Prepatellar bursitis
For patient information page click here
| Prepatellar bursitis | |
 | |
|---|---|
| Aseptic prepatellar bursitis | |
| ICD-10 | M70.4 |
| ICD-9 | 726.65 |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor-In-Chief: Cafer Zorkun, M.D., Ph.D. [2] Please Take Over This Page and Apply to be Editor-In-Chief for this topic: There can be one or more than one Editor-In-Chief. You may also apply to be an Associate Editor-In-Chief of one of the subtopics below. Please mail us [3] to indicate your interest in serving either as an Editor-In-Chief of the entire topic or as an Associate Editor-In-Chief for a subtopic. Please be sure to attach your CV and or biographical sketch.
Synonyms and keywords: Housemaid's knee
Overview
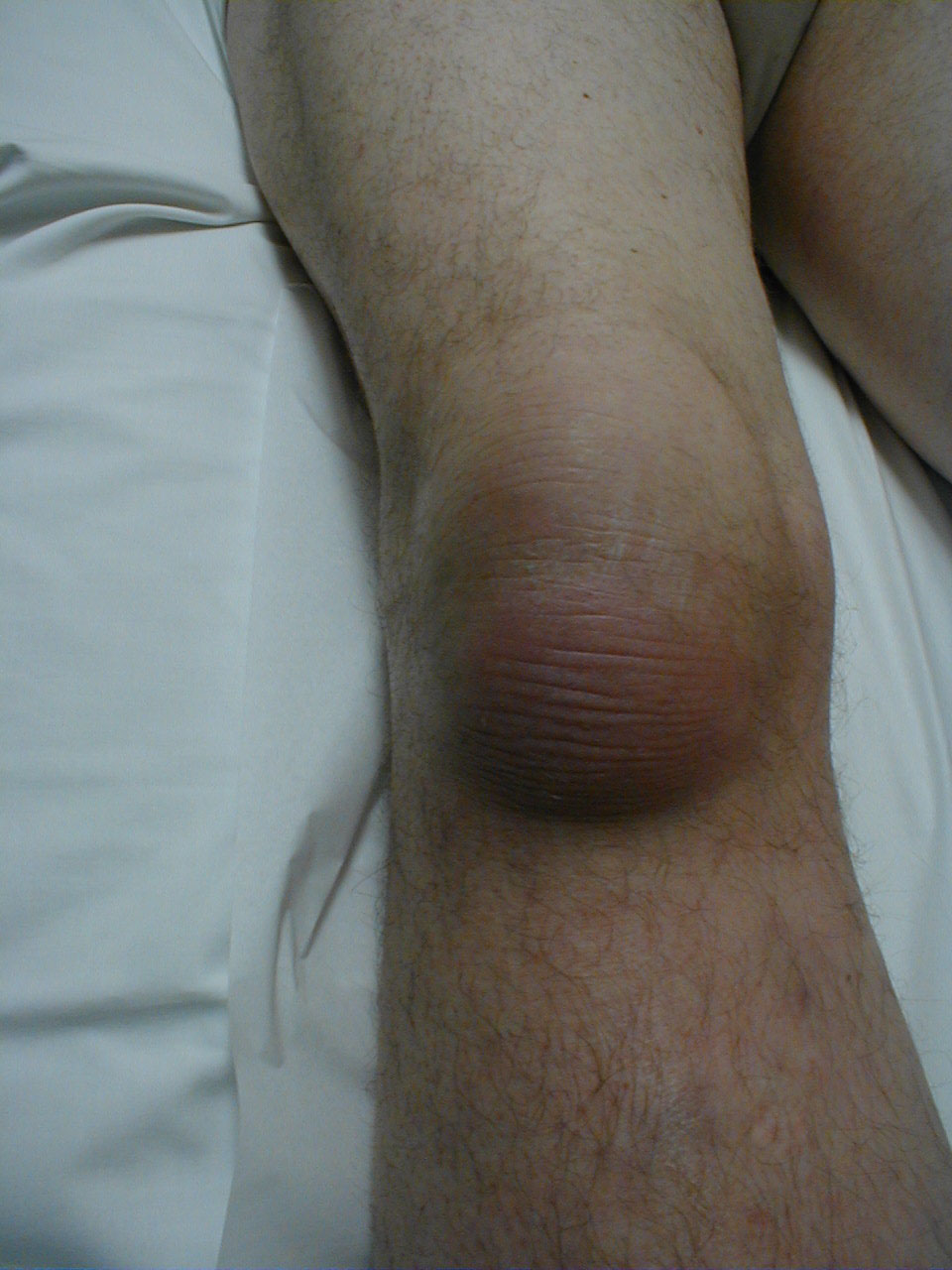
Prepatellar bursitis, also known as housemaid's knee, is a common cause of swelling and pain above the patella (kneecap), and is due to inflammation of the prepatellar bursa. This structure is a superficial bursa with a thin synovial lining located between the skin and the patella. The bursa develops within the first years of life as a result of mechanical pressure and friction, and it serves the purpose of reducing friction on underlying structures and allowing maximal range of motion in the knee.
