Follitropin beta
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Ammu Susheela, M.D. [2]
Disclaimer
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Follitropin beta is an endocrine metabolic agent that is FDA approved for the treatment of anovulatory infertile women,. Common adverse reactions include acne, injection site reactions, rash.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Indiacations
- Follitropin beta injection is indicated:
- In Women for:
- Induction of ovulation and pregnancy in anovulatory infertile women in whom the cause of infertility is functional and not due to primary ovarian failure.
- Prior to initiation of treatment with Follistim AQ:
- Women should have a complete gynecologic and endocrinologic evaluation.
- Primary ovarian failure should be excluded.
- The possibility of pregnancy should be excluded.
- Tubal patency should be demonstrated.
- The fertility status of the male partner should be evaluated.
- Development of multiple follicles in ovulatory women participating in an Assisted Reproductive Technology (ART) program
- Prior to initiation of treatment with Follistim AQ:
- Women should have a complete gynecologic and endocrinologic evaluation and diagnosis of cause of infertility.
- The possibility of pregnancy should be excluded.
- The fertility status of the male partner should be evaluated.
- In Men for:
- Induction of spermatogenesis in men with primary and secondary hypogonadotropic hypogonadism (HH) in whom the cause of infertility is not due to primary testicular failure.
Dosage
- Prior to initiation of treatment with Follistim AQ:
- Men should have a complete medical and endocrinologic evaluation.
- Hypogonadotropic hypogonadism should be confirmed and primary testicular failure should be excluded.
- Serum testosterone levels should be normalized with human chorionic gonadotropin (hCG) treatment.
- The fertility status of the female partner should be evaluated.
- Follistim AQ Single-Use Vial 75 international units per 0.5 mL - Follistim AQ Single-Use Vial 150 international units per 0.5 mL
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Follitropin beta in adult patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Follitropin beta in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
There is limited information regarding Follitropin beta FDA-Labeled Indications and Dosage (Pediatric) in the drug label.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Follitropin beta in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Follitropin beta in pediatric patients.
Contraindications
- Follistim AQ is contraindicated in women and men who exhibit:
- Prior hypersensitivity to recombinant hFSH products.
- High levels of FSH indicating primary gonadal failure.
- Presence of uncontrolled non-gonadal endocrinopathies (e.g., thyroid, adrenal, or pituitary disorders).
- Hypersensitivity reactions to streptomycin or neomycin. Follistim AQ may contain traces of these antibiotics.
- Tumor of the ovary, breast, uterus, testis, hypothalamus or pituitary gland.
- Follistim AQ is also contraindicated in women who exhibit:
- Pregnancy.
- Heavy or irregular vaginal bleeding of undetermined origin.
- Ovarian cysts or enlargement not due to polycystic ovary syndrome (PCOS).
Warnings
- Follistim AQ should be used only by physicians who are experienced in infertility treatment. Follistim AQ is a potent gonadotropic substance capable of causing Ovarian Hyperstimulation Syndrome (OHSS) with or without pulmonary or vascular complications and multiple births. Gonadotropin therapy requires the availability of appropriate monitoring facilities.
- Careful attention should be given to the diagnosis of infertility and in the selection of candidates for Follistim AQ therapy.
Abnormal Ovarian Enlargement
- In order to minimize the hazards associated with abnormal ovarian enlargement that may occur with Follistim AQ therapy, treatment should be individualized and the lowest effective dose should be used. Use of ultrasound monitoring of ovarian response and/or measurement of serum estradiol levels is important to minimize the risk of overstimulation.
- If the ovaries are abnormally enlarged on the last day of Follistim AQ therapy, hCG should not be administered in order to reduce the chances of developing Ovarian Hyperstimulation Syndrome (OHSS). Intercourse should be prohibited in patients with significant ovarian enlargement after ovulation because of the danger of hemoperitoneum resulting from ruptured ovarian cysts.
Ovarian Hyperstimulation Syndrome (OHSS)
- OHSS is a medical entity distinct from uncomplicated ovarian enlargement and may progress rapidly to become a serious medical condition. OHSS is characterized by a dramatic increase in vascular permeability, which can result in a rapid accumulation of fluid in the peritoneal cavity, thorax, and potentially, the pericardium. The early warning signs of OHSS developing are severe pelvic pain, nausea, vomiting, and weight gain. Abdominal pain, abdominal distension, gastrointestinal symptoms including nausea, vomiting and diarrhea, severe ovarian enlargement, weight gain, dyspnea, and oliguria have been reported with OHSS. Clinical evaluation may reveal hypovolemia, hemoconcentration, electrolyte imbalances, ascites, hemoperitoneum, pleural effusions, hydrothorax, acute pulmonary distress, and thromboembolic reactions. Transient liver function test abnormalities suggestive of hepatic dysfunction with or without morphologic changes on liver biopsy have also been reported in association with OHSS.
