Hereditary elliptocytosis
| Hereditary elliptocytosis | |
 | |
|---|---|
| Blood smear showing elliptocytes | |
| ICD-10 | D58.1 |
| ICD-9 | 282.1 |
| DiseasesDB | 4172 |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Please Take Over This Page and Apply to be Editor-In-Chief for this topic: There can be one or more than one Editor-In-Chief. You may also apply to be an Associate Editor-In-Chief of one of the subtopics below. Please mail us [2] to indicate your interest in serving either as an Editor-In-Chief of the entire topic or as an Associate Editor-In-Chief for a subtopic. Please be sure to attach your CV and or biographical sketch.
Overview
Hereditary elliptocytosis is a blood disorder in which a large proportion of the sufferer's erythrocytes (i.e. red blood cells) are elliptical rather than bi-concave disc-shaped. It is also known as ovalocytosis. The disorder predisposes to haemolytic anaemia.
Historical perspective
Elliptocytosis was first described in 1904, and was first recognised as a hereditary condition in 1932. More recently it has become clear that there is much genetic heterogeneity amongst sufferers, and the severity of the condition is highly variable.
Aetiology
The incidence of hereditary elliptocytosis is hard to determine, as many sufferers of the milder forms of the disorder are asymptomatic and their condition never comes to medical attention. Around 90% of those with this disorder are thought to fall into the asymptomatic population. It is estimated that its incidence is between 3 and 5 per 10,000 in the USA, and that those of African and Mediterranean descent are of higher risk. Some subtypes of hereditary elliptocytosis are significantly more prevalent in regions where malaria is endemic. For example, in equatorial Africa its incidence approaches 160 per 10,000, and in Malayan natives its incidence is over 15% (1500-2000 per 10,000). Being an almost wholly autosomal dominant disorder, there is no predilection towards either sex in hereditary elliptocytosis. The most important exception to this rule of autosomal dominant inheritance is for a subtype of hereditary elliptocytosis called hereditary pyropoikilocytosis (HPP). This condition is autosomal recessive.
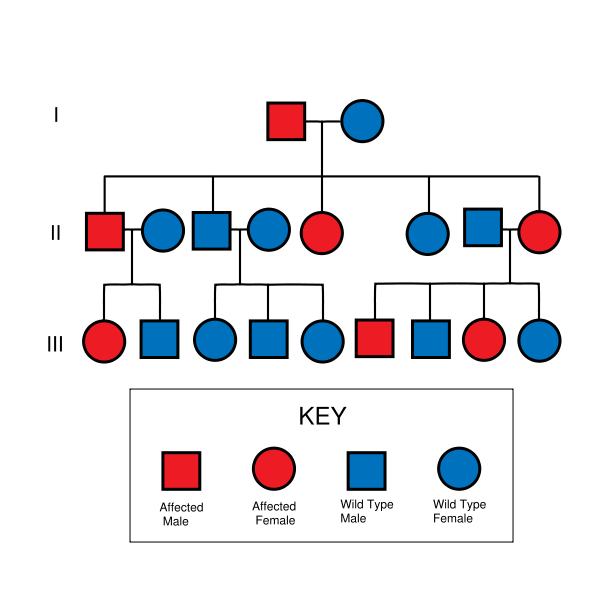
There are a number of different subtypes of hereditary elliptocytosis. A clinically significant haemolytic anaemia occurs only in 5-10% of sufferers, with a strong bias towards those with more severe subtypes of the disorder. The following categorisation of the disorder demonstrates its heterogeneity (in approximate order from least severe to most severe)[1]:
- Common hereditary elliptocytosis
- With asymptomatic carrier status - the individual has no symptoms of disease and diagnosis is only able to be made on blood film
- With mild disease - the individual has no symptoms and a mild and compensated haemolytic anaemia
- With sporadic haemolysis - the individual has a predilection towards haemolysis in the presence of particular comorbidities, including infections, and [[Cyanocobalamin|vitamin BTemplate:Ssub]] deficiency
- With neonatal poikilocytosis - during the first year of life only the individual has a symptomatic haemolytic anaemia with poikilocytosis
- With chronic haemolysis - the individual has a moderate to severe symptomatic haemolytic anaemia (this subtype has variable penetrance in some pedigrees)
- With homozygosity or compound heterozygosity - depending on the exact mutations involved, the individual may lie anywhere in the spectrum between having a mild haemolytic anaemia and having a life-threatening haemolytic anaemia with symptoms mimicking those of HPP (see below)