Aseptic prepatellar bursitis is commonly caused by repetitive work in a kneeling position, hence the name "housemaid's knee".
Inflammation of the prepatellar bursa may be aseptic (most common) or septic (e.g. bacterial infection), the septic variants being most common in children and immunocompromised individuals.
Prepatellar bursitis is more common in men than women.
Physical Examination
-
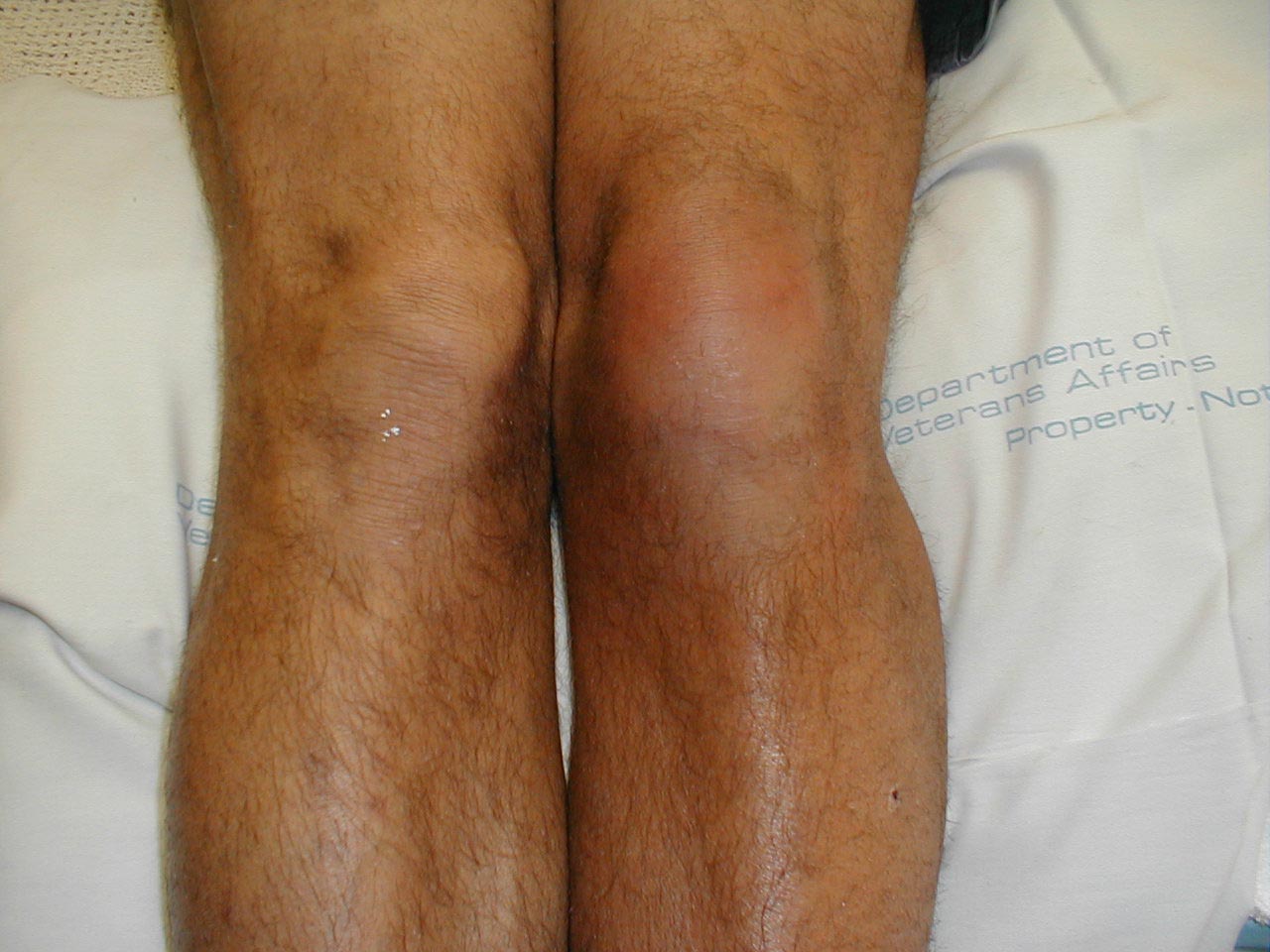