- OHSS occurs after gonadotropin treatment has been discontinued and it can develop rapidly, reaching its maximum about seven to ten days following treatment.
- Usually, OHSS resolves spontaneously with the onset of menses. If there is evidence that OHSS may be developing prior to hCG administration, the hCG must be withheld. Cases of OHSS are more common, more severe, and more protracted if pregnancy occurs; therefore, women should be assessed for the development of OHSS for at least two weeks after hCG administration.
- If serious OHSS occurs, treatment should be stopped and the patient should be hospitalized. Treatment is primarily symptomatic and overall should consist of bed rest, fluid and electrolyte management, and analgesics (if needed). Because the use of diuretics can accentuate the diminished intravascular volume, diuretics should be avoided except in the late phase of resolution as described below. The management of OHSS may be divided into three phases as follows:
- Acute Phase:
- Management should be directed at preventing hemoconcentration due to loss of intravascular volume to the third space and minimizing the risk of thromboembolic phenomena and kidney damage. Fluid intake and output, weight, hematocrit, serum and urinary electrolytes, urine specific gravity, BUN and creatinine, total proteins with albumin: globulin ratio, coagulation studies, electrocardiogram to monitor for hyperkalemia, and abdominal girth should be thoroughly assessed daily or more often based on the clinical need.
- Treatment, consisting of limited intravenous fluids, electrolytes, human serum albumin, is intended to normalize electrolytes while maintaining an acceptable but somewhat reduced intravascular volume. Full correction of the intravascular volume deficit may lead to an unacceptable increase in the amount of third space fluid accumulation
- Chronic Phase:
- Resolution Phase:
- As third space fluid returns to the intravascular compartment, a fall in hematocrit and increasing urinary output are observed in the absence of any increase in intake. Peripheral and/or pulmonary edema may result if the kidneys are unable to excrete third space fluid as rapidly as it is mobilized. Diuretics may be indicated during the resolution phase, if necessary, to combat pulmonary edema OHSS increases the risk of injury to the ovary. The ascitic, pleural, and pericardial fluid should not be removed unless there is the necessity to relieve symptoms such as pulmonary distress or cardiac tamponade.
- Pelvic examination may cause rupture of an ovarian cyst, which may result in hemoperitoneum, and should therefore be avoided. If bleeding occurs and requires surgical intervention, the clinical objective should be to control the bleeding and retain as much ovarian tissue as possible.
- During clinical trials with Follistim therapy, OHSS occurred in 7.6% of 105 women (OI) and 5.2% of 591 women (ART) treated with Follistim.
Pulmonary and Vascular Complications
- Serious pulmonary conditions (e.g., atelectasis, acute respiratory distress syndrome) have been reported in women treated with gonadotropins. In addition, thromboembolic reactions both in association with, and separate from, OHSS have been reported following gonadotropin therapy. Intravascular thrombosis, which may originate in venous or arterial vessels, can result in reduced blood flow to vital organs or the extremities. Women with generally recognized risk factors for thrombosis, such as a personal or family history, severe obesity, or thrombophilia, may have an increased risk of venous orarterial thromboembolic events, during or following treatment with gonadotropins. Sequelae of such reactions have included venous thrombophlebitis, pulmonary embolism, pulmonary infarction, cerebral vascular occlusion (stroke), and arterial occlusion resulting in loss of limb and rarely in myocardial infarction. In rare cases, pulmonary complications and/or thromboembolic reactions have resulted in death. In women with recognized risk factors, the benefits of ovulation induction or in vitro fertilization (IVF) treatment need to be weighed against the risks. It should be noted that pregnancy itself also carries an increased risk of thrombosis.
Ovarian Torsion
- Ovarian torsion has been reported after treatment with Follistim AQ and after intervention with other gonadotropins. This may be related to OHSS, pregnancy, previous abdominal surgery, past history of ovarian torsion, previous or current ovarian cyst and polycystic ovaries. Damage to the ovary due to reduced blood supply can be limited by early diagnosis and immediate detorsion.