- With pyropoikilocytosis (HPP) - the individual is typically of African descent and has a life-threateningly severe haemolytic anaemia with micropoikilocytosis (small and misshapen erythrocytes) that is compounded by a marked instability of erythrocytes in even mildly elevated temperatures (pyropoikilocytosis is often found in burns victims and is the term is commonly used in reference to such people)
- Spherocytic elliptocytosis (also called hereditary haemolytic ovalocytosis) - the individual is typically of European descent and both elliptocytes and spherocytes are simultaneously present in their blood
- South-east Asian ovalocytosis (SAO) (also called stomatocytic elliptocytosis) - the individual is of South-East Asian descent (typically Malaysian, Indonesian, Melanesian, New Guinean or Filipino, has a mild haemolytic anaemia, and has resistance to malaria
Pathophysiology
Common hereditary elliptocytosis
A number of genes have been linked to common hereditary elliptocytosis. These mutations have a common end result; they destabilise the cytoskeletal scaffold of cells. This stability is especially important in erythrocytes as they are constantly under shear forces which deform them. As disc-shaped erythrocytes pass through capillaries, which can be 2-3 micrometres wide, they are forced to assume an elliptical shape in order to fit through. Normally, this deformation lasts only as long as a cell is present in a capillary, but in hereditary elliptocytosis the instability of the cytoskeleton means that erythrocytes which are deformed as a result of passing through a capillary are forever rendered elliptical. These elliptocytotic cells are taken up by the spleen and removed from circulation when they are younger than they would normally be, meaning that the erythrocytes of people with hereditary elliptocytosis have a shorter than average life-span (a normal person's erythrocytes average 120 days or more).

The most common genetic defects (present in two-thirds of all cases of hereditary elliptocytosis) are in genes for the polypeptides α-spectrin or β-spectrin. These two polypeptides combine with one another in vivo to form an αβ heterodimer. These αβ heterodimers then combine together to form spectrin tetramers. These spectrin tetramers are among the basic structural subunits of the cytoskeleton of all cells in the body. Although there is much interindividual variability, it is generally true that 'α'-spectrin mutations result in an inability of α-spectrin to interact properly with β-spectrin to form a heterodimer. In contrast, it is generally true that 'β'-spectrin mutations lead to αβ heterodimers being incapable of combining to form spectrin tetramers[2]. The end result is a weakness in the cytoskeleton of the cell. Individuals with a single mutation in one of the spectrin genes are usually asymptomatic, but those who are homozygotes or are compound heterozygotes (i.e. they are heterozygous for two different elliptocytosis-causing mutations) have sufficient cell membrane instability to have a clinically significant haemolytic anaemia.
Less common than spectrin mutations are protein 4.1 mutations. Spectrin tetramers must bind to actin in order to create a proper cytoskeleton scaffold, and protein 4.1 is an important protein involved in the stabilisation of the link between spectrin and actin. Similarly to the spectrin mutations, protein 4.1 mutations cause a mild haemolytic anaemia in the heterozygous state, and a severe haemolytic disease in the homozygous state. Erythrocytes of individuals who are homozygous for this mutation type show not only a destabilised cytoskeleton but also disorder of molecules within the cell membrane itself, which is evidence that protein 4.1 plays some part in maintaining the normal organisation of the cell membrane.