Prepatellar Bursitis: Redness and swelling of left prepatellar bursa caused by bacterial infection.
-
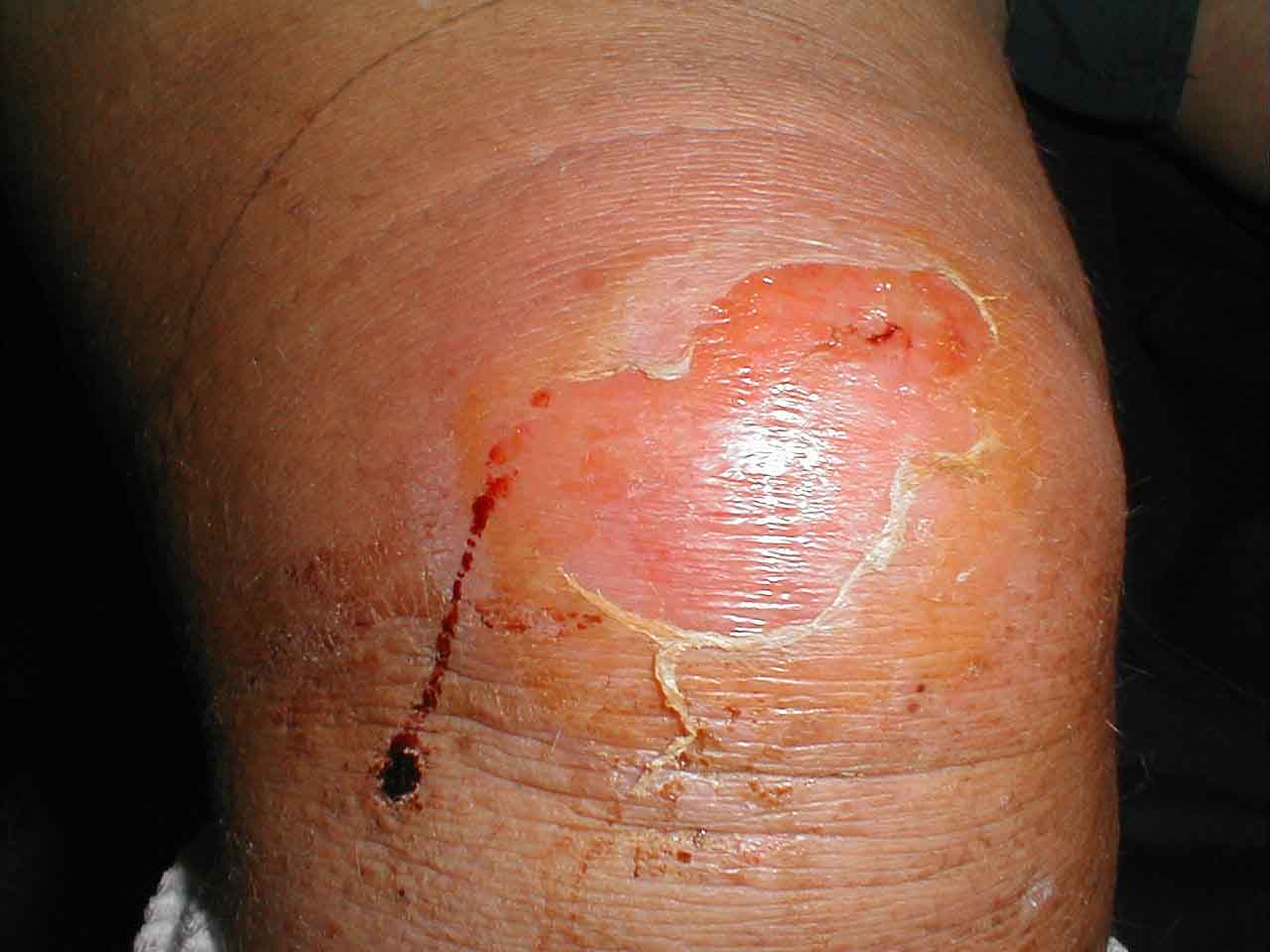
Prepatellar Bursitis: Redness and swelling of prepatellar bursa caused by bacterial infection. Inflammation