Multi-fetal Gestation and Birth
- Multi-fetal gestation and births have been reported with all gonadotropin treatments including Follistim AQ treatment. The woman and her partner should be advised of the potential risk of multi-fetal gestation and births before starting treatment.
Congenital Anomalies
- The incidence of congenital malformations after ART may be slightly higher than after spontaneous conception. This slightly higher incidence is thought to be related to differences in parental characteristics (e.g., maternal age, sperm characteristics) and to the higher incidence of multi-fetal gestations after ART.
- There are no indications that the use of gonadotropins during ART is associated with an increased risk of congenital malformations.
Ectopic Pregnancy
- Since infertile women undergoing ART, and particularly IVF, often have tubal abnormalities the incidence of ectopic pregnancies might be increased. Early confirmation of an intrauterine pregnancy should be determined by hCG testing and transvaginal ultrasound.
Spontaneous Abortion
- The risk of spontaneous abortions (miscarriage) is increased with gonadotropin products. However, causality has not been established. The increased risk may be a factor of the underlying infertility.
Ovarian Neoplasms
- There have been infrequent reports of ovarian neoplasms, both benign and malignant, in women who have undergone multiple drug regimens for ovulation induction; however, a causal relationship has not been established.
Laboratory Tests
- For Women:
- In most instances, treatment with Follistim AQ will result only in follicular growth and maturation. In order to complete the final phase of follicular maturation and to induce ovulation, hCG must be given following the administration of Follistim AQ or when clinical assessment indicates that sufficient follicular maturation has occurred. The degree of follicular maturation and the timing of hCG administration can both be determined with the use of sonographic visualization of the ovaries and endometrial lining in conjunction with measurement of serum estradiol levels. The combination of transvaginal ultrasonography and measurement of serum estradiol levels is also useful for minimizing the risk of OHSS and multi-fetal gestations.
- The clinical confirmation of ovulation is obtained by the following direct or indirect indices of progesterone production as well as sonographic evidence of ovulation.
- Direct or indirect indices of progesterone production are:
- Urinary or serum luteinizing hormone (LH) rise
- A rise in basal body temperature
- Increase in serum progesterone
- Menstruation following the shift in basal body temperature
- The following provide sonographic evidence of ovulation:
- Collapsed follicle
- Fluid in the cul-de-sac
- Features consistent with corpus luteum formation
- Sonographic evaluation of the early pregnancy is also important to rule out ectopic pregnancy.
- For Men:
- Clinical monitoring for spermatogenesis utilizes the following indirect or direct measures:
- Serum testosterone level
- Semen analysis.
Adverse Reactions
Clinical Trials Experience
- The following serious adverse reactions are discussed elsewhere in the labeling:
- Ovarian Hyperstimulation Syndrome
- Atelectasis
- Thromboembolism
- Ovarian Torsion
- Multi-fetal Gestation and Birth
- Congenital Anomalies
- Ectopic Pregnancy
- Spontaneous Abortion
Clinical Study Experience
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
Ovulation Induction
- In a single cycle, multi-center, assessor-blind, parallel group, comparative study, a total of 172 chronic anovulatory women who had failed to ovulate and/or conceive with clomiphene citrate therapy, were randomized and treated with Follistim (105) or a urofollitropin comparator. Adverse reactions with an incidence of greater than 2% in either treatment group are listed in Table 1.
Postmarketing Experience
- The following adverse reactions have been identified during post approval use of Follistim and/or Follistim AQ. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Vascular disorders:
Drug Interactions
No drug-drug interaction studies have been performed.
Use in Specific Populations
Pregnancy
Pregnancy Category (FDA): X
Pregnancy Category X: Follistim AQ should not be used during pregnancy
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Follitropin beta in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Follitropin beta during labor and delivery.
Nursing Mothers
- It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in the nursing infant from Follistim AQ, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
Geriatic Use
Clinical studies of Follistim did not include subjects aged 65 and over.
Gender
There is no FDA guidance on the use of Follitropin beta with respect to specific gender populations.
Race
There is no FDA guidance on the use of Follitropin beta with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Follitropin beta in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Follitropin beta in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Follitropin beta in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Follitropin beta in patients who are immunocompromised.
Administration and Monitoring
Administration
Monitoring
- Prior to beginning therapy with Follistim AQ, inform women and men about the time commitment and monitoring procedures necessary to undergo treatment.