The third group of mutations which lead to elliptocytosis are those which cause glycophorin C deficiencies. There are three phenotypes caused by abnormal glycophorin C, these are named Gerbich, Yus and Leach (see glycophorin C for more information). Only the rarest of the three, the Leach phenotype, causes elliptocytosis. Glycophorin C has the function of holding protein 4.1 to the cell membrane. It is thought that elliptocytosis in glycophorin C deficiency is actually the consequence of a protein 4.1 deficit, as glycophorin C deficient individuals also have reduced intracellular protein 4.1 (probably due to the reduced number of binding sites for protein 4.1 in the absence of glycoprotein C). Plasmodium falciparum (the pathogen responsible for malaria) has a surface protein called erythrocyte-binding antigen 140, which is now known to bind to glycophorin C. This suggests that plasmodium falciparum is less able to bind to the erythrocytes of those with the Leach phenotype, suggesting these individuals have a relative resistance to malaria. Clinically, this has not yet been shown.
Multiplication of mutations tends to infer more serious disease. For instance, in HPP, the most common genotype results from receiving an α-spectrin mutation from one parent (i.e. one parent has hereditary elliptocytosis) and the other parent passes on an as-yet-undefined defect which causes the affected individual's cells to preferentially produce the defective α-spectrin rather than normal α-spectrin.
Spherocytic elliptocytosis
The molecular defect associated with spherocytic elliptocytosis has yet to be elucidated. As with common hereditary elliptocytosis, multiple gene defects are probably capable of causing this phenotype. Mutations in the genes coding for β-spectrin, glycophorin C and protein 4.2 have all been implicated in spherocytic elliptocytosis. Except for protein 4.2 linked disease (which is autosomal recessive), spherocytic elliptocytosis is an autosomal dominant condition.
Southeast Asian ovalocytosis
The primary defect in SAO differs significantly from other forms of elliptocytosis in that it is a defect in the gene coding for a protein that is not directly involved in the cytoskeleton scaffolding of the cell. Rather, the defect lies in a protein known as the band 3 protein, which lies in the cell membrane itself. The band 3 protein normally binds to another membrane-bound protein called ankyrin, but in SAO this bond is stronger than normal. Other abnormalities include tighter tethering of the band 3 protein to the cell membrane, increased tyrosine phosphorylation of the band 3 protein, reduced sulfate anion transport through the cell membrane, and more rapid ATP consumption. These (and probably other) consequences of the SAO mutations lead to the following erythrocyte abnormalities[3]:
- a greater robustness of cells to a variety of external forces, including:
- a reduction in cellular sensitivity to osmotic pressures
- a reduction in fragility related to temperature change
- greater general rigidity of the cell membrane
- loss of sensitivity to substances which cause spiculation of cells
- reduced anion exchange
- partial intracellular depletion of ATP
- a reduction in expression of multiple antigens
These changes are thought to give rise to the scientifically and clinically interesting phenomenon that those with SAO exhibit - a marked in vivo resistance to infection by the causative pathogen of malaria, Plasmodium falciparum. Unlike those with the Leach phenotype of common hereditary elliptocytosis (see above), there is a clinically significant reduction in both disease severity and prevalence of malaria in those with SAO. Because of this, the 35% incidence rate of SAO along the north coast of Madang Province in Papua New Guinea, where malaria in endemic, is a good example of natural selection[4].
