Sexcord/ stromal ovarian tumors MRI
|
Sexcord/ stromal ovarian tumors Microchapters |
|
Differentiating Sexcord/ Stromal Ovarian Tumors from other Diseases |
|---|
|
Diagnosis |
|
Treatment |
|
Case Studies |
|
Sexcord/ stromal ovarian tumors MRI On the Web |
|
American Roentgen Ray Society Images of Sexcord/ stromal ovarian tumors MRI |
|
Risk calculators and risk factors for Sexcord/ stromal ovarian tumors MRI |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: ; Maneesha Nandimandalam, M.B.B.S.[2]
Overview
There are no MRI findings associated with [disease name].
OR
[Location] MRI may be helpful in the diagnosis of [disease name]. Findings on MRI suggestive of/diagnostic of [disease name] include [finding 1], [finding 2], and [finding 3].
OR
There are no MRI findings associated with [disease name]. However, a MRI may be helpful in the diagnosis of complications of [disease name], which include [complication 1], [complication 2], and [complication 3].
MRI
- MRI may be helpful in the diagnosis of Sexcord/ stromal ovarian tumors[1][2][3][4][5][6][7][8][9][10][11]
- Findings on MRI differ according to the subtypes of tumors
Granulosa cell tumors:
- They show heterogeneous signal intensity on both T1WI and T2WI and high signal intensity on DWI images
- They appear as solid masses, tumors with hemorrhagic or fibrotic changes, multilocular cystic lesions or completely cystic tumors
- Heterogeneity within a solid tumor is caused by intra-tumoral bleeding, infarct or fibrous degeneration

Fibroma, Fibrothecoma, and Thecoma:
- As the name indicates fibromas have abundant collagen and fibrous contents, these tumors show relatively diagnostic imaging findings
- They appear as hypointense masses on T1-weighted MRI with very low signal intensity on T2-weighted imaging
- Dense calcifications are often noted
- Scattered areas of high-signal-intensity in the mass indicate either edema or cystic degeneration

Sclerosing Stromal Tumor of Ovary:
- They show hyperintense cystic components or a heterogeneous solid mass of intermediate to high signal intensity on T2-weighted MRI
- There is clear-cut contrast enhancement with internal small cleft and cysts
- The tumors show early peripheral enhancement with centripetal progression on dynamic contrast-enhanced imaging
- Characteristic early enhancement reflects the cellular areas with their prominent vascular networks, whereas an area of prolonged enhancement in the inner portion of the mass represents the collagenous hypocellular area
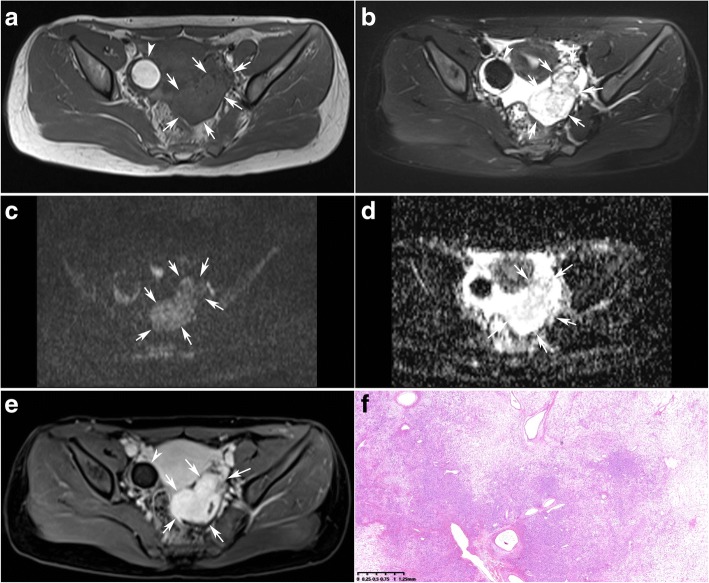
References
- ↑ Jung SE, Rha SE, Lee JM, Park SY, Oh SN, Cho KS, Lee EJ, Byun JY, Hahn ST (July 2005). "CT and MRI findings of sex cord-stromal tumor of the ovary". AJR Am J Roentgenol. 185 (1): 207–15. doi:10.2214/ajr.185.1.01850207. PMID 15972425.
- ↑ Zhang H, Zhang H, Gu S, Zhang Y, Liu X, Zhang G (June 2018). "MR findings of primary ovarian granulosa cell tumor with focus on the differentiation with other ovarian sex cord-stromal tumors". J Ovarian Res. 11 (1): 46. doi:10.1186/s13048-018-0416-x. PMC 5989475. PMID 29871662.
- ↑ Zhao SH, Li HM, Qiang JW, Wang DB, Fan H (August 2018). "The value of MRI for differentiating benign from malignant sex cord-stromal tumors of the ovary: emphasis on diffusion-weighted MR imaging". J Ovarian Res. 11 (1): 73. doi:10.1186/s13048-018-0444-6. PMC 6116557. PMID 30165895.
- ↑ Matsutani H, Nakai G, Yamada T, Yamamoto K, Ohmichi M, Narumi Y (December 2018). "Diversity of imaging features of ovarian sclerosing stromal tumors on MRI and PET-CT: a case report and literature review". J Ovarian Res. 11 (1): 101. doi:10.1186/s13048-018-0473-1. PMC 6302382. PMID 30572921.
- ↑ Stein EB, Wasnik AP, Sciallis AP, Kamaya A, Maturen KE (August 2017). "MR Imaging-Pathologic Correlation in Ovarian Cancer". Magn Reson Imaging Clin N Am. 25 (3): 545–562. doi:10.1016/j.mric.2017.03.004. PMID 28668159.
- ↑ Zhang P, Cui Y, Li W, Ren G, Chu C, Wu X (November 2012). "Diagnostic accuracy of diffusion-weighted imaging with conventional MR imaging for differentiating complex solid and cystic ovarian tumors at 1.5T". World J Surg Oncol. 10: 237. doi:10.1186/1477-7819-10-237. PMC 3514117. PMID 23137333.
- ↑ Mohaghegh P, Rockall AG (October 2012). "Imaging strategy for early ovarian cancer: characterization of adnexal masses with conventional and advanced imaging techniques". Radiographics. 32 (6): 1751–73. doi:10.1148/rg.326125520. PMID 23065168.
- ↑ Forstner R, Meissnitzer M, Cunha TM (2016). "Update on Imaging of Ovarian Cancer". Curr Radiol Rep. 4: 31. doi:10.1007/s40134-016-0157-9. PMC 4826654. PMID 27110476.
- ↑ Imaoka I, Wada A, Kaji Y, Hayashi T, Hayashi M, Matsuo M, Sugimura K (2006). "Developing an MR imaging strategy for diagnosis of ovarian masses". Radiographics. 26 (5): 1431–48. doi:10.1148/rg.265045206. PMID 16973774.
- ↑ Kitajima K, Kaji Y, Sugimura K (2008). "Usual and unusual MRI findings of ovarian fibroma: correlation with pathologic findings". Magn Reson Med Sci. 7 (1): 43–8. PMID 18460848.
- ↑ Chung BM, Park SB, Lee JB, Park HJ, Kim YS, Oh YJ (June 2015). "Magnetic resonance imaging features of ovarian fibroma, fibrothecoma, and thecoma". Abdom Imaging. 40 (5): 1263–72. doi:10.1007/s00261-014-0257-z. PMID 25273949.