- Use of ultrasound monitoring of ovarian response and/or measurement of serum estradiol levels is important to minimize the risk of overstimulation.
- Fluid intake and output, weight, hematocrit, serum and urinary electrolytes, urine specific gravity, BUN and creatinine, total proteins with albumin: globulin ratio, coagulation studies, electrocardiogram to monitor for hyperkalemia, and abdominal girth should be thoroughly assessed daily or more often based on the clinical need.
- Clinical monitoring for spermatogenesis utilizes the following indirect or direct measures:
- Serum testosterone level
- Semen analysis
IV Compatibility
There is limited information regarding the compatibility of Follitropin beta and IV administrations.
Overdosage
- Aside from the possibility of Ovarian Hyperstimulation Syndrome and multiple gestations , there is no additional information concerning the consequences of acute overdosage with Follistim AQ.
Pharmacology
There is limited information regarding Follitropin beta Pharmacology in the drug label.
Mechanism of Action
- Women:
- Follicle-stimulating hormone (FSH), the active component in Follistim AQ, is required for normal follicular growth, maturation, and gonadal steroid production.
- In women, the level of FSH is critical for the onset and duration of follicular development, and consequently for the timing and number of follicles reaching maturity. Follistim AQ stimulates ovarian follicular growth in women who do not have primary ovarian failure. In order to effect the final phase of follicle maturation, resumption of meiosis and rupture of the follicle in the absence of an endogenous LH surge, human chorionic gonadotropin (hCG) must be given following treatment with Follistim AQ when patient monitoring indicates appropriate follicular development parameters have been reached.
- Men:
- Follistim when administered with hCG stimulates spermatogenesis in men with hypogonadotropic hypogonadism. FSH, the active component of Follistim, is the pituitary hormone responsible for spermatogenesis.
Structure
There is limited information regarding Follitropin beta Structure in the drug label.
Pharmacodynamics
There is limited information regarding Follitropin beta Pharmacodynamics in the drug label.
Pharmacokinetics
- Exposures of follitropin beta from Follistim AQ and Follistim are expected to be equivalent. The following information is based on studies conducted with Follistim.
Absorption
- Women:
- The bioavailability of Follistim following subcutaneous and intramuscular administration was investigated in healthy, pituitary-suppressed, women given a single 300 international units dose. In these women, the area under the curve (AUC), expressed as the mean ± SD, was equivalent between the subcutaneous (455.6 ± 141.4 IU*h/L) and intramuscular (445.7 ± 135.7 IU*h/L) routes of administration. However, equivalence could not be established with respect to the peak serum FSH levels (Cmax). The Cmax achieved after subcutaneous administration and intramuscular administration was 5.41 ± 0.72 international units/L and 6.86 ± 2.90 international units/L, respectively. After subcutaneous or intramuscular injection the apparent dose absorbed was 77.8% and 76.4%, respectively.
- The pharmacokinetics and pharmacodynamics of a single, intramuscular dose (300 international units) of Follistim were also investigated in a group (n=8) of gonadotropin-deficient, but otherwise healthy women. In these women, FSH (mean ± SD) AUC was 339 ± 105 international units*h/L, Cmax was 4.3 ± 1.7 international units/L. Cmax occurred at approximately 27 ± 5.4 hours after intramuscular administration.
- A multiple dose, dose proportionality, pharmacokinetic study of Follistim was completed in healthy, pituitary-suppressed, women given subcutaneous doses of 75, 150, or 225 international units for 7 days. Steady-state blood concentrations of FSH were reached with all doses after 5 days of treatment based on the trough concentrations of FSH just prior to dosing (Ctrough). Peak blood concentrations with the 75, 150, and 225 international units dose were 4.30 ± 0.60 international units/L, 8.51 ± 1.16 international units/L and 13.92 ± 1.81 international units/L, respectively.
- A multiple dose, dose proportionality, pharmacokinetic study of Follistim was completed in healthy, pituitary-suppressed, women given intramuscular doses of 75, 150, or 225 international units for 7 days. Steady-state blood concentrations of FSH were reached with all doses after 4 days of treatment based on the minimum concentrations of FSH just prior to dosing (Cmin). Peak blood concentrations with the 75, 150, and 225 international units dose were 4.65 ± 1.49 international units/L, 9.46 ± 2.57 international units/L and 11.30 ± 1.77 international units/L, respectively.