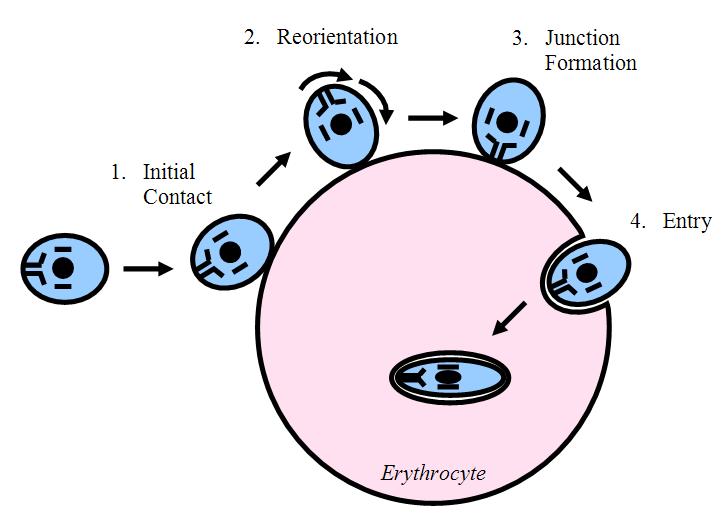
The reasons behind the resistance to malaria become clear when given an explanation the way in which Plasmodium falciparum invades its host. This parasite is an obligate intracellular parasite, which must enter the cells of the host it is invading. The band 3 proteins aggregate on the cell membrane at the site of entry, forming a circular orifice that the parasite squeezes through. These band 3 proteins act as receptors for the parasite. Normally a process much like endocytosis occurs, and the parasite is able to isolate itself from the intracellular proteins that are toxic to it while still being inside an erythrocyte (see figure 2). The increased rigidity of the erythrocyte membrane in SAO is thought to reduce the capacity of the band 3 proteins to cluster together, thereby making it more difficult for the malaria parasite to properly attaching to and enter the cell. The reduced free ATP within the cell has been postulated as a further mechanism behind which SAO creates a hostile environment for Plasmodium falciparum.
Treatment
The vast majority of those with hereditary elliptocytosis require no treatment whatsoever. They have a mildly increased risk of developing gallstones, which is treated surgically with a cholecystectomy if pain becomes problematic.
Folate helps to reduce the extent of haemolysis in those with significant haemolysis due to hereditary elliptocytosis.
Because the spleen is the bodily organ which breaks down old and worn-out blood cells, those individuals with more severe forms of hereditary elliptocytosis can have a splenomegaly which causes a worsening of the signs and symptoms of their anaemia. These can include:
- Vague, poorly localised abdominal pain
- Fatigue and dyspnoea
- Growth failure
- Leg ulcers
- Gallstones.
Removal of the spleen (splenectomy) is effective in reducing the severity of these complications, but is associated with an increased risk of overwhelming bacterial septicaemia, and is only performed on those with significant complications. Because many neonates with severe elliptocytosis progress to have only a mild disease, and because this age group is particularly susceptible to pneumococcal infections, a splenectomy is only performed on those under 5 years old when it is absolutely necessary.
Because chronic haemolysis increases an individual's risk of gallstones, people with elliptocytosis have an increased risk of suffering from gallstones. This risk is relative to the severity of the disease, and those with symptomatic elliptocytosis should have regular abdominal ultrasounds to monitor the progression of their gall bladder disease.
Prognosis
Those with hereditary elliptocytosis have a good prognosis, only those with very severe disease have a shortened life expectancy.
References
- ↑ Coetzer T, Lawler J, Prchal JT and Palek J (1987). "Molecular Determinants of Clinical Expression of Hereditary Elliptocytosis and Pyropoikilocytosis" (PDF). Blood. 70 (3): 491–588. Retrieved 2006-10-31. Unknown parameter
|month=ignored (help) - ↑ McMullin MF (1999). "The molecular basis of disorders of the red cell membrane" (PDF). Journal of Clinical Pathology. 52 (4): 245–248. Retrieved 2006-11-02. Unknown parameter
|month=ignored (help) - ↑ Liu S, Palek J, Yi SJ, Nichols PE, Derick LH, Chiou S, Amato D, Corbett JD, Cho MR and Golan DE (1 July 1995). "Molecular Basis of Altered Red Blood Cell Membrane Properties in Southeast Asian Ovalocytosis: Role of the Mutant Band 3 Protein in Band 3 Oligomerization and Retention by the Membrane Skeleton" (PDF). Blood. 86 (1): 349–358. Retrieved 2006-10-31. Unknown parameter
|month=ignored (help) - ↑ Mgone CS, Koki G, Paniu MM, Kono J, Bhatia KK, Genton B, Alexander ND and Alpers MP (1996). "Occurrence of the erythrocyte band 3 (AE1) gene deletion in relation to malaria endemicity in Papua New Guinea". Transactions of the Royal Society of Tropical Medicine and Hygiene. 90 (3): 228–231. Retrieved 2006-10-31. Unknown parameter
|month=ignored (help)