and edema have led to desquamation.
-
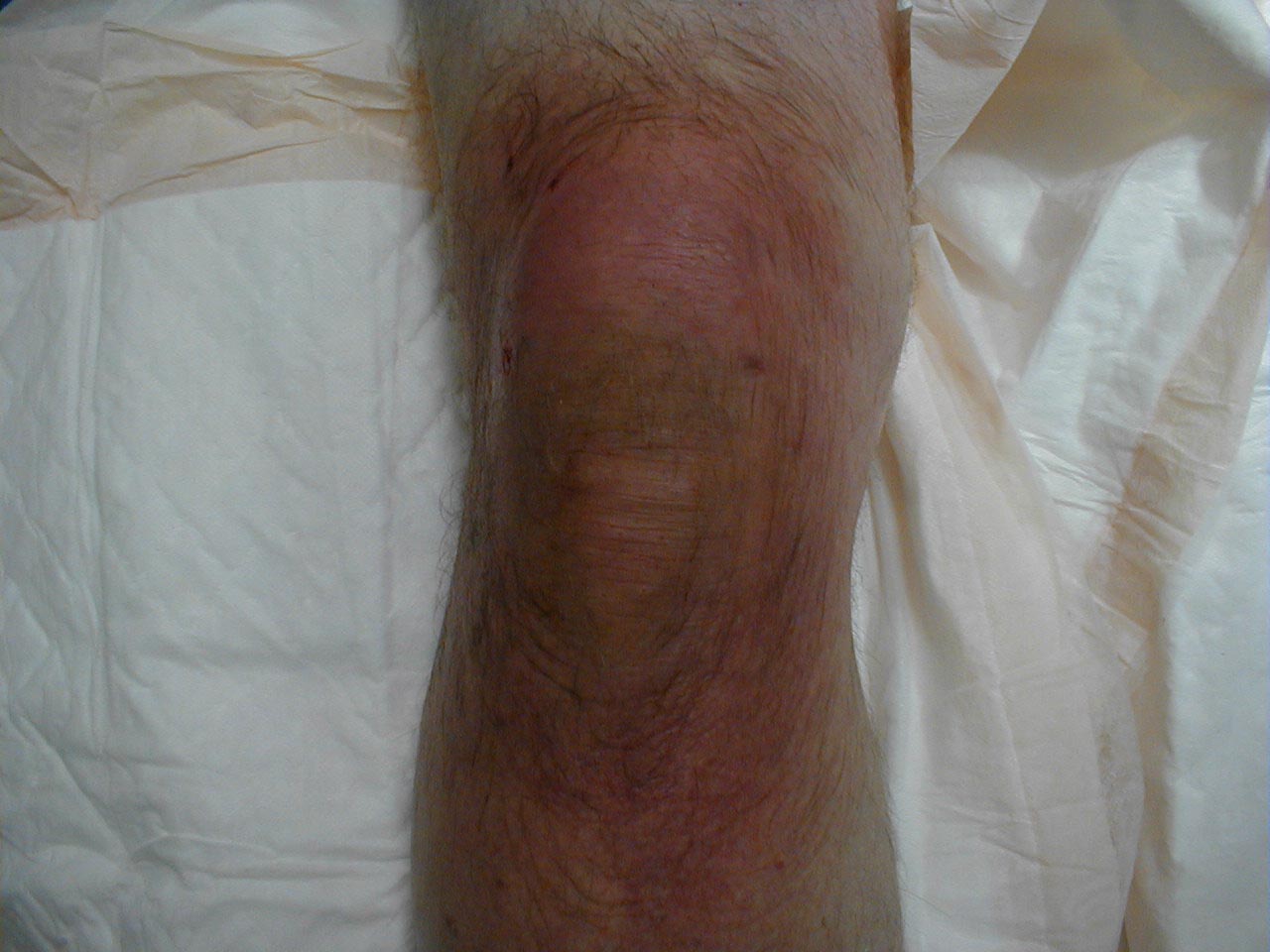
Prepatellar Bursitis: Extensive redness and swelling caused by bacterial infection involving pre patellar bursae.
-
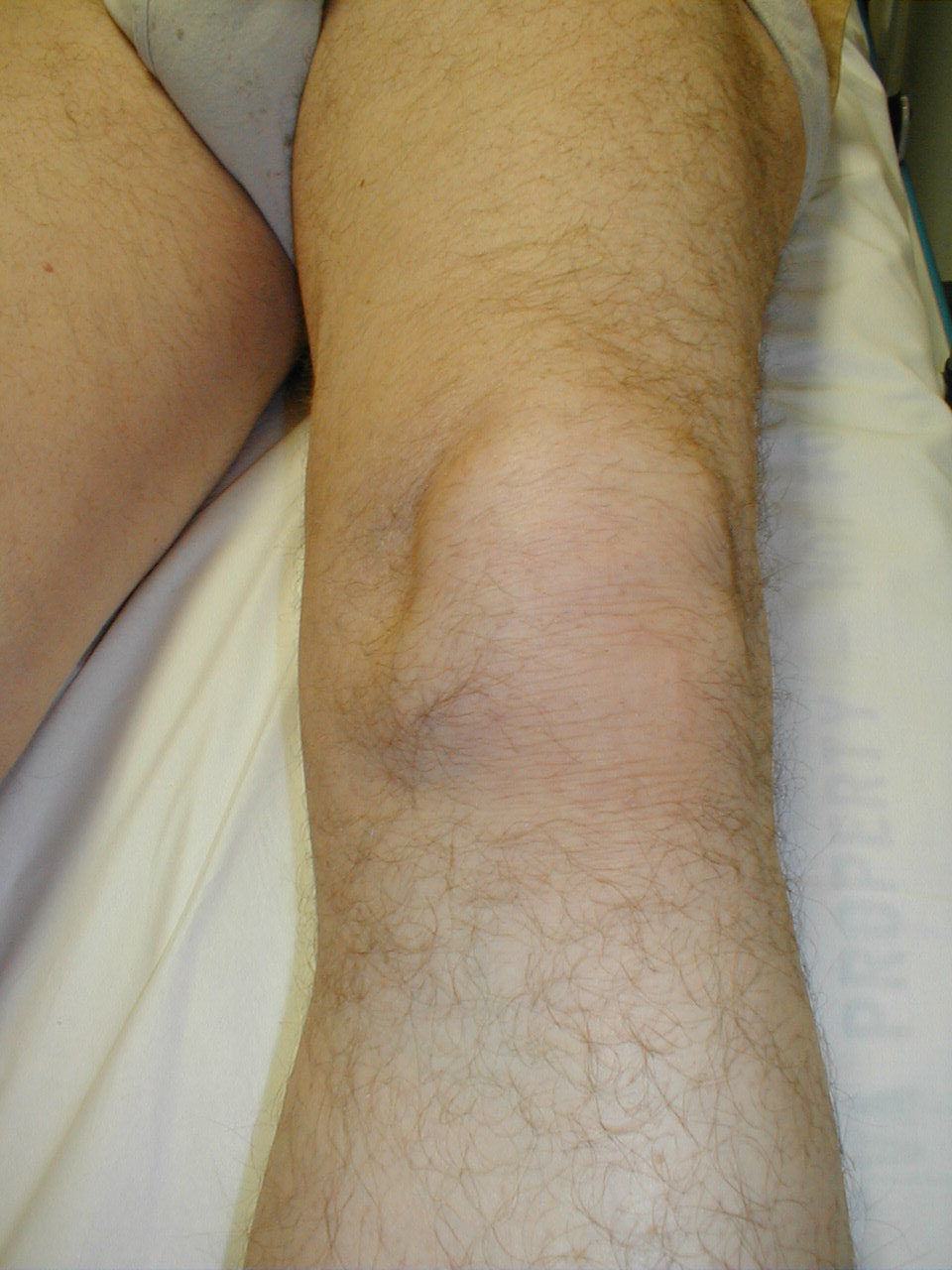