- Men:
- Serum levels of FSH were measured in a clinical study that compared the effects of two different dosing schedules of Follistim (150 international units three times a week or 225 international units twice a week) administered by subcutaneous injection concurrently with chorionic gonadotropin for injection for induction of spermatogenesis in hypogonadotropic hypogonadal men. Administration of Follistim was started at Week 17. Mean serum trough concentrations of FSH remained fairly constant over the treatment period. At the end of treatment (Week 64), the mean serum trough concentrations of FSH were 2.09 international units/L in the 150 international units group and 3.22 international units/L in the 225 international units group. Serum trough concentrations of FSH measured prior to the first Follistim injection on the Mondays of active treatment period (Weeks 17 to 64) and one week after the end of treatment period are presented in Figure 1.

This image is provided by the National Library of Medicine. - FIGURE 1: Mean (SD) Serum Trough Concentrations of FSH in Men Following Subcutaneous Administration of Follistim Using Two Different Dosing Schedules (150 International Units Three Times a Week or 225 International Units Twice a Week)
- Distribution:
- The volume of distribution of Follistim in healthy, pituitary-suppressed, women following intravenous administration of a 300 international units dose was approximately 8 L.
- Metabolism:
- The recombinant FSH in Follistim AQ is biochemically very similar to urinary FSH and it is therefore anticipated that it is metabolized in the same manner.
- Elimination:
- The elimination half-life (t1/2) following a single intramuscular dose (300 international units) of Follistim in women was 43.9 ± 14.1 hours (mean ± SD). The elimination half-life following a 7-day intramuscular treatment of women with 75, 150, or 225 international units was 26.9 ± 7.8 hours (mean ± SD), 30.1 ± 6.2 and 28.9 ± 6.5, respectively.
- Use in Specific Populations:
- Body weight: The effect of body weight on the pharmacokinetics of Follistim was evaluated in a group of European and Japanese women who were significantly different in terms of body weight. The European women had a body weight of (mean ± SD) 67.4 ± 13.5 kg and the Japanese subjects were 46.8 ± 11.6 kg. Following a single intramuscular dose of 300 international units of Follistim, the AUC was significantly smaller in European women (339 ± 105 international units*h/L) than in Japanese women (544 ± 201 international units*h/L). However, clearance per kg of body weight was essentially the same for the respective groups (0.014 and 0.013 L/hr/kg).
- Geriatric Use: The pharmacokinetics of Follistim has not been studied in geriatric subjects.
- Pediatric Use: The pharmacokinetics of Follistim has not been studied in pediatric subjects.
- Renal Impairment: The effect of renal impairment on the pharmacokinetics of Follistim has not been studied.
- Hepatic Impairment: The effect of hepatic impairment on the pharmacokinetics of Follistim has not been studied.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
- Long-term toxicity studies in animals have not been performed with Follistim to evaluate the carcinogenic potential of the drug. Follistim was not mutagenic in the Ames test using S. typhimurium and E. coli tester strains and did not produce chromosomal aberrations in an in vitro assay using human lymphocytes.
Clinical Studies
Ovulation Induction
- The efficacy of Follitropin beta for Ovulation Induction was evaluated in a randomized, assessor-blind, parallel-group comparative, multicenter safety and efficacy study of 172 chronic anovulatory women (105 subjects on Follitropin beta) who had previously failed to ovulate and/or conceive during clomiphene citrate treatment. The study results for ovulation rates are summarized in Table 4 and those for pregnancy rates are summarized in Table 5.
How Supplied
- Follitropin beta AQ (follitropin beta injection) is supplied as a sterile aqueous solution in a 2-mL vial to deliver 0.5 mL of the drug in the following concentrations and packaging:
- Follitropin beta AQ Single-Use Vial 75 international units per 0.5 mL
This image is provided by the National Library of Medicine.
Storage
- Store refrigerated, 2-8°C (36-46°F) until dispensed. Upon dispensing, the product may be stored by the patient at 2-8°C (36-46°F) until the expiration date, or at or below 25°C (77°F) for 3 months or until expiration date, whichever occurs first. Protect from light, keep container in carton. Do not freeze.
Images
Drug Images
{{#ask: Page Name::Follitropin beta |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel


{{#ask: Label Page::Follitropin beta |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
- Read the Patient Information that comes with follitropin beta before you start using it and each time you get a refill. There may be new information. This information does not take the place of talking with your healthcare provider about your medical condition or treatment.
