral Venous System and Implications for Sclerotherapy, Journal of Derm Surg Onc, Vol 19 No 10 (Oct 1993) p947-951.
- ↑ Schul M., McDonagh B., Guptan R.C. (2005). "High Prevalence Of Restless Leg syndrome In Patients With Chronic Venous Insufficiency." RLS & varicose veins
- ↑ BMJ 2006;333:287-292 (5 August), Varicose veins and their management, Bruce Campbell (subscription)
- ↑ Curri SB et al. Changes of cutaneous microcirculation from elasto-compression in chronic venous insufficiency. In Davy A and Stemmer R, editors: Phlebology '89, Montrouge, France, 1989, John Libbey Eurotext.
- ↑ New Dietary Ingredients in Dietary Supplements, U. S. Food and Drug Administration Center for Food Safety and Applied Nutrition Office of Nutritional Products, Labeling, and Dietary Supplements February 2001 (Updated September 10, 2001), http://www.cfsan.fda.gov/~dms/ds-ingrd.html
- ↑ Memorandum [3]
- ↑ van Rij AM et al. Incidence of Deep Venous Thrombosis after Varicose Vein Surgery, Br J Surg 2004 Dec;91(12):1582-5
- ↑ Hammarsten J, Pedersen P, Cederlund CG, Campanello M. Department of Surgery and Radiology, Hospital of Varberg, Sweden Long saphenous vein saving surgery for varicose veins. A long-term follow-up. Eur J Vasc Surg. 1990 Aug;4(4):361-4.
- ↑ claude Franceschi, Cure CHIVA, 1988, Editions de L'Armançon, 21390 Precy-Sous-Thil France
- ↑ [4]
- ↑ Maeso and all, Comparision of clinical outcome of Stripping and CHIVA for Treatment of varicose veins in Lower Extremities, Ann Vasc Surg 2001; 15: 661-665
- ↑ " Zamboni and all: Minimally Invasive Surgical management of primary Venous Ulcers vs Compression Treatment: a randomized Clinical Trial. Eur J Vasc Endovsc Surg 00,1-6 (2003)
- ↑ Varicose Vein Stripping vs. Haemodynamic Correction (C.H.I.V.A.): a Long Term Randomised Trial S. Carandina and all; Eur J Vasc Endovasc Surg xx, 1e8 (2007) doi:10.1016/j.ejvs.2007.09.011, online http://www.sciencedirect.com
- ↑ Goldman M, Sclerotherapy Treatment of varicose and telangiectatic leg vein, Hardcover Text, 2nd Ed, 1995
- ↑ "Veins & Lymphatics," L. K. Pak et al, in Lange's Current Surgical Diagnosis & Treatment, 11th ed., McGraw-Hill,
- ↑ Tisi PV, Beverley C, Rees A. Injection sclerotherapy for varicose veins. Cochrane Database of Systematic Reviews 2006, Issue 4. Art. No.: CD001732.
- ↑ Paul Thibault, Sclerotherapy and Ultrasound-Guided Sclerotherapy, The Vein Book / editor, John J. Bergan, 2007.
- ↑ Padbury A, Benveniste G L, Foam echosclerotherapy of the small saphenous vein, Australian and New Zealand Journal of Phlebology Vol 8, Number 1 (December 2004)
- ↑ Kanter A, Thibault P. Saphenofemoral junction incompetence treated by ultrasound-guided sclerotherapy, Dermatol Surg. 1996. 22: 648-652.
- ↑ http://www.mrw.interscience.wiley.com/cochrane/clsysrev/articles/CD001732/abstract.html
- ↑ Rigby KA, Palfreyman SJ, Beverley C, Michaels JA. Surgery versus sclerotherapy for the treatment of varicose veins. Cochrane Database of Systematic Reviews 2004, Issue 4. Art. No.: CD004980. [5]
- ↑ Michaels JA, Campbell WB, Brazier JE, MacIntyre JB, Palfreyman SJ, Ratcliffe J, et al. Randomized clinical trial, observational study and assessment of cost-effectiveness of the treatment of varicose veins (REACTIV trial). Health Technol Assess 2006;10(13). [6] This Health Technology Assessment monograph includes reviews of the epidemiology, assessment, and treatment of varicose veins, as well as a study on clinical and cost effectiveness of surgery and sclerotherapy
- ↑ William R. Finkelmeier, Sclerotherapy, Ch. 12, ACS Surgery: Principles & Practice, 2004, WebMD (hardcover book)
- ↑ Medical Services Advisory Committee, Endovenous laser therapy (ELT) for varicose veins. MSAC application 1113, Dept of Health and Ageing, Commonwealth of Australia, 2008. http://www.msac.gov.au/internet/msac/publishing.nsf/Content/2E0BACBB8704139ACA25745E001C2F21/$File/1113report.pdf
- ↑ 28.0 28.1 Elmore FA and Lackey D, Effectiveness of laser treatment in eliminating superficial venous reflux, Phlebology 2008 :23 :21-31
- ↑ Rautio, T, et al., Endovenous oblitration versus conventional stripping operation in the treatment of primary varicose veins, J Vasc Surg 2002:35:958-65
- ↑ Lurie F, et al., Prospective randomized study of endovenous radiofrequency oblitration (closure) versus ligation and vein stripping (EVOLVeS: two-year follow-up. Eur J Vasc Endovasc Surg 2005;29:67-73
- ↑ Kenneth Myers, An opinion —surgery for small saphenous reflux is obsolete!" Australian and New Zealand Journal of Phlebology, Vol 8, Number 1 (December 2004)
- ↑ Goldman M. Sclerotherapy, Treatment of Varicose and Telangiectatic Leg Veins. Hardcover Text, 2nd Ed, 1995