Normal knee
-
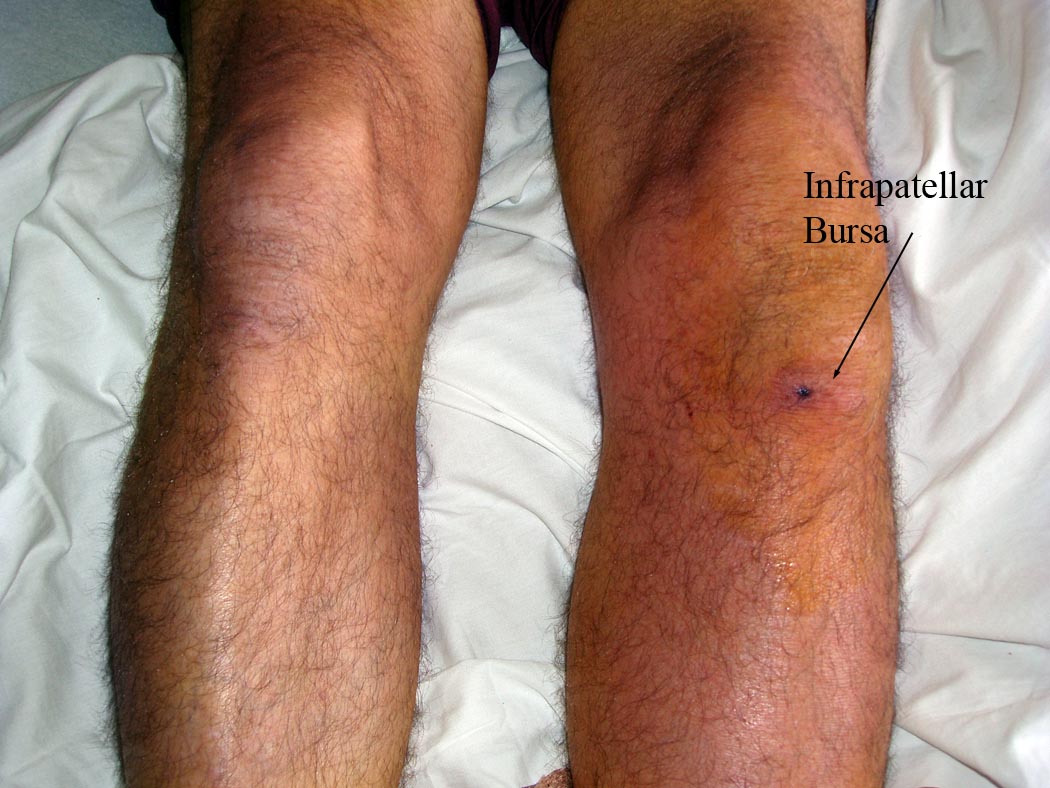
Infrapatellar Bursitis: Redness and swelling of right infrapatellar bursa
-
Infrapatellar Bursitis: Redness and swelling of left infrapatellar bursa.