- What is Follitropin beta AQ?
- Follitropin beta AQ is a prescription medicine that contains follicle-stimulating hormone (FSH).
- Follitropin beta AQ is used:
- In women:
- To help healthy ovaries to develop (mature) and release eggs
- As part of an Assisted Reproductive Technology (ART) program to help the ovaries produce more mature eggs
- In men:
- To help bring about the production and development of sperm
- Who should not take Follitropin beta AQ?
- Do not take follitropin beta AQ if you are a Woman or Man who:
- Is allergic to recombinant human FSH products
- Has a high level of FSH in your blood indicating that your ovaries (women only) or Testes (men only) may be permanently damaged and do not work at all.
- Has uncontrolled thyroid, pituitary, or adrenal gland problems
- Is allergic to streptomycin or neomycin (types of antibiotics)
- Has a tumor of the hypothalamus, pituitary gland, breast, uterus (women only), ovary (women only), or testis (men only)
- Do not take follitropin beta AQ if you are a Woman who:
- Is pregnant or think you may be pregnant
- Has heavy or irregular vaginal bleeding and the cause is not known
- Has ovarian cysts or enlarged ovaries, not due to polycystic ovary syndrome (PCOS)
- Talk to your healthcare provider before taking this medicine if you have any of the conditions listed above.
- What should I tell my healthcare provider before taking follitropin beta AQ?
- Before you take follitropin beta AQ, tell your healthcare provider if you:
- Have an increased risk of blood clots (thrombosis)
- Have ever had a blood clot (thrombosis), or anyone in your immediate family has ever had a blood clot (thrombosis)
- Had stomach (abdominal) surgery
- Had twisting of your ovary (ovarian torsion)
- Had or have a cyst in your ovary
- Have polycystic ovary disease
- Have any other medical conditions
- Are breastfeeding or plan to breastfeed. It is not known if follitropin beta AQ passes into your breast milk. You and your healthcare provider should decide if you will take follitropin beta AQ or breastfeed. You should not do both.
- Tell your healthcare provider about all the medicines you take, including prescription and non-prescription medicines, vitamins, and herbal supplements.
- Know the medicines you take. Keep a list of them and show your healthcare provider and pharmacist when you get a new medicine.
- How should I use follitropin beta AQ?
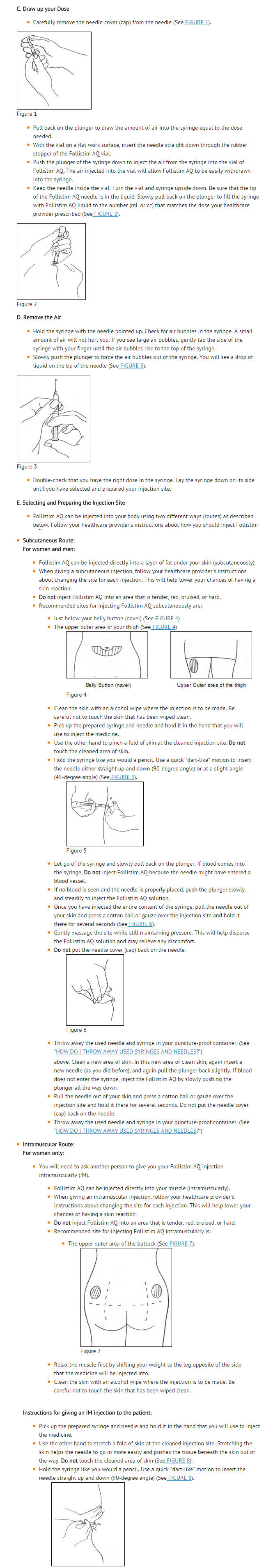
- Be sure that you read, understand, and follow the "Patient Instructions for Use" that come with follitropin beta AQ.
- Use follitropin beta AQ exactly as your healthcare provider tells you to.
- Your healthcare provider will tell you how much follitropin beta AQ to use, how to inject it, and how often it should be injected.
- Do not inject follitropin beta AQ at home until your healthcare provider has taught you the right way.
- Do not mix follitropin beta AQ with any other medicines in the same vial or in the same syringe.
- Do not change your dose of follitropin beta AQ unless your healthcare provider tells you to.
- Call your healthcare provider immediately if you use too much follitropin beta AQ.
- If you miss or forget to take a dose, do not double your next dose. Ask your healthcare provider for instructions.
- Your healthcare provider will do blood and urine hormone tests while you are taking follitropin beta AQ. Make sure you follow-up with your healthcare provider to have your blood and urine tested when told to do so.
- Women:
- Your healthcare provider may do ultrasound scans of your ovaries. Make sure you follow-up with your healthcare provider to have your ultrasound scans.
- Men:
- Your healthcare provider may test your semen while you are taking follitropin beta AQ.
- Make sure you follow-up with your healthcare provider to give a semen sample for testing.
- What are the possible side effects of follitropin beta AQ?
- Follitropin beta AQ may cause serious side effects.
- Serious side effects in women include:
Ovarian Enlargement
- Ovarian hyperstimulation syndrome (OHSS). OHSS is a serious medical problem that can happen when the ovaries are over stimulated. In rare cases it has caused death.
- OHSS causes fluid to build up suddenly in your stomach and chest areas and can cause blood clots to form. Call you healthcare provider right away if you have:
- Decreased urine output
- Trouble breathing
- Lung problems. Follitropin beta AQ can cause you to have fluid in your lungs (atelectasis) and trouble breathing (acute respiratory distress syndrome).
- Blood clots. Follitropin beta AQ may increase your chance of having blood clots in your blood vessels. Blood clots can cause:
- Blood vessel problems (thrombophlebitis)
- Stroke
- Loss of your arm or leg
- Blood clot in your lungs (pulmonary embolus)
- Heart attack
- Ovarian torsion. Follistim AQ may increase the chance of twisting of the ovaries in women with certain conditions such as OHSS, pregnancy and previous abdominal surgery.
- Twisting of the ovary could cause the blood flow to the ovary to be cut off.
- Pregnancy and birth of multiple babies. Having a pregnancy with more than one baby at a time increases the health risk for you and your babies. Discuss your chances of multiple births with your healthcare provider.
- Birth defects. A woman's age, certain sperm problems, genetic background of both parents and a pregnancy with multiple babies can increase the chance that your baby might have birth defects.
- Ectopic pregnancy (pregnancy outside of the womb). The chance of a pregnancy outside of the womb is increased in women with damaged fallopian tubes.
- Miscarriage. The chance of loss of an early pregnancy may be increased in women who have difficulty with becoming pregnant at all.
- The most common side effects of Follistim AQ include:
- In women:
- Cyst in the ovary.
- Stomach pain.
- In men:
- Headache.
- Pain at the injection site.
- Bruising, swelling or redness at the injection site.
- Breast enlargement.
- Acne.
- These are not all the possible side effects of Follistim AQ. For more information, ask your healthcare provider or pharmacist.
- Call your healthcare provider immediately if you get worsening or strong abdominal pain. Also, call your healthcare provider immediately if this happens some days after the last injection has been given.
- Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
- Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
- How should I store Follistim AQ?
- Store Follistim AQ in the refrigerator between 2° - 8°C (36° - 46°F) until the expiration date.
- Follistim AQ can be stored at or below 25°C (77°F) for 3 months or until the expiration date, whichever comes first.
- Keep Follistim AQ away from light.
- Do not freeze.
- Keep Follistim AQ and all medicines out of the reach of children.
- General information about Follistim AQ
- Medicines are sometimes prescribed for purposes other than those listed in the Patient Information leaflet. Do not use Follistim AQ for a condition for which it was not prescribed. Do not give Follistim AQ to other people, even if they have the same condition that you have. It may harm them.
- This Patient Information leaflet summarizes the most important information about Follistim AQ. If you would like more information, talk with your healthcare provider. * You can ask your pharmacist or healthcare provider for more information about Follistim AQ that is written for healthcare professionals.
- For more information, go to www.follistim.com or call 1-866-836-5633.
- What are the ingredients in Follistim AQ?
- Active ingredient: follitropin beta
- Inactive ingredients: sucrose, sodium citrate, L-methionine, polysorbate 20, water for injection, hydrochloric acid, and/or sodium hydroxide.
Precautions with Alcohol
Alcohol-Follitropin beta interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
- FOLLISTIM AQ®[1]
Look-Alike Drug Names
There is limited information regarding Follitropin beta Look-Alike Drug Names in the drug label.
Drug Shortage Status
Price
References
The contents of this FDA label are provided by the National Library of Medicine.