Copyleft Images courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA
Differential diagnosis
Prepatellar bursitis must be differentiated from other causes of bursitis
| Type of Bursitis | Differential diagnosis |
|---|---|
| Subacromial bursitis[1] | |
| Olecranon bursitis[2][3] |
|
| Trochanteric bursitis[4][5] |
|
| Prepatellar bursitis[6][7][8] | |
| Retrocalcaneal bursitis[9][10] |
|
Treatment
Aseptic bursitis is usually managed conservatively, but complicated cases may be treated with oral NSAIDs or corticosteroid injections when infection has been ruled out. Surgical excision is seldom necessary.
Acute bursitis can develop into a chronic issue if the cause is not identified and addressed.
References
- ↑ Walker‐Bone, Karen, et al. "Prevalence and impact of musculoskeletal disorders of the upper limb in the general population.
- ↑ Stell IM (1996). "Septic and non-septic olecranon bursitis in the accident and emergency department--an approach to management". J Accid Emerg Med. 13 (5): 351–3. PMC 1342774. PMID 8894865.
- ↑ Lockman L (2010). "Treating nonseptic olecranon bursitis: a 3-step technique". Can Fam Physician. 56 (11): 1157. PMC 2980436. PMID 21075998.
- ↑ Brinks A, van Rijn RM, Bohnen AM, Slee GL, Verhaar JA, Koes BW; et al. (2007). "Effect of corticosteroid injection for trochanter pain syndrome: design of a randomised clinical trial in general practice". BMC Musculoskelet Disord. 8: 95. doi:10.1186/1471-2474-8-95. PMC 2045096. PMID 17880718.
- ↑ Karpinski MR, Piggott H (1985). "Greater trochanteric pain syndrome. A report of 15 cases". J Bone Joint Surg Br. 67 (5): 762–3. PMID 4055877.
- ↑ Aaron, Daniel L., et al. "Four common types of bursitis: diagnosis and management." Journal of the American Academy of Orthopaedic Surgeons 19.6 (2011): 359-367.
- ↑ Huang, Yu-Chih, and Wen-Lin Yeh. "Endoscopic treatment of prepatellar bursitis." International orthopaedics 35.3 (2011): 355-358.
- ↑ Meyerding, Henry W., and ROBERT E. VanDEMARK. "POSTERIOR HERNIA OF THE KNEE:(BAKER'S CYST, POPLITEAL CYST, SEMIMEMBRANOSUS BURSITIS, MEDIAL GASTROCNEMIUS BURSITIS AND POPLITEAL BURSITIS)." Journal of the American Medical Association 122.13 (1943): 858-861.
- ↑ Fauci, Anthony S., and Carol Langford. Harrison's rheumatology. McGraw Hill Professional, 2010.
- ↑ Lyman, Jeffrey, Paul S. Weinhold, and Louis C. Almekinders. "Strain behavior of the distal Achilles tendon implications for insertional Achilles tendinopathy." The American Journal of Sports Medicine 32.2 (2004): 457-461.
Template:Diseases of the musculoskeletal system and connective tissue